Total Femoral Replacement Sarah Smith SPTA In 2015

















- Slides: 23

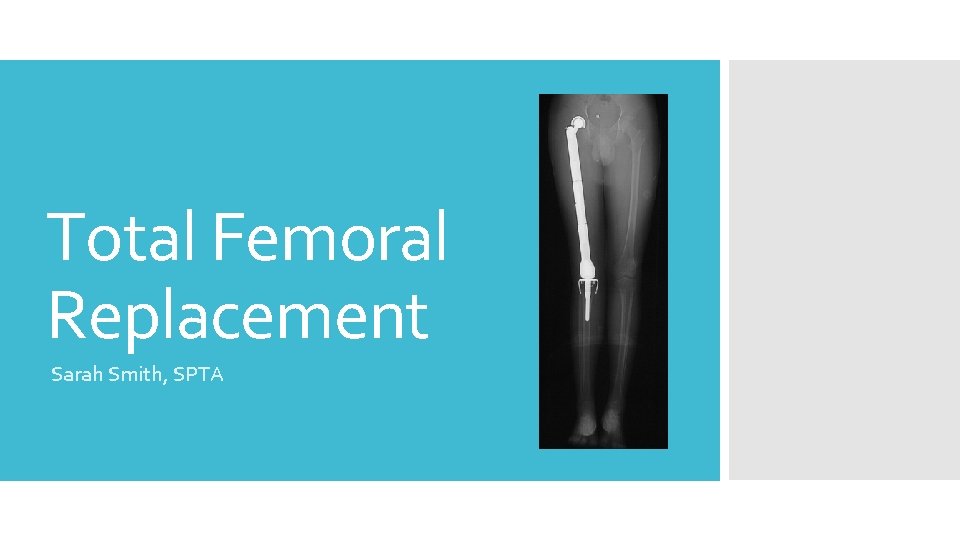
Total Femoral Replacement Sarah Smith, SPTA

In 2015, over 3000 individuals were diagnosed with primary bone cancer and over 925, 000 TKAs and 378, 000 THAs were performed along with 75 K TKA and 50 K THA revisions. [1] Introduction Due to the increase of arthroplasties and subsequent revisions being performed along with an increase in primary bone cancers, Total Femoral Replacements (TFR) are growing in demand as a limb salvaging procedure for these challenging patient populations. As part of a patient’s healthcare team, we need to be aware of their precautions, rehabilitation guidelines, expected outcomes and potential complications to appropriately treat and educate these patients throughout their recovery.

§ Recognize the value of a TFR as a limb salvaging procedure optimizing function § Know TFR precautions Objectives § Understand TFR rehabilitation guidelines § Understand expected TFR functional outcomes § Understand the possible complications associated with a TFR

§ Failed THA or TKA with insufficient bone stock for reimplantation of prosthesis. (i. e. multiple revisions) § Complex periprosthetic fracture not amendable to other treatment. (i. e. Internal fixation) § Failed internal fixation of complex periprosthetic fracture. Indications § Limb salvage procedure for oncology patients § Osteomyelitis § Complex trauma of femur

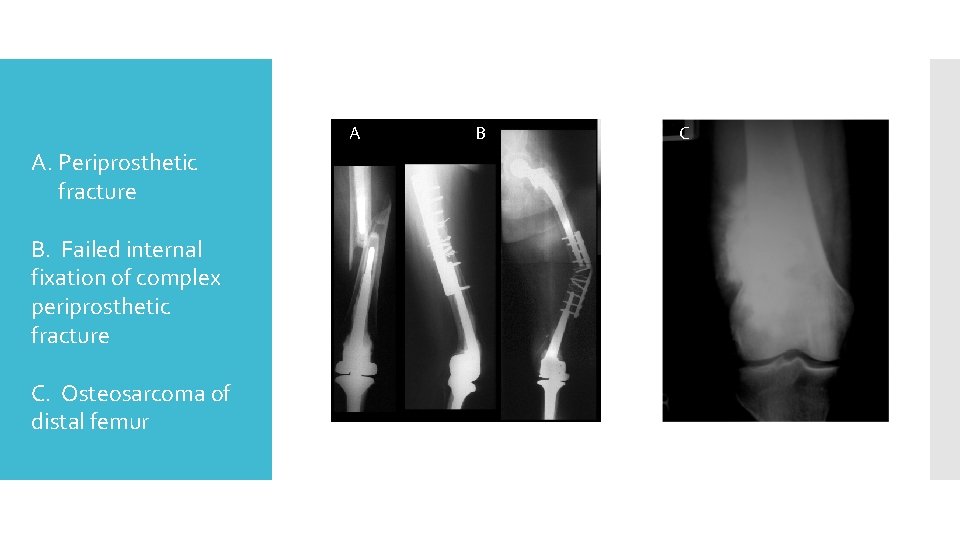
A. Periprosthetic fracture B. Failed internal fixation of complex periprosthetic fracture C. Osteosarcoma of distal femur A A B B TFR Procedure C

Contraindications §Nonfunctional quadriceps mechanism §Inadequate tibial host bone for fixation

§ Comprehensive Patient Evaluation § Patient Education Course of Action § Possible Complications § Precautions § Expected Outcomes § Rehabilitation guidelines § TFR prostheses § Intramedullary TFR (IM-TFR) § Conventional TFR (“tumor-type” ) § Custom-made § Modular § Surgical Procedure

§ Identify the cause of implant failure § Infection screening & blood tests Comprehensive Patient Evaluation § Examine the soft tissues of the lower extremity to ensure adequate soft tissue coverage of the prosthesis. § Evaluate motor strength of hip and knee, compare leg lengths, and assess distal neurovascular status. § Document any history of hip instability. § Imaging

§ Explain the complexity of a TFR § Explain alternative treatments § Possible complications Patient Education § Precautions post surgery § Rehabilitation guidelines § Explain expected outcomes, i. e. procedure will not return them to normal function, may require an assistive device for the remainder of their lives. § Donning and Doffing brace if necessary

IM-TFR IM-TFR: is the prosthetic linkage of a previously implanted THA and TKA components. Advantage of the IM-TFR: reduction in extensive dissection and the ability of maintaining soft tissue attachments.

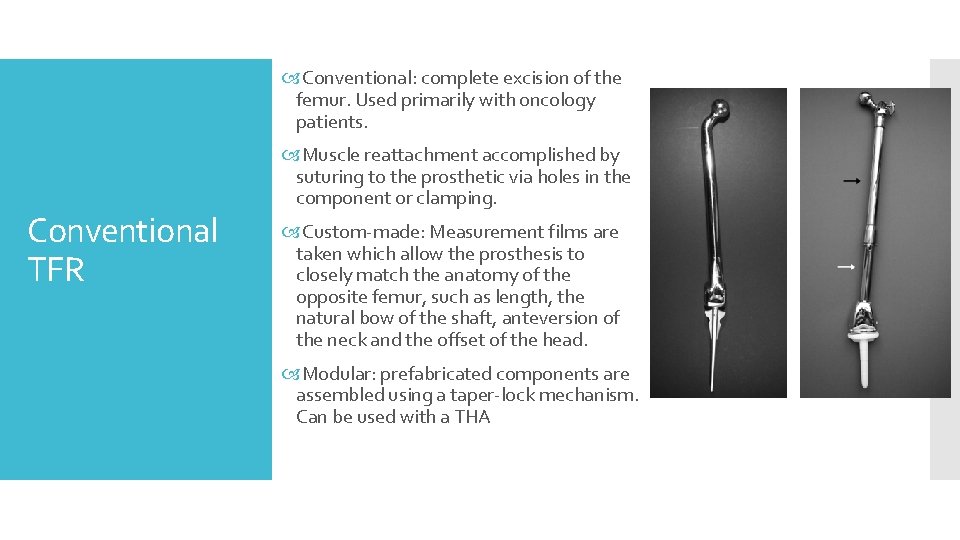
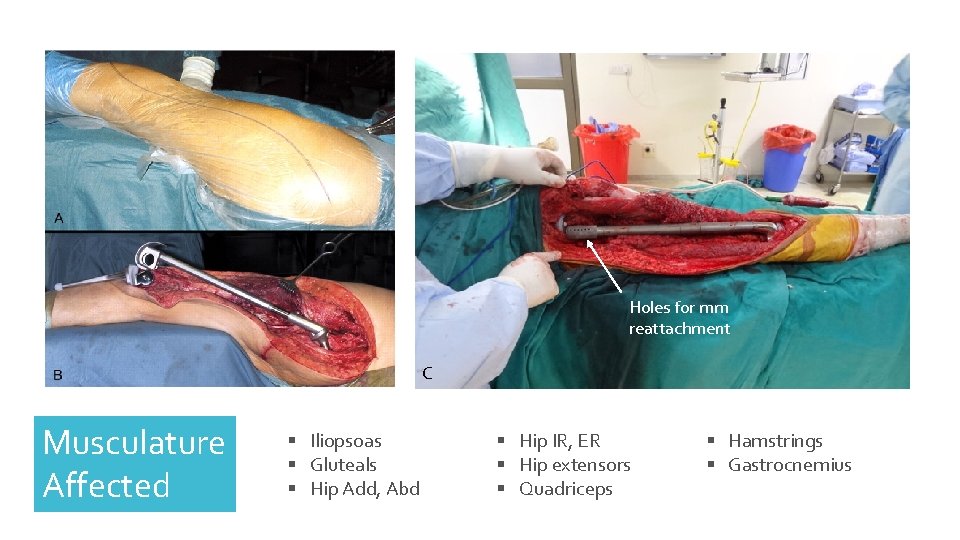
Conventional: complete excision of the femur. Used primarily with oncology patients. Conventional TFR Muscle reattachment accomplished by suturing to the prosthetic via holes in the component or clamping. Custom-made: Measurement films are taken which allow the prosthesis to closely match the anatomy of the opposite femur, such as length, the natural bow of the shaft, anteversion of the neck and the offset of the head. Modular: prefabricated components are assembled using a taper-lock mechanism. Can be used with a THA

Posterior approach to the hip -> lateral femur -> lateral parapatellar Split TFL and IT band in line with the incision. Conventional Surgical Technique (in a nutshell) Release the short external rotators, and lateral, anterior, posterior aspects of the femur. Osteotomy at mid femur to mobilize the proximal and distal segments, allowing for release of the medial side of the femur Remove the proximal femur and peel the abductors from the greater trochanter Perform trial of Femur, assess hip stability, knee range of motion, leg length, patellar tracking, and overall soft tissue tension. Assemble components. Cement the tibia in place, and then link the femoral prosthesis and reduce at the hip. Place deep drains. Reattach the vastus lateralis, abductors, and external rotators to the prosthesis via sutures and/or clamps Repair the TFL with sutures, then close the subcutaneous tissues and skin

Holes for mm reattachment C Musculature Affected § Iliopsoas § Gluteals § Hip Add, Abd § Hip IR, ER § Hip extensors § Quadriceps § Hamstrings § Gastrocnemius

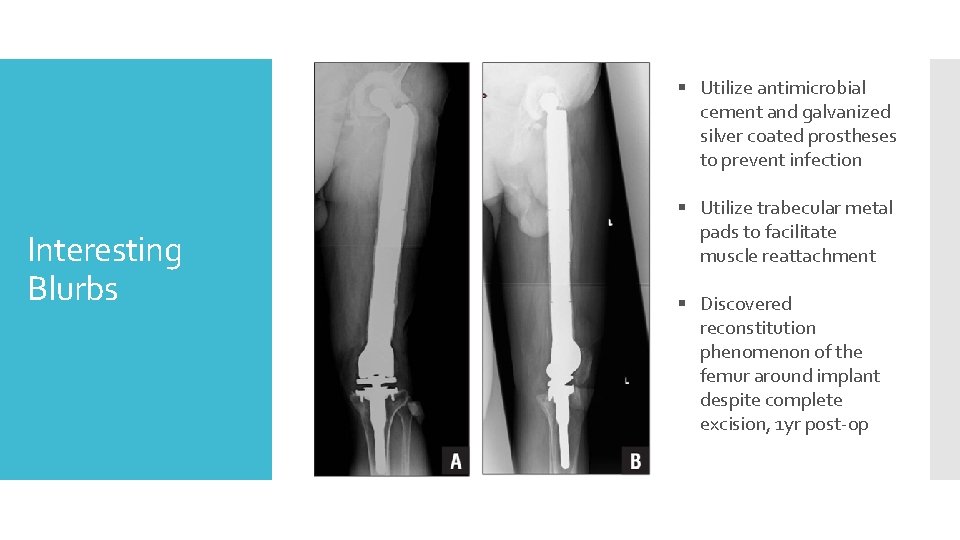
§ Utilize antimicrobial cement and galvanized silver coated prostheses to prevent infection Interesting Blurbs § Utilize trabecular metal pads to facilitate muscle reattachment § Discovered reconstitution phenomenon of the femur around implant despite complete excision, 1 yr post-op

§ Periprosthetic Infection § Hip instability, dislocation § Soft-tissue failures § Aseptic loosening § Structural failure Possible Complications § Transfusion § Neuropraxia § TFR Revision § Admission to high-dependency unit § Hip disarticulation § “The implant survival rate was 86% at 10 years; however, the 10 year mortality rate was 58%. Although TFR for salvage of a periprosthetic fracture of the femur offers good functional outcome and implant survival, it is at the expense of postoperative complications, . . . TFR is associated with a high long-term mortality rate. ” (Total Femoral Replacement for Salvage of Periprosthetic Fractures, Sept. 2014 - Volume 37 – Isuue 9: e 789 e 795)

§ No hip flexion > 90 § No hip adduction beyond midline § No IR of operated hip § No twisting of the knee or kneeling Precautions § *WB restrictions if allograft was used § *No knee flexion § Patellar tendon was reattached § Immobilizer ~2 wks § *No abduction against gravity § Abductors were reattached with sutures and/or clamp to prosthesis § Abd brace ~6 -8 wks

§ 12 -18 months to achieve an optimal outcome § Knee ROM 0 - 120 § Possible 5 quads lag Expected Outcomes § Independent or Modified Independent, most will require an assistive device § Independent with ADLs with/without adaptive equipment. § Grade 4 hip abduction is an optimal outcome, some patients may not achieve this, may walk with a Trendelenburg gait or lateral tilt bend

§ Static LE strengthening-> AROM § PROM Abd -> AROM gravity minimized § Knee Flexion once brace is discontinued ~2 wks § Teach to don and doff brace independently Rehabilitation 0 -6 wks § Maintain full AROM at knee and ankle § Gait training with appropriate AD, adhering to WB restrictions and precautions § Practice stairs as appropriate. § Practice transfers as appropriate, maintaining precautions. § Educate and encourage independence with HEP.

§ Progress ROM and strengthening of LE, (focus on abd, quads, gluteals) § Wean off Abd brace § Gait training § Progress Assistive Device Rehabilitation 6 wks-18 mths § Increase Proprioception § Increase WB § Balance Activities § Core stability and posture exercises § Hydrotherapy § Swimming: Once brace is removed with sufficient hip control § Educate and encourage independence with HEP. § Progress may continue up to 18+ months

Pros & Cons § Avoid amputation, retain ability to ambulate § High 10 yr mortality rate 58% § Immediate fixation permits early mobilization § Require an AD indefinitely § Improved overall function § Hip and/or Knee instability requiring revision § High implant survival 86% § Infection § Numerous possible complications

The TFR is a useful procedure for patients that would otherwise require amputation due to extensive femoral bone loss as a result of revision arthroplasty, periprosthetic infection and fractures as well as oncology patients. Despite the possibility of numerous complications associated with a TFR, overall function and quality Summary of life is improved. Careful patient selection, excellent surgical technique, a comprehensive rehabilitation program including patient education, and the prompt management of postoperative complications are essential to ensure optimal long-term outcomes in this challenging patient population.

References 1. Kurtz SM, Ong KL, Lau E, Bozic KJ. Impact of the economic downturn on total joint replacement demand in the United States: updated projections to 2021. J Bone Joint Surg Am. 2014; 96: 624 -630. 2. Total Femur Arthroplasty. Orthopaedics. One Articles. In: Orthopaedics. One - The Orthopaedic Knowledge Network. Created Aug 20, 2011 20: 20. Last modified Sep 07, 2011 14: 57 ver. 5. Retrieved 2016 -09 -19 3. Standardization of rehabilitation after limb salvage surgery for sarcomas improves patients’ outcome, Shehadeh, Ahmad et al. Hematology/Oncology and Stem Cell Therapy , Volume 6 , Issue 3 , 105 – 111. September–December, 2013 Volume 6, Issues 3 -4, Pages 105– 111. 4. Hwang J, Beebe K, Patterson F, Benevenia J. Infected Total Femoral Replacements: Evaluation of Limb Loss Risk Factors. ORTHOPEDICS. 1; 34: e 736 -e 740. doi: 10. 3928/01477447 -20110922 -11 5. Clement N, Mac. Donald D, Ahmed I, Patton J, Howie C. Total Femoral Replacement for Salvage of Periprosthetic Fractures. ORTHOPEDICS. 2014; 37: e 789 -e 795. doi: 10. 3928/01477447 -20140825 -55 6. Rehabilitation guidelines following Total Femoral Replacement Surgery, Royal National Orthopaedic Hospital with UCL Institute of Orthopaedics and Musculodkeletal Science, March 2014 RC/SH/KS, Review March 2016, https: //www. rnoh. nhs. uk/ourservices/rehabilitation-guidlelines 7. Ramanathan, Deepak et al. “Current Concepts in Total Femoral Replacement. ” World Journal of Orthopedics 6. 11 (2015): 919– 926. PMC. Web. 21 Sept. 2016.
