Treatment Guidelines for Preoperative Radiation Therapy for Retroperitoneal

















- Slides: 27

Treatment Guidelines for Pre-operative Radiation Therapy for Retroperitoneal Sarcoma: Preliminary Consensus of an International Expert Panel EH Baldini, D Wang, CN Catton, DJ Indelicato, DG Kirsch, C Deville, C Le Pechoux, R Haas, IA Petersen, K May, D Roberge, BA Guadagnolo, B O'Sullivan, R Abrams, TF De. Laney

None of the authors have disclosures

Background • The role of RT for extremity soft tissue sarcoma is well established • However, the role of RT for retroperitoneal sarcoma (RPS) is unproven

EORTC 62092 -22092 (STRASS Trial) RPS: Randomize Pre-Op RT Surgery Ongoing, results are eagerly anticipated

Background • In the meantime, many centers recommend Pre-op RT for RPS after multidisciplinary discussion • But, there are no RT guidelines for this approach

Purpose • To define radiation treatment guidelines for Pre-operative RT for RPS

RT Treatment Nomenclature • GTV: Gross Tumor Volume • CTV: Clinical Target Volume – Expansion of GTV to include areas at risk for harboring potential microscopic disease • PTV: Planning Target Volume – Expansion of CTV to account for daily patient set-up inaccuracies and/or patient movement • Treatment Field Borders – Extend beyond the PTV by about 7 mm to deliver full dose to PTV

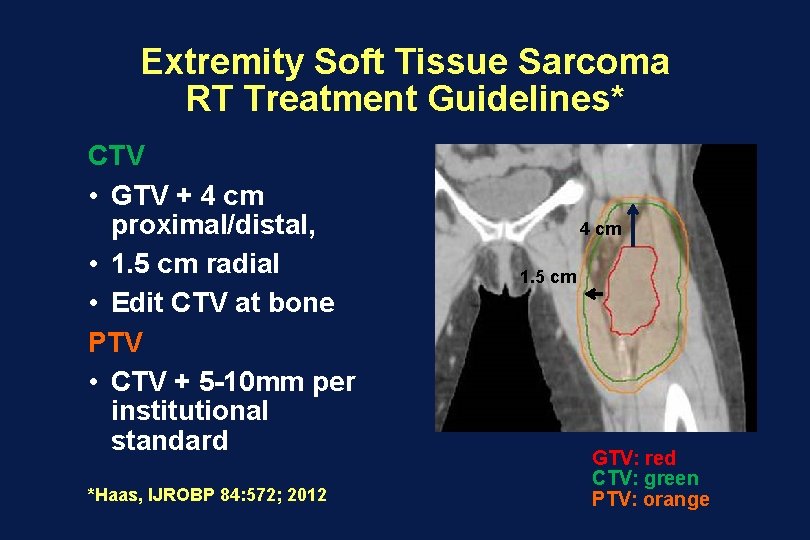
Extremity Soft Tissue Sarcoma RT Treatment Guidelines* CTV • GTV + 4 cm proximal/distal, • 1. 5 cm radial • Edit CTV at bone PTV • CTV + 5 -10 mm per institutional standard *Haas, IJROBP 84: 572; 2012 4 cm 1. 5 cm GTV: red CTV: green PTV: orange

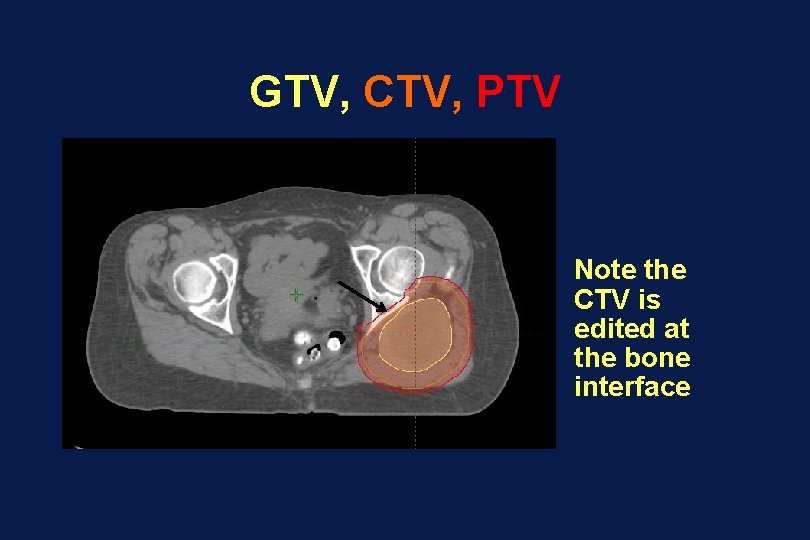
GTV, CTV, PTV Note the CTV is edited at the bone interface

GTV CTV Expansions Vary by Tumor Lymphoma Prostate Cancer Lung Cancer GTV CTV Expansion 0 mm 5 -7 mm Glioblastoma Multiforme 2 cm beyond edema Extremity STS 1. 5 cm radial 4 cm proximal/distal ? Retroperitoneal Sarcoma

Methods • An expert panel of 15 academic radiation oncologists who specialize in sarcoma was convened • Panel members reached consensus recommendations following several meetings, conference calls and email correspondence

Expert Panel: US Institutions (10) • • • Dana-Farber/Brigham & Women’s Hospital Massachusetts General Hospital Medical College of Wisconsin University of Florida, Jacksonville Duke University of Pennsylvania Mayo Clinic Roswell Park Cancer Institute MD Anderson Cancer Center Rush University

Expert Panel: European and Canadian Institutions (4) Canada – Princess Margaret Cancer Centre – Mc. Gill University Health Centre France – Institut Gustave Roussy Netherlands – Netherlands Cancer Institute

Results Consensus Recommendations

Essential Collaboration between Surgeon + Radiation Oncologist Discuss resection margins of concern Discuss potential resection of kidney, liver – If nephrectomy is planned: » Adequate contra-lateral renal function should be documented » Minimize dose to contra-lateral kidney – If partial liver resection is planned: » Minimize dose to remaining liver

Radiation Simulation • Oral and IV contrast is optional • Assessment of 4 D motion (4 D CT) – Strongly recommended for tumors above iliac crest to define GTV 4 D • Contour GTV on the planning CT – Register planning CT with diagnostic CT or MR T 1 contrast images if necessary

CTV Definition Expand GTV symmetrically by 1. 5 cm Edit CTV: • • • Bone: 0 mm Bowel and Air Cavity: 5 mm Renal and Hepatic interfaces: 2 mm Skin Surface: 3 -5 mm If tumor extends through inguinal canal, add 3 cm distally (as per extremity STS) • If 4 D CT is not performed, larger expansions are necessary for upper abdominal tumors

PTV Definition • Expand CTV by 5 mm – If frequent volumetric soft tissue imaging will be performed to confirm set-up accuracy (i. e. cone beam CT) • Expand CTV by 9 -12 mm – If no volumetric imaging is performed to confirm set-up

Dose 5040 c. Gy 180 c. Gy fractions 5 ½ weeks

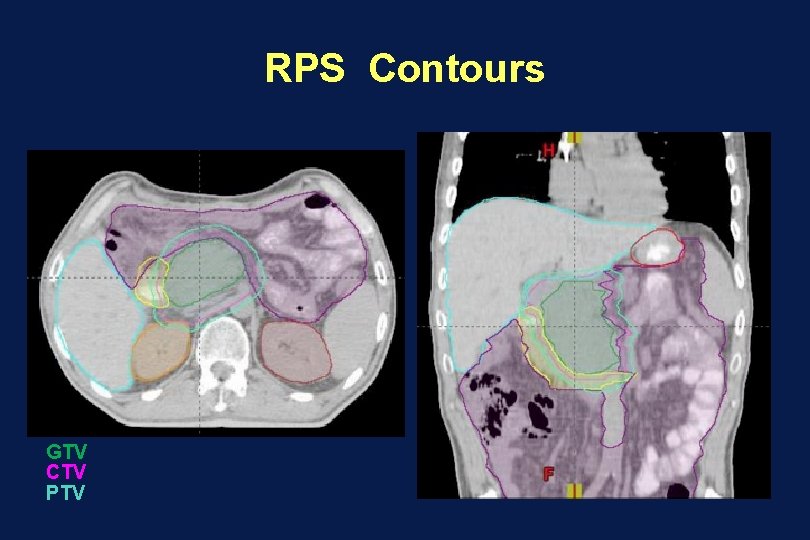
RPS Contours GTV CTV PTV

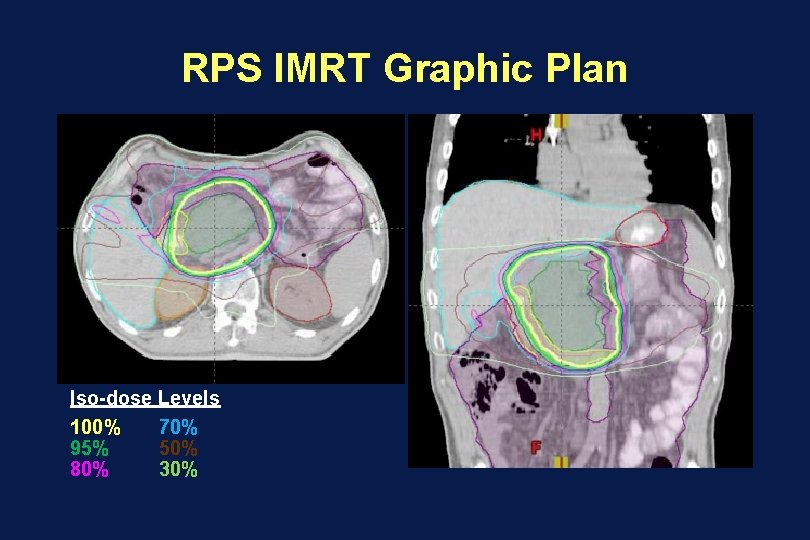
RPS IMRT Graphic Plan Iso-dose Levels 100% 70% 95% 50% 80% 30%

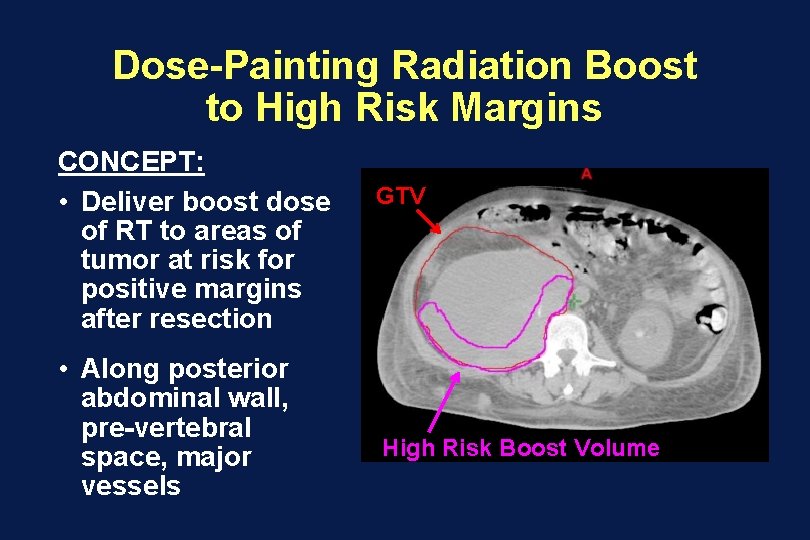
Dose-Painting Radiation Boost to High Risk Margins CONCEPT: • Deliver boost dose of RT to areas of tumor at risk for positive margins after resection • Along posterior abdominal wall, pre-vertebral space, major vessels GTV High Risk Boost Volume

Dose-Painting Radiation Boost to High Risk Margins • Efficacy is unproven • Technique is under investigation • May be considered, particularly on protocol – De. Laney Phase I/II Multi-Center Dose. Painting Boost, Dose-Escalation Trial

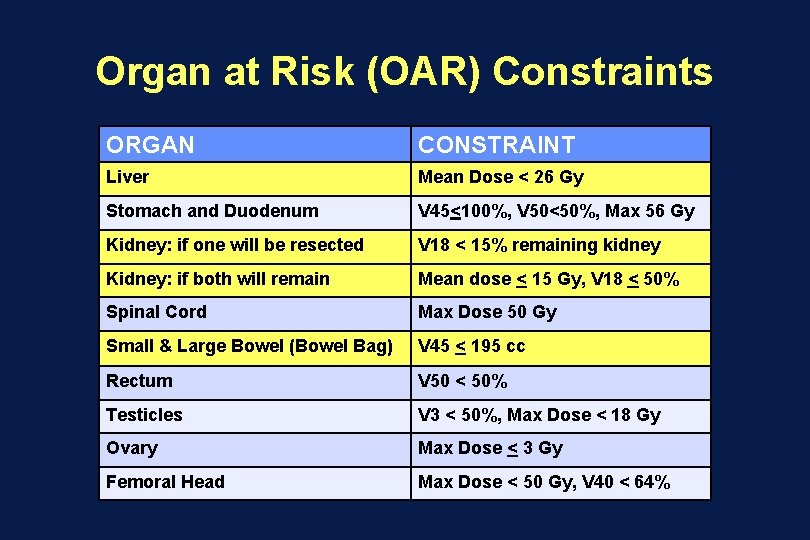
Organ at Risk (OAR) Constraints ORGAN CONSTRAINT Liver Mean Dose < 26 Gy Stomach and Duodenum V 45<100%, V 50<50%, Max 56 Gy Kidney: if one will be resected V 18 < 15% remaining kidney Kidney: if both will remain Mean dose < 15 Gy, V 18 < 50% Spinal Cord Max Dose 50 Gy Small & Large Bowel (Bowel Bag) V 45 < 195 cc Rectum V 50 < 50% Testicles V 3 < 50%, Max Dose < 18 Gy Ovary Max Dose < 3 Gy Femoral Head Max Dose < 50 Gy, V 40 < 64%

Treatment Technique • Intensity modulated radiation therapy (IMRT) preferred unless OAR constraints can be met with 3 D-conformal technique

Conclusion • Consensus guidelines were achieved and are recommended for use –To establish uniformity of treatment –Aid future efficacy and toxicity assessment

Thank You • • Tom De. Laney Dian Wang Charles Catton Danny Indelicato David Kirsch Curt Deville Cecile Le Pechoux • • Rick Haas Ivy Petersen Kilian May David Roberge Ashleigh Guadagnolo Brian O’Sullivan Ross Abrams