Tuberculosis in children dr Ery Olivianto Sp A

Tuberculosis in children dr. Ery Olivianto, Sp. A Dr. dr. Wisnu Barlianto, Sp. A(K) Prof. Dr. dr. HMS. Chandra Kusuma, Sp. A(K) Child Health Department Faculty of Medicine Brawijaya University Saiful Anwar General Hospital 1

Back Ground WHO : 1990 – 1999 � 30 millions died 1/3 world population �infected Per year � 8 milions new cases � 3 milions die 5 – 10% infected �active TB Eradication is difficult : MDR HIV Pandemi BCG : various protection rate 2
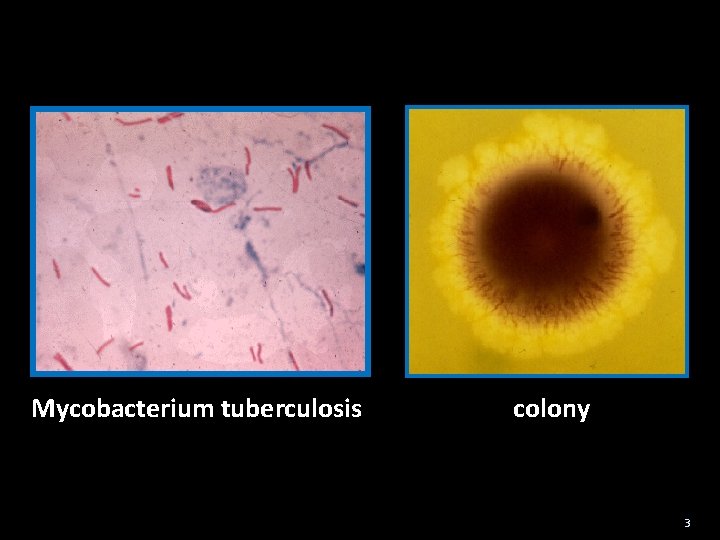
Mycobacterium tuberculosis colony 3
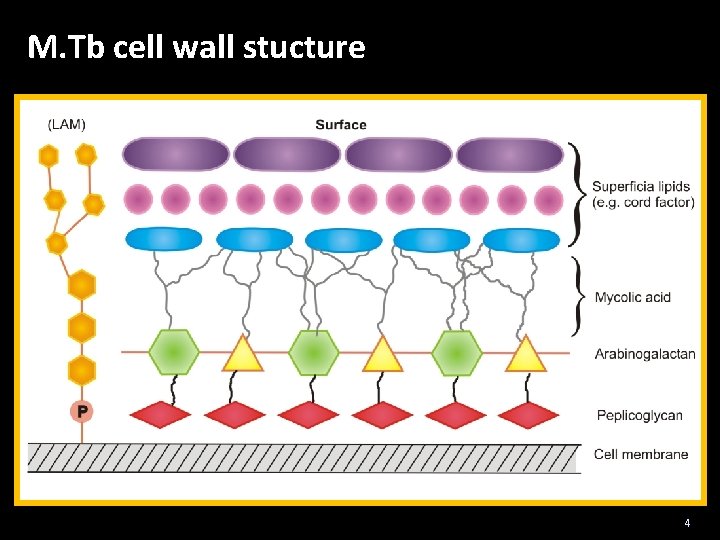
M. Tb cell wall stucture 4
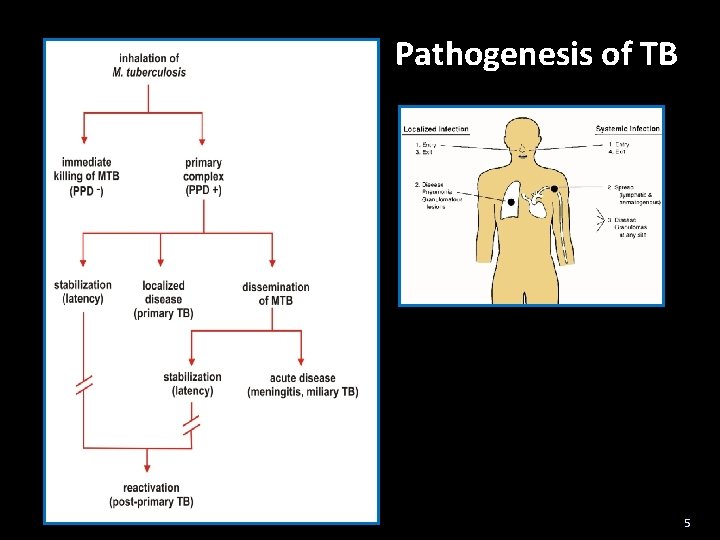
Pathogenesis of TB 5
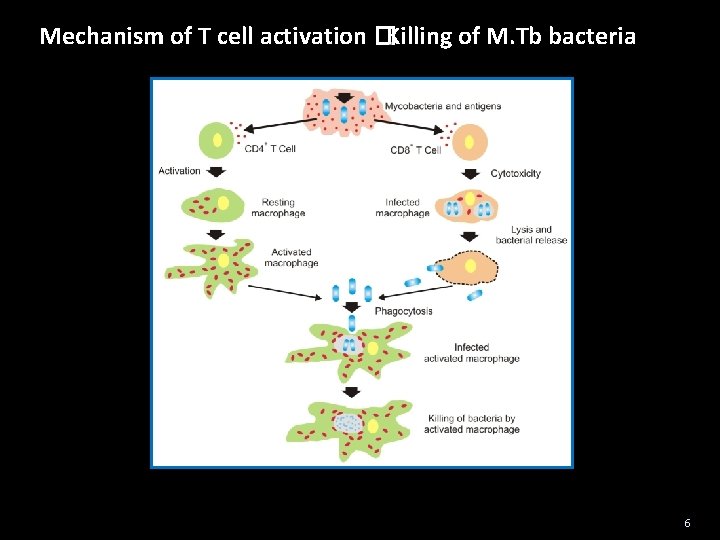
Mechanism of T cell activation �Killing of M. Tb bacteria 6
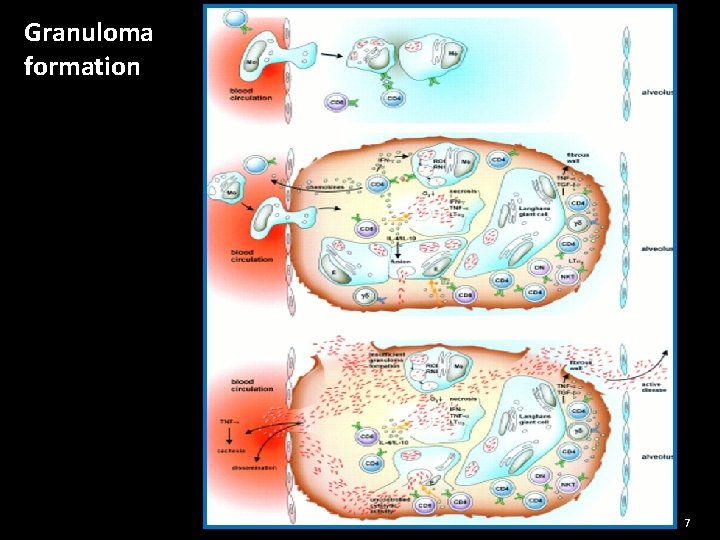
Granuloma formation 7
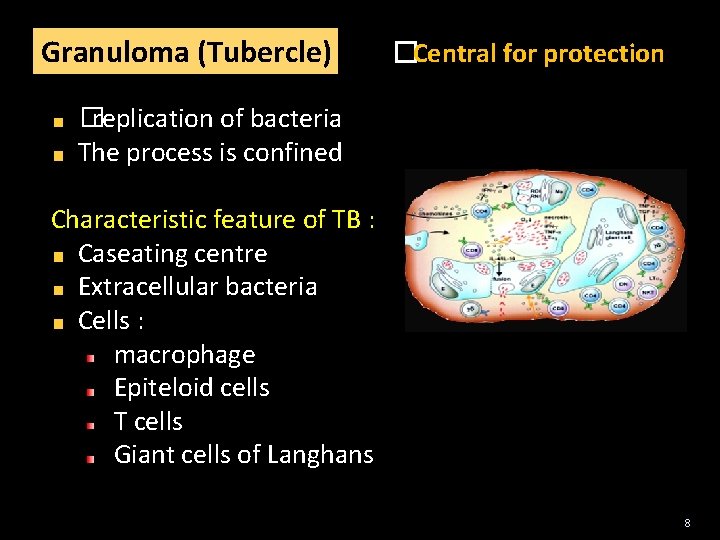
Granuloma (Tubercle) �Central for protection �replication of bacteria The process is confined Characteristic feature of TB : Caseating centre Extracellular bacteria Cells : macrophage Epiteloid cells T cells Giant cells of Langhans 8
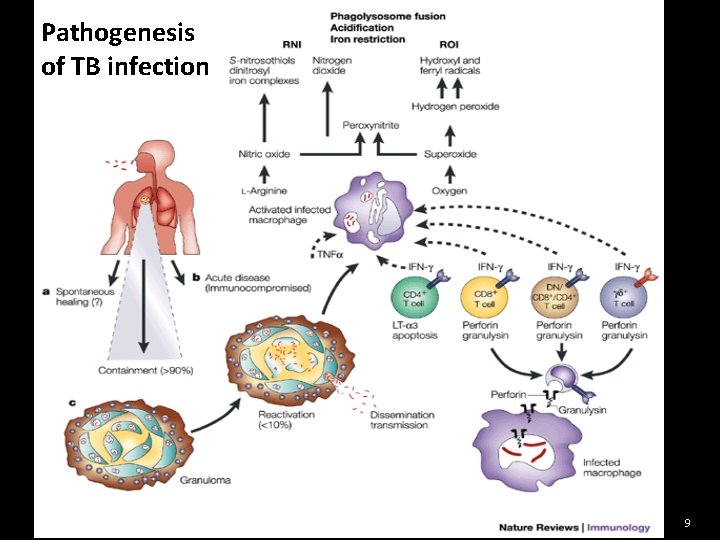
Pathogenesis of TB infection 9

Primary focus: Structural and cellular changes due to response to multiplication of M. Tb in tissues first to be implanted � usually lungs Primary adenitis = regional lymphadenitis Changes in lymphnode secondary to drainage from primary focus Primary nodes : Anatomic reflection of primary focus Primary complex : Primary focus + regional lymphadenitis 10
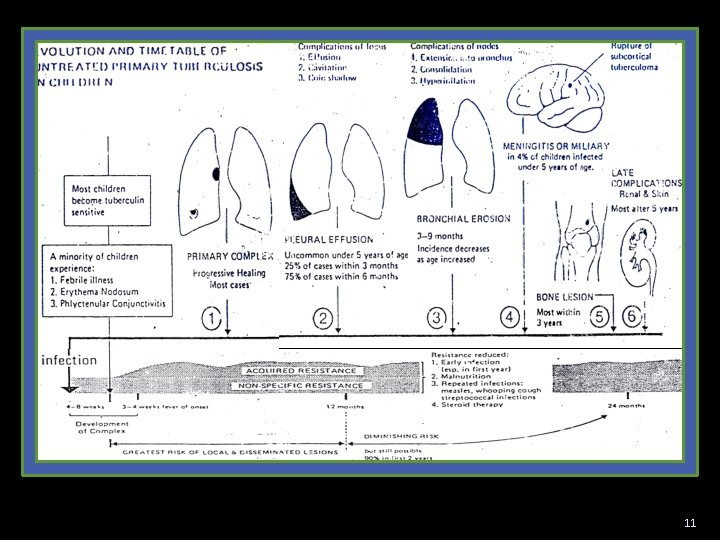
11
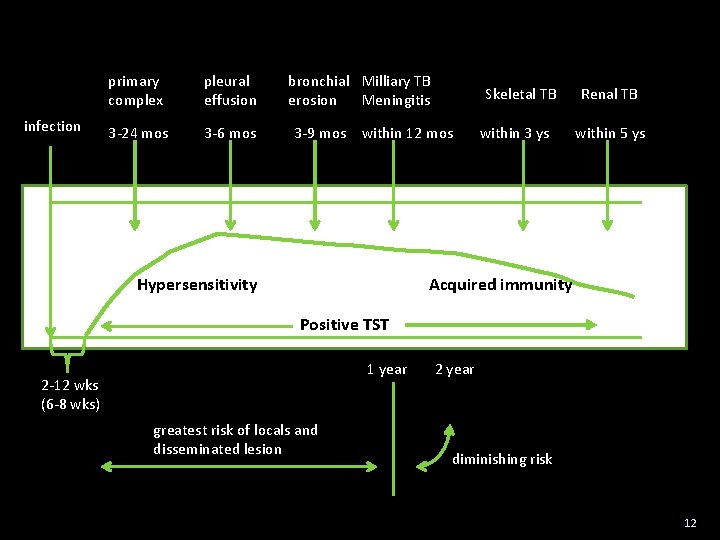
infection primary complex pleural effusion 3 -24 mos 3 -6 mos bronchial Milliary TB erosion Meningitis Skeletal TB 3 -9 mos within 12 mos Hypersensitivity within 3 ys Renal TB within 5 ys Acquired immunity Positive TST 1 year 2 -12 wks (6 -8 wks) greatest risk of locals and disseminated lesion 2 year diminishing risk 12

Primary focus undergo caseation � Focus enlarged �disrupted to bronchus �cavity persisted Round/coin lesions (>>) calsification 1 years Caseation depends on: Host immunity Nutrition Amount of bacteria and its virulence 13
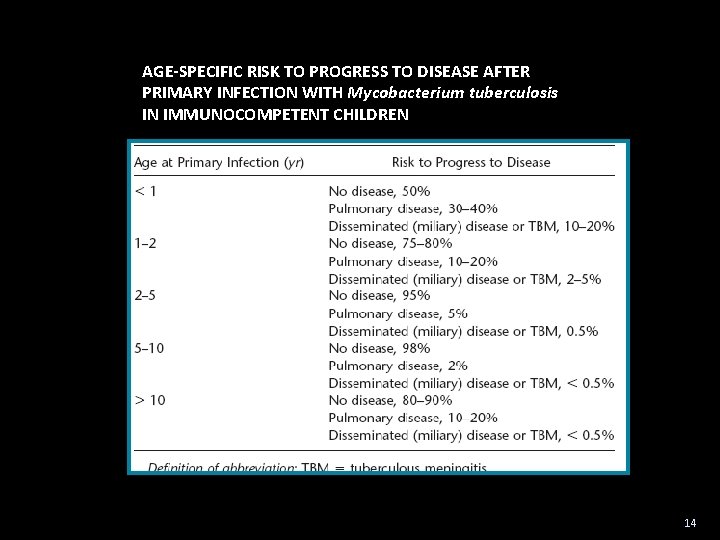
AGE-SPECIFIC RISK TO PROGRESS TO DISEASE AFTER PRIMARY INFECTION WITH Mycobacterium tuberculosis IN IMMUNOCOMPETENT CHILDREN 14

Time table primary focus regional lymphadenitis hematogenic spread 15
Primary focus : Sensitization : Usually single One /both lung(s) near pleura 4 – 8 wks after infection depends on : age nutrition Phenomena of sensitization : 1. Febrile illness lasting 2 -3 wks 2. Phlyctenularis conjuctivitis 3. Erythema nodosum 16

Pleural Effusion Essential sensitivity reaction Massive effusion is rare for < 5 years 75% 6 months after infection 25% 3 months after infection Usually serous (empyema ) 17

Hematogenic spread 1. Miliary dan meningitis TB Within 1 st year after infection More common in younger age Decreased immunity : Malnutrition HIV infection Measles Pertussis Streptococcus infection 18

Hematogenic spread 2. Bone and joint 3 years after infection younger age 3. Renal, skin 5 years after infection first 5 years : rare 10 years : often 19

Regional Lymphnodes Complications are more common (than primary focus) Compliactions occur within first 9 months after infection: 1. Disrupted �abscess 2. Endobronchitis with : a. Incomplete bronchial obstruction b. Complete bronchial obstruction 20

c. Segmental lesions : d. permanent changes (common): Bronchial stricture Bronchiectasis Lung fibrosis e. Bronchopneumonia : Immunity Bacteria 21

Diagnosis TBC in children 1. History 2. Contact /sources 3. Tuberculin Test (Mantoux) 4. Physic Diagnostic 5. X – ray 6. AFB /Hystopathology 22

Algorithm for Early Detection and Referral for Childhood Tuberculosis in Indonesia Suspected TB: Close contact with adult with AFB sputum (+) Early reaction of BCG (in 3 -7 days) Weight loss with no apparent cause, or underweight with no improvement in 1 month with adequate nutritional support (failure to thrive) Prolonged /recurrent fever with no apparent cause Cough more than 3 weeks Specific enlargement of superficial lymph node Scrofuloderma Phlychten conjunctivitis Tuberculin test positive (> 10 mm) Radiological findings suggestive TB If > 3 positive Next page 23
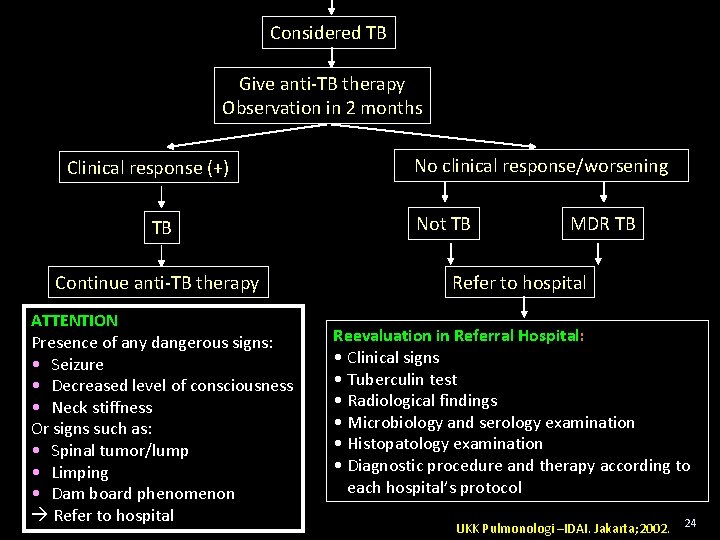
Considered TB Give anti-TB therapy Observation in 2 months Clinical response (+) TB Continue anti-TB therapy ATTENTION Presence of any dangerous signs: • Seizure • Decreased level of consciousness • Neck stiffness Or signs such as: • Spinal tumor/lump • Limping • Dam board phenomenon Refer to hospital No clinical response/worsening Not TB MDR TB Refer to hospital Reevaluation in Referral Hospital: • Clinical signs • Tuberculin test • Radiological findings • Microbiology and serology examination • Histopatology examination • Diagnostic procedure and therapy according to each hospital’s protocol UKK Pulmonologi –IDAI. Jakarta; 2002. 24
History : Chronic Fever Chronic cough Source of infection: Body Weight Difficult Malaise Important: Activity Diagnosis Therapy 25
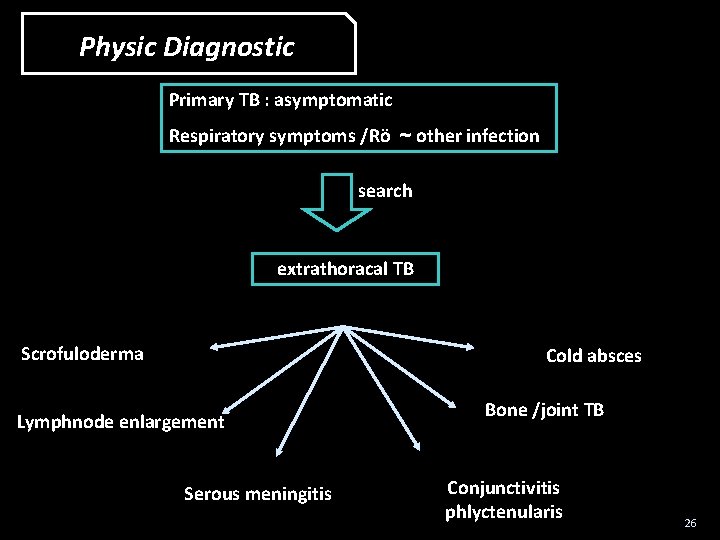
Physic Diagnostic Primary TB : asymptomatic Respiratory symptoms /Rö ~ other infection search extrathoracal TB Scrofuloderma Cold absces Lymphnode enlargement Serous meningitis Bone /joint TB Conjunctivitis phlyctenularis 26

TUBERCULIN TEST Important role in diagnostic Agents : OT 0, 9 mg PPD RT-23 2 TU / PPD S 5 TU Intra-cutaneusly, antebrachii volar area Intepretation: 48 -72 h after injection Transversal diameter of induration, ≠ erythema 27
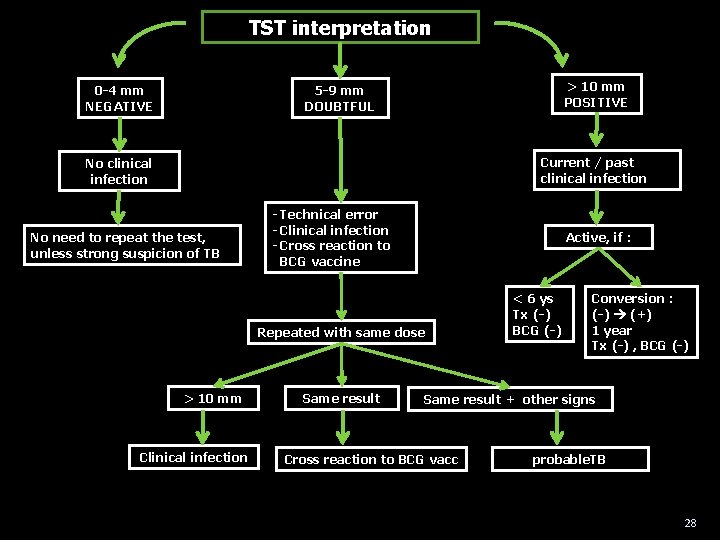
TST interpretation 0 -4 mm NEGATIVE > 10 mm POSITIVE 5 -9 mm DOUBTFUL Current / past clinical infection No need to repeat the test, unless strong suspicion of TB - Technical error - Clinical infection - Cross reaction to BCG vaccine Active, if : Repeated with same dose > 10 mm Clinical infection Same result < 6 ys Tx (-) BCG (-) Conversion : (-) (+) 1 year Tx (-) , BCG (-) Same result + other signs Cross reaction to BCG vacc probable. TB 28

False Negative : Positive : Post BCG vaccination Mycobacterium atypis Incubation : 2 – 10 mgg Morbus Hansen Severe TB : miliary/meningitis Severe Malnutrition Dehydration Diseases with high fever Tx. Corticosteroid / immunosupresive Certain infections : Morbili (or its vaccination) : 10 ds – 6 wks Rubella : 1 – 3 wks Pertussis HIV 29

Notifications: I. Tuberculin Test (Mantoux) Should be routinally started at 6 – 8 mos �every year if contact (+) and TST (-) �repeat after 10 wks still in close �TST each 3 mos Interpretation of TST post BCG difficult Induration varies : 0 – 20 mm Kendig 1972 : susp. active infection if 15 mm Lotte 1971 : active infection if: pre /post BCG 18 mm 30

Notifications: II. BCG Scar (+) not exclude the disease �active infection when BCG vaccination : Within incubation period Active TB already Infected during incubation of BCG Not effective vaccine 31

CHEST X RAY Not specific Normal chest X ray : not excluding the process DIAGNOSIS CAN NOT BE ACHIEVED BASE ON CHEST X RAY Strongly suggestive TB: miliary paratracheal lymphnode enlargement 32
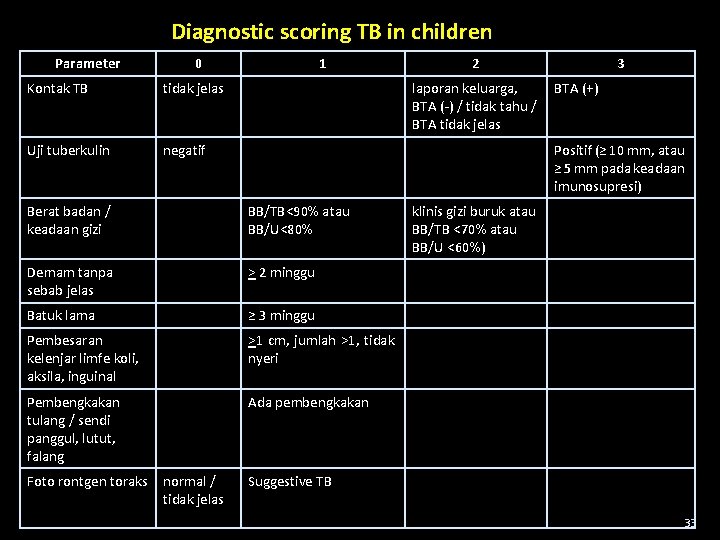
Diagnostic scoring TB in children Parameter 0 Kontak TB tidak jelas Uji tuberkulin negatif 1 laporan keluarga, BTA (-) / tidak tahu / BTA tidak jelas BB/TB<90% atau BB/U<80% Demam tanpa sebab jelas > 2 minggu Batuk lama ≥ 3 minggu Pembesaran kelenjar limfe koli, aksila, inguinal >1 cm, jumlah >1, tidak nyeri Pembengkakan tulang / sendi panggul, lutut, falang Ada pembengkakan normal / tidak jelas 3 BTA (+) Positif (≥ 10 mm, atau ≥ 5 mm pada keadaan imunosupresi) Berat badan / keadaan gizi Foto rontgen toraks 2 klinis gizi buruk atau BB/TB <70% atau BB/U <60%) Suggestive TB 33

Note : • • • Diagnosis using scoring system performend by a doctor If scrofuloderma is present �diagnose Tuberculosis Body weight assessed at the time of admission (moment opname) Fever /cough which not respond to standard therapy Chest x ray is not main diagnostic tool in childhood TB Children with rapid BCG reaction shoud be evaluated using scoring system • diagnosis TB when the score > 6, (max 14) 34

Diagnosis of TB in children If you find the diagnosis of TB in children easy, you probably overdiagnosing TB If you find the diagnosis of TB in children difficult, you are not alone It is easy to over-diagnose TB in children It is also easy to miss TB in children Carefully assess all the evidence, before making the diagnosis Anthony Harries & Dermot Maher, 1997 35

Hospitalization 1. Ascertain diagnosis: repeated AFB, biopsy 2. Initial treatment in : severe. TB /life threatening /infants 3. Corticosteroid /surgical treatment 4. Severe adverse reaction to TB regiment 5. Treatment for concomitant disease 6. Initial treatment for children whose parents /environments are not adequate 36
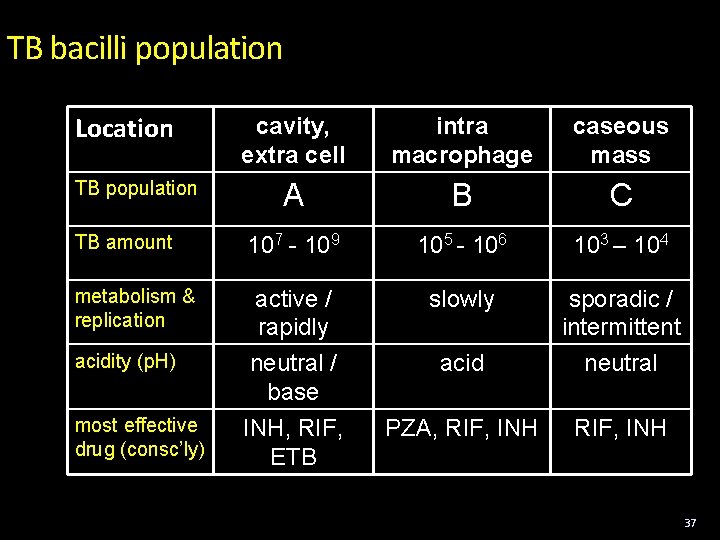
TB bacilli population Location cavity, extra cell intra macrophage caseous mass A B C TB amount 107 - 109 105 - 106 103 – 104 metabolism & replication active / rapidly neutral / base INH, RIF, ETB slowly acid sporadic / intermittent neutral PZA, RIF, INH TB population acidity (p. H) most effective drug (consc’ly) 37
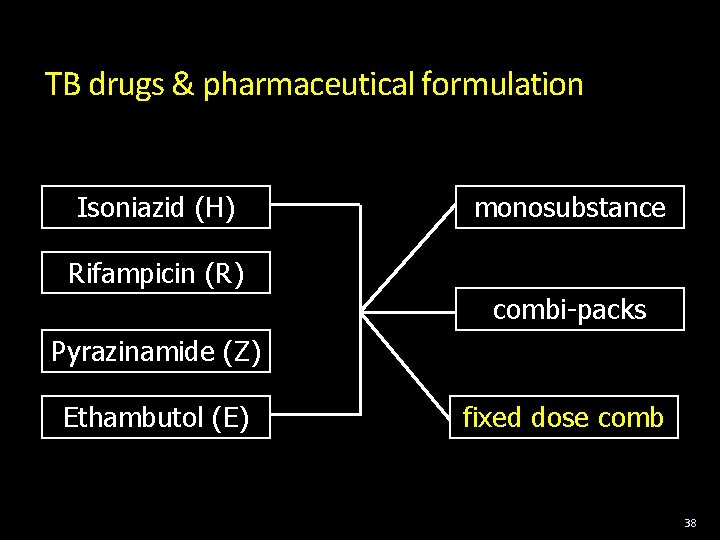
TB drugs & pharmaceutical formulation Isoniazid (H) monosubstance Rifampicin (R) combi-packs Pyrazinamide (Z) Ethambutol (E) fixed dose comb 38
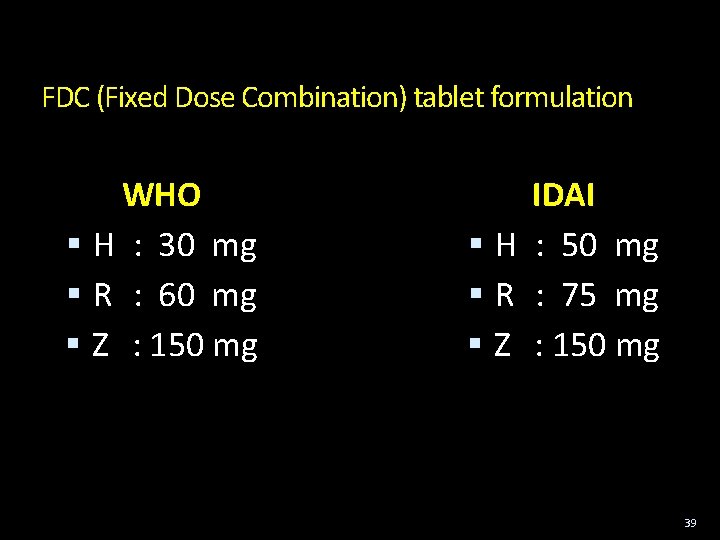
FDC (Fixed Dose Combination) tablet formulation WHO H : 30 mg R : 60 mg Z : 150 mg IDAI H : 50 mg R : 75 mg Z : 150 mg 39
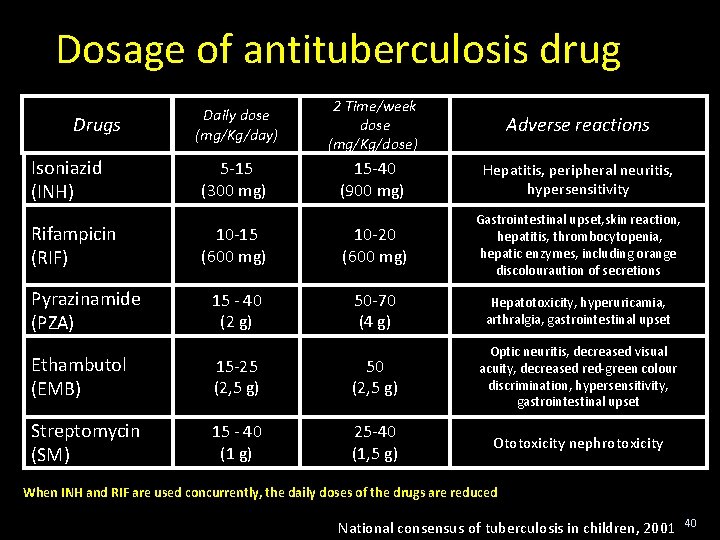
Dosage of antituberculosis drug Drugs Isoniazid (INH) Rifampicin (RIF) Pyrazinamide (PZA) Daily dose (mg/Kg/day) 2 Time/week dose (mg/Kg/dose)) Adverse reactions 5 -15 (300 mg)) 15 -40 (900 mg)) Hepatitis, peripheral neuritis, hypersensitivity 10 -15 (600 mg)) 10 -20 (600 mg) Gastrointestinal upset, skin reaction, hepatitis, thrombocytopenia, hepatic enzymes, including orange discolouraution of secretions 15 - 40 (2 g) 50 -70 (4 g) Hepatotoxicity, hyperuricamia, arthralgia, gastrointestinal upset Ethambutol (EMB) 15 -25 (2, 5 g) 50 (2, 5 g) Optic neuritis, decreased visual acuity, decreased red-green colour discrimination, hypersensitivity, gastrointestinal upset Streptomycin (SM) 15 - 40 (1 g) 25 -40 (1, 5 g) Ototoxicity nephrotoxicity When INH and RIF are used concurrently, the daily doses of the drugs are reduced National consensus of tuberculosis in children, 2001 40
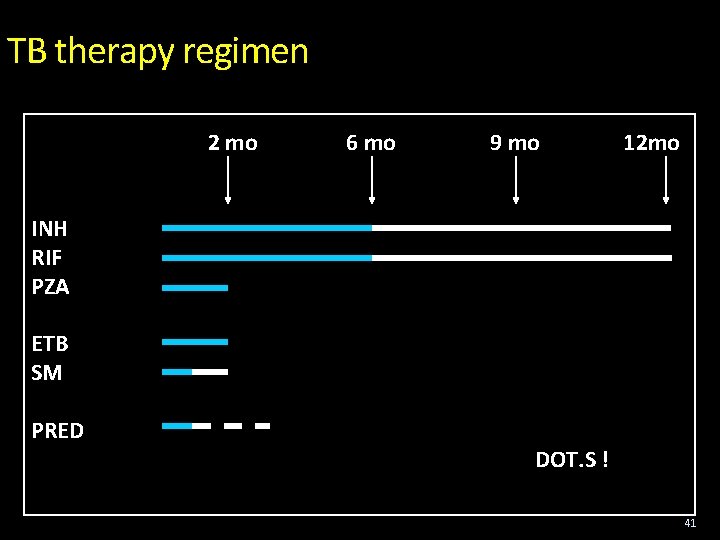
TB therapy regimen 2 mo 6 mo 9 mo 12 mo INH RIF PZA ETB SM PRED DOT. S ! 41

Therapy problem solutions DOTS : Directly Observe Treatment Short-course FDC : Fixed Dose Combination i. e. >2 drugs in one tablet / capsule in a fixed dose formulation 42

Corticosteroid Meningitis Serositis (pleura, pericard, peritoneal) Endotracheal Miliary 43

STOP therapy Regular treatment : 6 bln – 1 ½ th improvement, BW , fever (-) Chest x ray �improvement ESR , if previous ESR Source of infection (-) If source (+) : continue with IPT (INH prophylaxis treatment) 44

Side Effects Streptomycin : 20 mg/kg. BW/day Nefrotoxic : rare N. VIII disturbance (mainly vestibular nerve) Ataxia Vertigo rare : deafness Pyrazinamide : 30 – 40 mg/kg. BW/day Hepatotoxic 45

INH : 10 – 20 mg/kg. BW/day – 1 dd Periferal neuritis : rare due to B 6 defisiensi Hepatotoxic : previous liver disorder other hepatotoxic drug : rifampicin Other : GI irritability hypersensitive reaction neurology : psichosis seizure confusion 46

ETB : 15 – 20 mg/kg. BW/day – 1 DD Reversible occular complications Blurred Color blindness Narrowed visual field 47

Rifampicin : 15 – 20 mg/kg. BW/day – 1 dd Orange discoloration : saliva, tear, conjunctiva GI. Symptom Hepatotoxic Trombocytopenia – leukopenia “Influenza syndrome” Fever headache Malaise “Respiratory syndrome” Tightness Wheezing 48

INH Prophylaxis Single treatment : 5 -10 mg/kg. BW/day 1. Infection prophylaxis Healthy child Exposed to adult with AFB (+) TST (-) 3 mos TST (+) 1 y 49

2. Disease prophylaxis prevent the disease (current /past TB infection): 2. 1. latent TB: TST (+), BCG (-), Tx (-), < 6 y, healthy conversion (+), BCG (-), Tx (-) duration : 1 year 2. 2. prevent exacerbation: healed �morbili, pertussis Narcose Tx. Corticosteroid duration : 6 wks 50

Advantage of INH prophylaxis Proven to be effective Not interupt TST result if infection (+) Disadvantage of INH prophylaxis Non complience in prophylactic medication Pharmacologic effect on neonates : data 51

PREVENTION INH prophylaxis Avoid contact active TB BCG Infants of mother with active TB 50% disease within 1 year Prophylaxis is important!! INH BCG ? 52

Advantage of BCG Effective, one dose Toksisitoxicity (-) no need long term follow-up Disadvantage of BCG Individual response varies interupt TST test result need isolation/weaned until TST (+) (2 months) 53
- Slides: 53