Traumatic Hemorrhage Shock and Resuscitation LTC James R


































- Slides: 39

Traumatic Hemorrhage, Shock, and Resuscitation LTC James R. Reed CRNA

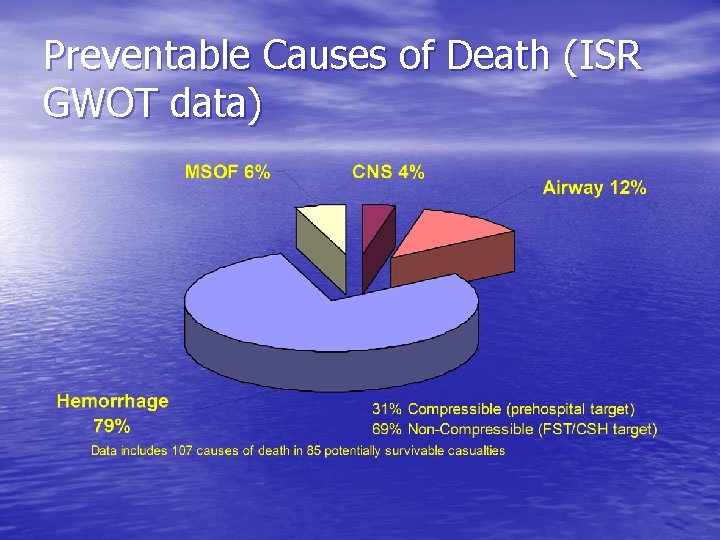
Preventable Causes of Death (ISR GWOT data)

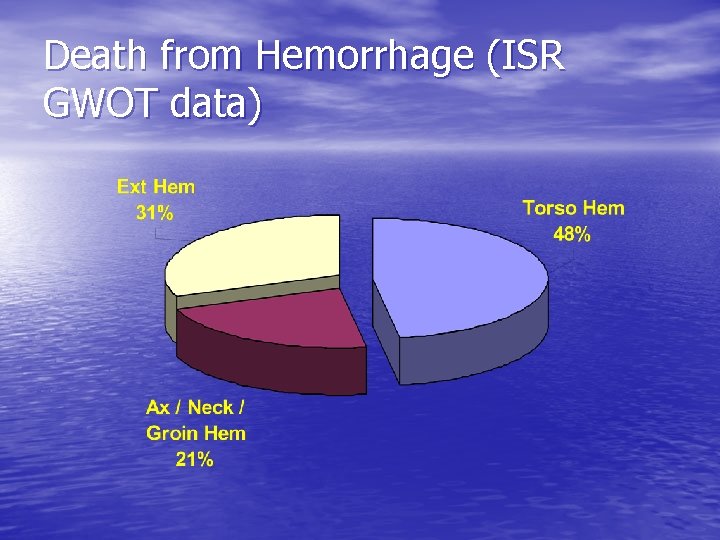
Death from Hemorrhage (ISR GWOT data)

Massive Hemorrhage and How much is too much? • Total blood volume for 90 kg adult. 07 x 90 kg = 6. 3 liters • 50% of total blood volume for 90 kg adult. 50 x 6. 3 liters = 3. 15 liters • 40% of total blood volume for 90 kg adult. 40 x 4. 9 liters = 2. 52 liters An acute loss of 40% blood volume is immediately life threatening!

Estimated Blood Loss It’s an estimate and almost always wrong • Factors effecting • adequate estimation are many A function of experience • Depends on what they • • bleed onto or into How much blood can the leg hold? Pelvis? Chest? Can you measure? If it looks like a lot, it probably is…

Massive Traumatic Hemorrhage Mortality versus units of blood transfusion • Mortality 28% if received 10 to 19 units • Mortality 65% if received 20 to 39 units • Mortality 83% if received 40 or more units • Average mortality 47% if > 10 u PRBC • Mortality multifunctional: ie. DIC, ARDS→MOSF→DEATH

Hemorrhage (How do you Stop It? ) • Extermities (arterial v. venous) • Chest • Abdomen • Retroperitoneum • Long bones • Diffuse (Think Blasts)

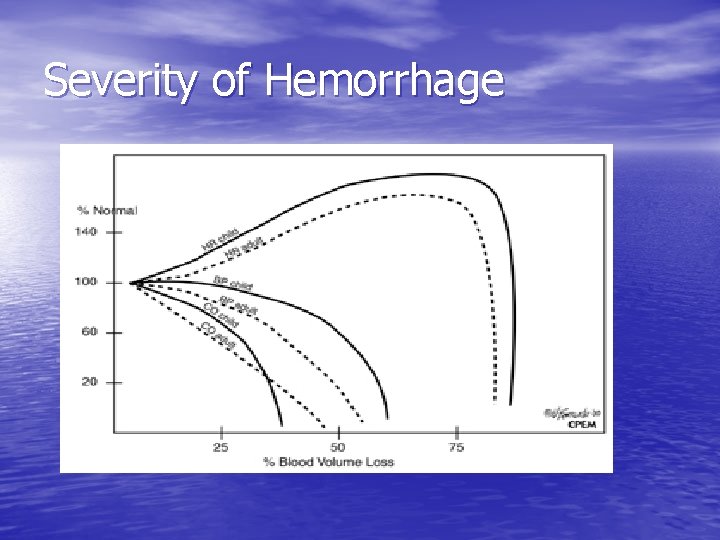
Severity of Hemorrhage

STOPPING THE BLEEDING/TREATING (preventing) SHOCK • • Direct pressure Tourniquet Clotting Agents Ligation/Tying of vessels Tube thoracostomy Damage control surgery Angiographic embolization (telangactasia)

Definition of Shock • A clinical syndrome arising from inadequate perfusion of tissues resulting in an insufficient cellular supply/demand ratio for oxygen resulting in cellular injury • After cellular injury, inflammatory mediators induce functional and structural changes within the microvasculature.

Definition of Shock continued The definition of shock does not involve low blood pressure, rapid pulse or cool clammy skin - these are merely the signs. Simply stated, shock results from inadequate perfusion of the body’s cells with oxygenated blood.

Shock “A rude unhinging of the machinery of life” defn. circa 1852 “A brief pause in the act of dying”

Types of Shock • Hypovolemic (Low Volume, Hemorrhagic) • Cardiogenic (Pump Failure) • Distributive (Sepsis) • Neurogenic (Spinal Cord Injury)

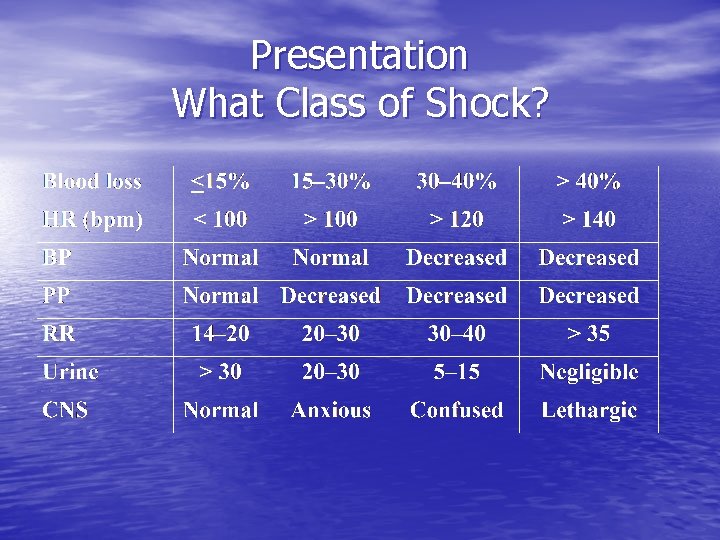
Presentation What Class of Shock?

SHOCK Hypovolemic Shock = Low Volume – Trauma – Non-traumatic blood loss • Vaginal • GI • GU – Burns – Diarrhea – Vomiting – Diuresis (DI) – Sweating

Shock Cardiogenic Shock = Pump Failure – Acute M I – CHF – Bradyarrhythmias (Heart Blocks) – Tachyarrhythmias (PSVT) – Mechanical obstruction • Cardiac tamponade • Tension pneumothorax • Pulmonary embolism

SHOCK Distributive Shock=Fluid in the wrong place – Septic Shock • Overwhelming infection • Inflammatory response occurs • Blood vessels – Dilate (loss of resistance) – Leak (loss of volume) • Fever – Increased O 2 demand – Increased anaerobic metabolism • Bacterial toxins – Impaired tissue metabolism

Distributive Shock (Cont) • Anaphylactic Shock – Severe allergic reaction – Histamine is released – Blood vessels v. Dilate (loss of resistance) v. Leak (loss of volume) • Extravascular smooth muscle spasm – Laryngospasm – Bronchospasm

Shock • Vasogenic Shock = Low Resistance – Spinal cord trauma • neurogenic shock • Sx’s? – Depressant drug toxicity – Simple fainting

Shock • Progressive syndrome • Three phases – Compensated – Decompensated – Irreversible

Decreased Cardiac Output Aldosterone, ADH Release Catecholamine Release Increased Blood Volume Increased PVR Increased Cardiac Output Increased Myocardial Work, O 2 Demand Myocardial Ischemia Increased Volume Loss Compensated Shock Leading to Decompensation

Key Issues In Shock Recognize & Treat during compensatory phase Restlessness, anxiety, combativeness = Earliest signs of shock Best indicator of resuscitation effectiveness = Level of Consciousness

Shock • Homeostasis – cellular state of balance – perfusion of cells with oxygen is one of its cornerstones • Adequate Cellular Oxygenation – Red Cell Delivery To Tissues Fick Principle

Fick Principle • Air’s gotta go in and out. • Blood’s gotta go round and round. • Any variation of the above is not a good thing!

The End Game • Cellular injury further compromises perfusion leading to more cellular damage, producing more widespread derangements of cellular metabolism • The end result if unchecked is multiple organ failure syndrome (MOSF) and death

Treatment of SHock • Fix the problem – Control hemorrhage – Replace fluid deficit – Fix the pump problem – Squeeze the vasculature (neurogenic and distributive)

Treatment of Shock (hypovolemic or hemorrhagic) and Resuscitation • Control Hemorrhage • • • – Treat life threatening problems (ie. Ptx) Control Airway Assist breathing if necessary Augment Circulation Establish venous access – Replace fluid – Give drugs, as appropriate – Don’t delay definitive therapy Maintain body temperature – Cover patient with blanket if needed – Avoid cold IV fluids

Goals of Resuscitation • Restoration or maintenance of tissue perfusion in the combat trauma patient prevents the cascade of shock and its deleterious effects on the total organism • Prevention or treatment of shock allows for body systems that are p. H and temperature dependent to function effectively (clotting, gas exchange)

Goals of Resuscitation (cont) • • TO RESTORE NORMAL TISSUE PERFUSION �� Blood pressure �� Pulse �� Respirations �� Skin Appearance �� Sensorium �� Urine output (0. 5 -1 ml/kg/hr) �� Hemoglobin 8 -10 gm or Hematocrit 24 -30

Treatment • • • Surgery: immediate vs. delayed vs. none �� Establish airway and deliver O 2 �� Insert 2 large bore IVs with relatively short length of tubing; infuse Normal saline or Lactated Ringer’s �� Treat mechanical causes of shock if they are present �� Tension pneumothorax �� Pericardial tamponade �� Exsanguinating hemorrhage

Trueisms of Combat Resuscitation • Keeping up is better than catching up (The SRT) • Oxygen delivery to the tissues is paramount • Controlling bleeding is primary objective at point • • • of injury Blood/components are the best fluid for resuscitation of the hemorrhaging patient Low volume resuscitation has shown itself to be effective until more robust facilities/personnel are attained HBOC not ready to be fielded

Fluid Resuscitation • Isotonic Crystalloid Infusion (Na. Cl or LR) • Volume expansion, increase in cardiac • • output, increase in blood pressure (can blow clots) Reduction in vasoconstriction (improves acidosis) Hemodilution, reduction of hematocrit (less red cell loss) Reduction in temperature (give warmed if possible) Immune dysfunction

Fluid Resuscitation • Colloid v. Crystalloid – Crystalloid (Na. Cl and LR) too much Na. Cl can lead to hyperchloremic acidosis, tend towards LR unless transfusing blood – Hespan, Hextend up to 20 mg/kg, can interfere with clotting if this amount is exceeded – Investigators have concluded albumin and Na. Cl were clinically equivalent for intravascular fluid volume resus.

Resuscitation • Type Specific Whole blood transfusion has produced amazing results resuscitating the multi -trauma patient – Contains red cells (oxygen), plasma (clotting), platelets (clotting) – Crystalloid (Na. Cl and LR) too much Na. Cl can lead to hyperchloremic acidosis, tend towards LR – Hespan, Hextend up to 20 mg/kg, can interfere with clotting if this amount is exceeded

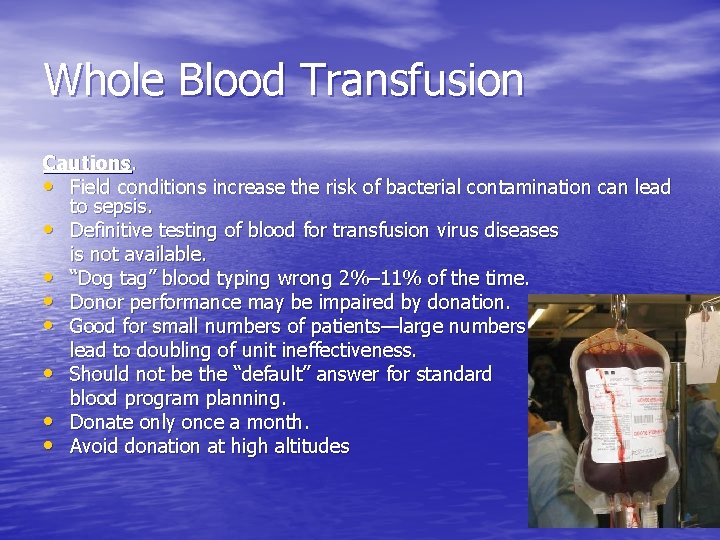
Whole Blood Transfusion Cautions. • Field conditions increase the risk of bacterial contamination can lead to sepsis. • Definitive testing of blood for transfusion virus diseases is not available. • “Dog tag” blood typing wrong 2%– 11% of the time. • Donor performance may be impaired by donation. • Good for small numbers of patients—large numbers lead to doubling of unit ineffectiveness. • Should not be the “default” answer for standard blood program planning. • Donate only once a month. • Avoid donation at high altitudes

Blood Typing and Collection

Whole Blood Transfusion • In combat trauma the risks of whole blood • • transfusion are mitigated by the circumstances of limited component supplies and the overall safety of the military donor population Type specific only to mitigate risk further, if mass casualty then type O (46% of US pop. ) Highly recommend confirming all personnel blood types before deployment and appropriate data base be maintained

Recombinant Factor VIIa • Clotting factor in the extrinsic clotting cascade (Vit K) dependent • Dose 90 -100 ug/kg in the trauma patient • If patient hypothermic or acidotic = renders Factor VIIa ineffective (get in early if patient situation and condition warrant or may need to administer Na HCO 3 for transient correction)

Questions • PLEASE