Total Parenteral Nutrition TPN By E Salehifar Clinical


Total Parenteral Nutrition (TPN) By: E. Salehifar (Clinical Pharmacist)

Malnutrition Incidence: 50 % of hospitalized patients n Common causes: - Hypermetabolic states: Trauma, Infection, Major surgery, Burn - Poor nutrition n Consequences: Weakness, Decreased wound healing, increased respiratory failure, decreased cardiac contractility, infections (pneumonia, abscesses), Prolonged hospitalization n

Nutritional Support Enteral Nutrition ( Physiologic, less expensive) n Parenteral Nutrition - GI should not be used (Obstruction, Pancraitis) - GI can not be used ( Vomiting, Diarrhea, Resection of intestine, IBD) n

Parenteral Nutrition n n Peripheral Parenteral Nutrition (15 lit D 5 W/day for a 70 kg !!!) Central Parenteral Nutrition (TPN) n Needs CV-line to administer hyperosmolar solutions

Estimation of energy expenditure Harris-Benedict equations: n BEE (men) (kcal/day): 66. 47+13. 75 W+5 H-6. 76 A n BEE (women) (kcal/day): 655. 1+9. 56 W+1. 85 H 4. 68 A n TEE (kcal/day): BEE × Stress factor × Activity factor n Stress factors: Surgery, Infection: 1. 2 Trauma: Stress factors: 1. 5 Sepsis: 1. 6 Burns: 1. 6 -2 n Activity factors: sedentary: 1. 2 , normal activity: Activity factors: 1. 3, active: 1. 4 , very active: 1. 5

Stress level Normal/mild stress level: 20 -25 kcal/kg/day n Moderate stress level: 25 -30 kcal/kg/day n Severe stress level: 30 -40 kcal/kg/day Ø Pregnant women in second or third trimester: Add an additional 300 kcal/day n

Fluid: m. L/day n 30 -40 m. L/kg

Protein (amino acids) Maintenance: 0. 8 -1 g/kg/day n Normal/mild stress level: 1 -1. 2 g/kg/day n Moderate stress level: 1. 2 -1. 5 g/kg/day n Severe stress level: 1. 5 -2 g/kg/day n Burn patients (severe): Increase protein until significant wound healing achieved n Solid organ transplant: Perioperative: 1. 5 -2 g/kg/day n

Protein need in Renal failure Acute (severely malnourished or hypercatabolic): 1. 5 -1. 8 g/kg/day n Chronic, with dialysis: 1. 2 -1. 3 g/kg/day n Chronic, without dialysis: 0. 6 -0. 8 g/kg/day n Continuous hemofiltration: ≥ 1 g/kg/day n

Protein need in Hepatic failure n Acute management when other treatments have failed: With encephalopathy: 0. 6 -1 g/kg/day n Without encephalopathy: 1 -1. 5 g/kg/day n n Chronic encephalopathy n n Use branch chain amino acid enriched diets only if unresponsive to pharmacotherapy Pregnant women in second or third trimester n Add an additional 10 -14 g/day

Fat n Initial: 20% to 40 % of total calories (maximum: 60% of total calories or 2. 5 g/kg/day) n Note: Monitor triglycerides while receiving intralipids. Safe for use in pregnancy n I. V. lipids are safe in adults with pancreatitis if triglyceride levels <400 mg/d. L n

Components of TPN Formulations Macro: Calorie: Dextrose 20%, 50% Intralipid 10%, 20% Protein: Aminofusion 5%, 10% Micro: Electrolytes (Na, K, Mg, Ca, PO 4) Trace elements (Zn, Cu, Cr, Mn, Se)

Dextrose n 20%, 50% ( from CV-line) n 3. 4 kcal/g n 60 -70% of calorie requirements should be provided with dextrose
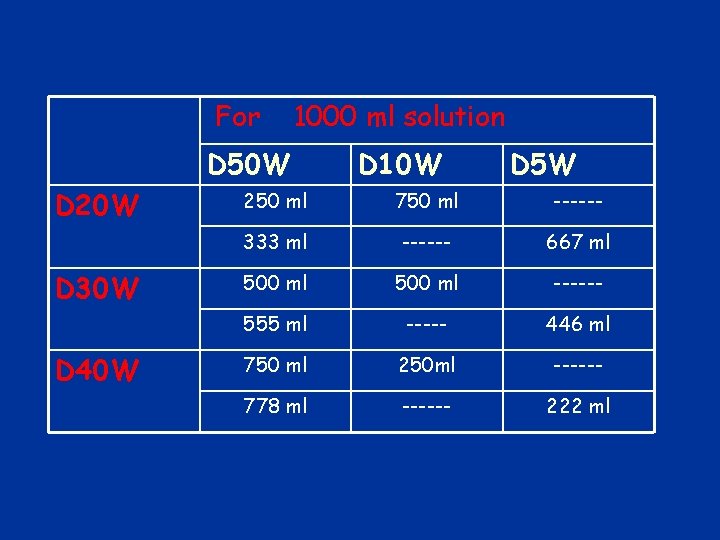
For 1000 ml solution D 50 W D 20 W D 30 W D 40 W D 10 W D 5 W 250 ml 750 ml ------ 333 ml ------ 667 ml 500 ml ------ 555 ml ----- 446 ml 750 ml 250 ml ------ 778 ml ------ 222 ml

Dextrose: Contraindications Hypersensitivity to corn or corn products n Hypertonic solutions in patients with intracranial or intraspinal hemorrhage n

Abrupt withdrawal n Infuse 10% dextrose at same rate and monitor blood glucose for hypoglycemia

Intralipid n 10%, 20% ( from peripheral or CV- line) n 1. 1 kcal/ml (10%), 2 kcal/ml (20%) n 30 -40% of calorie requirements should be provided with Intralipid

1022 Kcal/L 345 mosmol/L 1080 Kcal/L

Intralipid: Contraindication Hypersensitivity to fat emulsion or any component of the formulation; severe egg or legume (soybean) allergies n Pathologic hyperlipidemia, lipoid nephrosis, pancreatitis with hyperlipemia (TG>400 mg/dl) n

Aminofusion n 5%, 10% ( from CV-line) n 1 -1. 5 g/kg/day n Should not be used as a calorie source
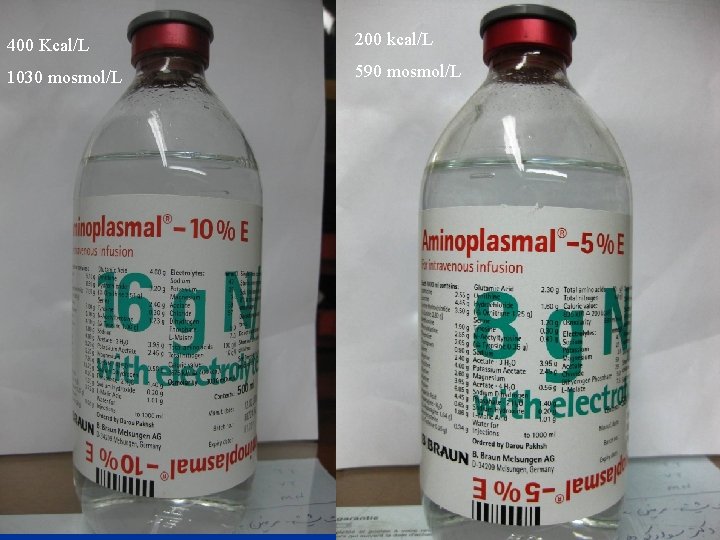
400 Kcal/L 200 kcal/L 1030 mosmol/L 590 mosmol/L


Amino acids: Contraindications Hypersensitivity to one or more amino acids n Severe liver disease or hepatic coma n

Case n D. C a 38 y. o man with a 12 -year history of crohn’s disease is admitted to surgery ward of Imam hospital in Sari for a compliant of increasing abdominal pain, nausea & vomiting for 7 days and no stool output for 5 days. Because of N & V, he has been drinking only liquids during the past weeks. His crohn disease had several exacerbations during the past 2 years and 10 cm of his ileum has been resected 6 month ago.

case (continue) Drugs: Mesalamine 1000 mg qid + prednisolone 10 mg/d. Abdominal x-ray is consisting with bowel obstruction. Exploratory laparotomy was performed and 25 cm of his ileum resected. Bowel sounds are absent. He has a right subclavian CV-line. Considering that his Ht=180 cm, Wt=60 kg (6 month ago: 70 kg) and Age=38 y. o, what is your recommended TPN formula for him?
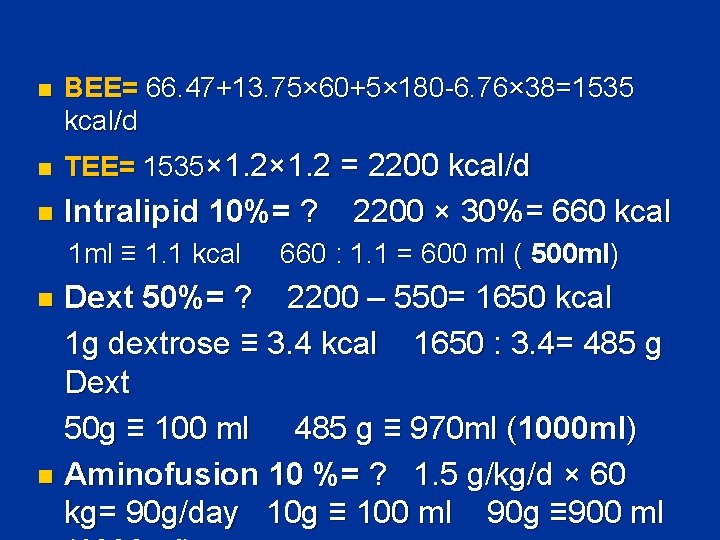

n BEE= 66. 47+13. 75× 60+5× 180 -6. 76× 38=1535 kcal/d n TEE= 1535× 1. 2 = 2200 kcal/d n Intralipid 10%= ? 2200 × 30%= 660 kcal 1 ml ≡ 1. 1 kcal 660 : 1. 1 = 600 ml ( 500 ml) Dext 50%= ? 2200 – 550= 1650 kcal 1 g dextrose ≡ 3. 4 kcal 1650 : 3. 4= 485 g Dext 50 g ≡ 100 ml 485 g ≡ 970 ml (1000 ml) n Aminofusion 10 %= ? 1. 5 g/kg/d × 60 kg= 90 g/day 10 g ≡ 100 ml 90 g ≡ 900 ml n

Electrolytes (daily requirements for TPN): n Na: 80 -100 m. Eq (50 - 100 ml Na. Cl 5%) n K: 60 -80 m. Eq (30 ml KCl) n Cl: 50 -100 m. Eq n Mg: 8 -16 m. Eq (5 -10 ml Mg. So 4 20%) n Ca: 5 -10 m. Eq (10 -20 ml Ca Gluconate 10%) n P 04: 15 -30 m. Eq n Acetate: 50 -100 m. Eq

Vitamins: A, D, E, Water soluble vitamins n Trace Elements: n n Zn, Se, Cu, Cr, Mn n ↓ Zn n Delayed ulcer healing, Dermatitis, Alopcia (5α reductase), Diarrhea n↓ Se: Low activity of SOD & Deiodinase n Amp B Complex + Amp Vit C MV Therapeutic ( Zn, Cu, Mn)



Special Considerations Max infusion rate of dextrose: 0. 5 g/kg/h (to avoid hyperglycemia, glycosuria, fatty liver, hyperosmolar coma) n K should be added to dextrose solutions n Slow starting & slow tapering of Dext 50% n If BS>200, Insulin should be added n some brands of lipids can be mixed with Dext+Aminifusion in the same IV container n

Special Considerations n Intralipid contraindications: Severe egg allergy n Hyperlipidemia n n Special aminoacid products: n Hepatamine: for Hepatic Failure n ↑ branched chain aa ( leu, isoleu, val) n Nephramine: for Renal Failure n Primarily essential aa with lower concentrations

Monitoring: n Baseline: Wt, Na, K, BUN, Cr, Glu, Ca, P, Mg, CBC, PT, INR, TG, LFT, Alb, Pre-Alb n Daily: Wt, V/S, I-O, Na, K, BUN, Cr, Glu, Sign/Symptoms of infection 2 -3 times a week: CBC, Ca, P, Mg n Weekly: Alb, Pre-Alb, LFT, INR, Nitrogen n Balance

Adding other drugs to TPN INS n Heparin n H 2 -blocker n Alb n Aminophylline n n Vit K & Bicarbonate should not be added

Complications n Endocrine & metabolic n n Hepatic n n Cholestasis, cirrhosis (<1%), gallstones, liver function tests increased, pancreatitis, steatosis, triglycerides increased Renal n n Fluid overload, hypercapnia, hyperglycemia, hyper/hypokalemia, hyper-/hypophosphatemia, refeeding syndrome Azotemia, BUN increased Infectious n Bacteremia, catheter-induced infection, exit-site infections

Refeeding syndrome In patients with long-standing or severe malnutrition n Is a medical emergency, consist of: n Electrolyte disturbances (eg, potassium, phosphorus) n Respiratory distress n Cardiac arrhythmias, resulting in cardiopulmonary arrest n n Do not overfeed patients; caloric replacement should match as closely as

Conclusion Malnutrition is a common problem & Nutritional support is indicated in many hospitalized patients n Enteral nutrition is better, but some patients with GI problems need TPN n Dextrose & Intralipid should be used as calorie sources and Aminofusion as aminoacid source n Special monitoring should be considered for patients especially I-O, Na, K and Glu n

- Slides: 43