Treatment of acute exacerbations of asthma in adults

Treatment of acute exacerbations of asthma in adults D. Anan Esmail

What is the definition of Asthma exacerbation?
the classic symptoms of asthma Wheeze Cough Shortness of breath

acute exacerbations of asthma 1. acute or subacute episodes of progressively worsening • Wheezing • Cough • shortness of breath some combination of these symptoms

acute exacerbations of asthma 2. decreases in expiratory airflow • documented by measurement of lung function (spirometry or PEF)

What are the causes?

Triggers
Treatment • inhaler techniques
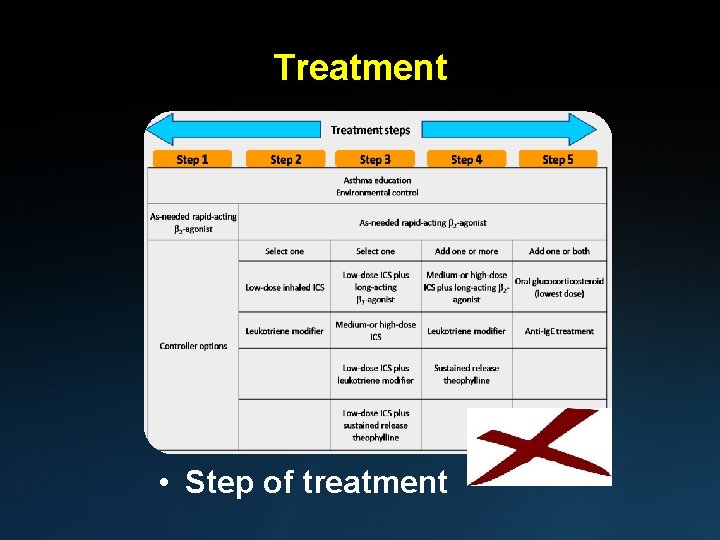
Treatment • inhaler techniques • Step of treatment

Treatment Stop of medicatiom

What is management ?

The best strategy for management of acute exacerbations of asthma is: • early recognition and intervention • before attacks become severe and potentially life threatening

Detecting the onset of an exacerbation

Some patients are very sensitive to increased asthma symptoms

while others perceive reduced airflow only when it becomes marked decrease in peak expiratory flow may be the first sign that asthma control is deteriorating
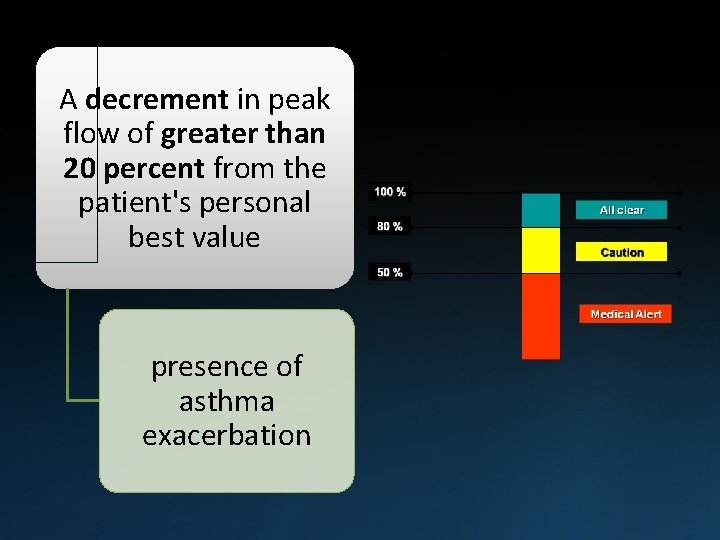
A decrement in peak flow of greater than 20 percent from the patient's personal best value presence of asthma exacerbation

When patients recognize the onset of an exacerbation • they should self-administer an inhaled short-acting beta agonist as follows:

inhaled short-acting beta agonist Two to six puffs repeated in 20 minutes for the first hour if needed MDI with spacer

inhaled short-acting beta agonist (albuterol 2. 5 mg) repeated every 20 minutes for first hour if needed nebulization
After the first hour symptoms improvement repeat a peak flow measurement
Good response to initial home treatment patient’s symptoms resolve PEF ↑ to above 80 % of baseline safely continue self- treatment at home

Good response to initial home treatment short course of oral glucocorticoids if symptoms recur
Incomplete response to initial home treatment continued symptoms PEF ˂ 80 % of baseline

Incomplete response to initial home treatment continued of inhaled short- acting beta agonists initiate oral glucocorticoids contact the clinician urgently for advice
Incomplete response to initial home treatment contact the clinician symptoms or signs of severe exacerbation high risk for a fatal attack

Fatal Asthma Attack Previous severe exacerbation (intubation or ICU admission)

Fatal Asthma Attack Two or more hospitalizations for asthma in the past year

Fatal Asthma Attack Three or more emergency department visits for asthma in the past year

Fatal Asthma Attack Hospitalization or emergency department visit for asthma in the past month

Fatal Asthma Attack Use of more than two canisters of short-acting beta agonist per month

Fatal Asthma Attack Low socioeconomic status inner city residence

Fatal Asthma Attack illicit drug use major psychosocial problems

Fatal Asthma Attack Comorbidities such as Cardiovascular chronic lung psychiatric disease
Incomplete response to initial home treatment contact the clinician symptoms or signs of severe exacerbation high risk for a fatal attack

Clinical Findings Respiratory rate >30 /minute Pulse >120 /minute

Clinical Findings Talks in (Sentences, Phrases, Words) Alertness (agitated, Drowsy or confused)

Clinical Findings Position • Prefers sitting • inability to lie supine
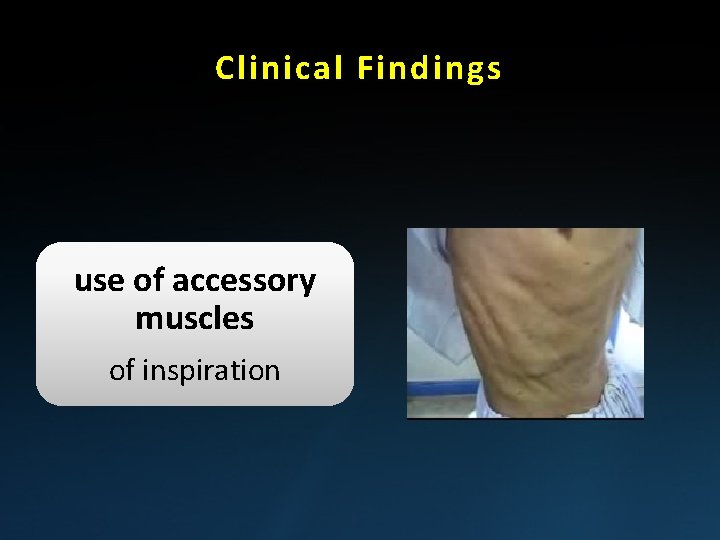
Clinical Findings use of accessory muscles of inspiration

Clinical Findings Diaphoresis
Clinical Findings Pulsus paradoxus (ie, a fall in systolic blood pressure by at least 12 mm. Hg during inspiration)
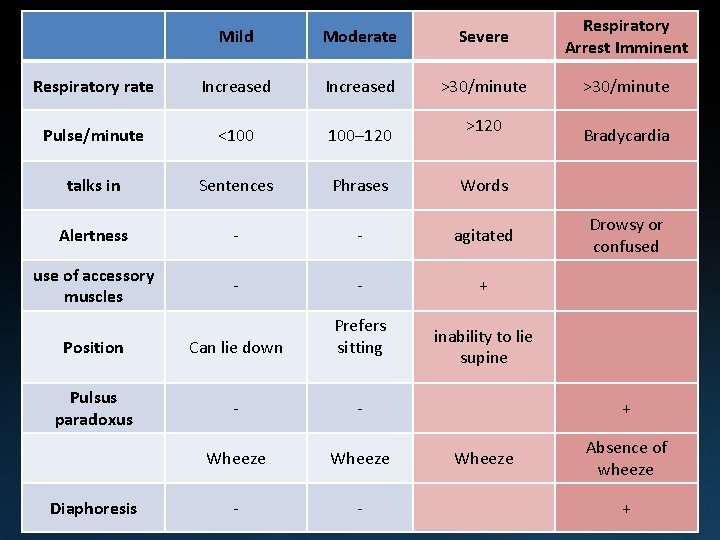
Mild Moderate Severe Respiratory Arrest Imminent Respiratory rate Increased >30/minute Pulse/minute <100 100– 120 talks in Sentences Phrases Words Alertness - - agitated use of accessory muscles - - + Position Can lie down Prefers sitting Pulsus paradoxus - - Wheeze - - Diaphoresis >120 Bradycardia Drowsy or confused inability to lie supine + Wheeze Absence of wheeze +

Unfortunately these findings are not sensitive up to 50 % of indicators of severe patients with severe attacks airflow obstruction will not manifest any of these abnormalities
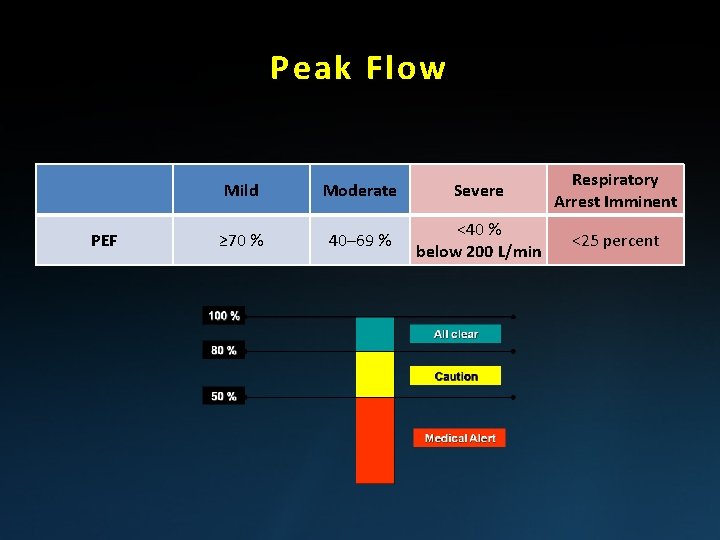
Peak Flow PEF Mild Moderate Severe Respiratory Arrest Imminent ≥ 70 % 40– 69 % <40 % below 200 L/min <25 percent

Oxygen Saturation Sa. O 2 Mild Moderate Severe Respiratory Arrest Imminent >95 % > 95% 90 to 95% <90 %

Hypercapnia (ABG) Pa. CO 2 Mild Moderate Severe Respiratory Arrest Imminent - - - normal or elevated
Chest radiograph The most common abnormality is pulmonary hyperinflation
Chest radiograph Other abnormal findings Pneumothorax Pneumomediastinum Pneumonia Atelectasis occurring in only about 2% of chest radiographs

Chest radiograph not routinely required
Chest radiograph should obtained temperature >38. 3ºC unexplained chest pain leukocytosis hypoxemia

Chest radiograph should obtained patient requires hospitalization diagnosis is uncertain

Chest radiograph should obtained Intravenous drug abuse immunosuppression recent seizures

Chest radiograph should obtained cancer chest surgery heart failure

TREATMENT Mild Moderate severe Threatening
goals of therapy airflow airway obstruction inflammation Short Acting bronchodilator Corticosteroid

Mild & Moderate Asthma exacerbation

Inhaled beta agonists (SABA) albuterol 2. 5 to 5 mg every 20 minute for the first hour then 2. 5 to 10 mg every one to four hours as needed nebulization

Inhaled beta agonists (SABA) four to eight puffs every 20 minute for the first hour then dosing every one to four hours as needed MDI with spacer

Good Response No wheezing or dyspnea PEF ≥ 80% predicted or personal best Discharge Home

Discharge Home SABA every 3– 4 hours for 24 – 48 hours short course of oral systemic corticosteroids (prednisone 40 -60 mg po 5 to 10 day)
Mild & Moderate exacerbation unresponsive to treatment Admit to Hospital Severe exacerbation Risk factors for a fatal asthma attack

Inhaled beta agonists (SABA)

Inhaled anticholinergics

Inhaled anticholinergics (SAMA) recommend the addition of ipratropium for patients with severe exacerbations in the emergency department

Inhaled anticholinergics (SAMA) the combination provides greater bronchodilation than beta agonists alone

Inhaled anticholinergics (SAMA) Ipratropium 500 mcg every 20 minutes for three doses nebulization

Inhaled anticholinergics (SAMA) Ipratropium eight inhalations every 20 minutes for three doses MDI with spacer

Steroids 10 to 14 days may be given orally or IM or IV • methylprednisolone 60 – 80 mg every 6 to 12 hours • dexamethasone • Hydrocortisone • Prednisone 40 -60 mg Steroids

Good Response No symptoms PEF ≥ 80 predicted or personal best Discharge Home

For critically ill patients Inhaled beta agonists (SABA) continuous nebulization Administering 10 to 15 mg over one hour
Add Magnesium sulfate

Magnesium sulfate magnesium sulfate has bronchodilator activity in acute asthma

Magnesium sulfate Intravenous magnesium sulfate 2 gm infused over 20 min

Magnesium sulfate contraindicated • renal insufficiency • hypermagnesemia

Nonstandard therapies

Nonstandard therapies 1. helium-oxygen gas mixtures 2. leukotriene receptor antagonists 3. anesthetic agents 4. Nebulized furosemide 5. macrolide antibiotics 6. Parenteral beta-agonists

Helium-oxygen (low density gas) nebulization of albuterol using a heliumoxygen gas mixture increase the mass of albuterol delivered by allowing smaller particles to better penetrate to the lung periphery

Nonstandard therapies 1. helium-oxygen gas mixtures 2. leukotriene receptor antagonists 3. anesthetic agents 4. Nebulized furosemide 5. macrolide antibiotics 6. Parenteral beta-agonists

(Parenteral beta-agonists) Epinephrine severe asthma exacerbation unable to use inhaled bronchodilators anaphylactic reaction no evidence of anaphylaxis 0. 3 to 0. 5 mg IM 0. 3 to 0. 5 mg SC

(Parenteral beta-agonists) Terbutaline severe asthma exacerbation unresponsive to standard therapies 0. 25 mg SC every 20 minutes 3 doses
(Parenteral beta-agonists) epinephrine OR terbutaline not both

Mechanical ventilation noninvasive positive pressure ventilation

asthma exacerbation severe symptoms despite initial therapy we suggest trial of NPPV

mechanical ventilation Slowing of the respiratory rate depressed mental status worsening hypercapnia and respiratory acidosis oxygen saturation ˂95% despite high-flow supplemental oxygen

Ineffective therapies intravenous methylxanthines (theophylline or aminophylline ) inhaled glucocorticoids

recommendations for treating asthma exacerbations

Oxygen give sufficient oxygen to maintain Sa. O 2 > 92 percent

Oxygen give sufficient oxygen to maintain Sa. O 2 >95 percent in pregnancy

The Expert Panel does not recommend: aggressive hydration chest physical therapy Mucolytics

Antibiotics not generally recommended for the treatment of acute asthma exacerbations • because most respiratory infections that trigger an exacerbation of asthma are viral rather than bacterial
Antibiotics Exception comorbid conditions Fever AND purulent sputum evidence of pneumonia bacterial sinusitis

Medications upon discharge
All patients should receive prednisone: 30 to 60 mg once a day for 7 to 14 days then evaluated at a two-week

adequate supply of reliever (B 2 agonist) And controller (inhaled corticosteroid)

What is the prevention?

Trigger avoidance

How to use a peak flow meter
Asthma inhaler techniques

Prompt communication between patient and clinician

written asthma action plan

- Slides: 101