Total Bowel Dysmotility TPN Dependency A Case Study

Total Bowel Dysmotility & TPN Dependency A Case Study Ashley Ropolo Spring 2012

Patient Information • 21 year old African American Male • Allergies: Amoxicillin & Vancomycin

Social History • Denies alcohol, tobacco or drug use

Past Medical History • Chronic TPN dependency • Atonic/dysfunctional bladder • Multiple port-a-cath infections • Chronic malnutrition • Total bowel dysmotility

Past Surgical History • Colectomy • Ileostomy • G-tube: venting • J-tube: feeding • Cholecystectomy • 7 port-a-cath placement & removals

Current Admission • Admitted to Mc. Kay-Dee on March 6, 2012 • Admit Dx: – Abdominal pain – Distention – Decreased ostomy output • Short bowel resection & revision of ileostomy

Total Bowel Dysmotility • Abnormality of smooth muscle function in the GI tract, i. e. gastroparesis – When impaired, contents may become trapped and cause distention • Symptoms: Bloating, N/V or malnutrition

Nutrition Support • TPN dependency when GI tract not functioning – Life expectancy lower – Life span is ~50 years – High risk for infection • TF used when GI tract is functioning – Recently placed J-tube to initiate enteral feedings

Complications of long-term TPN dependency • Doesn’t preserve GI tract structure and function • Infections >50% of patients • Glucose abnormalities and/or liver dysfunction in >90% of patients **Also very expensive

Reasons for Nutrition Support • Unable to consume sufficient energy orally – Malnourishment

Anthropometrics • Current Wt: 52. 7 kg/116 lbs • Current Ht: 175 cm/69” • BMI: 17. 21 • IBW: 72. 3 kg/159 lbs %IBW: 73%
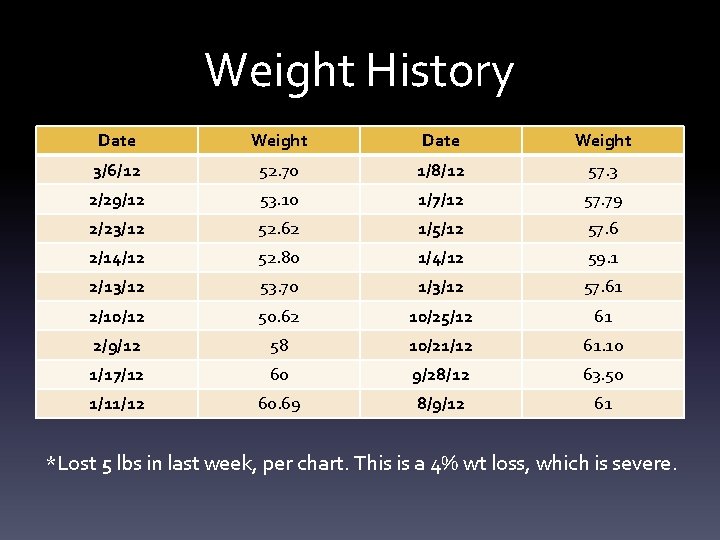
Weight History Date Weight 3/6/12 52. 70 1/8/12 57. 3 2/29/12 53. 10 1/7/12 57. 79 2/23/12 52. 62 1/5/12 57. 6 2/14/12 52. 80 1/4/12 59. 1 2/13/12 53. 70 1/3/12 57. 61 2/10/12 50. 62 10/25/12 61 2/9/12 58 10/21/12 61. 10 1/17/12 60 9/28/12 63. 50 1/11/12 60. 69 8/9/12 61 *Lost 5 lbs in last week, per chart. This is a 4% wt loss, which is severe.
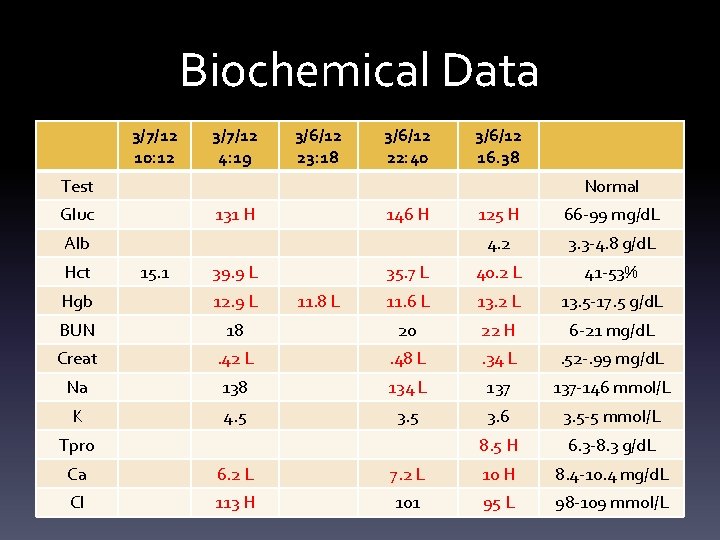
Biochemical Data 3/7/12 10: 12 3/7/12 4: 19 3/6/12 23: 18 3/6/12 22: 40 3/6/12 16. 38 Test Normal Gluc 131 H 146 H 125 H 66 -99 mg/d. L 4. 2 3. 3 -4. 8 g/d. L 35. 7 L 40. 2 L 41 -53% 11. 6 L 13. 2 L 13. 5 -17. 5 g/d. L Alb Hct 15. 1 39. 9 L Hgb 12. 9 L 11. 8 L BUN 18 20 22 H 6 -21 mg/d. L Creat . 42 L . 48 L . 34 L . 52 -. 99 mg/d. L Na 138 134 L 137 -146 mmol/L K 4. 5 3. 6 3. 5 -5 mmol/L 8. 5 H 6. 3 -8. 3 g/d. L Tpro Ca 6. 2 L 7. 2 L 10 H 8. 4 -10. 4 mg/d. L Cl 113 H 101 95 L 98 -109 mmol/L
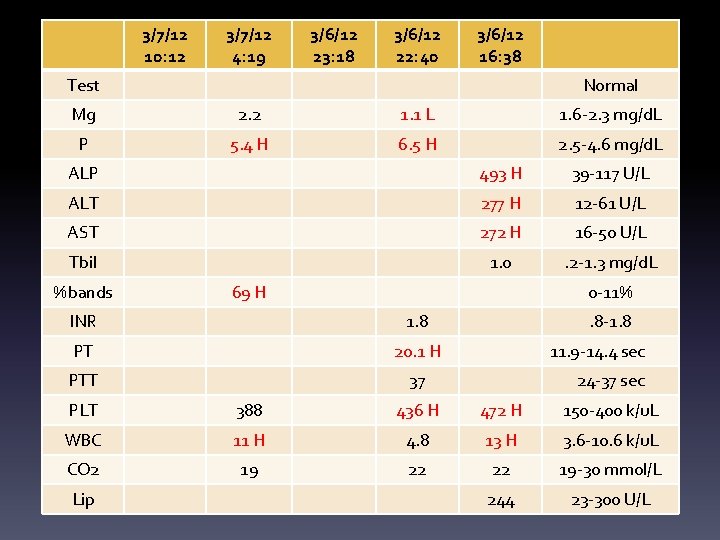
3/7/12 10: 12 3/7/12 4: 19 3/6/12 23: 18 3/6/12 22: 40 3/6/12 16: 38 Test Normal Mg 2. 2 1. 1 L 1. 6 -2. 3 mg/d. L P 5. 4 H 6. 5 H 2. 5 -4. 6 mg/d. L ALP 493 H 39 -117 U/L ALT 277 H 12 -61 U/L AST 272 H 16 -50 U/L Tbil 1. 0 . 2 -1. 3 mg/d. L %bands 69 H 0 -11% INR 1. 8 PT 20. 1 H PTT 37 . 8 -1. 8 11. 9 -14. 4 sec 24 -37 sec PLT 388 436 H 472 H 150 -400 k/u. L WBC 11 H 4. 8 13 H 3. 6 -10. 6 k/u. L CO 2 19 22 22 19 -30 mmol/L 244 23 -300 U/L Lip

Biochemical Information • High glucose levels likely d/t infection and stress • Lower Hct and Hgb with surgery (bowel resection, revision of ileostomy and bowel adhesions) – Pt is likely anemic given he is malnourished, not compliant with feedings and d/t his chronic condition • BUN is likely high on first day with infection • Low creatinine likely low with muscular atrophy • Low Na d/t IV fluids, but is not a concern as it has returned to normal • High tpro with possible dehydration upon admit • Low calcium with elevated P and high P with hypocalcemia • Low Mg d/t IV’s • High ALP, AST and ALT d/t stress and initially, TPN overfeeding • High PT with anticoagulant therapy and high PLT with anticoagulant therapy and possible iron deficiency anemia • High WBC with infection.

Pertinent Medications • Regular Insulin – Antihyperglycemic • Merrem – Antibiotic

Estimated Needs • Energy: 1550 -1850 kcals – 30 -35 kcals/kg • Protein: 130 g – 2. 5 g/kg • Fluid: 1800 m. L – 35 m. L/kg **Used actual body weight

Diet Order • TPN: initial – 130 g 10% aminosyn, 900 kcal D 70, 200 kcal 20% lipid = 1620 kcal (31 kcal/kg) 130 g pro (2. 5 g/kg) • Trophic TF started 3/13 at 10 m. L/hr – Impact Peptide 1. 5 – Tolerating – 3/16: increased to 20 m. L/hr • Scheduled to increase to 30 m. L/hr at midnight – 3/18: 30 m. L/hr - tolerated • Fluid increased to 3 L/day – 1. 75 L out of ileostomy, 2. 5 L out of G-tube – Pt felt dehydrated: LR bolus ordered (lactated ringers = fluid) – 3/18: TF placed on hold, abdominal fluid drained; start TF in the am • 3/20: ALK trending up = overfeeding – Decrease kcals on TPN, TF remains at 30 m. L/hr with fair tolerance • 3/21: discharged on TF and TPN

Diet Evaluation • Experienced overfeeding with initial volumes; feedings decreased – ALK trending up, decreased kcals in TPN. TF at 30 ml/hr with fair tolerance. Advance as tolerated. • Goal rate: 75 m. L/hr • Liver tests elevated (ALT=1000’s) which is indicative of overfeeding

Diet Hx • Chronic TPN use – 7 years – Non-compliant at home (stops early) • Adjusted feedings, so eventually he would receive appropriate nutrition with current habits – Initiated tube feed to wean from TPN

Nutrition Note • Pt with stable weight since recent D/C and normal admit Alb, suggesting home nutrition support (TF + TPN) adequate for maintenance. Estimated intake based on notes from Imed NSS team is ~2700 kcals (51 g/kg) and 140 -170 g pro (2. 7 -3. 2 g/kg). Note that pt does have hx of noncompliance with TPN. ? if he has received all kcal and protein as ordered. Current TF calculated to provide 40 kcal/kg and 2. 5 g/kg pro, which is adequate to promote weight gain.

Treatment & Progress • Note that TF and TPN changed since note was written. TPN rate decreased d/t overfeeding. • Operation: – Cut the adhesions (scar tissue between bowel and peritoneal cavity) decompressed bowel, 5 L liquid stool removed (likely caused the obstruction) – Revision of ileostomy fix the opening – Partial bowel obstruction

Nutrition Care Plan • Problem – Alterned GI fxn R/t hx dysmotility, SBO requiring resection AEB hx of poor TF tolerance at home, GI surgery. • Goal – Meet nutritional needs • Intervention – TPN via port-a-cath: 130 g 10% aminosyn, 900 kcal D 70, 200 kcal 20% lipid = 1620 kcal (31 kcal/kg), 130 g (2. 5 g/kg)

Conclusion • High nutrition risk – Malnutrition and need for nutrition support • Chronic TPN use for 7 years. Recently placed G-tube for venting/suction and J-tube for feeding in hope that he would eventually be able to meet his needs through TF • Recently had a total colectomy with an ileostomy to attempt to move from TPN to enteral nutrition • Pt d/c on TPN and TF • Overall prognosis fair

References • The Merck Manual of Diagnosis and Therapy. 19 th ed. Whitehouse Station, NJ: Merck Sharp and Dohme Corp; 2011. • Taber’s Cyclopedic Medical Dictionary. 21 st ed. Philadelphia, PA: F. A. Davis Company; 2009.
- Slides: 25