TORCH Toxoplasma Clamydia Rubella Herpes and CMV TORCH

TORCH Toxoplasma, Clamydia, Rubella, Herpes and CMV

TORCH tsets • The five categories of organisms whose antibodies are mea sured by the. TORCH test are grouped together because the y can cause abortion for pregnant woman and/or birth defects in newborns. • Toxoplasmosis. • Others e. g: Chlamydia, syphilis, hepatitis B, coxsackie virus, Epstein. Barr virus, varicella-zoster virus(chickenpox), and humanparvovirus. • Rubella. • Cytomegalovirus(CMV). • Herpes(HSV)

• There are several causes for abortion, some of them are related to viral infection from these viruses: 1. Cytomegalovirus ( CMV). 2. Rubella. 3. Herpes. • Other non-viral causative agents for abortion include: – – Clamydia Toxoplasma gondii (parasite)

TOXOPLASMOSIS • Toxoplasmosis is a zoonotic disease caused by infection with the protozoan Toxoplasma gondii • Toxoplasmosis may cause flu-like symptoms in some people, but most people affected never develop signs and symptoms. • For infants born to infected mothers and for people with weakened immune systems, toxoplasmosis can cause extremely serious complications.

Toxoplasma Gondii • An obligate intracellular parasitic protozoan. • T. gondii is capable o f infecting virtually all warmblooded animals(lack of host specificity). • Cats are the definitive hosts in which the parasite can undergo sexual reproduction. • During infection two forms of parasite may form: – Tackyzoit: Rapidly growing form (acute infection). – Bradyzoit: Slowly growing form in cysts ( chronic infection). • Tissue cysts formed in any organ especially brain, eyes and strained muscles.
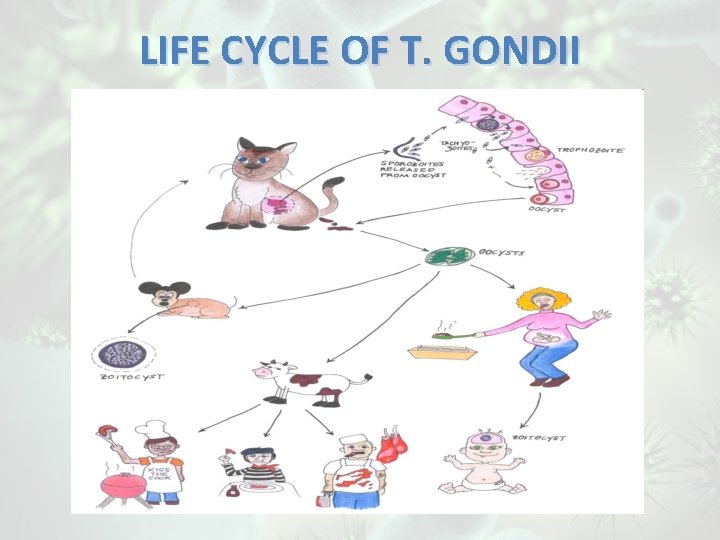
LIFE CYCLE OF T. GONDII

INFECTION • Eating undercooked, contaminated meat. • Eating food that was contaminated by knives, utensils, cutting boards and other foods that have had contact with raw, contaminated meat (cross contamination). • Drinking water contaminated with Toxoplasma gondii.
• Mother-to-child (congenital) transmission. • Accidentally swallowing the parasite through contact with cat feces that contain Toxoplasma. • Receiving an infected organ transplant or infected blood via transfusion, though this is rare.

IS TOXOPLASMOSIS SERIOUS? • Toxoplasmosis is usually nothing to worry about because the immune system is normally strong enough to fight the infection and stop it from causing serious illness. After getting the infection, most people are immune to it for the rest of their life. • However, it can lead to serious problems in: – women who become infected while they're pregnant Toxoplasmosis could cause a miscarriage or stillbirth, or the infection could spread to the baby and cause serious complications (congenital toxoplasmosis) – people with weak immune systems. Such as those who've had an organ transplant, those with HIV and those having chemotherapy this could mean the infection is able to spread to the eyes, heart, lungs or brain

CONGENITAL TOXOPLASMOSIS • Approximately 10 -20% of pregnant women infected with T gondii become symptomatic, The most common signs of infection are lymphadenopathy and fever. • When a mother is infected with T gondii during gestation, the parasite may be disseminated hematogenously to the placenta. When this occurs, infection may be transmitted to the fetus transplacentally.

Infection during pregnancy If infection was shortly before conception (within a few weeks before): – carries a one percent risk or below of transmission to the baby, but there is a risk of miscarriage if the baby does become infected. If infection was in the first trimester (week one to 12) – carries about 10 -15 percent risk of transmission to the baby. A baby infected at this stage has a risk of being miscarried or stillbirth.
If infection was in the second trimester (week 13 to 28): – about 25 percent risk of transmission. A baby infected at this stage is less likely to be miscarried, but is still at risk of developing severe symptoms as: • Hydrocephaly (water on the brain) • Calcifications of the brain • Retinochoroiditis (inflammation of the retina) blindness • Microcephaly. • Neurological disorders.

If infection was in the third trimester (week 29 to 40) – Risk of transmitting the infection rises again if toxoplasmosis is caught at this stage of pregnancy, and may be as high as 70– 80 percent. – Most babies infected will be apparently healthy at birth, but a large proportion will develop symptoms later in life, usually eye damage and Neurological problems.

Retinochoroiditis (ocular toxoplasmosis) • Retinochoroiditis usually results from reactivation of congenital infection, or a part of acute infection. • When the organism reaches the eye through the bloodstream, depending on the host's immune status, a clinical or subclinical focus of infection begins in the retina.
• As the host's immune system responds, the cyst forms which is resistant to the host's immune system, and a chronic, latent infection ensues. • The cyst remains in the normal-appearing retina. • Whenever the host's immune function declines for any reason, the cyst wall rupture, releasing organisms into the retina, and the inflammatory process starts. If an active clinical lesion is present, healing occurs as a retinochoroidal scar.

Diagnosis serologic tests. Ø Amplification of specific nucleic acid sequences (i. e. , polymerase chain reaction [PCR]). ØHistologic demonstration of the parasite and/or its antigens (i. e. , immunoperoxidase stain). ØIsolation of the organism. ØOther rarely used methods include: Ø – Demonstration of antigen in serum and body fluids. – Atoxoplasmin skin test. – Antigen-specific lymphocyte transformation.
• Serologic testing: • Different serological tests often measure different antibodies that possess unique patterns of rise and fall with time after infection. • A combination of serological tests is frequently required to establish whether an individual has been more likely infected in the distant past or has been recently infected.
• Ig. G antibodies: – Ig. G antibodies usually appear within 1– 2 weeks of acquisition of the infection, peak within 1– 2 months, decline at various rates, and usually persist for life. – The most commonly used tests for the measurement of Ig. G antibody are the Sabin-Feldman Dye Test (DT), ELISA, IFA, and the modified direct agglutination test.
• Ig. M antibodies: – Ig. M antibody titres rise from 5 days to weeks following acute infection, reaching a maximum within 21 days and decline more rapidly than Ig. G. – The most commonly used tests for the measurement of Ig. M antibody are ELISA kits, the IFA test, and the immunosorbent agglutination assay (ISAGA).

Note: Ecteric phase is the period when switching b/w Ig. G and Ig. M production ocure results in low levels of both. • Ig. A Antibodies: – Ig. A antibodies may be detected in sera of acutely infected adults and congenitally infected infants using ELISA or ISAGA methods. – It appears in sera when the parasite attacks the eye (toxoplasmic chorioretinitis). – In a number of newborns with congenital toxoplasmosis and negative Ig. M antibodies, the serological diagnosis has been established by the presence of Ig. A and Ig. G antibodies.

• Ig. E Antibodies: – Ig. E antibodies are detectable by ELISA in sera of acutely infected adults, congenitally infected infants. – The duration of Ig. E seropositivity is less than with Ig. M or Ig. A antibodies and hence appears useful as an adjunctive method for identifying recently acquired infections.

• Histologic diagnosis: – Diagnosis also can be made by direct observation of the parasite in stained tissue sections from biopsy. – Immunoflorscence stain and sabin field man stain can be used. – These techniques are used less frequently because of the difficulty of obtaining these specimens. • Isolation: – Parasites can also be isolated from blood or other body fluids by animal inoculation or cell cultures, but this process can be difficult and requires considerable time.

• PCR: – Molecular techniques that can detect the parasite's DNA in the amniotic fluid can be useful in cases of possible mother-to-child (congenital) transmission. – Amniocentesis: • to identify T. gondii in the amniotic fluid by PCR (the most sensitive and specific), done if serologic testing cannot confirm or exclude acute infection, and if there abnormal ultrasound findings suggestive of toxoplasmosis infection. – Fetal blood sampling (cordocentesis): • was previously the gold standard for diagnosing fetal infection but no longer, because of the associated higher fetal risk
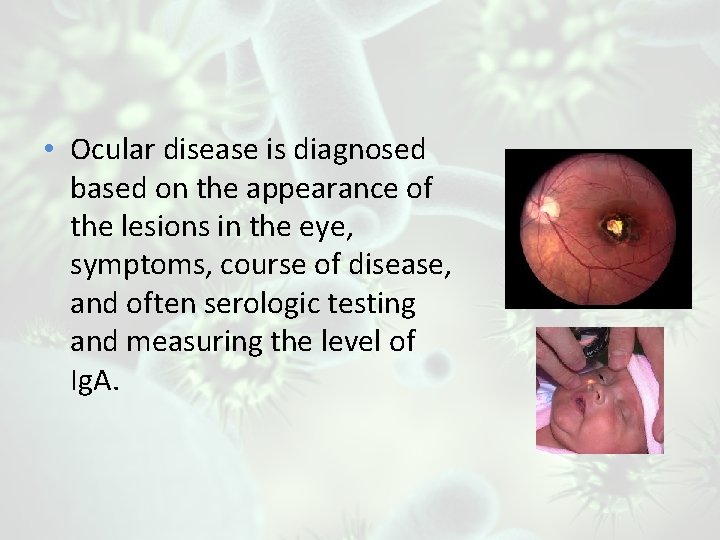
• Ocular disease is diagnosed based on the appearance of the lesions in the eye, symptoms, course of disease, and often serologic testing and measuring the level of Ig. A.

TREATMENT • There are 2 goals of drug therapy for toxoplasmosis, depending on whether or not fetal infection has occurred. – If maternal infection has occurred but the fetus is not infected, spiramycin is used for fetal prophylaxis (to prevent spread of organisms across the placenta from mother to fetus). – If fetal infection has been confirmed or is highly suspected, pyrimethamine and sulfadiazine are used for treatment and decrease in disease severity.

PREVENTION • Do not eat undercooked meat. • Wash hands after handling raw meat. • Keep children's play areas free from cat and dog feces. • Wash your hands thoroughly after touching soil that may be contaminated with animal feces.

Chlamydia • Small obligate intracellular parasite. • Confusion occurred by the discovery of Chlamydia as it was classified as both bacteria and virus. • It is classified as virus for it’s: – Basophilic staining in the host cell to form the elementary body, which are small, dense and about 0. 3 u in diameter. – Intracellular microorganism, they can’t synthesize ATP, but use the host cell for this purpose.

• Causes for classification of chlamydia as bacteria: – They have both DNA and RNA. – Have their self-metabolic system. – They are able to grow and multiply by binary fission. – They are surrounded by a cell membrane. – Response to antibiotic therapy.

Species of chlamydia 1. C. psittsci, cause psittacosis. 2. C. lymphogranulomatis, cause lymphogranuloma venerum ( LGV). 3. C. trachomatis, cause conjuctival and cornea disease (Trachoma) 4. C. occulogenitalis, cause conjunctivitis.

• Psittacosis: – Is a respiratory disease of man acquired from contact with infected birds, which excretes the organism in their stool. – It causes infection in the upper respiratory system and pneumonia. • Laboratory diagnosis: 1. Sputum and blood test. • Smear to show elementary bodies. • ELISA. • PCR
2. isolation: by inoculation of the yolk sack of an embryonated egg or intracerebral, intranasal or intraperitonial injection into a mice. 3. Serological tests: – Complement fixation. – Agglutination test. – Neutralization test.

• Lymphogranuloma venerum: – It is a venereal disease characterized by: • Enlargement of lymph regional lymph nodes, tend to form sinuses. • Infect the urethral parts and cause urethritis and is accompanied by systemic symptoms. – Laboratory diagnosis: • Smears (biopsy from the infected lymph node), pus cells can be seen in infected LN and stain (elementary bodies) • Culture: is not useful as it will give negative result and resist all antibiotics.
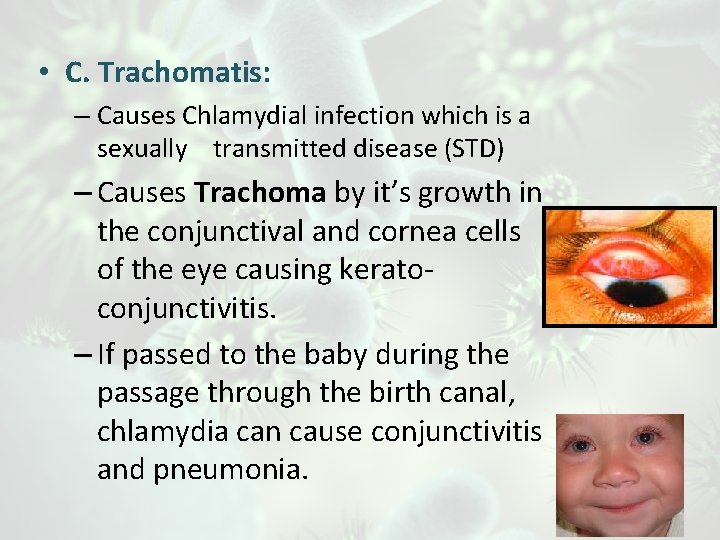
• C. Trachomatis: – Causes Chlamydial infection which is a sexually transmitted disease (STD) – Causes Trachoma by it’s growth in the conjunctival and cornea cells of the eye causing keratoconjunctivitis. – If passed to the baby during the passage through the birth canal, chlamydia can cause conjunctivitis and pneumonia.

– Many women who are infected do not even realize it because they often have no symptoms. However, when untreated, chlamydia can cause a scarring infection of the woman's internal reproductive organs, increasing her risk of a potentially fatal tubal pregnancy. – Laboratory diagnosis: • Smear(eye swab). • ELISA (Ig. M, Ig. G or Ig. A).

Rubella • Rubella is a rather mild disease spread by the way of respiratory secretion, skin contact or congenitally. • Cause German measles, causing the following symptoms: – Firstly, catarrhal symptoms and mild fever. – Irregular rash. • Incubation period is (3 -4) weeks. • The tragic aspect of Rubella may become evident of infection occurs during pregnancy. • MMR vaccine. (Ig. G pesist for life)

symptoms • The virus can cross placental wall and infect the fetus, this may lead to fetal death or congenital defect which may be: – – – – Hearing loss Mental retardation heart disease retarded growth blood disorders vision problems pneumonia
Laboratory Diagnosis • • Complement fixation. Neutralization test. Heme agglutination inhibition (HAI). ELISA Ig. M and Ig. G.

Herpes Human Viruses (HHV) • There are eight types of herpes viruses known to affect humans: • HSV 1 (Herpes Simplex Virus 1 commonly known as oral herpes) • HSV 2 (Herpes Simplex Virus 2 commonly known as genital herpes) • HHV 3 - VZV (Varicella Zoster Virus commonly known as chickenpox or shingles) • HHV 4 - EBV (Ebstein Barr Virus commonly known as infectious mononucleosis [mono or glandular fever])

• HHV 5 - CMV (Cytomegolo Virus is the most common virus transmitted to a pregnant woman's unborn child) • HHV 6 - Roseolovirus more commonly known as the 6 th disease or Roseola Infantum • HHV 7 - Similar to HHV 6 (not yet classified) • HHV 8 - A type of rhadinovirus known as the Kaposi's sarcoma-associated herpesvirus (KSHV)
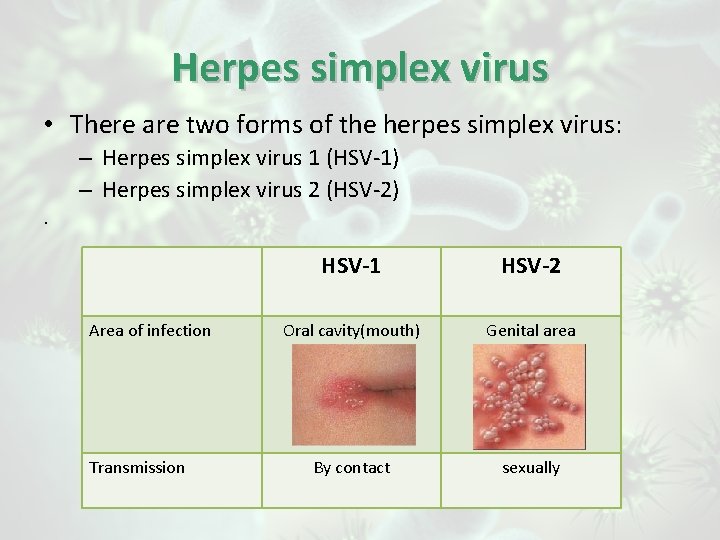
Herpes simplex virus • There are two forms of the herpes simplex virus: – Herpes simplex virus 1 (HSV-1) – Herpes simplex virus 2 (HSV-2). Area of infection Transmission HSV-1 HSV-2 Oral cavity(mouth) Genital area By contact sexually
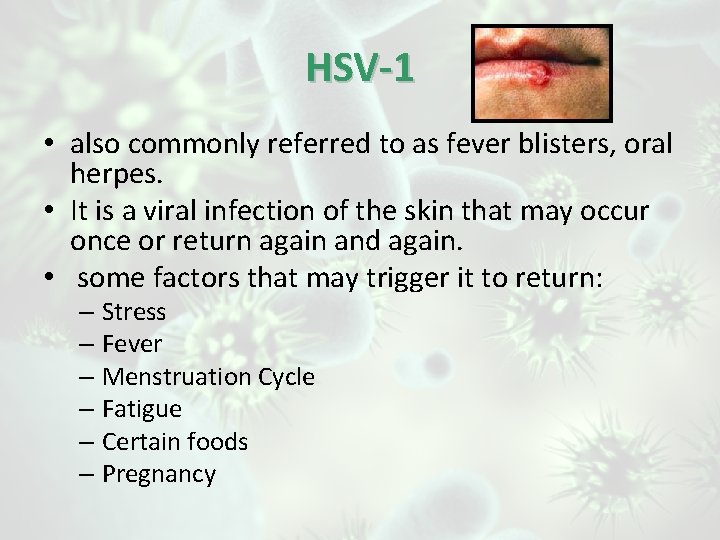
HSV-1 • also commonly referred to as fever blisters, oral herpes. • It is a viral infection of the skin that may occur once or return again and again. • some factors that may trigger it to return: – Stress – Fever – Menstruation Cycle – Fatigue – Certain foods – Pregnancy

HSV-2 • Genital herpes outbreaks are contagious viral infection that affects primarily the genitals of men and women. • It is characterized by recurrent clusters of lesions in the genital areas. • It is sexually transmitted (STD)
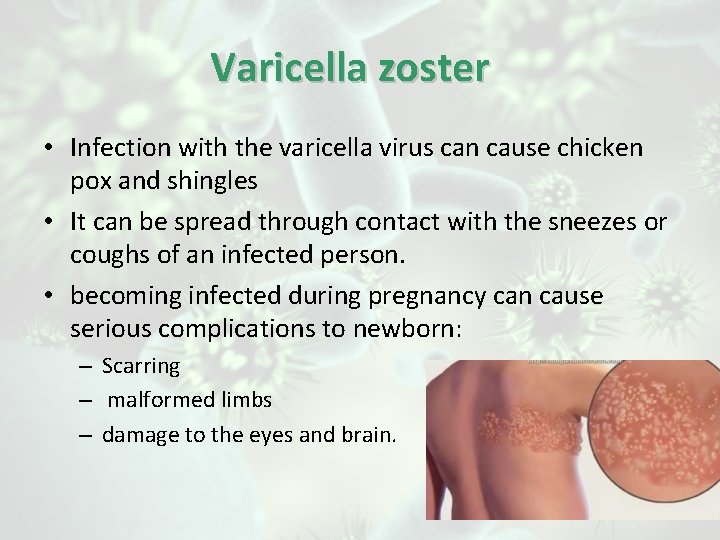
Varicella zoster • Infection with the varicella virus can cause chicken pox and shingles • It can be spread through contact with the sneezes or coughs of an infected person. • becoming infected during pregnancy can cause serious complications to newborn: – Scarring – malformed limbs – damage to the eyes and brain.
Diagnosis of HSV and herpes zoster 1. Viral culture. 2. Tzanck smear. 3. Direct immunofluorescence study with monoclonal antibodies (DFA) 4. PCR 5. Type-specific serologic tests for HSV.

Cytomegalo virus (CMV) • CMV is also called salivary gland virus which may infect salivary glands or parotid gland. • An increase number of infections with the virus have reported in adults with neoplastic disease, leukemia or tissue transplation. • we can isolate this virus from all body fluids.

Symptoms of congenital CMV • 90% of congenital CMV cases are asymptomatic at birth. • 0. 5 – – 15% of these are at risk for psychomotor, hearing, neurologic, ocular, or dental abnormalities within first few years of life. microcephaly, seizures, petechial rash also can be manifeted. • 10% of cases may have sensorineural hearing loss.

Laboratory diagnosis • Histopathological studies, this virus leads to the formation of certain inclusion in the infected cells. • Virus isolation. • ELISA(Ig. M and Ig. G) – Note: when we measure Ig. G, it rarely negative and often positive, so we determine the titer, suppose it is 300 IU/ml, after 2 -3 weeks we make follow up and do the CMV again: • The titer in the same level or less it is negative. • The titer is higher, it is positive.
- Slides: 47