TraumaFocused CognitiveBehavioral Therapy Anthony P Mannarino Ph D

Trauma-Focused Cognitive-Behavioral Therapy Anthony P. Mannarino, Ph. D. Judith A. Cohen, M. D. Center for Traumatic Stress in Children and Adolescents Allegheny General Hospital Drexel University College of Medicine Pittsburgh, PA 2018 © Mannarino & Cohen,

Types of Childhood Trauma • • • Sexual abuse or assault Physical abuse Witness to domestic violence Victim or witness of community violence Victim or witness of school violence Bullying Suicide Motor vehicle or other travel accidents Weather-related events Terrorism Mass disasters Kidnapping; fires, etc.

Additional Types of Trauma • Traumatic loss • Medical trauma - Cancer - Burns - Transplant or other life-threatening procedures - Mutilating accidental or intentional injury

Adverse Child Experiences (ACEs) • ACEs overlap significantly with childhood trauma • In addition to DSM 5 -defined traumas, ACEs include: - Neglect - Caregiver drug and/or alcohol abuse - Parental criminal behavior/incarceration (possible traumatic separation) - Divorce - Parental psychiatric problems - Psychological abuse

Trauma Impact • Acute distress almost universal • Impact can be long lasting • Childhood trauma is risk factor for numerous adult psychiatric and medical problems • Impact varies; most recover time without treatment but a significant minority will develop moderate to serious PTSD symptoms and will require treatment

Affective Trauma Symptoms • • • Fear Sadness Anger Anxiety Affective dysregulation

Physiologic Trauma Symptoms • • • Irritability Difficulties with concentration Sleep problems Angry outbursts Impulsivity Reckless behavior

Cognitive Trauma Symptoms • Irrational or erroneous beliefs (e. g. , “The abuse was my fault. ” “I should have stopped him from drinking. ”) • Reduced trust • Negative self-Image (e. g. , “I am bad. ” “I am damaged. ”) • Potentially accurate, but unhelpful, cognitions (e. g. , “Most men are dangerous. ” “There will probably be another terrorist attack today. ”)

Behavioral Trauma Symptoms • Avoidance • Maladaptive behaviors – Sexualized behaviors – Violent behaviors – Bullying • Traumatic bonding • Angry outbursts/temper tantrums • Substance abuse • Self-injury

Common Diagnoses • • PTSD Depressive disorders Other anxiety disorders Comorbidity is common Ø ADHD Ø Oppositional Defiant Disorder Ø Substance Use Disorder Ø Bipolar Disorder Ø Psychotic disorders- up to 20% of traumatized children have psychotic symptoms

Chronic Trauma Exposure (Complex Trauma) • Typically includes complex trauma experiences and complex trauma outcomes • Trauma sequelae are often broader than one diagnosis and may include: Ø Severe affective dysregulation Ø Interpersonal difficulties Ø Adversely affected belief systems Ø Somatic distress or disorganization Ø Serious self-esteem issues • Typically results in significant functional impairment

TF-CBT Studies and Complex Trauma • Complex trauma experiences: TF-CBT studies have focused on interpersonal traumas (e. g. , sexual abuse, domestic violence); contrary to the belief that “TF-CBT is for simple traumas”, research cohorts have documented multiple ongoing interpersonal traumas (Average number of trauma in recent studies: 3. 4) • Complex trauma outcomes: TF-CBT studies consistently assess these, e. g. , PTSD, affective dysregulation, behavior problems, cognitive and perceptional issues, relationship/attachment outcomes

Trauma Assessment • Assessment is frequently viewed as not important BUT: How will you know whether a child needs trauma treatment? • Has there been trauma exposure? • Are there any trauma symptoms? • What type of trauma treatment is most appropriate? • Are there psychiatric co-morbidities that may account for the symptoms?

Trauma Assessment (cont’d) • Clinical interview with child and caretakers • Structured instruments: - UCLA PTSD Reaction Index (RI)- young child, adolescent, and parent versions - Child PTSD Symptom Scale (Foa) - Trauma Symptom Checklist for Children (Briere) - Parent Emotional Reaction Questionnaire {PERQ} (Mannarino & Cohen) - Children’s Attributions and Perceptions Scale (Mannarino & Cohen)

Trauma Assessment (cont’d) • Is a full PTSD diagnosis necessary? • Symptoms + functional impairment • There will likely be other diagnoses in addition to PTSD • New DSM 5 criteria for children age six and under

Pathway to Trauma Treatment • What is the clinical presentation? - Presence of trauma symptoms • What is the connection between the trauma exposure and current symptoms? • What is “driving the train”? • Start with different treatment and sequence to TFCBT? • Therapist needs to be convinced of the need for trauma treatment if the family is going to get on board

Engaging Families in Treatment • Inform caretakers that TF-CBT is a treatment for families, not just for children; build this expectation! - Let parents know why it is important that they participate • Establish common ground/form an alliance • Recognize concrete barriers to participating in treatment • Emphasize importance/primacy of parental role

Engaging Families (cont’d) • Be flexible about scheduling • Focus on what parents need and want from therapy • Provide education about psychotherapy (what to expect: it occurs over time, not all at once, etc. ) • Address such issues as stigma, cultural concerns, and previous experiences with therapists • Shannon Dorsey’s work on the effectiveness of engagement with foster families

Engaging Families in Treatment (cont’d) • NO SHAME AND NO BLAME • Praise and reinforce parents/caretakers for bringing child for treatment

Small Group Activity Related to Parental Engagement • Identify concrete and/or psychological barriers to parental participation in TF-CBT • Identify at least one and hopefully multiple solutions to the problem • Spokesperson for the small group will report to the larger group about the problem and potential solutions

Getting “Buy-in” for TF-CBT • Review trauma assessment - Connection between exposure and current clinical symptoms • Explain what TF-CBT is: for trauma symptoms and trauma-related behavioral problems • Obtain consent from caregiver and child (if youth is old enough to provide consent) • If you don’t get “buy-in”, DO NOT go forward with TF-CBT - Will need to do different trauma treatment or treat a different set of problems

What Are Evidence Based Treatments for Traumatized Children? • What They Are Not: Rigid Lockstep Inflexible…

What is TF-CBT? A HYBRID TREATMENT MODEL THAT INTEGRATES: § Trauma sensitive interventions § Cognitive-behavioral principles § Attachment theory § Developmental Neurobiology § Family Therapy § Empowerment Therapy § Humanistic Therapy

For Whom IS TF-CBT Appropriate? • Children with known trauma history- single or multiple, any type • Children with prominent trauma symptoms (PTSD, depression, anxiety, with or without behavioral problems) • Children with severe behavior problems may need additional or alternative interventions • Parental/caretaker involvement is optimal - However, PTSD improves even in the absence of caretaker involvement

For Whom is TF-CBT Appropriate? (cont’d) • Treatment settings: clinic, school, residential, home, inpatient • TF-CBT is appropriate for the following groups: - Children in foster care - Children with exposure to chronic trauma - Children with PTSD or other trauma symptoms - Children ages 3 -18 - Children on autism spectrum who function at higher level - Children of different cultural groups including Latino, African-American, and Native-American

Major Barriers to Trauma Treatment • Fear of retraumatizing the child • Vicarious traumatization • “Our clients are different”

Laura Murray’s Project in Cambodia • Sex trafficked girls • Initial response from local counselors: “Our population is different so TF-CBT won’t work”; “These girls aren’t ready to tell their stories”. • Recent comment from counselor: “I have worked with this client for two years already and never had a story like this. I did not know her real story. I think TF-CBT has helped me so much”.

TF-CBT Treatment Research: Randomized Clinical Trials • 22 RCTs • 9 RCTs have been completed by the Cohen, Deblinger, and Mannarino team • Two RCTs in the Democratic Republic of Congo for sex trafficked girls and boy soldiers • Study in Zambia by Laura Murray • One RCT in Norway by Tine Jensen and her group • The Netherlands: TF-CBT vs. EMDR • One RCT in Germany that included youth with complex trauma

Treatment Research • Studies have been conducted with children exposed to sexual abuse, domestic violence, traumatic losses, civil war, sex trafficking and multiple traumas • Improved PTSD, depression, anxiety, shame and behavior problems compared to client-centered or nondirective therapy • Improved parental distress, parental PTSD, parental support, and parental depression compared to clientcentered or nondirective treatment

TF-CBT Web-based Dissemination • TF-CBTWeb- NO LONGER ACCESSIBLE • TF-CBTWeb 2. 0 (www. musc. edu/tfcbt 2) • CTGWeb (www. musc. edu/ctg) • TF-CBTConsult (www. musc. edu/tfcbtconsult)

TF-CBT Therapist Certification Program • Therapist Certification Program started in September, 2013. • Website: https: //tfcbt. org

Core Values of TF-CBT • CRAFTS § Components-based § Respectful of cultural values § Adaptable and flexible § Family focused § Therapeutic relationship is central § Self-efficacy is emphasized

Child and Parent Components • Inform caretakers that TF-CBT is a treatment for families, not just for children; build this expectation! • Individual sessions for both child and parent • Parent sessions - generally parallel child sessions • Same therapist for both child and parent • Child and parent receive about the same amount of time at each session • Treatment length: 8 -25 sessions

TF-CBT Components • PRACTICE § Psychoeducation and Parenting Skills § Relaxation § Affective Modulation § Cognitive Processing § Trauma Narrative § In Vivo Desensitization § Conjoint parent-child sessions § Enhancing safety and social skills

Safety • Starting with safety is often clinically appropriate with most youth and their families • Therapist potentially as a trauma reminder • Developing safety plans • Identifying other safe adults in youth’s environment

Components- and Phase-Based Treatment PRACTICE COMPONENTS: PHASES: Psychoeducation; Parenting Skills Relaxation Skills PHASE Affective regulation Skills Cognitive processing Skills Trauma narration and processing PHASE In vivo mastery of trauma reminders Conjoint child-parent sessions PHASE Enhancing safety TF-CBT STABILIZATION TN INTEGRATION
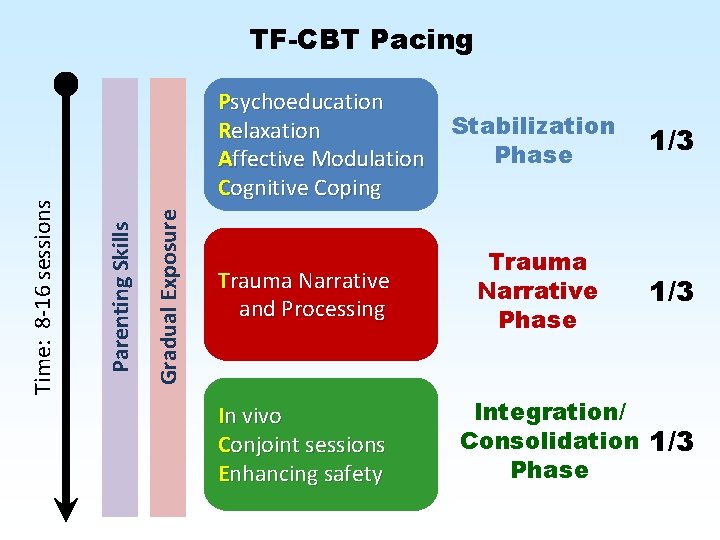
Gradual Exposure Psychoeducation Relaxation Affective Modulation Cognitive Coping Parenting Skills Time: 8 -16 sessions TF-CBT Pacing Trauma Narrative and Processing In vivo Conjoint sessions Enhancing safety Stabilization Phase 1/3 Trauma Narrative Phase 1/3 Integration/ Consolidation 1/3 Phase
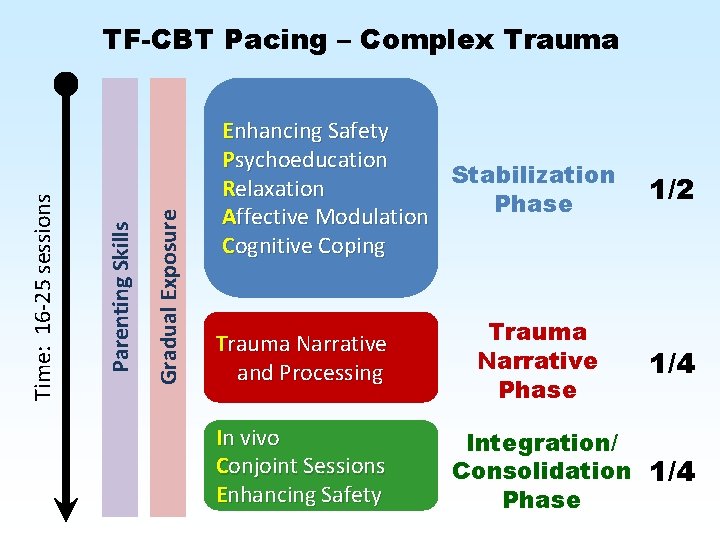
Gradual Exposure Parenting Skills Time: 16 -25 sessions TF-CBT Pacing – Complex Trauma Enhancing Safety Psychoeducation Stabilization Relaxation Phase Affective Modulation Cognitive Coping Trauma Narrative and Processing In vivo Conjoint Sessions Enhancing Safety Trauma Narrative Phase 1/2 1/4 Integration/ Consolidation 1/4 Phase

Critical TF-CBT Treatment Themes • Order of PRACTICE components • Incorporating gradual exposure into the skillsbased components • Importance of behavioral interventions with parents/caretakers • TF-CBT is a treatment model which emphasizes proportion and balance

TF-CBT Treatment Themes (cont’d) • Flexibility vs. fidelity • Implement TF-CBT based on therapist’s knowledge of child’s skills, talents, and interests • TF-CBT at every treatment session: Do not let COWs (crises of the week) get you off track • TF-CBT treatment has to be FUN!

TF-CBT Fidelity • All of the TF-CBT components are implemented • TF-CBT components in order of PRACTICE acronym, unless there is clinically appropriate justification • Appropriate proportionality and pacing of components • Completion of TF-CBT within appropriate time frame

Psychoeducation • Goals: § Normalize child’s and parent’s reactions to severe stress § Provide information about psychological and physiological reactions to stress § Instill hope for child and family recovery § Educate family about the benefits and need for early treatment § Educate family about trauma reminders § PSYCHOEDUCATION GOES ON THROUGHOUT THERAPY!

Psychoeducation (Cont’d) • Provide general information about the event v Frequency v Who experiences it v What causes it • Provide information about common emotional and behavioral responses to the specific event(s) • Provide information about the child’s symptoms/diagnosis • Emphasize positive coping • Sources for psychoeducation: • www. NCTSN. org • www. aacap. org Facts for Families • “What Do You Know” game for SA, PA, DV

Parenting Skills • TF-CBT views parents/caretakers as critical therapeutic agent for change • Explain the rationale for parent inclusion in treatment – Not because parent is part of the problem but because parent can be the child’s strongest source of healing • Emphasize positive parenting skills and enhancing enjoyable child-parent interactions • Clinical anecdotal data that TF-CBT enhances the quality of the parent-child relationship, including youth with attachment-related issues

Treatment of Parents Research Evidence that treating parent is important: § Deblinger et al. (1996): Treating parents resulted in decreased behavioral and depressive symptoms in child § Cohen and Mannarino (1996): Parents’ emotional reaction to trauma was the strongest predictor of treatment outcome (other than treatment type) § Cohen and Mannarino (1997): At the 12 month follow -up, parental support was significantly related to decreased symptoms in child • Delaware study of session by session TF-CBT parent work

Common Parental Issues in Child Traumatization • • • Inappropriate self-blame and guilt Inappropriate child blame Overprotectiveness Overpermissiveness PTSD Symptoms

Complicated Caregiver Situations • When the caregiver is unsupportive or does not believe that the child was exposed to a trauma • When the caregiver is the perpetrator (e. g. , physical abuse or domestic violence) - Different treatment (e. g. , Alternatives for Families: Cognitive-Behavioral Therapy- AF-CBT) • Can perpetrators ever be involved in TF-CBT?

Praise and Positive Attention • Focus on actively praising the child § Praise a specific behavior § Provide praise ASAP after behavior occurs § Be consistent § Do not qualify your praise § Provide praise with same level of intensity as criticism

Functional Behavioral Analyses • Antecedents of behavior • Behavior • Consequences

Selective Attention • No reaction to certain negative behaviors – Defiant or angry verbalizations to parent – Nasty faces, rolling eyes, smirking – Mocking, mimicking • Walk away, busy oneself with an activity • Remain calm, dispassionate • Expect a reaction of more provocative behavior

Time Out • Purpose: Interrupt child’s negative behaviors and allow him/her to regain control • Explain to child • Location: quiet, low stimulation • Duration: 1 minute per year of age • Timer starts when child stops screaming • Once in time out, parent should refrain from comments, and maintain calm demeanor. • Be consistent

Contingency Reinforcement Programs • Purpose: Decrease unwanted behaviors and increase desired behaviors • Select only one behavior to target • Explain process to child • Involve child in decisions about rewards • Add stars and give rewards weekly.

Behavior Management • Reasonable developmental expectations • Limit-setting • Behavioral interventions for: – Anxieties – Sleep problems – Aggressive behaviors – Sexually inappropriate behaviors

Behavior Management Vignette #1 Jason is a 10 year-old boy who has been bullied at school by three older children. In one instance, they stole his new jacket and punched him several times. These bullies have been disciplined by the school principal and are no longer bothering Jason. Nonetheless, he often is afraid to go to school, wakes up with stomach aches, and frequently misses the bus. At home, he is irritable and has been aggressive with two younger siblings. Many times Jason has outbursts when his Mom and Dad ask him to do something. What suggestions would you have for his parents?

Behavior Management Vignette # 2 Kelly is a 4 year-old girl who was sexually abused over several months by her uncle. Now Kelly is touching her genitals and rubbing herself at school and at home. She has also started to touch her younger brother and two playmates. Kelly attends therapy with her mother who is very distressed with these behaviors but does not know how to respond. Her mother often becomes overwhelmed and upset when talking about the abuse and Kelly’s symptoms. She typically overreacts to Kelly’s sexualized behaviors. What would your interventions be with Mom?

Relaxation • Reduce physiologic manifestations of stress and PTSD • Reduce distress related to trauma reminders • Can help to lower the body’s alarm reactions • Can be used at anytime so child will probably need more than one skill to use • Can be coupled with other skills like feeling expression or cognitive coping during the trauma narrative component

Relaxation (cont’d) • Develop individualized relaxation strategies for manifestations of stress (headache, stomach ache, dizzy, racing heart, etc. ) • Focused breathing/mindfulness/meditation • Progressive muscle relaxation • Physical Activity • Yoga, singing, dance, blowing bubbles • “If it’s not fun, you’re not doing it right” • Relaxation strategies for trauma reminders

Relaxation (cont’d) • Importance of practice • One strategy - Child rates level of distress prior to practice - Child practices for 10 -15 minutes - Child re-rates level of distress • Child keeps simple chart of practice sessions • If not successful, consider other relaxation strategies

Parental Involvement in Relaxation Component • Parent may need own relaxation strategies • Brief joint session for child to demonstrate newly learned relaxation strategies • Parent should be aware of child’s relaxation strategies so that child can be prompted to practice

Affective Modulation • Traumatized children may have inappropriate (e. g. , excessive anger) and/or restricted range of affective expression • Activities to help children identify and express a range of different feelings - Board games (Emotional Bingo) - Feeling brainstorm - Color Your World or person - Emotions Color Wheel • Importance of feeling identification and expression when there are trauma reminders

Parental Involvement in Affective Regulation Component • Therapist models appropriate affective regulation • Cultural norms/concerns related to affective expression are discussed • Role plays with caregiver to support child with appropriate affective expression - Sadness - Anger

Thought Interruption and Positive Imagery • Use when overwhelmed with trauma reminders • Temporary measure early in treatment • Teaches child control over their thoughts § Changing the channel § Saying “go away” or “snap out of it” § Imagining a stop sign • Replace unwanted thought with a positive one

Affective Regulation (cont’d) • Positive Self-Talk- focus on strengths • Improving social skills: interpreting other’s affective expressions accurately • Develop a safety plan

Cognitive Processing • Help children and parents understand the cognitive triad: connections between thoughts, feelings and behaviors, as they relate to everyday events • Help children distinguish between thoughts, feelings, and behaviors • Help children and parents view events in more accurate and helpful ways • Encourage parents to assist children in cognitive processing of upsetting situations, and to use this in their own everyday lives for affective modulation

GE: Cognitive Coping and Processing • This is one exception to GE in PRAC components - Children are not asked about their trauma-related cognitions until the trauma narration and processing component • Why? Dysfunctional thoughts are more likely to be expressed during the narrative than before. • Communicate to child that trauma-related cognitions will be addressed later in treatment

Cognitive Processing (cont’d) • Strategies to deal with trauma-related distortions and/or unhelpful thoughts at this stage of treatment - Validation, empathy, and support - Psychoeducation - Relaxation strategies • Parents are encouraged to examine traumarelated cognitions during this component.

COGNITIVE PROCESSING the process starts with feelings identification, then children learn that they can change how they act and feel by thinking differently. The Cognitive Triangle Thoughts Behavior Feelings


Cognitive Work with Children. Identifying Thoughts HELPING CHILDREN TO TALK ABOUT THEIR THOUGHTS • Use appropriate child language • Adjust to their developmental level, BE CREATIVE! – What do you think about when you’re ______(insert feeling)? – Are there any thoughts or pictures that go through your mind? – What popped into your head? What did you say to yourself? – What went through your head? – Use a cartoon bubble and fill it in

Example to Illustrate Cognitive Triad • You and your friend are supposed to go to the movies together this afternoon. He sends you a text message in the morning that he can’t go. No explanation. – What are some reasons for this? What goes through your head? – How does that make you feel? What do you do?

Cognitive Processing in Young Children • Cognitive triangle will have little utility • Young children can understand the concrete idea of “Who made that happen? ” • Cognitive coping in young children: “The Little Engine That Could” “Eggbert: The Slightly Cracked Egg” “Giraffes Can’t Dance”

Cognitive Processing Video Game TF-CBT TRIANGLE OF LIFE • Currently available on the Google Play Store • Currently available on the Apple Store

Wise Cognitive Coping “One evening an old Cherokee told his grandson about a battle that goes on inside people. He said, “My son, the battle is between two wolves inside of us all. One is Evil. It is anger, envy, jealousy, sorrow, regret, greed, arrogance, self-pity, guilt, resentment, inferiority, lies, false pride, superiority, and ego. The other is Good. It is joy, peace, love, hope, serenity, humility, kindness, benevolence, empathy, generosity, truth, compassion and faith. ” The grandson thought about it for a minute and then asked his grandfather: “Which wolf wins? ’ The old Cherokee simply replied, “The one you feed. ”

Direct Discussion of Traumatic Events Reasons we avoid this with children • Child discomfort • Parent discomfort • Therapist discomfort • Legal issues - It is the child’s narrative, not therapist - Keep the narrative out of child’s official record - What to do with the narrative at the end of treatment - Therapists should not testify in court, if possible

Direct Discussion of Traumatic Events (cont’d) • Reasons to directly discuss traumatic events: • Gain mastery over trauma reminders • Resolve avoidance symptoms • Identify and correct distorted cognitions • Contextualize traumatic experiences into overall life

2, 000 Years Ago The philosopher Epictetus said: “The thing that upsets people is not what happens but what they think it means. "

Preparation for Trauma Narrative • Should the idea of a TN as part of TF-CBT be introduced at the start of treatment with both child and parents? • When should the child be told that s/he will be starting the TN? • Do the child/parents need a rationale for the TN?

Creating the Trauma Narrative • Many options (to be discussed) • Can introduce the TN by reading a book • First chapter : innocuous information about the child (name, age, school, hobbies, etc) • Second chapter : “Before”, for example, what the relationship was like with the person before the trauma started (if interpersonal trauma); or what life was like before the index traumatic event occurred

Creating the Trauma Narrative (cont’d) • Third chapter: Encourage the child to “tell what happened” during the trauma itself using words and drawings

Creating the Trauma Narrative (cont’d) • If multiple episodes, let the child choose one (example: first time, last time, one best remembered) • May include disclosure(s), legal procedures, medical exams, other secondary adversities

Creating the Trauma Narrative (cont’d) Review the child’s description § Help the child to describe more details § Encourage child to describe thoughts, feelings and body sensations related to the trauma § Desensitize child to talking about the event

How To Encourage Children To Tell What Happened • Avoid asking “Do you remember…. ? ” • Instead encourage “telling the story”: • “I wasn’t there so tell me all about what happened…” • “What happened next…? ”

My uncle came into my room to kiss me goodnight. He pulled down the covers and touched me down there. I felt scared. I pretended I was asleep. When he was done, he left. The next morning I got up and my uncle said, “Good morning, how are you? ” and I said, “Fine”. I went to school.

My uncle came into my room to kiss me goodnight. I felt good. He pulled down the covers and touched me down there, on my vagina. I felt scared and dirty, and thought why is he doing this, he’s my favorite uncle. I pretended I was asleep. When he was done touching my vagina, he left. The next morning I got up and my uncle said, “Good morning, how are you? ” and I said, “Fine”. Inside I felt scared and I didn’t know what to say or do. I went to school.

Creating the Trauma Narrative (cont’d) • Identify “hot spots” or “worst moments” • Rate distress before, during, and after (SUDS thermometer for children)

Creating the Trauma Narrative (cont’d) • Final Chapter: include the following: • What have you learned? • What would you tell other kids who experienced this? • How are you different now from when it happened/when you started treatment?

What I Learned in Therapy I came here because I was sexually abused by my uncle. I used to feel scared and dirty. Now I know my body is OK. I don’t know why he did that, but he has a problem and it wasn’t my fault. I didn’t know what to say or do about the sexual abuse. I felt like I didn’t do anything, but I did. I told my Mom and a wrote a book about it. That makes me feel proud. If this ever happens to you, you could say, “No!”, get away and tell. If it’s hard to say no or get away – just tell - that is the most important thing anyway! Tell someone you trust.

Tips for Implementing Trauma Narrative • How much time should be spent on TN in one session? • Leaving time at the end of the session for transitional or relaxation/fun activities • How about children who are distractible and/or hyperactive? • Significant distress during TN- how should this be handled? • Therapist’s emotional reaction to the creation of the TN

How Much Detail in the TN? • The TN is not the same as prolonged exposure in the Foa Prolonged Exposure model • Level of detail will be dependent on the child’s age and developmental level • Child may only describe the details of one abusive episode (although there may have been many episodes) • Or, the child may describe the details of one trauma in the context of multiple traumas • The critical importance of generalization along with the integration of the PRAC skills

Trauma Narrative Strategies Alternative methods for creating a trauma narrative: • Cartoon strip • Poem • Talk Show Interview • Song • Drawings • Instant message/text message • Play narrative for young children • RELY ON CHILD’S STRENGTHS AND INTERESTS TO OVERCOME AVOIDANCE

Trauma Narrative When There Are Multiple Traumas or Youth Presents with Complex Trauma Which trauma is the focus of the TN? • What were the findings from the clinical interview and any structured instruments? - Which trauma was most disturbing or caused the greatest amount of distress? - Was child highly avoidant of one more than the others? • Do you start with the most disturbing trauma or one that the child can more easily deal with? • Include traumas that are contributing to trauma symptoms

Trauma Narrative When There Are Multiple Traumas or Complex Trauma (cont’d) • Limit the number of sessions for the TN so that it is not overwhelming for the child • Provide some structure so that the child understands what will be covered • Possible utility of life narrative or timeline • Provide details about at least one trauma experience • Look for underlying core trauma themes of blame, shame, betrayal, feeling damaged

Sharing the Trauma Narrative with the Parent • Parent may not know details of what happened - Avoidance - Legal issues • Explore what parent knows about the traumatic event • Share with parent what child has said in therapy - Confidentiality - Developmental issues • Sharing TN may not be appropriate, especially in complex trauma cases when trust is a major theme

Cognitive Processing of the Trauma • Explore inaccurate or unhelpful cognitions about the trauma and the feelings that accompany them § Inaccurate thoughts (ex: “the sexual abuse was my fault”) § Unhelpful thoughts (ex: “this may be the day of the next terrorist attack”) § Inaccurate AND unhelpful thoughts (ex: “it’s my fault my mother was killed in the hurricane. I should have made her evacuate sooner. ”) § Replace distorted cognitions with more accurate, realistic, or helpful ones § Responsibility vs. regret

Cognitive Distortions: Clinical Example Dear Dad, I will never get over what you did to me. It hurt me that you thought I was nothing but a piece of garbage. Now everyone knows what happened to me. Although you called me a liar in court I know I told the truth. I will never know whether you forgive me for testifying. I know you will pay for this because we have both sinned. The daughter you hate

Ways to Identify Cognitive Distortions • Trauma Narrative • Assessment measures - Children’s Attributions and Perceptions Scale - Child Post-Traumatic Cognitions Inventory • Attending to child’s comments throughout PRAC • Parent’s observations

What Is Usually Not Helpful • Telling child something like “it’s not your fault” • Children have heard this sort of statement from many others (e. g. , parents; police; advocates, etc. ) • If these statements from others were truly helpful, children would no longer have these types of distortions • They need to figure this out for themselves with the help of their therapists

Where to Start • Normalize thoughts - “Many children believe they should have told sooner. ” - “I’ve talked to many children who think they should have been able to stop their father from hurting their Mom. ” • Validate feelings - “I can see how badly it makes you feel when you think it was your fault. ”

Techniques for Challenging Trauma. Related Cognitive Distortions • Progressive Logical Questioning - Lists and Definitions • “Responsibility Pie” • The “Best Friend” role play

Socratic Questioning Questions that gently challenge beliefs or thoughts: • Implemented in a positive, fun manner • Each question is a step on the bridge • May need several steps to get from one triangle to the on the other side of the bridge • May take more than one session

Socratic Questioning Example • Example: Thought = The sexual abuse was my fault. • Therapist: What makes you say it was your fault? • Client: Because I didn’t tell anyone it was happening. I should not have gone back there. • T: Thinking back, why didn’t you tell anyone? • C: Well, he said he would hurt my mother. • T: Oh. Did you believe him? • C: Yes, at the time I did. • T: That sounds really scary. Any other reasons you didn’t tell? • C: I guess I was worried my mom wouldn’t believe me. • T: And when you did tell her, she actually did have a hard time believing you.

Socratic Questioning Example (cont’d) • C: Yeah. • T: So you weren’t far off on that, actually. Any other reasons you didn’t tell? • C: Well, he told me I would go to jail if the police found out. • T: Did you believe that? • C: Well, I was young. I guess I did. • T: Hmm. . . Sounds like you actually had some important reasons for not telling. You were worried he would hurt your mother, you were worried about your mom’s reaction, and you were convinced you could go to jail for telling. Do those seem like good reasons for a 9 - year-old to keep silent? • C: Well, now that I think about it more. . . I guess it did make sense.

Lists and Definitions • Good strategy for negative thoughts involving overgeneralization of untrue or unhelpful thoughts - “I am a bad kid. ” - “My child has lost her innocence and had her childhood taken away by the abuse. ” • Make a list of all the qualities that make for a good kid • “Let’s make a list of what are signs that a child is innocent and enjoying their childhood. ”

Cognitive Processing of Trauma with Caregiver • Help parent identify his/her own cognitive distortions and related feelings – “I should have known this would happen” – “My child will never be happy/can never recover from this” – “My child’s childhood is ruined” – “Our family is destroyed” – “I can’t handle anything anymore” – “I can’t trust anyone anymore” – “The world is terribly dangerous” • Help parent challenge his/her own distortions and replace them with more accurate and helpful cognitions • Help parent identify and practice effectively challenging child’s cognitive distortions

Cultural Considerations for Cognitive Processing of the Trauma • Explore possible culturally-related beliefs/distortions • Focus on healthy and helpful aspects of cultural values vs. unhealthy/unhelpful aspects • Use progressive logical questioning and reframing

In Vivo Mastery of Trauma Reminders • Mastery of trauma reminders is critical for resuming normal developmental trajectory • To be used only if the feared reminder is innocuous (not if it’s truly dangerous) • Hierarchical exposure to innocuous reminders which have been paired with the traumatic experience • Gradually help the child to get used to the feared situation • Resolve generalized avoidant behaviors

In Vivo Mastery of Trauma Reminders • CRITICAL ELEMENTS: • Identify and assess feared situation/triggers • Engage child and/or parent in creating specific desensitization plan to gradually approach feared situation • Ensure parent is committed to follow through with plan; parent uses praise, selective attention, and rewards • Therapist MUST have confidence that this will work or it won’t • Goal: improved adaptive functioning for child and child regains sense of competence and mastery

Case Vignette: Ellen You have been working with five year old Ellen for the past 2 months. She and her grandmother regularly attend sessions and have just finished sharing the trauma narrative. Trauma History: : Ellen was referred for treatment after witnessing the homicide of her mother. Ellen’s mother was shot and killed by her father who is now in jail. Ellen initially presented with significant regressive behaviors including nightmares, bedwetting, and refusal to sleep in her own room. Her grandmother has been supportive and they have made a great deal of progress in therapy. However, Ellen still refuses to sleep in her room and usually sleeps on the floor in her grandmother’s room (sometimes she sneaks into grandma’s bed after grandma has fallen asleep). Develop an in vivo plan to address these problems.

Sample Desensitization Plan for Child who Fears Going to Sleep in His/Her Own Bed • Educate parent on importance of quality sleep for recovery and developmental importance of child being able to sleep alone • Efforts to make child feel safer in room (i. e. nightlight, flashlight, checking closets, etc. ) • Bed-time rituals, transitional objects, and relaxation techniques • Warn parents that first few nights will likely be difficult (first try over the weekend) but persistence is key • Plan: parent initially stays in child’s room for 15 minutes, gradually reduces time spent in room, and eventually moves to chair outside room • Parent reassures child s/he will check in at regular intervals (not when child is crying) • Parent praises child for complying (staying in bed quietly) for increasing intervals • Special reward: extra TV time; time with parent

Conjoint Parent-Child Sessions GOALS: • Share trauma narrative • Address and correct cognitive distortions (child and parent) • Encourage optimal parent-child communication about the trauma(s) • Prepare for future trauma reminders • Praise for progress made

Conjoint Parent-Child Sessions (cont’d) FORMAT OF SESSIONS: § Meet individually with parent and child prior to joint part of session § Meet together after child and parent prepared for session

Conjoint Parent-Child Sessions (cont’d) • WHEN NOT TO HAVE JOINT SESSIONS: § Parent unable to provide appropriate support § Parent continues to be overly emotional in response to child’s traumatic experience § Child adamantly opposed (evaluate how realistic objections are)

Conjoint Parent-Child Sessions (cont’d) Other Options: • Have joint session with parent and child but do not include review of child’s TN • Instead focus on general communication, conflict resolution, praising each for what they have done successfully and for persisting with therapy

Vignette #1 • You have been providing home-based services to 10 year-old Susanna for the past few months. You have worked with mom and grandma to prepare for the sharing of the TN and feel confident that they are ready. When you get to their home on the day that the sharing is supposed to take place, Susanna’s uncle, aunt, and adult cousin are also present and mom tells you that they also want to be part of the session. • How would you proceed?

Vignette #2 • Jackie is an 11 year-old girl who experienced physical and sexual abuse by her stepfather. Over the course of treatment, you learn that Jackie’s mom, Jane, was sexually and physically abused as a child. You have recommended that Jane receive her own therapy and, as far as you can tell, Jane has not complied. During your preparation sessions with Jane, she continues to evidence extreme distress when you talk about her daughter’s abuse. Jackie is ready to share her story. • How would you proceed?

Vignette #3 • You are a school-based clinician, who has been using TF-CBT with Steve who was abused by his stepfather. You have tried to include his grandmother (with whom he lives) in the sessions but it is really difficult for her to get to the school because of health issues and multiple doctors’ appointments. Steve’s guidance counselor has been a resource for you and Steve’s family. • What adaptations to the conjoint sessions could you make?

Enhancing Safety Skills • May be done individually or in joint sessions • Develop a safety plan which is responsive to the child’s and family’s circumstances and the child’s realistic abilities • Develop children’s body safety skills • Practice these skills outside of therapy • For sexually abused children, include education about healthy sexuality • For children exposed to DV, PA, CV, may include education about bullying, conflict resolution, etc.

Demonstration of Safety Skills • • • Establishing a “personal safety space” Saying “no” to invasions of personal space Leave, escape, report (“NO, GO, TELL”) Assuming an assertive stance Being vigilant without being hypervigilant

Vicarious Trauma • • • This is hard work Take care of yourself and your colleagues Ask for consultation Have a life outside of work Get help if you need it.
- Slides: 119