TRAUMATIC THORACOLUMBAR SPINE INJURIES ON CT ELIZABETH DU

TRAUMATIC THORACOLUMBAR SPINE INJURIES ON CT ELIZABETH DU, MD & ROBERT VANDORPE, MD 54 TH ANNUAL ATLANTIC RADIOLOGY CONFERENCE OCTOBER 4 -6, 2019

LEARNING OBJECTIVES • Recognize the role of bone and soft tissue integrity in determining spine stability • Describe the use of the Thoracolumbar Injury Classification and Severity Score in evaluating traumatic spine injury on imaging • Discuss CT characteristics of each of the four patterns of injury morphology on CT • Discuss CT findings predicting posterior ligamentous complex integrity on CT

SPINE STABILITY • Ability of the spine to • Prevent neurologic injury and progressive deformity • Accommodate physiologic loading and normal range of movement • Road traffic accidents = the majority of traumas leading to spinal trauma/instability
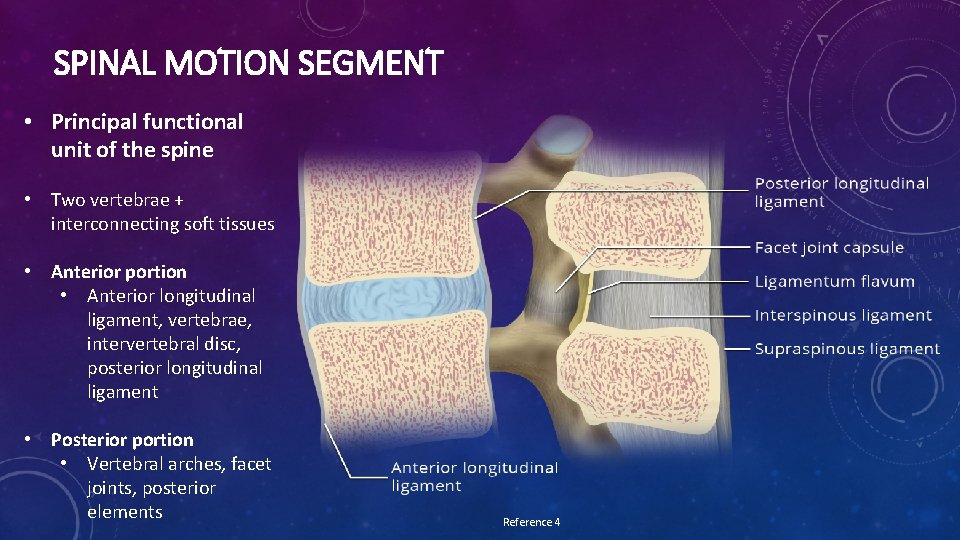
SPINAL MOTION SEGMENT • Principal functional unit of the spine • Two vertebrae + interconnecting soft tissues • Anterior portion • Anterior longitudinal ligament, vertebrae, intervertebral disc, posterior longitudinal ligament • Posterior portion • Vertebral arches, facet joints, posterior elements Reference 4

POSTERIOR PORTION ANTERIOR PORTION • Guides spinal movement • Axial loading • Vertebral bodies • Resist compressive loading • Nucleus pulposus + annulus fibrosus • Absorb & hydrostatically distribute compressive loading Reference 2 • Posterior ligamentous complex (PLC) • Supraspinous ligament • Strong, cordlike, high collagen, C 7 -S • Interspinous ligament • Weak, thin, high collagen • Ligamentum flavum • Thick, broad, high elastin • Articular facets • Resist rotational & torsional forces Ligamentum • Fulcrum during flavum extension
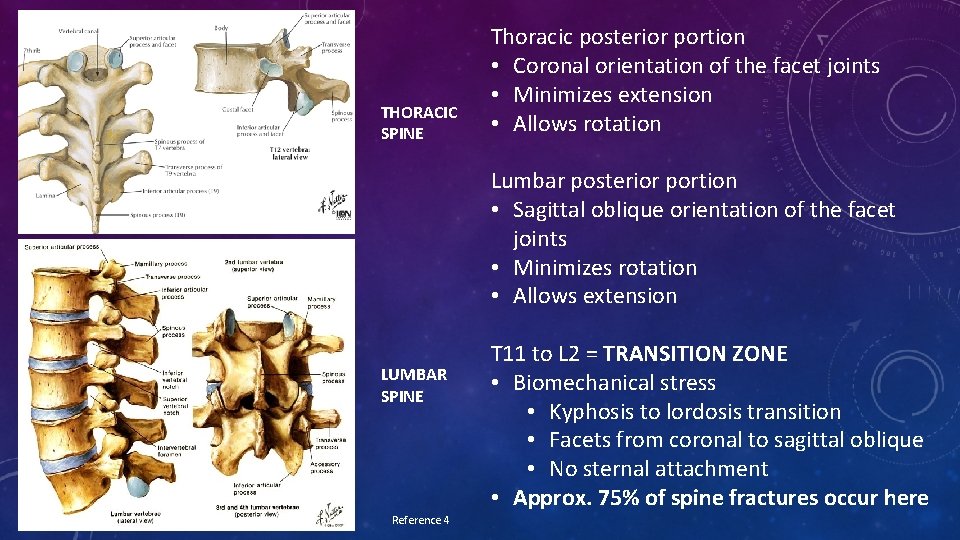
THORACIC SPINE Thoracic posterior portion • Coronal orientation of the facet joints • Minimizes extension • Allows rotation Lumbar posterior portion • Sagittal oblique orientation of the facet joints • Minimizes rotation • Allows extension LUMBAR SPINE Reference 4 T 11 to L 2 = TRANSITION ZONE • Biomechanical stress • Kyphosis to lordosis transition • Facets from coronal to sagittal oblique • No sternal attachment • Approx. 75% of spine fractures occur here

WHITESIDE’S CRANE ANALOGUE Think of the spine as a crane: Anteriorly displaced center of gravity Compressive force on the crane lifting arm i. e. vertebrae Equilibrium/counter tension provided by the crane’s lifting cable i. e. spine’s posterior ligamentous complex (PLC) http: //clinicalgate. com/trauma-surgery-thoracic-and-thoracolumbar-junction/

DENIS 3 -COLUMN CLASSIFICATION SYSTEM FOR INJURIES Reference 4 Older classification system Classified according to morphology/mechanism • Compression fracture • Burst fracture • Seat-belt injury • Fracture-dislocation Is there involvement of the middle column? • Spine mechanically unstable with middle column injury • Confusing concept of fractures involving 2 columns as “unstable” Issues • No prognostic information • Does not consider patient’s neurologic status
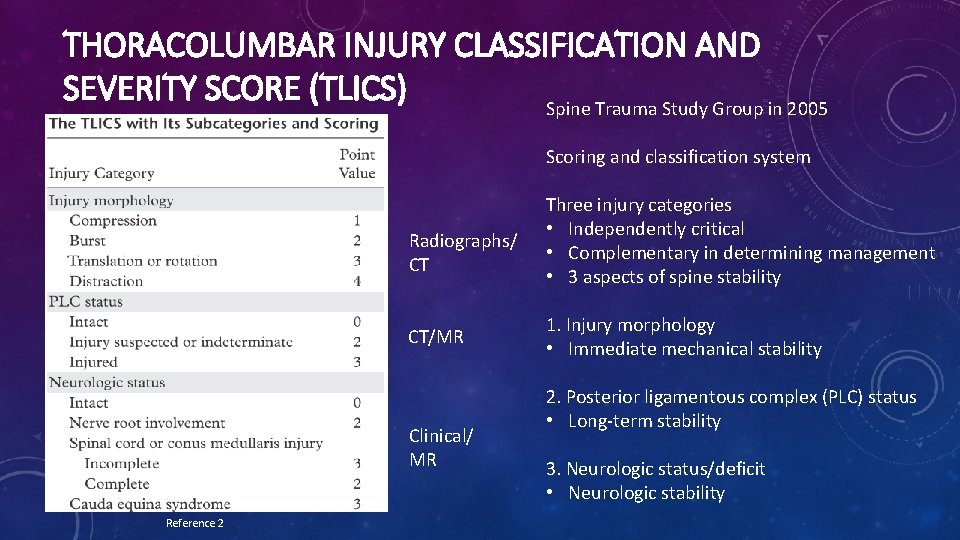
THORACOLUMBAR INJURY CLASSIFICATION AND SEVERITY SCORE (TLICS) Spine Trauma Study Group in 2005 Scoring and classification system Radiographs/ CT CT/MR Clinical/ MR Reference 2 Three injury categories • Independently critical • Complementary in determining management • 3 aspects of spine stability 1. Injury morphology • Immediate mechanical stability 2. Posterior ligamentous complex (PLC) status • Long-term stability 3. Neurologic status/deficit • Neurologic stability
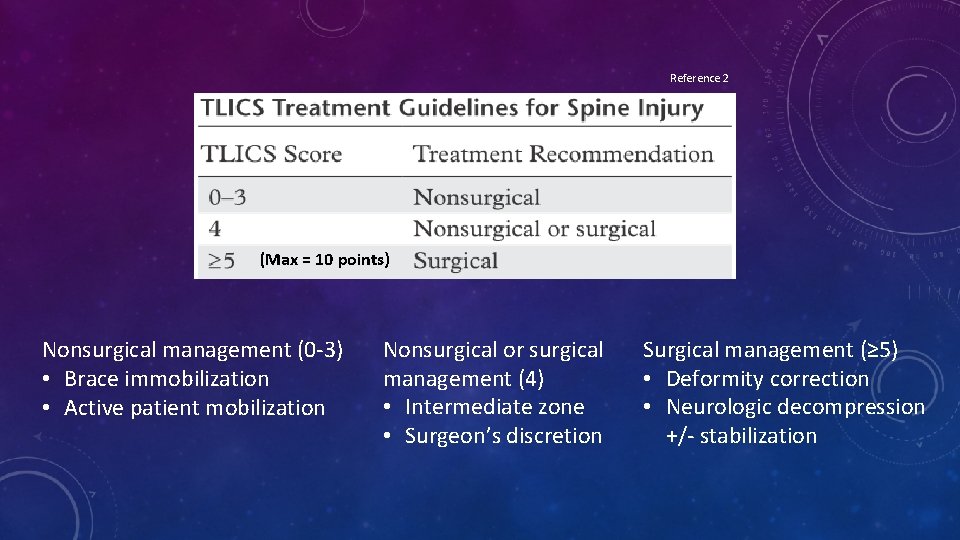

Reference 2 (Max = 10 points) Nonsurgical management (0 -3) • Brace immobilization • Active patient mobilization Nonsurgical or surgical management (4) • Intermediate zone • Surgeon’s discretion Surgical management (≥ 5) • Deformity correction • Neurologic decompression +/- stabilization
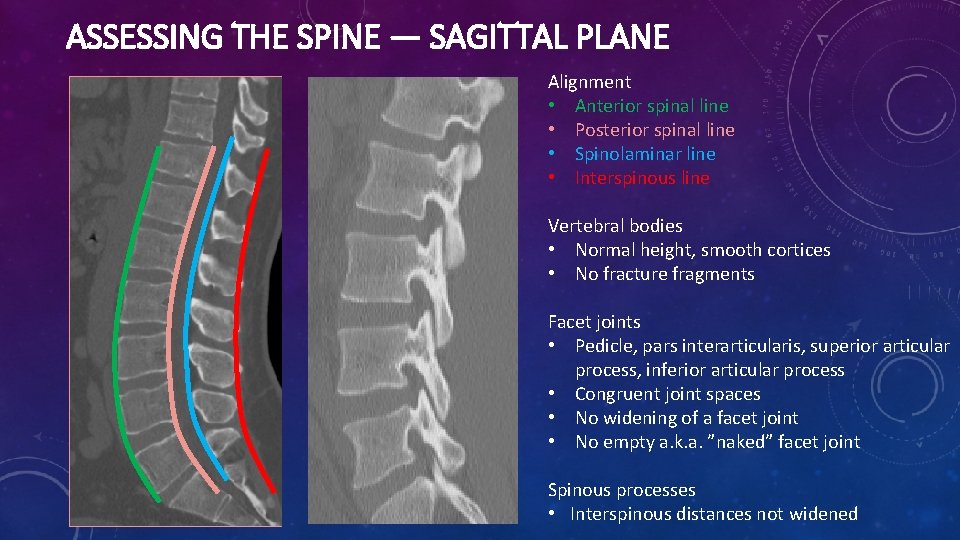
ASSESSING THE SPINE — SAGITTAL PLANE Alignment • Anterior spinal line • Posterior spinal line • Spinolaminar line • Interspinous line Vertebral bodies • Normal height, smooth cortices • No fracture fragments Facet joints • Pedicle, pars interarticularis, superior articular process, inferior articular process • Congruent joint spaces • No widening of a facet joint • No empty a. k. a. ”naked” facet joint Spinous processes • Interspinous distances not widened
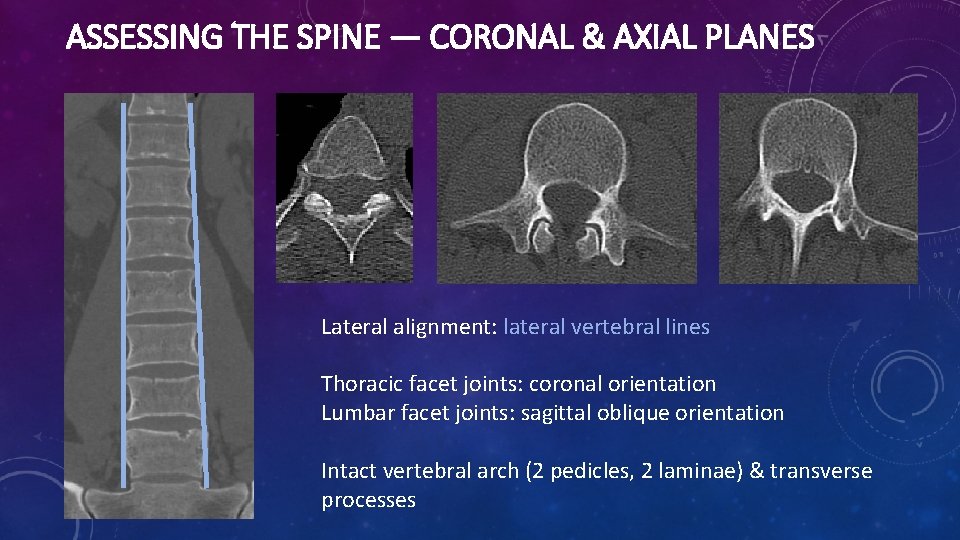
ASSESSING THE SPINE — CORONAL & AXIAL PLANES Lateral alignment: lateral vertebral lines Thoracic facet joints: coronal orientation Lumbar facet joints: sagittal oblique orientation Intact vertebral arch (2 pedicles, 2 laminae) & transverse processes

COMPRESSION FRACTURE • Most common morphology (90% of cases) • Usually from axial force with flexion • CT findings • Anterior vertebral body height loss • Disruption of vertebral endplate • More common = superior endplate (force directed downward) • Less common = inferior endplate • Horizontal sclerotic band (trabecular impaction) • Upper anterior wall cortical break • No acute change in vertebral body alignment • Posterior cortex of vertebral body intact (differentiates from burst fracture) • Cortex may bulge slightly posteriorly • No posteriorly displaced free fragment

COMPRESSION FRACTURE 63 M in MVC Acute compression fractures of T 6 and T 10 Anterior vertebral body height loss Disruption of superior endplate Trabecular impaction at T 6 on coronal Posterior T 6 and T 10 cortices intact
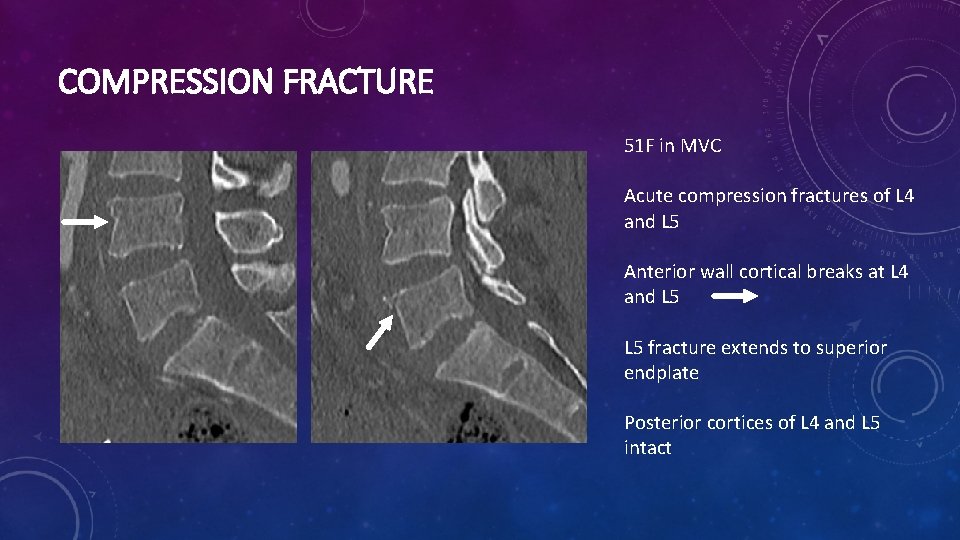
COMPRESSION FRACTURE 51 F in MVC Acute compression fractures of L 4 and L 5 Anterior wall cortical breaks at L 4 and L 5 fracture extends to superior endplate Posterior cortices of L 4 and L 5 intact
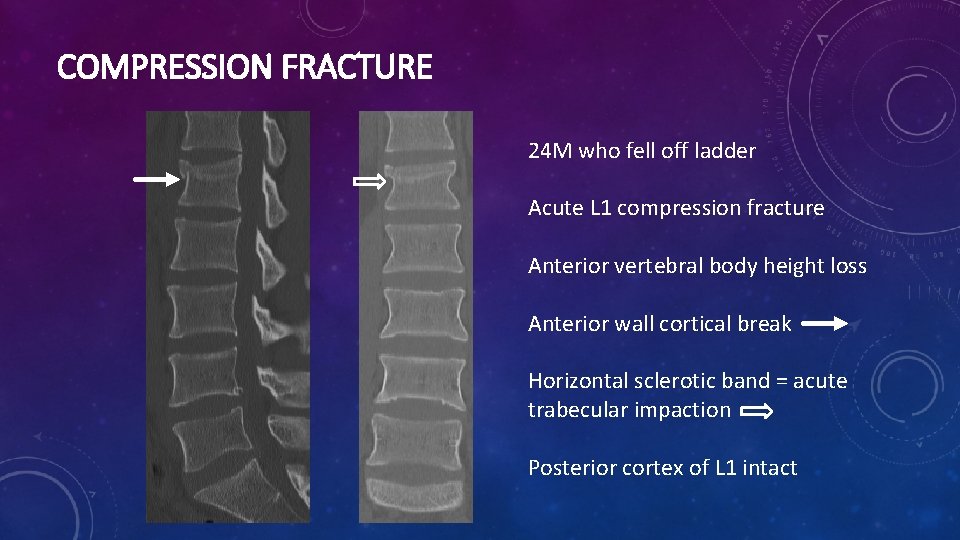
COMPRESSION FRACTURE 24 M who fell off ladder Acute L 1 compression fracture Anterior vertebral body height loss Anterior wall cortical break Horizontal sclerotic band = acute trabecular impaction Posterior cortex of L 1 intact
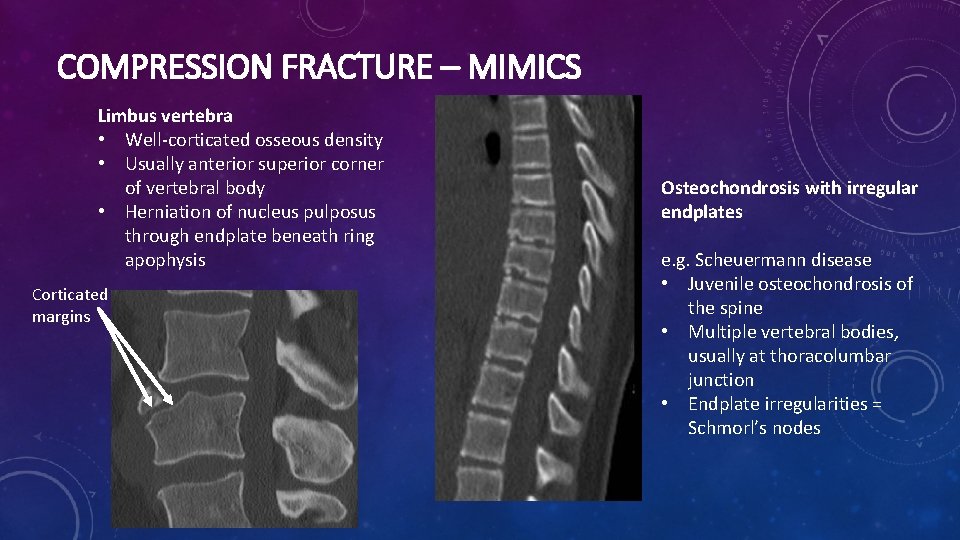
COMPRESSION FRACTURE – MIMICS Limbus vertebra • Well-corticated osseous density • Usually anterior superior corner of vertebral body • Herniation of nucleus pulposus through endplate beneath ring apophysis Corticated margins Osteochondrosis with irregular endplates e. g. Scheuermann disease • Juvenile osteochondrosis of the spine • Multiple vertebral bodies, usually at thoracolumbar junction • Endplate irregularities = Schmorl’s nodes

BURST FRACTURE • Usually results from compression with severe axial loading • CT findings • Retropulsion of fracture fragments into the spinal canal • Compression fractures may bulge the posterior cortex, but there should be absence of retropulsion • Sagittal fracture of the vertebral body (90%) • Sagittal posterior bony element fracture (85%) • Interpedicular distance widening (80%) compared to vertebrae above and below • If severe enough, possible PCL injury (discussed later)
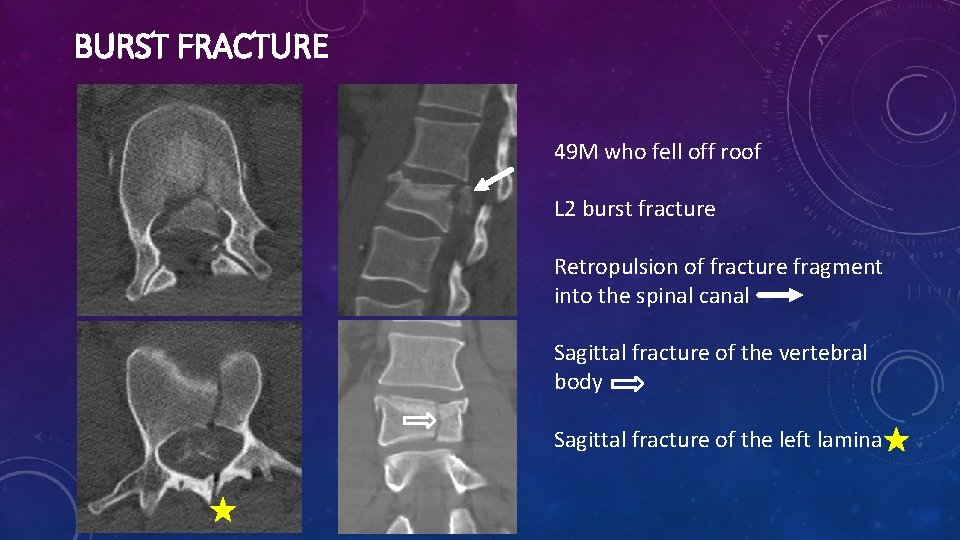
BURST FRACTURE 49 M who fell off roof L 2 burst fracture Retropulsion of fracture fragment into the spinal canal Sagittal fracture of the vertebral body Sagittal fracture of the left lamina
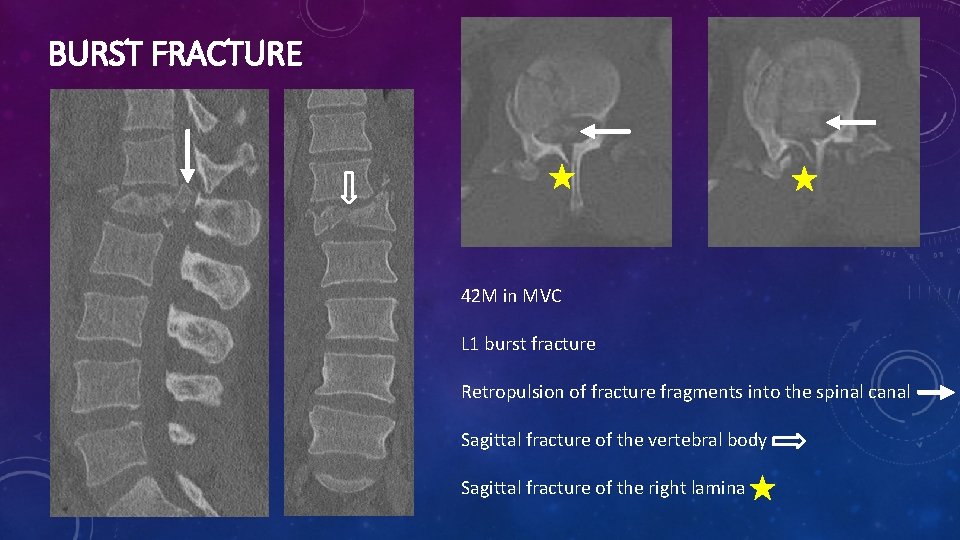
BURST FRACTURE 42 M in MVC L 1 burst fracture Retropulsion of fracture fragments into the spinal canal Sagittal fracture of the vertebral body Sagittal fracture of the right lamina

In order to better understand the last two injury morphologies, we need to first discuss the posterior ligamentous complex (PLC)

PLC INJURY • Posterior “tension band” of the spinal column • Protects spine from excessive flexion, rotation, translation and distraction • Torn PLC tends not to heal progressive kyphosis and collapse • CT findings inferring PLC disruption • Interspinous space widening/splaying of the spinous processes • Avulsion or transverse fractures of contiguous spinous processes • Widening or dislocation of facet joints • Vertebral body translation or dislocation • MR provides direct visualization of the PLC (almost always requested by Neurosurgery) • 3 points: loss of low-signal continuous black stripes on T 1 and T 2 (tears of the ligamentum flavum and supraspinous ligament) • 2 points: isolated edema without clear ligament disruption
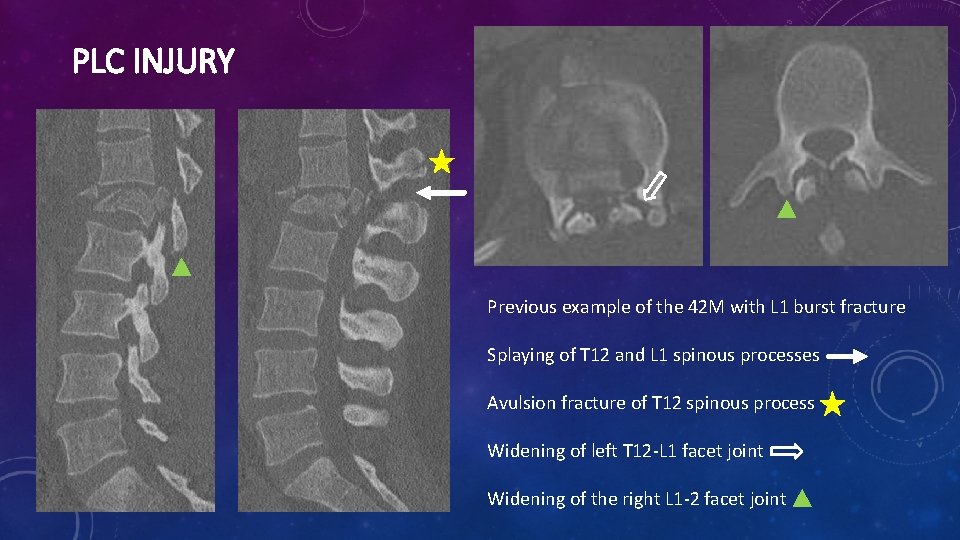
PLC INJURY Previous example of the 42 M with L 1 burst fracture Splaying of T 12 and L 1 spinous processes Avulsion fracture of T 12 spinous process Widening of left T 12 -L 1 facet joint Widening of the right L 1 -2 facet joint

Keep the PLC injury in mind as we discuss the next two fracture morphologies

TRANSLATION-ROTATION FRACTURE • Results from displacement in the horizontal plane • Left-to-right or anteroposterior motion • Rotary motion of one vertebra on another • CT findings • Anterior/lateral displacement or rotation of one vertebra with respect to another • Facet joint disruption or dislocation • ALWAYS PCL INJURY • 3 (injury morphology) + 3 (PCL status) + __ (neurological status) ≥ 6 on the TLICS chart already in the surgical management category • If thoracic often associated transverse process or rib fractures

TRANSLATION-ROTATION FRACTURE T 6 49 M who fell 20 feet, can’t move legs Just a T 6 burst fracture? Mild rotation of T 6 on T 7 (axial images) T 7 Need to look for findings of PLC injury in translation-rotation fracture! • T 6 spinous process fracture • Left T 6 -7 perched facet T 6 left pedicle/lamina, left transverse process, and bilateral rib fractures

DISTRACTION FRACTURE • Results from separation of two adjacent vertebrae • Severe injury, high chance of cord injury • CT findings • Posterior osseous distraction • Horizontal fractures through the posterior elements with widening • Associated with vertebral body compression (think lever) • ALWAYS PCL INJURY • Anterior osseous distraction • POSSIBLE PCL INJURY • Chance fracture little to no vertebral body compression Reference 8

CHANCE FRACTURE Transverse fracture through the left pedicle and spinous process with posterior osseous distraction T 11 vertebral body compression fracture • Mild anterior height loss • Disruption of superior endplate • Horizontal sclerotic band = acute trabecular compression

• If more than one injury morphology exists • Single injury with the highest score is used • If multiple levels of injury exist • Each injury is assessed independently

CHARACTERIZING ISN’T ALWAYS STRAIGHTFORWARD … T 11 43 M male who fell 20 feet Bilateral T 10 inferior articular facet fractures + T 10 spinous process fracture • Mild posterior osseous distraction T 11 burst-like fracture • Posterior cortex disrupted • Faint fracture fragment in spinal canal • Fracture left lamina (sagittal posterior bony element fracture)

• Severe T 11 burst fracture with extension into the T 10 and T 11 posterior osseous elements • Associated PLC injury OR • Distraction injury (posterior osseous distraction) with associated anterior compression fracture • Always PLC injury
I’M ON-CALL, TIRED AND IT’S 2 A. M. Burst fracture with posterior extension + PLC injury vs. Posterior distraction + Anterior vertebral compression 2 + 3 + __ ≥ 5 4 + 3 + __ ≥ 7 Characterize the injury as best you can with the energy reserve you have Surgical management Don’t delay patient care stressing over fine details if the end result is the same Think about the PLC (Neurosurgery will ask for MRI to assess this and the cord)

NEUROLOGIC STATUS • Critical indicator of degree of cord injury • Complete spinal cord injury = 2 points • Incomplete spinal cord injury or cauda equina = 3 points • Greater potential benefit from surgical decompression • Bump these patients into surgical management when possible • Role of radiologist • Assess extent of retropulsion & spinal canal narrowing • Epidural hematoma? • MRI to assess the cord

REFERENCES 1. Hsu JM, Joseph T, Ellis AM. Thoracolumbar fracture in blunt trauma patients: guidelines for diagnosis and imaging. Injury 2003; 34(6): 426 -433. 2. Khurana B, Sheehan SE, Sodickson A, et al. Traumatic thoracolumbar spine injuries: what the spine surgeon wants to know. Radio. Graphics 2013; 33: 2031 -2046. 3. Patel AA, Vaccaro AR. Thoracolumbar spine trauma classification. J Am Acad Orthop Surg 2010; 18(2): 63 -71. 4. Raniga SB, Skalski MR, Kirwadi A, et al. Thoracolumbar spine injury at CT. Radio. Graphics 2016; 36: 2234 -2235. 5. Sethi MK, Schoenfeld AJ, Bono CM, et al. The evolution of thoracolumbar injury classification systems. Spine J 2009; 9(9): 780 -788. 6. Vaccaro AR, Lehman RA Jr, Hurlbert RJ, et al. A new classification of thoracolumbar injuries: the importance of injury morphology, the integrity of the posterior ligamentous complex, and neurologic status. Spine (Phila Pa 1976). 2005 Oct 15; 30(20): 2325 -2333. 7. Vaccaro AR, Zeiller SC, Hulbert RJ, et al. The thoracolumbar injury severity score: a proposed treatment algorithm. J Spinal Disord Tech 2005; 18(3): 209 -215. 8. West C, Roosendaal S, Bot J, et al. Spine injury—TLICS classification. http: //www. radiologyassistant. nl/en/p 54885 e 620 ee 46/spine-injury-tlics-classification. html (last access February 15 2017).
- Slides: 34