Translating Evidence Based Medicine to Evidence Based Practice

Translating Evidence Based Medicine to Evidence Based Practice! Roger F. Soll, MD H. Wallace Professor of Neonatology Larner College of Medicine, University of Vermont Coordinating Editor, Cochrane Neonatal Vice President, Vermont Oxford Network Trusted evidence. Informed decisions. Better health. 1

Use the chat feature to engage with the faculty by sending questions and comments to “Everyone”. Click this button: Select “Everyone” Type in your question Press Enter/Return

Guest Discussants Danielle Ehret, MD, MPH Associate Professor, University of Vermont Director, Global Health, Vermont Oxford Network Deirdre O'Reilly, MD, MPH Associate Professor, University of Vermont Director, NPM Fellowship, University of Vermont

Guest Discussants Gary M. Weiner, MD, FAAP Associate Professor, Pediatrics and Communicable Diseases Director, Neonatal-Perinatal Medicine Fellowship Training Program University of Michigan Health System/C. S. Mott Children’s Hospital

Guest Discussants Myra Wyckoff, M. D. Professor of Pediatrics UT Southwestern Medical Center

Sponsors Section on Neonatal-Perinatal Medicine

Translating Evidence Based Medicine To Evidence Based Practice! Roger F. Soll, M. D. is the Vice President of the Vermont Oxford Network and the Coordinating Editor of Cochrane Neonatal No other relevant financial issues to disclose

Translating Evidence Based Medicine To Evidence Based Practice! To develop an understanding of the strengths and weaknesses of evidence provided by systematic reviews and meta-analyses to inform our practice of neonatal-perinatal medicine. Today’s session specifically focuses on how evidence is translated to guidelines and recommendations
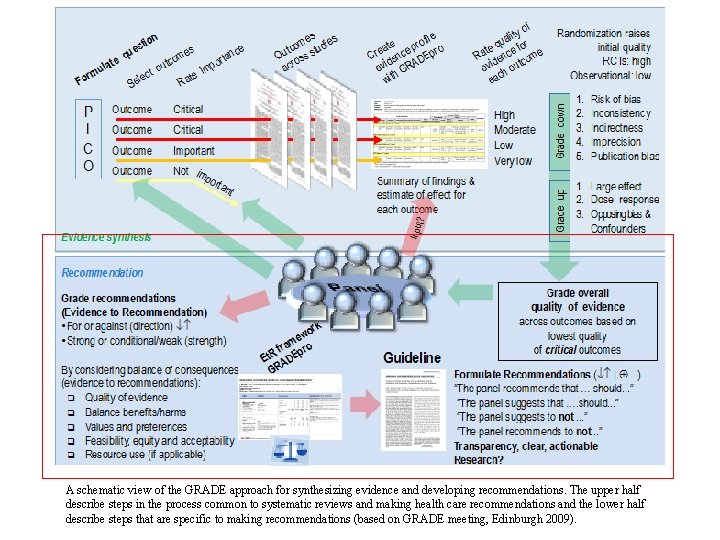
A schematic view of the GRADE approach for synthesizing evidence and developing recommendations. The upper half describe steps in the process common to systematic reviews and making health care recommendations and the lower half describe steps that are specific to making recommendations (based on GRADE meeting, Edinburgh 2009).

The strength of a recommendation reflects the extent to which a guideline panel is confident that desirable effects of an intervention outweigh undesirable effects across the range of patients for whom the recommendation is intended.

• Strong Recommendation: benefits outweigh risks of the intervention • Weak Recommendation: most informed people would chose this recommendation, but a substantial number would not

Strength of recommendation on a continuum: categorical terminology Strong Against Weak For Strong For continuum Only in Research Strength of recommendation: a continuum divided into categories

Evidence to Decision Table Problem: Is the problem a priority? Benefits and Harms • Desirable Effects: How substantial are the desirable anticipated effects? • Undesirable Effects: How substantial are the undesirable anticipated effects? Certainty of evidence: What is the overall certainty of the evidence of effects? Outcome importance: Is there important uncertainty about or variability in how much people value the main outcomes? Balance of effects: Does the balance between desirable and undesirable effects favor the intervention or the comparison? Resource Use: Does the cost-effectiveness of the intervention (the out-of-pocket cost relative to the net benefits) favor the intervention or the comparison? Acceptability: Is the intervention acceptable to key stakeholders? Feasibility: Is the intervention feasible to implement? Equity: What would be the impact on health equity?

The evolving landscape of evidence-based care in the delivery room

Part 7: Neonatal Resuscitation: 2015 International Consensus on Cardiopulmonary Resuscitation and Emergency Cardiovascular Care Science With Treatment Recommendations. Perlman JM, Wyllie J, Kattwinkel J, Wyckoff MH, Aziz K, Guinsburg R, Kim HS, Liley HG, Mildenhall L, Simon WM, Szyld E, Tamura M, Velaphi S; on behalf of the Neonatal Resuscitation Chapter Collaborators. Circulation. 2015; 132(suppl 1): S 204–S 241.

Use of oxygen in preterm infants Administration of Oxygen to Preterm Newborns 2015: Resuscitation of preterm newborns of < 35 weeks’ gestation should be initiated with low oxygen (21% to 30%) and the oxygen concentration should be titrated to achieve a preductal oxygen saturation approximating the interquartile range measured in healthy term infants after vaginal birth at sea level. Initiating resuscitation of preterm newborns with high oxygen (65% or greater) is not recommended. This recommendation reflects a preference for not exposing preterm newborns to additional oxygen without data demonstrating a proven benefit for important outcomes. Why: Data are now available from a meta-analysis of 7 randomized studies demonstrating no benefit in survival to hospital discharge, prevention of bronchopulmonary dysplasia, intraventricular hemorrhage, or retinopathy of prematurity when preterm newborns (less than 35 weeks of gestation) were resuscitated with high (65% or greater) compared with low (21% to 30%) oxygen concentration. https: //eccguidelines. heart. org/index. php/circulation/cpr-ecc-guidelines-2/part 13 -neonatal-resuscitation/

Initial Oxygen Use for Preterm Newborn Resuscitation: A Systematic Review With Meta-analysis. Welsford M, Nishiyama C, Shortt C, Weiner G, Roehr CC, Isayama T, Dawson JA, Wyckoff MH, Rabi Y; International Liaison Committee on Resuscitation Neonatal Life Support Task Force. Pediatrics. 2019 Jan; 143(1). pii: e 20181828. doi: 10. 1542/peds. 2018 -1828.

Initial Oxygen Use for Preterm Newborn Resuscitation: A Systematic Review With Meta-analysis. CONTEXT: The International Liaison Committee on Resuscitation prioritized to review the initial fraction of inspired oxygen (Fi. O 2) during the resuscitation of preterm newborns. OBJECTIVES: This systematic review and meta-analysis provides the scientific summary of initial Fi. O 2 in preterm newborns (< 35 weeks' gestation) who receive respiratory support at birth. DATA SOURCES: Medline, Embase, Evidence-Based Medicine Reviews, and Cumulative Index to Nursing and Allied Health Literature were searched between January 1, 1980 and August 10, 2018. Welsford M, Nishiyama C, Shortt C, Weiner G, Roehr CC, Isayama T, Dawson JA, Wyckoff MH, Rabi Y; International Liaison Committee on Resuscitation Neonatal Life Support Task Force. Pediatrics. 2019 Jan; 143(1). pii: e 20181828. doi: 10. 1542/peds. 2018 -1828.
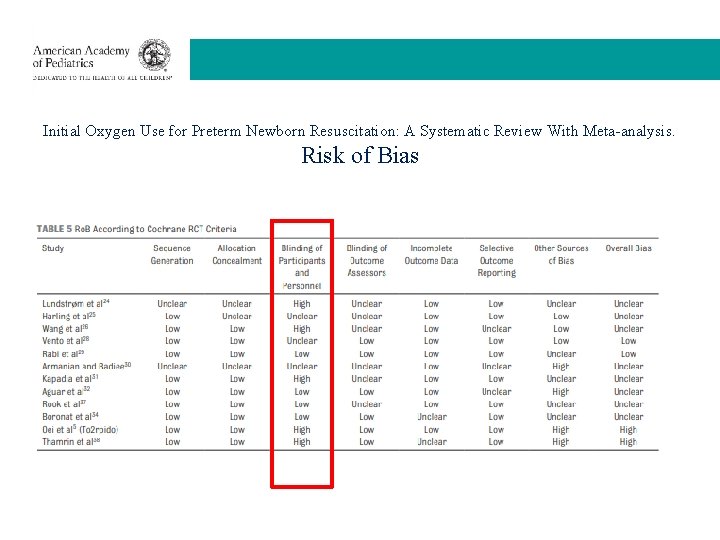
Initial Oxygen Use for Preterm Newborn Resuscitation: A Systematic Review With Meta-analysis. Risk of Bias
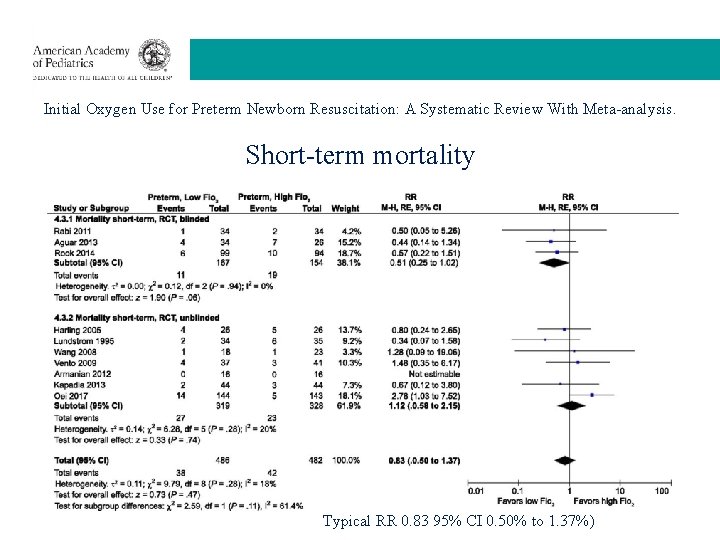
Initial Oxygen Use for Preterm Newborn Resuscitation: A Systematic Review With Meta-analysis. Short-term mortality Typical RR 0. 83 95% CI 0. 50% to 1. 37%)
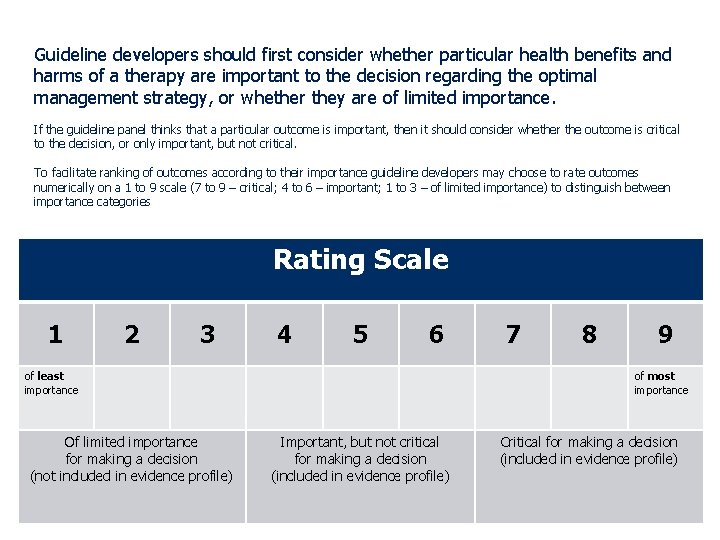
Guideline developers should first consider whether particular health benefits and harms of a therapy are important to the decision regarding the optimal management strategy, or whether they are of limited importance. If the guideline panel thinks that a particular outcome is important, then it should consider whether the outcome is critical to the decision, or only important, but not critical. To facilitate ranking of outcomes according to their importance guideline developers may choose to rate outcomes numerically on a 1 to 9 scale (7 to 9 – critical; 4 to 6 – important; 1 to 3 – of limited importance) to distinguish between importance categories Rating Scale 1 2 3 4 5 6 of least importance Of limited importance for making a decision (not included in evidence profile) 7 8 9 of most importance Important, but not critical for making a decision (included in evidence profile) Critical for making a decision (included in evidence profile)
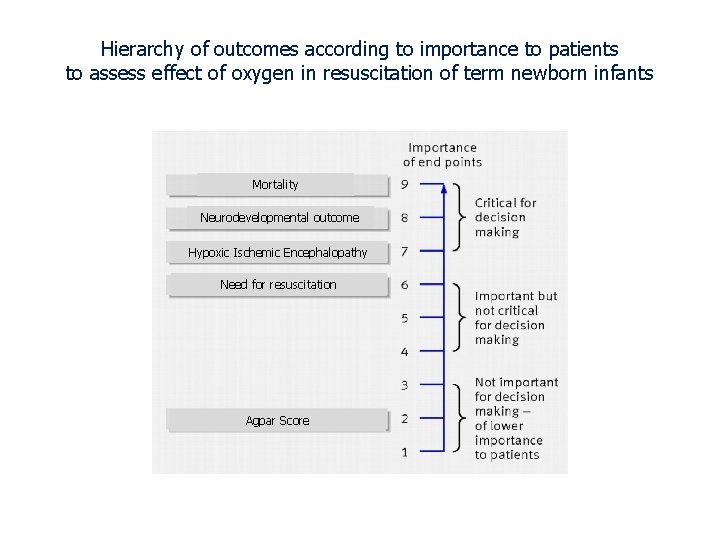
Hierarchy of outcomes according to importance to patients to assess effect of oxygen in resuscitation of term newborn infants Mortality Neurodevelopmental outcome Hypoxic Ischemic Encephalopathy Need for resuscitation Agpar Score

Initial Oxygen Use for Preterm Newborn Resuscitation: A Systematic Review With Meta-analysis. RESULTS: Ten randomized controlled studies and 4 cohort studies included 5697 patients. There are no statistically significant benefits of or harms from starting with lower compared with higher Fi. O 2 in • short-term mortality • long-term mortality, • neurodevelopmental impairment, • or other key preterm morbidities. A sensitivity analysis in which 1 study with a high Ro. B was excluded failed to reveal a reduction in mortality with initial low Fi. O 2 (n = 681; risk ratio = 0. 63 [95% confidence interval 0. 38 to 1. 03]). LIMITATIONS: The Grading of Recommendations Assessment, Development and Evaluation certainty of evidence was very low for all outcomes due to Ro. B, inconsistency, and imprecision. Welsford M, Nishiyama C, Shortt C, Weiner G, Roehr CC, Isayama T, Dawson JA, Wyckoff MH, Rabi Y; International Liaison Committee on Resuscitation Neonatal Life Support Task Force. Pediatrics. 2019 Jan; 143(1). pii: e 20181828. doi: 10. 1542/peds. 2018 -1828.



Umbilical Cord Management at Term and Late Preterm Birth: A Systematic Review and Meta-Analysis

Umbilical Cord Management: Delayed Cord Clamping: 2015 Delayed cord clamping after 30 seconds is suggested for both term and preterm infants who do not require resuscitation at birth. There is insufficient evidence to recommend an approach to cord clamping for infants who require resuscitation at birth. https: //eccguidelines. heart. org/index. php/circulation/cpr-ecc-guidelines-2/part 13 -neonatal-resuscitation/

Umbilical Cord Management at Term and Late Preterm Birth: A Systematic Review and Meta-Analysis Update Objective: To assess effects of umbilical cord management strategies (clamping timing and cord milking) in infants ≥ 34 weeks' gestational age. Methods: We searched bibliographic databases through July 2019 for randomized controlled trials assessing cord clamping timing and/or cord milking. Two authors independently assessed trial eligibility and risk of bias, extracted data, and assessed evidence certainty (GRADE). Judith Gomersall, Ph. D, and colleagues. Submitted for publication. 2020

Umbilical Cord Management at Term and Late Preterm Birth: A Systematic Review and Meta-Analysis Results: We identified 46 studies (9, 159 women and their infants) investigating seven comparisons. Compared to early cord clamping (ECC) < 30 seconds, delayed cord clamping (DCC) ≥ 30 seconds (33 studies), intact-cord milking (ICM) (1 trial), and cutcord milking (CCM) (2 trials) probably improve hematologic measures but may not affect major neonatal morbidities. No differences in major neonatal morbidities are seen in studies comparing methods of optimizing placental transfusion (DCC vs. CCM (3 studies), longer delays in clamping (7 studies) or physiologic parameters (3 studies)). Strategies that promote increased placental transfusion may be associated with greater phototherapy use. Evidence for all outcomes was low or very low certainty.
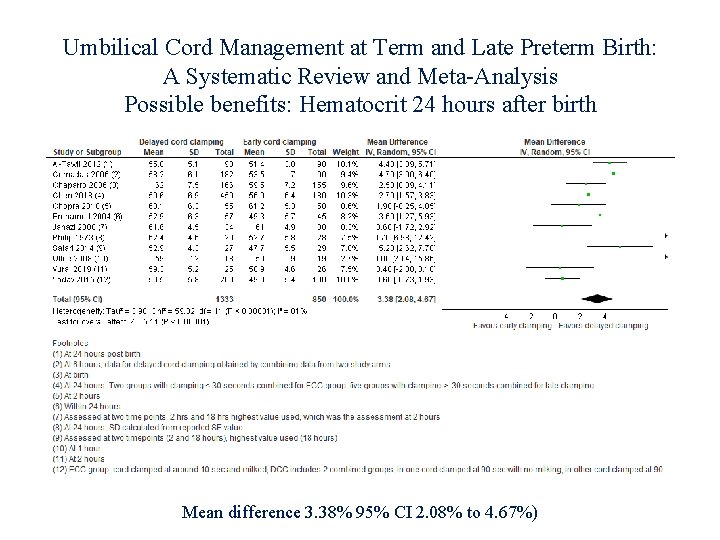
Umbilical Cord Management at Term and Late Preterm Birth: A Systematic Review and Meta-Analysis Possible benefits: Hematocrit 24 hours after birth Mean difference 3. 38% 95% CI 2. 08% to 4. 67%)
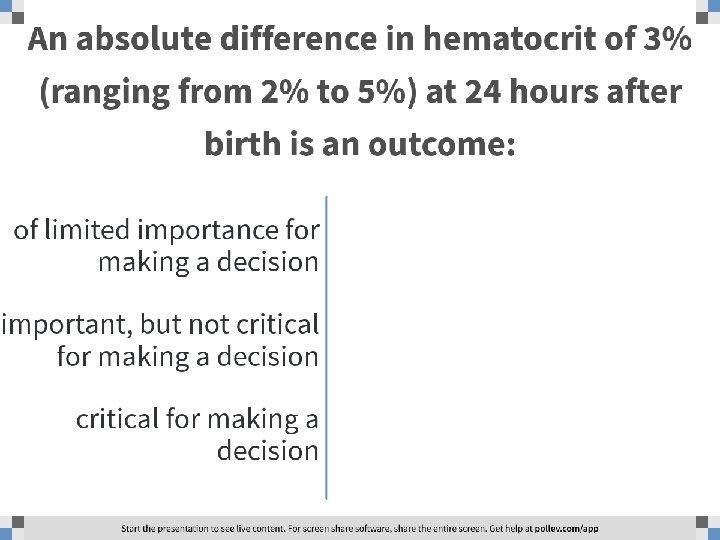
Umbilical Cord Management at Term and Late Preterm Birth: A Systematic Review and Meta-Analysis Possible harms? Hyperbilirubinemia requiring phototherapy Typical RR 0. 72 95% CI 0. 37 to 1. 40) Typical RR 1. 54 95% CI 1. 01 to 2. 34) Typical RR 1. 28 95% CI 0. 90 to 1. 82)



Umbilical Cord Management at Term and Late Preterm Birth: A Systematic Review and Meta-Analysis Limitations Incompleteness and low certainty of findings limits applicability. Conclusions Compared to ECC, DCC or cord milking increases hemoglobin and hematocrit immediately after birth in infants ≥ 34 weeks' gestational age. The uncertain effects of DCC and cord milking compared to ECC on survival without neurodisability, anemia in early infancy, or maternal postpartum hemorrhage inhibit usefulness of available evidence for policy and practice.
What about the preterm infant?

Effect of timing of umbilical cord clamping and other strategies to influence placental transfusion at preterm birth on maternal and infant outcomes. Rabe H, Diaz-Rossello JL, Duley L, Dowswell T.

Effect of timing of umbilical cord clamping and other strategies to influence placental transfusion at preterm birth on maternal and infant outcomes. MAIN RESULTS: Fifteen studies (738 infants) were eligible for inclusion. Participants were between 24 and 36 weeks' gestation at birth. The maximum delay in cord clamping was 180 seconds.

Effect of timing of umbilical cord clamping and other strategies to influence placental transfusion at preterm birth on maternal and infant outcomes. Transfused for anemia (7): • typical RR 0. 61. 95% CI 0. 46 to 0. 81 Inotropic support for low blood pressure (4): • typical RR 0. 42, 95% CI 0. 23 to 0. 77 Intraventricular hemorrhage (IVH)(10): • typical RR 0. 59 95% CI 0. 41 to 0. 85 Necrotizing enterocolitis (NEC)(5): • typical RR 0. 62, 95% CI 0. 43 to 0. 90 No proven benefits or harms regarding • Severe intraventricular hemorrhage (severe IVH)(6): • Oxygen Supplementation at 36 weeks’ postmenstrual age (5) • Mortality (13)


Umbilical Cord Management: Delayed Cord Clamping 2015: Delayed cord clamping after 30 seconds is suggested for both term and preterm infants who do not require resuscitation at birth. There is insufficient evidence to recommend an approach to cord clamping for infants who require resuscitation at birth. Why: In infants who do not require resuscitation, delayed cord clamping is associated with less intraventricular hemorrhage, higher blood pressure and blood volume, less need for transfusion after birth, and less necrotizing enterocolitis. The only adverse consequence found was a slightly increased level of bilirubin, associated with more need for phototherapy. https: //eccguidelines. heart. org/index. php/circulation/cpr-ecc-guidelines-2/part 13 -neonatal-resuscitation/

How does the APTS Study help further inform our decision?

Umbilical Cord Management for Newborns < 34 weeks' gestation: a meta-analysis Comparison: Later (delayed) cord clamping (DCC) vs. early cord clamping (ECC) We identified 23 studies including 3514 infants comparing delayed cord clamping DCC to early cord clamping ECC. Studies were undertaken in a range of countries, mostly high-income. Most studies included births before 32 to 34 weeks' gestation and were conducted at a single center (78%), but the largest RCTs were multicenter (22%). The studies covered a variety of timings of cord clamping and positioning of the infant. Timing of DCC ranged between 30 seconds and ≥ 120 seconds, with half the studies (52%) delayed by 30 -45 seconds. Timing of early or immediate cord clamping ranged from within 5 seconds to within 30 seconds across studies; most studies (69%) clamped within 10 seconds. Anna Lene Seidler and colleagues. Accepted for publication. Pediatrics 2020

Umbilical Cord Management for Newborns < 34 weeks' gestation: a meta-analysis Compared to ECC, DCC may improve neonatal survival (or reduce neonatal mortality) or may make no difference (survival: risk ratio (RR) 1. 02, 95% confidence interval (CI) 1. 00 to 1. 04; Number needed to benefit (NNB) 50, 95% CI 25 to no benefit; 16 studies, 2988 infants; I 2 = 0%, (certainty of evidence moderate). This translates into a RR 0. 80 (95% CI 0. 63 to 1. 02) for the inverse outcome of mortality. There was no clear difference in the number of infants with • severe intraventricular hemorrhage (IVH) (RR 0. 98, 95% CI 0. 67 to 1. 42) • necrotizing enterocolitis (NEC) (RR 0. 83, 95% CI 0. 61 to 1. 13) • chronic lung disease (RR 1. 03, 95% CI 0. 94 to 1. 13) • hyperbilirubinemia treated by phototherapy (RR 0. 99, 95% CI 0. 95 to 1. 03). The evidence was unclear for survival without moderate or severe neurodevelopmental impairment in early childhood (RR 0. 96, 95% CI 0. 78 to 1. 17). None of the included studies assessed other early childhood outcomes.

Umbilical Cord Management for Newborns < 34 weeks' gestation: a meta-analysis Compared to Early Cord Clamping, Later (Delayed) Cord Clamping probably improves hematologic measures: Within 24 hours after birth • peak hemoglobin: mean difference (MD) 1. 24 g/d. L, 95% CI 0. 01 to 2. 47 • peak hematocrit: MD 2. 63%, 95% CI 1. 85 to 3. 42 Within 7 days after birth • peak hematocrit: MD 2. 70%, 95% CI 1. 88 to 3. 52 Compared to ECC, infants in the DCC group had • less inotropic support for hypotension during the first 24 hours of life (RR 0. 36, 95% CI 0. 17 to 0. 75), • a higher measurement of lowest mean arterial blood pressure in the first 12 hours of life (MD 1. 79 mm. Hg, 95% CI 0. 53 to 3. 05), • lower incidence of any blood transfusion (RR 0. 83, 95% CI 0. 77 to 0. 90), and a • lower total number of blood transfusions per infant (MD -0. 63, 95% CI -1. 08 to -0. 17) during hospital course.




Upcoming EBM Webinars September 23, 2020 Session 7: The pros and cons of probiotics CME Contact Hours: An email will be sent to all participants with links to post-webinar surveys. Upon completion of the survey, participants will receive their certificates. Surveys will be open for 2 weeks. Questions: colleen. ovelman@uvm. edu

- Slides: 53