Toxicology Grand Rounds Carbon Monoxide Poisoning Mark Yarema

Toxicology Grand Rounds: Carbon Monoxide Poisoning Mark Yarema, MD FRCPC Poison and Drug Information Service Calgary, Alberta PADIS/Emergency Medicine/Critical Care Rounds January 27, 2011

Acknowledgements n n n n PADIS: Rosalee Sears-Ford, Nina Walny Critical Care: Paul Boiteau, Sid Viner Emergency Medicine: Ian Rigby, Jay Green, Kevin Hanrahan Miscericordia Hospital: Malcolm Young HBOT Clinics: Terry Stewart, Karen Keats, Caroline Bain AHS Telehealth PLP: Marianna Hofmeister, Holly Donaldson, Kyle Dormer Podcast website: http: //www. ucalgary. ca/plppodcasts/

Disclosure n I have no commercial interest in any of the products or therapies discussed in this presentation.

Outline n n n n Cases Intro to CO Pathophysiology Clinical features Diagnosis Management Special presentations: q Misericordia Hospital HBO Unit q HBOT Clinics Inc. Q and A

Case 1 n n n 63 y. o. male Last seen July 1 Found by wife July 2 AM in garage with riding tractor running EMS called, pt. in cardiorespiratory arrest Intubated, ventilated, CPR Return of spontaneous circulation 15 minutes after resuscitation initiated

Case 1 n In E. D. : q q n ABG: p. H < 6. 8 PC 02 58, p 02 31, HC 03 15, Lactate > 20, COHb 61% ST depression on EKG Another cardiac arrest resuscitated Multiple pressors PADIS consulted: candidate for HBO?

Case 1 n n n d/w PADIS: meets accepted criteria for HBO. Recommended speaking with Misericordia HBO MD on call Transferred to Misericordia 1 HBO treatment given July 2 Transferred to ICU July 3 Died 19: 29 hours July 3

Case 1. 5 n n n 4 days after death of Case 1 21 y. o. male Texted girlfriend at 0400, found asystolic in car by EMS at 0500 ROSC after 30 minutes CPR by EMS In E. D. : q q intubated, unresponsive ABG p. H 6. 82, COHb 57. 3%, Lactate 22

Case 1. 5 n n n d/w PADIS: meets accepted criteria for HBO. Recommended speaking with Misericordia HBO MD on call Pt. deemed not appropriate candidate Died 1700 hrs July 7 th

Case 2 n n 62 y. o. female, 16 y. o. male, 35 y. o. male Hx of ‘faulty furnace’ in home Furnace turned on during last period of Canucks game, then everyone fell asleep 4. 5 hour ‘soaking period’

Case 2 n n n 1: 00 am: 16 y. o. gets up to go to fridge, falls 62 y. o. hears the fall and wakes up EMS called q q n 16 y. o. and 35 y. o. : headache, nausea, no other symptoms 62 y. o. : disoriented, combative, vomiting, headache Does anyone need HBO?

Case 2 n n n d/w PADIS: 62 y. o. most concerning, meets accepted criteria for HBO. Recommended speaking with HBOT Clinics MD on call MD speaks with HBOT clinics HBO MD on call Patient accepted by HBOT, treated with HBO

Intro to CO n n Colorless, odorless, tasteless gas Formed by incomplete combustion of carboncontaining compounds Normal byproduct of hemoglobin degradation Many different sources of exposure

Sources of CO n n n n n Fires Auto exhaust Cigarette smoke Malfunctioning water heaters, gas stoves, furnaces Wood-burning fireplaces, blocked chimneys Propane forklifts Ice resurfacing machines Generators Inappropriate heat sources (e. g. barbecues)

www. coolestspringbreak. com Source: The Arizona Republic, November 29, 2000 (Maureen West and Judd Slivka, reporters)
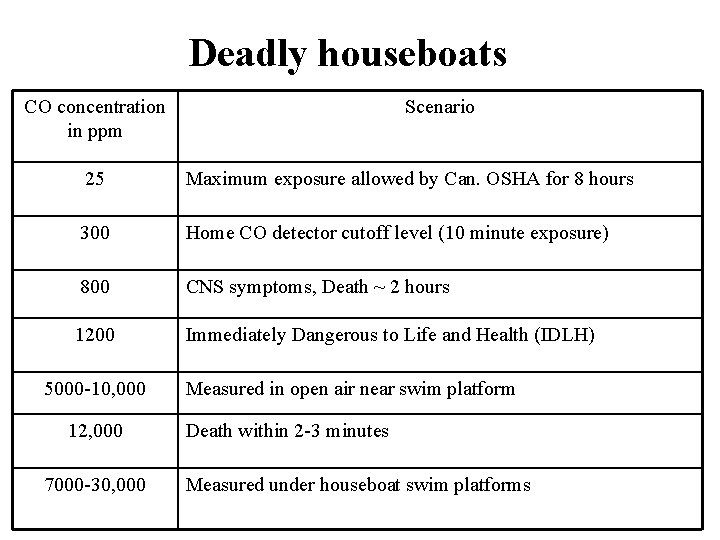
Deadly houseboats CO concentration in ppm Scenario 25 Maximum exposure allowed by Can. OSHA for 8 hours 300 Home CO detector cutoff level (10 minute exposure) 800 CNS symptoms, Death ~ 2 hours 1200 Immediately Dangerous to Life and Health (IDLH) 5000 -10, 000 12, 000 7000 -30, 000 Measured in open air near swim platform Death within 2 -3 minutes Measured under houseboat swim platforms

Physiology n n n Rapidly diffuses across alveolar-capillary membranes Binds to hemoglobin with 200 -250 X greater affinity than oxygen 10 -15% of total body CO taken up by tissue, bound to extravascular proteins q q Myoglobin Cytochrome oxidase Catalase Peroxidases

Pathophysiology

Pathophysiology n n n Left shift oxyhemoglobin dissociation curve Binding to cytochrome oxidase Activation of excitatory amino acids Binding to myoglobin Nitric oxide (NO)

Left shift n n CO increases the affinity of oxygen for hemoglobin Oxygen not displaced by CO is bound more tightly to Hb Lower oxygen delivery to cells Hypoxia
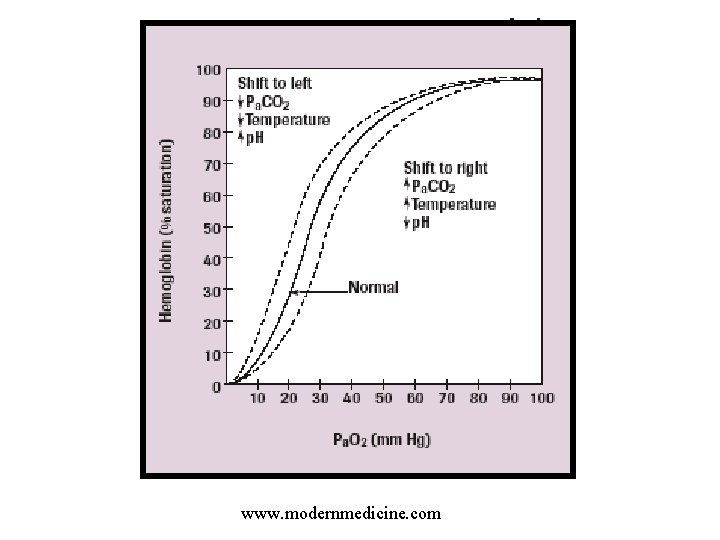
www. modernmedicine. com

Left shift / hypoxia n n n Does not explain all manifestations of poisoning Patients may remain comatose even after COHb undetectable Dissolved CO in plasma and delivery to target organs also important

Cytochrome oxidase inhibition n n n CO interferes with cellular respiration Decreased ATP production Initiates inflammatory cascade Lipid peroxidation Ischemic brain injury Binding may be increased under hypotensive or hypoxic conditions
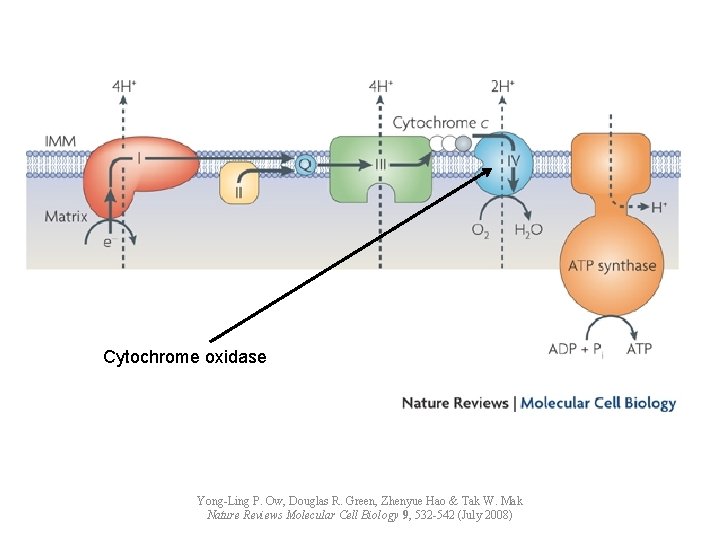
Cytochrome oxidase Yong-Ling P. Ow, Douglas R. Green, Zhenyue Hao & Tak W. Mak Nature Reviews Molecular Cell Biology 9, 532 -542 (July 2008)

Activation of excitatory amino acids n n n Tissue hypoxia increases excitatory amino acid levels Glutamate stimulates NMDA receptors and causes intracellular Ca++ release Delayed neuronal cell death

Myoglobin n CO binds with 60 X > affinity than O 2 q n n Binding enhanced under hypoxic conditions Leads to myocardial depression Carboxymyoglobin may explain dysrhythmias and ischemia that may occur with mild exposures q Especially with pre-existing CAD

Oh NO! n n CO displaces nitric oxide (NO) from platelets Actions of NO: q q Vasodilator Forms peroxynitrite radicals inactivate cytochrome oxidase Formation of platelet-neutrophil aggregates neutrophil adhesion in brain microvasculature End result: delayed lipid peroxidation
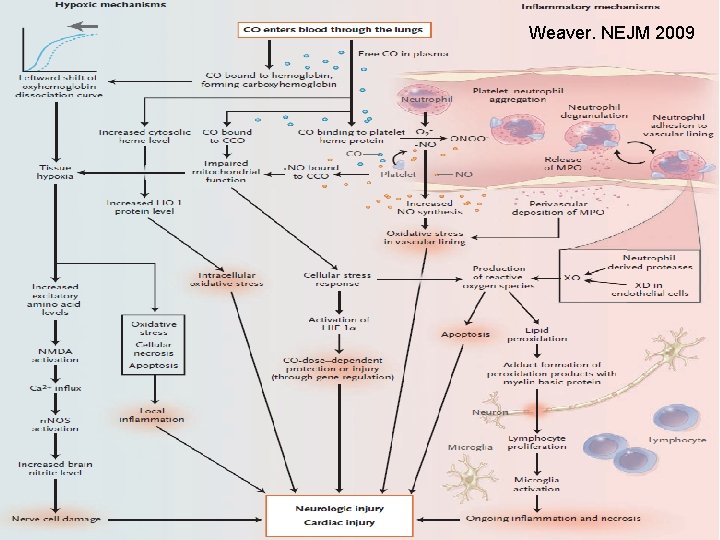
Weaver. NEJM 2009

Simpler version of previous slide n Too much CO = Bad

Clinical features of poisoning

Clinical features n n Early symptoms very nonspecific Often confused with other illnesses: q q Influenza Food poisoning Gastroenteritis Colic

Neurologic n Initial q n Headache, dizziness, nausea Later (higher levels/longer exposures) q q q Syncope, focal neuro sx suggesting CVA, LOC, confusion, seizures, coma Persistent neurologic sequelae Delayed neurologic sequelae (DNS)

Delayed Neurologic Sequelae n n Incidence between 2 -43% 2 days – 5 weeks after initial poisoning Neurologic and psychiatric symptoms q amnesia ■ headaches q psychosis ■ apraxia q parkinsonism ■ incontinence q paralysis ■ periph. neuropathy q chorea ■ dementia 50 -75% of cases resolve (may take months 1 year)

Who is at risk for DNS? n post-hoc analysis of Weaver 2002 RCT q n plus additional pts treated only with NBO not in trial Those most at risk of DNS: q q History of LOC Patients with long exposures (> 24 hours) Age > 36 COHb > 25%* n *Randomized trial data only, not separate NBO patients Weaver et al. Am J Resp Crit Care Med 2007; 176: 491 -7.

Cardiac n n n PVC’s and other dysrhythmias Myocardial ischemia Myocardial stunning With CAD, exacerbation of angina and arrhythmias can occur with COHb < 10% Acute mortality from CO usually from ventricular arrhythmias

n n 230 pts with moderate/severe poisoning all treated with HBO Indications for HBO: q LOC q Seizure q Focal neuro deficit q Ischemic chest pain q Dysrhythmias q COHb > 40% q COHb> 25% with Hx CV disease, age > 60, Hgb < 100, exposure > 2 hours

n n 85 (37%) had elevated Tn. I or CK-MB or diagnostic EKG changes of ischemia 32 (38%) eventually died compared with 22 (15%) of patients who had no myocardial injury q Effect persisted over many years
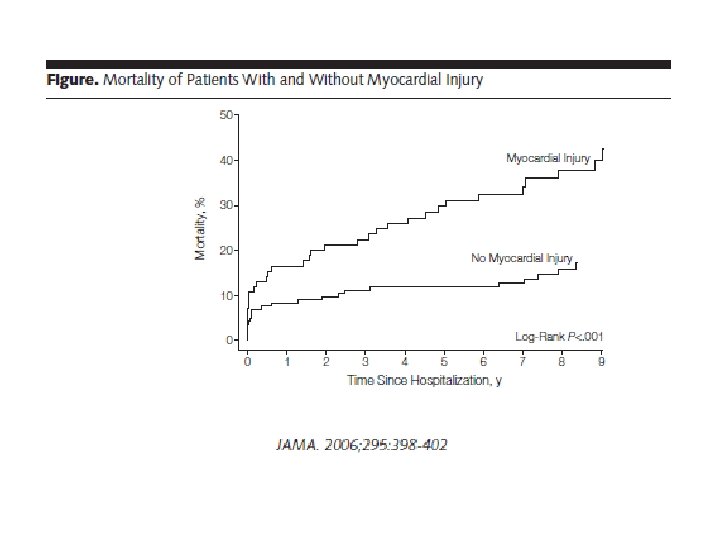

Diagnosis n n History and physical q Mini mental status exam Laboratory tests CO pulse oximetry q COHb / VBG q Select patients: EKG, cardiac markers Imaging q CT q MRI q n

COHb pulse oximeters n n Accurate 3% from COHb of 0 -40% Some false +ves q n Pre-hospital q n More during early use? Incident response paramedics Calgary Zone availability q q FMC, PLC, RGH triage UCC’s www. masimo. com
![[COHb] n n n Measured with co-oximeter Venous blood as accurate as arterial Normal [COHb] n n n Measured with co-oximeter Venous blood as accurate as arterial Normal](http://slidetodoc.com/presentation_image/31b3ec016fa2c03544e4e968a7729469/image-41.jpg)
[COHb] n n n Measured with co-oximeter Venous blood as accurate as arterial Normal levels 0 -5%, up to 10% in smokers Wide variation in clinical manifestations with identical levels Inaccurate predictor of peak levels q Variations in half lives q Effect of 02 given prior to sampling Not predictive of symptoms or final outcome

Blood gas n n Some HBO trials have used lactate > 2. 5 or base excess < -2 as indications for HBO Metabolic acidosis (hydrogen ion concentration) on presentation a better predictor of need for multiple HBO treatments than COHb* *Turner et al. J Accid Emerg Med 1999

Neuroimaging n n Abnormalities may be seen within 12 hours of CO exposure causing LOC Basal ganglia most commonly affected q q q n Caudate Putamen Globus pallidus Also subcortical white matter and hippocampus
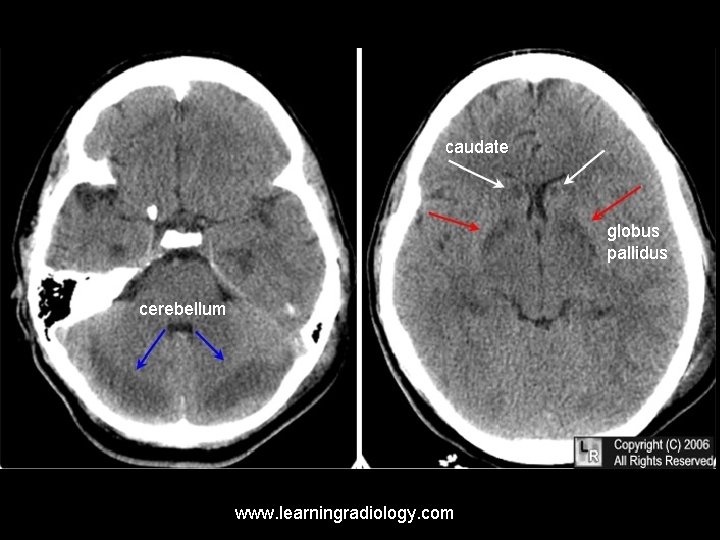
caudate globus pallidus cerebellum www. learningradiology. com

Management n n ABC’s O 2 via nonrebreather q Alters t ½ of COHb n n n 5 -6 hours at room air 40 -90 minutes on 02 via NRB Hyperbaric oxygen

HBO n n n 100% O 2 while exposed to increased atmospheric pressure Reduces the half-life of COHb to 23 minutes Mechanisms: q q q n Increases dissolved plasma [02] tenfold May help regenerate cytochrome oxidase Inhibits leukocyte adherence to the microvascular endothelium Does HBO prevent development of delayed neurologic sequelae?

n n n Non-blinded, randomized study of 629 adults, Rx within 12 h exposure q pregnant women, pts < 15 y. o. excluded Patients separated into LOC vs. no LOC prior to randomization into one of four groups q No LOC: 6 h NBO vs 4 h NBO +1 HBO Rx (2. 0 ATA X 1 hour) q LOC: 4 h NBO + 1 HBO vs 4 h NBO + 2 HBO Rx (all + 4 h NBO) Self-assessment questionnaire at 1 month following Rx re: neurologic sequelae

n n % complete recovery at 1 month: q No LOC: 66% NBO vs 68% HBO q LOC: 54% 1 HBO vs 52 % 2 HBO Conclusion: HBO not useful in pts with no LOC, and 2 sessions not useful in those who did have LOC

n n Randomized, non-blinded, 65 patients with mild poisoning , <6 hours of removal from exposure q LOC, cardiac compromise excluded 1 HBO Rx (120 mins, 2. 8 ATA) vs NBO until Sx resolved Mean time from randomization to HBO 2 hours Neuropsych tests done after Rx (baseline) then 3 -4 weeks after poisoning

n n Incidence of DNS: 23% NBO group, 0% HBO group Conclusion: HBO decreased incidence of DNS after CO poisoning

Scheinkestel et al, Med J Aust March 1999 n n Randomized, double-blind trial with 191 patients, all severities included q pregnancy, peds excluded Time to treatment 6. 6 -7. 5 h HBO: 3 days of 60 min Rx at 2. 8 ATA + continuous NBO q potentially 3 more HBO Rx if clinically ab. N after the first 3 NBO: continuous hi flow 02 for 3 days + sham dives

Scheinkestel et al, Med J Aust March 1999 n n n 46% lost to follow up Incidence of DNS: HBO 5/104; NBO 0/87 Conclusion: No benefit from HBO and may have worsened outcome, cannot be recommended

n n n Randomized trial of 152 patients Extensive inclusion criteria HBO group: 3 treatments (1 X 2. 8 ATA, 2 X 2. 0 ATA) NBO group: 100% 02 via NRB during 3 sham dives Neuropsych testing after chamber sessions 1 and 3, then 2 wks, 6 mos, 12 mos Primary outcome: cognitive sequelae at 6 wks.

n n n Higher cerebellar dysfunction in NBO group (15% vs 4%) At 6 wks, lower incidence DNS in HBO group (25% vs 46%) q persisted when adjusting for cerebellar dysfunction and also at 12 months (ITT analysis) Conclusion: 3 HBO Rx within 24 h period reduced risk of cognitive sequelae at 6 weeks and 12 months

n n Non blinded, randomized trial of 385 pts. aged 15 years and up Domestic CO poisoning only, October 1989 - January 2000 Patients separated into LOC vs. coma prior to randomization into one of four groups q LOC: NBO vs NBO +1 HBO Rx (2. 0 ATA X 1 hour) q coma: NBO +1 HBO Rx (2. 0 ATA X 1 hour) vs 2 HBO Rx Self-assessment questionnaire at 1 month re: neurologic sequelae

n n % complete recovery at one month following treatment q LOC: 58% NBO vs. 61% HBO q Coma: 68% HBO X 1 vs. 47% HBO X 2 (significant) Conclusion: no evidence superiority of HBO > NBO in patients with LOC. 2 HBO treatments associated with worse outcomes.

HBO Clinical Trials n Study design flaws: q q q q Randomization procedures Blinding Intent to treat analyses Follow up (most 15 -20% lost to f/u except one at 46%) Outcomes (questionnaires vs neuropsych battery, “complete recovery” vs. “cognitive sequelae”) NBO and HBO therapies used (duration, number of treatments) Excluded patients (pregnant, peds) Buckley et al. Toxicol Rev 2005; 24(2): 75 -92

HBO-suggested indications* n Syncope Altered LOC Coma Seizure Abnormal cerebellar function Age > 36 years Prolonged CO exposure (> 24 hours) COHb > 25% n Missing: myocardial ischemia n n n n Goldfrank’s Toxicologic Emergencies, 2011

Pregnant patients n n Fetal COHb concentrations tend to be higher than maternal levels (animal studies) Human studies suggest fetal Hgb affinity is similar to maternal Hgb affinity in low 02 states q n n More important issue is fetal hypoxia Maternal COHb does not predict fetal outcome Normal mental status with no LOC in mother = good outcomes, normal deliveries

Pregnant patients n n NBO treatment of pregnant patients q similar to nonpregnant patients q treat until mother is asymptomatic q benefit of prolonged Rx to mother unclear Indications for HBO in pregnant patients q same as for nonpregnant patients except: n lower COHb in mother at which HBO recommended (arbitrarily set at 15 -20%) n any features of fetal distress

Outcomes n Cardiac arrest patients

n n n 18 patients given HBO after cardiac arrest with ROSC Resuscitation time range 19 -45 min. Mean time to HBO 4. 3 hours post exposure COHb range 14 -55% All patients died during hospitalization (range 9 hours-7 days post discovery) HBO director survey of fictitious CO-induced arrest case: q q q 100% recommended HBO Chance of survival 74% Chance of recovery w/o neurologic sequelae 28%

CO poisoning and cardiac arrest n Quick summary of other studies: q q q n 5 peds smoke inhalations: 0 survivors 10 peds CO patients: 8 died, 2 had DNS 10 adult smoke inhalations: 0 survivors 11 adult CO patients: 0 survivors 23 adult CO patients: 17 died, 6 unknown outcome ? Role of CN poisoning in smoke inhalation victims

Objectives n By the end of the presentation, the participant should be able to: q q q List the mechanisms by which carbon monoxide (CO) causes toxicity Describe the clinical features seen with acute and delayed toxicity from CO Discuss the controversies in the management of CO poisoning, including the role of hyperbaric oxygen (HBO)

How to reach us n Poison and Drug Information Service: q q n 403 - 944 -1414 (Calgary) 1 -800 -332 -1414 (Alberta) Mark. yarema@albertahealthservices. ca
- Slides: 65