Transforming Diabetes Care c 1 Transforming Diabetes Care

Transforming Diabetes Care (c) 1

Transforming Diabetes Care Program Content • Product training to enhance care • Applying the Chronic Care Model to diabetes • • • care Reimbursement through improved coding New standards, guidelines and decision points in therapy Changing behaviors in healthcare (c) 2
Transforming Diabetes Care How adults learn… What I hear, I forget; What I see, I remember; but what I do, I understand. ” ~ Confucius, 451 B. C (c) Problem solving, role playing, case studies, myths and truths, downloading, testing, injecting, “pumping” 3

• What proportion of people with diabetes have… – Controlled BP (<130/80 mm. Hg) – LDL at the goal level (<100 mg/dl) – A 1 C at the goal level (<7%) • What proportion have met all three? (c) 4

• What proportion of people with diabetes have… – Controlled BP (<130/80 mm. Hg) 40% – LDL at the goal level (<100 mg/dl) 36% – A 1 C at the goal level (<7%) 49. 8% • What proportion have met all three? 7. 3% Sayday, et al JAMA 2004; 291: 335 (c) 5

(c) Wagner EH. Chronic disease management: What will it take to improve care for chronic illness? Effective Clinical Practice. 1998; 1(1): 2 -4. ] 6

Looking at Our Practice: Questions we should ask ourselves • • • What aspects of the model can we adopt? Which guidelines will we follow? How do we make sure our coding is correct? Who in our community do we involve? Would we benefit from a diabetes registry? (c) 7

Meet Joel Henderson and his family – 43 yr old obese male – Type 2, HTN, dyslipidemia, sleep apnea – Family hx - heart disease, depression – A 1 c 8. 6% – BP 146/96 – Chol 192 Admits his diabetes is not a priority Busy stressful life “My wife worries about my diabetes for me” Understands family history and risks Adult daughter and granddaughter recently moved back home “I really don’t know what questions to ask. ” 8
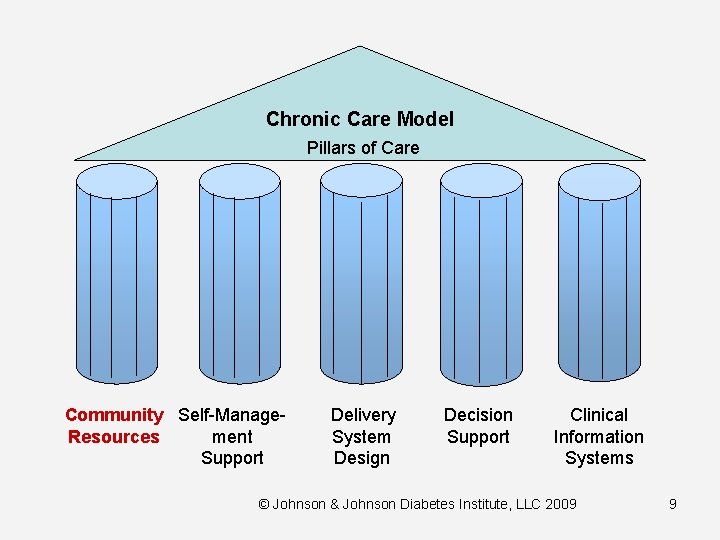
Chronic Care Model Pillars of Care Community Self-Manage. Resources ment Support Delivery System Design Decision Support Clinical Information Systems © Johnson & Johnson Diabetes Institute, LLC 2009 9

Community Resources and Collaborations • • • Local Malls (for ‘mall walking’) Public Library Local Restaurants Beauty Salons Barber Shops Parks & Recreation Dept. Visiting Nurse Organizations Literacy Volunteers of American Diabetes Association Local Senior Centers Local Health Care Providers (c) • • Churches Service Organizations Housing Authority Grocery Stores Schools Local Worksites Media 10
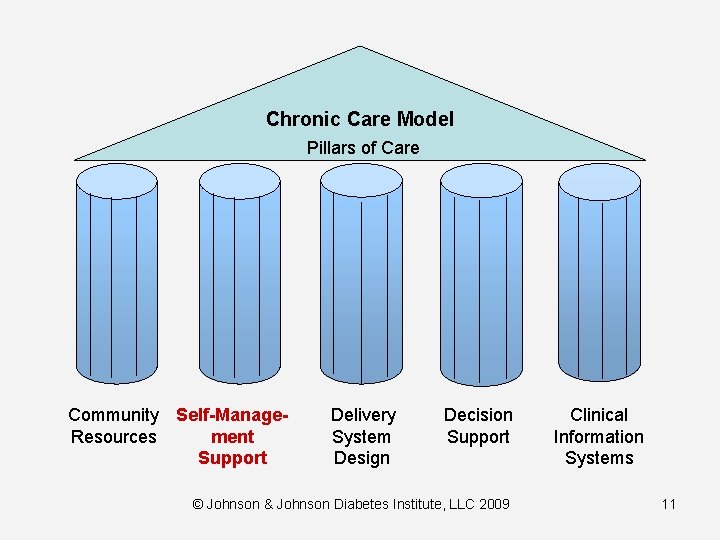
Chronic Care Model Pillars of Care Community Self-Manage. Resources ment Support Delivery System Design Decision Support © Johnson & Johnson Diabetes Institute, LLC 2009 Clinical Information Systems 11

Self-Management Support • Joel’s role includes: – Testing his blood glucose – Learning food’s effect on his glucose – Begin exercising regularly • Our role includes: – Assessing his readiness to make these changes – Provide visits and perhaps referrals that support his efforts such as: • Medical Nutrition Therapy • Diabetes Self Management Education – Provide support (c) 12

Self-Management Support Medical Nutrition Therapy Referral Joel and his wife learn: • Relationship between his food choices and his glucose control • Value of SMBG in helping him make food choices • Effects of exercise on glucose control (c) 13

Self-Management Support Changing Behavior “Joel won’t change his eating habits. ” “Joel isn’t getting enough exercise. ” “I can’t seem to get through to him!” Our role: Assess where Joel is on the road to change Work to motivate him to change behaviors Tools that can help: Importance and Confidence Rulers (c) 14

Chronic Care Model Pillars of Care Community Resources Self-Management Support Delivery System Design © Johnson & Johnson Diabetes Institute, LLC 2009 Decision Support Clinical Information Systems 15

Delivery System Design Shared Medical Appointments Benefits of SMA • Improves access to good care • Improves patient satisfaction • Improves patient-provider communication (c) 16
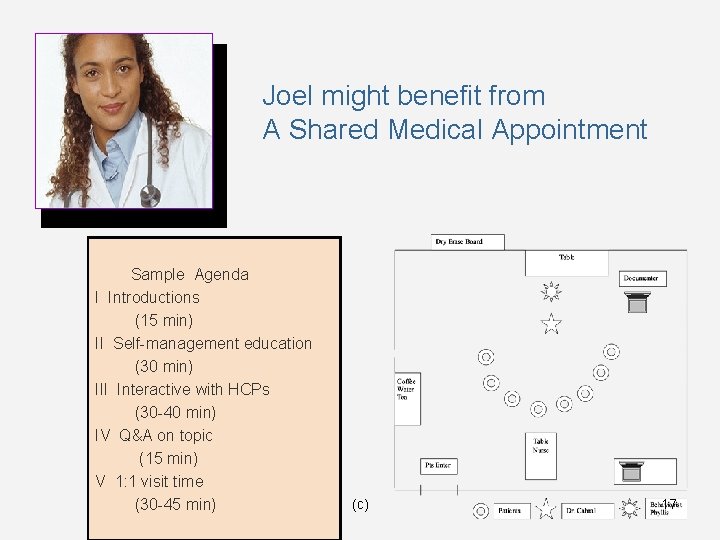
Joel might benefit from A Shared Medical Appointment Sample Agenda I Introductions (15 min) II Self-management education (30 min) III Interactive with HCPs (30 -40 min) IV Q&A on topic (15 min) V 1: 1 visit time (30 -45 min) (c) 17

Benefits of Shared Medical Appointments to our practice include: ü Fewer ER visits/admissions ü Patient retention ü Increased satisfaction ü Efficiency ü Less isolation CLEVELAND CLINIC JOURNAL OF MEDICINE, VOLUME 71, NUMBER 5, MAY 2004 (c) 18
Chronic Care Model Pillars of Care Community Resources Self-Management Support Delivery System Design Decision Support © Johnson & Johnson Diabetes Institute, LLC 2009 Clinical Information Systems 19
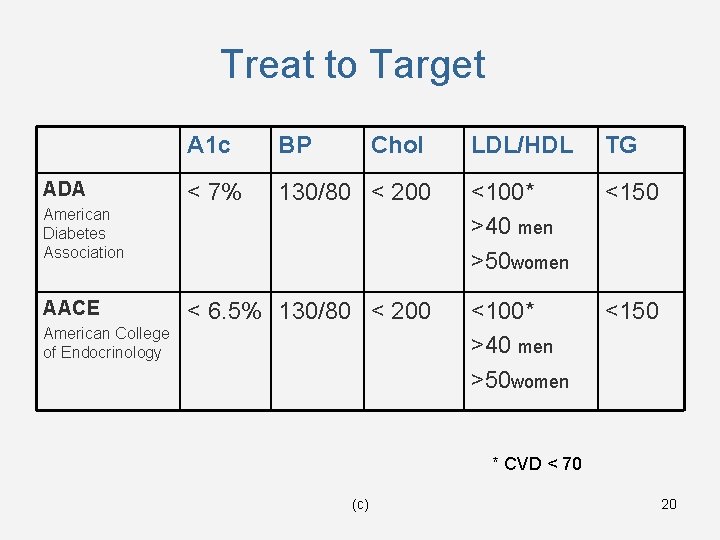
Treat to Target ADA A 1 c BP Chol < 7% 130/80 < 200 American Diabetes Association AACE < 6. 5% 130/80 < 200 American College of Endocrinology LDL/HDL TG <100* >40 men >50 women <150 * CVD < 70 (c) 20
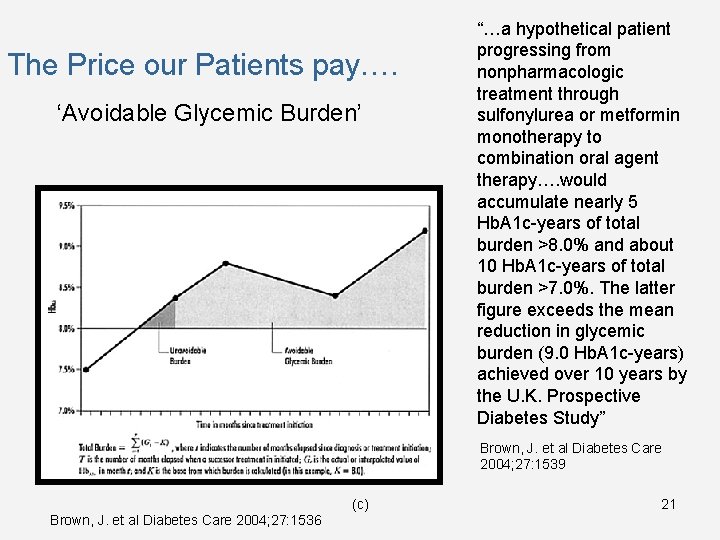
The Price our Patients pay…. ‘Avoidable Glycemic Burden’ “…a hypothetical patient progressing from nonpharmacologic treatment through sulfonylurea or metformin monotherapy to combination oral agent therapy…. would accumulate nearly 5 Hb. A 1 c-years of total burden >8. 0% and about 10 Hb. A 1 c-years of total burden >7. 0%. The latter figure exceeds the mean reduction in glycemic burden (9. 0 Hb. A 1 c-years) achieved over 10 years by the U. K. Prospective Diabetes Study” Brown, J. et al Diabetes Care 2004; 27: 1539 (c) Brown, J. et al Diabetes Care 2004; 27: 1536 21
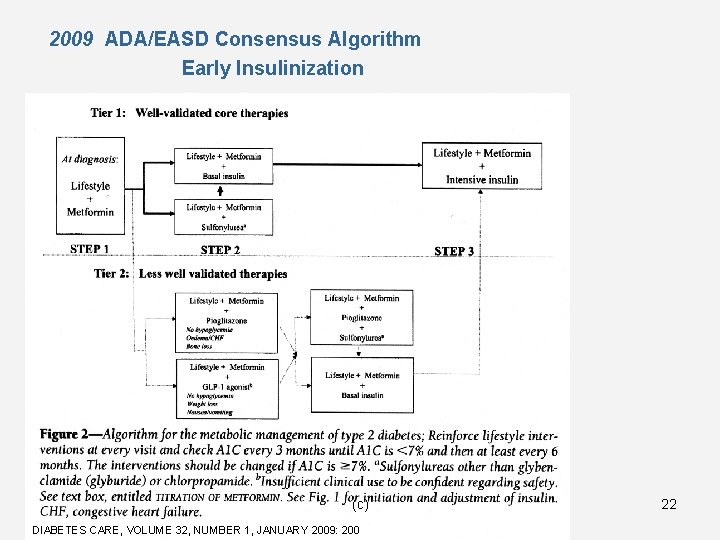
2009 ADA/EASD Consensus Algorithm Early Insulinization (c) DIABETES CARE, VOLUME 32, NUMBER 1, JANUARY 2009: 200 22
Early Insulinization • • • Barrier Frequent Hypoglycemia Weight gain Needle phobia • • Guilt and failure • • Time to titrate • Solution Analogue insulins RD consult, metformin “Adam’s technique”, an insulin injection technique Explain progressive nature of diabetes “Do it yourself” algorithms prescribed by the healthcare professional (c) 23

As an office, we need to define Decision Support resources for us • Using evidence based guidelines – Define targets and algorithms • ADA, AACE, Staged Diabetes Management etc • Regular updates (c) 24

A decision point… Joel is now on max doses of metformin and glyburide. His A 1 C is 7. 0% today. What is the likelihood that it will be above 7. 0% on his next visit in 6 months? (c) 25
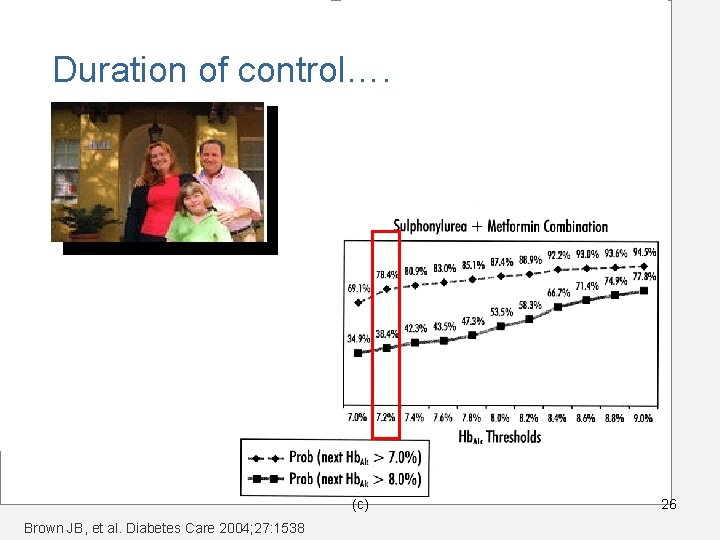
Duration of control…. (c) Brown JB, et al. Diabetes Care 2004; 27: 1538 26

Decision Points involve a number of factors – TARGET • What is the goal you are shooting for? – METHOD • What is your choice of therapy to get there? – TIMING • When do you decide it isn’t working? • How often do you make changes? (c) 27
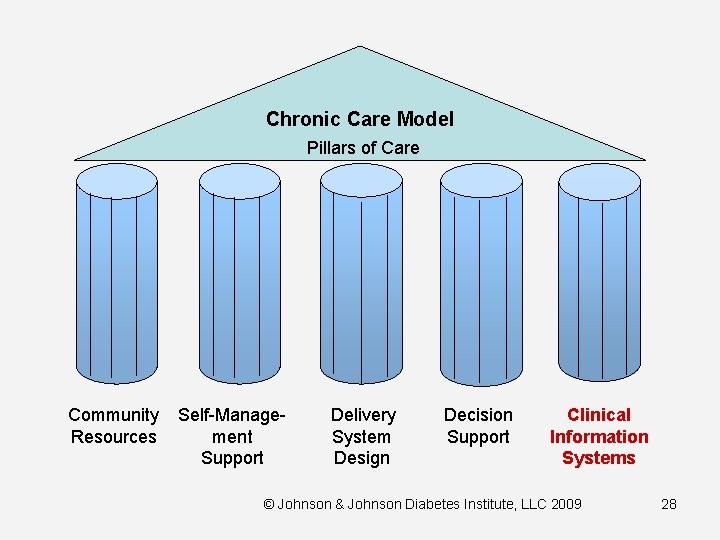
Chronic Care Model Pillars of Care Community Resources Self-Management Support Delivery System Design Decision Support Clinical Information Systems © Johnson & Johnson Diabetes Institute, LLC 2009 28

Clinical Information Systems • • EMRs Diabetes Registry Real time data Identifies gaps in care Care reminders and feedback Individual patient care planning Proactive population-based care (c) 29

Reimbursement Barrier • Identifying all billable Solution • Find a coder to identify • • • moments Not getting reimbursed for diabetes education Not paid for preventive counseling -“Diet and Exercise” Knowing what can be billed on the same day Cannot bill for MNT + DSMT on same office visit • • (c) billable moments ADA Recognition will open doors Always get a referral for DSMT and for MNT Get referrals for additional hours of MNT if requested from the professional for treatment changes 30

Key Learnings • Recognize barriers and provide solutions to: – Treat to target • Early insulinization – Reimbursement • New approaches – Changing behaviors • Assessing readiness (c) 31

How will we change our practice? As a practice, which of these key learnings should we implement ? And when do we begin ? (c) 32

(c) 33
- Slides: 33