Triangular Fibrocartilage Complex Manny Moore Clinic III Triangular

Triangular Fibrocartilage Complex Manny Moore Clinic III
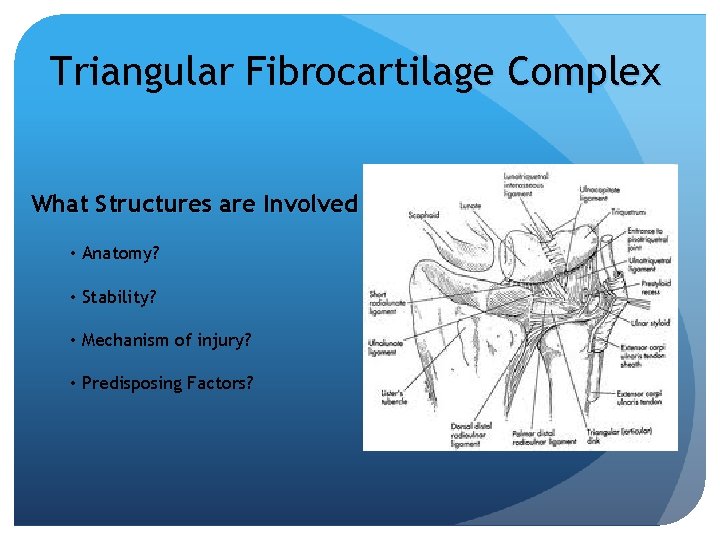
Triangular Fibrocartilage Complex What Structures are Involved • Anatomy? • Stability? • Mechanism of injury? • Predisposing Factors?

Injury Assessment • History • Inspection • Palpation • Range of Motion • Neurological Testing • Special Test
Nonoperative versus Operative Management Conservative Treatment Guidelines • Rest • Avoid Stressful Motions • Rehabilitation • Splints or brace • NSAIDS • Surgical intervention is suggested if the patient symptoms are not alleviated Within 4 -6 weeks depending on the type of lesion. Refer out for Imaging

Palmer Classification for TFCC Lesions Traumatic Lesions • Class IA: Central rupture • Class IB: Ulnar avulsion with/without disruption of the ulnar styloid process • Class IC: Distal avulsion • Class ID: Radial avulsion with/without osseous lesion of the radius Degenerative Lesions • Class IIA: Superficial degenerative lesion • Class IIB: Degenerative tear with cartilage lesion of the lunate or the ulna • Class IIC: Degenerative disc perforation with cartilage lesion of the lunate or the ulna • Class IID: Degenerative disc perforation with cartilage lesion of the lunate or the ulna and lunotriquentral instability Class IIE: Degenerative disc perforation with cartilage lesion of the lunate or the ulna, lunotriquentral instability and ulnocarpal arthrosis
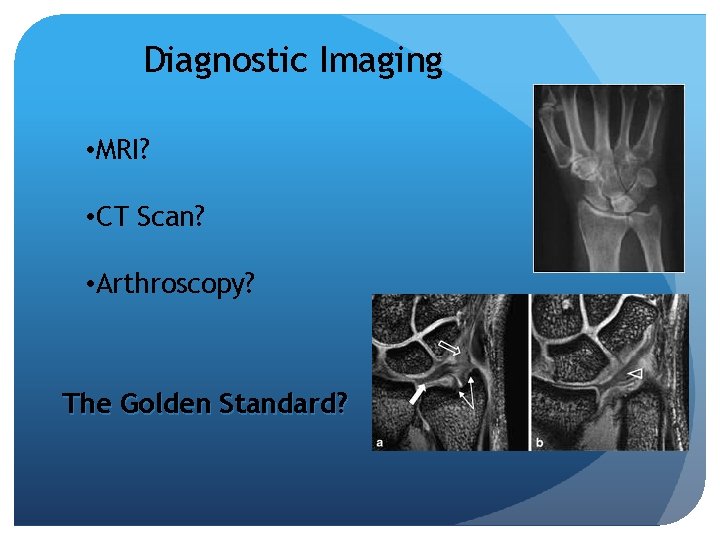
Diagnostic Imaging • MRI? • CT Scan? • Arthroscopy? The Golden Standard?

Which Surgical Procedure? • Open Dissection, Arthroscopy, or Direct Repair Deciding Factors? • Central Tears • Peripheral Tears • Ulnar Varience Goals? • Preoperative Rehabilitation? • Postoperative Rehabilitation?

Phase I for Central Debridement (3 -5 days) Goals: • Control edema • Pain • Protect repair • Minimize deconditioning Intervention: • Remove post-op dressing • Edema control with light compressive dressing to hand forearm • Active ROM exercises for wrist and forearm are begun 4 -8 times a day • A wrist splint is fabricated to wear between exercises and at night

Phase II for Central Debridement (10 -14 days) Goals: • Control edema • Pain • Continue to protect repair • Minimize deconditioning • Scar management Intervention: • Scar management begun within 48 hours of suture removal • Initiation of active-assist ROM for wrist and forearm
Phase III for Central Debridement Weeks 3 -4 Goals: • Control edema • Pain • Improve ROM Intervention: • Passive ROM of wrist and forearm may be initiated • Dynamic wrist splinting may be begun to improve ROM • Weighted wrist stretches may be initiated – also to increase ROM

Phase IV for Central Debridement Week 6 Goals: • Continue with ROM gains • Begin strengthening Intervention: • Progressive strengthening may be begun using putty or a hand exerciser • The wrist immobilization splint may be discontinued if the patient is asymptomatic

Phase I for Peripheral Repair (Week 1) Goals: • Edema control • Protect repair Intervention: • Patient remains in bulky post-op dressing • Instructions in edema control
Phase II for Peripheral Repair (Week 2) Goals: • Edema and pain control • Continue to protect repair Intervention: • Removal of bulky dressing • Edema control with retrograde massage, Isotoner glove, and/or coban wrapping • Daily pin care as needed • Long arm cast with 90° elbow flexion and wrist in neutral or wrist cock-up splint fabricated • Active and passive ROM for wrist and digits, include tendon glides (lumbrical grip, hookfist, full fist) • Isometric exercises forearm/hand: 10 repetitions 4 times/day • Low-grade isotonic exercises can be initiated if edema is not present (i. e. , lightest putty) • Light ADLs with 5 pound limit
Phase III for Peripheral Repair (Week 3 -6) Goals: Edema Pain Increase ROM Scar management Improve strength Intervention: • Scar management with massage, scar pad • Discontinue splint (unless patient is still symptomatic) • Increase isotonic exercises up to 10 pounds maximum for upper arm, forearm • Wrist mobility/weighted stretches with less than 5 pounds 3 -4 times/day • ADLs with less than 10 pounds

Phase IV for Peripheral Repair (Week 8) Goals: • Continue to improve ROM • Continue to increase strength • Simulate work requirements Intervention: • Dynamic splinting as necessary to increase ROM • Progress strengthening with putty, hand exerciser, free weights • Simulate work tasks as able Precautions • Aggressive PROM or Strengthening that increases pain • Increased ulnar-sided wrist pain • If ulnar shortening in addition to the TFCC repair or Debridement, the course of post-operative therapy will be altered.

Conclusion • Rehabilitation ranges from 6 -8 weeks depending on surgical methods used • Arthroscopic and debridment is successful in acute and chronic lesions, however chronic lesions are more successful with ulna shortening. • Arthroscopy is still considered the golden standard when diagnosing lesions and has showed success in pain management function and stability in TFCC repairs. • Despite its high sensitivity of MRI detecting TFCC lesions MRI has its limitations in the detection of peripheral TFCC tears.

References Usama Albastaki, MD, " Dimitris Sophocleous, MD, ^ Jan Gothlin, MD, Ph. D. MRI Imaging in TFCC injuries. Journal of Munipulotive and Physiological Therapeutics Volume 30, Number 7 Jui Tien Shih, Huung Maan Lee. Functional Results of TFCC. Department of Orthopedics and Hand Surgery, Vol 10, 2005 169 -176. Cuong Pho DPT, Joe Godges DPT. Triangular Fibrocartilage Complex (TFCC) Repair and Rehabilitation. Indiana Hand Therapy Protocols Jan-Ragnar Haugstvedt and Torstein Husby. RESULTS OF REPAIR OF PERIPHERAL TEARS IN THE TRIANGULAR FIBROCARTILAGE COMPLEX USING AN ARTHROSCOPIC SUTURETECHNIQUE. Journal of hand Surgery 1999.

? Questions
- Slides: 18