TransferenceFocused Psychotherapy for Borderline other Personality Disorders Lietuvos

Transference-Focused Psychotherapy for Borderline & other Personality Disorders Lietuvos Psichoanalizès Draugija Vilniaus Universitetas Medicinos Fakultetas Psichiatrijos Klinika September 2, 3, 4, 2016 Frank Yeomans, M. D. , Ph. D. Personality Disorders Institute/Weill Cornell Medical College Columbia Center for Psychoanalysis International Society for TFP Borderline Personality Disorder Resource Center

Websites Personality Disorders Institute/Weill Cornell Medical College Borderlinedisrorders. com International Society for TFP www. istfp. org Borderline Personality Disorder Resource Center BPDresourcecenter. org

PERSONALITY DISORDERS INSTITUTE Weill Cornell Medical College Otto F. Kernberg, M. D. , Director John F. Clarkin, Ph. D. , Co-Director Nicole Cain, Ph. D Eve Caligor, MD Monica Carsky, Ph. D Jill Delaney, MSW Mark Lenzenwger, Ph. D Kenneth Levy, Ph. D Kevin Meehan, Ph. D Lina Normandin, Ph. D Diana Diamond, Ph. D Barry Stern, Ph. D Karen Ensink, Ph. D Michael Stone, MD Catherine Haran, Psy. D Alan Weiner, Ph. D Frank E. Yeomans, MD

Key TFP Manuals Yeomans FE, Clarkin JF, Kernberg OF. Transference. Focused Psychotherapy for Borderline Personality: A Clinical Guide. Washington: American Psychiatric Press (2015). Yeomans FE, Clarkin JC, Kernberg OF. A Primer on Transference-Focused Psychotherapy for Borderline Patients. Northvale, NJ: Jason Aronson; 2002. Caligor, E. , Kernberg O. F. & Clarkin, J. F. (2007). Handbook of Dynamic Psychotherapy for Higher Level Personality Pathology. Washington, DC: American Psychiatric Publishing.

An Early Book on Contracting Yeomans FE, Selzer MA, Clarkin JF. Treating the Borderline Patient: A Contract-Based Approach. Basic Books, New York; 1992

Principle TFP Manuals 2015 2002

Key TFP Books 2007 1992

Main research articles • Clarkin, J. F. , Levy, K. N. , Lenzenweger, M. F. , & Kernberg, O. F. (2007). Evaluating three treatments for borderline personality disorder: a multiwave study. American Journal of Psychiatry, 164, 922 -928. • Levy, K. N. ; Meehan, K. B. ; Kelly, K. M. ; Reynoso, J. S. , et al (2006). Change in attachment and reflective function in the treatment of borderline personality disorder with transference focused psychotherapy. J of Consulting and Clinical Psychology 74: 1027 -1040. • Doering, S. et al (2010). TFP vs. treatment by community therapists for BPD: RCT. British Journal of Psychiatry , 196(5)

Educational Objectives • Understand psychodynamic approaches to severe personality disorders: – Personality structure and identity – Phenomenology and functioning • • Understand basic object relations theory Understand basic assessment and its importance Understand treatment contracting Understand strategies, tactics and techniques of TFP • Identify patterns of change in treatment – Evolution of therapy: early, middle, late phases

What is TFP? An evidence-based manualized individual outpatient therapy for serious personality disorders It combines structure and limit-setting with an exploratory psychodynamic approach to target the split, intrapsychic structure that results in the borderline phenomenology

Some Key Differences with Traditional Psychodynamic Therapy - 1 n The therapist is more active n The therapist has a sense of the priorities to address (in contrast to pure free association) n The initial focus is on the here-and-now of the interaction between patient and therapist: this activates the patient’s affect systems so that affect and cognition are present together

Some Key Differences with Traditional Psychodynamic Therapy - 2 n Interpretations are based on the idea that “an affect is the manifestation of an underlying object relation”

Goals and objectives of TFP n Phase I: The containment of acting out behaviors n Phase II: Core of the treatment - the resolution of identity diffusion and the development of a coherent sense of self and others

The Resolution of Identity Diffusion • This is done through fostering reflection on mental states of self and other • The reflection focuses of the patient’s split internal world where representations of self and others are divided into radically opposed extremes

Who is TFP for and why learn it? - It is for patients with personality disorders at the borderline level of personality organization BPO (not just BPD in narrow sense) - These include borderline personality disorder, narcissistic personality disorder, histrionic, dependent and avoidant PD - The goal of TFP is to go beyond symptom change and effect change in the personality that makes it possible to find satisfaction in work and love.


What do we mean by a manual? – A book: derived from discussing videotapes of analysts’/therapists’ – Viewing videos – Peer supervision, with an emphasis on countertransference and projective identification – Overarching concept: principle-driven – Rating adherence and competence

What are the elements of our manualized therapy? • Diagnosis-specific • Articulate specific treatment goals [how specific? ] • Set the Contract (v. “meet the patient”) • Look for activated dyads in the here-and-now • Conceptualize drives and defenses as embodied in dyads

Elements of manualization – cont’d • Respect priorities of intervention (v. free association, which can be in the service of defense and omnipotent control) • Increased level of therapist activity • use interpretations, starting with “experience-near” • On-going attention to the patient’s “external life”

Manualization in the context of a research study • one impact: staying with the case • on and off- camera: the drift to be supportive – drift as developing one’s individual style of therapy – drift as colluding with resistance to deep exploration. The ucs never loses its potential to make us uneasy

TFP – Focus on the intrapsychic – Why bother working at this level? • Symptom Change • Change in sense of self and experience of the world • Change in underlying psychological functions • Satisfaction in love and work – a ”full” life

How do we consider personality?

Two Dominant Approaches to PERSONALITY • Dispositional or trait theory approach: goal is to characterize people in terms of a comprehensive but small set of stable behavioral dispositions • Processing approach: personality as a system of mediating units (expectancies, goals, motives) and psychological processes (cognitive-affective units) that interact with the situation Mischel & Shoda, 1999

Four Aspects of Psychological Processing • Organized pattern and sequence of activation of cognitive-affective mental representations • Behavioral expressions of individual’s processing • Perceptions of self across situations • Particular environments the individual seeks out and constructs Mischel & Shoda, 1999

Personality - 1 • It is an umbrella concept: the total psychological structure and functioning of the individual • It is a permanent organization of how one perceives and reacts to stimuli – it involves how one perceive self and other • Assessment of and adaptation to the environment Ref: Kernberg & Caligor (2005). A psychoanalytic theory of personality disorders. In: Major Theories of Personality Disorders, 2 nd Ed. Eds: Clarkin & Lenzenweger. NY, Guilford, 115 -156.

Personality - 2 • To understand personality organization, we describe the major personality structures (combinations of functions that group together at the biological or psychological level): –Temperament –Character –Identity –Ethical values –Intelligence/Cognition

Using Structural Features of Personality to Develop a Diagnostic System for Personality Disorders • The focus is on key psychological processes (“structures”) that process information and affects, thus influencing behavior • This focus leads to the concepts of “Structural diagnosis” and “level of personality organization”

Component Structures of Personality: Temperament arises from genetic endowment and comprised of four motivational systems: appetitive, defensive, aggressive, nuturant Temperament involves individual differences in both motor and emotional reactivity and self-regulation Effortful control is the self regulation dimension of temperament; ability to inhibit a dominant response in order to perform a subdominant response

Temperament and Interaction with Caregivers The combination of temperament and interactions with caregivers leads to the internalization of perceived interactions. These determine habitual ways of perceiving, reacting/behaving, or character traits. • Affects guide the infant to pleasurable stimuli, experiences and away from painful ones. • In interacting with mother, mother may do “right” thing which leads to pleasure, or “wrong” to pain • These experiences internalized as guiding system for future behavior n

Component Structures of Personality: Character: the integration of habitual behavioral patterns into a structure. It is the psychological organization developed from interactions that are internalized and repeated in habitual ways Character structure determines one’s reaction to the environment Character is observable by behavior, affective responses Character is the behavioral manifestation of Identity: ways of thinking, feeling, and relating to the world.

Component Structures of Personality: Identity is the structural correlate of both the subjective sense of self and the experience of significant others Normal identity is manifested subjectively in experiences of self and others that are complex, well differentiated, characterized by subtlety and depth, continuous over time and across situations, flexible and realistic Normal identity is associated with the ability to accurately appreciate the internal experience of others

Component Structures of Personality: Moral Values • Commitment to values and ideals that is consistent, flexible, and fully integrated • A dynamic integration of developmental influences

Component Structures of Personality: Intelligence: the capacity for cognitive assessment The cognitive ability of establishing the context in which affect emerges Analyze reality in more and more complex ways Helps develop symbolic ways of relating to reality Avoids distortions of reality under extreme affects Plays an important role in impulse control Affects become cognitively framed by the action of the cortex

Descriptive Features of Personality Disorder PD’s are distortions of normal personality characterized by: • Rigidity or loss of flexibility of behavior patterns, resulting in poor adaptation • Inhibition of normal behaviors • Exaggeration of certain behaviors • Chaotic alternation between inhibitory and impulsive behavior patterns • Vicious circles develop: abnormal behaviors elicit abnormal responses

Consequences of Personality Disorders: - A reduction in the capacity to adapt to the psychosocial environment and to satisfy internal psychological needs (e. g. , selfaffirmation, sexuality, and dependency). - In turn, personality disorders tend to be reenforced by the pathological responses that patients elicit in their environment.

Structural Features/Variables at the Center of the Diagnostic Sysgtem • Identity - Sense of self and sense of others • Defensive Operations - Customary ways of coping with external stress and internal conflict • Reality Testing - Appreciation of conventional notions of reality • Quality of Object Relations - Understanding of the nature of interpersonal relations • Moral Functioning - ideals and values, expressed in ethical, or unethical behavior

Structural Diagnosis and Levels of Personality Organization • These structural features of personality determine: – Severity of pathology / level of functioning: – Ability to deal with life tasks and with related instinctual impulses (aggression, love, sexuality, and interdependence) • Treatments that effect change at the level of psychological structures result in change at the symptom level and quality of life

Structural Change The overarching goals of TFP are defined in structural terms: • To integrate the identity • To develop more adaptive defenses (to move beyond splitting) and thus enhance coping and adaptation to life

Clinical Manifestations of Structural Change at the level of psychological structures will lead to: • Reduction of symptoms and maladaptive behaviors • Better functioning • Change in the patient’s sense of self and experience of the world • Ability to cope with stress and adversity • Enhanced satisfaction and effectiveness in love and sex, work and social life: living a “full” life

The Structural Classification of Personality Disorders by Levels of Severity Normal personality: Consolidated identity, adaptive defenses, stable RT, flexible moral functioning, full object relations including capacity for intimacy and healthy dependency Neurotic level of personality organization : Rigidity of defenses, inflexible morality, +/- problems with intimacy Borderline level of personality organization : More fully described below – High level borderline: dependent, needy, depressive – Low level borderline: hostile, aggressive Psychotic level of functioning (loss of reality testing)

Borderline Personality Organization Basic Characteristics • Identity Diffusion vs. integrated view of self and others (internal sense of continuity) • Primitive Defenses – – – Splitting Idealization/devaluation Projective identification Omnipotent control Denial • Variable Reality Testing

Prognostic Factors • • Pervasive aggression Antisocial features Secondary gain (chronic support system) Severely restricted object relations No love life; low attractiveness Low intelligence No work or shifting lifestyle Negative therapeutic reaction

Borderline Level of Personality Organization: The Defining Psychological Characteristics and their Clinical Correlates I. Identity pathology – Sense of self and others is fragmented, distorted and superficial – Difficulty “reading” others… and self – Lack of continuity in time – Feelings of emptiness

Borderline Personality Organization: Clinical Correlates of Structural Features II. Splitting- based/Lower level defenses - These dissociative defenses based on splitting involve projecting negative aspects of the self to attempt to avoid anxiety – They lead to unstable, black and white experiences of the world (of self and of others) – They also lead to difficulty modulating affects

Borderline Personality Organization: Clinical Correlates of Structural Features III. Variable Reality Testing – Difficulty distinguish internal and external sources of affect – Deficits in social reality testing – Possible gross distortion under stress with micro-psychotic phenomena

Borderline Personality Organization: Clinical Correlates of Structural Features IV. Pathology of Object relations – Difficulty appreciating the needs of the other independent of the self, difficulty with healthy dependency, difficulty with intimacy V. Pathology of Moral Functioning – Inconsistent or lacking values and ideals – Unethical behavior

Personality Disorders from a Personality Organization Point of View – Levels of Organization A mixed Categorical and Dimensional System 1 -Normal flexibility and adaptation 2 -Neurotic level of personality organization 3 -Borderline level of personality organization: – High level borderline – Low level borderline 4 -Psychotic level of personality organization

The following slide shows: The relationship between familiar, prototypic, personality types and structural diagnosis. Severity of illness ranges from mildest, at the top of the page, to extremely severe at the bottom. Arrows indicate range of severity. Kernberg & Caligor (2005). A psychoanalytic theory of personality disorders. In: Major Theories of Personality Disorders, 2 nd Ed. Eds: Clarkin & Lenzenweger. NY, Guilford, 115 -156.
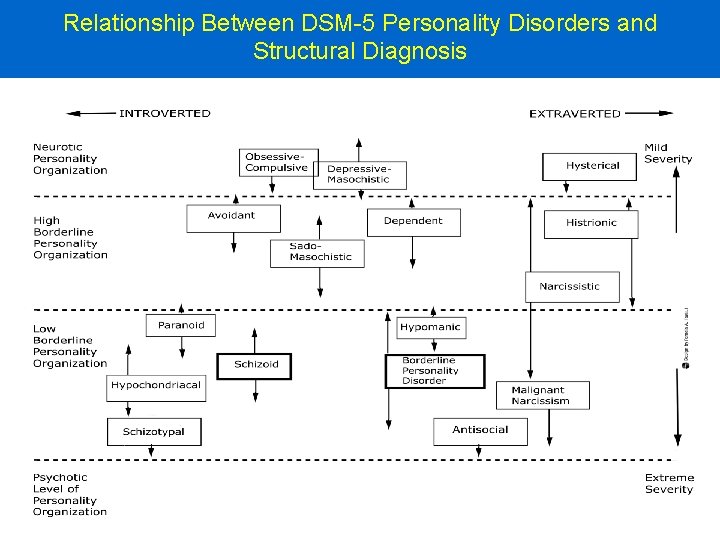
Relationship Between DSM-5 Personality Disorders and Structural Diagnosis

Comparison with DSM 5 –PD Diagnostic Criteria: Section 3 A. Degree of Impairment in Personality Functioning 1. Identity: frail or distorted experience of self 2. Self-direction: unrealistic standards and goals 3. Empathy: limited capacity to understand feeling and behaviors of others, and one’s own impact on them 4. Intimacy: limited capacity to establish enduring and mutually satisfactory relations with others B. Abnormal Personality Traits Negative affectivity Detachment Antagonism Disinhibition Psychoticism

Etiology of BPD • A complex etiology: no single pathway • Genetic Disposition, involving: – – Neurotransmitter Systems Abnormal Affectivity: Negative affects, aggression Abnormal control of affects/constraint system Temperament • Object Relations – Chronic chaotic relations and blurring of generational boundaries – Neglect – Trauma/Abuse – Insecure/Disorganized Attachment

Neurobiology and Object Relations Theory • The primitive mental mechanism of splitting and its derivatives are based on biological developments of separate positive and negative affective systems • There is the potential of integrating these at a cortical level of processing • Intrapsychic structures reflect a second level of organization, based upon the primary neurobiological one • The integration of self and of object representations depends on the predominance of positive relationships, and is threatened by the predominance of ones charged with negative affects

Getting back to What is TFP? An evidence-based manualized individual outpatient therapy for serious personality disorders It combines structure and limit-setting with an exploratory psychodynamic approach to target the split, intrapsychic structure that results in the borderline phenomenology What is “Psychodynamic”? : -the mind in motion/conflict -the view that symptoms can be related to underlying conflicts

Why use TFP? First: theory behind the treatment An object relations theory understanding of the split internal psychological structure as the basis for Identity Diffusion and the clinical picture of borderline pathology.

Treatments for Borderline Personality • Psychopharmacology – Mood Stabilizers, Low-dose Neuroleptics, SSRI’s • Psychotherapy – Cognitive Behavioral • Dialectical Behavior Therapy (Linehan) • Schema Therapy (Young) – Psychodynamic • • Supportive Psychotherapy (Rockland; Appelbaum) Mentalization-Based Therapy (Batemen &Fonagy) Eclectic; Supportive-Expressive (Gunderson; Gabbard) Transference-Focused Psychotherapy

Treatments: The Cochrane Meta-Analysis of Therapy Research • Beneficial effects of psychotherapeutic interventions for BPD • DBT has been studied most intensively, followed by MBT, TFP, SFT and STEPPS • None of the treatments has a very robust evidence basis • There are some concerns regarding the quality of individual studies • Overall, the findings support a substantial role for psychotherapy in the treatment of BPD but clearly indicate a need for replication studies

Introducing theory behind the treatment The concept of the split internal psychological structure as the basis for Identity Diffusion and the clinical picture of borderline pathology described thus far.
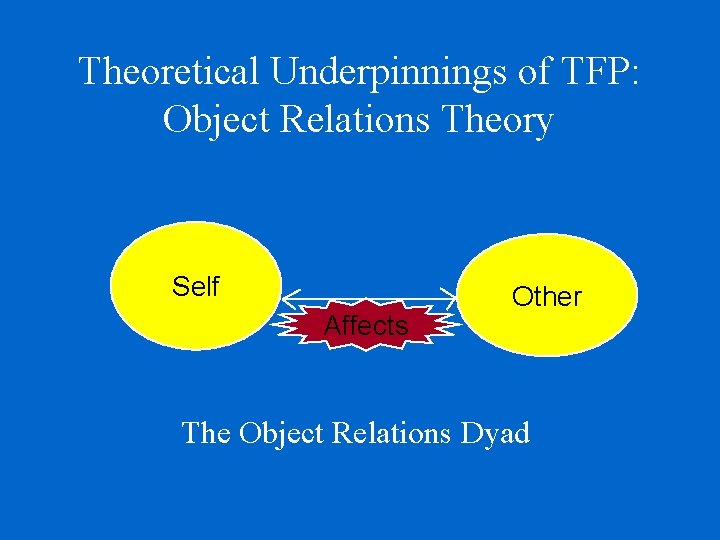
Theoretical Underpinnings of TFP: Object Relations Theory Self Affects Other The Object Relations Dyad
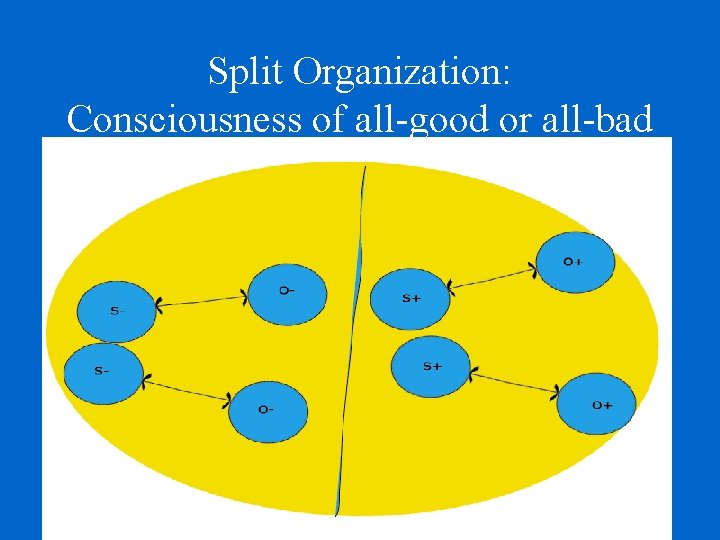
Split Organization: Consciousness of all-good or all-bad

Normal Organization: Consciousness of Integration/complexity


The Evolution of Treatment From Splitting to Integration; From the projection of negative motivations to the capacity to take responsibility for one’s thoughts, feelings, actions and integrate them. (In older psychoanalytic terminology, to move from the Paranoid-schizoid position to the Depressive position) --------------------- How does focusing on the transference facilitate this change?

Transference • The activation of internal object relations in the relationship with therapist. • These internalized relations with significant others are not literal representations of past relations, but are modified by fantasies and defenses. • In borderline patients, internal object relations – have been segregated and split off from each other; – include fantasied persecutory and idealized relations. • Working with object relations that are activated in the immediate moment creates a therapy that is “experience-near”

Working with Transference • Since transference is the activation of internal object relations leads to the activation of affects and conflicts, the basic strategy is to: – to tease out these internal relationships, – to help the patient • Gain and tolerate awareness of these internal relationship representations, • Integrate them into a coherent whole, and • Generalize the experience in therapy to other relations
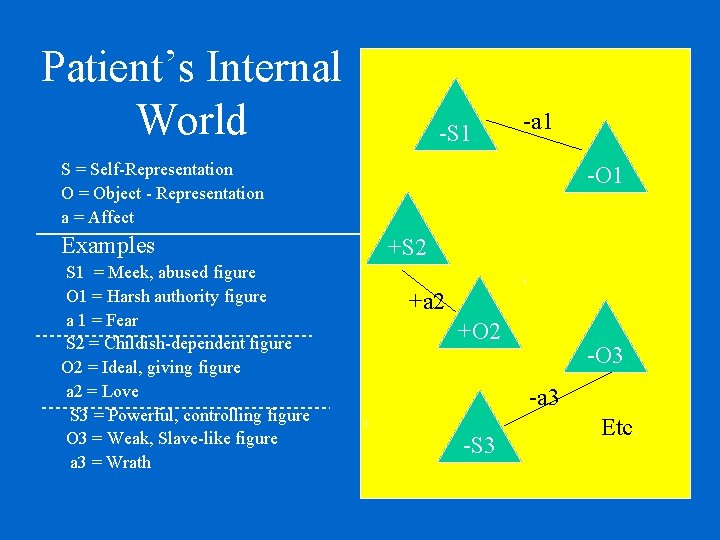
Patient’s Internal World -S 1 -a 1 S = Self-Representation O = Object - Representation a = Affect Examples S 1 = Meek, abused figure O 1 = Harsh authority figure a 1 = Fear S 2 = Childish-dependent figure O 2 = Ideal, giving figure a 2 = Love S 3 = Powerful, controlling figure O 3 = Weak, Slave-like figure a 3 = Wrath -O 1 +S 2. +a 2 +O 2 -O 3 -a 3 -S 3 Etc.

Why focus on TRANSFERENCE? (the immediate experience of self and other) • Experience of Self a 1 S 1 O 1 S 2 S 3 • …and of therapist a 2 a 3 O 2 O 3
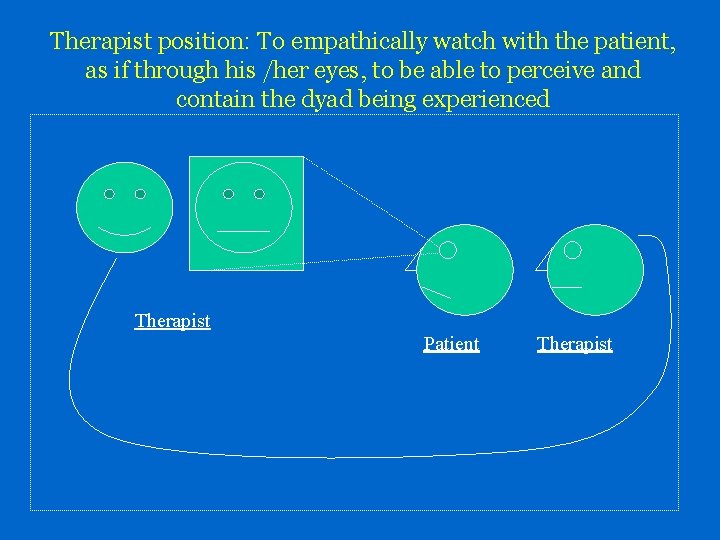
Therapist position: To empathically watch with the patient, as if through his /her eyes, to be able to perceive and contain the dyad being experienced Therapist Patient Therapist
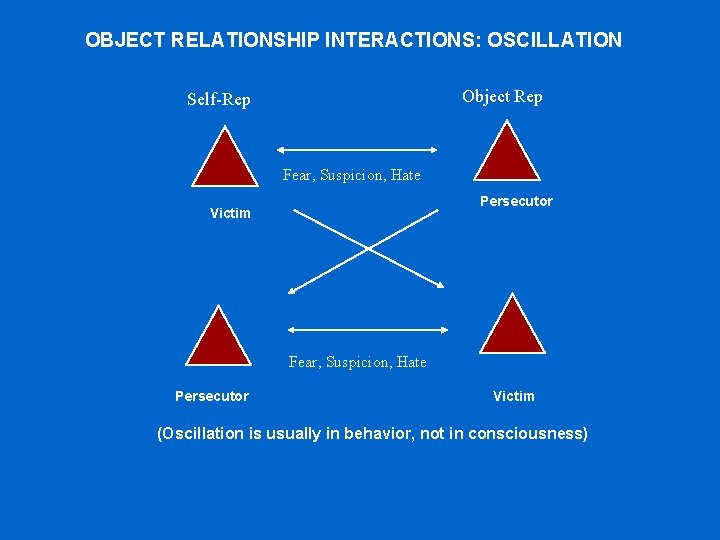
OBJECT RELATIONSHIP INTERACTIONS: OSCILLATION Object Rep Self-Rep Fear, Suspicion, Hate Persecutor Victim (Oscillation is usually in behavior, not in consciousness)
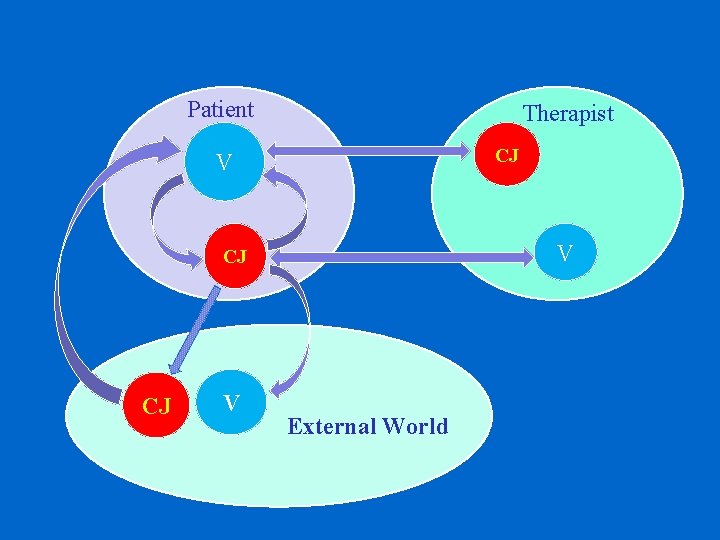
Patient Therapist CJ V V CJ CJ V External World
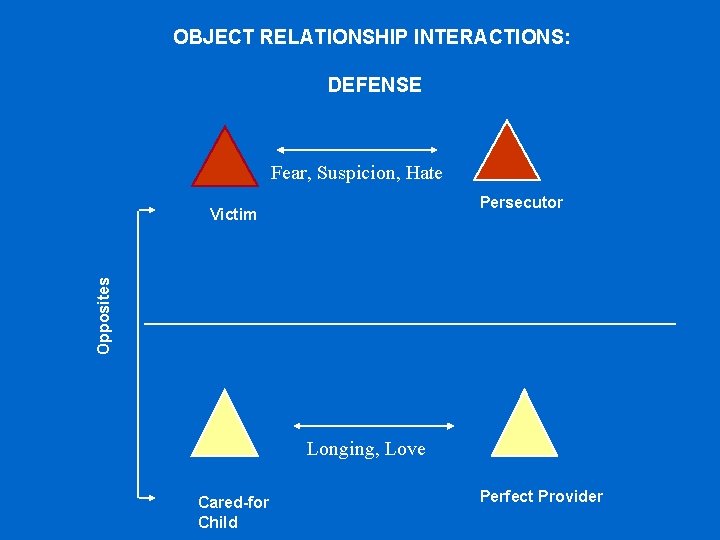
OBJECT RELATIONSHIP INTERACTIONS: DEFENSE Fear, Suspicion, Hate Persecutor Opposites Victim Longing, Love Cared-for Child Perfect Provider
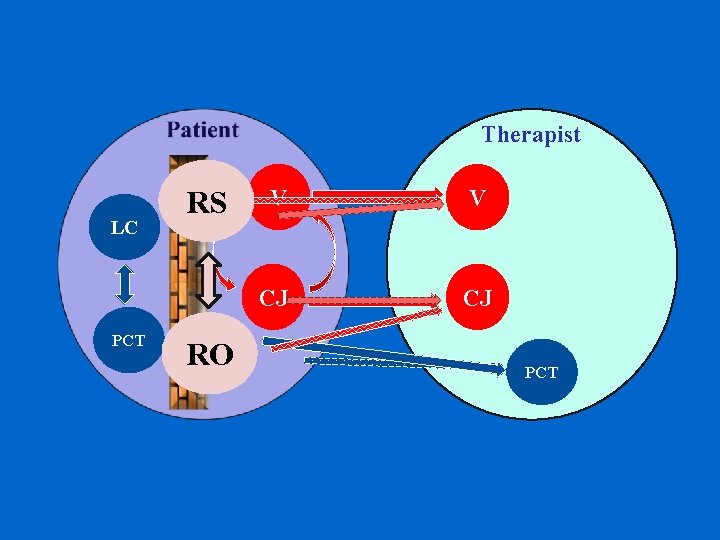
Therapist LC PCT RS RO V V CJ CJ PCT

TFP - What Changes? Clinical improvement results from structural change • Increased reflection, facilitated by: – Holding function of therapist – Interpretation • Decreased splitting • Identity consolidation

TFP- Summary of the Process of Change • Exploration of internal object relations as activated in interpersonal relations • Focus first on the transference, then on other affectladen material • Enhance mentalization through exploration of internal states; this provides cognitive containment of affect through exploration of psychological experience in the “here-and-now” • Promote integration by confronting and interpreting splitting and associated defensive operations • Integration and decreased splitting enhance – The capacity to contain affective states and reflect upon them – The capacity to appreciate self and others in more fullness and depth

Moving from Theory to Therapy A treatment that has been developed in a clinical research context over the past 25 years
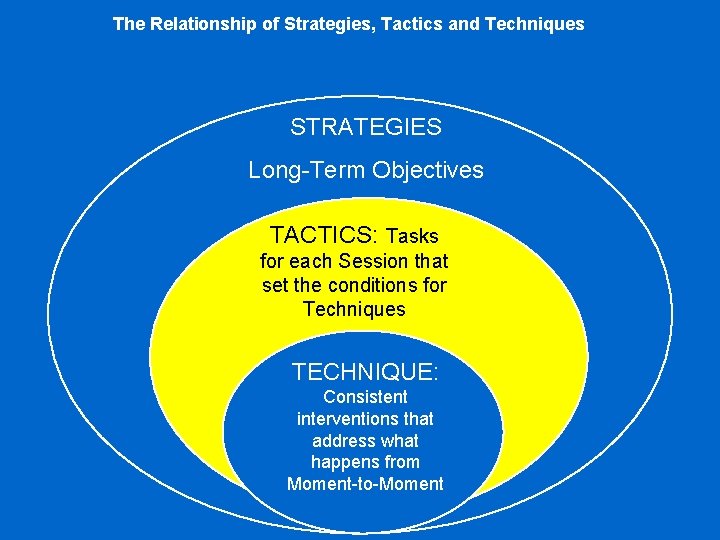
The Relationship of Strategies, Tactics and Techniques STRATEGIES Long-Term Objectives TACTICS: Tasks for each Session that set the conditions for Techniques TECHNIQUE: Consistent interventions that address what happens from Moment-to-Moment

The Specific Strategies - I Strategy 1: Defining the dominant object relation Step 1: The therapist experiences and tolerates the confusion of the patient’s inner world as it unfolds in the transference Step 2: The therapist identifies and formulates in his/her mind the object relation that is dominant in the moment Step 3: The therapist describes and explores this object relation – the actors and/or the action - with the patient

The Specific Strategies - II Strategy 2: Observing and interpreting patient role reversals in the transference Strategy 3: Interpreting the defensive function of the split between idealized and persecutory segments of the patient’s mind. This brings together broad elements of the patient’s contradictory affective experiences and leads to integration of the concept of self and others.

ILLUSTRATIVE ROLE PAIRS FOR PATIENT AND THERAPIST Unwanted, deprived child Absent, neglecting parent+ Defective, worthless child Contemptuous parent Threatened, abused victim Sadistic attacker/persecutor Controlled, enraged child Controlling parent Attacking, angry child Controlled, submissive parent -------------------------------+It must be remembered that the role pairs alternate. The therapist and the patient become, in turns, the depositories of part self and object representations. Often the parents are not clearly differentiated as a mother and father, but are merged as a single parent fragment.

Illustrative role pairs…. Cont’d Naughty, sexually excited child Seductive parent Dependent, gratified child Perfect provider Child longing to be loved Withholding parent Controlling, omnipotent self Impotent parent Friendly, submissive self Doting, admiring parent Aggressive, competitive self Punitive, sadistic parent
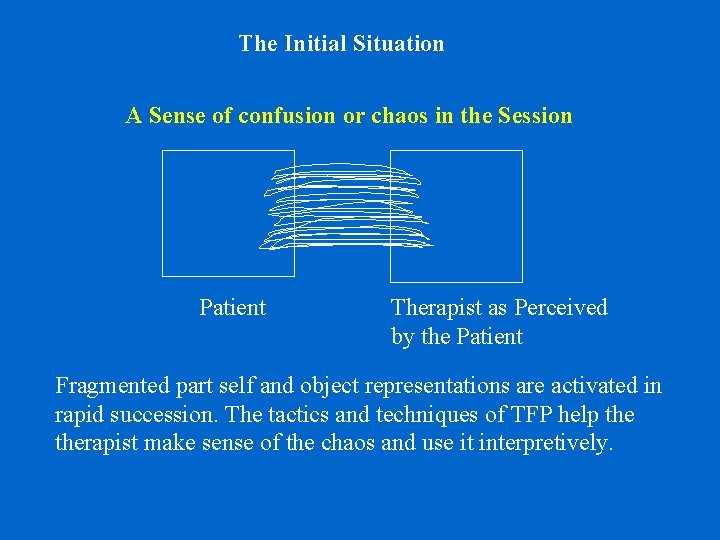
The Initial Situation A Sense of confusion or chaos in the Session Patient Therapist as Perceived by the Patient Fragmented part self and object representations are activated in rapid succession. The tactics and techniques of TFP help therapist make sense of the chaos and use it interpretively.

Clinical Assessment of Personality Organization Evaluate: • Identity • Object Relations • Defenses-Coping and Rigidity • Ethical Functioning • Aggression • Reality Testing

The Structural Interview • Reference: Kernberg: Severe Personality Disorders, 1984 – chapters 1 and 2 • “Structural” interview – to assess psychological structure (vs. a structured interview) • The “Symfora Tapes” • A more structured version: the STIPO

Otto F. Kernberg 1981

The Structural Interview • • begins with 3 questions: 1 - What brings you here? 2 - What is the overall extent of your problems? 3 - How do you understand your problems and what do you expect from treatment? • Also, at some point in the interview, the clinician asks the patient to: – - Describe him or herself. – - Describe a person who is important in his/her life.

To observe in the interview • Three Channels – Non-verbal – Verbal – Countertransference • Neutrality/Concerned Objectivity • Clarification Confrontation Trial Interpretation

The Structural Interview • Maintaining THERAPEUTIC NEUTRALITY (not taking sides in terms of the patient’s conflict) • This Neutrality (vs. overt support) leads to some increase in anxiety and tension in the patient. This may be uncomfortable, but is necessary to see if the patient might be able to have some awareness of and address conflicts within himself (vs. continue to deal with it by projection).

The Structural Interview • Maintaining empathy with the totality of the patient’s internal experience -- not just with the part of the subjective experience that the patient is consciously aware of.

Tactics – assuring the conditions for the analytic work and helping therapist maintain a sense of security

Treatment Tactics - function • Tactics form the bridge between the strategies of the treatment and the momentto-moment therapist interventions • Tactics guide therapist as s/he strives to implement the techniques in the service of meeting its central objectives: – They guide decision-making with regard to where, when, and how to intervene •

The Tactics • Set Contract – Setting the frame of treatment serves multiple functions • Maintain the frame and boundaries of treatment to control acting out • Select the focus of attention and intervention – Attend to what is affectively dominant – Attend to what is in the transference – Attend to the general priorities of treatment • Maintain common perceptions of reality • Analyze both positive and negative transferences • Regulate the intensity of affective involvement
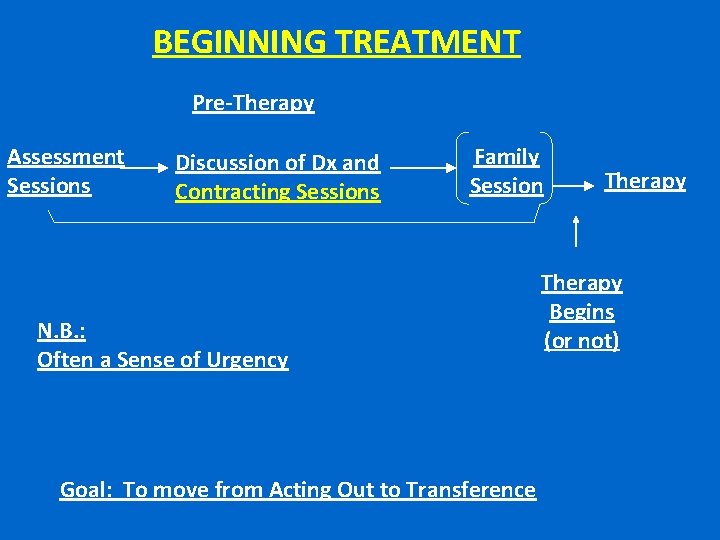
BEGINNING TREATMENT Pre-Therapy Assessment Sessions Discussion of Dx and Contracting Sessions Family Session N. B. : Often a Sense of Urgency Goal: To move from Acting Out to Transference Therapy Begins (or not)

Functions of the Contract - 1 1. Establish mutual understanding of problem and define the REALITY of the relation 2. Define patient and therapist responsibilities Protect the patient, therapist, and therapy Minimize Secondary Gain 3. Protect therapist’s ability to think clearly 4. Providing a safe place for the patient’s dynamics to unfold = contain the patient’s affects

Functions of the Contract - 2 5. Set the stage for interpreting the meaning of deviations from the contract 6. Provide an organizing therapeutic frame that permits therapy to become an anchor in the patient’s life 7. Begin to define patient’s choices = begin to clarify elements of identity

Contract: Standard Content Patient Responsibilities – Attendance – Paying fee – Participation: Reporting thoughts and feelings related to problems without censoring Therapist Responsibilities – Attending to the schedule – Containing the intense affects that arise – Making every effort to understand and, when useful, to comment – Clarifying the limits of therapist’s involvement – (if needed) Predicting Threats to the Treatment, and establishing parameters to address them

Treatment Contracting Process • Therapist presents a part of the contract • Patient responds to those conditions of treatment • Therapist pursues elaboration of patient’s response • Consensus -- or not

Examples of Resistances/Threats to the Treatment • Suicidal and self-destructive behaviors • Homicidal impulses or actions, including threatening therapist • Lying or withholding of information • Substance dependence • Eating disorder • Poor attendance • Excessive phone calls or other intrusions into therapist’s life • Not paying the fee or arranging not to be able to pay • Problems created external to the sessions that interfere with therapy • A chronically passive lifestyle, favoring secondary gain of illness

Contract around Suicidality in a Chronically Suicidal Borderline Pt. feels urge to kill self between sessions Scenario I The patient experiences suicidal ideation and feels he can control his behavior The patient does not call therapist and discusses it in the next session

Scenario II Pt. feels cannot control impulse Patient takes self to ER. I. Pt. is discharged from ER and attends next session OR II. Hospitalization recommended a) Pt. agrees and resumes therapy upon discharge OR a) Pt. refuses, ending therapy Patient calls therapist, who reminds him of contract. I. Patient goes to ER OR II. Pt. refuses. Tpist does what is necessary in the moment, then, when the treatment frame is back in place, discusses with the patient if therapy can continue

Scenario III – Pt. has taken suicidal action Pt. calls family, friend, 911, etc. to get to hospital for eval. Decision to admit or not admit Pt. calls therapist, who does all he can to help save the pt’s life. Then, when calm and neutrality re-instituted, therapist addresses possibility of continuing treatment or not

Offering a Second Chance • Some patients do not believe that others mean what they say – Therapist response: Point out the risk and consequences of this • Breaking the contract may be an attempt to get out of therapy and “blame” therapist for it – Therapist response: interpret the patient’s ambivalence about therapy and reasons for resistance

Once the Contract has been agreed upon… • The patient will often test or challenge an element of the contract to: – see if he or she can control therapist (which is wished for AND feared) – see if therapist “cares enough” maintain the contract • There is typically a decrease in acting out after the first few months of therapy: life settles down while dynamics get focused in therapy • There is an increasing awareness of the importance of therapist for the patient, and defenses against this (attachment themes); increase in affect intensity in sessions

The Other Tactics • Set Contract – To protect the survival of patient, therapist and treatment – To eliminate secondary gain of illness • Maintain the frame and boundaries of treatment to control acting out • Select the focus of attention and intervention – Attend to what is affectively dominant – Attend to what is in the transference – Attend to the general priorities of treatment • Address “incompatible realities” • Analyze both positive and negative transferences • Regulate the intensity of affective involvement

The Tactics after the Contract In every session: maintain the frame and boundaries of treatment - address emergencies, if necessary control acting out, if necessary (set limit, and interpret) transform acting out into an understanding of the object relations enacted in the transference (character analysis)

Tactics after the contract Select the focus of attention and intervention: when, why, and how to intervene • First – follow the affect • Then – follow the hierarchy of priority themes

HIERARCHY OF THEMATIC PRIORITY - I • Obstacles to Transference Exploration – Resistances to explore – suicide or homicide threats – Threats to treatment continuity (inc. financial probs, plans to move, requests to meet less often) – dishonesty or deliberate withholding in sessions (e. g. , lying to therapist, refusing to discuss certain subjects, silences occupying most of the sessions) – contract breaches (e. g. , failure to act on other parts of treatment such as AA, failure to take prescribed meds) – in-session acting out (e. g. , abusing office furnishings, refusing to leave at the end of the session, shouting) – narcissistic resistances – non-lethal between-session acting out – non-affective or trivial themes

HIERARCHY OF THEMATIC PRIORITY – II What, when, and how to interpret • Overt Transference Manifestations – verbal references to therapist – nonverbal references to therapist (e. g. , positioning body in overtly seductive manner) – as inferred by therapist (e. g. , references to other doctors, to figures of authority, etc. ) – the patient’s way of being with therapist • Nontransferential Affect-Laden Material

Techniques • Conducting transference analysis (systematic analysis of distortions in the relationship) • Managing technical neutrality (attitude of concerned objectivity; not drawn into patient’s problems) • Utilizing countertransference awareness • The interpretive process: – Consists of clarifying, confronting, and interpreting – Is a means of enhancing mentalization

The Techniques must be applied with attention to the 3 Channels of Communication 1 – the patient’s verbal communication 2 – the patient’s non-verbal communication 3 – therapist’s countertransference Channels 2 and 3 are often the most important channels in the early phase of therapy with borderline patients

Techniques: Consistent Transference Analysis • On-going analysis of distortions of a “normal” relationship in the treatment setting (“How would a ‘normal’ person react in this situation? ”) • The REALITY of therapeutic relation is defined in the contract • Link distortions explored in therapy to similar distortions in the patient’s relations outside of therapy

Techniques: Technical Neutrality in TFP • What is technical neutrality? • What are the functions of technical neutrality? • When do I deviate from technical neutrality? • How can I reestablish technical neutrality?

Technical Neutrality • A therapist who intervenes from a position of technical neutrality avoids siding with any of the forces involved in the patient’s conflicts • Neutrality means maintaining the position of an observer in relation to the patient and his difficulties • When working from a position of technical neutrality therapist is aligned with the patient’s “observing ego”
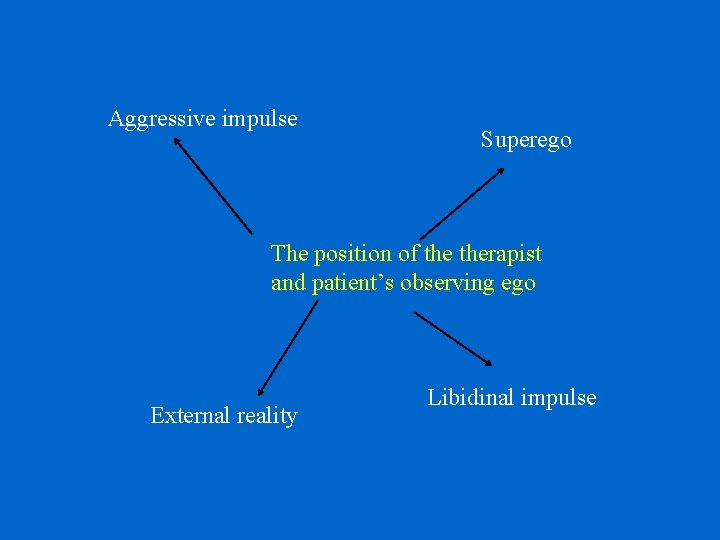
Aggressive impulse Superego The position of therapist and patient’s observing ego External reality Libidinal impulse

Technical Neutrality • Technical neutrality refers to the manner in which therapist frames his interventions • The therapist is not neutral in his attitude towards the patient—neutrality does not imply indifference • The therapist is not neutral in his internal reactions to the patient—neutrality does not imply emotional distance

Technical Neutrality A neutral intervention does not “take sides” among the various forces involved in patient’s conflicts: • The part of patient pushing the patient to act on a conflictual motivation or impulse • The part of patient that wants to inhibit expression of the conflictual motivation • The reality demands placed on the patient

Why Neutrality? • Encourages redirection of patient’s conflicts into therapy • Allows therapist to diagnose internal object relations dominant at any given moment • Strengthens patient’s observing ego • Interpretations presented from a position of neutrality facilitate integration of split off internal object representations

Technical Neutrality Clinical Example • Support observing ego • Point out the division within the patient • Describe the two sides of the division without siding with one or the other

Deviations From Technical Neutrality • Deviations from neutrality can be an appropriate part of the treatment strategy of TFP

Deviations from Technical Neutrality: Indications • • Threat to safety of patient Threat to safety of others Threat to continuation of the treatment Confrontation and interpretation fail to contain acting out

Deviating from Neutrality • Attempt to control acting out from a position of technical neutrality using clarification, confrontation and interpretation • Introduce a parameter to limit acting out • Point out that therapist is stepping out of role and explain why s/he has chosen to do so • Return to transference, making link between deviation from neutrality and self and object representations externalized and enacted in the transference

Reinstating Neutrality • Acknowledge the deviation and explain why • Explore the meanings patient attributes to therapist’s actions (Therapist as protector to child/patient) • Confront and interpret conflict that has been externalized (Responsible mother vs. negligent mother) • Link to underlying transferences (Negligent therapist-mother)

Technical Neutrality – link with Countertransference • Unnecessary deviations from neutrality result from countertransference that therapist is not aware of and acts out.

Techniques: Countertransference in TFP When evaluating countertransference, consider therapist’s total emotional reaction to the patient

Defining Countertransference Therapist’s transference to patient Classical view is “therapist-focused” Therapist’s reactions to patient’s transference Kleinian view is “patient-focused” Therapist’s total emotional reaction to patient “Countertransference in the broad sense”

Sources of the Countertransference • The patient’s transference to therapist • The patient’s external life • The therapist’s transference to the patient • The therapist’s external life

Countertransference in TFP • Countertransference to borderline patients says more about patient than it says about therapist • Borderline patients defensively project aspects o their inner worlds into therapist • Primitive defenses involve affecting therapist

Countertransference: Two Types Concordant Identification Therapist identifies with patient’s self experience Complementary Identification Therapist identifies with patient’s internal and external objects

Concordant Identifications in the Countertransference • Are the basis of ordinary empathy • “Putting ourselves in the patient’s shoes”

Complementary Identifications in the Countertransference • Predominate in the treatment of patients with borderline personality disorder • Reflect the impact of projective identification on the clinical process • If unrecognized by therapist, can interfere with therapist’s capacity to empathize with patient’s immediate emotional situation

Countertransference to Borderline Patients • • • Rapidly developing Intense Unstable Confusing Pressure to “Do something”

Countertransference • Countertransference is “Third channel of communication” serving as essential source of information about patient’s inner world and object relations activated in the transference • Countertransference can disrupt therapist’s ability to understand patient’s inner world and to effectively communicate with patient

The Third Channel of Communication • Borderline patients express in action what they cannot express in words • Dominant affective themes and object relations are expressed through inducing thoughts and feelings in therapist • To clarify how patient is experiencing therapist in the transference ask, “How am I being made to feel? ”

Containing Countertransference • • Careful assessment Clear treatment contract and frame Explicit theory of technique Consultation or peer supervision

Metabolizing Countertransference The therapist “metabolizes” the patient’s projections in the countertransference • Allows patient to affect him internally • Tolerates his emotional experience without turning to action • Reflects upon what the patient has stimulated in him and what this might say about the object relation enacted in the transference

ACUTE and CHRONIC COUNTERTRANSFERENCE Acute countertransference reactions • Affect therapist moment-to-moment • Rapidly shifting with borderline patients • Mirrors shifting developments in the transference • Affective intensity • Can be difficult to contain Chronic countertransference reactions • Affect therapist over periods of time • Stable attitude on the part of therapist • May be subtle / typically not highly affectively charged • Can be difficult to notice / often with the aid of a consultant • Reflects therapist’s characteristic response to transference

The Interplay of Countertransference and Technical Neutrality • Countertransference is most common cause of unnecessary deviations from neutrality • It is only from a position of neutrality that therapist can reflect upon and metabolize countertransferences to deepen her understanding of patient

Transference Interpretation Process • Conceptualized as a series of interventions that build on one another • May take many sessions to complete a single cycle of interpretation or may have many completed cycles in one session

The Interpretive Process starts with Clarification • This technique is requesting clarification, not offering clarification • Provides material for interpretation by clarifying – The patient’s perception of self in the moment – The patient’s perception of the other/the therapist • This technique sheds light on the patient’s internal world and helps to elaborate distortions (i. e. , enhances mentalization)

Confrontation • This technique is not a hostile challenge, but rather an honest inquiry into an apparent contradiction in the patient’s verbal and non -verbal communication • It is an invitation for the patient to reflect on different aspects of the self that are split off from one another

Confrontation – cont’d • The contradiction can be within one channel of communication: “You said earlier that I was a terrific therapist, now you’re saying I’m worthless…. ” • Or the contradiction can be between different channels of communication: “You’re saying you’re furious, but you’re looking at me with a smile…. ”

Interpretation per se • A hypothesis about unconscious determinants of present experience • Interpretations address and attempt to resolve psychological conflicts • Interpretations attempt to increase awareness of the impact of unconscious material on the patient’s thoughts, affects, and behaviors

Goal of the Interpretative Process • To interrupt cycle of dysregulation and pathological defense • To Integrate dissociated aspects of experience • To replace splitting based defenses with repression • To resolve identity diffusion. – Identity consolidation in turn leads to improved capacity for affect regulation and symbolic management of psychological conflict • To enhance the capacity to self reflect and contextualize experience

BPD Patient’s Experience of the Transference - 1 • Primitive object relations are activated in the transference – but experienced as strong AFFECTS • Patient’s experience of therapist is concrete (e. g. patient has limited capacity to appreciate the distinction between internal and external reality) • Patient’s experience of transference shows a predominance of primitive affect (hatred or idealization) without cognitive representation of object relation activated

BPD Patient’s Experience of the Transference - 2 • Intense affect floods clinical setting • Patient is unable to to establish any distance from or perspective on his immediate experience in the transference • Both therapist and patient experience a sense of confusion and anxiety • Transference dispositions may be most clearly expressed in patient’s behavior or in the countertransference

BPD Patients’ Experience of the Transference - 3 • Patient is not able to make use of traditional interpretations of underlying anxieties and defenses organizing his or her experience initially • May experience any sort of intervention as a criticism or an assault • Patient may be able to use more basic interventions to contain/hold affective experience and to promote the capacity to cognitively represent it • Leads gradually to capacity to symbolically manage and reflect on experience in the transference

The Focus of Interpretation with Borderline Patients Because of the predominance of splitting-based defensive operations (rather then repression-based defenses) in BPD patients: • Interpretation focuses on mutually dissociated aspects of experience that are accessible to consciousness, though at different times (rather than consistently repressed) • As treatment progresses, dissociative defenses give way to repressive defenses, when interpretations can shift to focus on repressed mental contents

Interpretation with Borderline Patients: Principles Interpretation first spells out the nature of the dominant object relation and the patient’s difficulty identifying with both poles of that dyad Interpretation then addresses the defensive split between persecutory dyads and idealized dyads. The dyad “on the surface” can change rapidly from one moment to another.

Steps of Interpretation - slide I 1 - a Understand/Identify self state in the moment (first level of mentalization) - b Elaborate understanding of therapist 2 – a Consider other’s/therapist’s possible experience of the moment, and that it may be different from the patient’s – b If necessary, offer the patient a version of how therapist experiences the moment

Steps of Interpretation - slide II 3 - Put the moment in a broader context: Contrast the immediate experience of self and of therapist with that seen at other times. (second level of mentalization) 4 - Address layering/splits/conflicts by – Clarifying the oscillation between identifying with the self representation and then the object representation – Interpreting the motivation of the split between dyads with opposite affective valences

Therapist-Centered Interpretations • Therapist-centered interpretations (Steiner, 1993) put patient’s concrete and affectively charged experience of therapist into words – Without suggesting alternative point of view – Without suggesting patient has anything to do with the experience • Provides cognitive containment of concretely experienced affect states • Provides patient with experience of being understood and therapist of genuinely attempting to understand

Summary of the Interpretation Cycle • Begins with efforts to help patient clarify his conscious emotional experience in the transference, elaborating the particular representations of self and object respectively enacted and projected onto the analyst • Next, confronts the patient with his experience of this same object relation enacted in the transference at other times but with roles reversed • Subsequently, interpretively links idealized and persecutory relations with the analyst that have been conscious, but defensively split off by mutual denial

Characteristics of Interpretations • Depth of interpretation – Surface to depth = defense before impulse, with maximum depth in crises • Timing and tempo of interpretations – related to the patient’s rapid shifts; we must try to follow each shift • Early interpretations focus on the “here and now” • Later interpretations link the “here and now” to the past • Accuracy of interpretation: judged by whether new material or awareness emerges
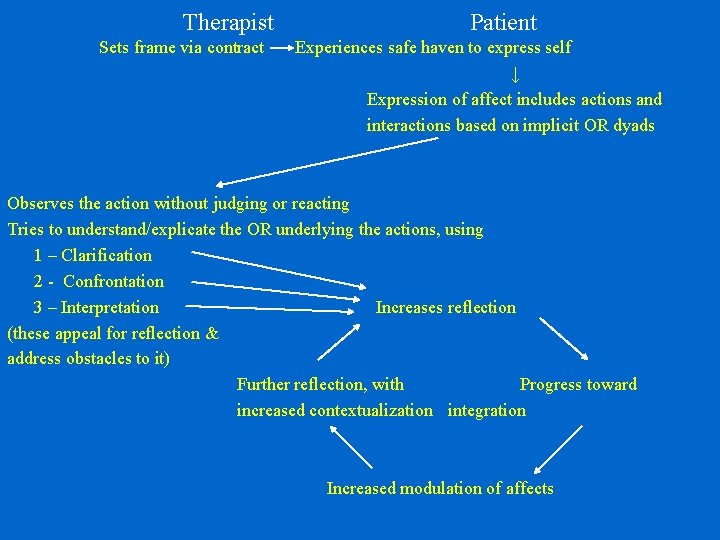
Therapist Sets frame via contract Patient Experiences safe haven to express self ↓ Expression of affect includes actions and interactions based on implicit OR dyads Observes the action without judging or reacting Tries to understand/explicate the OR underlying the actions, using 1 – Clarification 2 - Confrontation 3 – Interpretation Increases reflection (these appeal for reflection & address obstacles to it) Further reflection, with Progress toward increased contextualization integration Increased modulation of affects

Treatment Complications • Acting out--general principle: first interpret, then set limits -------------------------- • Suicide and self-destructive behavior • Eating disorders, substance abuse, antisocial behavior/psychopathic transference – all need containment, “extra” frame -------------------------- • The threat of drop-out • Affect storms – overt and silent • Paranoid regression/micro-psychotic episodes • Dissociative reactions – a form of splitting • Erotic Transference • Eroticized Transference • Hospitalizations

Typical evolution of therapy I • The patient tests/challenges the contract • Early emphasis on nonverbal and countertransference channels of communication • Decrease in acting out: life settles down while dynamics get focused in therapy • Increasing awareness of the importance of therapist for the patient, and defenses against this (attachment themes); increase in affect intensity in sessions • Alternation between persecutory and idealized transference – the ideal may be erotic

Typical evolution of therapy II As therapy advances to the midphase: • Interpretation of defenses against integration • A cycle (“looping”) where the problematic dynamics reappear, but in a more contained and limited way • There is evidence of integration, initially tentative and subject to frequent regressions to splitting • Practical problems arise stemming from earlier life choices that no longer “fit” well

Termination • Every separation (end of session, vacation, etc. ) can bring up the dynamics of termination – For borderline patients, separation is always an issue – Narcissistic patients may have difficulty getting involved before separation becomes an issue • The dynamics of separation and termination should be addressed throughout therapy • Successful termination involves successful internalization and integration • Termination involves the dynamics of healthy vs. pathological mourning

Example of Patient Comments in Termination Phase - 1 P: I heard from the job. I got it. I decided to take everything that way, like friends. I realize I have to be active. But I still feel a little lost. T: You're building an adult identity. P: And trying to change the way I think. I realize that people might react to me in a certain way because of something going on in their life. T: So it's not all about you? P: Right, it's ironic, it's like the opposite of narcissism.

Example of Patient Comments - 2 T: I could have imagined you having an angry reaction to the job. P: Me too T: Then that would have destroyed the opportunity and you would've felt hopeless.

Example of Patient Comments - 3 P: The hardest thing now is figuring out what to do with my boyfriend. T: It usually is. P: I met him when I was in a bad place in my life. I just wanted someone. Maybe I should date other people but it's like I don't know myself. I have to figure out what I want.

Example of Patient Comments - 4 P: For the first time I felt I didn't desperately need my boyfriend and could be independent. T: That might help you decide if you want the relationship. P: How do you know you love someone? T: There's a lot to think about but ultimately only you can decide. P: I always wanted the answer to be clear and certain. T: There might be a mix of things you have to consider; we can think about them here.

Example of Patient Comments - 5 P: I went to my high school reunion – a friend made me do it. I thought it would be a disaster, but I reconnected. I'm putting out positive energy – and getting it back. T: That's different from the negative energy. P: Yes, my boss gave me some suggestions. Before I would've thought it was all criticism. Now I realize they were interesting ideas. I still have a negative reaction but now I think about it.

Example of Patient Comments - 6 P: In the past, if anyone said anything, it would set off this swirl of low self esteem. Now… I'm not saying I'm the top – but I'm not an idiot – I’m okay – it sounds so cheesy!. . . Believing people can like me.

Example of Patient Comments - 7 P: It wasn’t just self-esteem, it was how I imagined others toward me…. To think all these years I’ve been imagining what’s in peoples heads – and I’m smart! I thought I was right. At the beginning of therapy I’d want to leave because I thought you was taking me away from the truth. I thought everything negative - all the attacks I saw on me - were right… … Now this better be real! – because I guess there is no absolute truth. ”

In-Session Indications of Integration and Structural Change • The patient’s comments indicate reflection on and exploration of therapist’s interventions • The patient is able to accept the exploration and interpretation of primitive defense mechanisms • The patient can contain and tolerate the awareness of previously projected affects • The patient can experience guilt/remorse and enter into the depressive position • The patient can tolerate fantasies and the development of a transitional space

Clinical Manifestations of Structural Change at the level of psychological structures with a more integrated psychological experience will lead to: • Better functioning, with a reduction of symptoms and maladaptive behaviors • Change in the patient’s sense of self and experience of the world • Ability to cope with stress and adversity • Living a “full” life with a realistic measure of satisfaction in love and work

Brief Summary of Structural Features of Narcissistic Personality Disorder (NPD) Slides by Eve Caligor, M. D.

NPD Structural Organization: the Pathological Grandiose Self -1 § NPD has a facsimile of identity integration § This “Grandiose self” distinguishes NPD from other Personality Disorders § It is a compensatory self structure overlaying a split self § It provides some stability of self functioning – but at a cost

NPD Structural Organization: the Pathological Grandiose Self - 2 § In contrast to normal identity, the grandiose self is a defensive structure § It is superficial and distorted, rigid and brittle § It requires constant external support and is vulnerable to abrupt discontinuity in response to environmental stressors § Yet, because of grandiose self, NPD can have more stable sense of self and more stable functioning than other PDs of comparable severity. This has treatment implications.

The Grandiose Self, Reality and Interpersonal Functioning • The need to maintain the illusion that the self has subsumed all that is ideal, and contains no negative elements, leads to a defensive withdrawal from genuine relationships and, to varying degrees, from reality • Contact with the real world threatens the person’s psychological equilibrium (defensive structure) • FOR THE NARCISSIST, REALITY IS AN AGGRESSION

The Grandiose Self, Reality and Interpersonal Functioning - 2 • It is not just self-esteem but the entire sense of self that is at stake The grandiose self defends against anxieties regarding dependency – against having genuine needs and having to rely on others It defends against § fears of humiliation, inferiority, exploitation, § shame and guilt in relation to aggression • Relationships with others are used to support the grandiose self

The Grandiose Self as a Defensive Structure – the Price to Pay § The grandiose self provides these protections but at the cost of sacrificing genuine connections with others and to some degree with reality

Two Subtypes of Narcissism Grandiose/”Thick-skinned” vs Vulnerable/”Thin-skinned”

Implications of the Grandiose Self for Treatment Therapy should: 1. dismantle the grandiose self - help the patient relinquish his defensive retreat from reality and from relatedness 2. Uncover the underlying split structure and fragmentation 3. Promote normal identity integration by exploring anxieties motivating splitting-based defenses Challenges in Therapy: 1. Dismantling the grandiose self poses a great challenge 2. There is a life or death quality for patient – his “self” is at stake A technique that can help is the “therapist-centered interpretation”
- Slides: 173