Transitional Care Model Allee Chaffee Abby Nordeen What
Transitional Care Model Allee Chaffee & Abby Nordeen

What is the Transitional Care Model ● “A broad range of time-limited services designed to ensure healthcare continuity, avoid preventable poor outcomes among at-risk populations, and promote the safe and timely transfer of patients from one level of care to another or from one type of setting to another” (Morrison et al, 2016, p 323). ● Designed for chronically ill and/or elderly patients ● Prevents complications and rehospitalizations ● Combines inpatient planning prior to discharge with post discharge actions ● Post discharge nurses follow up with home visits and phone calls to patients ● Purpose is to identify changes in health and manage health problems

History of the Transitional Care Model ● Began because hospitals needed to reevaluate their transitional care practices, in order to “reduce the 30 -day readmission rates, prevent adverse events, and ensure a safe transition from hospital to home” (Rennke & Ranji, 2015) ○ Approximately 1 in 5 patients have adverse events during this period, about 20% of older pts. hospitalized are readmitted within 30 days ● New payments models created incentives to coordinate transitional care ● 2010: bringing the model into the mainstream type of care ● 2012: Centers for Medicare & Medicaid instituted penalties for facilities with high readmission rates within 30 days of discharge (conditions)
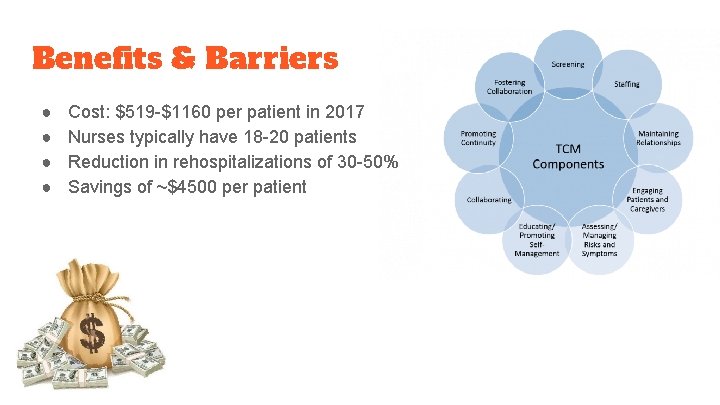
Benefits & Barriers ● ● Cost: $519 -$1160 per patient in 2017 Nurses typically have 18 -20 patients Reduction in rehospitalizations of 30 -50% Savings of ~$4500 per patient

Summary (Continuity of Care: TCM) ● ● ● “TCM intervention focuses on improving care; enhancing patient and family caregiver outcomes; and reducing costs among vulnerable, chronically ill, older adults identified in health systems and community-based settings” (Hirschman et. al. , 2015). Older adults who experienced the TCM had significantly fewer rehospitalizations throughout posthospital six month period “Findings from three reported multi-site National Institute of Nursing Research (NINR) funded randomized clinical trials have consistently demonstrated the capacity of the TCM to improve acutely ill older adults’ experiences with care, and health and quality of life outcomes. Outcomes have demonstrated reduced rehospitalizations and total healthcare costs, after accounting for the additional costs of the intervention” (Hirschman et. al. , 2015). EBP & comparing Components: screening, staffing, maintaining relationships, engaging patients/caregivers, assessing/managings for rsks, education and promoting self-management, collaborating, promoting continuity, fostering coordination

Transitional Care Model Delivery The most successful transitional care programs include: ● ● Nurse as manager of care Home visits Promotion of self-care & health management Coordination of primary and acute care providers

Example MC is a 77 year old man who was recently hospitalized because of heart failure exacerbation. He has since stabilized and is ready to discharge. The Transitional Care Model has helped to establish a care plan that is intended to reduce his risk for rehospitalization and help manage his condition at home. The transitional care nurse that worked with MC made daily rounds in the hospital to follow his progress, provided the patient and family with education and resources to self-manage, and has arranged for home visits to occur weekly until MC is comfortable adjusting the time frame. Hospital policies that connect appropriate patients with transitional care teams, insurance policies that cover the services, and public health policies that provide resources would be beneficial to this care model. Home health, physical therapy/occupational therapy, agencies that encourage and educate on self-care skills, and rehabilitation facilities would be examples of beneficial resources to this care model.

References (2018). The transitional care model. Social Programs That Work. evidencebasedprograms. org/programs/transitional-care-model/. Dreyer, T. (2014). Care transitions: Best practices and evidence-based programs. Center for Healthcare Research & Transformation. Retrieved from http: //www. chrt. org/publication/care-transitions-best-practices-evidence-based-programs/ Hirschman, K. , Shaid, E. , Mc. Cauley, K. , Pauly, M. , Naylor, M. , (September 30, 2015) "Continuity of Care: The Transitional Care Model" OJIN: The Online Journal of Issues in Nursing Vol. 20, No. 3, Manuscript 1. Morrison, J. , Van Palumbo, M. , & Rambur, B. (2016). Reducing preventable hospitalizations with two models of transitional care. Journal of Nursing Scholarships. 48(3). 322 -329. Naylor, M. & Sochalski, J. (2010). Scaling Up: Bringing the Transitional Care Model into the Mainstream. The Commonwealth Fund. Retrieved from https: //static 1. squarespace. com/static/59 f 0 c 113 fe 54 ef 2 f 67873 a 25/t/59 fb 8 f 82 e 2 c 483961 b 11 b 483/1509658500194/TCM_Forefront. pdfm Rennke, S. , & Ranji, S. R. (2015). Transitional Care Strategies From Hospital to Home: A Review for the Neurohospitalist. The Neurohospitalist, 5(1), 35– 42. http: //doi. org/10. 1177/1941874414540683
- Slides: 8