Treatment Planning for PatientCentered Care Treatment Planning Documentation













- Slides: 16

Treatment Planning for Patient-Centered Care

Treatment Planning Documentation Goals: What key Activities do our value propositions require? § Improve the ability to translate ASAM data into patient-centered problem statements and goals that address Medical Necessity

• IN PATIENT-CENTERED CARE PLANNING, the patient and family members participate in decisionmaking and their goals are addressed as part of the patient’s care plan. . . • The ASAM 6 dimension is the tool we use to provide a framework for: • Assessment • Level of Care Placement • Organizing the Care Plan And Plan’s need to be INDIVIDUALIZED Patient Centered means Patient Goals are most important

Some Notes on MEDICAL NECESSITY The CORNERSTONE of Admission A simple way to look at when services are MEDICALLY NECESSARY. . 1. There is a SUD diagnosis 2. There are impairments—functional and diagnostically related 3. It can be reasonably expected that treatment will improve functioning See 22 CCR § 51303; 42 CFR § 438. 210(a)(4) and, ASAM Criteria (2013)

Objectives Services Goals The ASAM and Medical Necessity tell us a lot. . . now lets use them to develop a Person-Centered Care Plan. . . Outcomes ASAM Assessment Assess Reassess

PROBLEM STATEMENTS. . and GOALS Getting to “Good Problem Statements and Goals” • Start with a Therapeutic Alliance--3 CRITICAL ELEMENTS • Shared Goals • Consensus on methods and tasks of Treatment • An emotional bond • The ASAM assessment must be brought into the “Alliance” • Medical Necessity must be addressed • “Identified problems” must be addressed q There is no agreed upon standard for how to conduct the Treatment Planning session however a review of the ASAM (Risk ratings and rational) and a discussion on the patient’s vision for “DESIRED RESULTS” is recommended.

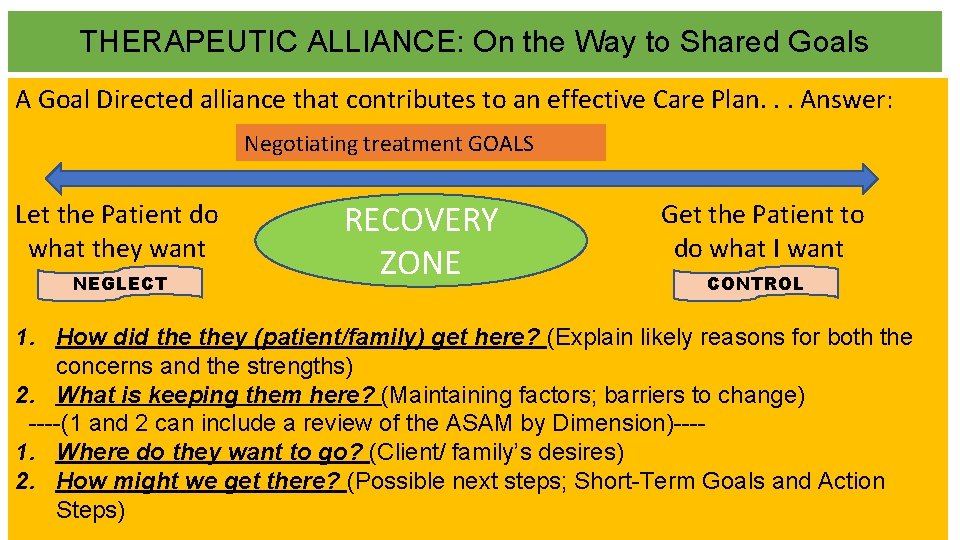
THERAPEUTIC ALLIANCE: On the Way to Shared Goals A Goal Directed alliance that contributes to an effective Care Plan. . . Answer: Negotiating treatment GOALS Let the Patient do what they want NEGLECT RECOVERY ZONE Get the Patient to do what I want CONTROL 1. How did they (patient/family) get here? (Explain likely reasons for both the concerns and the strengths) 2. What is keeping them here? (Maintaining factors; barriers to change) ----(1 and 2 can include a review of the ASAM by Dimension)---1. Where do they want to go? (Client/ family’s desires) 2. How might we get there? (Possible next steps; Short-Term Goals and Action Steps)

Dimension 1 Are withdrawal management services indicated? What is the severity risk of withdrawal symptoms; are there other medical complications? SAMPLE PROBLEM STATEMENTS: 1) “X” experiencing moderate-severe opiate withdrawal symptoms 2) “Y” has mild withdrawal symptoms but presents with high continued use risk 3) “X” presented with a B. A. L. of 1. 4 and a history of seizures during withdrawal Dimension 2 Other than withdrawal, what are the current physical illnesses that should be addressed? SAMPLE PROBLEM STATEMENTS: 1) “X” is 3 months pregnant and lacks regular prenatal care 2) “Y” has medical complaints and no primary care physician 3) “Z” has chronic pain which challenges recovery efforts (Dim 5) 8

Dimension 3 Are there psychiatric, psychological, behavioral, emotional or cognitive conditions needing to be addressed? Can she/he cope with the emotional, behavioral, or cognitive conditions? SAMPLE PROBLEM STATEMENTS: 1) “X” is troubled by depressed feelings 2) “Y” describes history of managing strong emotions with alcohol and other drug use (Dim 5) 3) “Z” experiences recurrent trauma-based emotions which interferes with daily functioning and recovery (Dim 5; Dim 6) Dimension 4 How ready, willing or able does the patient feel to make changes? What stage of change? SAMPLE PROBLEM STATEMENTS: 1) “X” has difficulty sustaining motivation for recovery efforts 2) “Y” is adverse to abstaining from marijuana 3) “Z” is unclear about the role of alcohol and drug use on current relationship problems (Dim 6) 9

Dimension 5 Is their any immediate danger of continued MH distress or substance use? Does the patient know his/her relapse trigger(s)? How well can she/he manage triggers; cope with craving, or impulses? SAMPLE PROBLEM STATEMENTS: 1) “X” experiences strong craving with limited recovery oriented self-management skills 2) For the past 5 years “Y” has been able to manage opioid use only when in a controlled environment (jail; hospital) 3) “Y” has insight into relapse triggers but coping skills have not been effective to prevent relapse Dimension 6 Does the patient’s environment poses a threat to safety or ability to engage in treatment? Are there environmental barriers that need to be addressed (transportation, child care, housing, employment, etc. ? ) SAMPLE PROBLEM STATEMENTS: 1) “X” is homeless and lacks recovery skills to cope with this stressor (Dim 5) 2) Alcohol and drug use impairs “Y’s” ability to fulfill parenting role and responsibilities 3) “Z” has been unable to obtain and sustain employment 10

SHORT TERM GOALS- Big Goals Take Many Smaller Steps Short Term Goal are the manageable steps leading to goal attainment PROBLEM- Homelessness is a personal stressor and continuing drug use risk factor GOAL- Find recovery supporting, secure housing • Short-Term Goal 1: Resolve ambivalence about drug use and committing to abstinence-based housing • Short-Term Goal 2: Use problem solving format to identify possible shelter/housing options • Short-Term Goal 3: Complete applications and interviews for housing

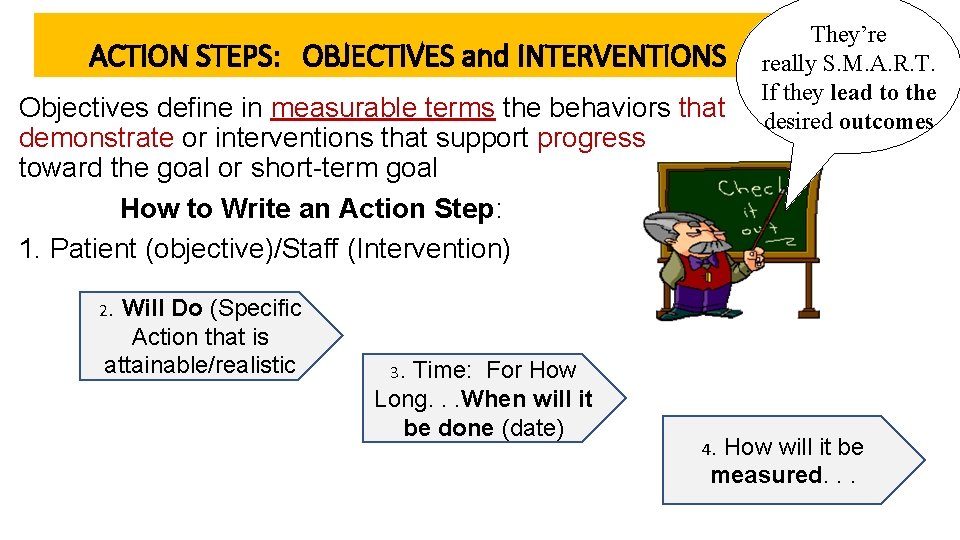
ACTION STEPS: OBJECTIVES and INTERVENTIONS Objectives define in measurable terms the behaviors that demonstrate or interventions that support progress toward the goal or short-term goal How to Write an Action Step: 1. Patient (objective)/Staff (Intervention) Will Do (Specific Action that is attainable/realistic They’re really S. M. A. R. T. If they lead to the desired outcomes 2. 3. Time: For How Long. . . When will it be done (date) 4. How will it be measured. . .

EXAMPLE OF A TREATMENT PLAN Dimension 5: Relapse/Continued Use Problem: “X” has limited social/community involvement and no experience structuring a personal recovery effort (I guess I could go to A. A. but then what do you do? ) Goal (Desired Result): Develop a personal, structured recovery program (Figure out how to not use) Short-Term Goal 1: learn what are the elements of a personal recovery program and how to organize them as daily practices Action Step by Patient: a) Participate in structured recovery program by attending seven sessions of Early Recovery Skills (ERS) Group: DUE: 2 x’s weekly ending (date) b) completing a daily recovery scheduling calendar. DUE: Daily for 3 weeks (dates), present in ERS group to peers, daily to staff for feedback. c) Review the “recovery resource guide” and “ 5 areas of focus for a balanced life” and include 1 recovery resource and 2 elements of a balanced life in each daily recovery calendar. DUE: Daily for 3 weeks (see b).

EXAMPLE OF A TREATMENT PLAN Dimension 6: Environmental Problem: “X” and his mother have a pattern of arguing which escalates to yelling, violence, and frequently ends with relapse (My Mom gets on me and I blow up; weed calms me down) Goal (Desired Result): Establish healthy conflict Mangement skills with relapse prevention (Get along better with Mom) Short-Term Goal 1: “X” will develop skills to communicate calmly and effectively with Mother Action Step By Patient and Family: “X” and Mother will attend family session to practice at least 1 conflict resolution exercise each session Due: 1 time weekly for 4 weeks ---Next Slide---

Short-Term Goal 2 Action Step By Patient : “X” will learn and demonstrate recovery supporting conflict management skills a) “X” will write a script for a common conflict situation and use it to roleplay practice conflict management skills in treatment process group Due: 1 time weekly for 4 weeks b) “X” will include managing conflict and strong emotions as a relapse trigger and include in personal relapse prevention plan (see Problem __for Dimension 5 for specific action steps and time lines) Action Step by Staff: Counselor will provide weekly family counseling with the following focus: a) Engage “X” and his Mother in role plays to help them learn empathic conflict management skills Due: 1 x weekly for 4 weeks b) Conduct collateral contacts with Mother to coach her in ways to deescalate arguments and threats of relapse with “X” Due: 2 x’s within next 4 weeks. c) Support “X” in practicing conflict resolution skills and making “I” statements to convey needs to others. Due: In group and individual sessions, as appropriate next 4 weeks

Oh, and we need to plan in a timely manner! Timely Treatment Plans Withdrawal Management- Complete on intake ü signed during treatment OP/OPT/Residential - Complete within 7 days ü signed by client and LPHA within 7 days for adults, 14 days for youth Treatment Plan Reviews OP/OPT- Every 30 days (min)- LPHA signature Residential- Every 15 days (min)-LPHA signature Treatment Plan Updates/Revisions: OP/OPT- Every 90 days (min) or as clinically necessary Residential - Every 30 days (min)/as clinically necessary