Transfusion Service and Blood Center Partnerships Suchi Pandey

Transfusion Service and Blood Center Partnerships Suchi Pandey, MD Chief Medical Officer Blood Centers of the Pacific Blood. Source United Blood Services CBBS Annual Meeting 5/6/17 1

Disclosure Slide • 2 I have no relevant financial relationships to disclose for this program

Objectives 1) Describe at least three ways to optimize communication between blood centers and transfusion services, especially in challenging clinical situations 2) Identify two examples of how quality has been enhanced via collaboration between the Blood Center and the Transfusion Service. 3

Describe at least three ways to optimize communication between blood centers and transfusion services, especially in challenging clinical situations 4
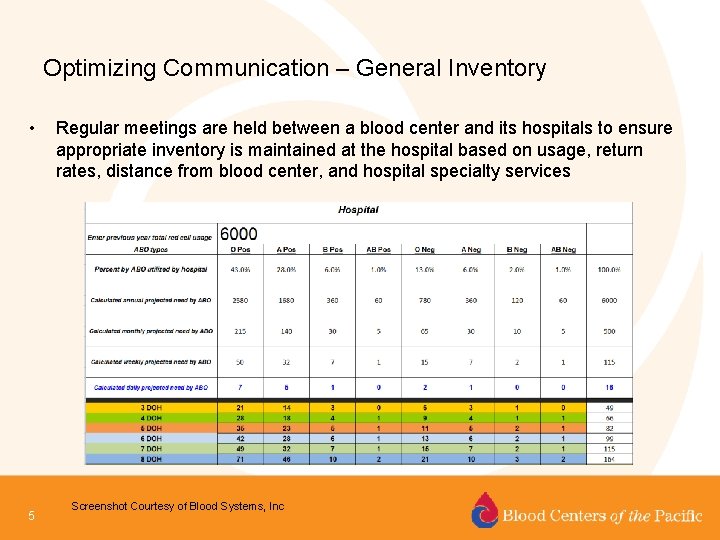
Optimizing Communication – General Inventory • 5 Regular meetings are held between a blood center and its hospitals to ensure appropriate inventory is maintained at the hospital based on usage, return rates, distance from blood center, and hospital specialty services Screenshot Courtesy of Blood Systems, Inc

Optimizing Communication – General Inventory • Inventory Management – On any given day/week, Blood Centers frequently communicate with hospitals to determine inventory levels. – This communication is often via phone calls but some Blood Centers have implemented electronic programs that facilitate sharing of the hospital’s inventory with the Blood Center 6
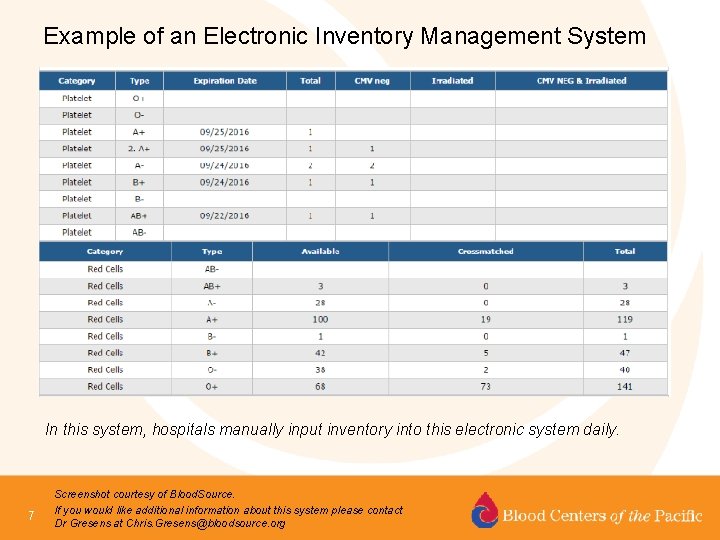
Example of an Electronic Inventory Management System In this system, hospitals manually input inventory into this electronic system daily. 7 Screenshot courtesy of Blood. Source. If you would like additional information about this system please contact Dr Gresens at Chris. Gresens@bloodsource. org
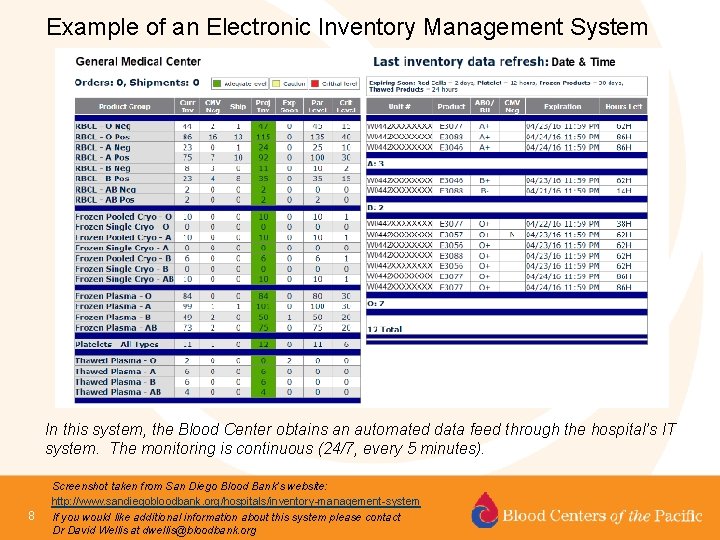
Example of an Electronic Inventory Management System In this system, the Blood Center obtains an automated data feed through the hospital’s IT system. The monitoring is continuous (24/7, every 5 minutes). 8 Screenshot taken from San Diego Blood Bank’s website: http: //www. sandiegobloodbank. org/hospitals/inventory-management-system If you would like additional information about this system please contact Dr David Wellis at dwellis@bloodbank. org

Optimizing Communication – General Inventory • Communication During Shortages – Important for Blood Centers and Transfusion Service to work together when there is a shortage and maintain frequent communication • During a shortage, hospital orders may not be filled. Blood center provides updates to hospitals about inventory status and when orders can be filled. • Blood Center Medical Director assists with triaging products and communicates directly with the transfusion service – During a shortage, hospitals will put additional measures in place to preserve inventory and also communicate with hospital clinicians • O-neg shortage: Reserve limited O-neg supply for females of child bearing age • AB plasma shortage: Use Type A plasma in Emergency situations • Platelet shortage: Consider emergency release if there is a medical need 9
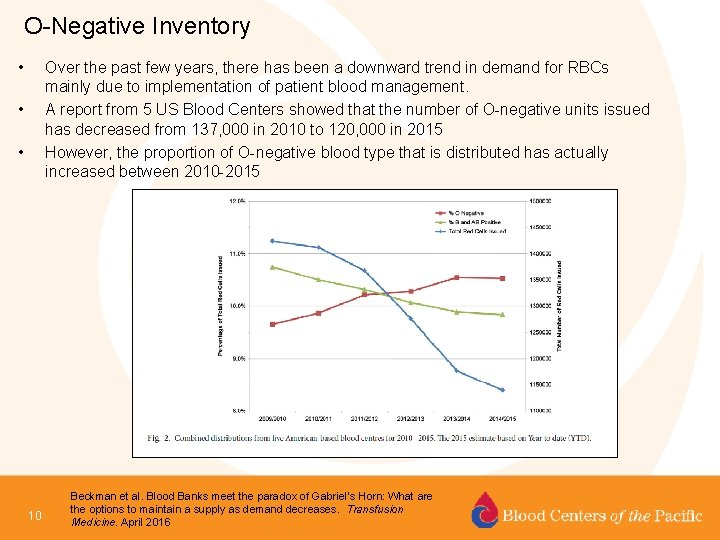
O-Negative Inventory • Over the past few years, there has been a downward trend in demand for RBCs mainly due to implementation of patient blood management. A report from 5 US Blood Centers showed that the number of O-negative units issued has decreased from 137, 000 in 2010 to 120, 000 in 2015 However, the proportion of O-negative blood type that is distributed has actually increased between 2010 -2015 • • 10 Beckman et al. Blood Banks meet the paradox of Gabriel’s Horn: What are the options to maintain a supply as demand decreases. Transfusion Medicine. April 2016

O-negative Inventory • There is a disconnect between supply and demand for O-negative : – Five US Blood Centers reported that in 2015, the blood type O-negative was seen in 6. 3% of first time donors but O-negative accounted for 10. 5% of RBCs distributed. • The Dilemma: – In response to decreased RBC demand, Blood centers logically will decrease RBC collections (e. g. fewer drives, fewer appointments). – However this causes a uniform decrease in all blood types which is problematic when demand for O-negative has NOT decreased – The end result: blood center numerically has enough units in inventory to meet demand BUT not enough units to meet demand for a specific blood type – The “$1, 000 O-negative unit” is becoming an increasing reality: • Example: An expensive drive is held just to obtain a small numbers of O-neg units although most of units end up to be blood types that are not needed. 11 Beckman et al. Blood Banks meet the paradox of Gabriel’s Horn: What are the options to maintain a supply as demand decreases. Transfusion Medicine. April 2016

During a critical O-negative shortage the following is communicated to hospitals: Reserve O-Negative Blood: Use O-Positive Blood: Other considerations For females of child bearing age, who are Rh-negative or blood type unknown, and patients with an anti-D. If the patient needs to be switched to Rh-positive blood, review this with the patient’s physician. * For adult males and adult females over child bearing age with an unknown blood type in emergency situations. * For neonatal transfusion, determine ABO type and transfuse ABO-compatible blood. For O-negative adult males and females over child bearing age (without an anti -D), if it is expected that more than 2 units will be required in a 24 hour period. * (for small volume transfusions, RBC units stored in additive solution and greater than 7 days old are acceptable). *The probability of a D-negative patient developing anti-D following exposure to Dpositive RBCs is approximately 30%. 12 Frohn C et al. Probability of anti-D development in D- patients receiving D+ RBCs. Transfusion 2003; 43: 893 -898

AB Plasma Inventory • • Over the past few years, there has been an increase in the amount of plasma used in emergency massive transfusion settings. During massive transfusions, an RBC to plasma ratio of 1: 1 is often used. Since AB plasma is the universal plasma type, there has been an increase in demand for AB plasma for massive transfusion protocols Similar to O-negative RBCs, there is a disconnect between supply and demand for AB plasma – Per the 2013 AABB Blood Survey Report, blood suppliers provided 16. 5% more of AB plasma in 2013 than 2011 – In 2013, 9. 7% of the plasma distributed for transfusion was AB. – Type AB is only seen in approximately 4% of the population 13 The AABB Blood Survey Report Final. 2013 http: //www. aabb. org/research/hemovigilance/bloodsurvey/Docs/2013 -AABB-Blood-Survey-Report. pdf

During an AB plasma shortage the following is communicated • Use Type A plasma instead of Type AB for emergency transfusions – Several large hospitals have been transfusing Type A plasma to bleeding patients with an unknown blood type. – In some hospitals, the Type A plasma is not screened for anti-B titers. – Published studies report that patients who received non-compatible plasma (e. g. Type A plasma provided to a Type B or AB patient) did not have an adverse transfusion reaction related to the mismatch – Studies have shown that most group A donors have low titers of anti-B. One hospital reported that 90% of their Type A plasma units had a titer less than 64 – Indicates that Group A plasma can be safely used in emergency situations when the patient’s blood type is unknown We are working with our trauma centers to add to their procedures the acceptance of using Type AB or A plasma for emergency transfusions to their procedures 14 Yazer M et al. How we manage AB plasma inventory in the blood center and transfusion service. Transfusion 2013; 53: 1627 -1633 Cooling L. Going from A to B: the safety of incompatible group A plasma for emergency release in trauma and massive transfusion patients. Transfusion 2014; 54: 1695 -1697
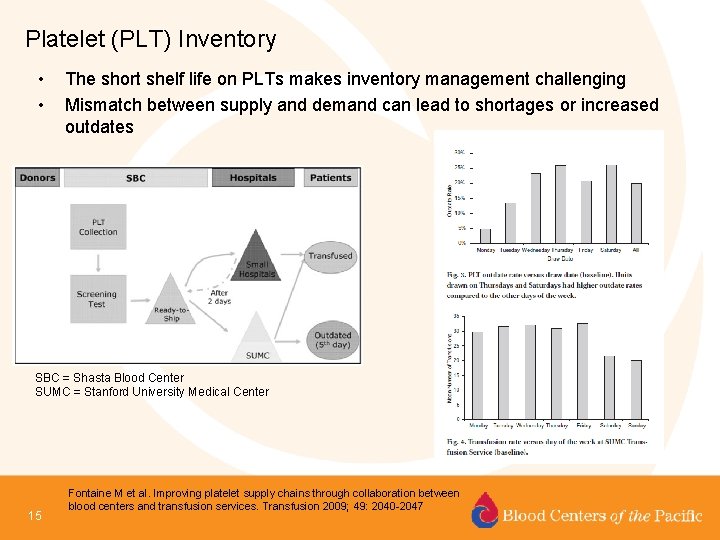
Platelet (PLT) Inventory • • The short shelf life on PLTs makes inventory management challenging Mismatch between supply and demand can lead to shortages or increased outdates SBC = Shasta Blood Center SUMC = Stanford University Medical Center 15 Fontaine M et al. Improving platelet supply chains through collaboration between blood centers and transfusion services. Transfusion 2009; 49: 2040 -2047

Platelet Inventory 16 Fontaine M et al. Improving platelet supply chains through collaboration between blood centers and transfusion services. Transfusion 2009; 49: 2040 -2047

Optimizing Communication – Antigen Negative RBCs • Over the past few years, there has been an increasing demand for antigen negative RBC units – Expanding practice of providing partially or fully phenotypically matched RBC units to patients with sickle cell anemia, thalassemia, and warm autoimmune antibodies – Studies show that these populations are more susceptible to antibody formation and providing phenotypically matched RBC units prevents allo -immunization – For sickle cell patients, some hospitals select units as follows: • If patient has no allo-antibodies, Rh and Kell matched units are provided • If patient forms an alloantibody, fully phenomatched units are provided 17 Osby et al. Phenotype matching of donor red blood cell units for nonalloimmunized sickle cell disease patient: a survey of 1182 North American laboratories. Arch Pathol Lab Med 2005; 129: 190 -

Optimizing Communication – Antigen Negative RBCs • Many of the patients requiring large numbers of antigen negative units are sickle cell patients who have scheduled outpatient transfusions (e. g. RBC exchange) • Our Blood Center serves two hospitals that manage multiple patients with sickle cell disease (SCD). Advanced communication of the transfusion schedule and patients’ transfusion requirements is crucial in ensuring units are ready for the patient. – Typically the hospitals will provide a 1 -2 week notice before the transfusion date. – Allows adequate time for Blood Center to locate units and also recruit if needed. 18
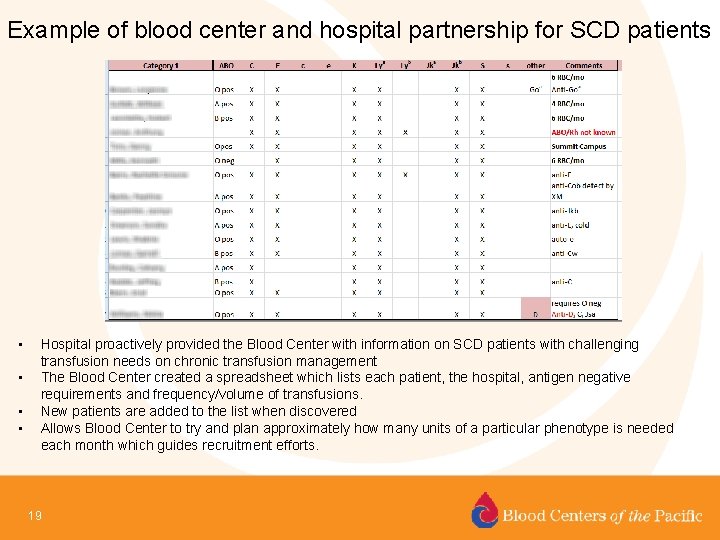
Example of blood center and hospital partnership for SCD patients • • Hospital proactively provided the Blood Center with information on SCD patients with challenging transfusion needs on chronic transfusion management The Blood Center created a spreadsheet which lists each patient, the hospital, antigen negative requirements and frequency/volume of transfusions. New patients are added to the list when discovered Allows Blood Center to try and plan approximately how many units of a particular phenotype is needed each month which guides recruitment efforts. 19

Optimizing Communication – Antigen Negative RBCs • Occasionally, there is very little lead time provided (e. g. sickle cell patient with stroke who requires a 8 unit exchange to decrease viscosity) or number of requests exceeds units available at the Blood Center. – In these cases, we rely on our network of Blood Centers to fill the order (liquid or frozen). If needed out of network Blood Centers are also contacted – Reference Lab, Blood Center physician, and/or hospital services are in constant communication with the hospital to provide updates on filling the order. 20

Optimizing Communication – Rare Antigen Negative RBCs • These can be extremely difficult cases to manage and requires significant collaboration and communication between the Blood Center, Transfusion Service, and Clinicians to manage the patient. • When the supply of Ag negative blood is limited, creating a transfusion plan is necessary if major bleeding is expected • Often times the patient will receive some incompatible blood if there is a large transfusion need. 21

Blood Center and Transfusion Service Partnership to Manage a High Risk Pregnancy - A 37 year old O-positive (O+) G 6 P 2 (history of 2 C-sections) Caucasian woman presented with mild vaginal bleeding at 28 weeks’ gestation. - Ultrasound at 28 weeks showed placenta accreta. - Antibody screen at 28 weeks was positive. - Sample was sent to the Immunohematology Reference Lab (IRL) for antibody identification. • Anti-Jra was identified: Patient ‘s RBCs were Jra negative [Jr(a-)] ; plasma was compatible with Jr(a-) RBCs – Anti –Jra titer at 30 weeks was 4 Anti- Jra has been associated with mild and moderate hemolytic transfusion reactions. HDFN is not typical, but one fatal case has been reported. 22 Jacquot C, et al. Management of a High Risk Pregnancy with Anti-Jra. AABB Annual Meeting 2016. Orlando, FL.

Blood Center and Transfusion Service Partnership to Manage a High Risk Pregnancy Frequent communication occurred between the Blood Center, Transfusion Service, and Clinicians for this case re: inventory status and patient’s medical plan. - A C-section with hysterectomy was planned at 34 weeks. - The patient had one sibling - unavailable for Jra testing. - A nationwide search for Jr(a-) units identified only 6 frozen units. - This donor was recruited and donated 2 “liquid” units in the 2 weeks before the scheduled surgery. - The 2 nd unit was collected 10 days after the 1 st. Medical Director approval required. - 7 Jr(a-) units (5 frozen, 2 liquid) were available for the delivery - 23 1 of the 6 frozen Jr(a-) units was unusable due to large clots identified after deglycerolization
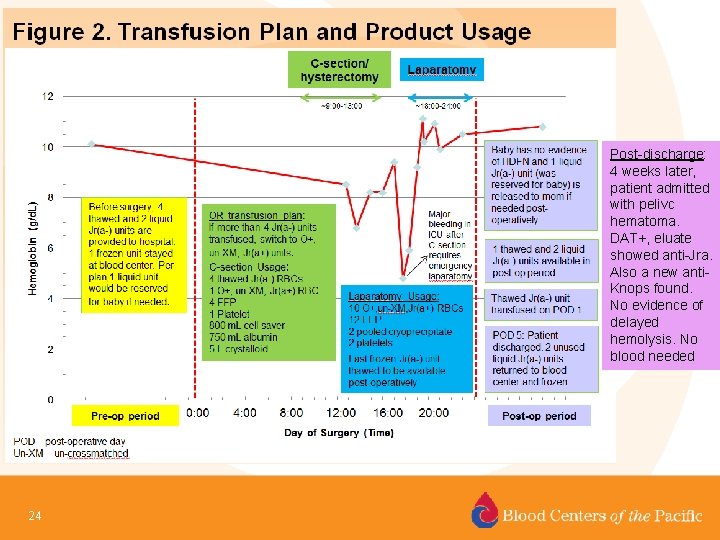
Post-discharge: 4 weeks later, patient admitted with pelivc hematoma. DAT+, eluate showed anti-Jra. Also a new anti. Knops found. No evidence of delayed hemolysis. No blood needed 24

Case Summary - Management of this high bleeding risk patient with placenta percreta and an anti-Jra required close coordination and communication between the blood center, transfusion service, and clinical services. - When the supply of antigen negative blood is limited, creating a transfusion plan is necessary if major bleeding is expected - Fortunately, in this case, the anti-Jra was not clinically significant for the mother or baby 25

Optimizing Communication – Specialized PLT Products • Patients who are refractory to PLT transfusions – Most experts agree that a 1 -hour post-transfusion corrected count increment (CCI) of less than 5000 to 7500 after two consecutive transfusions defines the refractory state – Management options in patients with immune mediated refractoriness include: • Crossmatch compatible platelets • HLA matched/compatible platelets 26 Curtis, Brian. Chapter 18: Platelet and Granulocyte Antigens and Antibodies. AABB Technical Manual. 18 th edition.

Optimizing Communication – Specialized PLT Products • Example of a management strategy for a refractory patient: – A PLT crossmatch is performed when a newly refractory patient is identified and crossmatch compatible PLTs are provided. – A Class I HLA type and HLA Antibody screen with specificities is obtained – Once HLA type and antibody specificities are known, HLA matched/compatible platelets are provided – If the patient has multiple HLA antibody specificities (high PRA), PLTs provided may have one or two “mismatched” antigens. 27

Optimizing Communication – Specialized PLT Products • Close collaboration between the hospital and the blood center results in optimal management of PLT refractory patients – Hospital closely monitors the in vivo response to transfused platelets – Hospital communicates the effectiveness of each unit to the Blood Center – Blood Center focuses recruitment effort on donors whose unit(s) provided a good response in the patient – Blood Center proactively updates hospital when donors are recruited and units will be available. 28

Optimizing Communication – Specialized PLT Products • A shared excel spreadsheet was developed with one hospital which was used for every refractory patient to facilitate the exchange of information between the hospital and the Blood Center – On the hospital side: A computer program extracted data from each PLT transfusion and CCIs calculated. This was securely shared with the Blood Center Coordinator daily. – On the Blood Center side: the Blood Center coordinator updated the spreadsheet with the following • • Added HLA types Identified donors that resulted in good CCIs for recruitment Identified “mismatched antigens” which still resulted in a good response Entered upcoming donations (scheduled donation date, availability, etc) • A modified version of this spreadsheet is now being rolled out to other hospitals. 29 Jacquot C et al. Partnership Between Transfusion Service and Blood Donor Center for Optimal Care of Platelet Refractory Patients. AABB Annual Meeting 2016. Orlando, FL.
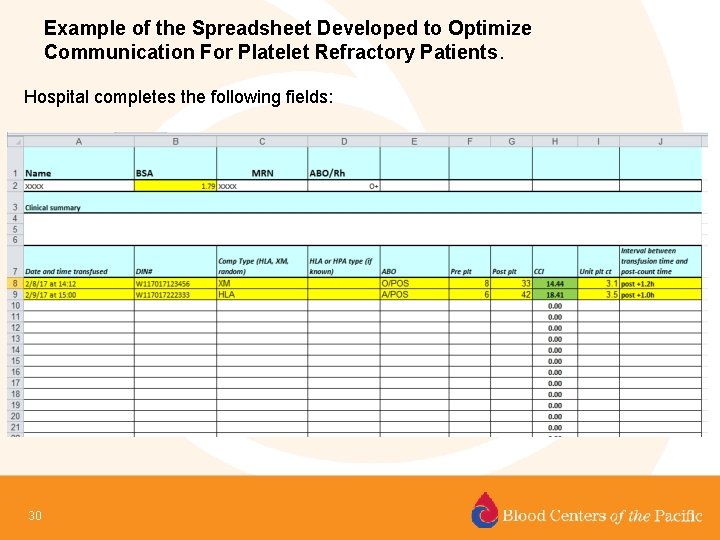
Example of the Spreadsheet Developed to Optimize Communication For Platelet Refractory Patients. Hospital completes the following fields: 30
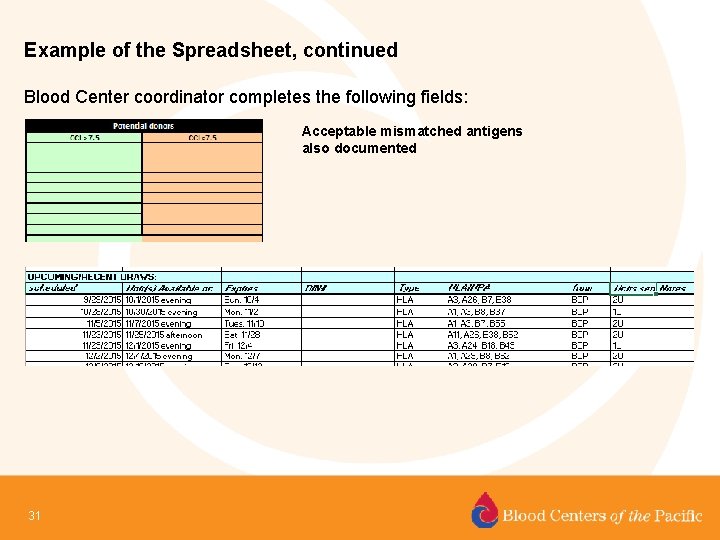
Example of the Spreadsheet, continued Blood Center coordinator completes the following fields: Acceptable mismatched antigens also documented 31

Optimizing Communication – Recall Event • It is the Blood Center’s responsibility to clearly communicate the impact to the hospital, provide guidance on the management of affected units, and share suggested messaging to clinicians. • It is the Transfusion Service’s responsibility to work with the Blood Center to manage inventory to maintain an adequate and safe supply for patient needs. 32 URGENT Recall Extension for Leukotrap RC System with RC 2 D Filter http: //www. fda. gov/Biologics. Blood. Vaccines/Safety. Availability/Recalls/ucm 507900. htm
33

Optimizing Communication – Large Recall Event • On 6/21/2016, the FDA posted an expanded action related to all Haemonetics Leukotrap RC System with RC 2 D Filter Kits (SKU 129 -63) distributed between April 14, 2016 and June 17, 2016. – This action was prompted by the finding of an unacceptable level of leukocyte reduction in certain Haemonetics in-line filter collection kits. – Impacted units were potentially nonleukoreduced and should not be provided to patients with indications for leukoreduction • Approximately 1/3 of the nation’s blood supply was impacted. 34

Optimizing Communication – Large Recall Event • Blood Center provided written communication(s) to hospitals which – Described the issue – Provided guidance on actions to take on units collected with the impacted lot #s – Provided a Work Aid to assist hospitals in identifying impacted units – Described the actions the blood center was taking to ensure a adequate supply of leukoreduced blood – Provided guidance on physician notification for units already transfused • Template letter provided • Blood Center physician and other staff were available 24 -7 for hospital questions during this time. 35

Optimizing Communication – Large Recall Event • • The Blood Center recommended that hospitals provide impacted units to patients without indications for leukoreduction. Transfusion Service Medical Directors developed guidelines for Blood Bank staff regarding which patients could receive the potentially non leukoreduced units – In some instances these instructions were crafted with the assistance of the Blood center physician • • 36 Some hospitals also agreed to take on more non leukoreduced inventory to prevent wastage This recall was a perfect example of the partnership and communication needed between the hospital and blood center to get through challenging and unexpected event. Overall the collaboration led to fewer wasted units.

Other Examples of Partnership between Hospitals and the Blood Center • Hospitals providing Blood Centers patient stories (de-identified) which can be for recruitment efforts • Hospital inviting Blood Center physician to be a part of the Transfusion Committee • Blood Center physician being available 24/7 for consultation with the hospital • Blood Centers providing additional support services such as: – – – 37 Therapeutic Apheresis Centralized Transfusion Service Transfusion Safety Officers Gap analysis Blood management programs

Other Examples of Partnership between Hospitals and the Blood Center • Educational/training partnerships: – Resident/Fellow Education – Lectures (CME/Grand Rounds) on a topic the hospital chooses – Blood Center organized seminars/symposiums (some quality focused) – In hospital training 38

Identify two examples of how quality has been enhanced via collaboration between the Blood Center and the Transfusion Service. 39

Quality Related Services • Quality staff at the Blood Center can offer their expertise and guidance to hospital transfusion services – Prospectively to address potential issues – In real time to address actual issues • Examples of this: – – – 40 Gap Analysis Transfusion Service Diagnostic Educational Forums Transfusion Safety Officer Ad hoc consultation with Blood Center Quality Staff

Gap Analysis • Gap Analysis – Hospitals can request that Blood Center quality staff perform a gap analysis for their transfusion service – Typically a hospital will request this before an upcoming inspection 41

Example 1: Hospital System Gap Analysis that included AABB and CAP standards. • • A gap analysis was requested for a hospital system with 6 hospitals in one large geographical region that ranged from hospitals with < 100 beds to > 500 with a scope of service that was from general practices to transplantation The evaluation was requested so – Each hospital in the system was individually compliant to AABB/ CAP standards – Determine if the system achieved standardization of existing policies, processes, and procedures with practices and testing being standardized in all six hospitals. – Prepare for an AABB assessment that was anticipated to occur within the year – Perform a crosswalk of AABB standards to CAP standards for an internal audit for compliance 42

Example 1: Hospital System Gap assessment that included AABB and CAP standards. A system nonconformance was defined as : • 50% (3) hospitals or more were not compliant in a certain area/standard then there was a system issue • The main facility providing quality/ management/ administrative support to all 6 hospitals was not in compliance to the standard affecting all 6 member hospitals. 43

Example 1: Hospital System Gap assessment that included AABB and CAP standards. Some of the System findings: • • • Systemwide there was a consistent process with documentation for determining competency post training for testing personnel. There was no evidence of a written SOP or an existing SOP for labeling syringes and verification of label application for neonatal transfusions. The SOP addressing the Lookback process did not reflect the required time frames stated by CFR regulation for notification and documentation of notification attempts Follow-Up • 44 AABB Assessment Identified a few nonconformances but all were previously identified by the Gap assessment … work was already in progress to correct nonconformances.

Example 2 – Ad hoc Quality Consultation 45 • “I need some help from BCP. We had our AABB survey last week and we were cited for not having a policy that addresses how much ABO incompatible platelets you can give. I’m looking for some recommendations from BCP that I can present to my Pathologist in how to handle this. “ • “Nonconformance, STD 5. 15. 4 The transfusion service shall have a policy concerning transfusion of components containing significant amounts of incompatible ABO antibodies. The current policy is incomplete

Example 2 – Ad hoc Quality Consultation • • • After further review, this Blood Bank’s SOP as stated that an attempt will be made to provide type specific platelets if possible based on availability. Neonatal transfusion is also addressed in their SOP (volume reduction if plasma incompatible). The inspector said they should specify the maximum volume of incompatible PLTs that can be given. Blood Center Quality Staff Response: – There is no standard re: volume limits for transfusing ABO incompatible plasma. The AABB standard does not specify that a max volume must be established. It just indicates that hospital must have a policy. – Some hospitals will establish a volume limit guideline in their policy but it is not required – The hospital’s policy was sufficient to meet the standard. 46

Research partnerships between the blood center and the hospital blood service. 47

Research – Partnerships between Blood Center and Hospital Donor-Recipient Linkage Studies. REDS III establishes a database to allow these types of studies Goals: • • 48 Continue research aimed at donor/donations and blood banking issues Address transfusion practice and recipient risk issues:
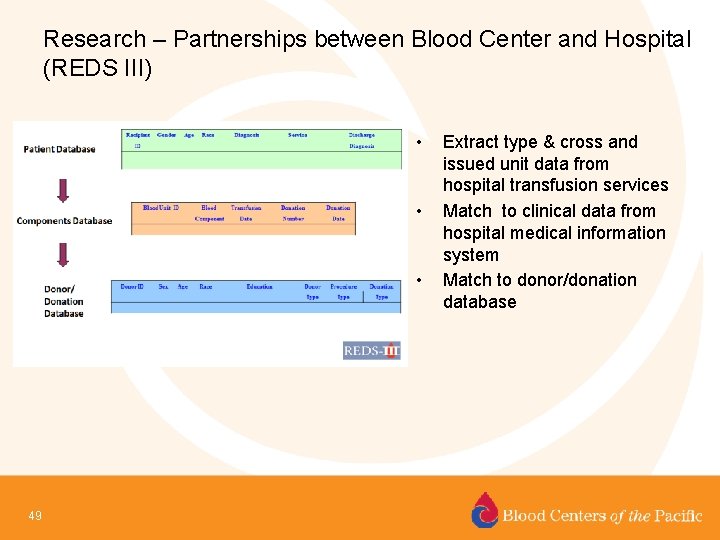
Research – Partnerships between Blood Center and Hospital (REDS III) • • • 49 Extract type & cross and issued unit data from hospital transfusion services Match to clinical data from hospital medical information system Match to donor/donation database

Research – Partnerships between Blood Center and Hospital • Evaluating new products or indications – Studies involving pathogen reduced products – Studies Involving new products. For example: • Frozen platelets • Cold stored platelets • Lyophilized plasma – The Plasma for Alzhemier Sympto. M Amerlioration (PLASMA) Study (PLASMA) • Plasma from young donors is administered to patients with Alzheimer's disease. Primary outcome: Measuring safety and tolerability of this treatment. Secondary outcome: Improvement in tests which assess neurologic function 50

Summary • • • 51 Blood Centers and Hospital Transfusion Service partnerships are required to maintain the blood supply and provide safe blood to patients These partnerships include effective communication between the Blood Center and Transfusion Service, clinical and quality related services, and research collaborations. There must be a mutual trust between the Blood Center and Hospital for the relationship to be successful
- Slides: 51