Transfer Guidelines for Malignant Hyperthermia Marilyn Green Larach
































- Slides: 35

Transfer Guidelines for Malignant Hyperthermia Marilyn Green Larach M. D. Senior Research Associate The North American Malignant Hyperthermia Registry of MHAUS

Disclosure Statement l Dr. Larach received an MHAUS honorarium – To support guideline development l Both MHAUS and the ASF sell transfer of care posters – No financial benefit to Dr. Larach

Goals of Talk l Introduce Transfer of Care Guidelines l Discuss Need for Guidelines l Provide Overview of Content l Review MH Presentation & Treatment

Assumes an ASC using MH Triggers has Available: l Anesthesia Care Provider l 36 Vials of Dantrolene l MHAUS Emergency Therapy Poster l MH Crisis Drills



Development of Guidelines for Emergent MH Transfers l Joint Consensus Document – – l ASF MHAUS 13 Panel Members – – – Anesthesiologists CRNA Emergency Medicine Physician Emergency Medical Technician ASC nurse/administrator ASF nurse/administrator

Guideline Goals l Assist ASC to prepare own individual emergent MH transfer plan predicated on the facilities and capabilities of the: ASC – Emergency transport services – Receiving hospital –

Guidelines and Not Protocol l ASC Locations Vary Staff Resources – Lab Resources – Distance to Receiving Hospital –

Guidelines and Not Protocol l Emergency Transport Services Vary Availability – Weather – Distance to Receiving Hospital – Severity of Patient Condition –

Guidelines and Not Protocol l Receiving Hospitals Vary – Facilities – Personnel


Recognition of Suspected MH l First – – – signs Hypercarbia Sinus tachycardia Masseter spasm l Temperature abnormalities may be early MH sign l Most common pattern – Respiratory acidosis and muscular abnormalities


Begin Treatment l l Declare MH Emergency Discontinue Triggering Agents 100% Oxygen at High Flow Give Dantrolene – – l 2. 5 mg/kg IV push Titrate to effect Initiate Transfer Plan – Whenever possible, don’t move unless clinician judges patient to be stable

Key Patient Stability Indicators l ETCO 2 is declining or normal l HR is stable or decreasing l No ominous dysrhythmias l Temperature is declining l Generalized muscular rigidity is resolving (if present) l IV dantrolene administration has begun

MH Morbidity and Mortality l l l l l Consciousness Level Change/Coma Cardiac Dysfunction Pulmonary Edema Renal Dysfunction Disseminated Intravascular Coagulation Hepatic Dysfunction Other Relapse Death

Factors Increasing MH Complication Likelihood l Increased time 1 st sign to 1 st dantrolene – l For every 30 minute increase in the interval between 1 st MH sign and 1 st dantrolene dose, the complication likelihood increased 1. 6 times. Increased maximal temperature – For every 2 C increase in maximal temperature, the complication likelihood increased 2. 9 times.

Transport Team Type varies with scenario & transport time l Capabilities l – – – l Ventilatory support Cardiopulmonary & temperature monitoring Fluid resuscitation Medication administration Life support Phone communication May require ASC anesthesia staff

Receiving Health Care Facility Existing transfer agreement l Inpatient capabilities l – – – – Adult/Pediatric Critical Care Continuous temperature and cardiopulmonary monitoring Non-invasive/invasive cooling Continuous sedation Dantrolene Dysrhythmia treatment Hemodialysis

Receiving Health Care Facility Consultant Availabilities l Anesthesiology l Critical Care l Hematology l Surgery l Nephrology l Medical Toxicology

Report Data from ASC l Cardiovascular signs l Temperature and site l Minute ventilation with ETCO 2 l Dantrolene amount given & response l Muscular rigidity status l Electrolytes l I. V. site l Urinary catheter & urine color

Communication Coordination l Direct communication concerning patient status & admission location between Anesthesia care provider at ASC AND – Physicians accepting care at Receiving Hospital –

Transfer Decisions by On-Site ASC Health Care Professional Timing of Transfer l Factor In: – Transport time l Choice of Transfer – Bed availability Team – Clinical stability l Choice of Receiving Hospital l

Implementation of Transfer Decision l Don’t delay transfer pending specific personnel or equipment availability if emergent transfer is mandatory l **Accompany patient with appropriate medications and equipment if needed to serve the best interests of the patient **Personal Recommendation



Create Your Own ASC MH Transfer Plan Start with Guidelines l Research available transport teams l Consult with physicians at referral hospitals l


Clinical Characteristics l 24. 1% – Emergency Sux 3. 8 times more often l Orthopedic, – ENT, General Surgery Sux 1. 9 times more often l Temperature Monitoring (n=259) 14% skin liquid crystal sole probe – In 10 patients, skin liquid crystal didn’t trend with core temp probe –

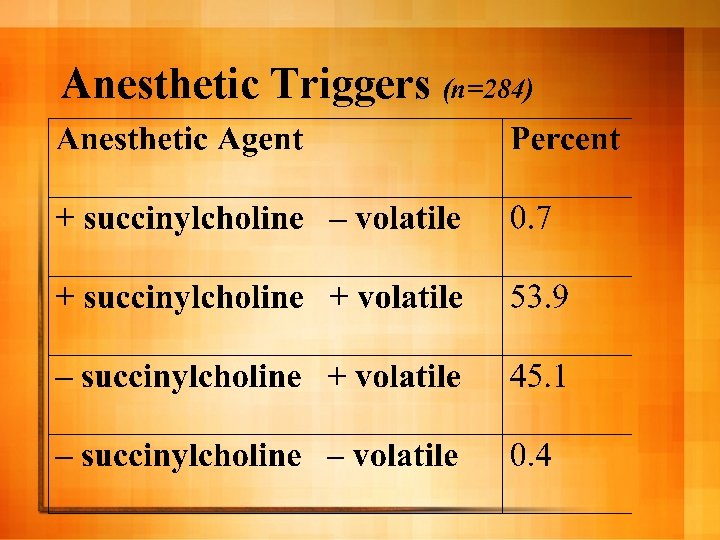
Anesthetic Triggers (n=284)

Presentation l 99% Respiratory Acidosis l 26% Metabolic Acidosis l 80% Muscular Abnormalities

Clinical Presentation Pattern (n=196) Presentation Pattern % +Respiratory +Metabolic +Muscular 20. 4 +Respiratory +Metabolic –Muscular 5. 1 +Respiratory –Metabolic +Muscular 58. 2 –Respiratory +Metabolic +Muscular 0. 5 +Respiratory –Metabolic –Muscular 15. 3 –Respiratory –Metabolic +Muscular 0. 5

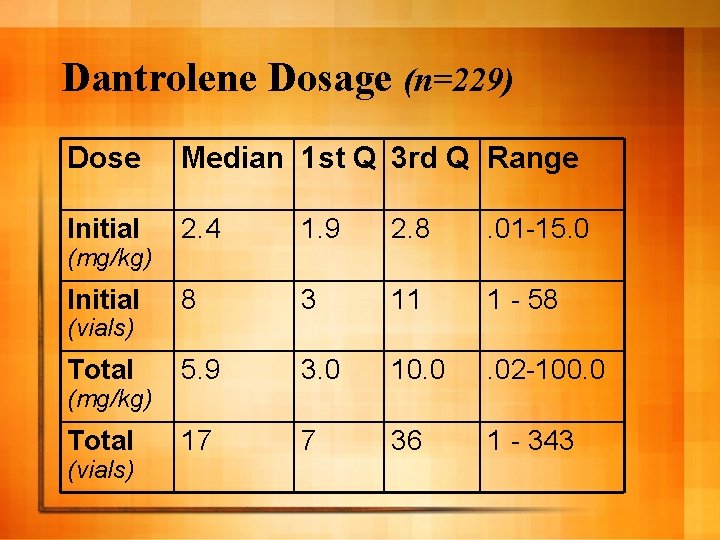
Dantrolene Dosage (n=229) Dose Median 1 st Q 3 rd Q Range Initial 2. 4 1. 9 2. 8 . 01 -15. 0 Initial 8 3 11 1 - 58 Total 5. 9 3. 0 10. 0 . 02 -100. 0 Total 17 7 36 1 - 343 (mg/kg) (vials)

Adjunctive Treatment (n=284) Treatment % Hyperventilation with Fi. O 2=1 IV fluid loading Active cooling Bicarbonate Anesthesia circuit change Mannitol Furosemide Glucose and insulin 87 77 70 54 48 34 32 14