TUBERCULOSIS Dr Vindya Rajakaruna MBBS COLOMBO MYCOBACTERIUM Acidfast

TUBERCULOSIS Dr. Vindya Rajakaruna MBBS (COLOMBO)

MYCOBACTERIUM • Acid-fast bacilli - after staining they resist decolorisation with strong acids • This is due to the complex composition of the cell wall which have a high lipid content. The lipids form complexes with the dye • Very slow growing – even the fastest growing mycobacteria take about 3 days to appear as colonies

• Aerobic bacilli • Non motile, non capsulated, non sporing bacteria • Require enriched media for growth – Egg based or agar based media enriched with serum or albumin is used

Mycobacterium tuberculosis • • Slender, beaded bacilli Generation time 18 hours Resistant to dry Destroyed by phenolic disinfectants and exposure to UV light • Takes 6 – 8 weeks to form colonies • Able to resist destruction by the lysosomal enzymes

Pathogenesis- Primary Infection • Inhaled aerosols Engulfed by alveolar macrophages Bacilli replicate Macrophages die • Infected macrophages migrate local lymph nodes • Develop Ghon’s focus Primary complex • Cell mediated immune response ( T lymphocytes ) stops cycle of destruction and spread of the pathogen • EVIDENCE Viable but. OF non. INFECTION replicating. WITH bacilli. Mpresent in TUBERCULOSIS macrophages Chest x-ray / positive skin test

Post Primary Infection • This occurs due to reinfection or reactivation • Due to high immunological reactivity activated macrophages liberate proteases which cause tissue destruction, necrosis, softening and liquifaction leading to caseation • Leads to wasting and evening pyrexia
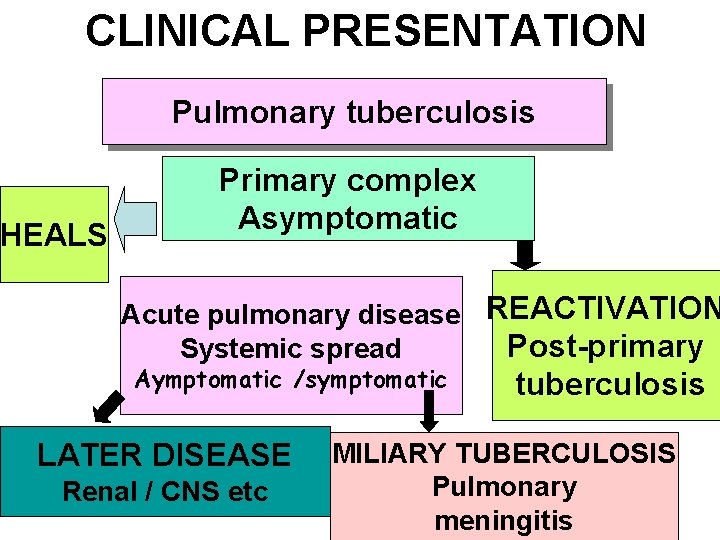
CLINICAL PRESENTATION Pulmonary tuberculosis HEALS Primary complex Asymptomatic Acute pulmonary disease REACTIVATION Post-primary Systemic spread Aymptomatic /symptomatic LATER DISEASE Renal / CNS etc tuberculosis MILIARY TUBERCULOSIS Pulmonary meningitis

DIAGNOSIS 1. Evidence of infection a. Chest x-ray - hilar lymphadenopathy calcification of primary focus/LN b. Delayed hypersensitivity response to purified protein derivative (PPD) MANTOUX /HEAF TEST 2. Evidence of active disease a. Sputum for AFB positive 3. Evidence of active disease a. Indirect evidence of infection b. Direct evidence of infection (Mantoux) PCR / culture

TREATMENT • Anti-tuberculous drugs – INAH – Rifampicin – Ethambutol – Pyrazinamide • DOT • Multi-drug resistant tuberculosis

PREVENTION • Incidence declined before availability of antituberculous drugs • Improved social conditions - housing /nutrition • Case detection & treatment • Contact tracing • Evidence of infection / disease • Treatment of infected / diseased contacts ROLE OF IMMUNIZATION BCG (bacillus Calmette Guerin)
- Slides: 10