Trochanteric fractures AO Trauma Basic Principles Course Learning

Trochanteric fractures AO Trauma Basic Principles Course

Learning objectives • Describe the (biological) difference between intra- and extracapsular proximal femoral fractures • Describe the biomechanics of extracapsular fractures and the (resulting) choice of implant • Explain the rationale of intra- as opposed to extramedullary fixation • Describe the causes of failure concerning reduction and placement of implant
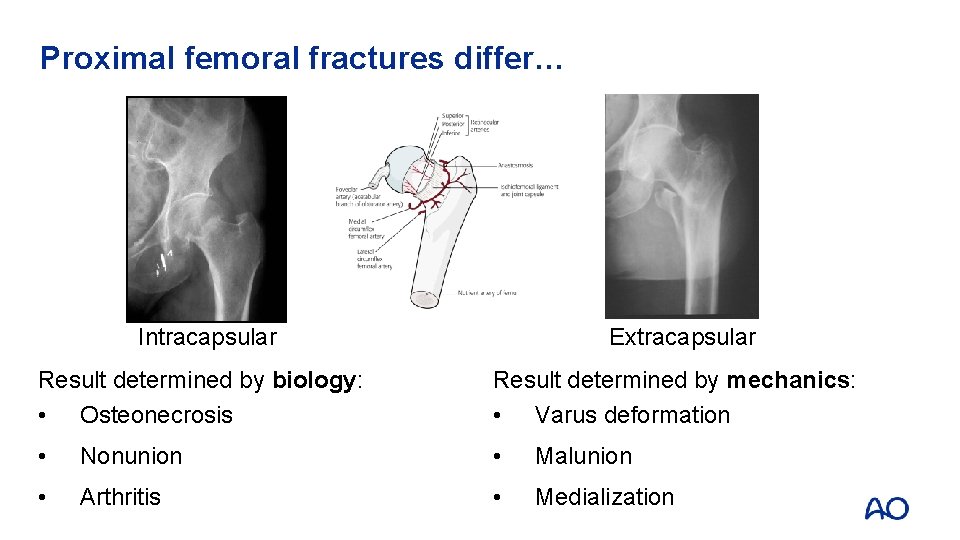
Proximal femoral fractures differ… Intracapsular Extracapsular Result determined by biology: • Osteonecrosis Result determined by mechanics: • Varus deformation • Nonunion • Malunion • Arthritis • Medialization

Trochanteric fractures—etiology Low-energy injury: • Usually elderly patients High-energy injury: • Usually younger patients
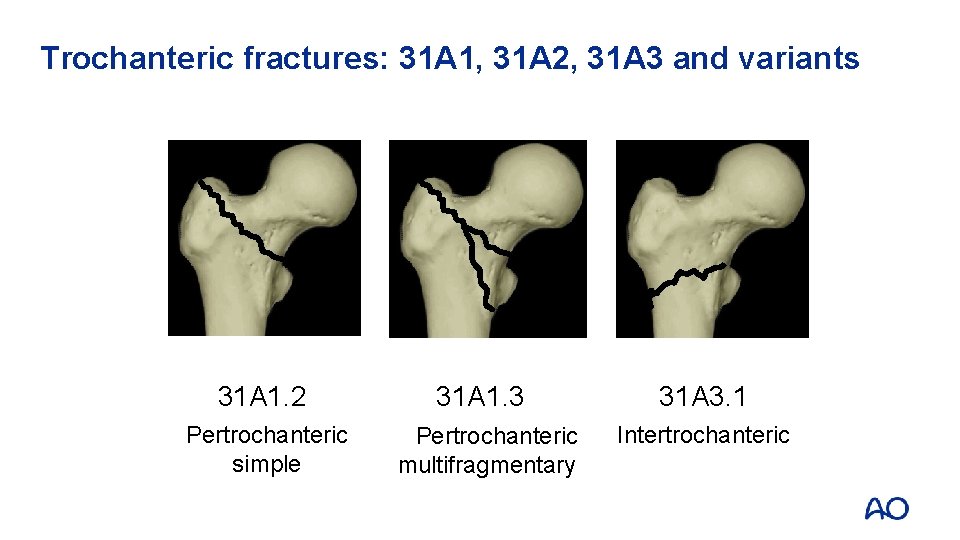
Trochanteric fractures: 31 A 1, 31 A 2, 31 A 3 and variants 31 A 1. 2 Pertrochanteric simple 31 A 1. 3 Pertrochanteric multifragmentary 31 A 3. 1 Intertrochanteric

What does the patient want? Treatment that enables the patient to return to, at least, pretrauma mobility as soon as possible
What does a doctor want for his/her patient ? • Early full weight bearing • Technically easy treatment

Treatment options • Nonoperative: • • About 14 weeks bed rest Virtually impossible for many reasons Secondary displacement obligatory Operative

Type of bone healing preferred: • Primary: • No means open, anatomical reduction • Secondary: • Given the biology, to be preferred
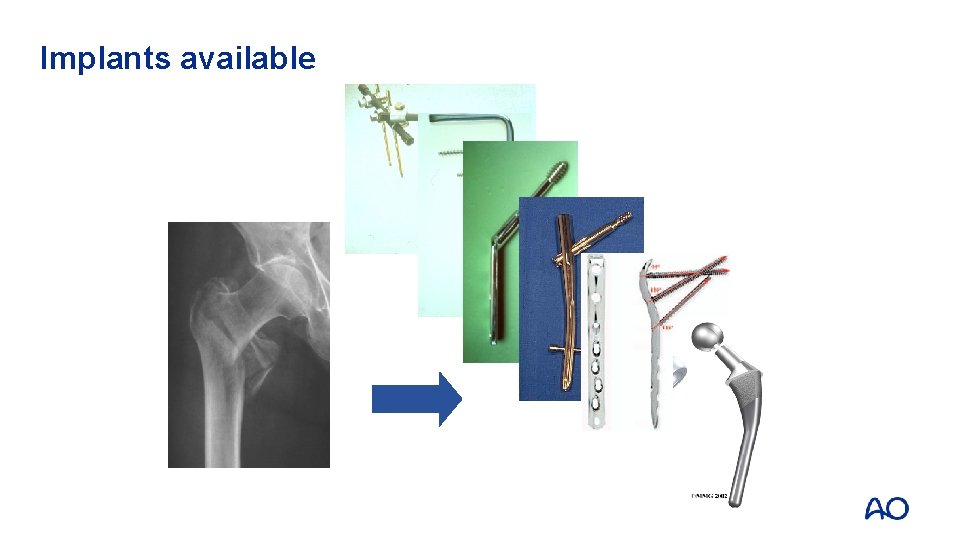
Implants available
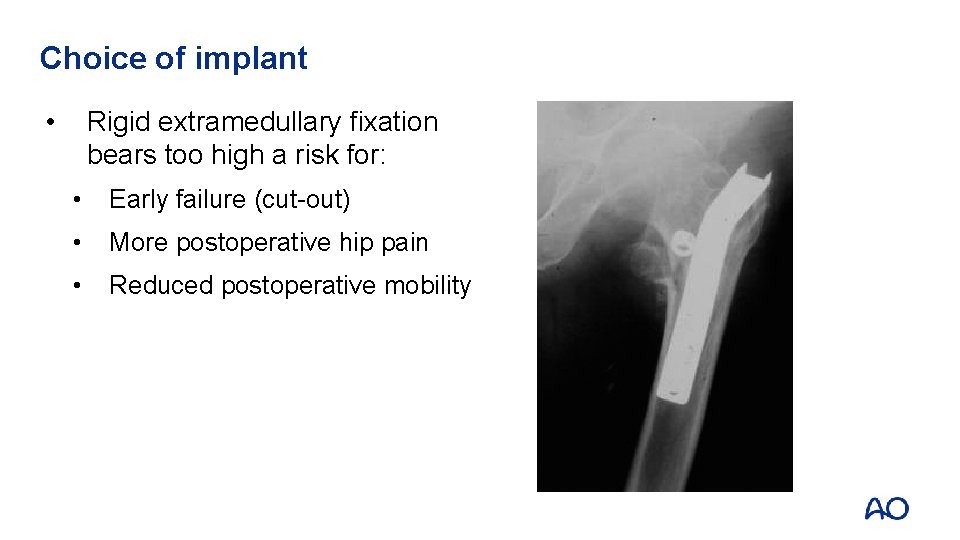
Choice of implant • Rigid extramedullary fixation bears too high a risk for: • Early failure (cut-out) • More postoperative hip pain • Reduced postoperative mobility
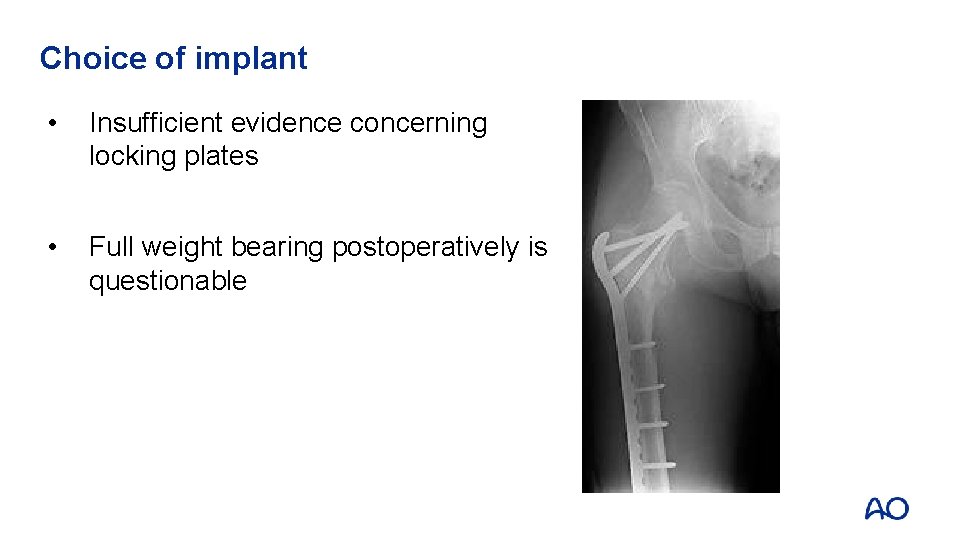
Choice of implant • Insufficient evidence concerning locking plates • Full weight bearing postoperatively is questionable
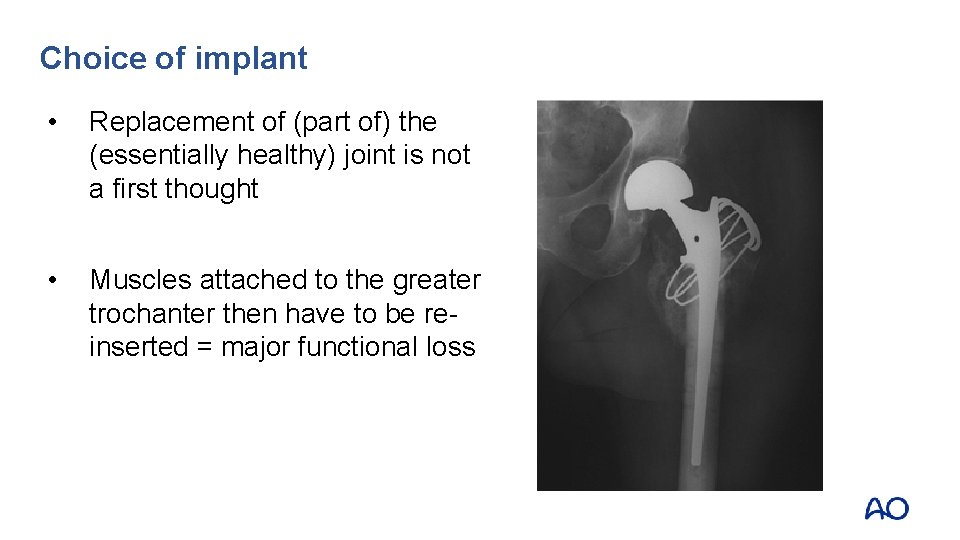
Choice of implant • Replacement of (part of) the (essentially healthy) joint is not a first thought • Muscles attached to the greater trochanter then have to be reinserted = major functional loss
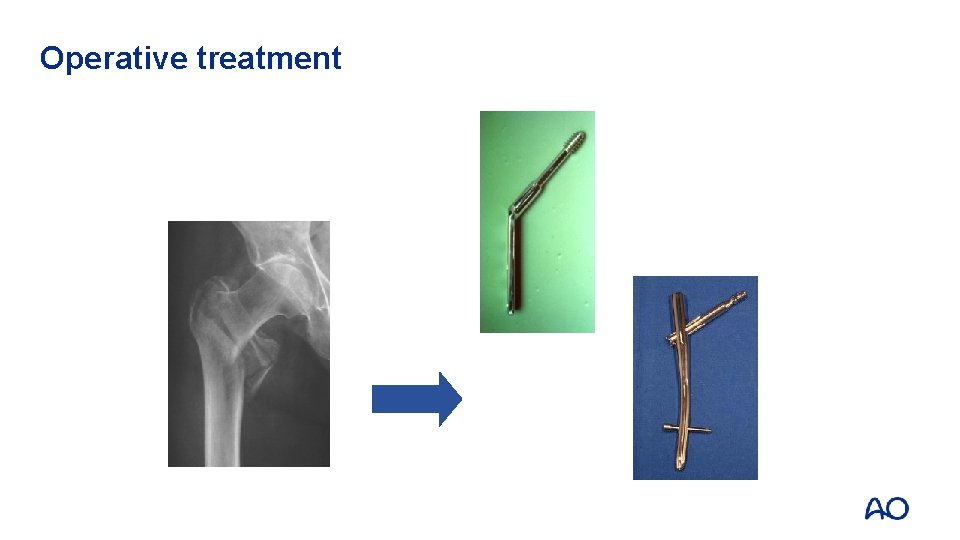
Operative treatment
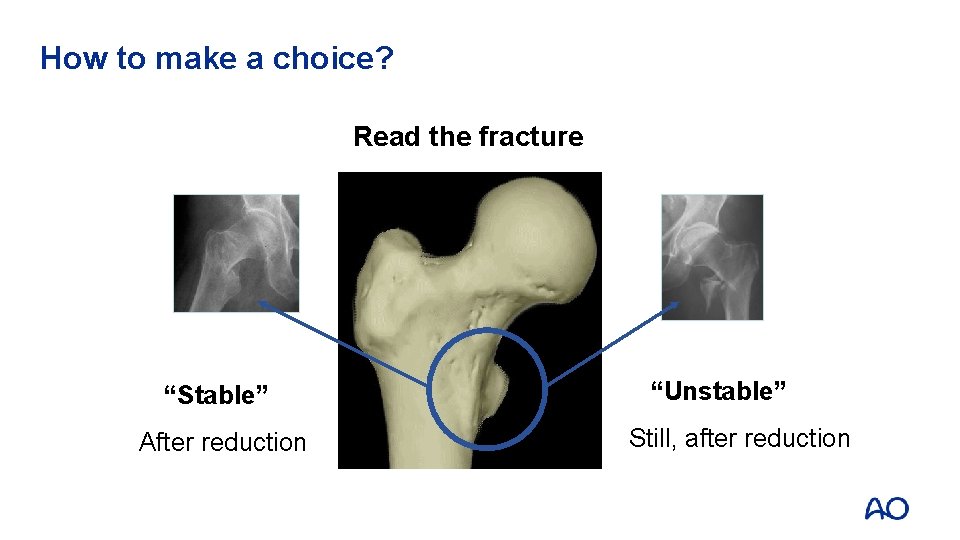
How to make a choice? Read the fracture “Stable” After reduction “Unstable” Still, after reduction
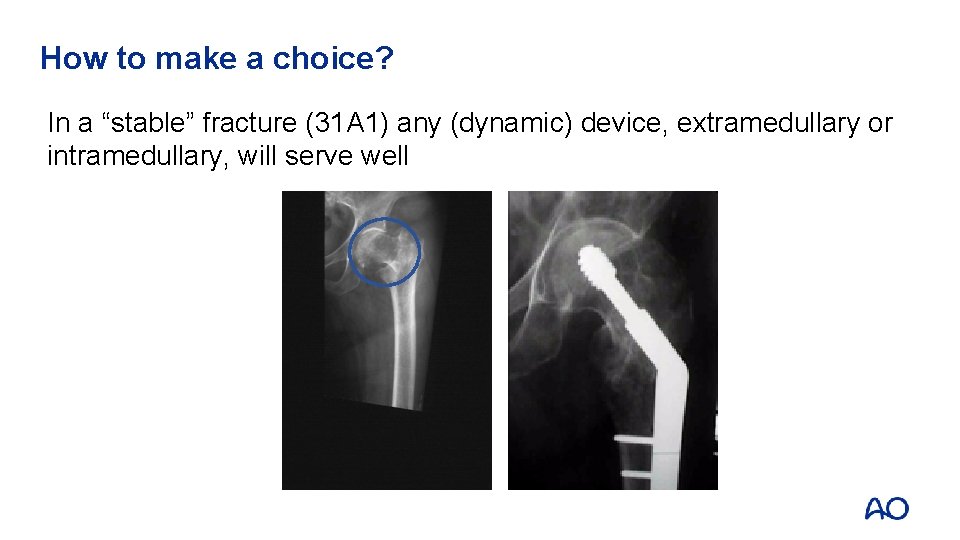
How to make a choice? In a “stable” fracture (31 A 1) any (dynamic) device, extramedullary or intramedullary, will serve well

How to reduce the fracture • Close reduction over fracture table: • Reducible and stable • Reducible by other means and unstable • If no close reduction, then open reduction achieving anteromedial contact and fixation with the implant
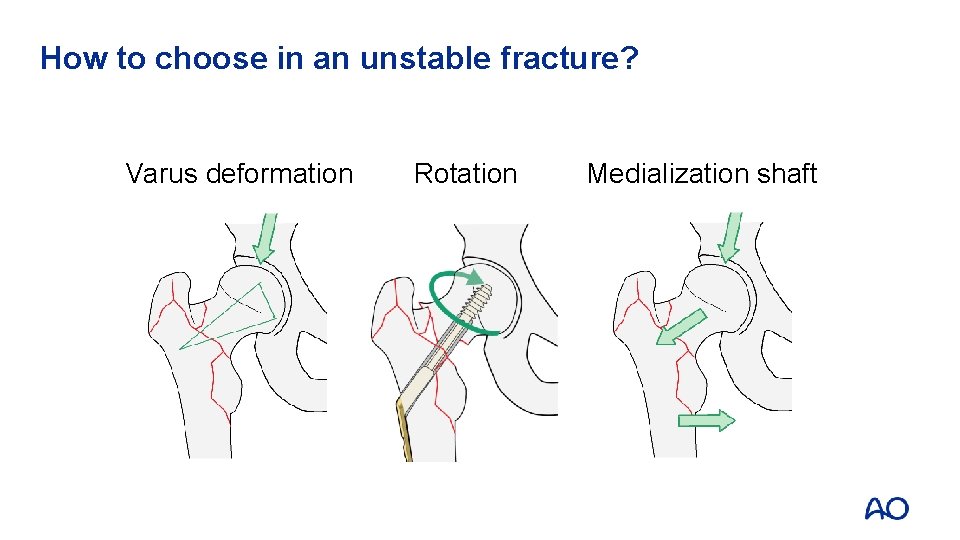
How to choose in an unstable fracture? Varus deformation Rotation Medialization shaft
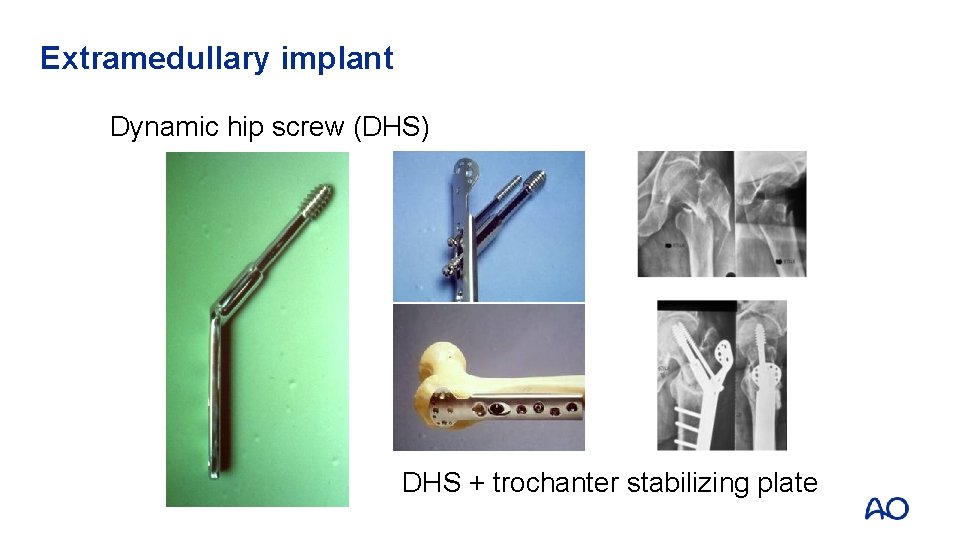
Extramedullary implant Dynamic hip screw (DHS) DHS + trochanter stabilizing plate
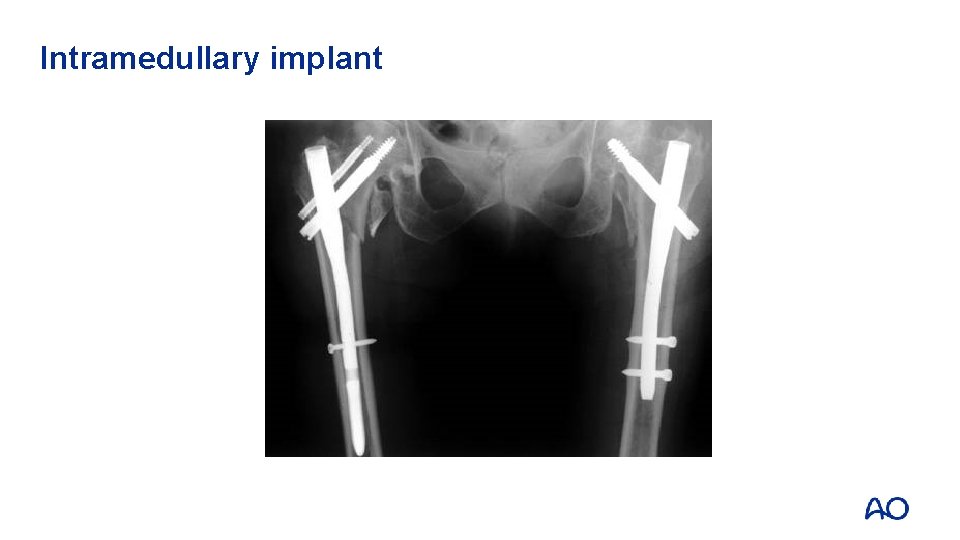
Intramedullary implant

Extra- or intramedullary implant Extramedullary: Intramedullary • (Nearly) anatomical reconstruction • Nonanatomical reconstruction • Less strong implant • Semi-open procedure • Semi-closed procedure • Partial weight bearing • Direct full weight bearing

Evidence • Nail versus sliding hip screw—no difference: • Huang X, Leung F, Xiang Z, et al. Proximal femoral nail versus dynamic hip screw fixation for trochanteric fractures: a meta-analysis of randomized controlled trials. Scientific. World. Journal. 2013; 2013: 805805. • Matre K, Vinje T, Havelin LI, et al. TRIGEN INTERTAN intramedullary nail versus sliding hip screw: a prospective, randomized multicenter study on pain, function, and complications in 684 patients with an intertrochanteric or subtrochanteric fracture and one year of follow-up. J Bone Joint Surg Am. 2013 Feb 6; 95(3): 200– 208.

Evidence slight change Intramedullary vs extramedullary: • …. tendency to better regain of mobility … with an intramedullary nail. . . (Parker [Injury. 2017; 48: 2762– 2767]) • …. supports the use of intramedullary nails for A 3 fractures (Bretherton et al [J Orthop Trauma. 2016 Dec; 30(12): 642– 646])
Take-home messages • 31 A 1 (“stable”) fractures: • Any sliding device • 31 A 2 and 31 A 3 (“unstable”) fractures: • Intramedullary device • (Sliding hip screw with a lateral support device)
- Slides: 24