Trigeminal Nerve V Lecture Objectives Discuss briefly how

Trigeminal Nerve (V)

Lecture Objectives • Discuss briefly how the face is developed. • Follow up the course of trigeminal nerve from its point of central connections, exit and down to its target areas. • Describe briefly important cranial reflexes involving the face and trigeminal nerve.
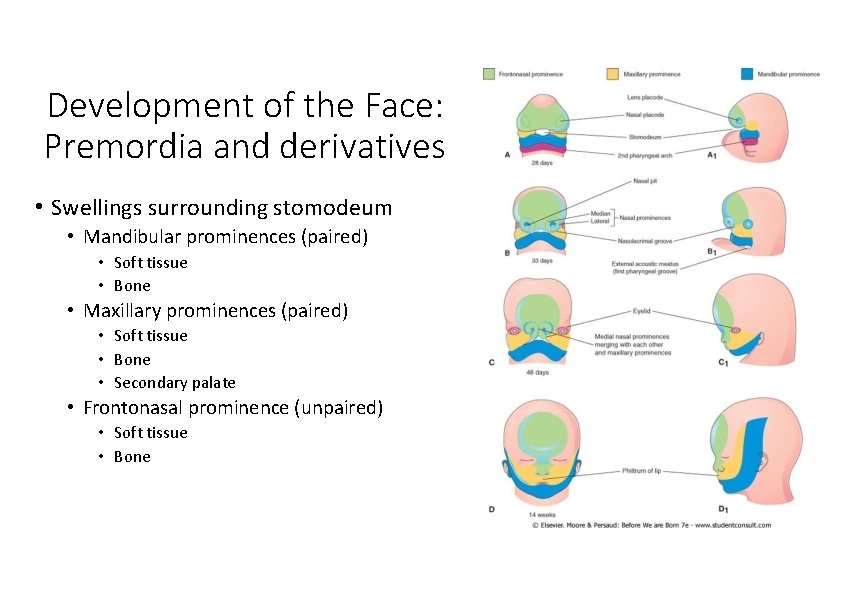
Development of the Face: Premordia and derivatives • Swellings surrounding stomodeum • Mandibular prominences (paired) • Soft tissue • Bone • Maxillary prominences (paired) • Soft tissue • Bone • Secondary palate • Frontonasal prominence (unpaired) • Soft tissue • Bone
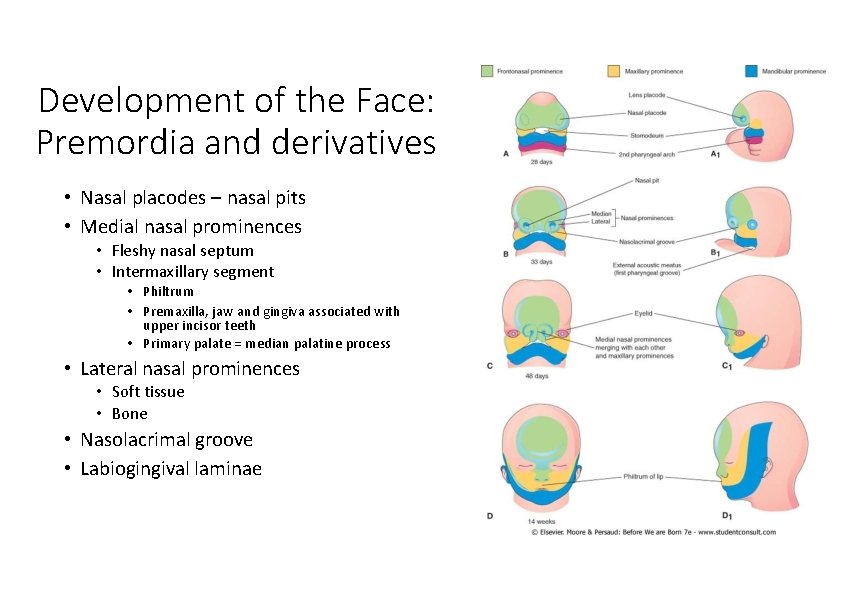
Development of the Face: Premordia and derivatives • Nasal placodes – nasal pits • Medial nasal prominences • Fleshy nasal septum • Intermaxillary segment • Philtrum • Premaxilla, jaw and gingiva associated with upper incisor teeth • Primary palate = median palatine process • Lateral nasal prominences • Soft tissue • Bone • Nasolacrimal groove • Labiogingival laminae
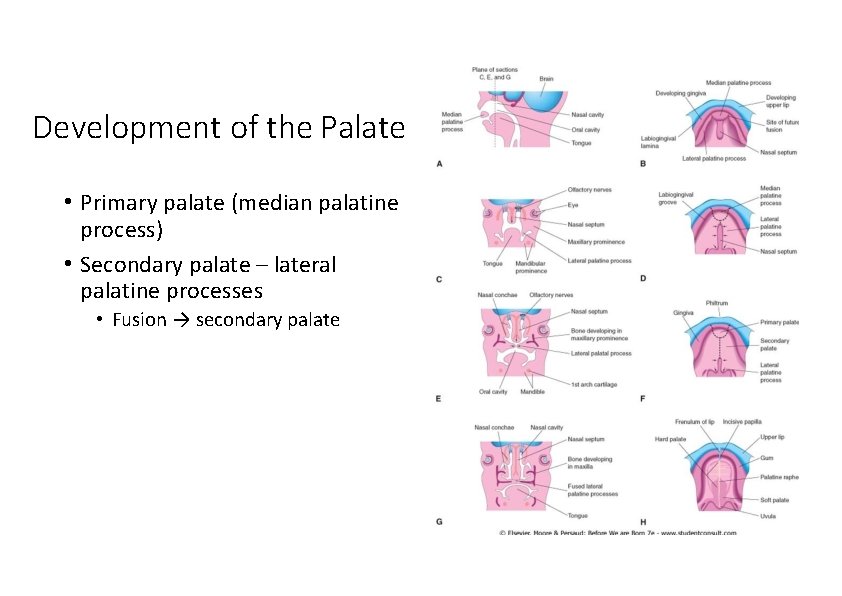
Development of the Palate • Primary palate (median palatine process) • Secondary palate – lateral palatine processes • Fusion → secondary palate
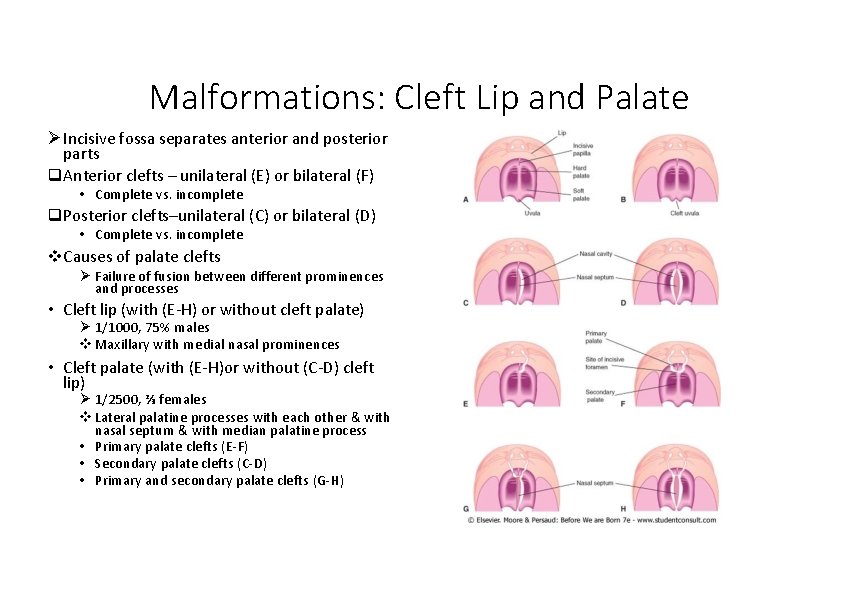
Malformations: Cleft Lip and Palate Incisive fossa separates anterior and posterior parts Anterior clefts – unilateral (E) or bilateral (F) • Complete vs. incomplete Posterior clefts–unilateral (C) or bilateral (D) • Complete vs. incomplete Causes of palate clefts Failure of fusion between different prominences and processes • Cleft lip (with (E‐H) or without cleft palate) 1/1000, 75% males Maxillary with medial nasal prominences • Cleft palate (with (E‐H)or without (C‐D) cleft lip) 1/2500, ⅔ females Lateral palatine processes with each other & with nasal septum & with median palatine process • Primary palate clefts (E‐F) • Secondary palate clefts (C‐D) • Primary and secondary palate clefts (G‐H)
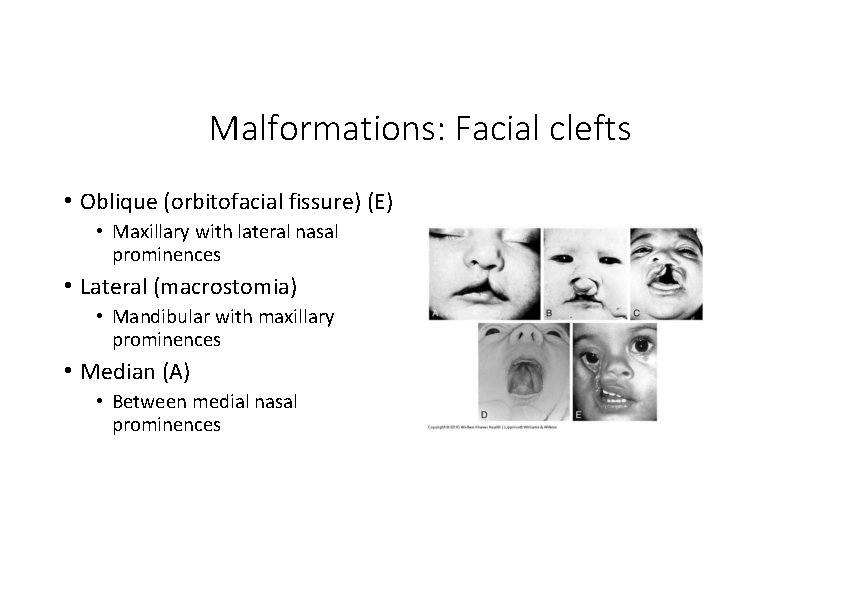
Malformations: Facial clefts • Oblique (orbitofacial fissure) (E) • Maxillary with lateral nasal prominences • Lateral (macrostomia) • Mandibular with maxillary prominences • Median (A) • Between medial nasal prominences
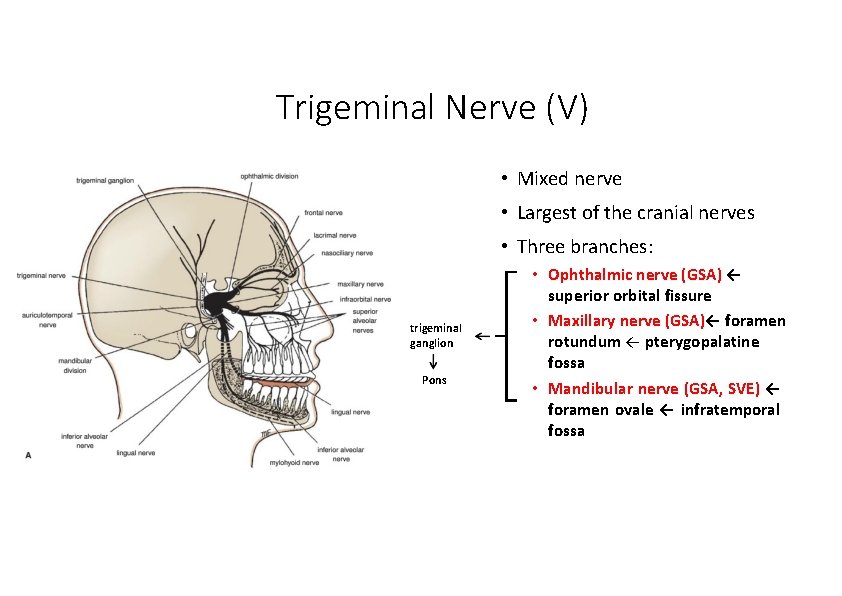
Trigeminal Nerve (V) • Mixed nerve • Largest of the cranial nerves • Three branches: trigeminal ganglion Pons • Ophthalmic nerve (GSA) ← superior orbital fissure • Maxillary nerve (GSA)← foramen rotundum ← pterygopalatine fossa • Mandibular nerve (GSA, SVE) ← foramen ovale ← infratemporal fossa
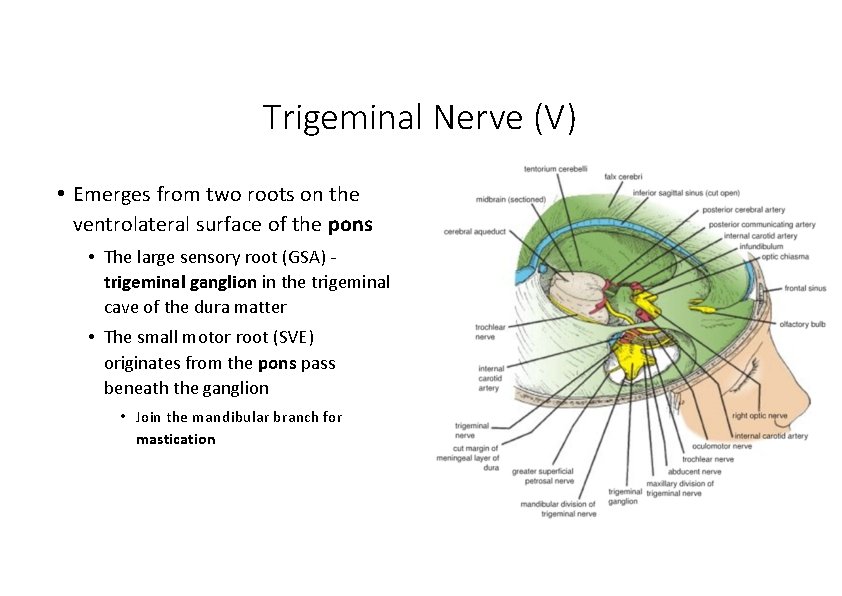
Trigeminal Nerve (V) • Emerges from two roots on the ventrolateral surface of the pons • The large sensory root (GSA) ‐ trigeminal ganglion in the trigeminal cave of the dura matter • The small motor root (SVE) originates from the pons pass beneath the ganglion • Join the mandibular branch for mastication
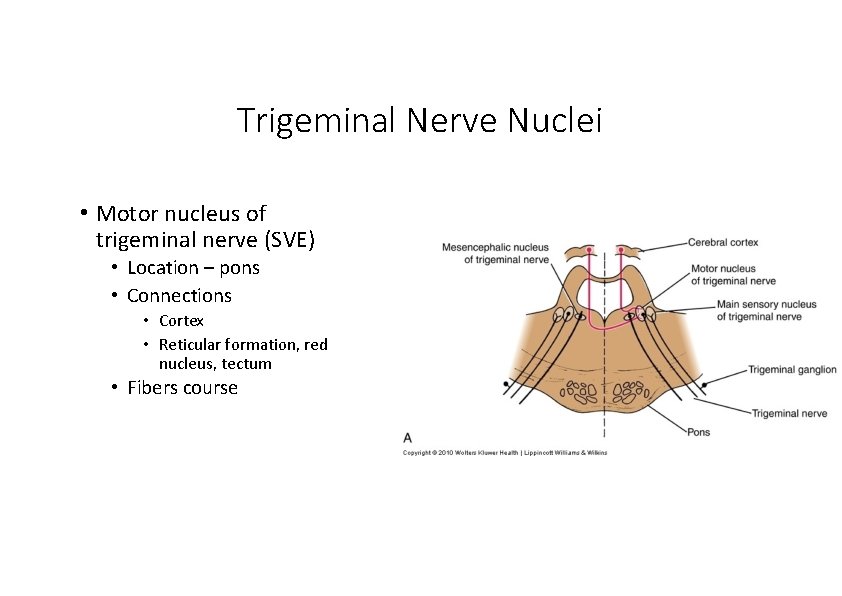
Trigeminal Nerve Nuclei • Motor nucleus of trigeminal nerve (SVE) • Location – pons • Connections • Cortex • Reticular formation, red nucleus, tectum • Fibers course
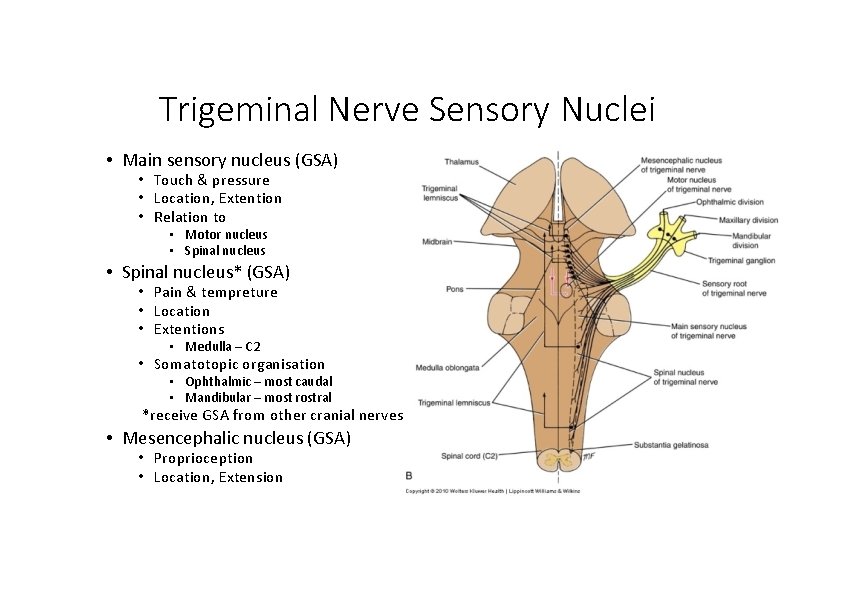
Trigeminal Nerve Sensory Nuclei • Main sensory nucleus (GSA) • Touch & pressure • Location, Extention • Relation to • Motor nucleus • Spinal nucleus* (GSA) • Pain & tempreture • Location • Extentions • Medulla – C 2 • Somatotopic organisation • Ophthalmic – most caudal • Mandibular – most rostral *receive GSA from other cranial nerves • Mesencephalic nucleus (GSA) • Proprioception • Location, Extension
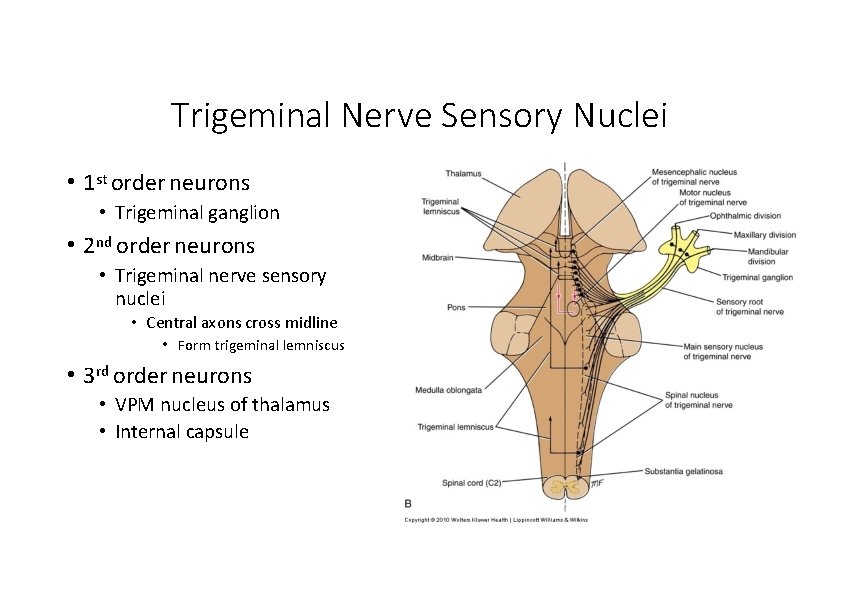
Trigeminal Nerve Sensory Nuclei • 1 st order neurons • Trigeminal ganglion • 2 nd order neurons • Trigeminal nerve sensory nuclei • Central axons cross midline • Form trigeminal lemniscus • 3 rd order neurons • VPM nucleus of thalamus • Internal capsule
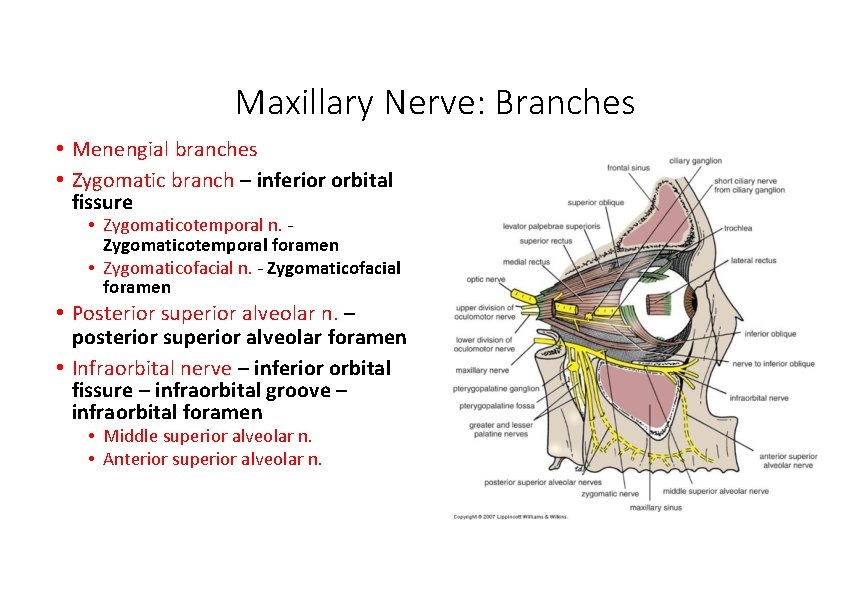
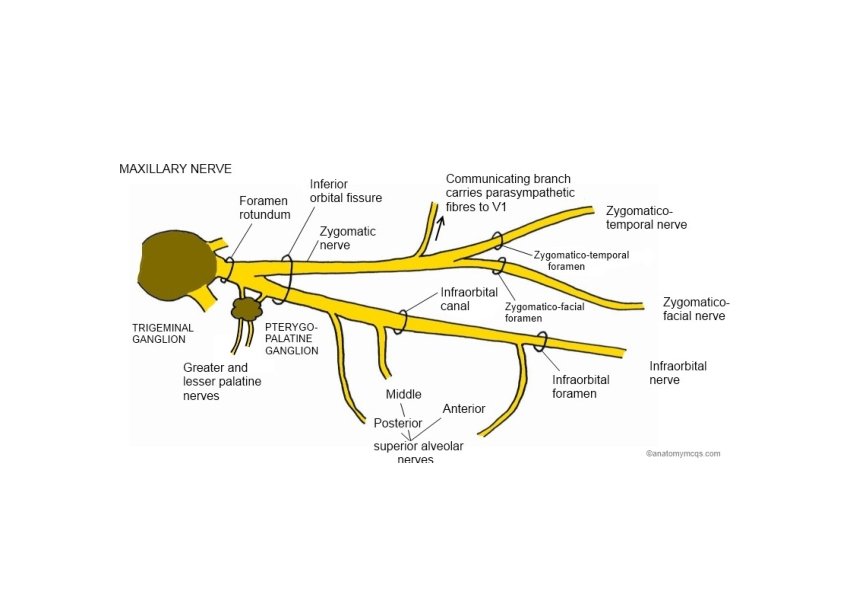
Maxillary Nerve: Branches • Menengial branches • Zygomatic branch – inferior orbital fissure • Zygomaticotemporal n. ‐ Zygomaticotemporal foramen • Zygomaticofacial n. ‐ Zygomaticofacial foramen • Posterior superior alveolar n. – posterior superior alveolar foramen • Infraorbital nerve – inferior orbital fissure – infraorbital groove – infraorbital foramen • Middle superior alveolar n. • Anterior superior alveolar n.
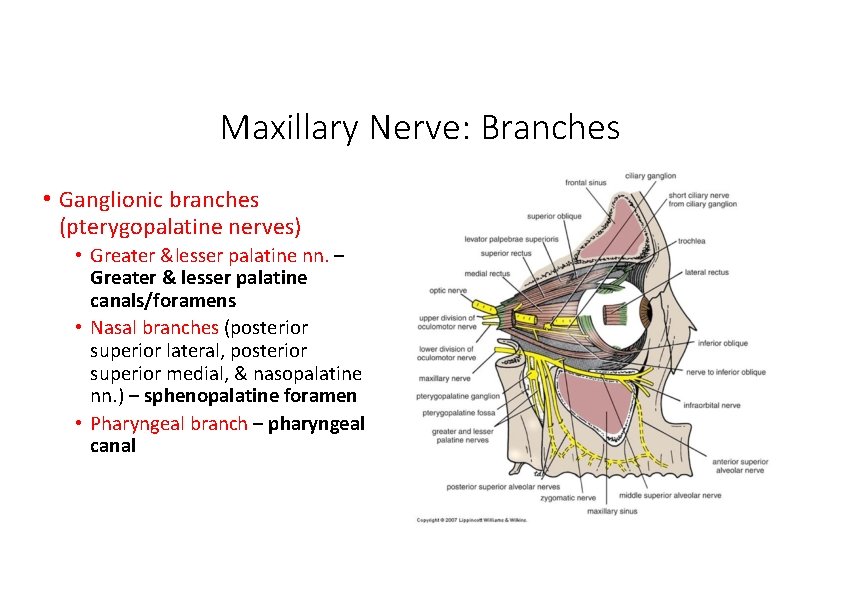
Maxillary Nerve: Branches • Ganglionic branches (pterygopalatine nerves) • Greater &lesser palatine nn. – Greater & lesser palatine canals/foramens • Nasal branches (posterior superior lateral, posterior superior medial, & nasopalatine nn. ) – sphenopalatine foramen • Pharyngeal branch – pharyngeal canal
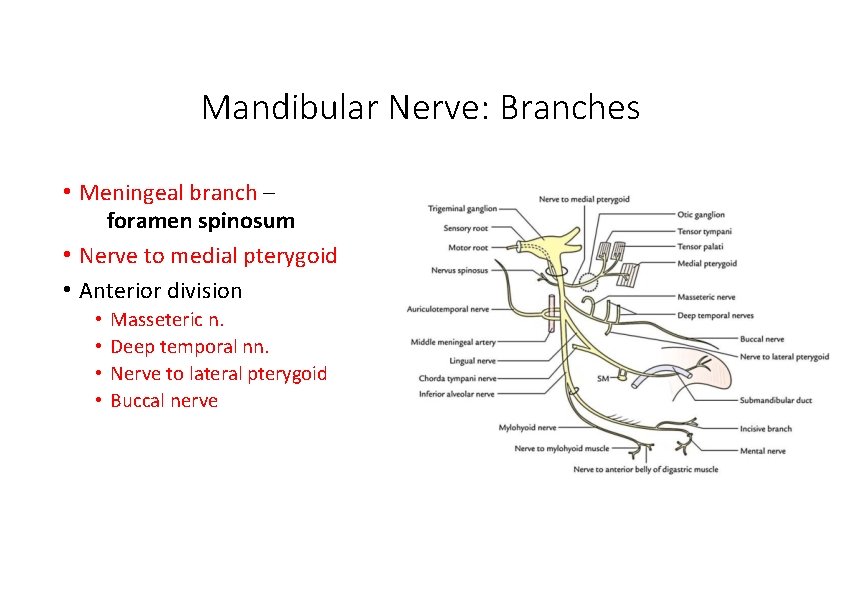
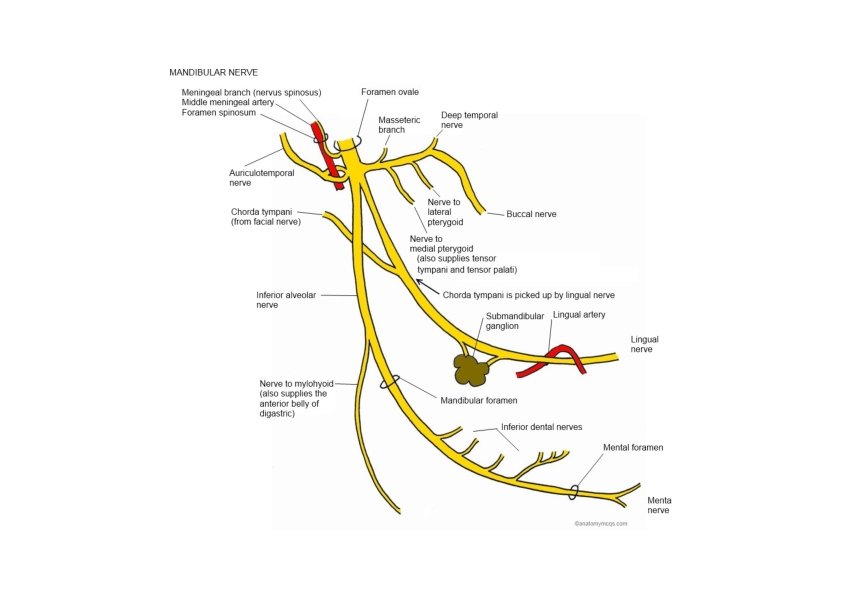
Mandibular Nerve: Branches • Meningeal branch – foramen spinosum • Nerve to medial pterygoid • Anterior division • • Masseteric n. Deep temporal nn. Nerve to lateral pterygoid Buccal nerve
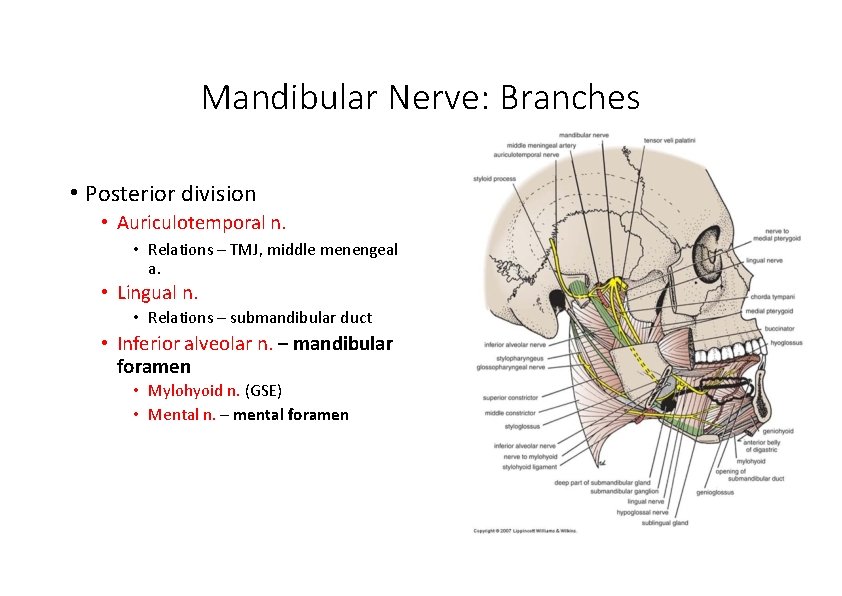
Mandibular Nerve: Branches • Posterior division • Auriculotemporal n. • Relations – TMJ, middle menengeal a. • Lingual n. • Relations – submandibular duct • Inferior alveolar n. – mandibular foramen • Mylohyoid n. (GSE) • Mental n. – mental foramen
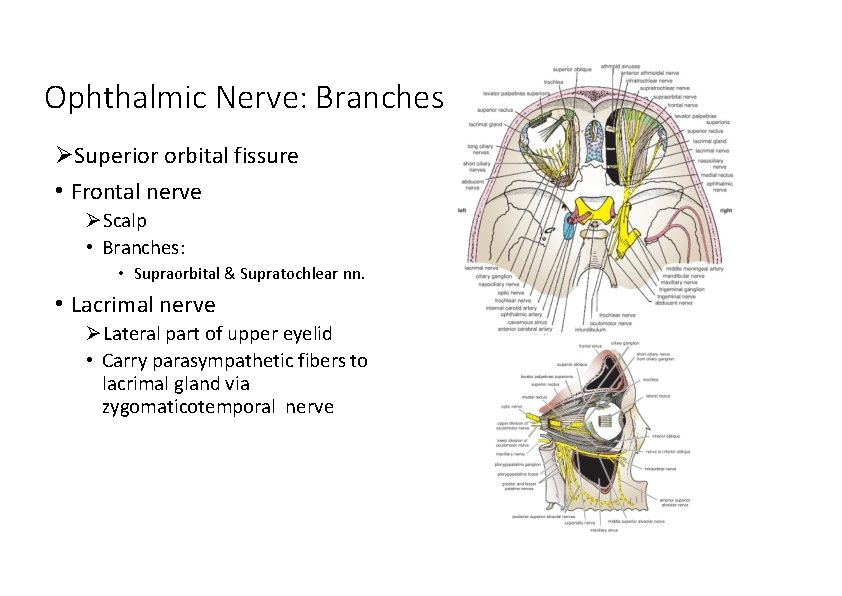
Ophthalmic Nerve: Branches Superior orbital fissure • Frontal nerve Scalp • Branches: • Supraorbital & Supratochlear nn. • Lacrimal nerve Lateral part of upper eyelid • Carry parasympathetic fibers to lacrimal gland via zygomaticotemporal nerve
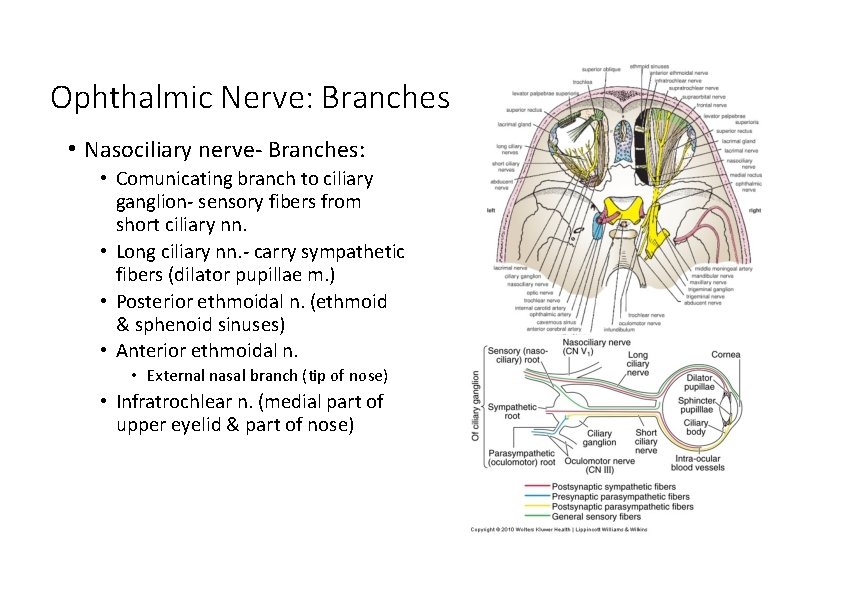
Ophthalmic Nerve: Branches • Nasociliary nerve‐ Branches: • Comunicating branch to ciliary ganglion‐ sensory fibers from short ciliary nn. • Long ciliary nn. ‐ carry sympathetic fibers (dilator pupillae m. ) • Posterior ethmoidal n. (ethmoid & sphenoid sinuses) • Anterior ethmoidal n. • External nasal branch (tip of nose) • Infratrochlear n. (medial part of upper eyelid & part of nose)
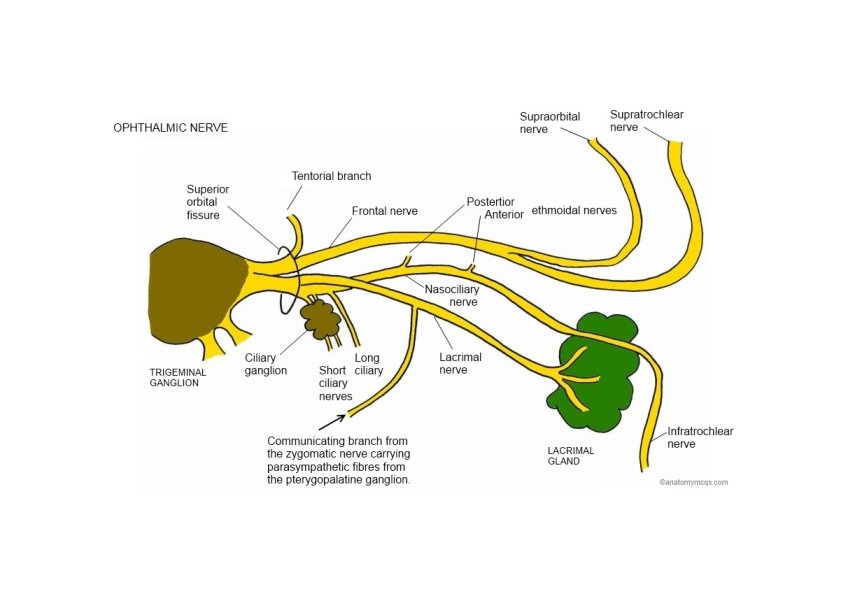
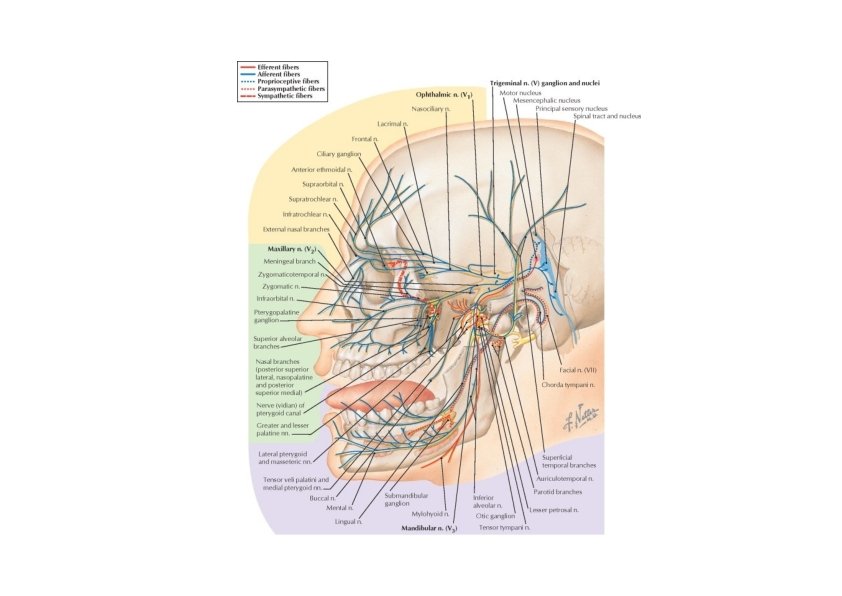

Trigeminal Nerve (V): Lesion • Loss of general sensation (hemianesthesia) from face and oral & nasal cavities • Loss of corneal reflex (V 1) (afferent limb) • Paralysis of the muscles of mastication • Deviation of the mandible to the weak side • Paralysis of the tensor tympani muscle – partial deafness to low‐pitched sounds • Trigeminal neuralgia • Test • Sensory – by touching face using cotton ball • Motor – by assisting masticatory muscles (masseter & temporalis) on clenching
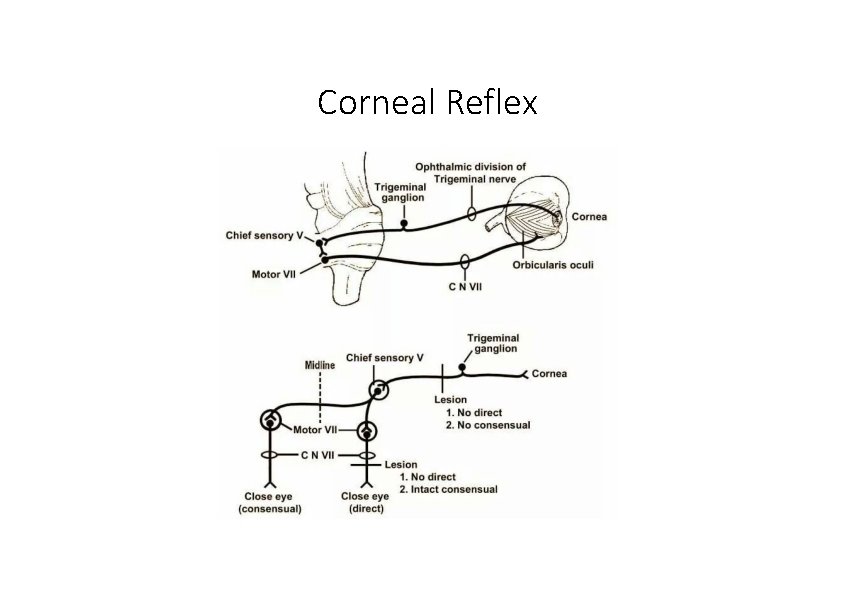
Corneal Reflex
- Slides: 24