Transformation towards becoming a Patient Centered Medical Home

Transformation towards becoming a Patient -Centered Medical Home – A mixed methods approach to measuring system change American Evaluation Association Conference October 2012 Humberto Reynoso-Vallejo, Ph. D Linda Cabral, MM

Project Team § § § § Ann Lawthers, Principal Investigator Terri Anderson Humberto Reynoso-Vallejo Linda Cabral Laura Sefton Bruce Barton Various Others – Thank you! 2

Today’s Session § Overall study design § Assessing one Primary Care Medical Home (PCMH) Core Competency • Enhanced Access 3

Mixed-Methods Evaluation Design of the PCMHI in MA Humberto Reynoso-Vallejo, Ph. D Center for Health Policy and Research UMass Medical School

Overview § Patient Centered Medical Homes and the MA -PCMHI § 46 Practices (+ 19 Comparison) Total n=65 § Mixed-Methods Design 5
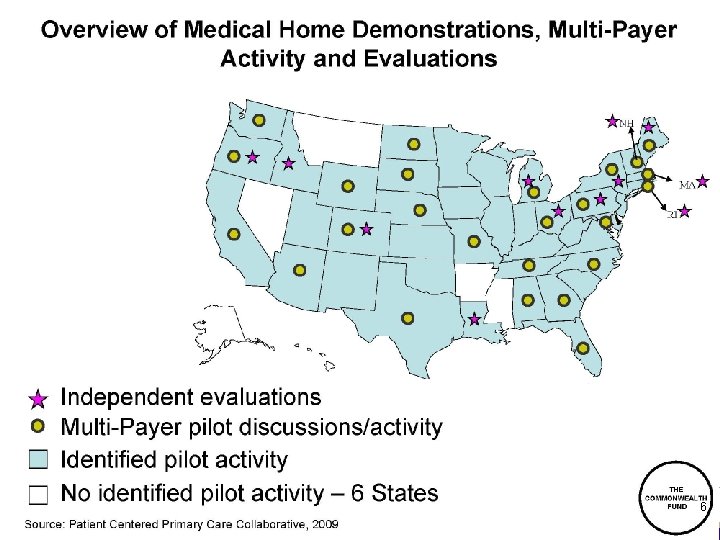
6
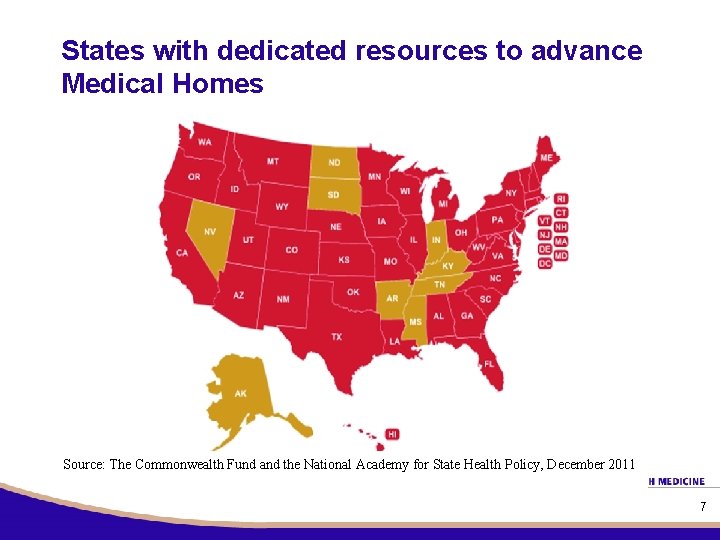
States with dedicated resources to advance Medical Homes Source: The Commonwealth Fund and the National Academy for State Health Policy, December 2011 7

MA Patient-Centered Medical Home Initiative § § § Statewide Initiative Sponsored by MA EOHHS Multi-payer 46 Participating Practices + 19 Comparison 3 year Demonstration Start Date: March 29, 2011 Vision: All MA primary care practices will be PCMHs by 2015 8

MA PCMHI: Objectives § To implement and evaluate the PCMH model as a means to achieve accessible, high quality primary care § To demonstrate cost-effectiveness in order to justify and support the sustainability and spread of the model § To attract and retain primary care clinicians into practice in Massachusetts by increasing resources available to practices and improving their quality of work life 9

MA PCMHI: Practice Redesign 12 Core Competencies • Patient/family centeredness • Team based care • Planned visits & followup care • Registry use for population and patient management • Care coordination • Care management for high risk patients • Self management support • Patient and family education • Shared decision making, patient action plans • Evidence based care • Integration of QI • Enhanced access 10

Practice Groups § Technical Assistance plus Payment (TA+P) n=18 § Technical Assistance Only (TAO) n=14 § Technical Assistance plus Payment + Qualis (TA+P+Q) n=14 § Comparison n=19 § Total Practice Groups n= 65 11

MA PCMHI: Evaluation Questions • To what extent do practices become medical homes? • To what extent and in what ways do patients become active partners in their health care? • What is the initiative’s impact on service use, costs, clinical quality, patient and provider outcomes? 12

Evaluation Methods Design § Mixed–Methods • Descriptive, Pre-Post with Comparison Group 13

Evaluation Methods Design Qualitative Data Sources: • Interviews and focus groups • Participant observation at Learning Sessions • Site Visits Quantitative Data Sources: • Medical Home Quotient Index (MHIQ) • Staff Member Satisfaction • Patient Experience Survey (CAHPS) • Claims data, clinical quality measures 14

Qualitative Analysis § In-depth semi-structured individual interviews and focus groups with MHF’s § Atlas ti § Summative Analysis § Participation in Learning Sessions § Site Visits 15

Quantitative Analysis § MHIQ Transfor. Med© instrument § Patient Experience Survey (CAHPS) § Staff Member Satisfaction Survey § Claims data, clinical quality measures 16

17

Conclusion § PCMHI § Mixed-methods for complex evaluations § Innovative approaches 18

Examining Enhanced Access in the Implementation of a Medical Home Linda Cabral, MM Center for Health Policy and Research UMass Medical School

Overview § § What is enhanced access? Why is it of interest? How is it measured? How did we use qualitative and quantitative data to better under how practices are enhancing access to care for their patients? 20

Enhanced access is the availability of easy and flexible access to the primary care team, including alternatives to face-to-face visits, such as e-mail and telephone. http: //www. mass. gov/eohhs/provider/guidelines-resources/services-planning/pcmhi/about/core-competencies. html 21

PCMHI Core Competency: Enhanced Access MHIQ Questions § Access to Care and Information (9 questions) • Same-Day Appointments • After-Hours Access Coverage • Accessible Patient and Lab Information • Online Patient Services • Electronic Visits • Group Visits 22

Time 1 Data Collection 23
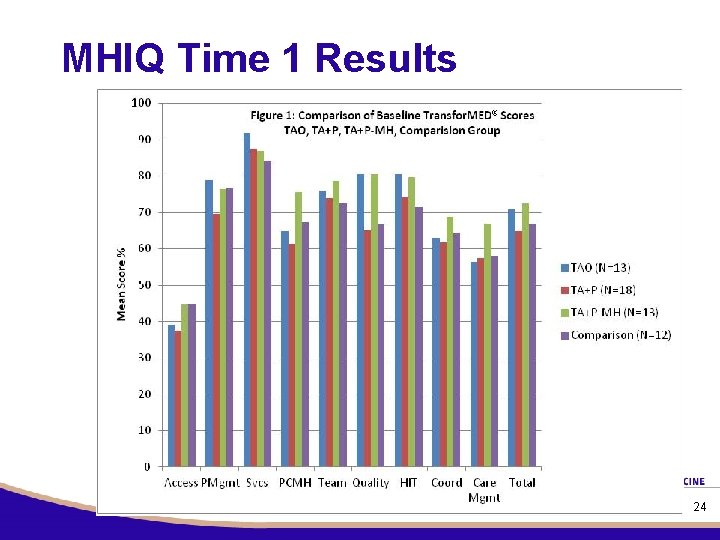
MHIQ Time 1 Results 24
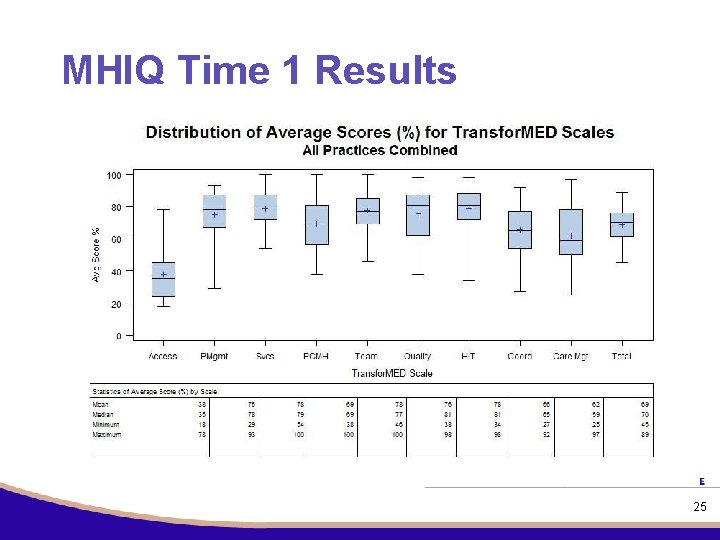
MHIQ Time 1 Results 25

Baseline Qualitative Data on Access Focus Group § We’d like to understand how you work with the practices to address the PCMHI initiative’s core competencies. What types of activities do you conduct with the practices? • Do practices view some competencies as more important than others? If so, which ones? 26

Baseline Qualitative Data on Access Individual Interviews Among the practices with whom you work, what are sites doing to enhance patient access to care? 27

Time 1 Qualitative Results § Competency in enhanced access depends: • Empanelment • Teamwork/collaboration across the practice staff • Managing patient flow within the office § One way that practices strived to meet this core competency was to introduce open access. This was met with varying levels of satisfaction among providers and patients. 28

Time 1 Qualitative Results § New positions such as “Access Facilitator” and “Patient Navigator” are being introduced in some practices. § Some practices feel that they have no access issues 29

Time 2 Data Collection 30
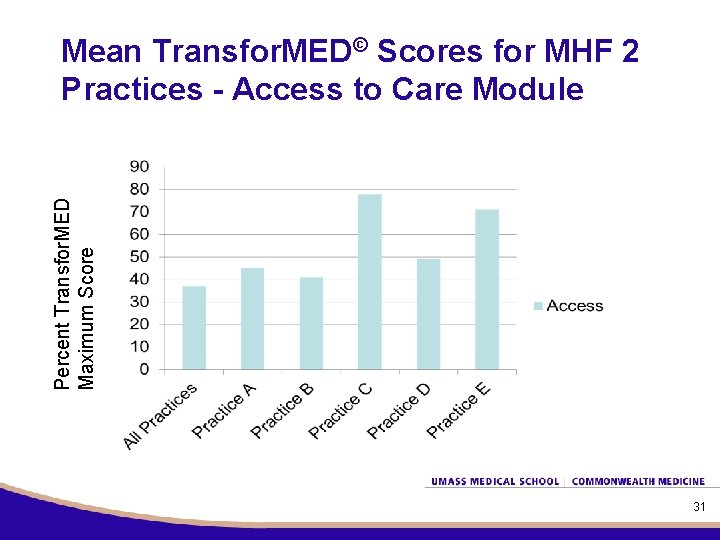
Percent Transfor. MED Maximum Score Mean Transfor. MED© Scores for MHF 2 Practices - Access to Care Module 31

Time 2 Qualitative Data Collection Q: We have a chart here which shows the Transfor. MED© survey scores which your practices achieved as well as the total for all practices for Access Domain. These data reflect the practice responses from March. From your knowledge, how do these scores reflect these practices? 32

Time 2 Qualitative Results § Practices are working on enhancing access by working in teams to increase chances of being able to be seen by team member, better utilizing their MA being smarter about scheduling, and hiring LPNs to offload RNs to offload NPs to offload MDs § Challenges arise when a practice has many part time providers, a residency program, or has a lot of turnover 33

Time 2 Qualitative Results § Access and continuity are intertwined; one can affect the other. Team-based care, where the patient is familiar with more than one provider, can mitigate potential problems. § Practices are working on Access and Empanelment at the same time. In order to ensure that visit time is adequate, the panels need to be the appropriate size. 34

35

Reactions § Thoughtful insights provided § Gained much more practicespecific information • However, the more practices a MHF had, the less practicespecific data we were able to gather 36

Using this Mixed Methods Approach… § Assumes participants have a certain comfort level with quantitative data § Allows for unique insights of the quantitative data § Generates a better understanding among participants of how quantitative data is being used 37

Contact Information Humberto. Reynoso@umassmed. edu 508 -856 -1531 Linda. Cabral@umassmed. edu 508 -856 -8423 38
- Slides: 38