Treatment Rehabilitation SHMD 249 23052013 1 Injury Timeline

Treatment Rehabilitation SHMD 249 23/05/2013 1
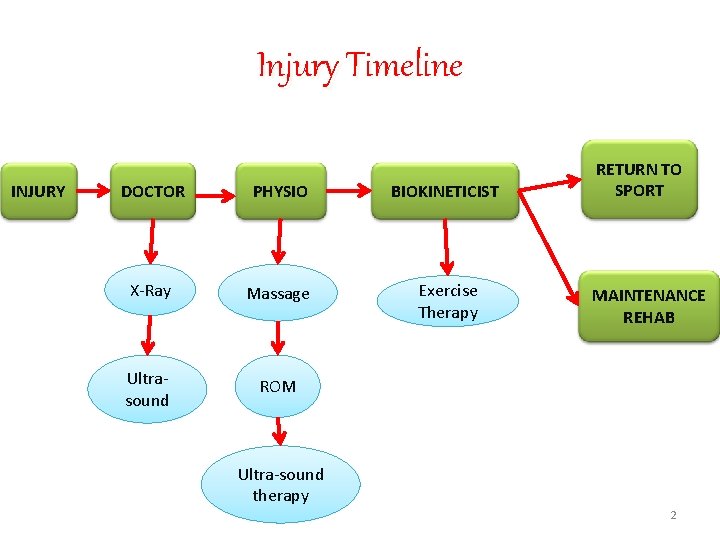
Injury Timeline INJURY DOCTOR PHYSIO BIOKINETICIST X-Ray Massage Exercise Therapy Ultrasound ROM RETURN TO SPORT MAINTENANCE REHAB Ultra-sound therapy 2

First Aid • First aid: The immediate treatment given to an injured person. • First establish what is wrong with the person: 1. Assess the situation – identify any risks to yourself or to the casualty. 2. Make the area safe. 3. Assess casualty & give first aid if appropriate. Establish if person is conscious, then check ABC: A. Airway – they have an open airway B. Breathing – they are breathing C. Circulation – assess if they have a pulse 4. Try to get help as soon as possible. 5. Complete and accident/incident report. 3

Calling for an Ambulance • Dial 911 & ask for an Ambulance. • Give them your exact location. • Give clear details of the accident and the severity of the injuries of the casualty. • Give the telephone number you are calling from and the gender and appropriate age of the casualty. Ø If you get someone else to phone, make sure they report back & an ambulance is on the way. Ø When paramedics arrive, tell them as much as possible about how the casualty behaved e. g. if casualty is unconscious, needed resuscitation etc. 4

SALTAPS: immediate treatment • See injury occur (mechanism of injury). • Ask casualty what is wrong & where they have pain. • Look for signs of bleeding, deformity of limbs, inflammation, swelling & redness. • Touch the injury for signs of heat, tenderness, loss or change of sensation & pain. • Active movement – ask casualty to move injured area if possible, through all ROM. • Passive movement – try to move injured site only if good ROM is possible. • Strength – if no pain during ROM, use resisted movements to assess further loss of function. 5

PRICED • Protect injured body part from further injury. • Rest – discontinue activity. • Ice – ice pack should be applied to injured area – reduce swelling & pain. • Compression – gentle pressure applied to injury site with padding/compression bandage thus reduce blood flow to injury & control swelling by decreasing fluid seeping into injury site. • Elevation – injury site should be supported in a raised position above level of heart in order to reduce blood flow to injury site thus further reduce swelling & bruising. • Diagnosis by a professional – examined as soon as possible so injury can be accurately diagnosed. 6

Cold Application - ICE • Ice bags/frozen veg packs/ice gel packs/ice bath immersion. • Every 2 hours for 10 - 20 minutes for up to 48 -72 hours. • Never apply ice directly to skin – burns skin. • Cold reduces circulation, thus minimize swelling & bruising & reduce pain (nerve endings). • 4 stages of sensation: – Cold. – Burning. – Aching. – Numbness (Therapy should be stopped) 7
Heat Treatments • Only after about 3 days. • Dilate blood vessels thus increasing blood flow to area – absorb swelling & remove dead cells from area. • Increase growth of new blood vessels to help scar tissue form. • Helps muscles relax & aids pain relief. • Contrast bathing: dilate & constrict blood vessels – increase blood flow then remove debris from injury site. 8

Support Mechanisms • Protect, support & stabilize. • Prevent re-injury – limit movement of joint. • Support Devices: • Bandage. • Kinesio taping. • Braces. • Moon boots. 9

Rehabilitation • Rehabilitation is the restoration of the ability to function in a normal or near normal manner following an injury. • No rehab = high risk of re-injury. • Involves: – Reducing pain & swelling. – Restoring range of motion (ROM). – Increasing muscle strength. – Improving stabilization. • Considerations: – Physical condition of player. – Severity of injury. – Timing (pre-season/competition). 10
- Slides: 10