Treatment of TB Spine Wayne Yap 27 th

Treatment of TB Spine Wayne Yap 27 th Aug 2015

Options for management • Medical therapy • Anti tuberculous drugs • Bracing • Surgical Intervention • CT Guided aspiration • Open Debridement • Decompression +/- Fusion

Medical Therapy • Anti tuberculous treatment • Various studies have shown that majority of patients (82%-95%) of patients with spinal TB respond well to medical therapy 1, 2, 3 • Response can be in the forms of pain relief, decrease in neurological deficit • Almost all anti tuberculous drugs penetrate well into tuberculous vertebral lesions 4 • 40% of patients with TB spine and paraplegia show recovery with anti tuberculous treatment only 5 1. 2. 3. 4. 5. Jutte PC et al. Routine surgery in addition to chemotherapy for treating spinal tuberculosis. Cochraine database Syst Rev. 2006 Jan 25(1) Lifeso RM et al. Tuberculous spondylitis in adults. J Bone Joint Surg Am. 1985 Dec; 67(9): 1405 -13 A 15 year assessment of controlled trials of the management of tuberculosis of the spine in Korea and Hong Kong. J Bone Joint Surg Br. 1998 May; 80(3): 456 -62 Ge Z et al. Measurement of concentration of three antituberculosis drugs in the focus of spinal tuberculosis. Eur Spine J. 2008 Nov; 17(11): 1482 -7 Garg RK et al. Spinal Tuberculosis: A Review. J Spinal Cord Med 2011 Sep; 34(5): 440 -454
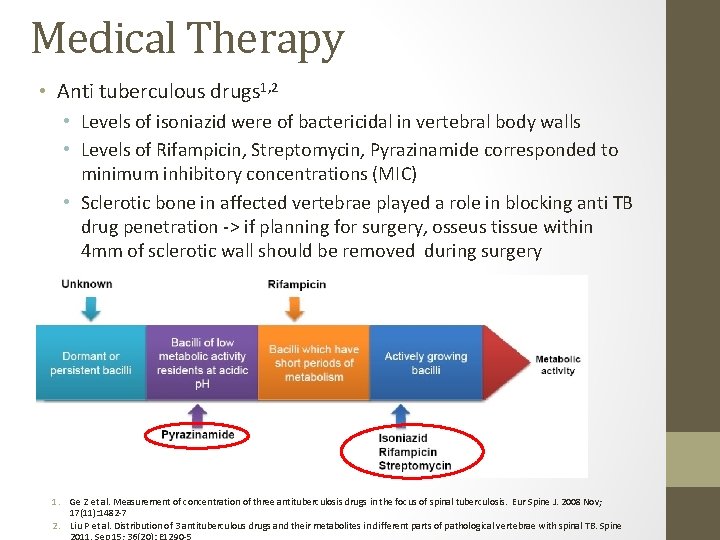
Medical Therapy • Anti tuberculous drugs 1, 2 • Levels of isoniazid were of bactericidal in vertebral body walls • Levels of Rifampicin, Streptomycin, Pyrazinamide corresponded to minimum inhibitory concentrations (MIC) • Sclerotic bone in affected vertebrae played a role in blocking anti TB drug penetration -> if planning for surgery, osseus tissue within 4 mm of sclerotic wall should be removed during surgery 1. Ge Z et al. Measurement of concentration of three antituberculosis drugs in the focus of spinal tuberculosis. Eur Spine J. 2008 Nov; 17(11): 1482 -7 2. Liu P et al. Distribution of 3 antituberculous drugs and their metabolites in different parts of pathological vertebrae with spinal TB. Spine

Medical Therapy • Anti tuberculous treatment regiment 1 • Divided into intensive phase and continuation phase • Intensive phase (2 months) • Isoniazid, rifampicin, pyrazinamide, ethambutol or streptomycin • Continuation phase (Up to 7 months) • Isoniazid, Rifampicin • Opinions differ and some experts prefer durations of 12 -24 months or until radiological evidence of disease occurs • No role for corticosteroids except for cases of spinal arachnoiditis or non osseus spinal TB 1. WHO guidelines for treatment of tuberculosis. 4 th edition. 2010.

Medical Therapy • Other non surgical forms of management 1 • Majority of patients are treated with ambulatory care without prolonged bed rest/recumbency • Cast or brace immobilization previously classic form of treatment, now found to be inefficient and has fallen out of favour • May still be used for pain control and prevention of deformity 1. Garg RK et al. Spinal Tuberculosis: A Review. J Spinal Cord Med 2011 Sep; 34(5): 440 -454

Surgical intervention • Cochrane database review concluded that evidence is insufficient to support routine use of surgery in Spinal TB patients already treated on medical therapy • Indications for Surgery 1, 2: 1. Garg RK et al. Spinal Tuberculosis: A Review. J Spinal Cord Med 2011 Sep; 34(5): 440 -454 2. Hsu LC et al. Pott’s paraplegia of late onset. The cause of compression and results after anterior decompression. J Bone Joint Surg Br. 1988 Aug 70(4): 534 -8

Surgical intervention • Broadly divided into 2 main types • Debridement • Mainly for control of infection through removal of infected material/abscesses etc • Role of CT guided aspiration of abscesses with good results • Complete resection of infected area is not absolutely essential to obtain bone healing and union 1 • Radical debridement of infected focus may damage remaining growth plates in children 2 • Decompression and stabilization/fusion • In general, anterior debridement w/ strut graft +/- posterior stabilization is the accepted surgical option • Approach and type of fusion has to take into account involvement of posterior elements, degree of kyphosis, foci of infection, presence sinus tracts etc 1. V. P. Djientcheu etal. The role of surgery in management of Pott’s disease in Yaounde. A review of 43 cases. Orthop & Traumatology; June 2013 99(4): 419 -423 2. Moon MS. Managing tuberculosis of Spine. Med Progr (Hong Kong) 2004; 31: 593 -602.

Surgical intervention • The “Hong Kong Operation” 1, 2 • In the past, controversy existed on optimal form of treatment for TB spine • MRC Working party designed prospective multicenter clinical trials to compare conservative VS debridement VS radical debridement w/strut graft • Radical procedure consisted of thorough excision of tuberculous focus, posteriorly until dura mater, cephalad and caudad until healthy bleeding cancellous bone exposed. Strut graft from cut rib or iliac crest docked. 1. A controlled trial of anterior spinal fusion and debridement in the surgical management of tuberculosis of the spine in patients on standard chemotherapy: a study in Hong Kong (1974). The British journal of surgery 61 (11): 853– 866 2. A 10 -year assessment of a controlled trial comparing debridement and anterior spinal fusion in the management of tuberculosis of the spine in patients on standard chemotherapy in Hong Kong. Eighth Report of the Medical Research Council Working Party on Tuberculosis of the Spine (1982). J Bone Joint Surg Br 64 (4): 393– 398
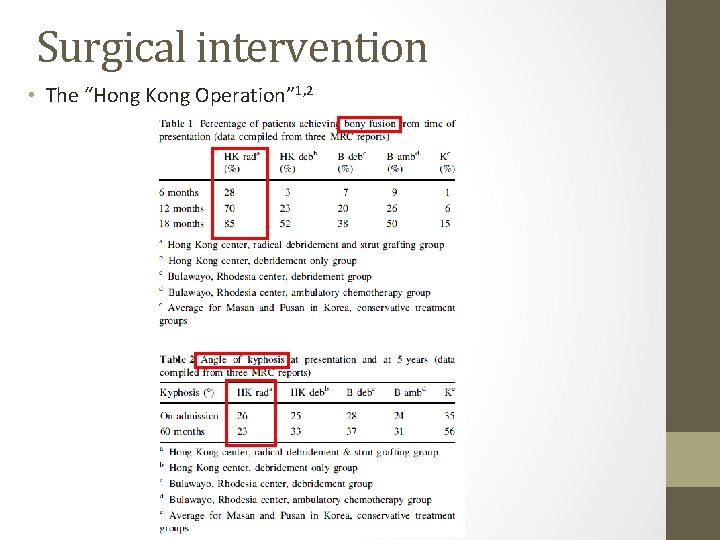

Surgical intervention • The “Hong Kong Operation” 1, 2

Surgical intervention • When is instrumentation indicated? 1, 2 • Instrumentation can be done anteriorly or posteriorly and provides added stability to the spine • Can be done as a single or 2 -stage procedure • Indications: • Radical debridement spanning 2 disks and a vertebral body or more • Graft length spanning 2 disk spaces • Severe deformity or risk of progression of deformity • • Age < 10 yo and loss of 1. 5 vertebral body Pre treatment kyphotic angle of >30 deg Cervicothoracic or thoracolumbar junctional kyphosis Radiological signs of facet joint separation, retropulsion, lateral translation 1. Kim CM. Surgical treatment of acute TB spondylitis: indicaions and outcomes. Eur Spine J 2013 22 (Supl 4): S 603 -S 611 2. Rajasekaran S. Kyphotic deformity in spinal TB and its management. SICOT 2012 36: 359 -365

Surgical intervention • Is it safe to place implants in a patient with TB Spine? • Oga et al in 1993 demonstrated that bio-film formation and adherence of mycobacterium tuberculosis to the metallic implants is negligible, making them susceptible to immune defence mechanisms and anti tuberculous drugs • The findings removed the phobia of using instrumentation in active TB, leading many surgeons to use instrumentation posteriorly in addition to anterior procedure 1. Oga M, Arizono T. Evaluation of the risk of instrumentation as a foreign body in spinal tuberculosis: A clinical and biologic study. Spine 1993 18(13): 1890 -1894 2. Ha K-Y, Ryoo S J et al. Adherence and biofilm formation of staph epidermidis and mycobacterium tuberculosis on various spinal implants. Spine 2004: 38 -43
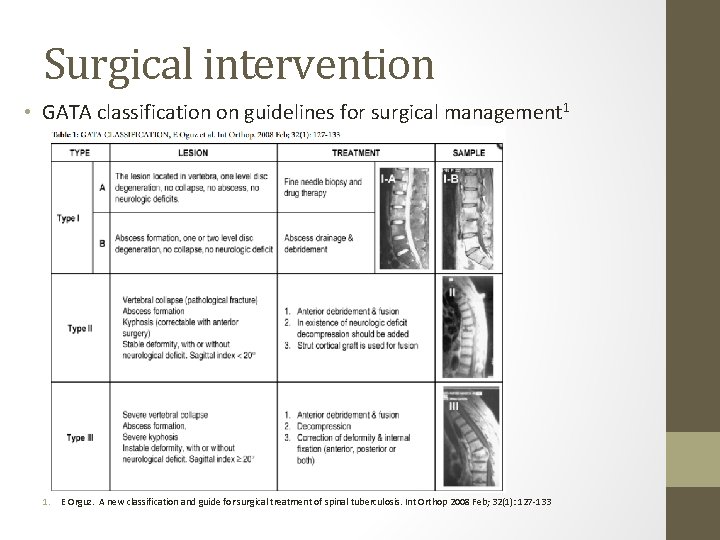

Surgical intervention • GATA classification on guidelines for surgical management 1 1. E Orguz. A new classification and guide for surgical treatment of spinal tuberculosis. Int Orthop 2008 Feb; 32(1): 127 -133

Surgical intervention - Outcomes • Most important prognostic indicator was neurological condition of patient at surgery (Asia A patients did not recover well)1 • Postulated that inflammation and abscess in spine reduces medullary perfusion pressure and this causes irreversible ischemia • Good tolerance to instrumentation and graft integration • Use of internal fixation and grafts in infected area does not generally cause problems • Chronic implant colonization less common in TB as opposed to other pyogenic infections 1. V. P. Djientcheu etal. The role of surgery in management of Pott’s disease in Yaounde. A review of 43 cases. Orthop & Traumatology; June 2013 99(4): 419 -423
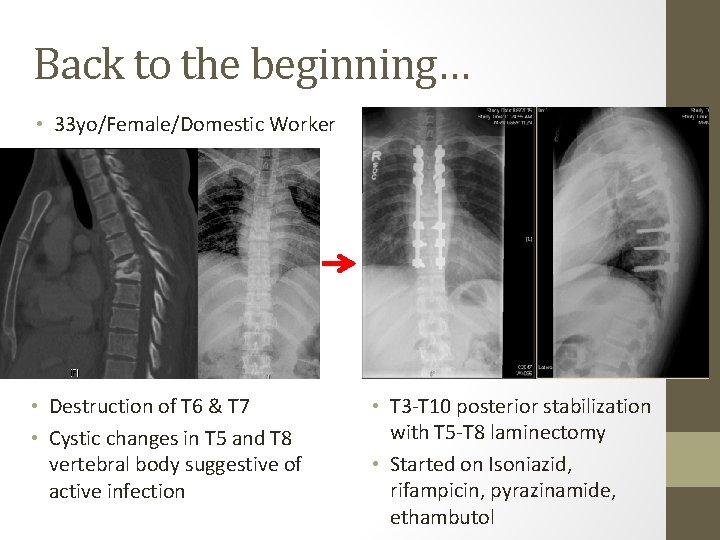
Back to the beginning… • 33 yo/Female/Domestic Worker • Destruction of T 6 & T 7 • Cystic changes in T 5 and T 8 vertebral body suggestive of active infection • T 3 -T 10 posterior stabilization with T 5 -T 8 laminectomy • Started on Isoniazid, rifampicin, pyrazinamide, ethambutol

Thank You
- Slides: 16