Training rural providers in cognitive behavioral therapy CBT

Training rural providers in cognitive behavioral therapy (CBT) via tele-psychiatry Katharina Manassis, MD, FRCPC, Child & Adolescent Psychiatrist Professor Emerita, University of Toronto

Faculty/Presenter Disclosure Faculty: Katharina Manassis, MD, FRCPC Relationships with commercial interests: Grants/Research Support: The research discussed was partially funded by Bell Canada Speakers Bureau/Honoraria: Unrestricted talks for Janssen and Shire Consulting Fees: None Other: Book royalties from Routledge, Guilford, and Barron’s Educational Mitigating Bias: I will not mention specific books or pharmaceuticals in this talk. I will not endorse any particular communications company.

Objectives The participant will recognize the need for increasing access to evidence-based psychotherapy outside urban centres; The participant will appreciate the opportunities and challenges of providing psychotherapy training via tele-psychiatry; The participant will learn about gaps in our understanding of how to best translate CBT to make it relevant to rural settings. In brief: Do we increase access or lose in translation?

Acknowledgments Dr. Paul Arnold Dr. Sandra Mendlowitz Dr. Kathryn Bennett Dr. Christopher J. Mushquash Ms. Tina Bobinski Dr. Behdin Nowrouzi Dr. Angela Fountain Dr. Fred Schmidt Dr. Abel Ickowicz Dr. Emily Jones Dr. Pamela Wilansky

Need for evidence-based treatment 1 in 5 children and youth could benefit from mental health treatment, but few have access outside major urban centres The most consistent evidence for non-medical treatments is for cognitive behavioral therapy (CBT), adding it to medication augments benefits (e. g. , CAMS trial, POTS trial), and relapse risk is lower when CBT is added CBT is easiest and quickest to access in or near urban centres, and via psychologists for those who can afford them Result: the poor and the rural are medicated; the rich city folks get CBT Given the benefits of CBT and higher risk of adverse events with medication, this clearly places children and youth in remote areas at a disadvantage

Technology and opportunity Given the highly structured, manualized nature of CBT it is one of the easiest psychotherapies for training Training is more effective when it involves case supervision Case supervision can be done effectively in a group format There is some evidence for doing such training via video link When multiple trainees work at the same agency, the chances of long term uptake are enhanced Trainees know their organization, community, and clientele: they have a good understanding aspects of CBT might need adaptation locally Evaluation is needed to show that such training is a good investment

What can go wrong with CBT? Failure to formulate: external factors interfering (bullies, severe family conflict, cultural biases, poverty & other priorities, etc. ) Failure to formulate: internal factors interfering (e. g. , undiagnosed learning disability/untreated ADHD/medical condition) NB: CBT requires verbal working memory Unrealistic treatment expectations (characterological goals; roles of child/parent/therapist unclear; rate of progress not spelled out) Lack of treatment fidelity (no homework, too little repetition, infrequent sessions, unstructured sessions, lack of consistent positive reinforcement) Failure to generalize to real life (needs time, routines, concrete reminders, parental support)

E. g. , How flexible should you be when using manuals? Don’t add concepts to the manual (interferes with repetition), read once before starting Ensure child masters all major concepts (even if you fall behind a session or two) Writing/reading help is fine Reinforce the most minimal participation, as engagement is key for success Support concrete reminders, even if not in the book Consider breaking into modules for complex cases Start with an ‘easy’ case and share your challenges as well as your successes in supervision

People to consider in knowledge translation… Client Trainee Trainer Mental Health Organization Community Culture

Coping Communities Pilot Project (child mental health providers, face to face) CBT workshops were well-received but not enough to instill confidence Community practitioners with limited training were being told to “do CBT” in non-ideal conditions/clients, with no help adapting it Great training need & few trainers *Group supervision model with some didactic teaching, one structured manual but with help adapting to diverse populations/ settings
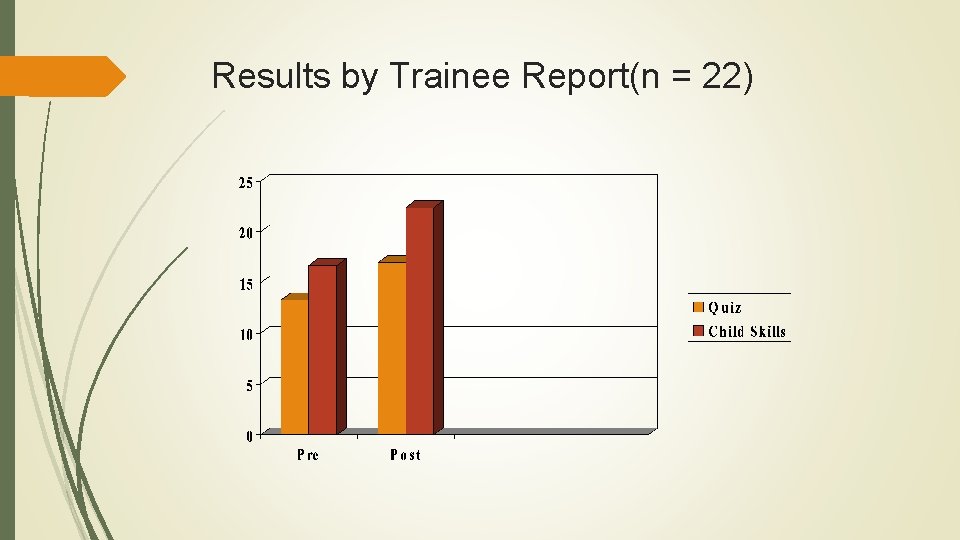
Results by Trainee Report(n = 22)

CBT Tele-psychiatry KT project 20 -week group supervision training, with trainers (3) at HSC telepsychiatry 10 different Northern Ontario children’s mental health agencies; one agency was First Nations 4 to 9 clinicians per group, familiar with child therapy but not CBT Trainee n=78, 51% social workers, 49% other mental health disciplines Each clinician was required to treat one child/youth with anxiety-focused child CBT Children had high rates of non-anxious comorbidity, need for psychotropic medication, family psychiatric history, and learning disabilities suggesting a more complex population than typically seen in academic settings
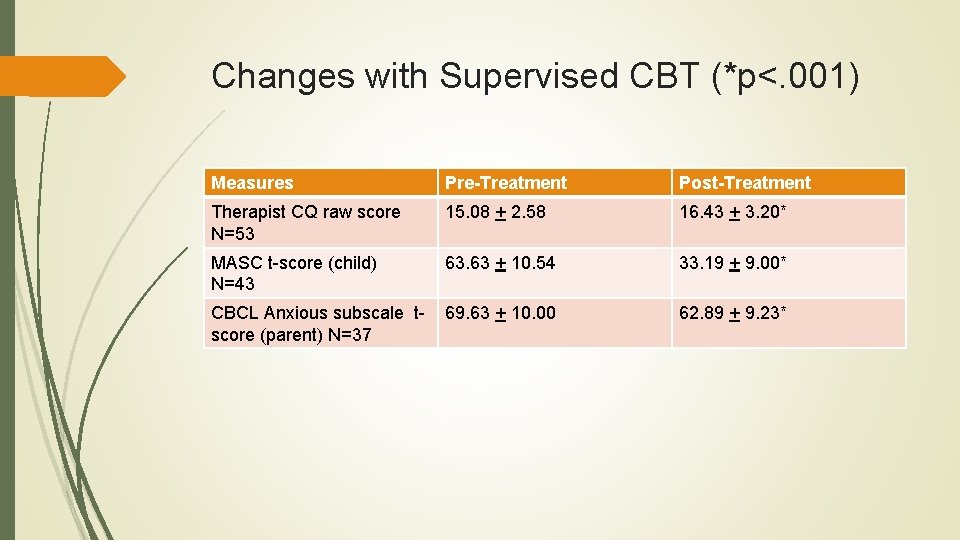
Changes with Supervised CBT (*p<. 001) Measures Pre-Treatment Post-Treatment Therapist CQ raw score N=53 15. 08 + 2. 58 16. 43 + 3. 20* MASC t-score (child) N=43 63. 63 + 10. 54 33. 19 + 9. 00* CBCL Anxious subscale tscore (parent) N=37 69. 63 + 10. 00 62. 89 + 9. 23*

More Observations… Technology did not seem to hinder training, despite some ‘glitches’ and occasional difficulty engaging all participants consistently Trainees managed the dual challenge of learning CBT and adapting it to local clientele (complex cases, family problems, cultural adaptations) and conditions (e. g. , covering emergencies, needing organizational champions for appropriate case selection and time for training/evaluation) No site-specific differences, nor demographic or severity differences between completers and non-completers, but measure completion rates could have been better (note: some completed the program but not the measures)
Qualitative Analysis Themes Client issues Patient and practitioner benefits Organizational issues Northern/Rural/Remote Challanges

Excerpt from Qualitative Paper “Although it is a relatively new modality for addressing emotional difficulties in First Nations youth, some elements of CBT are highly consistent with First Nations perspectives. For example, encouragement to relate the mental, physical, and emotional aspects of health is common to both, though spiritual aspects are typically emphasized as well in the First Nations perspective. First Nations healing practices are rooted in spirituality and connection to the land. Other elements of CBT contrast with First Nations perspectives. For example, CBT is very structured and typically uses written exercises to help children learn coping strategies. First Nations traditions, however, generally place more emphasis on narrative and relational aspects of mental health care, and on healing that comes from within the community. Moreover, children in First Nations communities may face social disadvantages that impact their treatment (e. g. , high rates of poverty and of foster care placement). Some families or communities may also harbor mistrust of mental health providers based on historical injustices. All of these factors underscore the need to work in partnership with First Nations mental health providers when adapting and evaluating CBT for children in First Nations communities. ”

Qualitative Highlights (First Nations) No difference in training-related therapist or child improvements between First Nations and other agencies Client issues: emphasis on coping was empowering for some; time was needed to build trust in therapeutic relationships Therapists were also First Nations, so able to see links between CBT and traditional healing (e. g. , Medicine Wheel) and provide culturally sensitive adaptations (e. g. , walking and talking vs. writing, mascot adapted to fit folklore); therapists appreciated ‘many heads are better than one’ Structured format of CBT and the need for weekly appointments was sometimes challenging to maintain, given high case complexity, dispersed population, and family/community challenges

Further study needed… Studies with non-CBT comparison groups Observational measures of treatment fidelity Consistent return of outcome measures (to avoid sampling bias) Assessment of the specific adaptations that were most effective Assessment of the role of family and community factors in relation to outcome Long term follow-up of clients Assessment of factors predicting ongoing adoption of CBT by involved mental health agencies. Applications to other disorders, other evidence-based therapies

Durability Ongoing trainer/trainee relationship—face to face meeting ahead of time; CBT ‘refreshers’ or adherence checks afterwards; option for contact when ‘stuck’ with a case; Organizational champions in respected positions At least 2 people trained per site to allow ongoing peer support Needs to be seen as a component of treatment plan, not a panacea Philosophies of care: specialized care versus one size fits all; the latter favors the ‘squeaky wheels’ (i. e. , externalizers) and the dissolution of specialty programs for internalizing disorders

Thank you for your attention! Questions?
- Slides: 20