Translating Research into Practice Diana HankeyUnderwood MS WHNPBC

Translating Research into Practice Diana Hankey-Underwood, MS, WHNP-BC, CRNP 1 st International Conference on Nursing Care Astana, Kazakhstan

RESEARCH/DEVELOPMENTS Chicago conference Innovating for Continence. International attendees share ideas and new technologies to help people with Incontinence.

What is Incontinence We can leak urine, gas, stool, mucous or blood. Words used in an English medical office are: Urinary incontinence Bowel, anal or fecal or faecal incontinence Bloody or mucous discharge

Common Emotional Reactions Personal Shame Societal Taboo Depression, Anger Withdrawal, Isolation

Stories your patients believe

According to Research, What do clients with incontinence want? Make “seeking help easier”, Make day-to-day life more manageable, Help finding out total costs, More knowledge about causes and the effects of lifestyle. Quality of life was considered by far the most important outcome.

Patients think the worse thing would be to have an embarrassing episode Research shows that the worst thing would be A fall while rushing to toilet Skin breakdown, Isolation and shame

BASHFUL The practical daily aspects of how to stay clean, the emotional aspects of embarrassment and anxiety, loss of a sense of independence; issues of femininity and masculinity, the mental aspects of confusion over who to tell and when, and how to continue to have a normal life are draining. How do I know? Because research says so!

Emotions • For a few people, there is also a spiritual aspect, if the distress becomes so significant that it interferes with their relationship with others. Grumpy

Effective Coping & Communication Finding the way from Grumpy to Happy

Design of Patient Assessments • Creation of Bladder Diary & Assessments • Consideration of outcome measurements 11
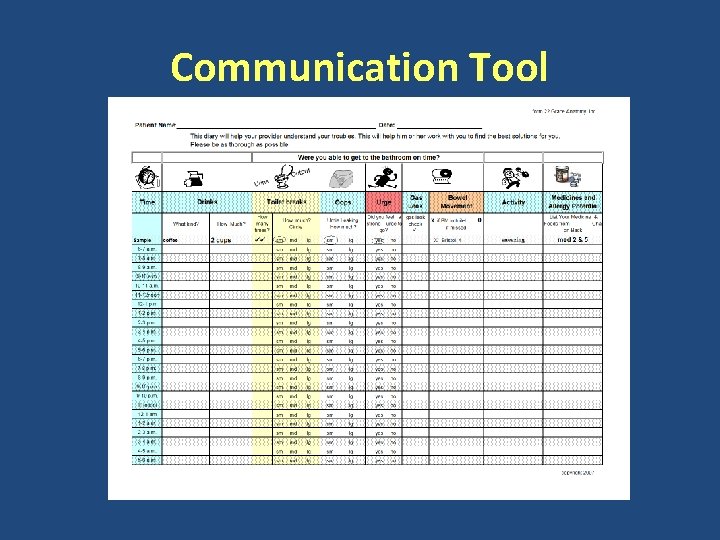
Communication Tool

A useful research tool

Am I the only one? Urinary Incontinence is COMMON. It affects 38% of women over the age of 60. Many men have to deal with it after prostate cancer treatment VERY common after stroke. 16% of the men and women who have urinary incontinence ALSO suffer from fecal incontinence. 50% of younger women deal with this for about 5 years after each birth. Half of these can be cured with lifestyle changes, others can improve quality of life tremendously even with non invasive means.

What is common is not always normal Having poor eyesight is common. Should this doctor get his eyes corrected, or try to hide the fact that his eyes are ‘not working perfectly? ” Reality: We can’t correct everyone’s eyes to 100%, but we can make dramatic improvements in almost everyone’s eyes. The same is true with incontinence!
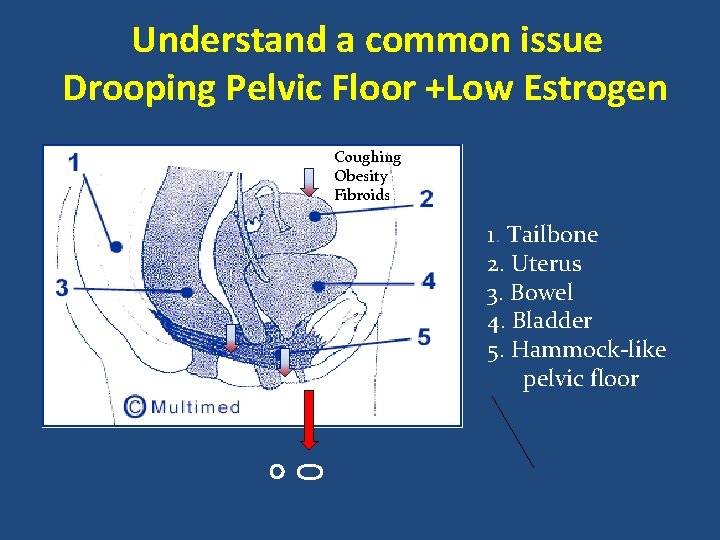
Understand a common issue Drooping Pelvic Floor +Low Estrogen Coughing Obesity Fibroids 1. Tailbone 2. Uterus 3. Bowel 4. Bladder 5. Hammock-like pelvic floor 0

Pessary Use • A pessary can lift the uterus and put a little pressure against the urethra to give it the right angle to close it. • Pessaries have been used since ancient times, and work surprisingly well. • The are soft and some are designed to stay in place during sex, others are designed to come out just like contact lenses.

Learn About Non Invasive Treatments Pelvic floor exercises- Kegels & Rolls; Biofeedback Weighted Cones; Products; Magnet, etc. Pessaries Diet Modifications Medications Lifestyle Modifications/Medication Routines Timed Voiding & Bladder Training (handout) Electrical Stimulation 9/25/2020 18

New for Urinary Incontinence 19
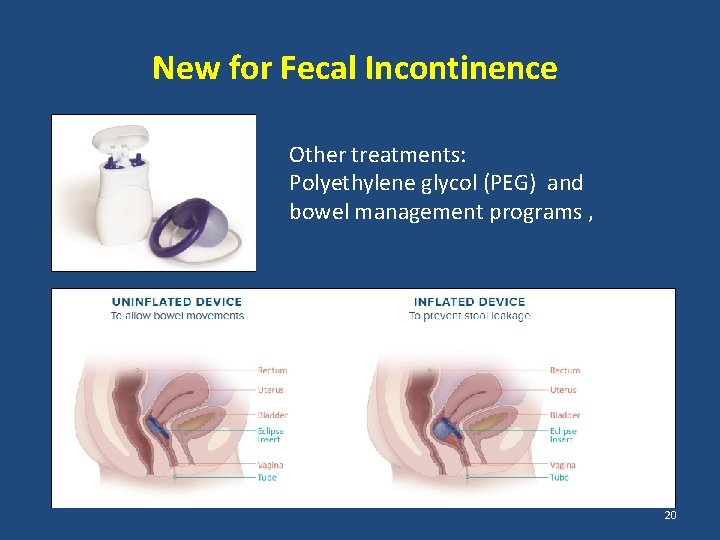
New for Fecal Incontinence Other treatments: Polyethylene glycol (PEG) and bowel management programs , 20

- Slides: 21