Trauma Dissociation and Psychosis CBT and Other Approaches

Trauma, Dissociation, and Psychosis: CBT and Other Approaches to Understanding and Recovery Presenter: Ron Unger LCSW 541 -513 -1811 4 ronunger@gmail. com

The connection between trauma and psychosis u Mainstream mental health system understanding: – Serious mental illnesses such as schizophrenia are biological in origin, & do not result from any special sorts of events u Cognitive therapy understanding: – Traumatic experiences can easily lead to things like “imbalances” in thinking which can lead to psychosis

What does the research say? u. A body of research now includes many large-scale population-based studies controlling for possible mediating variables u This research provides strong evidence that trauma can be a contributing cause for psychosis See “Childhood trauma and psychosis: Evidence, pathways, and implications”, W Larkin, J Read. J,

The Evidence that Trauma can Cause Psychotic Symptoms: u u u The high incidence of psychotic symptoms in people who have been traumatized The high incidence of trauma histories in people who have psychotic symptoms Studies that show the greater the severity of the trauma, the greater likelihood of more, and more intense, psychotic symptoms Brain changes sometimes linked with psychotic symptoms and “schizophrenia” are also found disproportionately in children who have been abused There are logical and meaningful connections between psychotic symptoms and normal reactions to traumatic experience
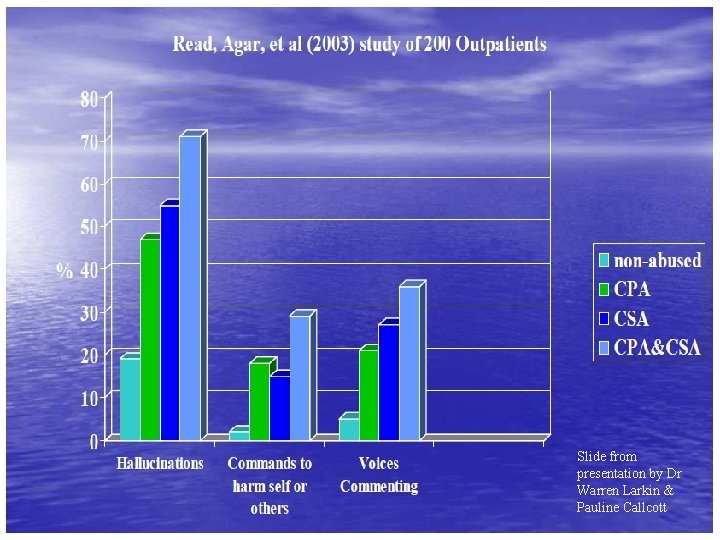
Slide from presentation by Dr Warren Larkin & Pauline Callcott

Three levels of possible relationship between trauma and psychosis: 1 Trauma, especially childhood sexual trauma, can cause psychosis later 2 Having psychotic symptoms can in itself cause trauma 3 The response by others to one’s psychosis can also be traumatizing Responses by the mental health system, by family & friends, can all add to trauma u Further trauma can cause more psychosis, in a vicious circle See “Relationships between trauma and psychosis: A review and integration” by Anthony P. Morrison, Lucy Frame and Warren Larkin 2003

Becoming more “open minded” when no solution is apparent u When people are trying to control something – And there is no direct way to do it u Then they become more likely to see unlikely patterns – Including seeing images in noise, perceiving conspiracies, and believing in superstitions Whitson, J. A. , & Galinsky, A. D. (2008). Lacking control increases illusory pattern perception. Science, 322(5898), 115 -117.

Schizotypy, creativity & illusory pattern perception, & trauma u People who are schizotypal habitually – have more creative associations 2006) (Nettle, – see more illusory patterns – & seem to have weakened contextual integration - (Marzillier & Steel, 2007) u People who are schizotypal are more easily traumatized - (Marzillier & Steel, 2007) – Also true that people who have been traumatized are more likely to become schizotypal - (Berenbaum, Valera, & Kerns, 2003)

Trauma and/or stress that one doesn’t know how to handle In attempt to solve the problem, mind tries weird/extreme things Psychosis (disorganization or mistaken way of being organized. ) Weird/extreme things seem to “work” but really cause more problems

Don’t assume a trauma history: there appear to be multiple roads that lead to psychosis Some are primarily biological, or physical (like too much methamphetamine) u Some are directly related to trauma u Some seem more related to a “buildup” of stress & negative emotions that aren’t well dealt with, that become overwhelming (even traumatic? ) u Some may result from a catastrophic interaction among all the above u – See “The catastrophic interaction hypothesis” by Fowler et al in the book “Trauma and Psychosis: New directions for theory and therapy”

How is “Psychological Trauma” Defined? u DSM focuses on perceived physical threat – But this is somewhat arbitrary u Psychological impact is key – Trauma is created by a combination of sense of overwhelming threat, or terror, with helplessness – It’s not a specific type of event, but our appraisal of the event, which causes psychological trauma u Even if the appraisal is mistaken, the terror & trauma may be real

Why is the role of trauma in causing psychosis commonly denied? u Hoping for a simple explanation: – since some psychoses have a biological cause, maybe they all do? Evidence of genetic causation is commonly exaggerated u Bias toward believing that if biology is involved at all, it must be primary u Pharmaceutical companies & their allies gain power when the explanation is biological u Denial of trauma has lessened overall, but this hasn’t yet reached the field of psychosis u

Why is the role of trauma in causing psychosis commonly denied? (continued) Past overly simplistic judgments and assumptions by some of those who did see a role for trauma in causing psychosis u Parallel process u – Neither the client, nor the mental health system, want to face the facts of the trauma u Idea that if trauma causes a mental problem, it will be PTSD

Positive and Negative Symptoms u Psychosis and PTSD can both be divided into clusters of positive and negative symptoms u (Mc. Gorry u Many 1991) of what are called the negative symptoms of PTSD – difficulty concentrating, withdrawal, emotional numbing, derealization, estrangement, self neglect – overlap with what are identified with the negative symptoms of psychosis u (Fowler, 1997; Stampfer, 1990)

Common factors in PTSD and psychosis: u u u u u High arousal & hypervigilance Sleep disturbance Avoidance Emotional numbing Selective Attention Safety behaviors Dysfunctional thought control strategies Expressed emotion causes relapse Dissociation Intrusive phenomena: thoughts, sensory, emotions See “Relationships between trauma and psychosis” by Larkin & Morrison, in the book “Trauma and Psychosis: New directions in theory and therapy” p. 260 -261
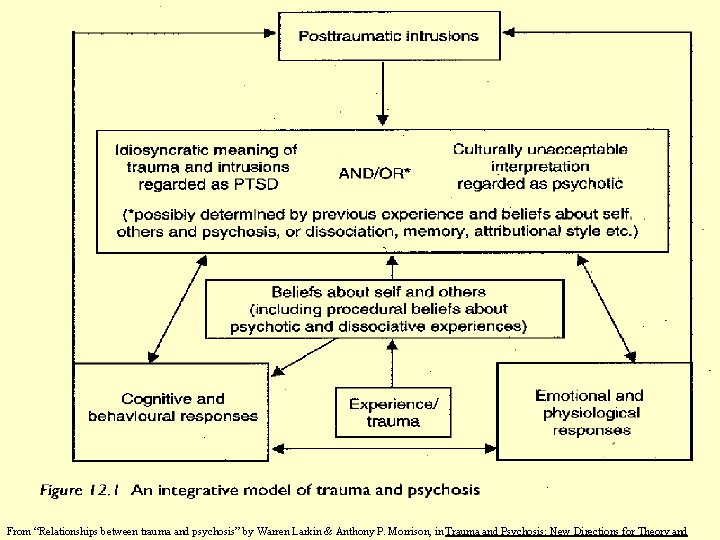
From “Relationships between trauma and psychosis” by Warren Larkin & Anthony P. Morrison, in Trauma and Psychosis: New Directions for Theory and

A key common factor: Fear of going mad u 70% of those diagnosed with psychosis reported “fear of going crazy” as the most common “prodromal symptom” out of 30 that were assessed u (Hirsch u & Jolley, 1989) Interpreting initial post trauma symptoms as a sign of impending madness was found in one study – to be common in those who developed PTSD compared to those who didn’t, and – to distinguish those who developed persistent PTSD from those who recovered u (Dunmore, Clark, & Ehlers, 1999)

What happens when a person fears madness? u Fears that intrusive mental phenomena are “madness” leads to attempts to avoid experiencing them – Which interferes with exposure, or finding out one can handle them, and putting them in perspective (as memories, etc. ) – Instead, person is (re) traumatized, as a desperate attempt to control experience fails.

What is the impact of the mental health system’s refusal to see the link between trauma & psychosis? u Trauma is often not even asked about, much less discussed – Potentially, through decades of treatment u Understandable reactions to trauma are defined as non-understandable u Psychotherapy for trauma is denied u Even self-understanding is discouraged

Assessment: Finding out about trauma u Need to ask – Often clients won’t say if not asked – Seldom harmful to ask, often harmful not to ask u Asking seems common-sense, but research says in our current mental health system, it commonly doesn’t happen for people with psychosis – Read, Hammersley, & Rudegeair, 2007
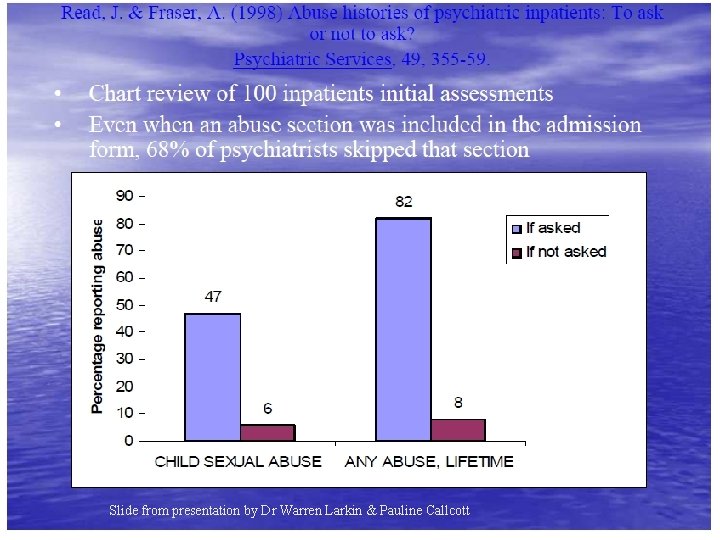
Slide from presentation by Dr Warren Larkin & Pauline Callcott

How to ask: u Prepare the person u Move questions from general to specific – Specific questions are much more likely to elicit reports of abuse u Know how to respond

How to respond to reports of abuse: u u u Not necessary gather a lot of details immediately Affirm it was positive to tell you Offer support – Like access to counseling u Check current safety – Including if abuser might currently be abusing others u u u Check emotional state end of session Offer follow-up or check in Has person told anyone before – if so how did that go? “Why, when and how to ask about childhood abuse“ John Read, Paul Hammersley and Thom Rudegeair (2007)

Also ask about possible trauma caused by by mental health treatment u One study – 31% had moderate to severe PTSD symptoms related to admission for mental health treatment u (Beattie, 2009) Shannon, Kavanagh & Mulholland, u Forced drugging, restraint, and seclusion have been identified as inducing fear, victimization and helplessness – Also a factor: Loss of control over identity as one is forced into the role of a “mental patient”

General principles of trauma informed CBT for psychosis: u Collaborative, – neither imposed structure nor lack of structure u Client prioritizes problems and goals – But address any issues that might interfere with therapy first u Have a clear rationale for each step – And get consent for each step u Also attend to supports outside of therapy

The role of therapist uncertainty: u“People wish to be settled; only as far as they are unsettled is there any hope for them. ” – RALPH WALDO EMERSON, “Circles, ” Essays: First Series, 1841

Key skill: soliciting feedback u Watch for signs you may be going in the wrong direction – Either lack of progress – Or client dissatisfaction u If client is unhappy, don’t automatically assume direction is wrong – Might just be need a better rationale – Or perhaps direction is partly wrong, partly right u Sorting that out may require some discussion
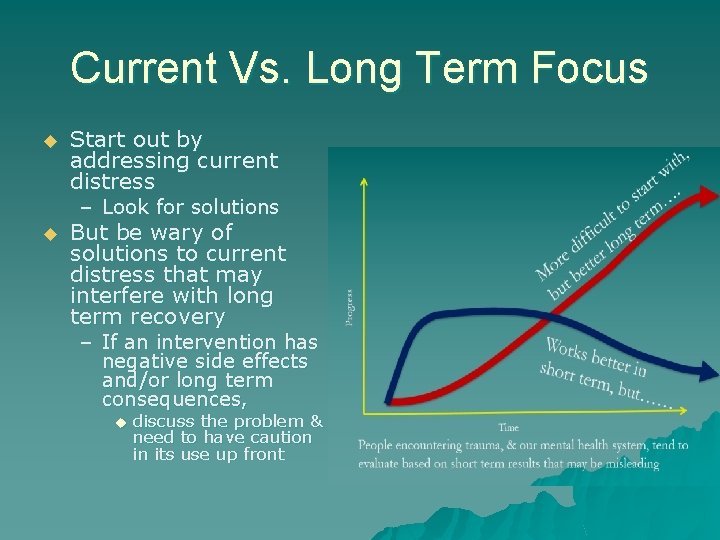
Current Vs. Long Term Focus u Start out by addressing current distress – Look for solutions u But be wary of solutions to current distress that may interfere with long term recovery – If an intervention has negative side effects and/or long term consequences, u discuss the problem & need to have caution in its use up front
Key role of pacing in facing difficult experience I don’t want to understand myself or my past experience: Please distract me from myself, or numb me out, no matter what the cost! I get to know myself gradually: I make sure I have resources to fall back on so that I can handle the difficult experiences that I am eventually willing to face. I am willing to face anything about myself, even that which I’m not ready to handle: I don’t have any sense of preparedness or pacing, so I overwhelm myself.

Areas for Interventions u Three basic areas – current problems – Longer term factors such as vulnerability, schemas, values – trauma u Often address in that order – But sometimes a different order makes sense u Or it makes sense to skip around

Don’t wait for problems to go away before addressing the future u Research suggests that when people focus on their values, symptoms diminish – Or at least, ability to act despite symptoms increases u Recovery is about regaining the ability to move in a meaningful way toward person’s values – Full recovery, with no remaining disability or need for treatment, is always a possibility

Integrating other methods when addressing trauma directly u The rationale for all methods used should fit with the formulation u Many trauma therapies can integrate easily with CBT for psychosis u Often start with a cognitive approach to trauma, to reduce distortions & increase grounding – Then more experiential or desensitizing approaches – And/or more depth oriented approaches

When desensitization is effective: u Trauma flashbacks and/or psychotic intrusions become simply memories or thoughts – That are put into an understandable and manageable context – That are neither avoided nor overly attended to u Once they are put into context no “illness” remains

When People Have Both Psychosis & a Trauma History u Not – “You have a mental illness” u Instead – Your experience may make sense as a “normal” kind of reaction once we know your story u So both – Normalizing – Developing the formulation

Effective Therapy: Shifting the Question u From “What’s wrong with you? ” u To: – “What happened to you? ” and – “What’s happening with you right now? ” and – “What would you like to see happen in the future, and what do you see as your possible role in making that happen? ”
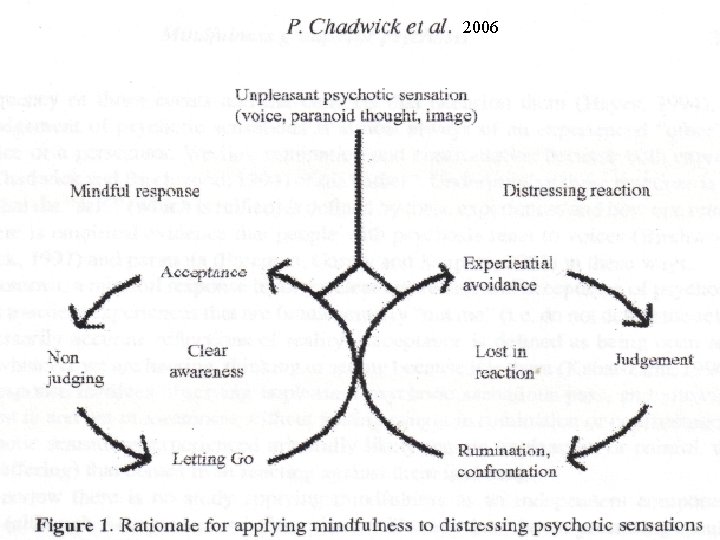
2006

“Take Your Voices for a Walk” Exercise u Split into groups of 2 or 3 – One person is a voice hearer, other person(s) are voices u “Voice hearer” tries walking around, noticing what is in the room – Or doing some other task u Practice acceptance of the voices, letting go of reaction to them – While re-focus on your intended activity

Two directions in good stress management u Detachment – Reducing the perceived need to “do something even when that leads to overwhelm” u “Letting go of what I cannot change” part u Empowerment – Helping a person get power over one’s own life u “Courage to change things I can” part

The Role of Assembling a Story: u Forming coherent narratives of the past, which help frame the present, and define future possibilities – with flexible capacity to integrate internal & external experience u The narrative should successfully explain both the traumatic experience and the psychosis – And it should do so in a way that promotes hope and self worth See “Narrative CBT for Psychosis” by Rhodes & Jakes, p. 117 -138

Working toward a narrative u Slow down the session & gently inquire about areas that seem broken or fragmented – See “Staying Well After Psychosis” p. 114 u Look at both the positive and negative side of coping strategies – This helps integrate positive and negative affect about the strategies, and about life direction in general

Steve, 23 years old u Several “psychotic breaks” u Lots of paranoia – Fear related mostly to “the government” u No recollection of childhood trauma – But family members were able to recount stories of physical abuse, sexual abuse, and exposure to severe domestic violence

What worked u Positive, supportive relationship u Gently questioning the beliefs about the government u Looking at past trauma as possible source for “emotional flashbacks” to terror that were being blamed on current threat from the government – At first, this explanation was more terrifying than the paranoid beliefs

When the reported “trauma” may be imaginary: u Two pronged strategy: – Help improve coping with the memories and related paranoia and psychosis u Just as you would for any reported trauma – Explore in detail what is known about that time period in person’s life u Adding fiction details may help sort fact from – As well as discern underlying themes that may be finding expression as delusional beliefs

Developing Self-Affirming Narratives u Not psychotic stories, and – NOT “the illness causes…” u Instead: – Consider explaining in terms of coping strategies that backfired, or were too extreme u If there may have been biological predisposing factors, consider the possibility of alternative ways of coping with those factors u Having a coherent story of what might have caused the psychosis creates room to imagine a story of recovery

Trauma narrows the focus u In a traumatic experience, a person’s focus & interests narrow to what seems necessary to survive – Possibilities are seen in black & white, u to aid sharp decision making and intense action – Some interests & needs must be sacrificed to carry out the survival strategy

Core dynamic in extended or unresolved trauma: intrapersonal conflict is amplified to point of dissociation u Struggle between incompatible reactions or strategies – When one extreme doesn’t work, a tendency to jump to opposite extreme u While organizing around one strategy, the other extreme is seen as “the enemy” or an intruder u This conflict accounts for much of the dynamics in both PTSD and psychosis

The most common, or Primary, Structural Dissociation u The Apparently Normal Part, or ANP – This part fuses with “daily life” motivations, and avoids or blocks traumatic memories and/or upsetting emotions u The Emotional Part, or EP – This part is fused with particular forms of threat response, and avoids considering the impact of that response on other concerns

Two Types of Dissociation u “Negative” dissociation – What is “shut out” depends on what is the focus of attention u ANP attempts to shut out EP – To better focus on everyday life u EP attempts to shut out ANP – To better focus on threat u “Positive” Dissociation – Results when formerly dissociated content or parts intrude or reconnect in a disorderly way

“Positive” Dissociation Can Be an Attempt to Heal That Backfires u Attempts to bring together what was formerly kept separate can lead to – disorder – preoccupation with internal realities that may be seen as external u These problems can lead to self and/or others perceiving and fearing madness – Resulting in attempts to shut down the process & return to “negative dissociation

A Paradox u The same process, positive dissociation, or creatively bringing together what has usually been kept separate, is – A risk for retraumatization & psychosis – A necessary part of healing u Finding successful ways to bring together parts that have been at war requires – Boundaries that also have some openness

Two types of hallucinations and/or delusions: u Those whose function is to get the person to focus on a threat – This type makes the threat appear PRESENT in some way u These are on a spectrum with “flashbacks” that are common after trauma u Those whose function is to protect the person from being overwhelmed by a sense of threat – This type makes the threat appear ABSENT in some way u All types of grandiosity for example can be understood as having a protective function

Relationship between dissociative identity disorders & schizophrenia u The more symptoms considered to be unique to schizophrenia a person has – The more likely that person is to fit criteria for dissociative identity disorder – (Foote & Park, 2008) u Experiences often considered to be the most clear indicators of schizophrenia, like voices conversing – Are actually pretty typical in dissociative identity disorder

Effect of dissociation on selforganization of dissociated content u Whatever is not integrated in some way may take on a life of its own u Content not yet integrated may be simple or complex – From automatic thoughts, emotions, memory fragments – To mood states, perspectives, voices – To complex identity states seen as “alternate personalities” or alien entities

Dissociation, and loss of contact with reality u Dissociation can lead to – Loss of “internal anchors” (the sense of being connected to one’s body, a sense of self or identity, and a sense of ownership over one’s actions) u The result of this may be – Not only impaired reality testing – Also severe confusion, disorganization, & disorientation u (Allen et al 1997)

Decontextualized Experience u Ordinarily, the hippocampus serves to bind individual features of incoming information into a spatial/temporal context – Then info goes to amygdala u But when trauma is too intense, info goes straight to the amygdala – Resulting in memory fragments that contain high affect u With no context See “The catastrophic interaction hypothesis” by Fowler et al. , in the book “Trauma and Psychosis: New Directions in Theory and Therapy”

Decontextualized trauma flashbacks can easily become “psychotic” u Problematic interpretations of the activation of trauma memories – Like a voice that echoes meanings first encountered during trauma u Might be interpreted as a current presence of the abuser, or as an alien or demon See “Relationship between child abuse and psychosis” by Read, Rudegeair & Farelly, p. 39 -41, in the book “Trauma and Psychosis: New Directions for Theory and Therapy”

Effects of trauma & child abuse is often apparent in “symptoms” u One study found that over half of the “schizophrenic symptoms” of abused adult inpatients appeared obviously related to the abuse – for example, hearing the voice of a perpetrator commanding them to commit suicide u (Read & Argyle, 1999)

Dissociation, Delusions and Disorganization u Delusions in themselves are not dissociative – But may be explanations that convey some truth while also disguising it u Disorganization dissociative is also not directly – But can result from functional impairment with too much dissociation – Or result from attempts to transcend dissociative ways of functioning
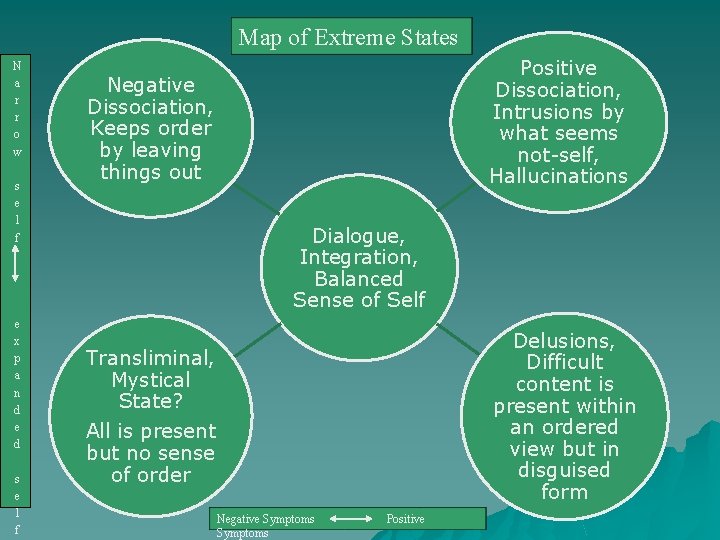
Map of Extreme States N a r r o w s e l f e x p a n d e d s e l f Positive Dissociation, Intrusions by what seems not-self, Hallucinations Negative Dissociation, Keeps order by leaving things out Dialogue, Integration, Balanced Sense of Self Delusions, Difficult content is present within an ordered view but in disguised form Transliminal, Mystical State? All is present but no sense of order Negative Symptoms Positive

Simple technique to address polarized experience u Draw a continuum, showing both extremes – Portray each extreme as potentially useful in the right circumstance u Ask the client to consider – what some more middle of the road options might be - how much of each extreme might fit particular circumstances
Drawing a continuum to illustrate the possibility of going too far in either direction: Focused on defending against interpersonal threats: Gullible for overreacting to signs of threat Vigilant for both kinds of threat but not overly so Focused on defending against overreacting to threat defending against being paranoid: Gullible for interpersonal betrayal

Working Toward Balance u Need to set limits with intrusive, disturbing, or polarized parts of the psyche u While also being open to hearing about, and addressing, the underlying concerns that those parts represent – Note that the second step will seldom be taken if the disturbing part is seen just as a “symptom” of an “illness”

Exercise on Identifying Two Extremes u “Client” briefly describes struggling with some problematic state or inner experience u “Therapist” helps explore the possibility this experience or part of the self is trying to be helpful u (though maybe too extreme) – Then therapist asks questions to figure out what an opposite extreme might be u Write it on paper! – Asks “client” how he or she might be able to identify a healthy middle ground

The Focus Widens in Healing u. A shift occurs, – From u “either/or” – To u “both/and” u Person identifies with both “opposing” forces within self, plus wider context and concerns – (While a shift to a wider focus can be helpful, a too radical shift can also cause disorganization and overwhelm)
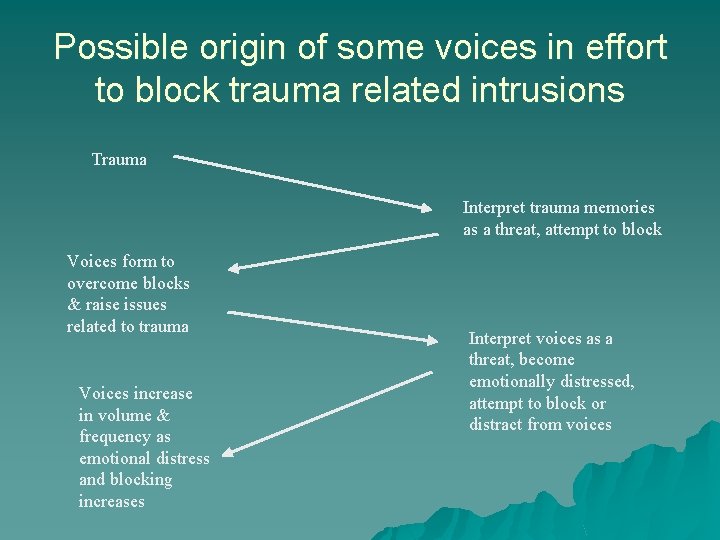
Possible origin of some voices in effort to block trauma related intrusions Trauma Interpret trauma memories as a threat, attempt to block Voices form to overcome blocks & raise issues related to trauma Voices increase in volume & frequency as emotional distress and blocking increases Interpret voices as a threat, become emotionally distressed, attempt to block or distract from voices

It is the “blocking” itself that sustains the power of the intrusion u Trying to get rid of the “madness” is actually part of the madness u “The way out of hell is through the center” – Just accepting the intrusion or unwanted trauma reminder or “psychotic” experience, allows us to put it into perspective for what it is – And it’s putting it into perspective, into context, that allows us to move on

Problematic ways of coping with voices: u Flight: Relying on avoidance and distraction – Issues aren’t dealt with, person feels too weak to face the voice u Fight: Arguing with the voice, trying to change it’s mind – Fighting with the voice is a distraction from life u Submission: Giving in to the voice – Even if voice demands are not harmful, personal power is diminished

Better way of coping with voices: u Alternating between attending to, and ignoring, the voices – Can choose the best method for the occasion, or set “appointments” with them u Be both assertive and friendly with the voices – Able to not take voices literally, while seeing them as clues regarding issues that may need attended to

Trauma Life goes increasingly out of control as preoccupation with the voices goes up Vicious Circle Seeking control & toughness to deal with trauma Voices appear as an internal representation of what cannot be controlled Voices “feed” off the tension involved in efforts to control them: they increase Voices are interpreted as a threat to sense of control, so attempts are made to control them

Less Trauma Life becomes increasingly manageable as preoccupation with voices decreases Virtuous Circle Accept vulnerability that exists alongside some toughness When voices appear, accept them as clues about areas of vulnerability Due to lack of tension around them, voices become less noticeable Voices are not interpreted as a threat to sense of control, so it does not seem necessary to eliminate them

Command Hallucinations u Reducing compliance is often essential u Compliance comes from a dominant/subordinate schema – Often first created during trauma u Surrender to the “higher power” of the voice may be helpful during trauma – But becomes a problem later on See "A Casebook of Cognitive Behaviour Therapy for Command Hallucinations: A Social Rank Theory Approach" by Byrne, S. , Birchwood, M. , Trower, P. , & Meaden

Common steps in therapy with command hallucinations: u Assess details, beliefs, habits u Work on beliefs that support appeasement & compliance – Establish that only something physical can hurt the body – Focus on the fact that voices and words are not physical – Point out voices rely on people to act, they just talk – Challenge the voice to hurt therapist – Establish the unreliability of the voices See "A Casebook of Cognitive Behaviour Therapy for Command Hallucinations: A Social Rank Theory Approach" by Byrne, S. , Birchwood, M. , Trower, P. , & Meaden

Role plays with voices u Therapist voice plays client, client plays the – Therapist responds in calm, detached, Socratic way u Then client plays a person the client likes & respects, therapist plays voice – Client practices calm detached response u Finally, voice client plays self, therapist plays See “Person-Based Cognitive Therapy for Distressing Psychosis” by Paul Chadwick, p. 101 -

Exercise/Role play u One person role plays a persecutory and commanding voice u the other person role plays a person responding to that voice – In a calm, detached, Socratic way – Be curious & friendly, but also selfrespecting u Notice & comment on any concerns that seem to underlie the comments of the voice

Interpret the destructive consequences of appeasement as proof that the best strategy is avoidance Decision is made to give in to or appease the emotion, impulse or voice, but the consequences are destructive Avoid a difficult emotion, impulse, or voice Never engaged with, the emotion, impulse or voice becomes larger, more intense, more autonomous Emotion, impulse, or voice finally breaks through barriers and is experienced as overwhelming

A Curious Option: Therapist Talking to the Voices u Explicitly talking directly to the voices may be helpful, to – Establish that a different way of relating to the voice is possible – Understand voice goals or viewpoints – Increase cooperation between adult self and voice u To meet joint, negotiated life goals One source: http: //www. en. transformationalpsychology. com/index. php? cmd=page&id=2676

Both being oblivious to metaphor and using metaphors without being aware they are metaphors may be trauma related u Metaphor can be an attempt to integrate perceptions that have as yet no words u The key to integrating metaphorical content is to see it as metaphor – partly fitting and partly not u But when things are polarized, it’s more likely the metaphor will be seen as – 100% literally true – or as nonsense
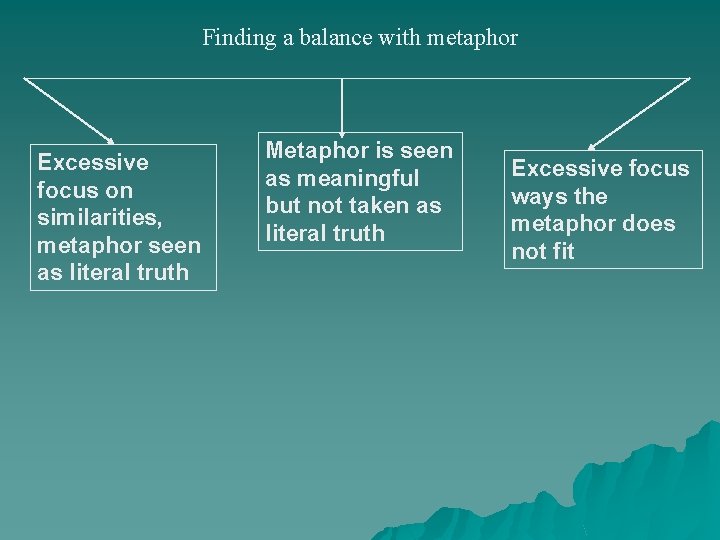
Finding a balance with metaphor Excessive focus on similarities, metaphor seen as literal truth Metaphor is seen as meaningful but not taken as literal truth Excessive focus ways the metaphor does not fit

Ways to work with psychotic content that may be metaphorical u Watch for themes – You can ask about possible experiences that relate to theme you detect u Just ask, “What other experiences in your life have been like that? u Or, for clients who are capable – Explain how the mind uses metaphor – Speculate together about what metaphorical meaning might be

Psychosis and Spirituality u Who are we…. – Beyond the way we are defined by our mundane context? u Mystical mental states involve letting go of one’s conventional orientation – Brain scan research confirms this u “The mystic swims in the same ocean in which the psychotic drowns. ” u Joseph Campbell said something like this.

Oscillating from too open-minded to too closed…. Excess dogma or fixed metaphor: Metaphor or mental content is taken as real, rather than as pointing at something else beyond it. Healthy dialogue between images & that which is beyond image: I can come up with metaphors, images and words for things, but also recognize that reality goes beyond those containers. Drowning in mysticism, lacking any metaphor: Seeing no metaphor for experience, no way to express it or put it into words or images, it is overwhelming.
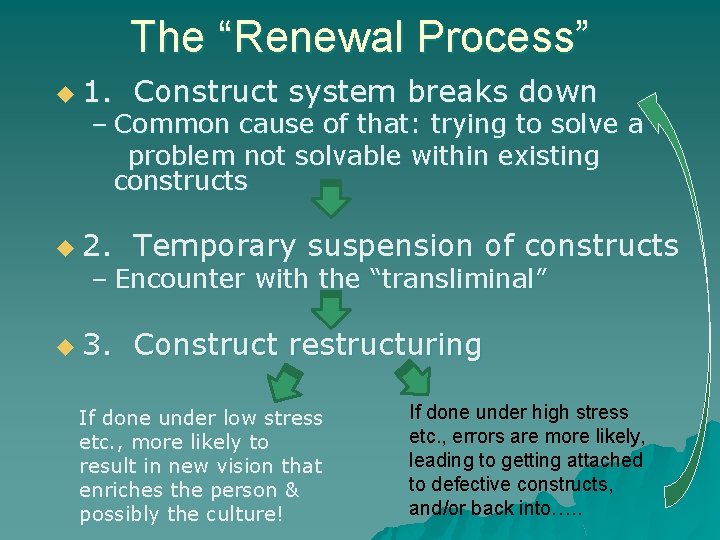
The “Renewal Process” u 1. Construct system breaks down u 2. Temporary suspension of constructs u 3. Construct restructuring – Common cause of that: trying to solve a problem not solvable within existing constructs – Encounter with the “transliminal” If done under low stress etc. , more likely to result in new vision that enriches the person & possibly the culture! If done under high stress etc. , errors are more likely, leading to getting attached to defective constructs, and/or back into…. .

DIALECTICAL BEHAVIOUR THERAPY: Linehan’s STATES OF MIND applied to PSYCHOSIS Slide by Isabel Clarke and Donna Rutherford

Rescripting: Step 1: Get a memory 1. Start with present problem and use affect (etc. ) to get childhood memory, or just get into known childhood situations directly u 2. Patient imagines safe place and then gets childhood memory u – what do you see, hear, smell, experience; what is happening? – what do you feel (emotionally)? – what do you think? – what do you need? u With trauma: not necessary to get whole trauma memory This & following 2 slides from “Imagery Rescripting as a Method to Change Emotional Memories & Schemata/Representations” by Arnoud Arntz of Maastricht University

Step 2: Change perspective to adult u 1. Ask patient to enter the scene as an adult u 2. Ask the patient: – what do you see, hear etc. What is happening? (look to the child!) – what do you feel (emotionally)? – what do you think? – what do you want to do? u 3. Prompt the patient to do this in fantasy – o. k. , do it! u 4. Then go back to 2 u 5. Just start again if patient is not satisfied

Step 3: Change perspective to child u u u 1. Ask patient to experience the rescripting by the adult-self as a child 2. Ask the patient: – – – what what do do do you you you see, hear etc. ; what is happening? feel (emotionally)? think? need? want to happen? 3. Prompt the patient to ask the adult to do what he/she needs: o. k. , ask it! 4. Then go back to 2 5. Until patient is satisfied (often after extra rescripting)

Paul, 54 years old u Early medical trauma & physical abuse – Learned to be hard on himself to cope u Used meth for 2 decades, then stopped u Then victim of assault (head injury) – Followed by disability u Voices emerged 6 years afterward

Formulation around intrusive thoughts and voices Brain injury and distress around disability led to re-traumatization & disorganization u Re-traumatization caused unwanted thoughts to emerge u Belief that unwanted thoughts were dangerous led to perceiving a need to eliminate them completely u Attempts to eliminate thoughts resulted in frustration & increased disorganization u Giving up thought control, and emphasizing life control, had better results u
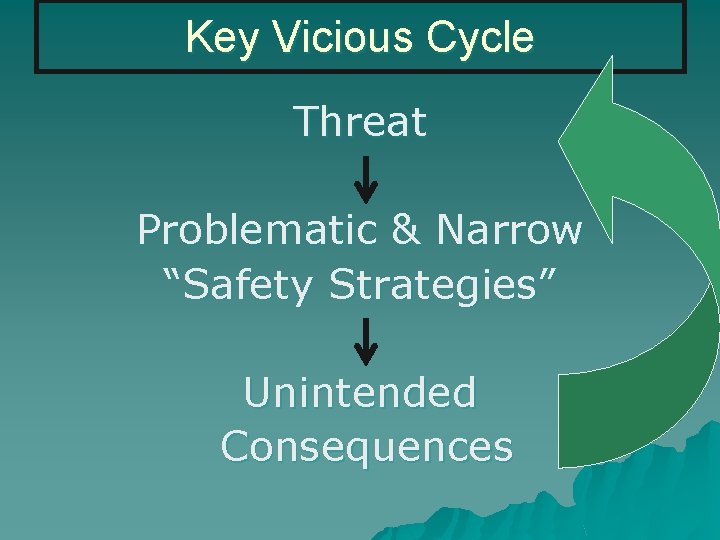
Key Vicious Cycle Threat Problematic & Narrow “Safety Strategies” Unintended Consequences
Key “Virtuous Cycle” Reduced Threat Balance of Risk Taking with Reasonable Precautions Positive Consequences

Discussion u As a result of this seminar, what are one or two innovations you plan to try out soon in your practice? – What barriers do you see to making important changes? u What supports etc. are available to help overcome those barriers?

Parting words…. May you have the commitment To heal what has hurt you To allow it to come close to you And, in the end, become one with you A Gaelic blessing
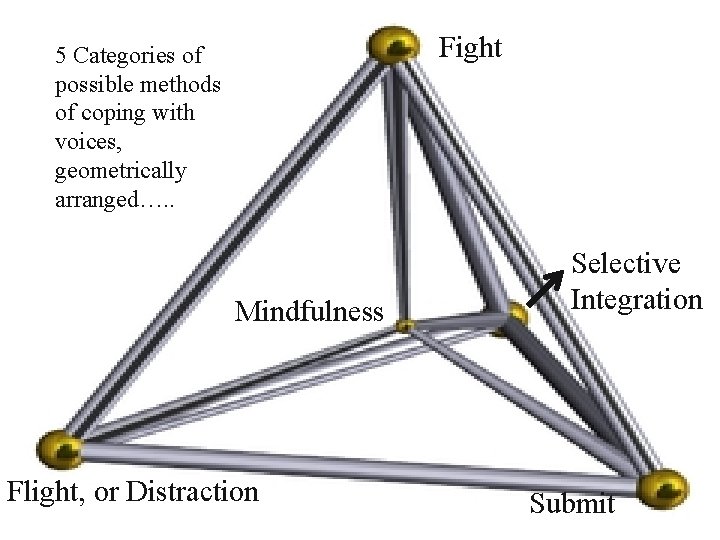
Fight 5 Categories of possible methods of coping with voices, geometrically arranged…. . Mindfulness Flight, or Distraction Selective Integration Submit

Pros and Cons of Fighting u Pro – Can be especially important when the voice is close to pushing the person into a way of seeing or behaving that is especially destructive u Con – Fighting can be exhausting, and often makes the person look “crazy” (yelling at the voices) – Fighting often results in further polarization, actually prolonging the voice problem

Pros and Cons of Flight, or Distraction u Pro: – Can make the problem seem to go away, with quick restoration of sense of wellbeing u Con: – While avoiding the experience of the voice, person often avoids or loses track of other aspect of person’s life as well – Avoiding the experience means failure to get more information about it, and creates a sense that one is not strong enough to handle it u Which is especially problematic when/if the experience eventually intrudes anyway

Pros and Cons of Submission u Pro: – It eases all the tension caused by fighting or avoiding – When voices are benign, this can give a person a sense of direction & spontaneity u Con: – If a person submits to a bad idea, harm can be done – The habit of submitting creates a sense of personal weakness

Pros and Cons of Mindfulness u Pro: – Calm is maintained, everything is faced, person is not overpowered, and the overall method is simple u Con: – When the voice is an indicator of a problem that needs to be addressed, but a person is just mindfully aware of it and doesn’t act, then the problem can be prolonged.

Pros and Cons of Selective Integration u Pro: – Person can take what is helpful from the voice and leave the rest – Leaves the person feeling competent u Con: – Can be a lot of work, take a lot of mental concentration and focus – Mistakes can be made, a person may inadvertently take in something that is not helpful, and/or leave out something that would be helpful.

u Anne – 34 yo, one son 14 yo – 8 yr hx psychiatry for psychosis u 5 u admissions – usually psychotic symptoms leading to overdose Symptoms: – Persecutory delusions of men in authority u Esp. men in uniform – They would do mind control u Read her mind through her eyes – Very distressing u Would call social worker several times per day for reassurance u When got worse, would OD or drink or quit self care – Also had "odd" memories of sexual abuse, wasn't sure they were true u Main current issue: – Wanted to deal with paranoia, authority figures – Also wanted to understand early memories
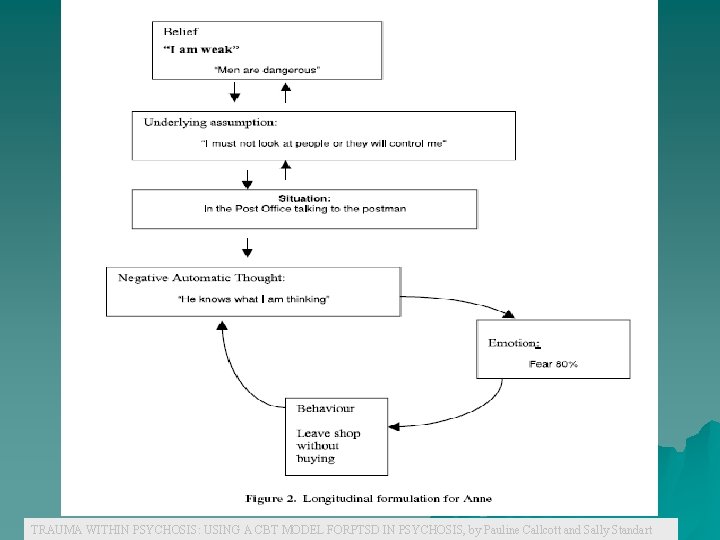
TRAUMA WITHIN PSYCHOSIS: USING A CBT MODEL FORPTSD IN PSYCHOSIS, by Pauline Callcott and Sally Standart
Overly risky behavior versus excess risk avoidance Overly risky behavior: I avoid noticing risks that are present, so I can feel free to move ahead in my life no matter what. Wise choices about what kinds of risks to take: I am thoughtful regarding which risks are best avoided and which risks it makes sense to take so I can move forward safely. Excess risk avoidance, or too many “safety behaviors”: I avoid danger even when risks are low compared to potential benefits, and this stops me from moving forward in my life.

Coping Strategies u No one option is best for all circumstances u Flexibility, fitting the best strategy to the circumstance, is key u A common problem is when someone relies too much on one or two methods, with little access to other methods – Recall the problem of “overdeveloped” and “underdeveloped” coping strategies.

Example of Creative/Psychotic Attempt to Heal u Thinking of one threat that is a metaphor for multiple or unthinkable threats – Then attempting to integrate by focusing on that u Shark on the ward u Backfires if take it literally, because then behavior & communication becomes “psychotic”
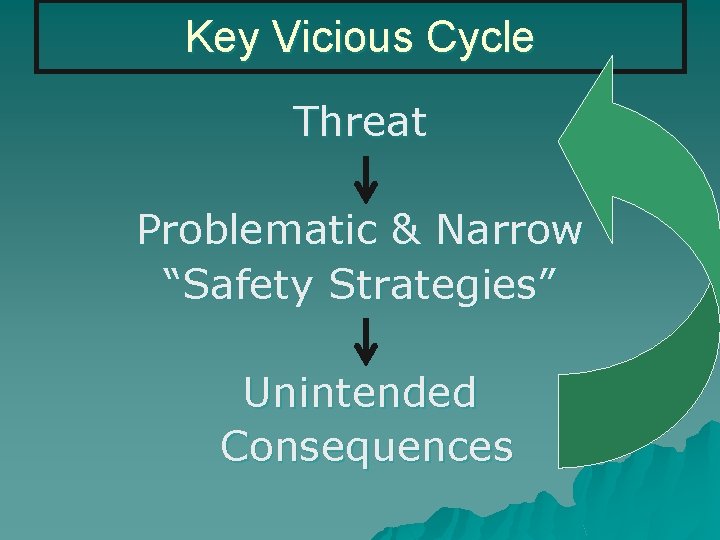
Key Vicious Cycle Threat Problematic & Narrow “Safety Strategies” Unintended Consequences
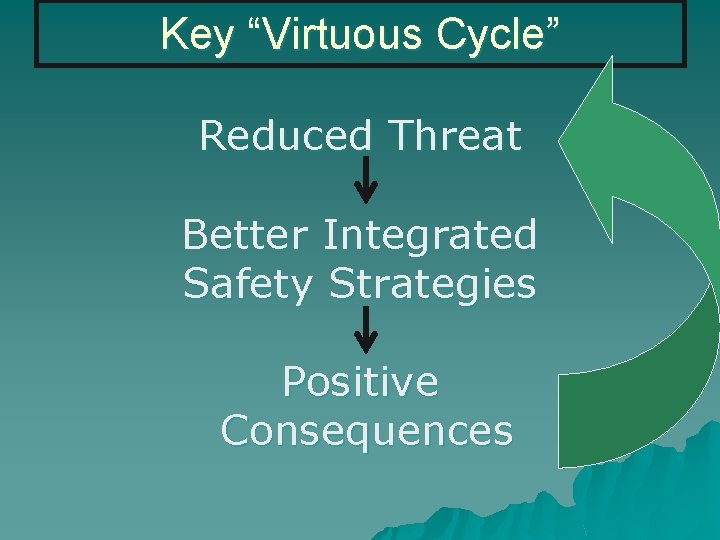
Key “Virtuous Cycle” Reduced Threat Better Integrated Safety Strategies Positive Consequences
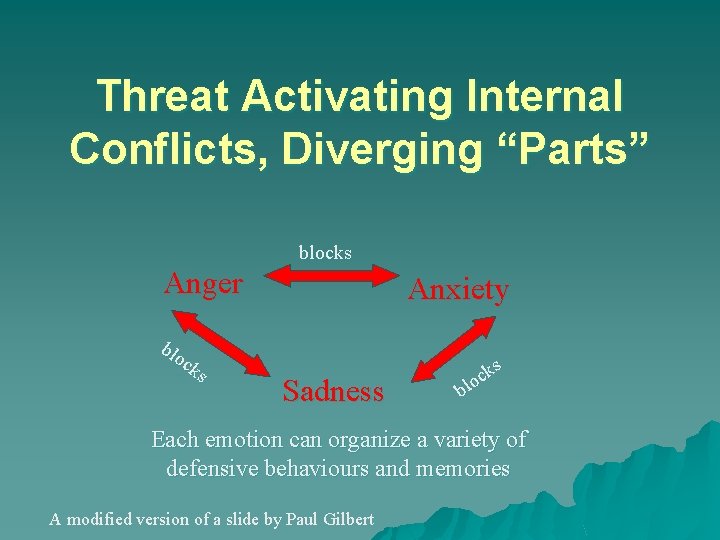
Threat Activating Internal Conflicts, Diverging “Parts” blocks Anger blo ck s Anxiety Sadness ks c blo Each emotion can organize a variety of defensive behaviours and memories A modified version of a slide by Paul Gilbert
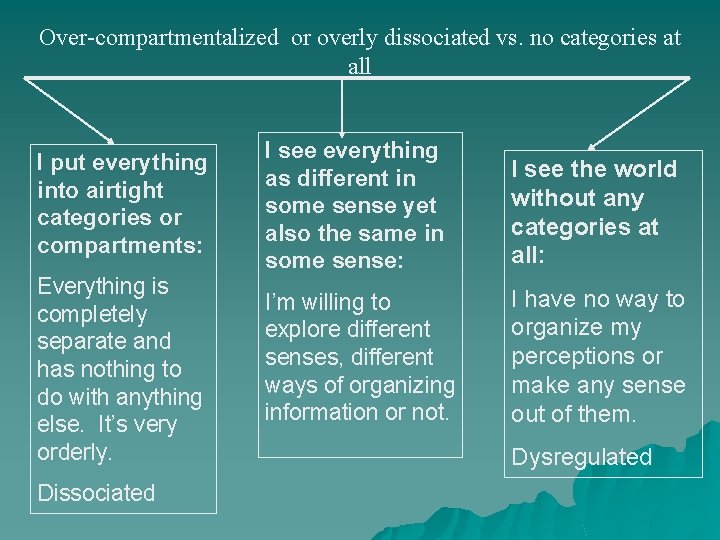
Over-compartmentalized or overly dissociated vs. no categories at all I put everything into airtight categories or compartments: Everything is completely separate and has nothing to do with anything else. It’s very orderly. Dissociated I see everything as different in some sense yet also the same in some sense: I see the world without any categories at all: I’m willing to explore different senses, different ways of organizing information or not. I have no way to organize my perceptions or make any sense out of them. Dysregulated
- Slides: 107