TREATMENT MODALITIES CLASS II OF MALOCCLUSION BYDR VEERENDRA

TREATMENT MODALITIES CLASS II OF MALOCCLUSION BYDR. VEERENDRA V KERUDI
INTRODUCTION Edward Angle 1899 “The classification of malocclusion” Class II malocclusion : The condition in which the permanent mandibular first molar occludes distal to the normal relationship with the permanent maxillary first molar. Normal occlusion : The mesio buccal cusp of the permanent maxillary first molar occludes with the mesiobuccal groove of the mandibular first molar. Class II div 1 : Maxillary incisors are protruding. /Subdivision Class II div 2 : Maxillary incisors are retruding. / Subdivision Term “Distoocclusion”: Benno Lischer 1912

PREVALENCE Angle: 27% Average : 25 - 30 % Prevalence appears to decrease with age: NHANES 1960 (NATIONAL HEALTH AND NUTRITIONAL EXAMINATION SURVEY ) No sex difference Asia: 10 -15 % Least: 1 -5% south pacific & black Africans
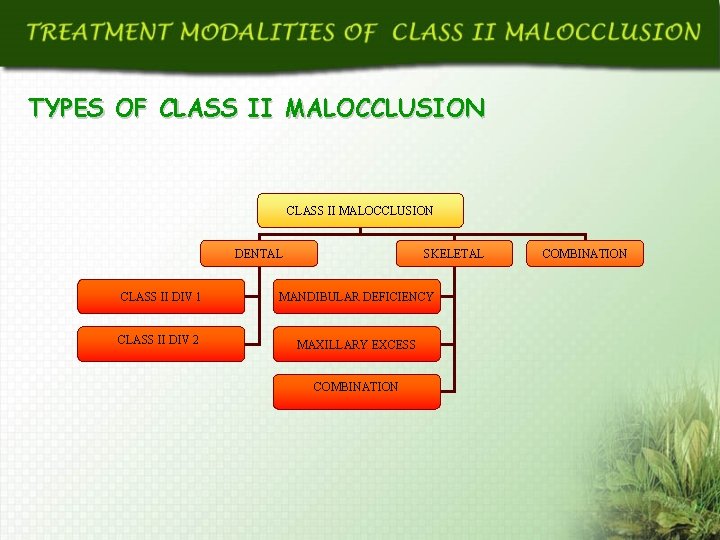
TYPES OF CLASS II MALOCCLUSION DENTAL SKELETAL CLASS II DIV 1 MANDIBULAR DEFICIENCY CLASS II DIV 2 MAXILLARY EXCESS COMBINATION
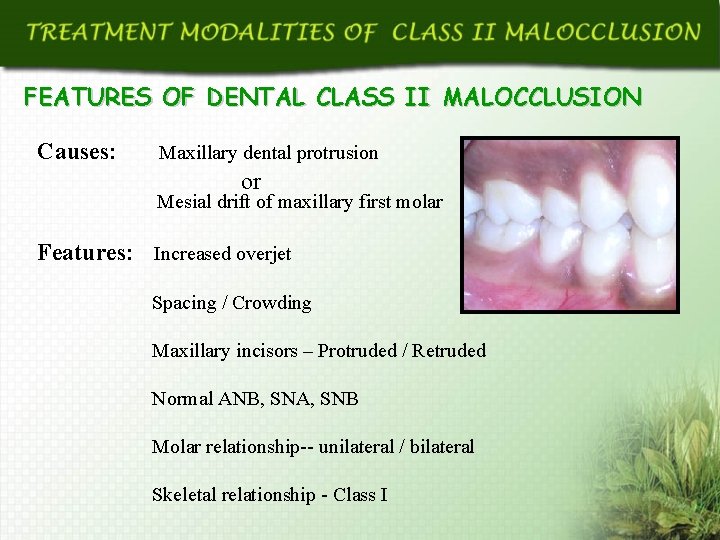
FEATURES OF DENTAL CLASS II MALOCCLUSION Causes: Maxillary dental protrusion or Mesial drift of maxillary first molar Features: Increased overjet Spacing / Crowding Maxillary incisors – Protruded / Retruded Normal ANB, SNA, SNB Molar relationship-- unilateral / bilateral Skeletal relationship - Class I

TREATMENT OBJECTIVES OF CLASS II DIV 1 (DENTAL) q q q Reduction of overjet Reduction of overbite Correction of crowding & rotation Correction of molar relationship Correction of posterior crossbite if any Normalizing the musculature

TREATMENT OBJECTIVES OF CLASS II DIV 2 (DENTAL) q Correction of incisor relationship q Correction of deep bite q Correction of crowding & rotation q Correction of molar relationship

FEATURES OF SKELETAL CLASS II MALOCCLUSION The term indicate that the class II malrelationship is one resulting from an anteroposterior disproportion in size or discrepancy in position of the jaws rather than malposition of the teeth relative to the jaws ( retrusion of mandible or protrusion of maxilla or both). Features: Often associated with Dental class II malocclusion May be associated with Dental class I malocclusion Dental compensation (Generally) Narrow maxillary arch Subdivided : Mandibular deficiency Maxillary excess Combination

SKELETAL CLASS II MAY BE DUE TO…… Mandibular Retrusion / Deficiency Maxillary Protrusion / Excess Combination

COMBINATION OF MANDIBULAR DEFICIENCY AND MAXILLARY EXCESS Common to have this condition Each of this will add to severity of malocclusion Thought to be: mandible at fault assuming the maxillary first molar, relative to maxilla, is biologically stable. After the advent of cephalometrics – maxillary skeletal deformities appreciated. Most patients with skeletal class II problems have a combination of mandibular deficiency & maxillary excess.
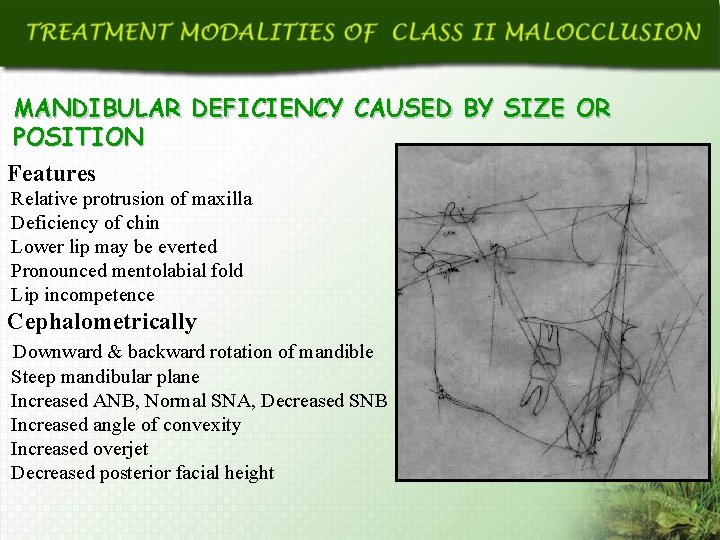
MANDIBULAR DEFICIENCY CAUSED BY SIZE OR POSITION Features Relative protrusion of maxilla Deficiency of chin Lower lip may be everted Pronounced mentolabial fold Lip incompetence Cephalometrically Downward & backward rotation of mandible Steep mandibular plane Increased ANB, Normal SNA, Decreased SNB Increased angle of convexity Increased overjet Decreased posterior facial height

ANOTHER VARIATION: SHORT MANDIBULAR BODY WITH NORMAL OR INCREASED RAMUS Features: Increased posterior facial height Flatter mandibular plane Lower anterior facial height – both lips are everted Deep anterior overbite Mask anteroposterior dental discrepancy Lingual inclination of maxillary incisors & reduced overjet
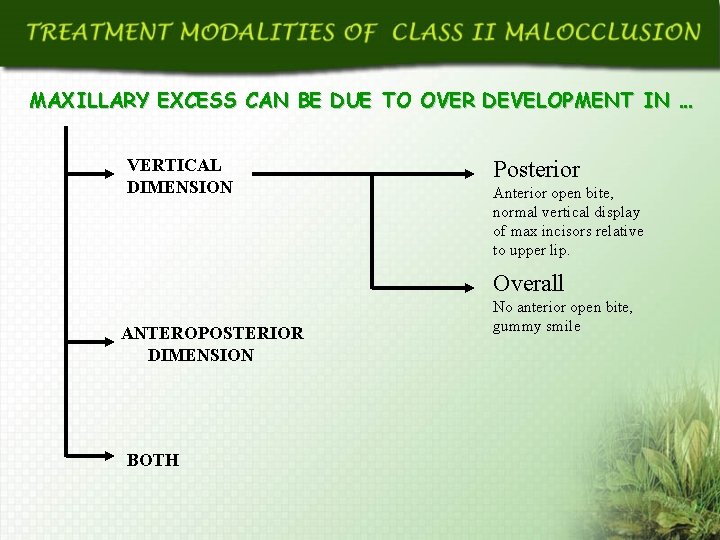
MAXILLARY EXCESS CAN BE DUE TO OVER DEVELOPMENT IN … VERTICAL DIMENSION Posterior Anterior open bite, normal vertical display of max incisors relative to upper lip. Overall ANTEROPOSTERIOR DIMENSION BOTH No anterior open bite, gummy smile

FEATURES OF VERTICAL MAXILLARY EXCESS Relative chin retrusion and relative maxillary protrusion Increased lower anterior facial height Increased ANB Increased angle of convexity, increased overjet Narrow nose with prominent dorsum Lip incompetence FEATURES OF ANTEROPOSTERIOR MAXILLARY EXCESS Midface protrusion Increased SNA Increased maxillary length

HISTORICAL BACKGROUND FOR CLASS II TREATMENT 19 th century : Limited to maxillary anterior retraction to decrease overjet. 1880, Norman Kingsley: Extraction of maxillary first premolars & retraction of maxillary anterior teeth with extraoral forces applied with headgear. Early 20 th century : Calvin Case influenced by Edward Angle’s nonextraction concept, believed in expansion & correction of class II malocclusion by class II elastic traction. In United States principle appliance for facial orthopaedic treatment was head gear, whereas in Europe functional appliances were used.

Charles Tweed in 1940 s : Renewed enthusiasm for treatment of class II malocclusion with extraction. After 1950 s Alan Brodie : Importance to genetics, only option is dental camouflage by extraction of the teeth. Silas Kloehn : Reintroduced extraoral forces in the form of cervical head gear. Meanwhile, Europeans emphasised on removable appliances. After 1960 s : Convergence of ideas. 1960 s & 1970 s : Surgical approach for treating class II malocclusion.
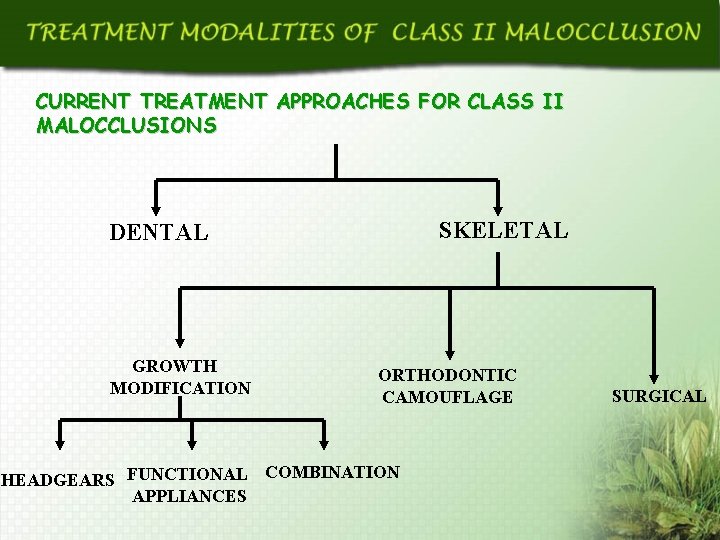
CURRENT TREATMENT APPROACHES FOR CLASS II MALOCCLUSIONS SKELETAL DENTAL GROWTH MODIFICATION ORTHODONTIC CAMOUFLAGE HEADGEARS FUNCTIONAL COMBINATION APPLIANCES SURGICAL

CURRENT TREATMENT APPROACHES FOR DENTOALVEOLAR CLASS II MALOCCLUSIONS Dental class II malocclusion with normal skeletal jaw relationship is less common & is caused by forward movement of maxillary molars relative to mandibular molars. Two approaches for treating this condition : Extraction Non Extraction

CURRENT TREATMENT APPROCHES FOR TREATING SKELETAL CLASS II MALOCCLUSIONS Important to distinguish the condition whether dental or skeletal Three treatment approaches for treating skeletal problems: Growth modification Dentoalveolar camouflage Orthognathic surgery

GROWTH MODIFICATION Whatever jaw discrepancy exists, the ideal solution is to correct it by modifying growth. The ideal time for growth modification is the period of rapid growth during the mixed dentition just before puberty. Growth modification, through either a functional appliance or extraoral force, is aimed at the mandibular condyles and/or the maxillary sutures by applying forces directly to the teeth and indirectly to the skeletal sutures. The focus of growth modification treatment is skeletal change, dental change also must be expected. Except for the most severe problems, growth modification therapy for skeletal discrepancies is best deferred until the preadolescent years when growth modification results are more stable.

A typical treatment plan for jaw discrepancies is in two phases: q The first phase is at mixed dentition stage which focuses on correcting skeletal problem. It should begin 1 to 3 years before the peak of the adolescent growth spurt. q Second phase focuses on comprehensive fixed appliance treatment.

THREE TYPES OF APPLIANCES FOR GROWTH MODIFICATION ü EXTRA ORAL APPLIANCE ü FUNCTIONAL APPLIANCE ü COMBINATION

EXTRAORAL FORCE (HEADGEAR) APPLIANCES Designed to deliver an adequate extraoral orthopedic force to compress the maxillary sutures, modifying the pattern of bone apposition at these sites. Posterior and superior forces intended to inhibit anterior and inferior development of the maxilla, also to inhibit mesial and occlusal eruption of maxillary posterior teeth. GOAL: Restrict maxillary growth so that mandibular growth catch up. FORCES: Sufficient magnitude, appropriate direction, adequate length of time.
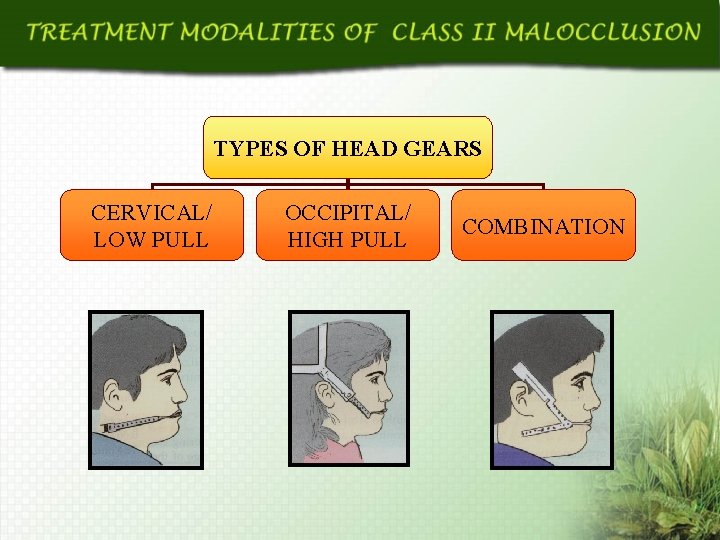
TYPES OF HEAD GEARS CERVICAL/ LOW PULL OCCIPITAL/ HIGH PULL COMBINATION

HISTORICAL BACKGROUND Extraoral force appliance was used by pioneer orthodontists in late 1800′s. Angle and Kingsley also used this appliance with reasonable success. By 1920 Angle and his followers believed that class II and class III elastics not only moved teeth but also caused significant skeletal changes. Therefore extraoral appliances and mixed dentition treatment were abandoned. In 1940′s the use of cephalometrics did not support the concept that significant skeletal changes occurred in response to intraoral forces. 1 n 1936 Oppenheim revived the idea that headgear would serve as valuable adjunct to treatment. After world war II kloehn′s results with headgear treatment of class II malocclusion became widely known.

SELECTION OF HEADGEAR ANCHORAGE LOCATION v Should provide a correct vertical component of force to the dental and skeletal structures HEADGEAR ATTACHMENT TO THE DENTITION v Face bow to tubes on first permanent molars v Face bow to removable appliances v Face bow to arch wire FORCE VALUE AND DURATION

EXTRAORAL FORCE APPLICATION FOR SKELETAL CLASS II TREATMENT FORCE VALUES: 400 – 600 gm (1 - 1. 5 pounds) per side -- maximizes skeletal change and minimizes dental change. DURATION: 12 -16 hrs/day (circadian pattern – evening and night) FORCE VECTOR: superior and posterior above, the center of resistance of maxillary molars. Treatment must be during active growth. It is necessary to control the magnitude, direction & duration of the extraoral force to achieve specific effects.
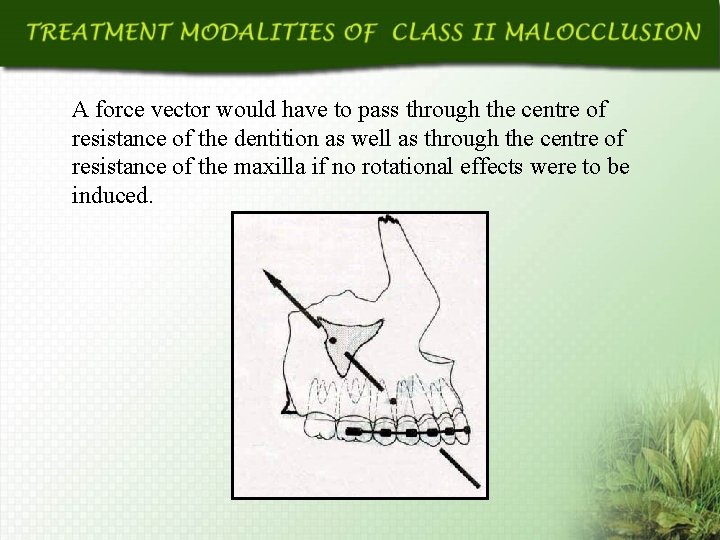
A force vector would have to pass through the centre of resistance of the dentition as well as through the centre of resistance of the maxilla if no rotational effects were to be induced.

IDEAL INDICATION: Correction of skeletal class II malocclusion with AP maxillary excess. CONDITION: Mandibular growth should be active in forward direction rather than downward direction. Cervical or neck strap is indicated in patients with flat mandibular and occlusal planes (closure to true horizontal) in which an increase in facial dimension is desired. Occipital attachments or head cap contributes for the correction of AP maxillary excess and vertical maxillary excess. Combination type modifies AP excess.

GROWTH MODIFICATION BY FUNCTIONAL APPLIANCES Mandibular deficiency: Small mandible or normal mandible in posterior position TREATMENT POSSIBILITY ØRestrain growth of maxilla with extraoral force and let the mandible grow – catch up the growth ØEnhancement of mandibular skeletal growth

PRINCIPLES IN GROWTH MODIFICATION The maxilla grows by apposition of new bone at its posterior and superior sutures in response to being pushed forward by lengthening cranial base and pulled downward and forward by the growth of the adjacent soft tissues. Tension at the sutures appears to be the stimulus for new bone formation Similarly The mandible is pulled downward and forward by the soft tissues in which it is embedded. In response the condylar process grows upward and backward to maintain the TMJ articulation. Therefore pressure resisting the downward and forward movement of either jaw should decrease the amount of growth and forces that pull them downward and forward should increase their growth.

EFFECTS OF FUNCTIONAL APPLIANCES ØWhen mandible is held forward, the elasticity of the soft tissues produces a reactive forces against the maxilla and restrain of maxillary growth often occurs. ØMandibular growth acceleration. ØExerts distal force on upper incisors and tends to tip them lingually. ØProtrusive effect on mandibular dentition. ØInfluences the eruption of anterior and posterior teeth. ØPossible to level curve of spee in lower arch by blocking eruption of lower incisors leaving the posterior teeth free to erupt. ØUpper posterior teeth are prohibited from erupting and moving forward, while lower posterior teeth are erupting upward and forward resulting in rotation of occlusal plane which corrects class II relationship.
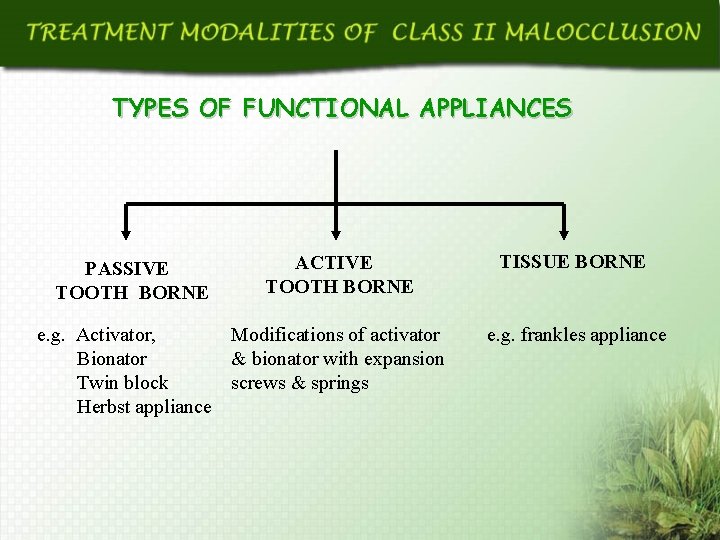
TYPES OF FUNCTIONAL APPLIANCES PASSIVE TOOTH BORNE ACTIVE TOOTH BORNE e. g. Activator, Modifications of activator Bionator & bionator with expansion Twin block screws & springs Herbst appliance TISSUE BORNE e. g. frankles appliance
WHICH ONE TO SELECT ? ?

ACTIVATOR v Originated by Andresen and modified by Haupl. v Fits loosely. v Advances the mandible for class II correction. v Tips anterior teeth. v Controls eruption of teeth to alter vertical dental relationships. v. Dental relationships in all three planes of space can be changed.
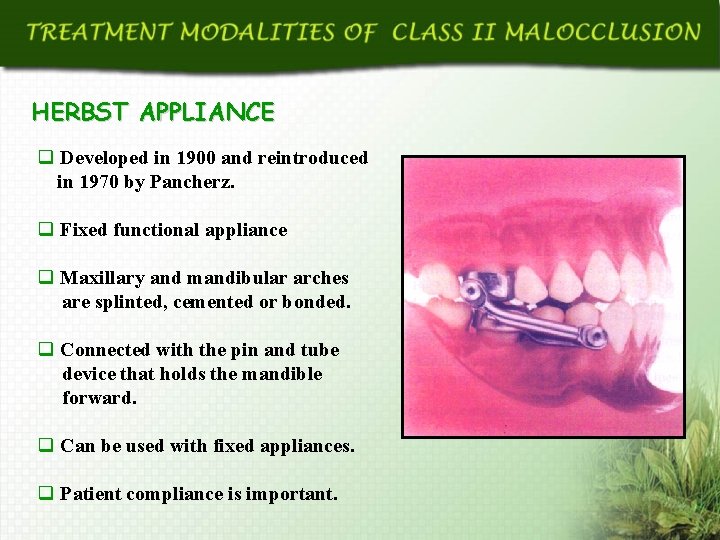
HERBST APPLIANCE q Developed in 1900 and reintroduced in 1970 by Pancherz. q Fixed functional appliance q Maxillary and mandibular arches are splinted, cemented or bonded. q Connected with the pin and tube device that holds the mandible forward. q Can be used with fixed appliances. q Patient compliance is important.
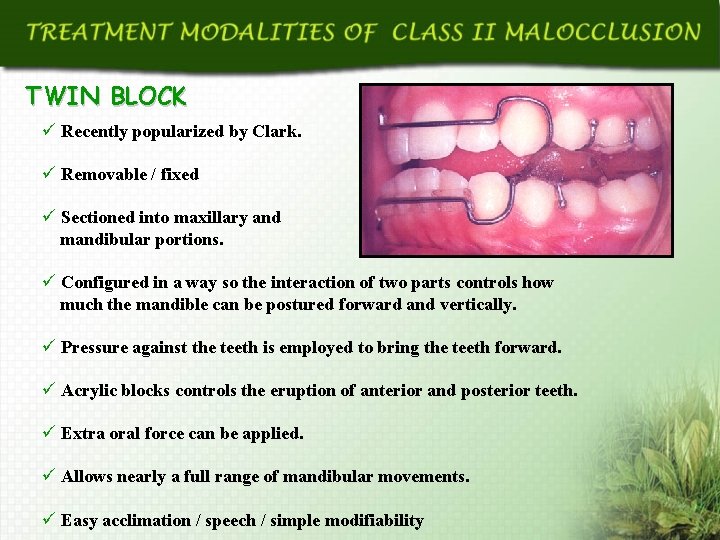
TWIN BLOCK ü Recently popularized by Clark. ü Removable / fixed ü Sectioned into maxillary and mandibular portions. ü Configured in a way so the interaction of two parts controls how much the mandible can be postured forward and vertically. ü Pressure against the teeth is employed to bring the teeth forward. ü Acrylic blocks controls the eruption of anterior and posterior teeth. ü Extra oral force can be applied. ü Allows nearly a full range of mandibular movements. ü Easy acclimation / speech / simple modifiability

FUNCTIONAL REGULATOR OF FRANKLE ü Tissue born. ü Much of the appliance is located in the vestibule. ü Alters the mandibular posture and contour of facial soft tissue. ü Enhances dental eruption. ü Alters dental relations. ü Arch expansion is possible. ü Effects the jaw growth.
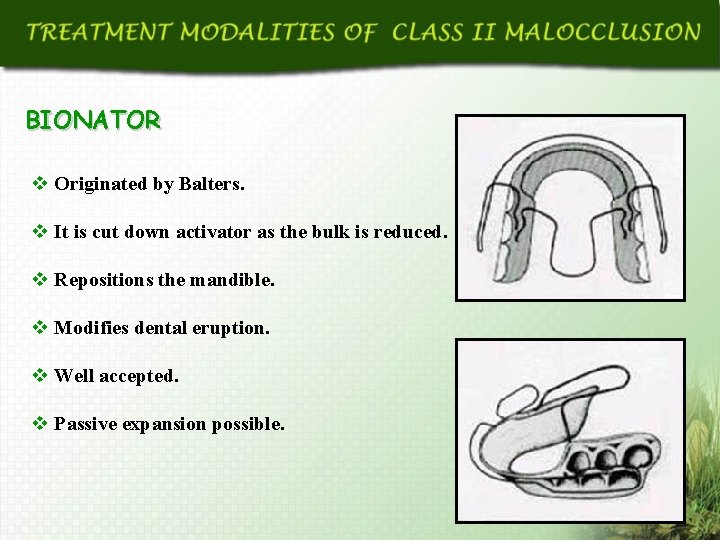
BIONATOR v Originated by Balters. v It is cut down activator as the bulk is reduced. v Repositions the mandible. v Modifies dental eruption. v Well accepted. v Passive expansion possible.

COMBINED GROWTH MODIFICATION TREATMENT Combined appliance approach to orthopedic treatment using extraoral force in combination with a functional appliance may provide greater cumulative skeletal growth effects than use of either appliance alone. Utilizes an occipital attachment connected to a facebow inserted into headgear tubes that are incorporated into the interocclusal acrylic in the premolar region. Combined approach is often reserved for more severe skeletal class II problems with severe maxillary excess & mandibular deficiency.
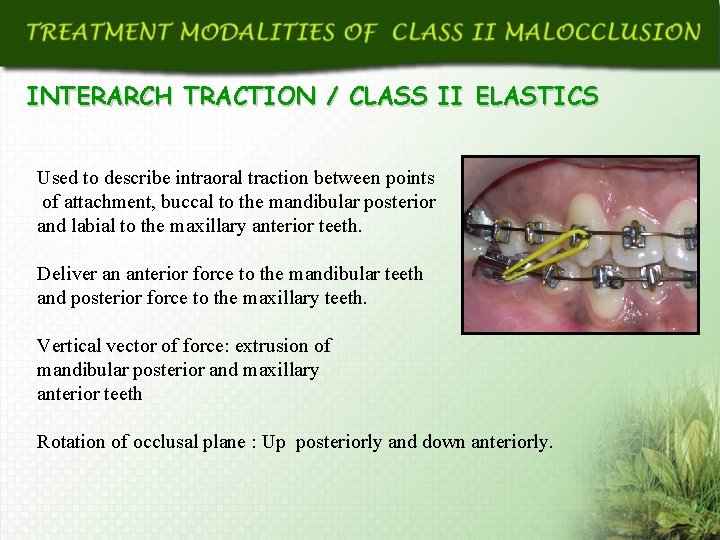
INTERARCH TRACTION / CLASS II ELASTICS Used to describe intraoral traction between points of attachment, buccal to the mandibular posterior and labial to the maxillary anterior teeth. Deliver an anterior force to the mandibular teeth and posterior force to the maxillary teeth. Vertical vector of force: extrusion of mandibular posterior and maxillary anterior teeth Rotation of occlusal plane : Up posteriorly and down anteriorly.

INDICATIONS OF INTERARCH TRACTION Ø Where anterior movement of mandibular teeth is desired and rotation of occlusal plane is not detrimental. Ø Protrusive and slight intrusive maxillary incisors and slight constriction of mandibular molars. ØMinimal mandibular growth potential with flat occlusal and mandibular planes where as increase in lower face height is desired. Limited to the permanent dentition with complete fixed orthodontic appliance.

DENTOALVEOLAR CAMOUFLAGE FOR SKELETAL CLASS II CORRECTION Goal is to disguise the unacceptable skeletal relationship by orthodontically repositioning the teeth in the jaws so that there is an acceptable dental occlusion and facial appearance. Dental camouflage is aimed at creating or accelerating dental compensation for the skeletal discrepancy. Indications : Older adolescents or adults – no longer have growth potential Mild to moderate Skeletal class II Patient not willing for surgery Types : Dentoalveolar camouflage without extractions Dentoalveolar camouflage with extractions

CAMOUFLAGE ? One of the difficult decisions is whether a patient with borderline skeletal discrepancy can be treated with orthodontics alone? How to decide which patient has the potential to be successfully camouflaged and which would be better surgical candidates? § Patients with long face or skeletal open bite are difficult to treat orthodontically § Short face or skeletal deep bite – possibility of camouflage § Amount of increased arch length discrepancy in class II and class III cases – possibility of camouflage is less. § Soft tissue relationship is an important factor § Transverse problems -Skeletal asymmetry can be camouflaged orthodontically only if chin and external body contours are not involved. § Greater the skeletal involvement more likely surgery is needed

DENTOALVEOLAR CAMOUFLAGE WITHOUT EXTRACTION Goal: To retract the maxillary dentition and protract the mandibular dentition to the extent that overjet is eliminated and normal posterior occlusion is achieved. Maximize maxillary posterior anchorage and maximize mandibular anterior anchorage INDICATIONS: Mild skeletal problems Mild excessive overjet

DENTOALVEOLAR CAMOUFLAGE WITH EXTRACTIONS TREATMENT APPROACHES Ø Extraction of maxillary first premolars with retraction of anteriors. ØExtraction of maxillary and mandibular first or second premolars with retraction of anteriors. ØExtraction of maxillary second molar & retraction of all the teeth.

SURGICAL APPROACH FOR THE CLASS II SKELETAL PROBLEMS FEATURES OF THE MALOCCLUSION FOR SURGERY In patients whose orthodontic problems are so severe that neither growth modification nor camouflage offer a solution and surgical realignment of the jaws or repositioning of dentoalveolar segments is the only possible treatment.

HISTORICAL BACKGROUND FOR SURGICAL CLASS II TREATMENT q Surgical treatment for mandibular prognathism began early in 20 th century but the progress was gradual. q Trauner and Obwegeser introduced a Sagittal split ramus osteotomy with intra oral approach in 1959 which marked the beginning of a new era in orthognathic surgery. q In 1960 s American surgeons began to use and modify techniques for maxillary surgery, which were developed in Europe. q Bell, Epker and Wolford played major role in development of maxillary surgeries. q Lefort I down fracture technique allowed repositioning of maxilla in all three planes of space. q In 1980 s repositioning of either or both the jaws in all three planes became possible.

TYPES OF SURGICAL ORTHODONTIC TREATMENT FOR SKELETAL CLASS II CORRECTION OF AP RELATIONSHIPS Maxillary surgery Mandibular advancement CORRECTION OF VERTICAL RELATIONSHIPS Maxillary surgery Mandibular surgery CORRECTION OF TRANSVERSE RELATIONSHIPS Maxillary surgery Mandibular surgery Genioplasty

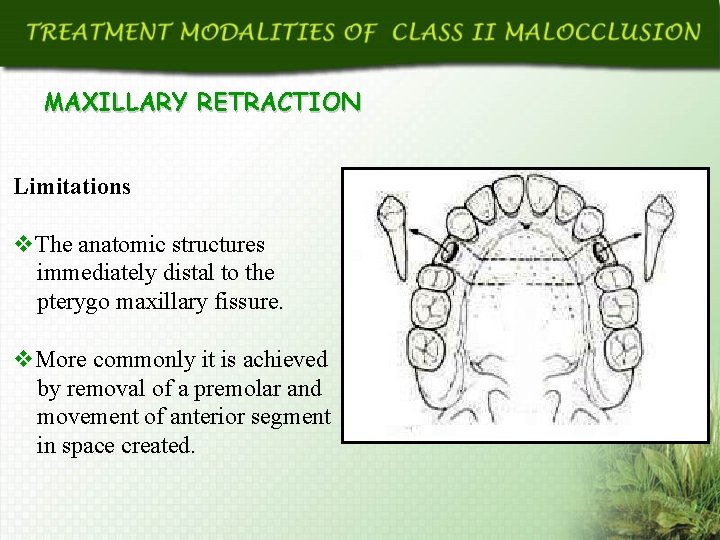
MAXILLARY RETRACTION Limitations v. The anatomic structures immediately distal to the pterygo maxillary fissure. v. More commonly it is achieved by removal of a premolar and movement of anterior segment in space created.
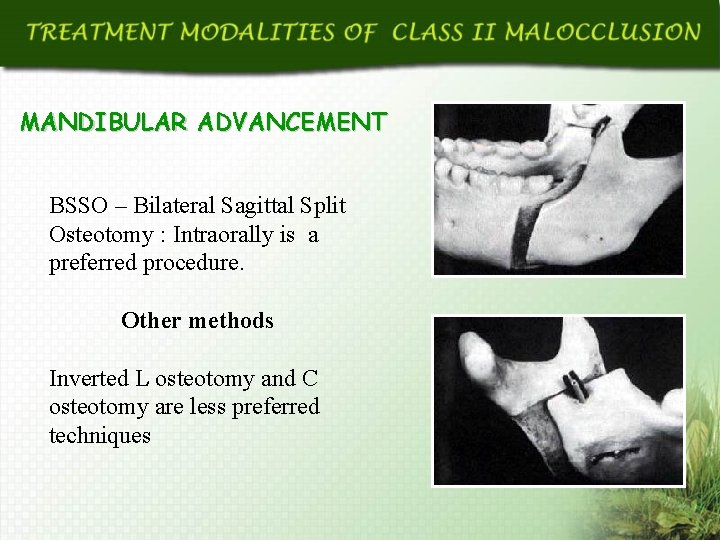
MANDIBULAR ADVANCEMENT BSSO – Bilateral Sagittal Split Osteotomy : Intraorally is a preferred procedure. Other methods Inverted L osteotomy and C osteotomy are less preferred techniques


Excessive face height : open bite Deficient face height : deep bite Maxilla can be moved up quite successfully but can be positioned downward with less predictability. Mandible can be moved up or down anteriorly but cannot be moved down at the gonial angle with stability.
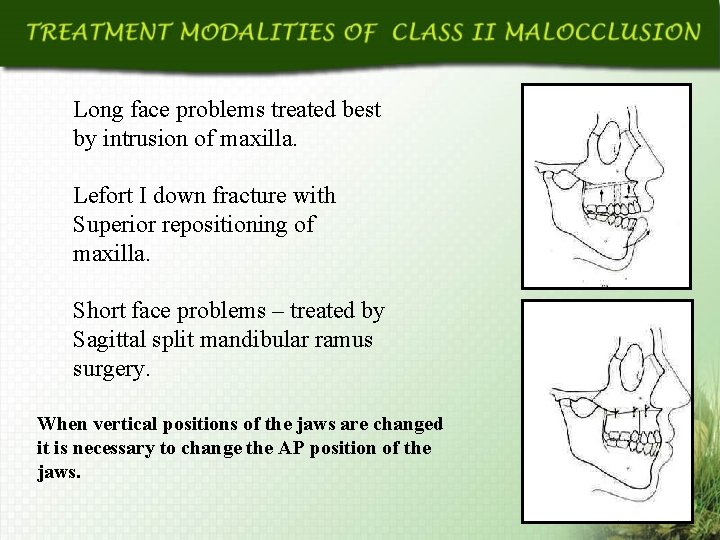
Long face problems treated best by intrusion of maxilla. Lefort I down fracture with Superior repositioning of maxilla. Short face problems – treated by Sagittal split mandibular ramus surgery. When vertical positions of the jaws are changed it is necessary to change the AP position of the jaws.

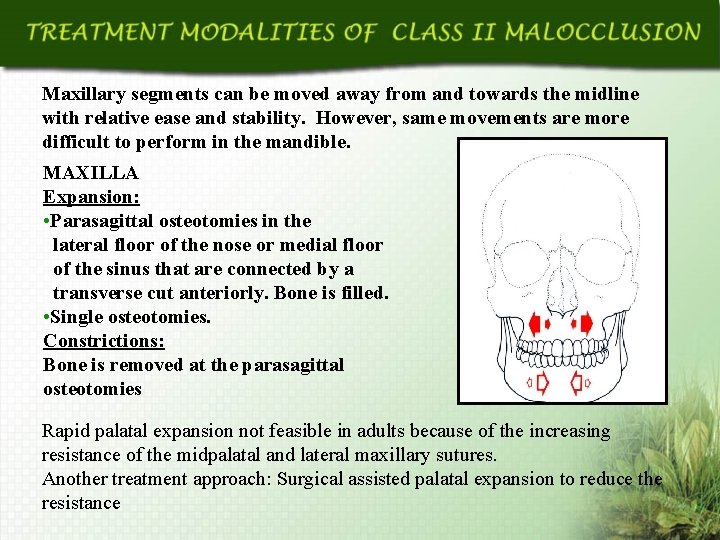
Maxillary segments can be moved away from and towards the midline with relative ease and stability. However, same movements are more difficult to perform in the mandible. MAXILLA Expansion: • Parasagittal osteotomies in the lateral floor of the nose or medial floor of the sinus that are connected by a transverse cut anteriorly. Bone is filled. • Single osteotomies. Constrictions: Bone is removed at the parasagittal osteotomies Rapid palatal expansion not feasible in adults because of the increasing resistance of the midpalatal and lateral maxillary sutures. Another treatment approach: Surgical assisted palatal expansion to reduce the resistance

TIMING OF TREATMENT In patients with excessive growth especially mandibular prognathism, orthognathic surgery should be delayed until growth is completed. In patients with growth deficiency surgery can be considered earlier.

COMBINED SURGICAL APPROACHES Not uncommon to require a combination of maxillary and mandibular surgeries to adequately address the malocclusion. Cases with significant maxillary deformity with mandibular deficiency

CONCLUSION

- Slides: 61