Tuberculosis and HIV HAIVN Harvard Medical School AIDS

Tuberculosis and HIV HAIVN Harvard Medical School AIDS Initiative in Vietnam

Learning Objectives By the end of this session, participants should be able to: n Explain the significance of TB/HIV coinfection n Describe the clinical presentation of TB in PLHIV n Outline TB treatment regimens n Explain drug-resistant TB n Describe common interactions between ARV and TB drugs 2

TB Epidemiology (1) n n Vietnam is ranked 12 th in the world for incident TB The incidence in the general population is 180/100, 000 3
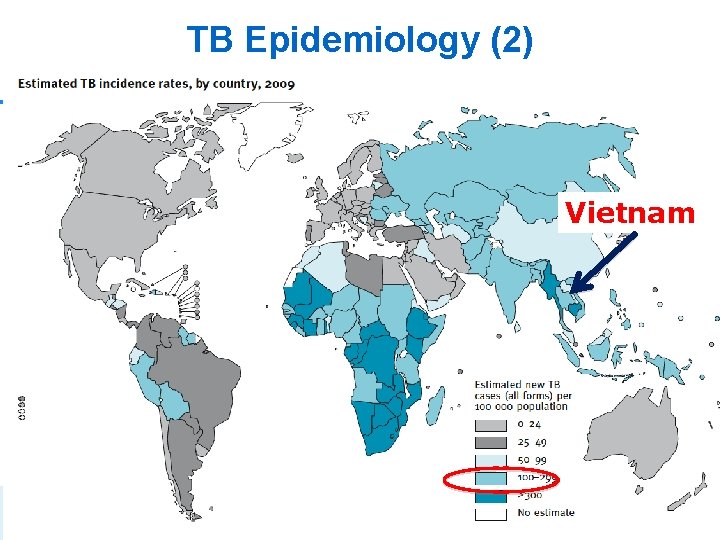
TB Epidemiology (2) Global TB Control. WHO 2010 Vietnam 4
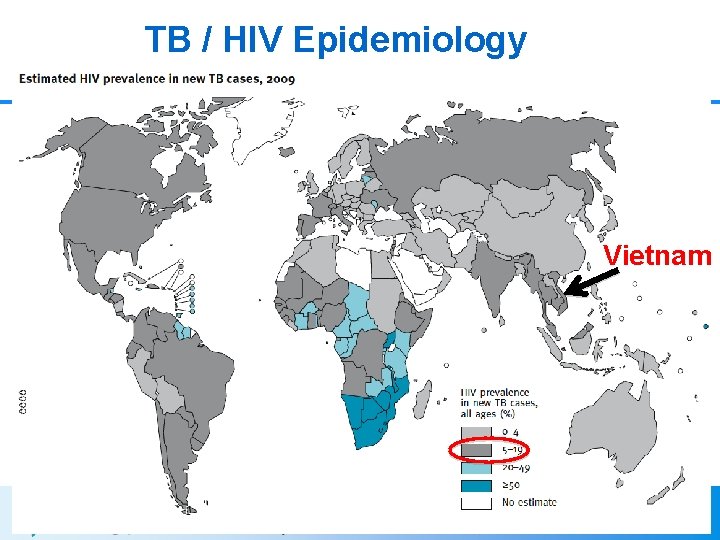
TB / HIV Epidemiology Global TB Control. WHO 2010 Vietnam 5

TB/HIV Interaction (1) n n TB is the most common OI in developing countries and the most common cause of death among HIV patients TB infection: • speeds the progression of HIV by increasing viral replication • worsens immunological suppression in HIV patients n HIV increases mortality among patients with TB 6

TB/HIV Interaction (2) n n Most TB cases are n HIV greatly caused by increases the reactivation of chance for latent TB infection to become active In Vietnam, an estimated 50 -60% Status Risk of active of the population TB infection has latent TB HIV negative 10% lifetime risk infection HIV negative 1% risk per year IDU HIV infected 10% risk per year 7

Clinical Presentation of PLHIV with TB

The Effects of HIV on TB HIV worsens the signs and symptoms of TB, as shown in the chart Ref: Chest 1994; 106: 1471 -6 Symptom /Sign HIV Positive HIV Negative Dyspnea 97% 81% Fever 79% 62% Sweats 83% 64% Weight loss 89% 83% Diarrhea Hepatomegaly Splenomegaly Lymphadenopathy 23% 41% 40% 35% 4% 21% 15% 13% 9

Clinical Presentation and CD 4 (1) 10

Clinical Presentation and CD 4 (2) Signs and Symptoms of Pulmonary TB CD 4 > 500 CD 4 < 200 • “Typical” presentation: • Fever • Cough • Weight loss • Bloody sputum • “Atypical” presentation: • fever of unknown etiology • weight loss • minimal cough • Extra-pulmonary disease more likely 11 • Sputum sample more likely to be negative
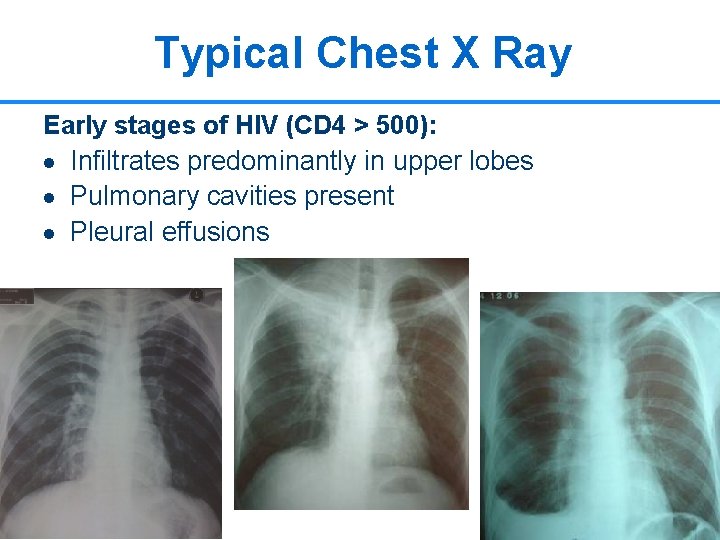
Typical Chest X Ray Early stages of HIV (CD 4 > 500): · Infiltrates predominantly in upper lobes · Pulmonary cavities present · Pleural effusions 12
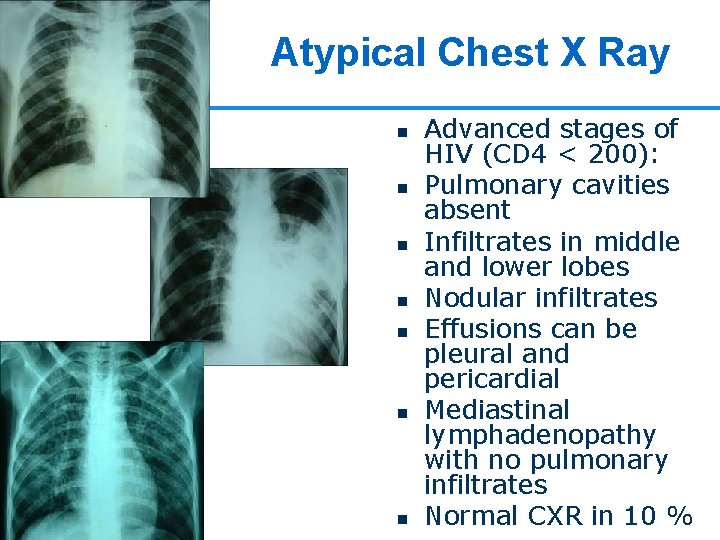
Atypical Chest X Ray n n n n Advanced stages of HIV (CD 4 < 200): Pulmonary cavities absent Infiltrates in middle and lower lobes Nodular infiltrates Effusions can be pleural and pericardial Mediastinal lymphadenopathy with no pulmonary infiltrates 13 Normal CXR in 10 %
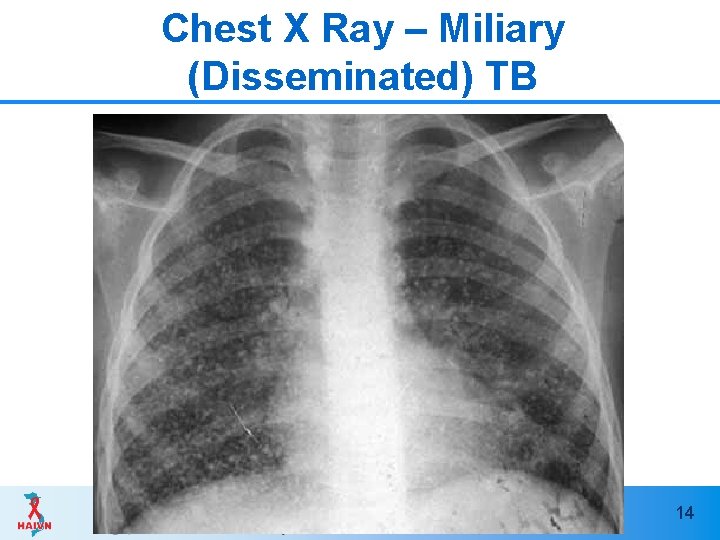
Chest X Ray – Miliary (Disseminated) TB 14

Extra-pulmonary TB (1) n Extra-pulmonary Tuberculosis (EPTB) occurs when bacteria spread outside of the lung and cause disease • Occurs more commonly in people with weak immune systems e. g. PLHIV • May occur with or without concomitant pulmonary TB 15

Extra-pulmonary TB (2) n n Occurs most often when a person’s CD 4 < 100 Most commonly manifests as: • • • Abdominal and lymph node TB (very often) TB meningitis (5 -10%), Tuberculoma Pericarditis Pleural effusion Cutaneous Renal 16
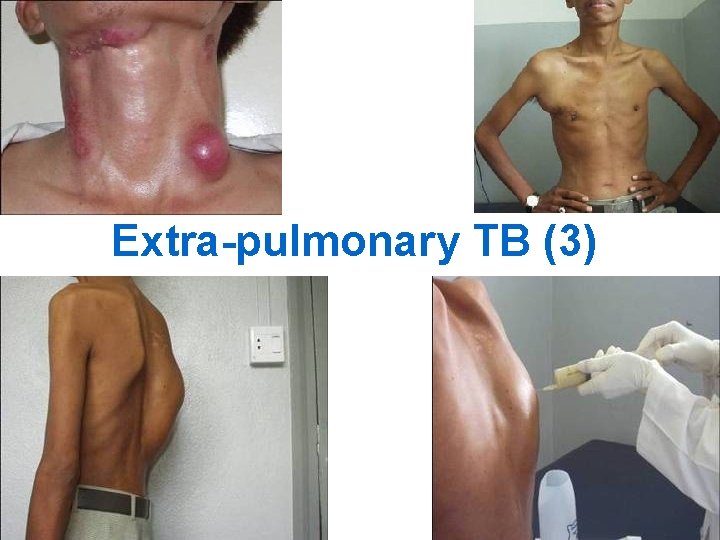
Extra-pulmonary TB (3) 17
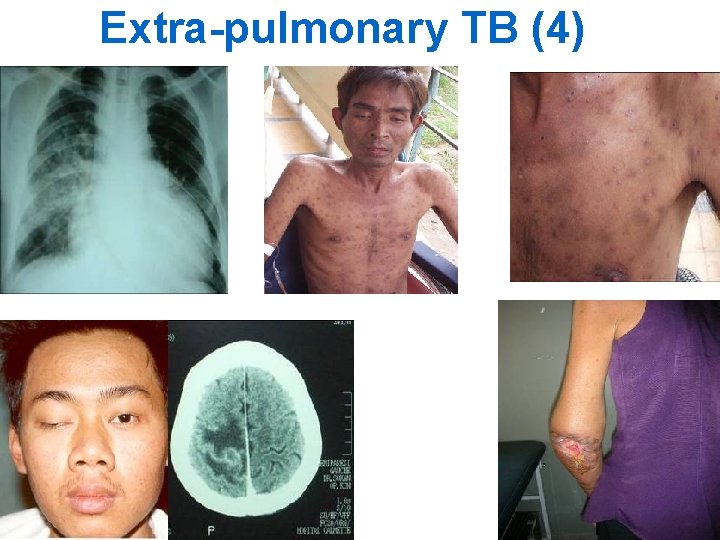
Extra-pulmonary TB (4) 18

Sputum Smear and HIV Status (1) n n n Diagnose TB by examining stained sputum samples for presence of acid fast bacilli (AFB) Sputum smear is the most rapid and inexpensive diagnostic test for TB The sensitivity of TB sputum smears depends on many factors including HIV status 19
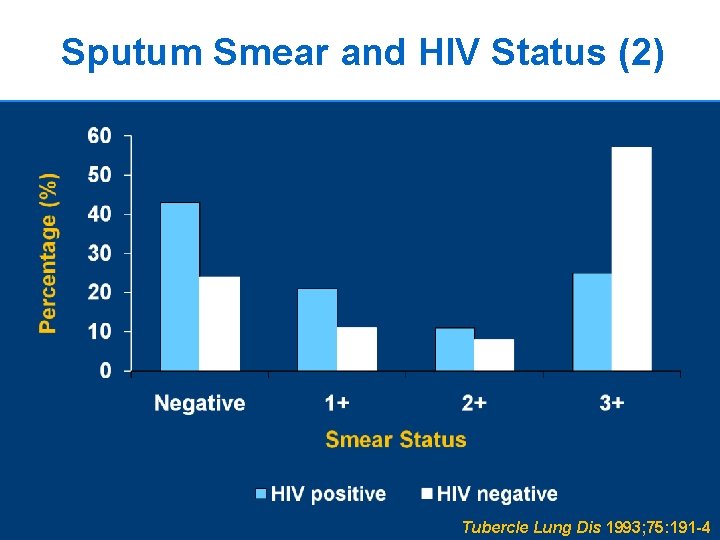
Sputum Smear and HIV Status (2) 20 Tubercle Lung Dis 1993; 75: 191 -4

TB HIV Co-infection Key Clinical Practice Points n n “Typical” pulmonary TB less common “Atypical”, smear negative and extrapulmonary TB more common • WHO and Vietnam MOH guidelines allow TB treatment on clinical suspicion without positive smear test 21

MOH and WHO Recommend: “THE ANTIBIOTIC TRIAL” n n When indicated, use one course of broad spectrum antibiotics including coverage for typical and atypical causes of community acquired pneumonia Under such circumstances, avoid Fluoroquinolones to prevent undue delay in diagnosis of TB 22

Treatment Regimens for PLHIV with TB
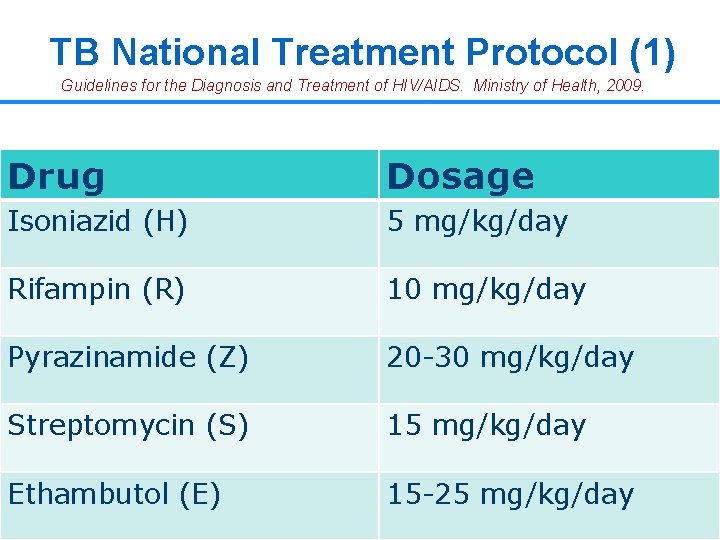
TB National Treatment Protocol (1) Guidelines for the Diagnosis and Treatment of HIV/AIDS. Ministry of Health, 2009. Drug Dosage Isoniazid (H) 5 mg/kg/day Rifampin (R) 10 mg/kg/day Pyrazinamide (Z) 20 -30 mg/kg/day Streptomycin (S) 15 mg/kg/day Ethambutol (E) 15 -25 mg/kg/day 24

TB National Treatment Protocol (2) For newly diagnosed TB cases, regimen 1: n 2 S(E)HRZ / 6 HE n 2 S(E)RHZ / 4 RH* * applied only if direct observation continued in maintenance phase Guidelines for the Diagnosis and Treatment of HIV/AIDS. Ministry of Health, 2009. 25

TB National Re-Treatment Protocol (3) n For recurrent TB and failure to Regimen 1, there is Regimen 2: • 2 SHRZE for 2 months: 5 drug THEN • 1 HRZE for 1 month: 4 drugs THEN • 5 H 3 R 3 E 3 for 5 months: 3 drugs given 3 times per week n Total duration: 8 months Guidelines for the Diagnosis and Treatment of HIV/AIDS. Ministry of Health, Vietnam. 2009. 26

TB Treatment: Special Situations n Some special situations require a more aggressive course of treatment, including: • • Miliary TB Pericarditis Meningitis Spondilitis with neurological complications n For pregnant women: avoid streptomycin - can cause permanent deafness in baby • Use ethambutol instead 27

Small Group Activity: Case Study 1

Drug Resistant TB (1) Drug resistant TB is TB for which anti-TB drugs have little or no effect against the TB causing agent Type Meaning Mono-resistance Resistant to only 1 anti-TB drug Poly-resistance (PDR) Resistant to more than 1 anti-TB drug, but not INH and RIF combination Multi-drug resistance (MDR) Resistant to at least INH and RIF, the 2 most effective anti-TB drugs Extensively drug MDR and further resistance to any -resistant (XDR) fluoroquinolone and at least one of three injectable second-line drugs: 29 amikacin, kanamycin, or capreomycin

Drug Resistant TB (2) Causes of drug resistant TB include: n Inadequate treatment regimens n Interrupted availability to drug treatment n Poor quality of drug treatment n Incomplete treatment adherence n Results from spontaneous mutations of MTB exposed to drugs Quy HT, Buu TN et al Int J Tuberc Lung Dis 2006; 10(2): 160 -166. 30

Multi Drug-Resistant (MDR) TB in Vietnam n Among reported cases in 2008, it is estimated that: • 2. 7% of new TB cases had MDR-TB • 19% of re-treatment cases had MDR-TB n 3500 MDR-TB cases among reported pulmonary TB cases in 2009 Global TB Control. WHO 2010 31

TB and ARV Drug Interactions (1) • Rifampicin decreases drug levels of some ARVs: ARV Effect Treatment/Solution NVP 37% Switch to EFV, if available (NVP OK, if necessary*) EFV 25% EFV still effective PI (LPV/r, IDV) 80 -90% Do not use PI with RIF: refer to specialty center for treatment 32
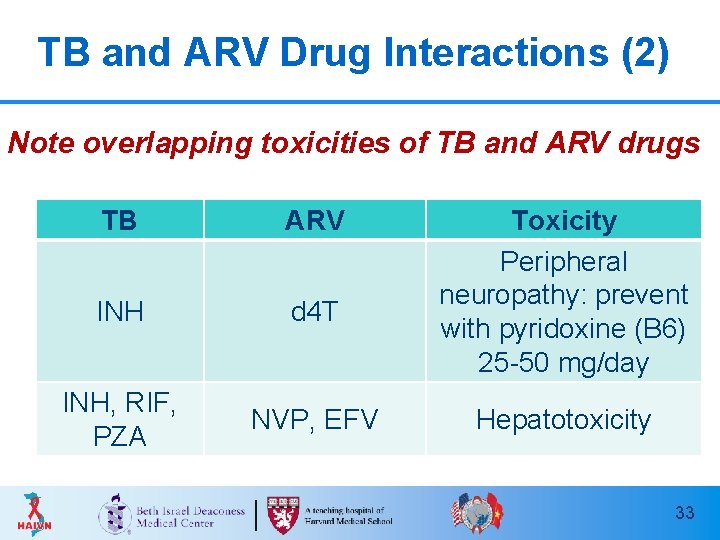
TB and ARV Drug Interactions (2) Note overlapping toxicities of TB and ARV drugs TB ARV INH d 4 T INH, RIF, PZA NVP, EFV Toxicity Peripheral neuropathy: prevent with pyridoxine (B 6) 25 -50 mg/day Hepatotoxicity 33
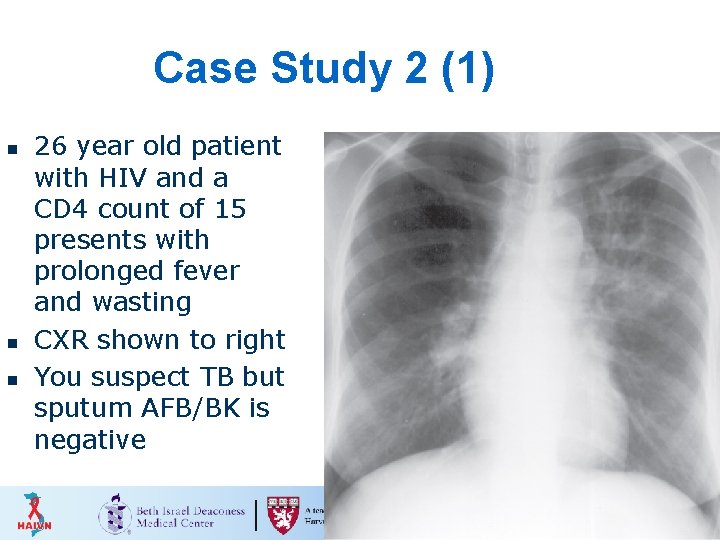
Case Study 2 (1) n n n 26 year old patient with HIV and a CD 4 count of 15 presents with prolonged fever and wasting CXR shown to right You suspect TB but sputum AFB/BK is negative 34
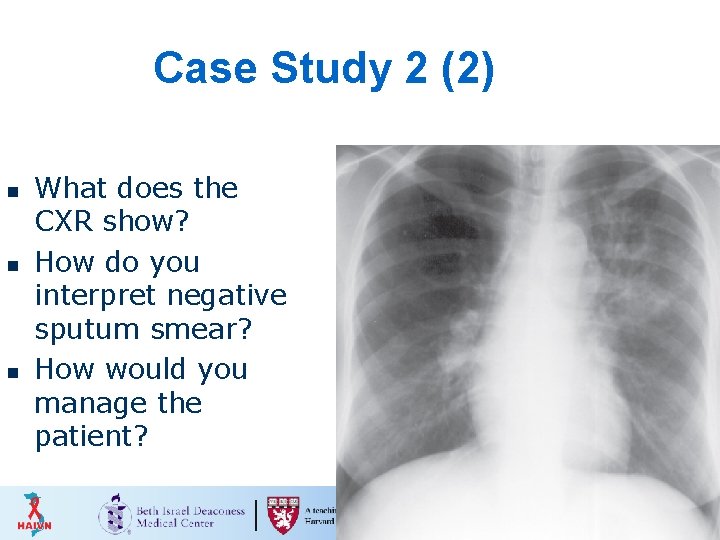
Case Study 2 (2) n n n What does the CXR show? How do you interpret negative sputum smear? How would you manage the patient? 35

Key Points n n TB/HIV co-infection is common among PLHIV in Vietnam HIV infection increases risk for active TB infection by over 100 fold Clinical presentation of TB varies by CD 4 count TB treatment regimens are the same for both HIV+/- patients 36

Thank you! Questions?
- Slides: 37