Transplantation Rejection in the Caribbean Prevention and Management

Transplantation Rejection in the Caribbean; Prevention and Management Vaughn Whittaker, MD, MPH, FACS 1 Immunology

Introduction • There is no published data on the incidence of rejection of transplanted patients in the Caribbean. • Transplant Programs are have limited volumes and no long term follow up data except in Trinidad. • Trinidad has experienced mostly antibody mediated rejection seen late in the post transplant phases, typically 10 years post transplant. This leads typically to graft failure

Introduction: An ounce of Prevention… • I will focus my remarks on understanding the phenomenon of rejection and the unique characteristics of Caribbean population. • I will also address preventive and management strategies. • The adage an ounce of prevention is worth a pound of cure is very important.

Challenges in Caribbean • Access to powerful antibody based immunosuppression for induction such as thymoglobulin related to cost and resource availability • Reduced access to standard therapeutic drugs such prograf, belatacept • Reduced access to screening test to properly evaluate for donor specific antibodies (DSA) to monitor developing antibodies • Inconsistent availability of drugs • Lack of sufficient immunological support to guide therapy in patients.

Challenges • Not detecting through screening donor specific antibodies can lead to development of antibody mediated rejection. • Cell mediated rejection may occur due to insufficient dosing of medications. Patients of African descent has been shown to require higher doses of prograf in order to achieve the same therapeutic levels as Caucasians.
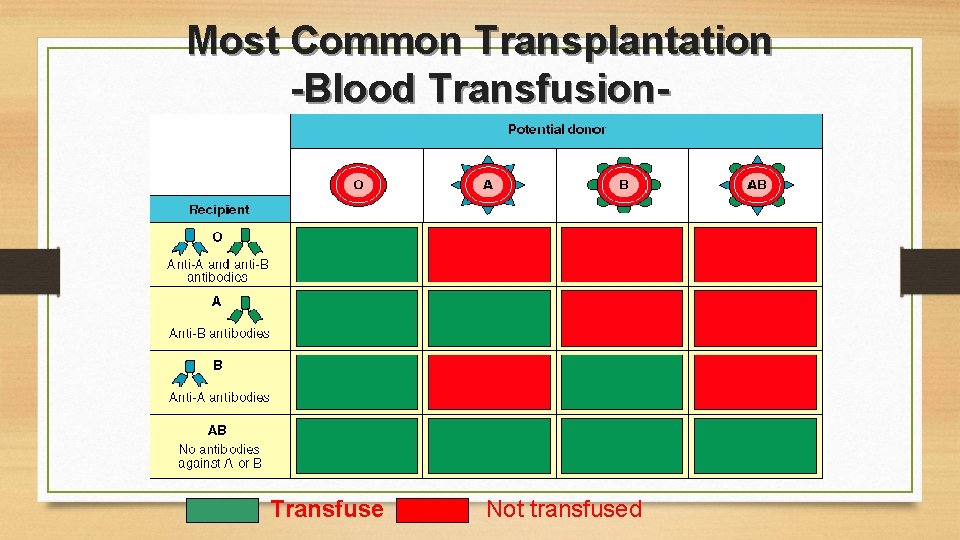
Most Common Transplantation -Blood Transfusion- Transfuse Not transfused

Transplantation antigens • Major histocompatibility antigens (MHC molecules) • Minor histocompatibility antigens • Other alloantigens Immunology 2006 -7 year 7

Major histocompatibility antigens • Main antigens of grafts rejection • Cause fast and strong rejection • Difference of HLA types is the main cause of human grafts rejection Immunology 2006 -7 year 8

Minor histocompatibility antigens • Also cause grafts rejection, but slow and weak • Mouse H-Y antigens encoded by Y chromosome • HA-1~HA-5 linked with non-Y chromosome Immunology 2006 -7 year 9

The Immunology of Allogeneic Transplantation • Recognition of transplanted cells that are self or foreign is determined by polymorphic genes (MHC) that are inherited from both parents and are expressed codominantly. • Alloantigens elicit both cell-mediated and humoral immune responses.

Effector Mechanisms of Allograft Rejection • Hyperacute Rejection • Acute Rejection • Chronic Rejection

Mechanism of allograft rejection • Cell-mediated • Humoral Immunity or antibody mediated • Role of NK cells Immunology 2006 -7 year 12
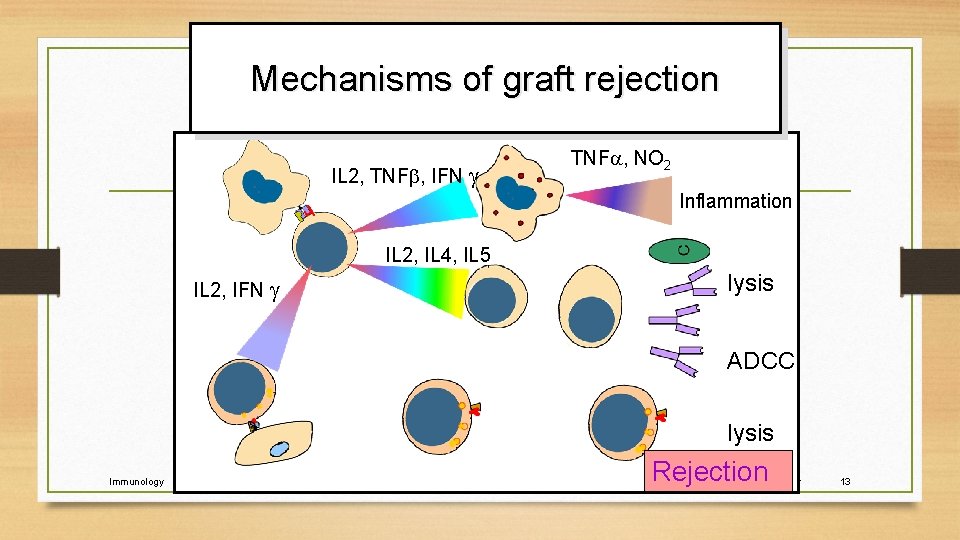
Mechanisms of graft rejection IL 2, TNF , IFN TNF , NO 2 Inflammation IL 2, IL 4, IL 5 IL 2, IFN lysis ADCC lysis Immunology Rejection 2006 -7 year 13

Immunology of Transplant Rejection Components of the Immune system involved in graft Rejection : 1) Antigen presenting cells – • • • Dendritic cells Macrophages Activated B Cells 2) B cells and antibodies – • • Preformed antibodies Natural antibodies Preformed antibodies from prior sensatization Induced antibodies 3) T cells 4) Other cells – • • • Natural killer cells T cells that express NK cell – associated Markers Monocytes/Macrophages
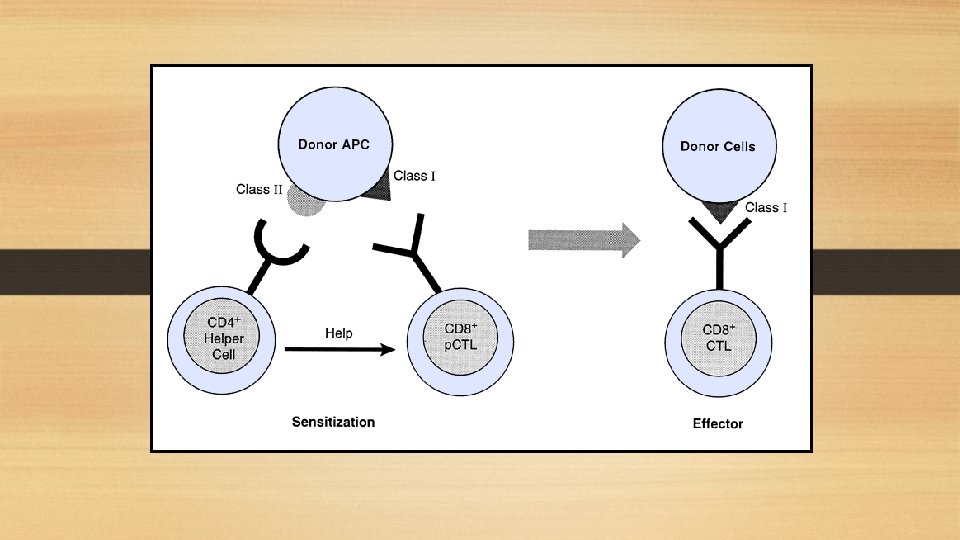
15 Immunology 20067 year

+ + Role of CD 4 and CD 8 T Cells • CD 4+ differentiate into cytokine producing effector cells • Damage graft by reactions similar to DTH • CD 8+ cells activated by direct pathway kill nucleated cells in the graft • CD 8+ cells activated by the indirect pathway are self MHC-restricted
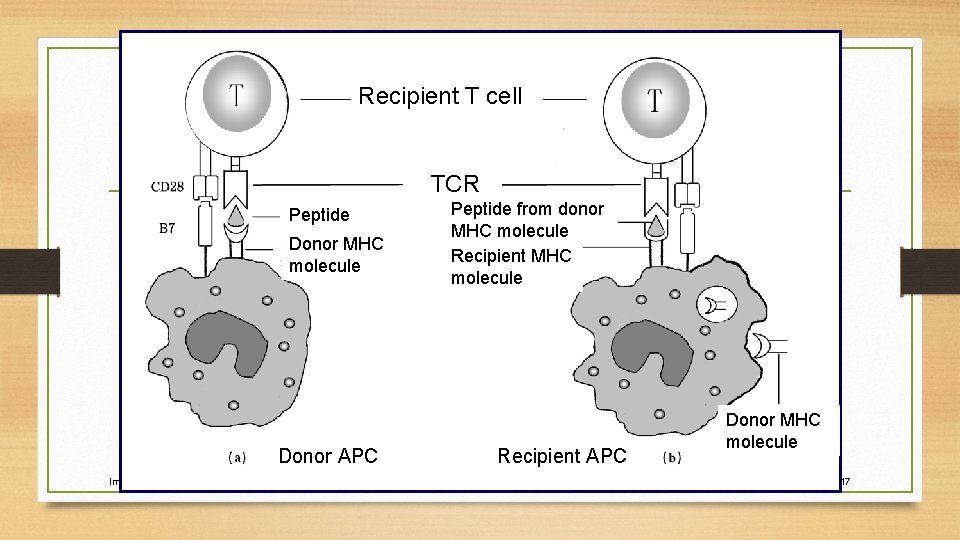
Recipient T cell TCR Peptide Donor MHC molecule Donor APC Immunology Peptide from donor MHC molecule Recipient APC Donor MHC molecule 2006 -7 year 17

Activation of Alloreactive T cells and Rejection of Allografts • Donor APCs migrate to regional lymph nodes and are recognized by the recipient’s TH cells. • Alloreactive TH cells in the recipient induce generation of TDTH cell and CTLs then migrate into the graft and cause graft rejection.

Hyperacute Rejection • Characterized by thrombotic occlusion of the graft • Begins within minutes or hours after anastomosis • Pre-existing antibodies in the host circulation bind to donor endothelial antigens • Activates Complement Cascade • Xenograft Response
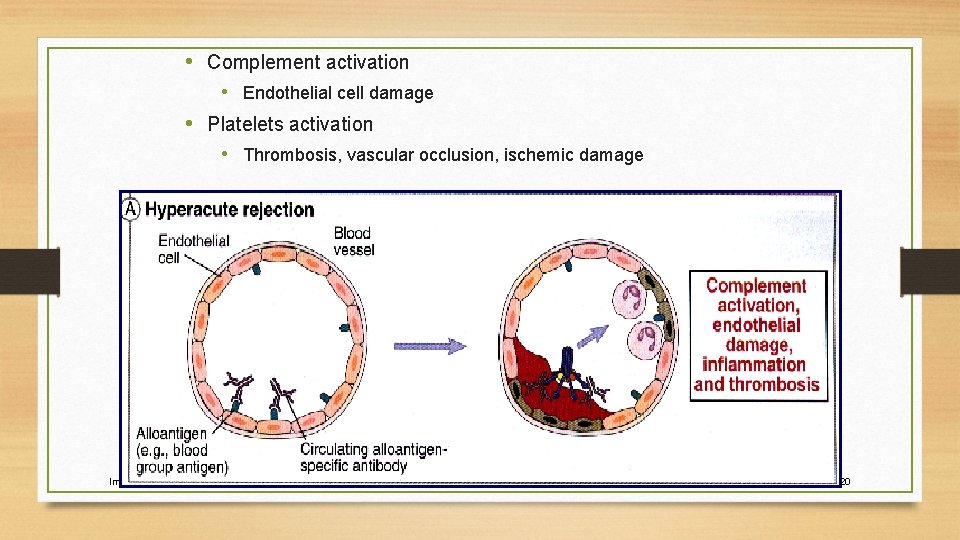
• Complement activation • Endothelial cell damage • Platelets activation • Thrombosis, vascular occlusion, ischemic damage Immunology 2006 -7 year 20

• Mechanisms • Preformed antibodies • Antibody against ABO blood type antigen • Antibody against VEC antigen • Antibody against HLA antigen Immunology 2006 -7 year 22

Acute Rejection • Vascular and parenchymal injury mediated by T cells and antibodies that usually begin after the first week of transplantation if there is no immunosuppressant therapy • Incidence as high as (30%) for the first 90 days but with adequate immunosuppression less than 5 -10%
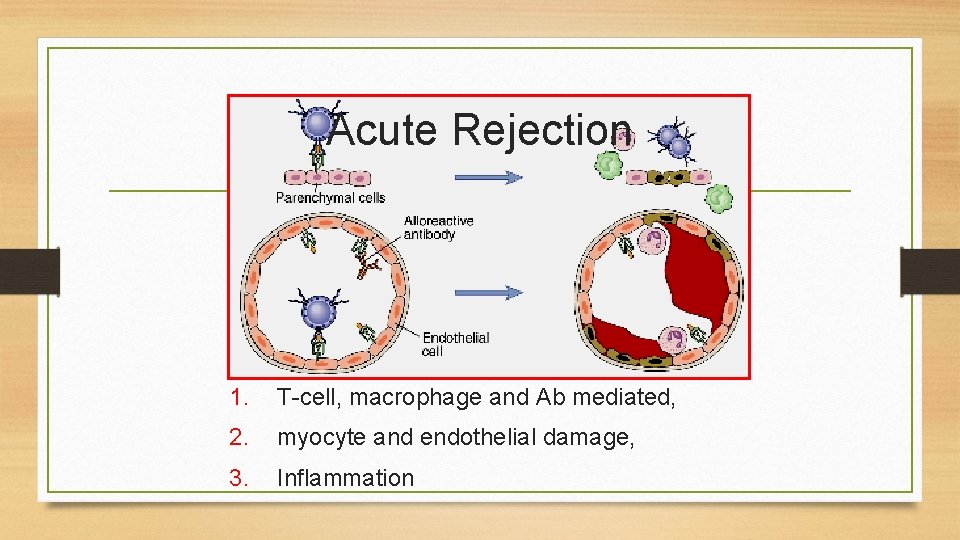
Acute Rejection 1. T-cell, macrophage and Ab mediated, 2. myocyte and endothelial damage, 3. Inflammation

Chronic Rejection • Occurs in most solid organ transplants • • Heart Kidney Lung Liver • Characterized by fibrosis and vascular abnormalities with loss of graft function over a prolonged period.
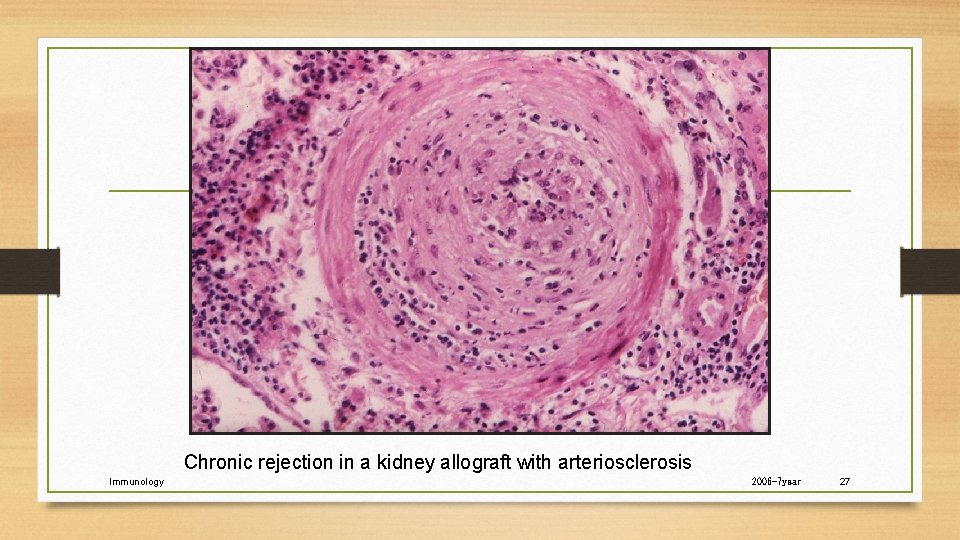
Chronic rejection in a kidney allograft with arteriosclerosis Immunology 2006 -7 year 27
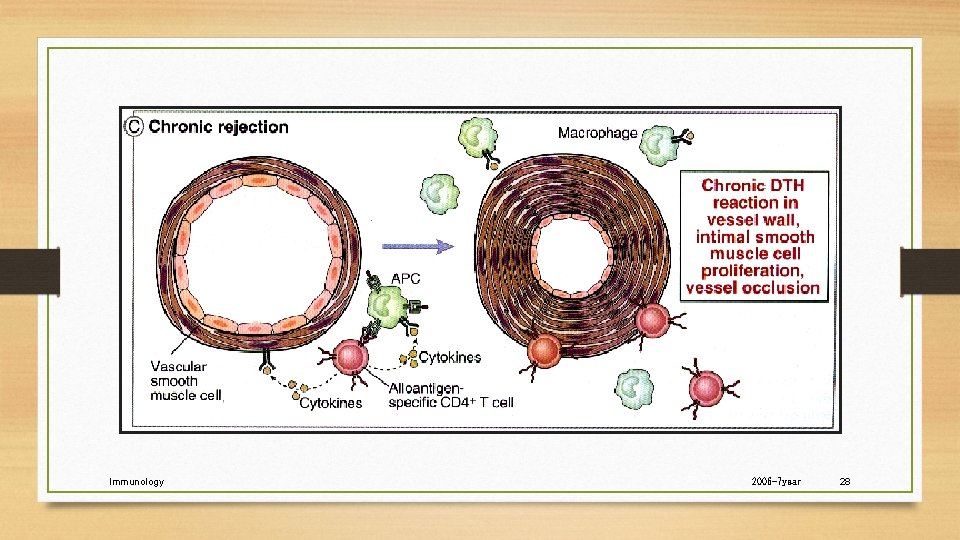
Immunology 2006 -7 year 28
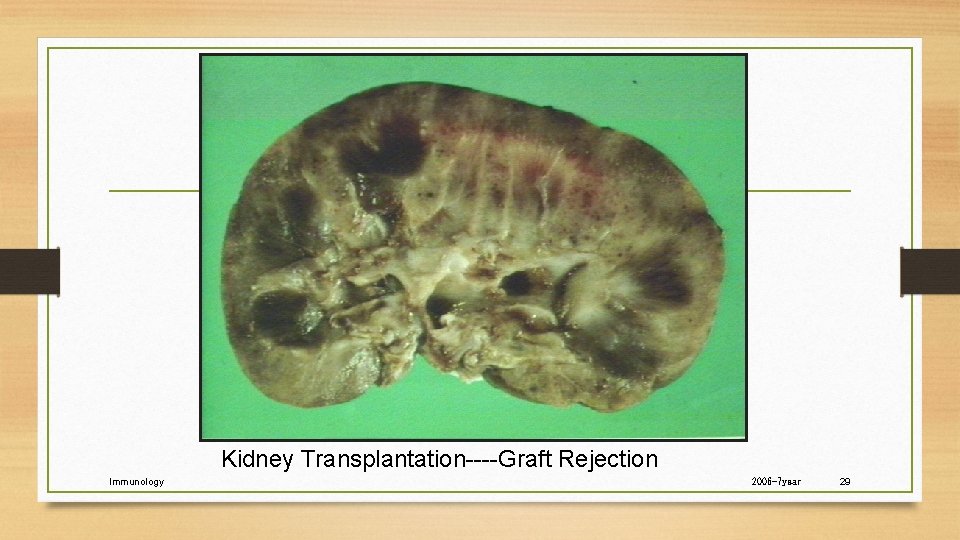
Kidney Transplantation----Graft Rejection Immunology 2006 -7 year 29

Prevention and Therapy of Allograft Rejection in Caribbean 30 Immunology 20067 year

Preventative Strategies • Tissue Typing: HLA A, B, DR, DQ • Immunosuppressive Therapy: Prograf, Mycophenolate, Steroids • Induction of Immune Tolerance Immunology 2006 -7 year 31

Tissue Typing • ABO and Rh blood typing • Crossmatching (Preformed antibodies) • HLA typing • HLA-A and HLA-B • HLA-DR Immunology 2006 -7 year 32

Immunosuppressive Therapy • Prograf levels 10 -12 ng/m. L , Cyclosporine(Cs. A)( calcineurin • • Immunology inhibitors) • Inhibit NFAT transcription factor Monoclonals such as Basiliximab Mycophenolate Mofitil ( Cellcept), Azathioprine • Block the proliferation of lymphocytes Ab against T cell surface molecules • Anti-CD 3 m. Ab----Deplete T cells eg Thymoglobulin • Costimulatory Blockade agents such as Belatacept Anti-inflammatory agents • Corticosteroids----Block the synthesis and secretion of cytokines 2006 -7 year 33

Banff Classification 2007 • Adequate sample: 2 cores with at least 10 glomeruli and 2 arteries • Should be stained for C 4 d to detect presence of antibody mediated rejection • • Results could be 1. Normal—no rejection Antibody mediated rejection C 4 d deposition: acute or chronic active Borderline changes suspicious for acute T cell mediated rejection which is further subclassified
T cell mediated Rejection • Type 1 A; significant interstitial infiltration (>25% parenchymal involvement, i 2, i 3 foci of moderate tubilitis t 2 • Type 1 B; significant interstitial infiltration (>25% and foci severe tubilitis t 3) • Type IIA: mild to moderate intimal arteritis V 1 • Type IIB: severe intimal arteritis >25% luminal area V 2 • Type III: transmural arteritis, arterial fibrinoid changes, necrosis of medial smooth muscle cells, accompanying lymphocytic inflammation

Chronic active T cell mediated rejection • Chronic allograft arteriopathy, arterial intimal fibrosis with mononuclear cells infiltration in fibrosis, formation of neointima. • Am J Transplant 2012; 563

Banff Classification 2017 Acute TCMR • Banff Criteria • Acute T Cell Rejection Grade IA Interstitial inflammation involving >25% of nonsclerotic cortical parenchyma (i 2 or i 3) with moderate tubulitis (t 2) involving 1 or more tubules, not including tubules that are severely atrophice Grade IB Interstitial inflammation involving >25% of nonsclerotic cortical parenchyma (i 2 or i 3) with severe tubulitis (t 3) involving 1 or more tubules, not including tubules that are severely atrophice Grade IIAc Mild to moderate intimal arteritis (v 1), with or without interstitial inflammation and/or tubulitis Grade IIBc Severe intimal arteritis (v 2), with or without interstitial inflammation and/or tubulitis Grade IIIc Transmural arteritis and/or arterial fibrinoid necrosis of medial smooth muscle with accompanying mononuclear cell intimal arteritis (v 3), with or without interstitial inflammation and/or tubulitis

Banff Classification 2017 Chronic Active TCMR Grade IA Interstitial inflammation involving >25% of the total cortex (ti score 2 or 3) and >25% of the sclerotic cortical parenchyma (i‐IFTA score 2 or 3) with moderate tubulitis (t 2) involving 1 or more tubules, not including severely atrophic tubules e ; other known causes of i‐IFTA should be ruled out Grade IB Interstitial inflammation involving >25% of the total cortex (ti score 2 or 3) and >25% of the sclerotic cortical parenchyma (i‐IFTA score 2 or 3) with severe tubulitis (t 3) involving 1 or more tubules, not including severely atrophic tubules e ; other known causes of i‐IFTA should be ruled out Grade II c Chronic allograft arteriopathy (arterial intimal fibrosis with mononuclear cell inflammation in fibrosis and formation of neointima) Chronic Active T cell Medicated Rejection

Banff Classification: Antibody Mediated Rejection-Active ABMR; all 3 criteria must be met for diagnosis • 1. Histologic evidence of acute tissue injury, including 1 or more of the following: Microvascular inflammation (g > 0 and/or ptc > 0), in the absence of recurrent or de novo glomerulonephritis, although in the presence of acute TCMR, borderline infiltrate, or infection, ptc ≥ 1 alone is not sufficient and g must be ≥ 1 • Intimal or transmural arteritis (v > 0)c • Acute thrombotic microangiopathy, in the absence of any other cause • Acute tubular injury, in the absence of any other apparent cause • 2. Evidence of current/recent antibody interaction with vascular endothelium, including 1 or more of the following: Linear C 4 d staining in peritubular capillaries (C 4 d 2 or C 4 d 3 by IF on frozen sections, or C 4 d > 0 by IHC on paraffin sections) • At least moderate microvascular inflammation ([g + ptc] ≥ 2) in the absence of recurrent or de novo glomerulonephritis, although in the presence of acute TCMR, borderline infiltrate, or infection, ptc ≥ 2 alone is not sufficient and g must be ≥ 1 • Increased expression of gene transcripts/classifiers in the biopsy tissue strongly associated with ABMR, if thoroughly validated 3. Serologic evidence of donor ‐specific antibodies (DSA to HLA or other antigens). C 4 d staining or expression of validated transcripts/classifiers as noted above in criterion 2 may substitute for DSA; however thorough DSA testing, including testing for non‐HLA antibodies if HLA antibody testing is negative, is strongly advised whenever criteria 1 and 2 are met

Banff Classification: Antibody Mediated Rejection- Chronic Active Chronic active ABMR; all 3 criteria must be met for diagnosis c • 1. Morphologic evidence of chronic tissue injury, including 1 or more of the following: Transplant glomerulopathy (cg >0) if no evidence of chronic TMA or chronic recurrent/de novo glomerulonephritis; includes changes evident by electron microscopy (EM) alone (cg 1 a) • Severe peritubular capillary basement membrane multilayering (requires EM)c • Arterial intimal fibrosis of new onset, excluding other causes; leukocytes within the sclerotic intima favor chronic ABMR if there is no prior history of TCMR, but are not required 2. Identical to criterion 2 for active ABMR, above 3. Identical to criterion 3 for active ABMR, above, including strong recommendation for DSA testing whenever criteria 1 and 2 are met C 4 d Staining without Evidence of Rejection; all 4 features must be present for diagnosisd 1. Linear C 4 d staining in peritubular capillaries (C 4 d 2 or C 4 d 3 by IF on frozen sections, or C 4 d>0 by IHC on paraffin sections) 2. Criterion 1 for active or chronic, active ABMR not met 3. No molecular evidence for ABMR as in criterion 2 for active and chronic, active ABMR 4. No acute or chronic active TCMR, or borderline changes Category 3: Borderline changes Suspicious (Borderline) for acute TCMR Foci of tubulitis (t > 0) with minor interstitial inflammation (i 0 or i 1), or moderate‐severe interstitial inflammation (i 2 or i 3) with mild (t 1) tubulitis; retaining the i 1 threshold for borderline with t > 0 is permitted although this must be made transparent in reports and publications No intimal or transmural arteritis (v = 0)
The Banff 2017 Kidney Meeting Report: Revised diagnostic criteria for chronic active T cell–mediated rejection, antibody‐mediated rejection, and prospects for integrative endpoints for next‐generation clinical trials American Journal of Transplantation, Volume: 18, Issue: 2, Pages: 293 -307, First published: 15 December 2017, DOI: (10. 1111/ajt. 14625)
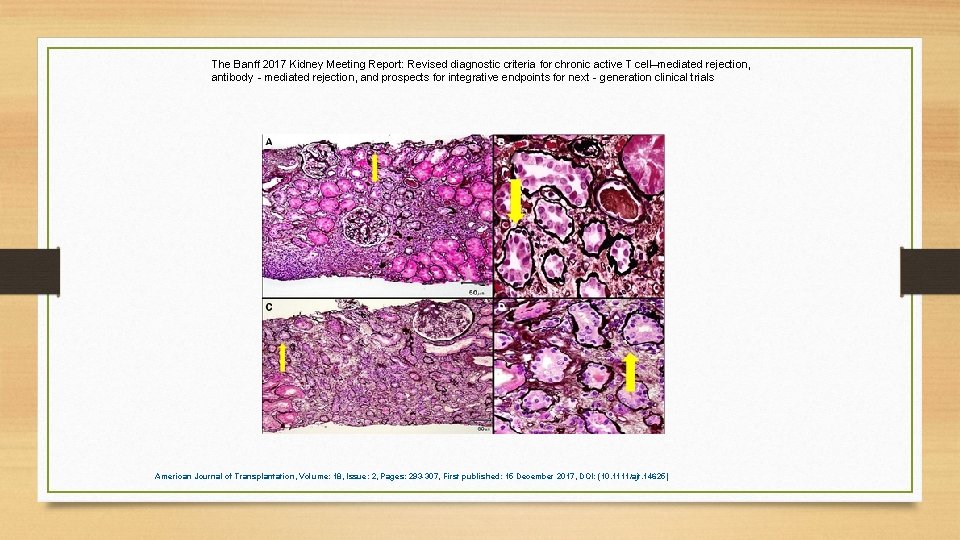
The Banff 2017 Kidney Meeting Report: Revised diagnostic criteria for chronic active T cell–mediated rejection, antibody‐mediated rejection, and prospects for integrative endpoints for next‐generation clinical trials American Journal of Transplantation, Volume: 18, Issue: 2, Pages: 293 -307, First published: 15 December 2017, DOI: (10. 1111/ajt. 14625)

Treatment: Antibody mediated rejection • • Normal Histology-No treatment Plasmapheresis with IVIG 100 mg/kg every other day As many as 5 -10 treatments maybe needed Check fibrinogen level and if less than 150 or 100 depending on center, administer cryoprecipitate • After each plasmapheresis check donor specific antibody levels with goal to get the titer to less than 1: 8 or crossmatch is negative • Rituximab or Bortezemab may be added to this regimen

Treatment of Cell mediated Rejection • 1 A: Pulsed steroids ---Solumedrol 500 mg per day x 3, followed by steroid taper • 1 B: Pulsed steroid followed by biologic agent such as Thymoglobulin 1. 5 mg/kg x 3 doses • IIA and IIB are treated the same way • III usually represents terminal rejection and is not usually salvageable.

Summary • Rejection is often a feared complication of transplantation • It is mostly preventable with current modern immunosuppressive protocols that involve antibody induction and maintenance immunosuppression • Prevention by screening for antibodies and drug levels are important strategies to prevent rejection • Rejection can be fully reversed if caught early and treated aggressively • Multidisciplinary team approach by patient educator, immunologist and renal pathologists helps to manage these complications well.

Thank You • Questions
- Slides: 44