Toxic Alcohols Rama B Rao BellevueNYU Medical Center

Toxic Alcohols Rama B. Rao Bellevue/NYU Medical Center New York City Poison Control Center
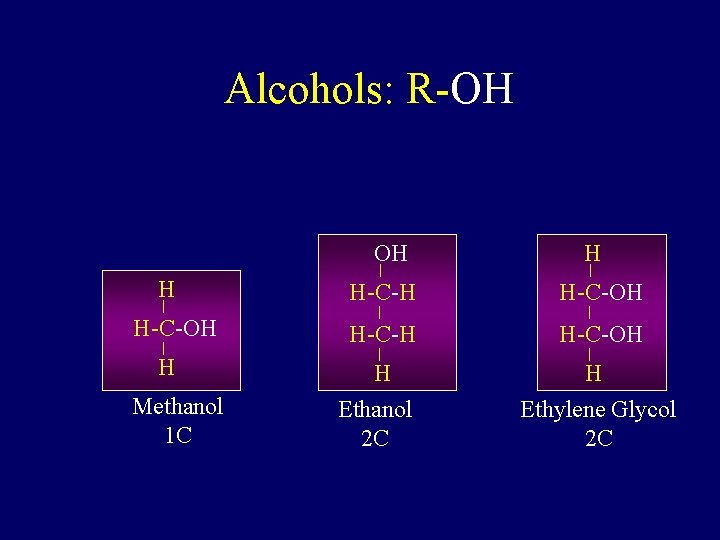
Alcohols: R-OH OH H H-C-OH H Methanol 1 C H H-C-H H-C-OH H Ethanol 2 C H Ethylene Glycol 2 C
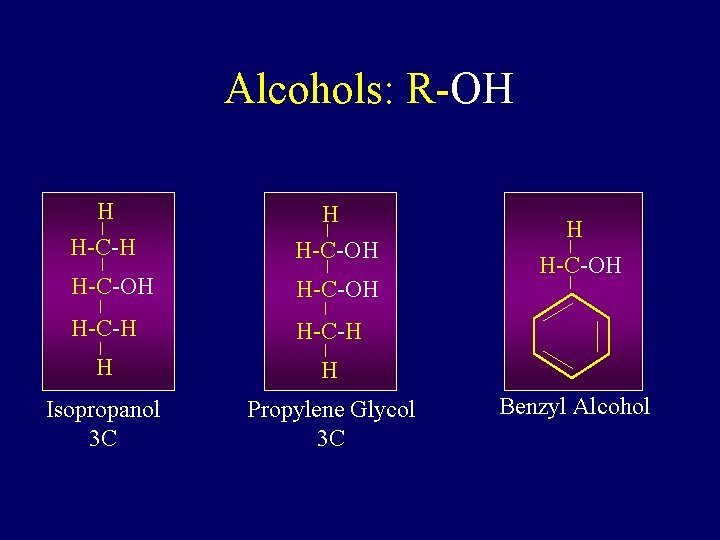
Alcohols: R-OH H H-C-OH H-C-H H H Isopropanol 3 C Propylene Glycol 3 C H H-C-OH Benzyl Alcohol

Ethanol OH H-C-H H Ethanol O ADH C-H H-C-H H Acetaldehyde ADH = Alcohol Dehydrogenase ALDH = Aldehyde Dehydrogenase O ALDH C-OH H-C-H H Acetic Acid

Methanol • Molecular weight 32 H • Low freezing point H-C-OH H • Highly volatility Methanol

Methanol • Gas Line Antifreeze 100% • Windshield washer fluid 30% • Varnish removers • Fuel for food warming 3 -70% • Industrial uses
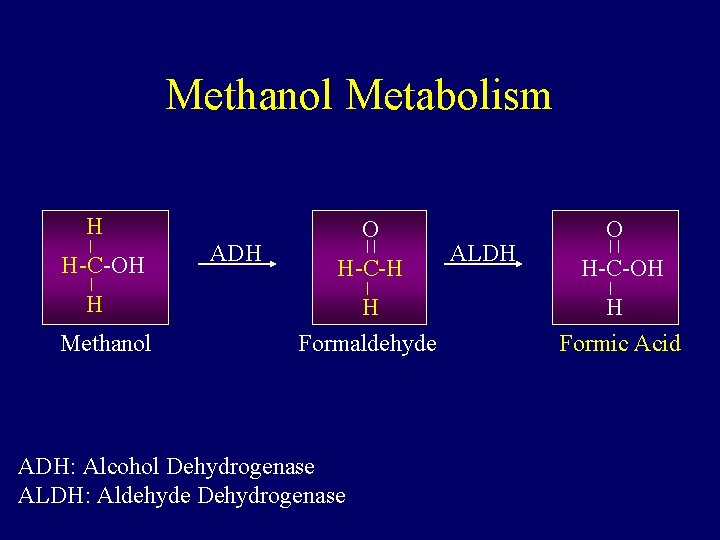
Methanol Metabolism H H-C-OH H Methanol ADH O H-C-H H Formaldehyde ADH: Alcohol Dehydrogenase ALDH: Aldehyde Dehydrogenase ALDH O H-C-OH H Formic Acid
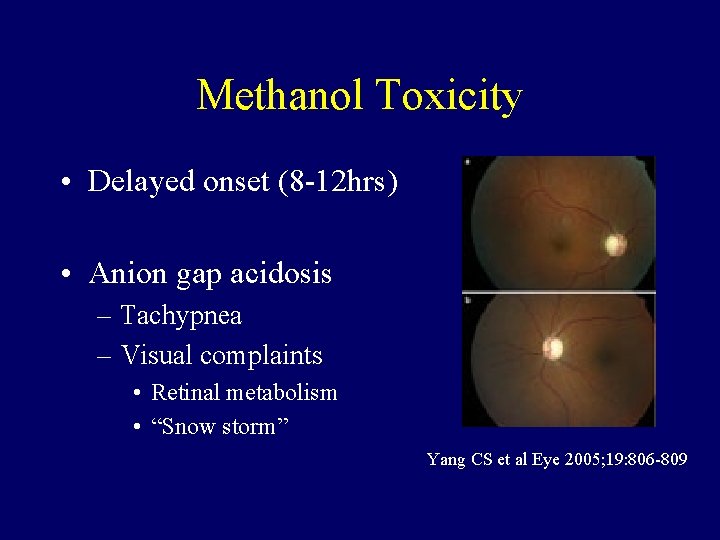
Methanol Toxicity • Delayed onset (8 -12 hrs) • Anion gap acidosis – Tachypnea – Visual complaints • Retinal metabolism • “Snow storm” Yang CS et al Eye 2005; 19: 806 -809

Methanol Toxicity • CNS depression – Bilateral hemmorhage putamen • Abdominal pain • Multisystem organ failure University of Western Ontario: Neurology Collection


Ethylene Glycol • Molecular Weight 62 H H-C-OH • Low Volatility • High boiling point H-C-OH H Ethylene Glycol

Ethylene Glycol • Coolant/Antifreeze • Solvents • De-Icer

Ethylene Glycol Metabolism H H-C-OH H Ethylene Glycol O ADH C-H O ALDH C-OH H-C-OH H Glycoaldehyde H Glycolic Acid ADH = Alcohol dehydrogenase ALDH = Aldehyde dehydrogenase

Ethylene Glycol Metabolism O O C-OH H-C-H H-C-OH H Glycolic Acid O Glyoxylic Acid LDH B 1, Mg 2+ -OH- Ketoadipic Acid O Oxalic Acid B 6 Glycine + Benzoic Acid Hippuric Acid LDH = Lactate dehydrogenase
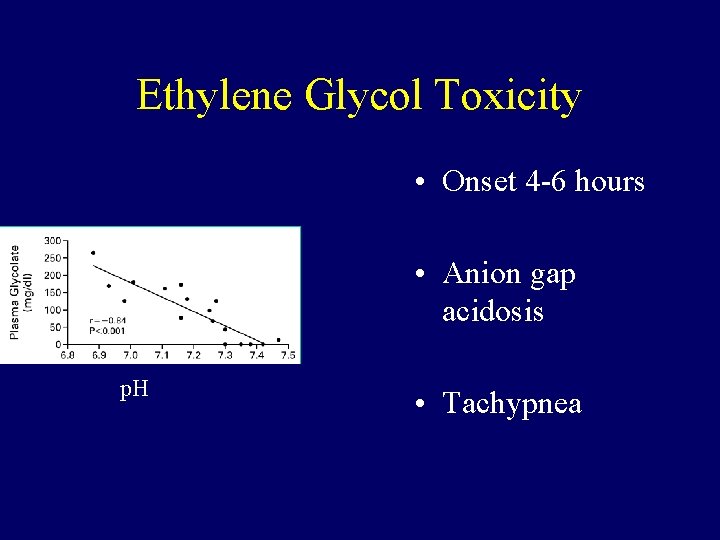
Ethylene Glycol Toxicity • Onset 4 -6 hours • Anion gap acidosis p. H • Tachypnea

Ethylene Glycol Toxicity • Abdominal pain • Hypocalcemia • Calcium oxalate crystals in urine • Renal failure

Identifying Patients for Treatment: Methanol/EG • Serum ethylene glycol or methanol level • Action level for treatment: 25 mg/d. L* * Or any level with acidosis

Treatment • Limit absorption: NG Tube • Prevent metabolism or parent compound to toxic metabolite ADH Inhibition • Enhance elimination Substrates/Other – Parent – Metabolites • Correct Derangements Hemodialysis
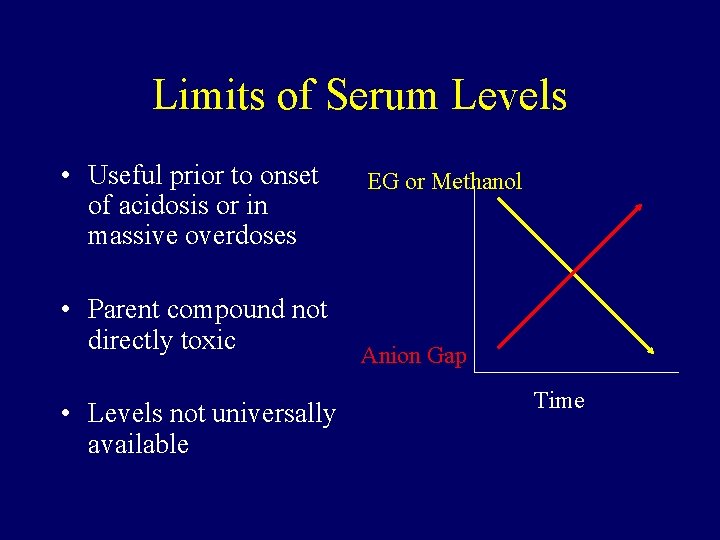
Limits of Serum Levels • Useful prior to onset of acidosis or in massive overdoses EG or Methanol • Parent compound not directly toxic Anion Gap • Levels not universally available Time
Arterial Blood Gas/Lactate • Acidosis indicates advanced poisoning • Lactate usually low* • Patients with acidosis should receive treatment *Some glycolates are misidentified as lactate

Adjunctive Information: Ethanol • Serum ethanol inhibits metabolism of EG and Methanol • Onset of toxicity EG/Methanol may be delayed

Adjunctive Information: Osmol Gap • Osmol Gap = Measured-Calculated Osmols • Calculated: 2 Na + BUN + Glucose + Alcohol 2. 8 18 N • N = MW Alcohol/10 • Must use freezing point depression
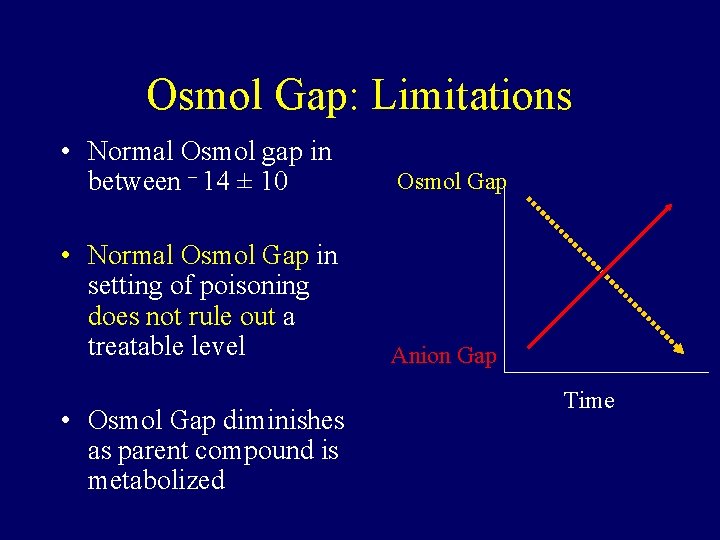
Osmol Gap: Limitations • Normal Osmol gap in between – 14 ± 10 Osmol Gap • Normal Osmol Gap in setting of poisoning does not rule out a treatable level Anion Gap • Osmol Gap diminishes as parent compound is metabolized Time
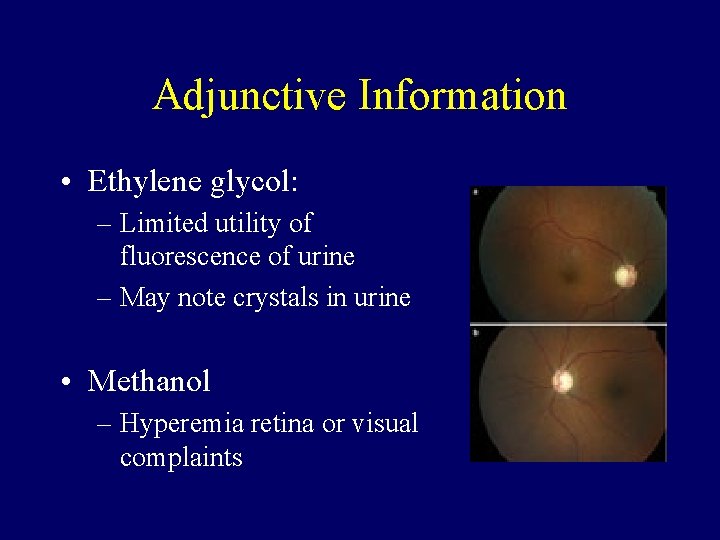
Adjunctive Information • Ethylene glycol: – Limited utility of fluorescence of urine – May note crystals in urine • Methanol – Hyperemia retina or visual complaints

Treatment: Methanol or Ethylene Glycol • Level 25 mg/d. L or • Anion gap metabolic acidosis ( non-lactate) with strong suspicion EG or Methanol exposure

Treatment Methanol Ethanol ADH Aldehyde ALDH Ethylene Glycol • Ethanol more avid for ADH – 6 -8 x more avid than ethylene glycol – 4 x more avid than methanol Acid

Ethanol • Concentration = Dose Vd (wt in kg) • Vd of ethanol = 0. 6 L/kg • Desired concentration 100 -200 mg/d. L

Ethanol • Target concentration 100 mg/d. L • Proof is 2 x concentration – 80 proof is 40% ethanol or 40 grams/100 m. L • 0. 8 gm/kg loading IV of 10% solution over 1 hour = 8 m. L/kg of 10% solution

Ethanol Infusion • 80 -130 mg/kg/hour depending on how fast a patient metabolizes • Needs to be increased to 250 mg/kg/hour or higher during dialysis

Ethanol Infusion: Management • Serial ethanol levels • Watch glucose* and sodium* • Observe for respiratory status* * Especially in children

Fomepizole • A blocker of alcohol dehydrogenase • Has replaced ethanol as the agent of choice in known or suspected exposures • Minimal adverse effects
Hemodialysis • Consult nephrology early in acidemic patients • Levels toxic alcohol 25 mg/d. L

Adjuncts for Methanol Poisoning • Sodium bicarbonate – p. H < 7. 30 – Can ion trap formic acid in urine and enhance elimination • Folate administration – Facilitates conversion of one carbon fragments to CO 2 – 1 mg/kg up to 50 mg every 4 hours

Adjuncts for Ethylene Glycol Poisoning O O C-OH H-C-H H-C-OH H Glycolic Acid O Glyoxylic Acid LDH B 1, Mg 2+ -OH- Ketoadipic Acid O Oxalic Acid B 6 Glycine + Benzoic Acid Hippuric Acid LDH = Lactate dehydrogenase

Adjuncts for Ethylene Glycol Poisoning • To enhance metabolism away from oxalates* – Thiamine 100 mg every 4 - 6 hours – Pyridoxine 50 mg every 4 -6 hours * Limited data

Diethylene Glycol • Elixir of Sulfanilamide disaster 1937 -38 • Renal failure 105 deaths • U. S. Legislation of Drug Safety

Benzyl Alcohol • Preservative in some medications H H-C-OH • Gasping Baby Syndrome – Potentially fatal in neonates Benzyl Alcohol

Isopropanol • Metabolized to acetone H H-C-OH • No acidosis H-C-H H • Supportive care Isopropanol 3 C

Glycol Ethers • Brake fluid • Solvents • Rarely metabolized to ethylene glycol • Supportive care

Propylene Glycol • Metabolized to lactate • Acidosis in ingestion H H-C-OH H-C-H • IV as diluent QRS widening, hypotension* H Propylene Glycol * Phenytoin diluent

Summary • For Methanol/EG Poisoning – Early Level, ABG, Lactate, Ethanol level – Caution in using osmol gap – Antidote: Ethanol or Fomepizole ( not both) – Hemodiaylsis – Consider sodium bicarbonate/folate for methanol – Thiamine and Pyridoxine for EG
- Slides: 41