Treating Life Threatening Asthma Toni PetrilloAlbarano MD Division

Treating Life Threatening Asthma Toni Petrillo-Albarano, MD Division of Pediatric Critical Care Children’s Healthcare of Atlanta
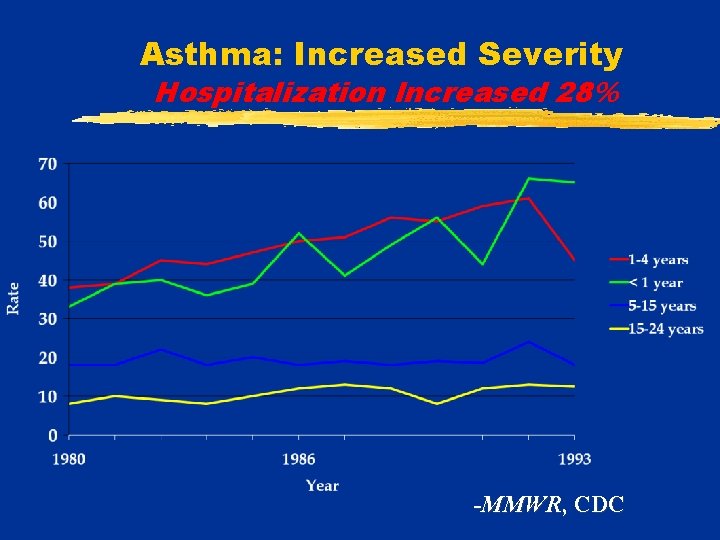
Asthma: Increased Severity Hospitalization Increased 28% -MMWR, CDC
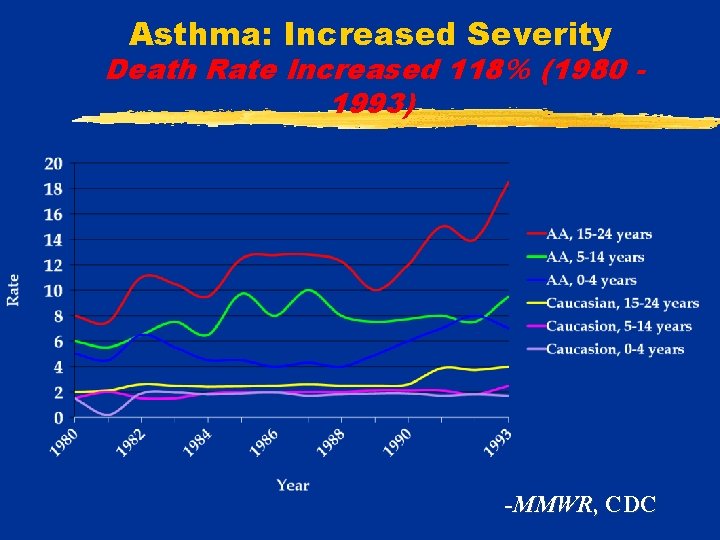
Asthma: Increased Severity Death Rate Increased 118% (1980 1993) -MMWR, CDC

The Cost of Asthma related costs v $6. 2 billion v Direct 3. 6 billion v Indirect $2. 6 billion v Pediatric $465 million

Children Who Die from Asthma v. Risk Factors: § Severe disease - history of intubation, seizures, rapid progress § Lack of adequate support systems § Psychologic disease

Children Who Die from Asthma v. Risk Factors: § Lack of perception of severity; selfweaning § Males § Exclusive reliance on b agonists v 50% of deaths prior to hospital
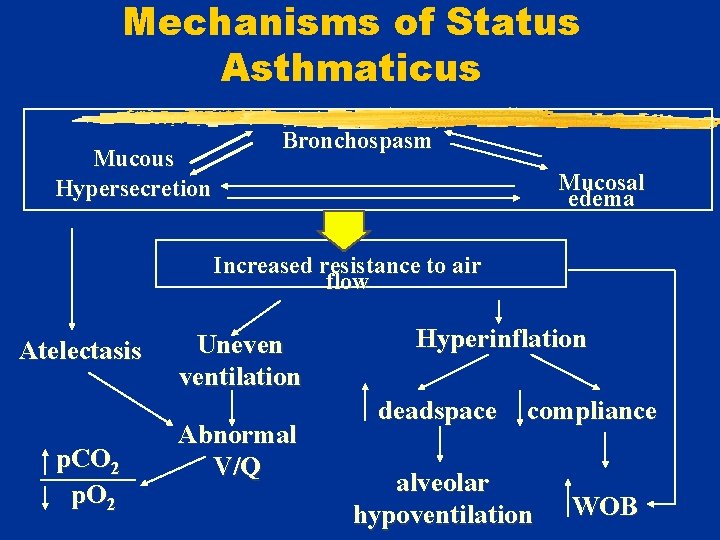
Mechanisms of Status Asthmaticus Mucous Hypersecretion Bronchospasm Mucosal edema Increased resistance to air flow Atelectasis p. CO 2 p. O 2 Uneven ventilation Abnormal V/Q Hyperinflation deadspace compliance alveolar hypoventilation WOB

Status Asthmaticus Oxygen v. Relative hypoxemia: § V/Q mismatch § hypoventilation v. Hypoxemia bronchoconstriction § agonists impair hypoxic pulmonary vasoconstriction shunt v. Oxygen to keep pulse ox > 92%

Status Asthmaticus Beta 2 Agonist Therapy v. Mainstay of therapy v. Rapid onset v. Selective 2: § Metaproterenol § Terbutaline § Albuterol v. Mode of delivery: § Inhaled vs Systemic § Intermittent vs Continuous § Nonintubated vs Intubated

Intravenous Agonists v. Most studies: § inhaled therapy > to IV agonist v. Greater side effects with IV v. Potential benefit severe bronchospasm v. Experience anecdotal with severe SA v. IV Terbutaline: § bolus 10 mcq/kg § infusion 0. 1 -4. 0 mcq/kg/min

Status Asthmaticus Isoproterenol (Isuprel) v. Almost pure effects v. Potent vasodilator § pulmonary § bronchial v. Increased cardiac output v. Widened pulse pressure v. Increases flow to non-critical tissue beds (skeletal muscle)

Status Asthmaticus Isoproterenol (Isuprel) v. Tachycardia v. Dysrhythmias v. Peripheral vasodilation v. Increased myocardial O 2 consumption v. Decreased coronary O 2 delivery v“Splanchnic steal” by skeletal muscle

Severe Asthma Intravenous Isoproterenol v. Equivocal results vhigh incidence of dysrhythmias v report of fatal myocardial ischemia v“DO not use IV Isuprel in the treatment of asthma. . . ” -NHLBI statement

Status Asthmaticus Subcutaneous Agonists v. Epinephrine/Terbutaline v. No advantage over inhaled agonists v. Increased side effects v. Indications: § inability to cooperate with inhalation therapy § rapidly decompensating patient § failure to respond to inhaled beta-agonists
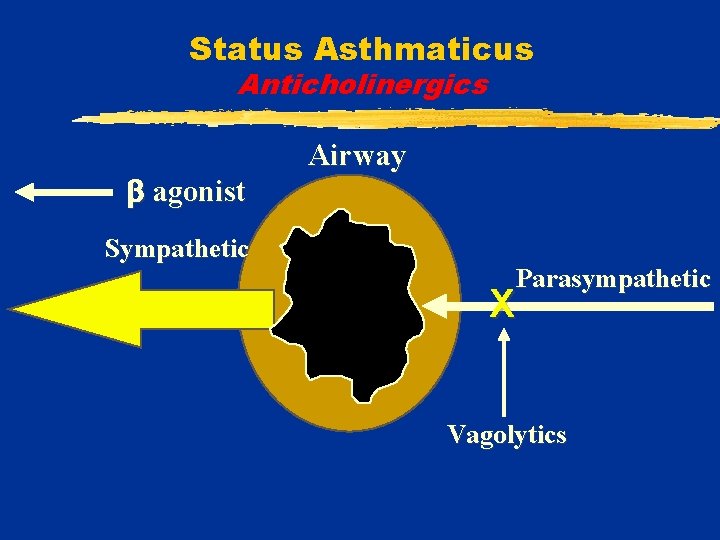
Status Asthmaticus Anticholinergics agonist Sympathetic Airway Parasympathetic X Vagolytics

Status Asthmaticus Inhaled Ipratropium + Albuterol v 120 children - severe acute asthma: § FEV 1 < 50% v. Albuterol (0. 15 mg/kg) x 3 within 60 minutes PLUS v. Randomized: § control saline § ipratropium 250 mcq x 1 § ipratropium 250 mcg x 3 -Schuh, J Peds, 1995
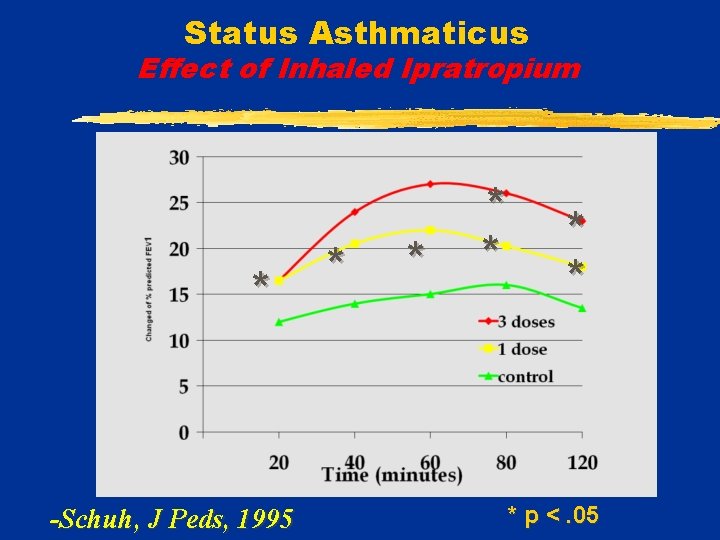
Status Asthmaticus Effect of Inhaled Ipratropium * -Schuh, J Peds, 1995 * * * * p <. 05
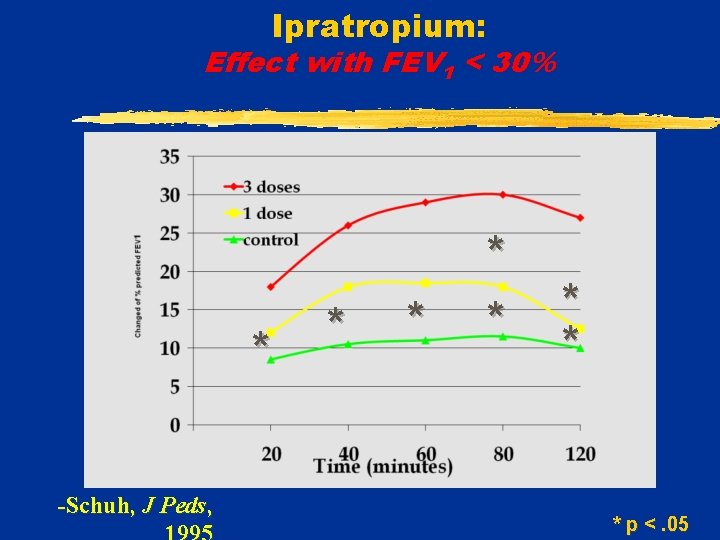
Ipratropium: Effect with FEV 1 < 30% * -Schuh, J Peds, * * * * p <. 05

Status Asthmaticus IV or oral Corticosteroids Mechanism of Effect: vinterferes with leukotriene, prostaglandins synthesis vprevent cell migration vup-regulate airway receptors

Status Asthmaticus IV or oral Corticosteroids v. Proven effective in 3 level I trials, metaanalysis v. Decreased hospital admission if given within 30 minutes v. Equally effective oral or IV v. IV dose effect in 1 -6 hours by reversing 2 receptor down-regulation

Status Asthmaticus IV or oral Corticosteroids v. Recommended dose § Prednisone or methylprednisolone § suggested initial dose 2 mg/kg § 1 mg/kg IV q 6 hours (max 60 mg) x 48 hours, § then 1 mg/kg q 12 hours for 3 -5 days -NHLBI Expert Panel

Status Asthmaticus Inhaled Corticosteroids v. SI asthma has several characteristic features § § severe asthma with persistent respiratory symptoms frequent nighttime symptoms chronic airflow obstruction (FEV 1 <70% of predicted) tend to have required systemic GC therapy at a younger age § require higher daily maintenance doses of oral GCs § are often African American.

Status Asthmaticus Inhaled Corticosteroids Acute Asthma v. ICS have been considered ineffective in treatment of acute exacerbations v. Nevertheless, many studies published in the last 15 years have showed therapeutic early effects (after minutes of its administration) suggesting a different mechanism of action of topical character

Status Asthmaticus Inhaled Corticosteroids Acute Asthma v. These rapid effects are initiated by specific interactions with membrane-bound or cytoplasmic CS receptors, or nonspecific interactions with the cell membrane vasthmatic patients present a significant increase in airway mucosal blood flow

Status Asthmaticus Inhaled Corticosteroids Acute Asthma v. ICS would decrease blood flow by modulating sympathetic control of vascular tone § This nongenomic action might reduce the airway obstruction, improving clinical and spirometric parameters v. Furthermore, the decrease of airway blood flow is likely to enhance the action of inhaled bronchodilators by diminishing their clearance from the airway

Status Asthmaticus Long term inhaled corticosteroid v. Most studies done on moderate to severe persistent asthma (beneficial) v. Data on mild or moderate and intermittent not well studied v. Studies by O‘Byrne et al and Lange et al reinforce current practice of preventing asthma events with the regular use of ICS in patients who have symptoms on most days

Status Asthmaticus IV Theophylline v. Phosphodiesterase inhibitor v. Randomized trials (x 2) - no benefit over standard 2 agonists and/or corticosteroids v. Uncertain benefit in episodes unresponsive to all otherapy

Status Asthmaticus IV Theophylline v 21 hospitalized children v. Standard nebulized albuterol, steroids v. Randomized: IV Aminophylline load/infusion OR Saline placebo -Carter, J Peds, 1993
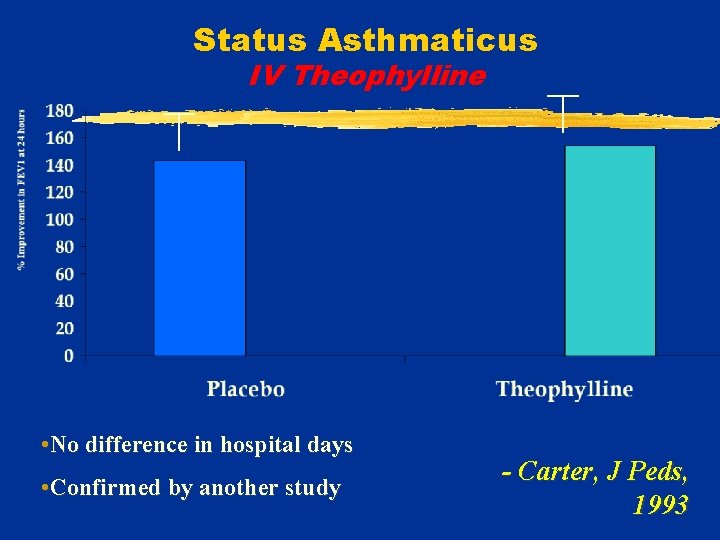
Status Asthmaticus IV Theophylline • No difference in hospital days • Confirmed by another study - Carter, J Peds, 1993
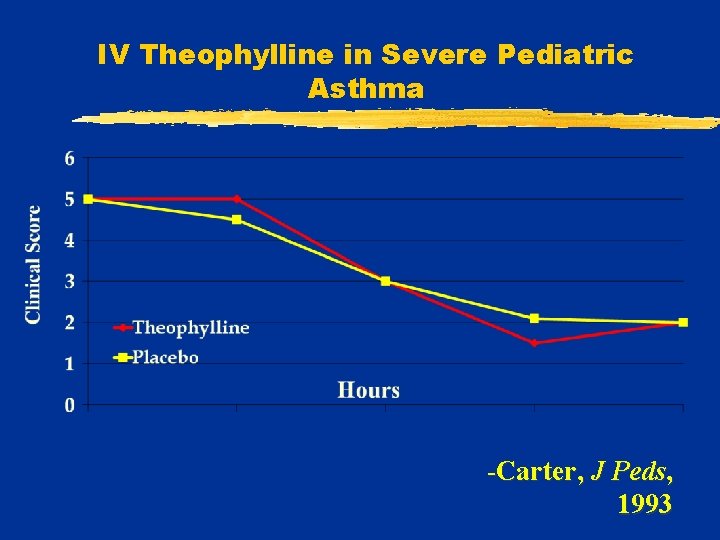
IV Theophylline in Severe Pediatric Asthma -Carter, J Peds, 1993

“Methylxanthines are NOT generally recommended. ” -Expert Panel, NAEPP

Status Asthmaticus Ketamine v. Dissociative anesthetic v. Direct bronchodilator v. Potentiates catecholamines v. Bronchorrhea v. Other side effects: § tachycardia § BP

Status Asthmaticus Ketamine v. Adult studies v. Case reports: § benefit in avoiding intubation v. Randomized trials: § no added benefit § required lower dose due to dysphoria v. Children might respond better, less dysphoria

Status Asthmaticus Ketamine in Pediatrics v 8 case reports: § 12 patients - not controlled v 8 months - 14 years v. Positive affect in all v 9/12 intubated v. Bolus/Infusion 0. 2 - 2. 5 mg/kg/hr

Status Asthmaticus Ketamine in Pediatrics v. One small pediatric study in non-intubated patients § 10 patients § ketamine bolus plus 1 hr infusion in addition to standard therapy § Improved CAS § improved indicators of distress

Status Asthmaticus Magnesium Sulfate v. Bronchodilator: § inhibits cellular Ca++ uptake/release § stabilizes most cell membranes v. Clinical effect: § 10/13 studies showed improved PEFR in adults, children v 2 adult studies no outcome benefit

Status Asthmaticus Magnesium Sulfate v 31 children (6 -18 yrs) in ER v. Asthma exacerbation: § PEFR < 60% after albuterol v. Randomized: Mg. SO 4 25 mg/kg OR Saline -Ciarallo, J Peds, 1996
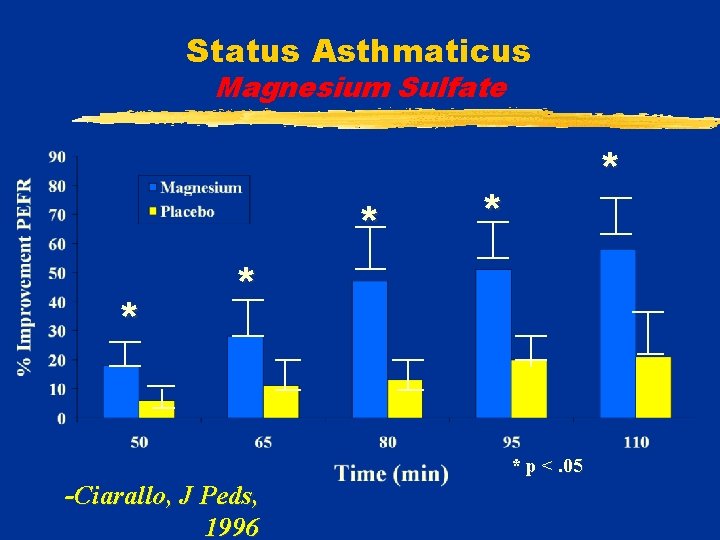
Status Asthmaticus Magnesium Sulfate * * * p <. 05 -Ciarallo, J Peds, 1996
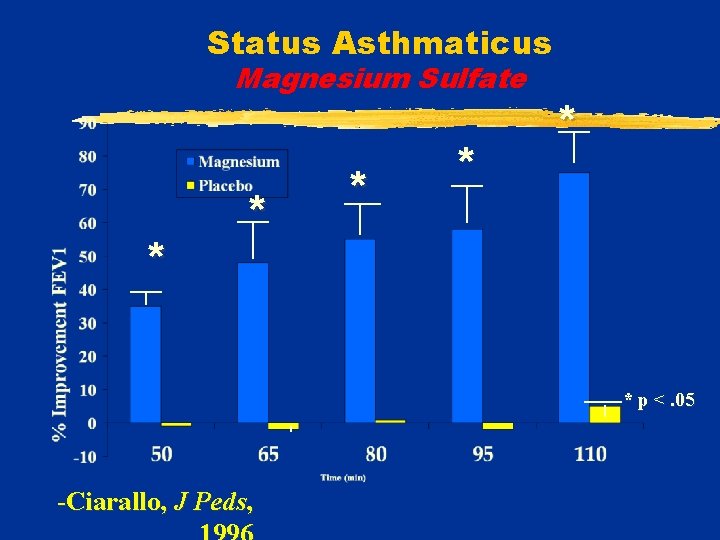
Status Asthmaticus Magnesium Sulfate * * * p <. 05 -Ciarallo, J Peds,

Status Asthmaticus Magnesium Sulfate Results: v. ER discharge home: § 27% vs 0% control (p =. 03) v. No difference in hospital stay v. No significant side effects -Ciarallo, J Peds, 1996

Status Asthmaticus Leukotriene Antagonist v. Mostly used as controller med v. Some newer small studies to suggest possible benefit in acute setting § Rapid improvement in FEv 1 with single IV monoleukast dose (Thorax 2000; 55: 260 -5) § 160 mg Po Zafirlukast improved ER outcomes ( Ann Emerg Med 2000; 35: S 10

Status Asthmaticus Helium - Oxygen (HELIOX) v Blend of 80: 20 helium: oxygen v Biologically inert v Insoluble in human tissue v No deleterious effects v Low density gas § Air: 1. 29 g/l § O 2: 1. 43 g/l § Helium: 0. 17 g/l

Status Asthmaticus Helium - Oxygen (HELIOX) v Major effects to reduce resistance: § Reduces turbulence v. Used in upper airway obstruction v. Improved pulsus paradoxus, PEFR in adult asthmatics

Status Asthmaticus Helium - Oxygen (HELIOX) v. Most recent case reports and clinical studies have found mixed results in the role of heliox for use in asthma

Status Asthmaticus Helium - Oxygen (HELIOX) v Kudukis et al showed that heliox therapy resulted in a significant decrease in pulsus paradoxus, a decrease in a modified dyspnea index, and an increase in peak flow v Manthous et al reported similar findings in dyspnea index and pulsus paradoxus accompanied by an increase in peak expiratory flow. v Rivera et al the heliox group had a lower admission rate compared with the placebo group (60% vs 81%). v Other studies have shown a decrease in carbon dioxide, reversal of acidosis, and an increase in peak expiratory flow rate

Status Asthmaticus Helium - Oxygen (HELIOX) v. Carter et al found that short-term inhalation of heliox offered no benefit in hospitalized children with severe asthma. v. Henderson et al found that 3 treatments of albuterol nebulized in heliox over 45 minutes offered no additional benefit in the ED management of mild to moderate asthma exacerbations v. Rose et al found that heliox-driven continuous albuterol in the ED management no difference in peak expiratory flow rate, respiratory rate, or oxygen saturation

Status Asthmaticus Inhaled Anesthetics v. Halothane, enflurane, isoflurane v. Mechanisms: § 2 agonist effect § vagolytic § direct airway relaxation v. No randomized (level I) trials

Status Asthmaticus Inhaled Anesthetics v 8 pediatric case reports: § effect in 7/8 § isoflurane 5/8 v. Duration 1 -34 hrs; § Time interval for changes: 1 -2 hrs v. Complications: § hypotension, § pneumothorax
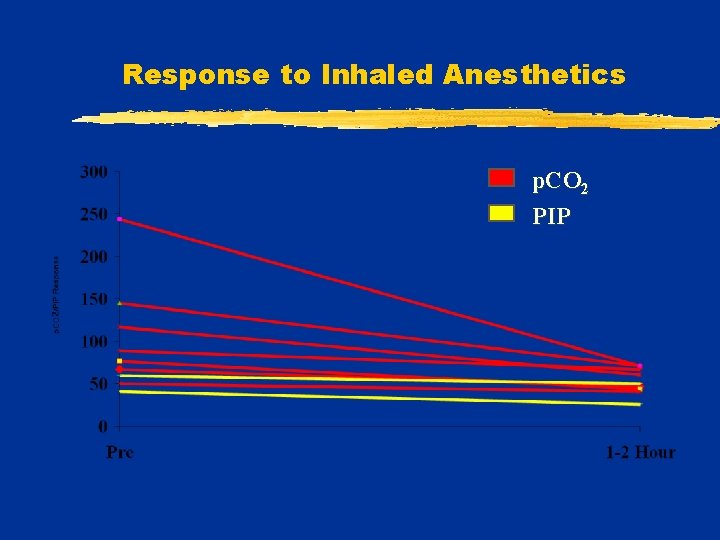
Response to Inhaled Anesthetics p. CO 2 PIP

Status Asthmaticus “Mechanical” Support v. Bi. PAP v. Intubation/Mechanical Ventilation v. Extracorporeal Life Support

Status Asthmaticus Non invasive Ventilation v. Positive-pressure by nasal mask (Bi. PAP) v. Potential benefits: § airway stenting § improve V/Q match v. CPAP improved hypoxemia in 8 asthmatic children

Status Asthmaticus Non invasive Ventilation v 26 children (+ 7. 2 years) in PICU v 19/26 managed without intubation: RR, HR, Sa. O 2 v 7/26 intubated v 11/26 Bi. PAP held v. Efficacy remains uncertain -Teague, Lang, et al, ATS, 1998

Status Asthmaticus Non invasive Ventilation v. Beers et al immediate improvement in subjects' clinical status upon initiation of Bi. PAP, with 77% showing a decrease in respiratory rate, averaging 23. 6% (range, 4%-50%), and 88% showing an improved oxygen saturation, averaging 6. 6 percentage points (1 -28 percentage points). There were no adverse events due to the use of Bi. PAP.

Status Asthmaticus Nitric Oxide v. Smith et al showed that FENO measurements provide a useful guide about whether benefits will be obtained from a trial of ICS treatment. vthe response to inhaled fluticasone for 4 weeks was significantly greater than placebo and occurred predominantly in the ⅓ of subjects whose FENO was greater than 47 ppb v. In the absence of high FENO levels, a response to steroid was much less likely

Status Asthmaticus Nitric Oxide v. Exhaled nitric oxide (FENO) surrogate marker for eosinophilic airway inflammation. v. FENO may be used to guide steroid requirements v. High FENO levels may be used to predict likely benefits with inhaled corticosteroid (ICS) vrepeated FENO measurements improve the costeffectiveness of ICS therapy when used to guide dose requirements

Status Asthmaticus Intubation v. Usually last resort v. Potential M&M v. Mortality rate § in adults 0 - 40% § in children 0 - 5% v 24 -33% of PICU admissions required mechanical ventilation (very high? )

Status Asthmaticus Intubation v. Wear Depends ! v. Intubation by MD with experience v. Have volume ready: hypotension due to ed intrathoracic pressure

Status Asthmaticus Intubation v. Best done semi-electively § earlier rather than later v. Drugs of choice: § Atropine § Ketamine/Midazolam § Succinylcholine

Status Asthmaticus Mechanical Ventilation v. GOALS: § Rest inspiratory muscles § Protect airway § Provide adequate gas exchange NOT normal exchange § Avoid barotrauma, catastrophe

Status Asthmaticus Mechanical Ventilation Indications Coma Absolute: Respiratory or cardiac arrest Relative: Cyanosis and hypoxemia on O 2 Pa. CO 2 greater than 50 and rising > 5 mm. Hg/hr Deteriorating mental status Minimal chest movement/air exchange Pneumothorax

Status Asthmaticus Mechanical Ventilation v. Key approach: permissive hypercapnia (“controlled hypoventilation”) vtolerate p. CO 2 to keep p. H > 7. 20 - 7. 25 vprolonged expiratory time v rate, inspiratory time v tidal volume v PEEP: auto-PEEP

Status Asthmaticus Extracorporeal Membrane Oxygenation v. Veno-venous bypass for life support in asthma unresponsive to all otherapy v. Membrane lung extremely efficient at CO 2 clearance, low-flow v. Allows for bronchoscopy

Status Asthmaticus Extracorporeal Membrane Oxygenation v 60 pediatric patients vp. CO 2 at cannulation: 37 -284 mm. Hg v. Maximal therapy v 83% survival v 7 here who all survived without sequelae

Therapies NOT Recommended v. Antibiotics v. Empiric, aggressive hydration v. Chest PT v. Mucolytics v. Sedation? ?

Evidence-Based Guidelines: Report Card A A: GOOD evidence to recommend for USE of treatment B B: FAIR evidence to recommend for USE C C: POOR evidence to support recommendation, but USE recommended on other grounds D D : FAIR evidence to recommend EXCLUSION FF : GOOD evidence to recommend EXCLUSION -CMAJ, 1993

Report Card: Status Asthmaticus Therapy Oxygen Agonists Inhaled IV Ipratropium Corticosteroids Methylxanthines C A+ B A A D

Report Card: Status Asthmaticus Therapy Magnesium Ketamine HELIOX Inhaled Anesthesia Bi. PAP B+ C BC+ C+

Questions? ?
- Slides: 68