Transfusion Reactions 1 Introduction Blood transfusion is safe

Transfusion Reactions 1

Introduction • Blood transfusion is safe, effective way to correct hematology defects and crucial part of supportive care of some patients • Sometimes unwanted results may occur during or after transfusion • One of these is transfusion reactions 2

Transfusion Reactions • They are adverse reactions associated with the transfusion of blood and its components • 3% of individuals receiving blood transfusions have a transfusion reaction 3

Transfusion reactions • • Non-threatening to fatal (Fatal ~ 1/50000) Immunological or Non-immunological May or may not cause RBC destruction Immediate to delayed – Immediate – rapid onset (<24 hours) – Delayed – >24 Hours, Occur days, weeks, • May involve infectious agents 4

Transfusion Reactions • Most common causes of transfusion related DEATHS: 1. 2. 3. 4. • Improper specimen identification Improper patient identification Antibody identification error Crossmatch procedure error Most transfusion reactions (not all) are the result of human error. 5
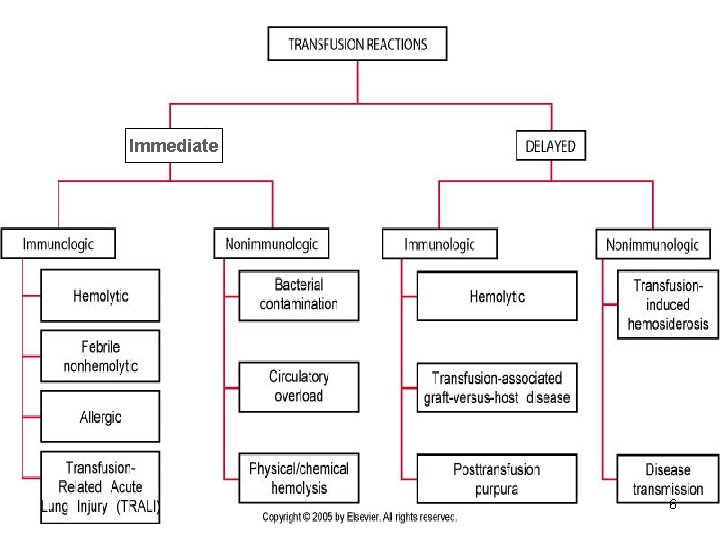
Immediate 6

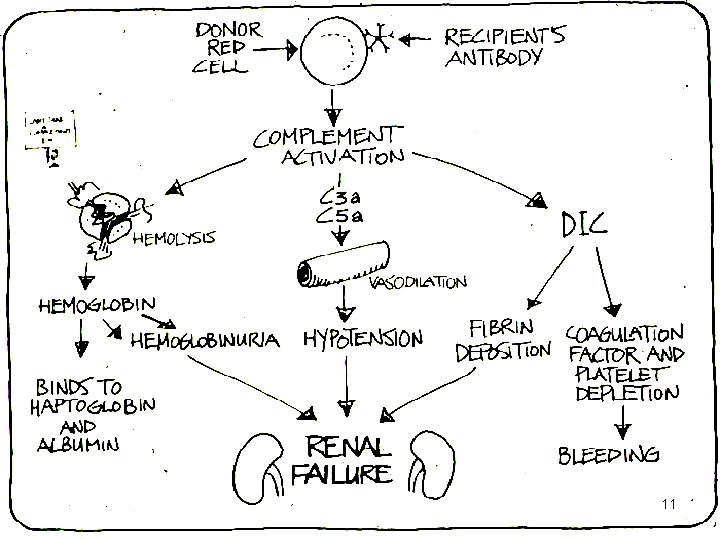
Immediate Hemolytic Reactions • Most common cause is ABO incompatibility (clerical error) • Red cell destruction due to complement activation by Ig. M • RBCs hemolysed due to reaction between Abs in recipient (A & B) & Ags on donor’s RBCs • As little as 10 -15 m. L can trigger a reaction 7

Symptoms • Fever • Pain at infusion site • Back/chest pain • Physical signs – Fever – Hypotension – Bleeding – Renal failure – Hemoglobinuria 8

Steps taken if hemolytic reaction is suspected • Stop transfusion • Keep IV line open with physiologic saline • Perform bedside clerical checks • Contacts patient’s physician & blood bank • Return unit, set & attached solutions to Lab • Collect suitable blood samples for evaluation – Microbiological on unit, culture of patient’s blood, Check for DIC, Renal function 9

Treatment • Treat hypotension by fluid replacement • Maintenance of renal blood flow • Replacement of depleted coagulation factors • Dialysis in case of renal failure 10
11

Transfusion of RBCs Allo-Abs • Rarely, patient’s red cells can be hemolyzed by Abs in transfused whole blood or plasma • Caused by anti-A or Anti-B in certain plasma products – Cryoprecipitate – Factor VIII or IX • Positive DAT, Anti-A or Anti-B can be eluted from red cells 12

Transfusion Induced Alloimmunization • Ags are administered during transfusion • In 1 st transfusion Induce alloantibodies • This will cause problems in subsequent transfusions • Prior transfusion beneficial in some cases – E. g. renal transplantation is more successful in patients with prior multiple transfusions 13

Pseudo-Hemolytic Reactions • Some transfusions may appear to be immediate HTR, but they are not due to immune RBC destruction • These are called pseudo-hemolytic TR 14
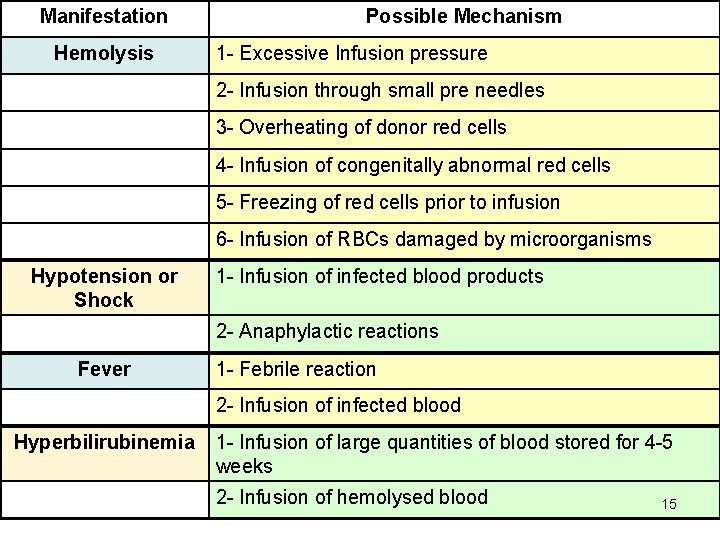
Manifestation Hemolysis Possible Mechanism 1 - Excessive Infusion pressure 2 - Infusion through small pre needles 3 - Overheating of donor red cells 4 - Infusion of congenitally abnormal red cells 5 - Freezing of red cells prior to infusion 6 - Infusion of RBCs damaged by microorganisms Hypotension or Shock 1 - Infusion of infected blood products 2 - Anaphylactic reactions Fever 1 - Febrile reaction 2 - Infusion of infected blood Hyperbilirubinemia 1 - Infusion of large quantities of blood stored for 4 -5 weeks 2 - Infusion of hemolysed blood 15

Delayed Hemolytic Transfusion Reactions • DHTRs occur at least 24 hrs after transfusion • Mediated by Ig. G antibodies – Patient previously exposed to RBC antigen and has low antibody titer until exposed again • Cannot be detected in crossmatch – Rh, Kidd, Duffy, and Kell 16

Delayed Hemolytic Transfusion Reactions • Patients have no symptoms • The only indication is a fall in hemoglobin • Diagnosis made by re-crossmatch – DAT is usually positive • Elutions are performed to identify Ab 17

White Cell Reactions Febrile Reactions • • • Most common, 2% of all transfusions Caused from HLAs on the WBCs of the donor that react with the recipient antibody Any component that contains WBCs could cause FNHTRs Cytokines IL-1, 6, 8 and Tnf-alpha generated in stored blood/products. Determining factor is age of blood products Leukocytes reduced units may be given 18

Pulmonary Infiltrates • Transfusion Related Acute Lung Injury • Can be due to: – Hypervolemia – Donor antibodies that react with the recipient’s granulocytes or vice versa • which cause embolism to blood vessels in lung tissue • Then fluids and proteins leak into alveolar space/ interstitium • The lungs fill with a high-protein fluid • Patient displays acute respiratory insufficiency with x-ray showing pulmonary edema without cardiac failure 19

Graft-versus-Host Disease • Rare but fatal condition that has a 90% mortality rate • May be caused by donor lymphocytes transfused into an immunocompromised recipient – acute graft-versus-host-disease is characterized by selective damage to the liver, skin and mucosa, and the gastrointestinal tract • Any components that contain T-lymphocytes should be irradiated to prevent GVHD 20

Platelet Reactions Post Transfusion Purpura (PTP) • PTP characterized by severe consumptive thrombocytopenia • Typically in women with a history of pregnancy, immunized with Human platelet Specific Alloantigen (HPA) • Thrombocytopenia is self-limiting and lasts for 26 weeks • Occur in patients who are negative for HPA-1 a 21

Plasma Protein Reactions Anaphylaxis • Cause • Infusion of Ig. A proteins into Pt with Ig. A antibodies • Ig. A deficiency about 1 in 700 • Hypotension and bronchospasm • Transfusion should be stopped immediately • Ig. A deficient patients should be transfused with blood products lacking Ig. A 22

Urticaria • Second most comon type of TR • Characterized by a pruritic rash during or following transfusion • Allergic reactions are Ig. E mediated. • These reactions are usually attributed to hypersensitivity to soluble allergens found in the transfused blood component. • Associated with anti-Ig. A in recipients who are Ig. A deficient. 23

Urticaria • If not accompanied by other signs or symptoms, transfusion can be continued • Anti-histamines are given 24
- Slides: 24