Treatment of Acute Asthma Exacerbation in Adults Therapeutic

Treatment of Acute Asthma Exacerbation in Adults: Therapeutic Update Jarred Kelly, B. Sc. Pharm, ACPR LMPS Year 2 Pharmacy Resident – Critical Care Oct 18, 2018 1

Objectives • Understand the place in therapy and evidence for each therapeutic alternative • Describe the clinical controversies of acute asthma exacerbation treatment • Develop an approach to pharmaceutical care for an acute asthmatic 2
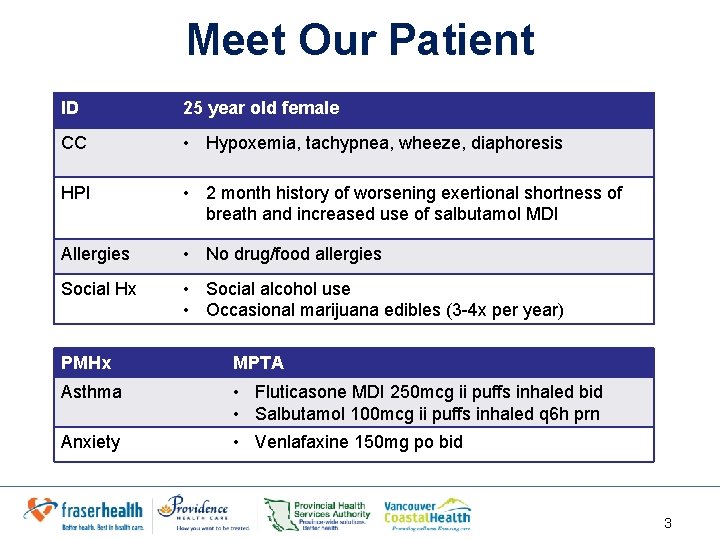
Meet Our Patient ID 25 year old female CC • Hypoxemia, tachypnea, wheeze, diaphoresis HPI • 2 month history of worsening exertional shortness of breath and increased use of salbutamol MDI Allergies • No drug/food allergies Social Hx • Social alcohol use • Occasional marijuana edibles (3 -4 x per year) PMHx MPTA Asthma • Fluticasone MDI 250 mcg ii puffs inhaled bid • Salbutamol 100 mcg ii puffs inhaled q 6 h prn Anxiety • Venlafaxine 150 mg po bid 3

Review of Systems Vitals and remarkable ROS at presentation to ED Vitals • T = 35. 1 BP = 140/85 HR = 130 -150 RR = 26 O 2 sat = 86% on RA (improved to 94% on 4 L O 2) CNS • A/O x 3, GCS 15, fatigued, anxious HEENT • Unremarkable CVS • Normal S 1/S 2, no murmurs Resp. • Wheeze on auscultation, SOB GI • Unremarkable GU • Unremarkable MSK/Derm • Diaphoretic, pale, cool 4

Clinical Course in ED • Initial blood gas – p. H 7. 32, p. O 2 102, p. CO 2 29, HCO 3 14 • Blood gas at intubation – p. H 6. 98, PO 2 121, p. CO 2 93, HCO 3 21 • Lactate 4. 7 • Intubated and mechanically ventilated • Transferred to ICU 5

Asthma “A common chronic disorder of the airways that is complex and characterized by variable and recurring symptoms, airflow obstruction, bronchial hyperresponsiveness, and an underlying inflammation” National Asthma Education and Prevention Program: Expert panel report III: Guidelines for the diagnosis and management of asthma. 2007. 6

Asthma Epidemiology – Global prevalence of 4. 3% – Prevalence 20% higher in women Consequences – Hospitalization – Disability – Impaired quality of life – Mortality National Asthma Education and Prevention Program: Expert panel report III: Guidelines for the diagnosis and management of asthma. 2007. 7

Asthma Exacerbation ‘Acute or subacute episodes of worsening in symptoms and lung function’ • Annual rate of ED visits for asthma around 8. 8 per 100 persons with asthma – Approximately 10% of these require hospitalization • Consequences – Large portion of asthma related healthcare and societal costs – Potentially worse future asthma control – Increased risk of future exacerbations Graham L, et al. Current Medical Research and Opinion. 2015; 31(4): 825 -35. 8

Asthma Exacerbation Symptoms Signs • • • Decreased FEV 1 • Decreased peak expiratory flow (PEF) • Elevated respiratory rate • Elevated pulse • Deceased oxygen sats • Use of accessory muscles • Decreased LOC • Low Pa. O 2 • Normal or increased p. CO 2 Shortness of breath Cough Wheezing Chest tightness Inability to speak sentences • Anxious/agitated • Confused 9
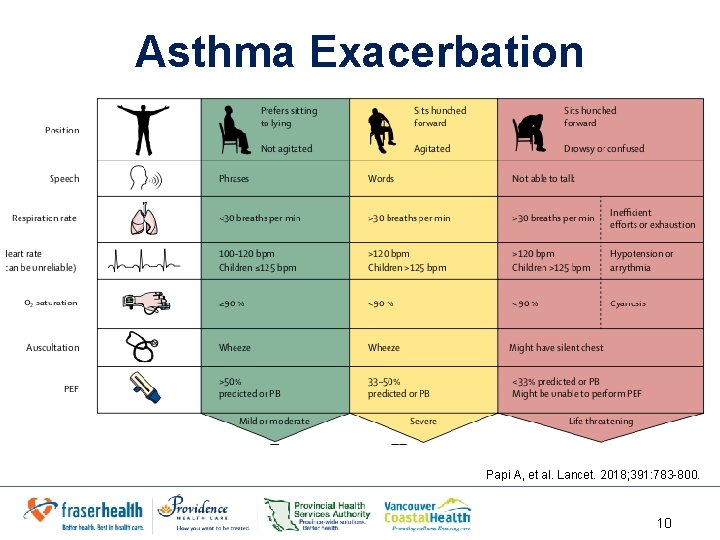
Asthma Exacerbation Papi A, et al. Lancet. 2018; 391: 783 -800. 10

Asthma Exacerbation • Triggers – Poor controller medication compliance – Allergens/irritant/pollution exposure – Cold air – Exercise – Infection (viral or bacterial) – Emotional stress Graham L, et al. Current Medical Research and Opinion. 2015; 31(4): 825 -35. 11
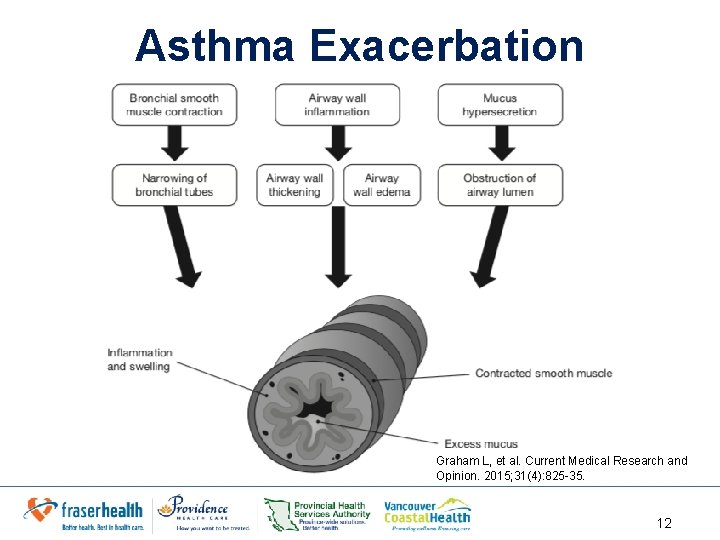
Asthma Exacerbation Graham L, et al. Current Medical Research and Opinion. 2015; 31(4): 825 -35. 12

Asthma Exacerbation • Factors that increase risk of asthma-related death – History of asthma exacerbation requiring intubation/ventilation – Hospitalization for asthma in past year – Poor medication adherence – Over-use of SABAs – Current/recent use of oral corticosteroids – History of psychiatric disease or psychosocial problems Papi A, et al. Lancet. 2018; 391: 783 -800. 13

Goals of Therapy • • Rapid reversal of airflow limitation Prevent hospital admission Resolve symptoms Reduce duration of ED and/or hospital stay Prevent subsequent exacerbations Improve quality of life Prevent adverse effects of medication 14

Inhaled Short-Acting Beta 2 Agonists • MOA – Bronchodilator via agonism of beta 2 receptors in airways • ADR – Tachycardia, hypokalemia, increased lactate • Dose – Mild-moderate/Severe • Salbutamol MDI 4 -10 puffs q 20 min for first hour • Then salbutamol up to 6 -10 puffs q 1 -2 h depending on response – Life threatening • Salbutamol 5 mg q 20 min for first hour via nebulizer Papi A, et al. Lancet. 2018; 391: 783 -800. 15

MDI + Spacer vs. Nebulizer • 2013 Cochrane Review – Similar improvement in lung function – No difference in hospital admissions RR 0. 94 (0. 61 to 1. 43), length of ED stay (adults) – Excluded life-threatening exacerbation • Nebulizer recommended if severe/lifethreatening exacerbation Cates J, et al. Cochrane Database Syst Rev. 2013; 9: CD 000052. 16

IV Beta-Agonists? • No benefit of IV vs. inhaled beta 2 agonists • Insufficient evidence to recommend adding IV beta-agonist to inhaled beta-agonist • Risk of adverse events – Hypokalemia, arrhythmias, elevated lactate, tremors • No role in treatment Travers AH, et al. Cochrane Database Syst Rev. 2012; 12: CD 010179 Travers AH, et al. Cochrane Database Syst Rev. 2001; 1: CD 002988. 17

Inhaled Anticholinergics • MOA – Blocks muscarinic cholinergic receptors in airways resulting in bronchodilation • ADR – Tremor, dry mouth, anxiety, palpitations • Dose – Ipratropium MDI 4 -8 puffs q 20 min for first hour, then as needed – 500 mcg q 20 min via nebulizer for first hour, then as needed Papi A, et al. Lancet. 2018; 391: 783 -800. 18

Inhaled Anticholinergics • 2017 Cochrane Review – Reduced risk of hospitalization RR 0. 72 (0. 59 to 0. 86) • Significance limited to severe subgroup – Increased adverse events OR 2. 03 (1. 28 to 3. 20) • No one adverse event statistically significant Kirkland SW, et al. Cochrane Database Syst Rev. 2017; 1: CD 001284. 19

Systemic Corticosteroids • MOA – Decreased inflammation, up-regulation of beta-2 receptors, decreased microvascular permeability, decreased mucus production • Onset – Will not see effects for 4 -6 hours, early administration key • ADR – Insomnia, nausea, dyspepsia, malaise, behavioral changes, hyperglycemia • Dose – Prednisone equivalent 1 mg/kg daily, max 50 mg 20

Systemic Corticosteroids • Use associated with more rapid resolution of symptoms, reduced hospitalizations and relapses • High vs. low dose – No difference in outcomes • Oral vs. IV – Equal efficacy – Consider IV if critically ill (too dyspneic to swallow or unsure of enteral absorption) • Duration – 5 to 7 days generally demonstrated equal efficacy to 1014 day courses Normansell, et al. Cochrane Database Syst Rev 2016; 5: CD 011801. Manser R, et al. Cochrane Database Syst Rev. 2001; 1: CD 001740. 21

Role for Inhaled Corticosteroids? • 2012 Cochrane Review – Possibly reduces hospital admissions in those with mild exacerbations not treated with systemic steroids – Insufficient evidence that ICS therapy can be used in place of systemic corticosteroids – Insufficient evidence that ICS + systemic steroids results in improved outcomes Edmonds ML, et al. Cochrane Database Syst Rev. 2012; 12: CD 002308 22

Magnesium • MOA – Relaxes smooth muscle by inhibiting calcium ion influx – May augment beta-receptor response to salbutamol • PK – Onset within minutes; duration up to 2 hours • ADR – Hypermagnesaemia with muscle weakness and respiratory fatigue, nausea, flushing • Dose – 2 g IV infusion over 20 minutes x 1 Kew KM, et al. Cochrane Database Syst Rev. 2014; 5: CD 010909 23

Magnesium • Can consider in patients with severe exacerbations unresponsive to initial treatment – Safety and efficacy of repeated IV doses or IV infusions not known – Appeared to reduce hospital admissions OR 0. 75 (0. 60 to 0. 92) in severe patients • Do not delay intubation for magnesium in patients with life-threatening exacerbation • Inhaled Magnesium? – Systematic review of inhaled magnesium showed no improvement in lung function or hospital admissions Knightly R et al. Cochrane Database Syst Rev. 2017; 11: CD 008998 Kew KM, et al. Cochrane Database Syst Rev. 2014; 5: CD 010909 24

Ketamine • MOA – Blocks NMDA receptor-induced bronchoconstriction – Sympathomimetic effect, antagonism to histamine and acetylcholine, calcium influx blockage, and a membrane-stabilizing effect • ADR – Increased airway secretions, hallucinations, negative inotropy, emergence reaction • Dose – IV infusion of 0. 5 to 2. 5 mg/kg/h Goyal S, et al. Indian J Crit Care Med. 2018; 17(3): 154 -161. 25

Evidence for Ketamine • Non-intubated patients – Two RCTs (one pediatric, one adult) showed no clinical benefit • Mechanically ventilated patients – No prospective trials – Case series show improved peak inspiratory pressures, lung compliance, gas exchange, and decreased O 2 requirements • Overall quality of evidence is poor Goyal S, et al. Indian J Crit Care Med. 2018; 17(3): 154 -161. 26

Antibiotics? • Not recommended except as needed for comorbid conditions – Use if purulent sputum, evidence of pneumonia • 2018 Cochrane Review • 2016 AZALEA RCT Johnson SL, et al. JAMA Intern Med. 2016; 176(11): 1630 -37. Normansell R, et al. Cochrane Database syst Rev. 2018; 6: CD 002741. 27

Methylxanthines? • Theophylline/aminophylline not recommended • 2012 Cochrane Review – No additional benefit to optimal SABA for hospital admissions OR 0. 58 (0. 30 to 1. 12) – No improvement in lung function – Increased frequency of ADRs (arrhythmias, vomiting) Nair P, et al. Cochrane Databse Syst Rev. 2012; 12: CD 002742. 28

Heliox? • Helium-oxygen (typically 70 -80: 30 -20%) mixtures administered instead of oxygen • Rationale: – Low density of helium decreases resistance to airflow in conditions of turbulent flow present in constricted airways • 2001 Cochrane Review – No difference in any outcome • 2014 Cochrane Review – Potential benefit of using Heliox for nebulization of Beta 2 agonists Rodrigo, et al. Cochrane Databse Syst Rev. 2001; 1: CD 002884 Rodrigo, et al. Ann of Allergy, Asthma & Immunology. 2014; 112(1): 29 -34. 29

Sedative/Anxiolytics? • Anxiolytic and hypnotics should not be used due to respiratory depressant effect • If comorbid anxiety focus treatment on asthma exacerbation • EXCEPTION – If patient is intubated/mechanically ventilated 30
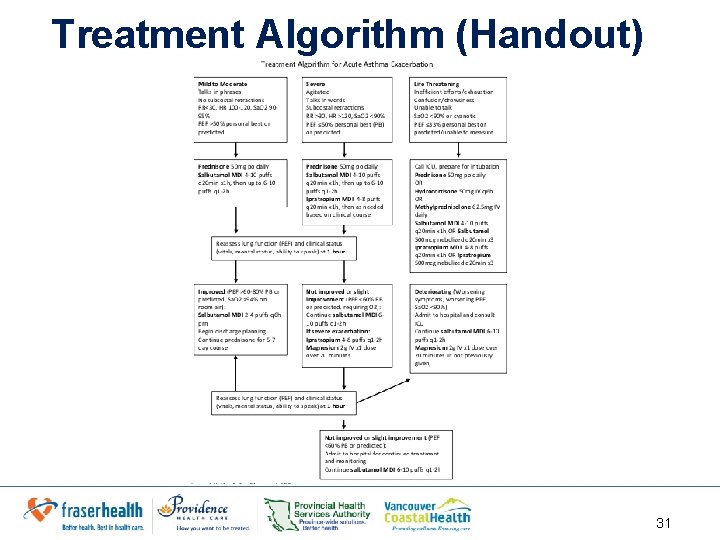
Treatment Algorithm (Handout) 31

Monitoring Parameter Frequency Vitals: HR, BP, RR, O 2 sat CNS: Agitation, anxiety, LOC, drowsiness, confusion, fatigue HEENT: Ability to talk CVS: fluid status Resp: PEF, wheeze, accessory muscle use, air entry DERM: cyanotic, pale, diaphoretic Labs (consider if admitted and/or life threatening): Arterial blood gas, electrolytes, CBC, lactate Q 1 h Q 1 h Depending on clinical status 32

Discharge Management • • Review inhaler technique Review PEF meter technique Optimize dose of ICS Asthma action plan – Oral corticosteroids – How to adjust reliever and controller medications – When to seek medical care 33

References 1. 2. 3. 4. 5. 6. 7. 8. 9. 10. 11. 12. 13. 14. 15. 16. 17. 18. 19. National Asthma Education and Prevention Program: Expert panel report III: Guidelines for the diagnosis and management of asthma. Bethesda, MD: National Heart, Lung, and Blood Institute, 2007. Graham L, Eid N. The impact of asthma exacerbations and preventative strategies. Current Medical Research and Opinion. 2015; 31(4): 825 -835. Global Strategy for asthma management and prevention. Updated 2018. Global Initiative for Asthma 2018. Available at: https: //ginasthma. org/2018 gina-report-global-strategy-for-asthma-management-and-prevention/ Papi A, Brightling C, Pedersen S, Reddel H. Asthma. Lancet. 2018; 391: 783 -800 Cates CJ, Welsh EJ, Rowe BH. Holding chambers (spacers) versus nebulisers for beta-agonist treatment of acute asthma. Cochrane Database Syst Rev. 2013; 9: CD 000052. Travers AA, et al. Intravenous beta 2 -agonists for acute asthma in the emergency department. Cochrane Database Syst Rev. 2001; 1: CD 002988. Travers AH, Milan SJ, Jones AP, Camargo CA jr, Rowe BH. Addition of intravenous beta(2)-agonists to inhaled beta(2)-agonists for acute asthma. Cochrane Database Syst Rev. 2012; 12: CD 010179. Kirkland SW, Vandenberghe C, Voaklander B, Nickel T, Campbell S, Rowe BH. Combined inhaled beta-agonist and anticholinergic agents for emergency management in adults with asthma (Review). Cochrane Database Syst Rev. 2017; 1: CD 001284. Normansell R, Kew KM, Mansour G. Different oral corticosteroid regimens for acute asthma (Review). Cochrane Database Syst Rev. 2016; 5: CD 011801. Manser R, Reid D, Abramson MJ. Corticosteroids for acute severe asthma in hospitalized patients. Cochrane Database Syst Rev. 2001; 1: CD 001470. Knightly R, Milan SJ, Hughes R, Knopp-Sihota JA, Rowe BH, Normansell R, Powell C. Inhaled magnesium sulfate in the treatment of acute asthma. Cochrane Database Syst. Rev. 2017; 11: CD 003898. Kew KM, Kirtchuk L, Michell, C. Intravenous magnesium sulfate for treating adults with acute asthma in the emergency department. Cochrane Database Syst Rev. 2014; 5: CD 010909 Goyal S, Agrawal A. Ketamine in status asthmaticus: A review. Indian J Crit Care Med. 2013; 17(3): 154 -161. Howton J, Rose J, Duff S, Zoltanski T, Levitt M. Randomized, double-bind, placebo-controlled trial of intravenous ketamine in acute asthma. Ann Emerg Med. 1996; 27(2): 170 -175. Normansell R, Sayer B, Waterson S, Dennett EJ, Del Forno M, Dunleavy A. Antibiotics for exacerbations of asthma. Cochrane Database of Syst Rev. 2018; 6: CD 002741. Johnston SL, et al. Azithromycin for acute exacerbations of asthma The AZALEA Randomized Clinical Trial. JAMA Internal Medicine. 2016; 176(11): 1630 -37. Nair P, Milan SJ, Rowe BH. Addition of intravenous aminophylline to inhaled beta(2)-agonists in adults with acute asthma. Cochrane Database Syst Rev. 2012; 12: CD 002742. Rodrigo G, Rodrigo C, Pollack C, Travers A. Helium-oxygen mixture for nonintubated acute asthma patients. Cochrane Database Syst Rev. 2001; 1: CD 002884. Rodrigo G, Castro-Rodriguez J. Heliox-driven B 2 -agonists nebulization for children and adults with acute asthma: a systematic review with metaanalysis. Annals of Allergy, Asthma, & Immunology. 2014. 112(1): 29 -34. 34
- Slides: 34