TORCH Infections AHMED BAMAGA MBBS KAUH TORCH Infections

TORCH Infections AHMED BAMAGA MBBS KAUH

TORCH Infections • • • T=toxoplasmosis O=other (syphilis) R=rubella C=cytomegalovirus (CMV) H=herpes simplex (HSV)

• You are taking care of a term newborn male with birth weight/length <10 th %ile. Physical exam is normal except for a slightly enlarged liver span. A CBC is significant for low platelets. • What, if anything, do you worry about? • How do you proceed with a work-up?

Index of Suspicion • When do you think of TORCH infections? • • • IUGR infants HSM Thrombocytopenia Unusual rash Concerning maternal history “Classic” findings of any specific infection

Diagnosing TORCH Infection !!!!!!DO NOT USE TORCH TITERS!!!!!!

Diagnosing TORCH Infection • Good maternal/prenatal history • Remember most infections of concern are mild illnesses often unrecognized • Thorough exam of infant • Directed labs/studies based on most likely diagnosis… • Again, DO NOT USE TORCH TITERS!

Screening TORCH Infections • Retrospective study of 75/182 infants with IUGR who were screened for TORCH infections • 1/75 with clinical findings, 11/75 with abnl lab findings • All patients screened: • TORCH titers, urine CMV culture, head US • Only 3 diagnosed with infection • NONE by TORCH titer!! • Overall cost of all tests = $51, 715 • “Shotgun” screening approach NOT cost effective nor particularly useful • Diagnostic work-up should be logical and directed by history/exam findings Khan, NA, Kazzi, SN. Yield and costs of screening growth-retarded infants for torch

Toxoplasmosis • Caused by protozoan – Toxoplasma gondii • Domestic cat is the definitive host with infections via: • • Ingestion of cysts (meats, garden products) Contact with oocysts in feces • Much higher prevalence of infection in European countries (ie France, Greece) • Acute infection usually asymptomatic • 1/3 risk of fetal infection with primary maternal infection in pregnancy • Infection rate higher with infxn in 3 rd trimester • Fetal death higher with infxn in 1 st trimester

Clinical Manifestations • Most (70 -90%) are asymptomatic at birth • Classic triad of symptoms: • Chorioretinitis • Hydrocephalus • Intracranial calcifications • Other symptoms include fever, rash, HSM, microcephaly, seizures, jaundice, thrombocytopenia, lymphadenopathy • Initially asymptomatic infants are still at high risk of developing abnormalities, especially chorioretinitis
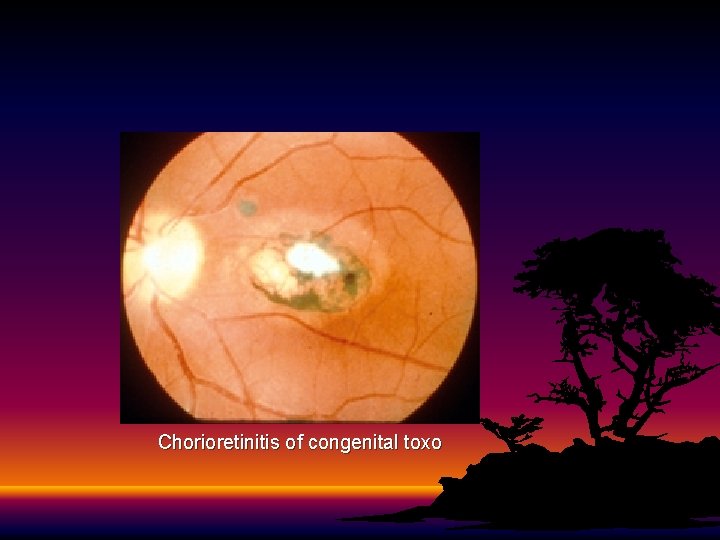
Chorioretinitis of congenital toxo

Diagnosis • Maternal Ig. G testing indicates past infection (but when…? ) • Can be isolated in culture from placenta, umbilical cord, infant serum • PCR testing on WBC, CSF, placenta • Not standardized • Newborn serologies with Ig. M/Ig. A
Toxo Screening • Prenatal testing with varied sensitivity not useful for screening • Neonatal screening with Ig. M testing implemented in some areas • Identifies infected asymptomatic infants who may benefit from therapy

Prevention and Treatment • Treatment for pregnant mothers diagnosed with acute toxo • Spiramycin daily • Macrolide antibiotic • Small studies have shown this reduces likelihood of congenital transmission (up to 50%) • If infant diagnosed prenatally, treat mom • Spiramycin, pyrimethamine (anti-malarial, dihydrofolate reductase inhib), and sulfadiazine (sulfa antibiotic) • Leucovorin rescue with pyrimethamine • Symptomatic infants • Pyrimethamine (with leucovorin rescue) and sulfadiazine • Treatment for 12 months total • Asymptomatic infants • Course of same medications • Improved neurologic and developmental outcomes demonstrated (compared to untreated pts or those treated for only one month)

Syphilis • • • Treponema pallidum (spirochete) Transmitted via sexual contact Placental transmission as early as 6 wks gestation • Typically occurs during second half • Mom with primary or secondary syphilis more likely to transmit than latent disease • Large decrease in congenital syphilis since late 1990 s • In 2002, only 11. 2 cases/100, 000 live births reported
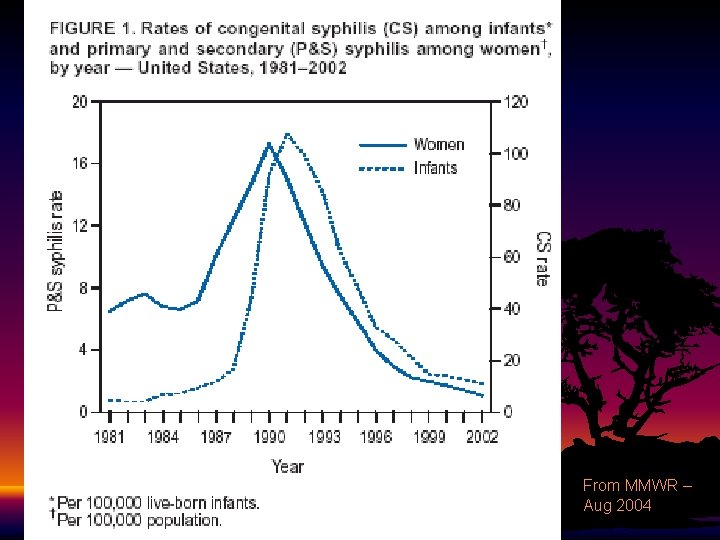
From MMWR – Aug 2004
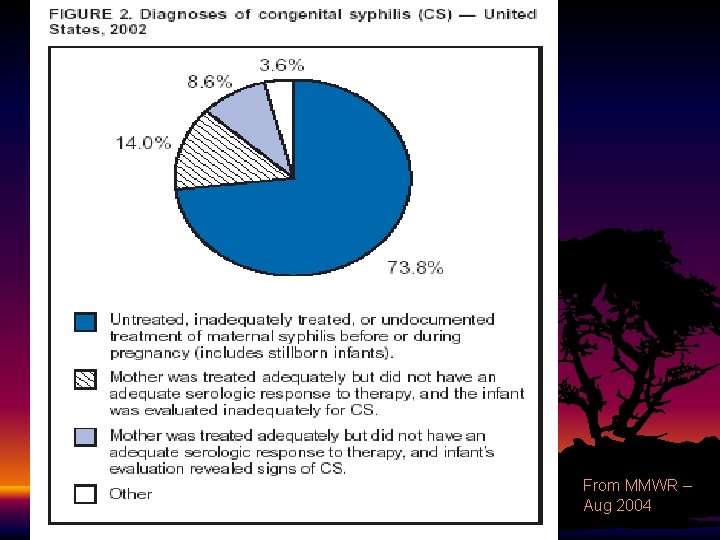
From MMWR – Aug 2004

Congenital Syphilis • 2/3 of affected live-born infants are asymptomatic at birth • Clinical symptoms split into early or late (2 years is cutoff) • 3 major classifications: • • • Fetal effects Early effects Late effects

Clinical Manifestations • Fetal: • • • Stillbirth Neonatal death Hydrops fetalis • Intrauterine death in 25% • Perinatal mortality in 25 -30% if untreated
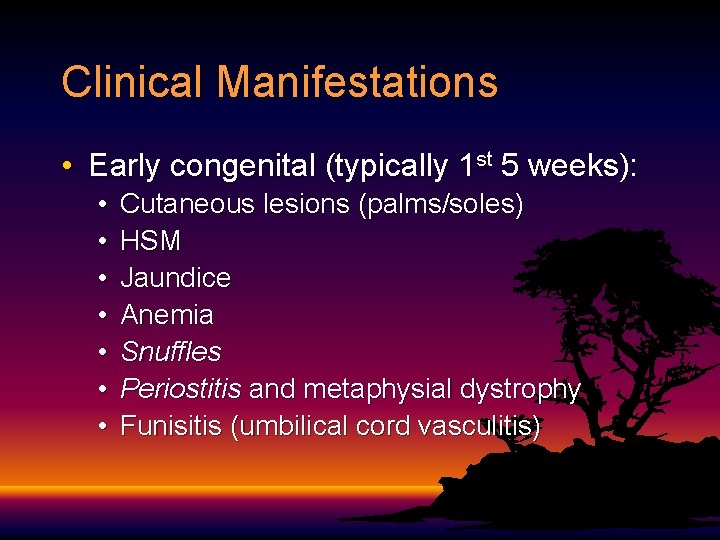
Clinical Manifestations • Early congenital (typically 1 st 5 weeks): • • Cutaneous lesions (palms/soles) HSM Jaundice Anemia Snuffles Periostitis and metaphysial dystrophy Funisitis (umbilical cord vasculitis)
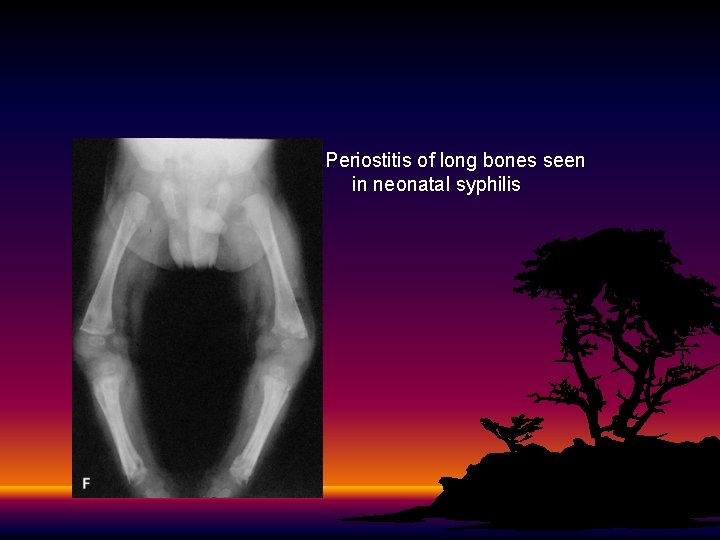
Periostitis of long bones seen in neonatal syphilis

Clinical Manifestations • Late congenital: • • Frontal bossing Short maxilla High palatal arch Hutchinson teeth 8 th nerve deafness Saddle nose Perioral fissures • Can be prevented with appropriate treatment
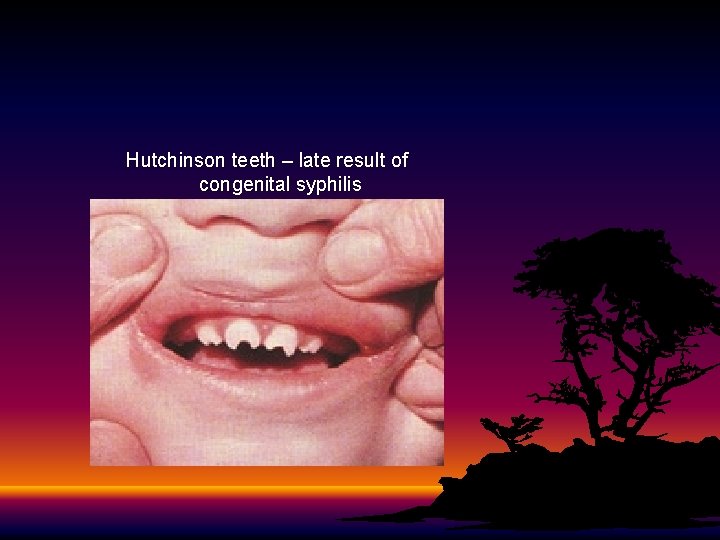
Hutchinson teeth – late result of congenital syphilis

Diagnosing Syphilis (Not in Newborns) • Available serologic testing • RPR/VDRL: nontreponemal test • • Sensitive but NOT specific Quantitative, so can follow to determine disease activity and treatment response • MHA-TP/FTA-ABS: specific treponemal test • • Used for confirmatory testing Qualitative, once positive always positive • RPR/VDRL screen in ALL pregnant women early in pregnancy and at time of birth • This is easily treated!!

CDC Definition of Congenital Syphilis • Confirmed if T. pallidum identified in skin lesions, placenta, umbilical cord, or at autopsy • Presumptive diagnosis if any of: • • • Physical exam findings CSF findings (positive VDRL) Osteitis on long bone x-rays Funisitis (“barber shop pole” umbilical cord) RPR/VDRL >4 times maternal test Positive Ig. M antibody

Diagnosing Congenital Syphilis • Ig. G can represent maternal antibody, not infant infection • This is VERY intricate and often confusing • Consult your Red. Book (or peds ID folks) when faced with this situation

Treatment • Penicillin G is THE drug of choice for ALL syphilis infections • Maternal treatment during pregnancy very effective (overall 98% success) • Treat newborn if: • • They meet CDC diagnostic criteria Mom was treated <4 wks before delivery Mom treated with non-PCN med Maternal titers do not show adequate response (less than 4 -fold decline)

Rubella • Single-stranded RNA virus • Vaccine-preventable disease • No longer considered endemic in the U. S. • Mild, self-limiting illness • Infection earlier in pregnancy has a higher probability of affected infant
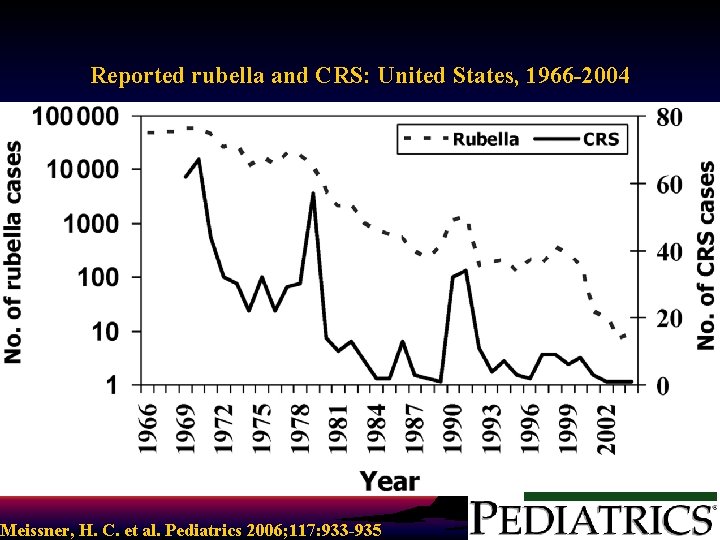
Reported rubella and CRS: United States, 1966 -2004 Meissner, H. C. American et al. Pediatrics Copyright © 2006 Academy of 2006; 117: 933 -935 Pediatrics

Clinical Manifestations • • • Sensorineural hearing loss (50 -75%) Cataracts and glaucoma (20 -50%) Cardiac malformations (20 -50%) Neurologic (10 -20%) Others to include growth retardation, bone disease, HSM, thrombocytopenia, “blueberry muffin” lesions
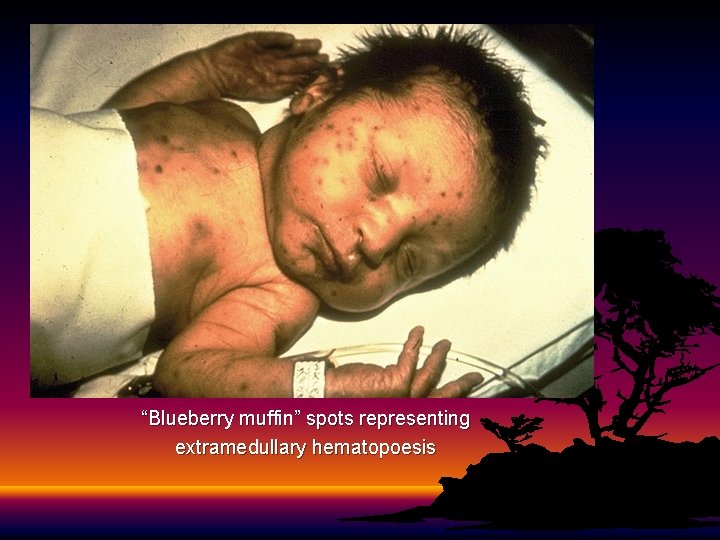
“Blueberry muffin” spots representing extramedullary hematopoesis

Diagnosis • Maternal Ig. G may represent immunization or past infection - Useless! • Can isolate virus from nasal secretions • Less frequently from throat, blood, urine, CSF • Serologic testing • Ig. M = recent postnatal or congenital infection • Rising monthly Ig. G titers suggest congenital infection • Diagnosis after 1 year of age difficult to establish

Treatment • Prevention…immunize, immunize! • Supportive care only with parent education

Cytomegalovirus (CMV) • Most common congenital viral infection • ~40, 000 infants per year in the U. S. • Mild, self limiting illness • Transmission can occur with primary infection or reactivation of virus • 40% risk of transmission in primary infxn • Studies suggest increased risk of transmission later in pregnancy • However, more severe sequalae associated with earlier acquisition

Clinical Manifestations • 90% are asymptomatic at birth! • Up to 15% develop symptoms later, notably sensorineural hearing loss • Symptomatic infection • SGA, HSM, petechiae, jaundice, chorioretinitis, periventricular calcifications, neurological deficits • >80% develop long term complications • Hearing loss, vision impairment, developmental delay
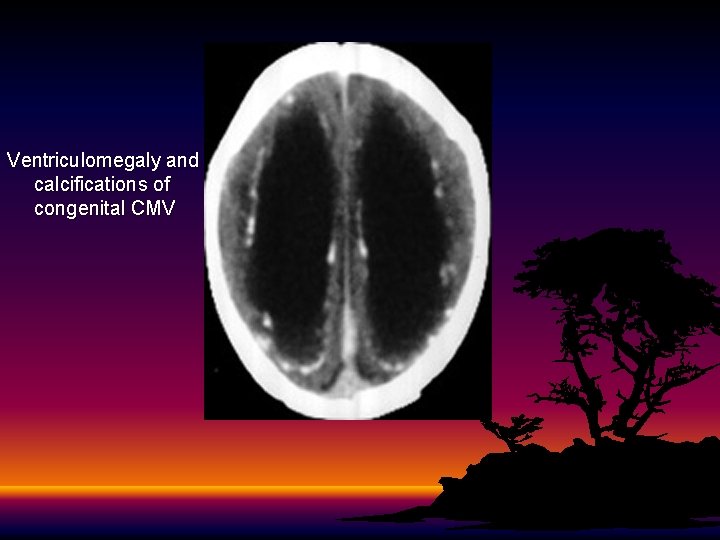
Ventriculomegaly and calcifications of congenital CMV

Diagnosis • Maternal Ig. G shows only past infection • Infection common – this is useless • Viral isolation from urine or saliva in 1 st 3 weeks of life • Afterwards may represent post-natal infection • Viral load and DNA copies can be assessed by PCR • Less useful for diagnosis, but helps in following viral activity in patient • Serologies not helpful given high antibody in population

Treatment • Ganciclovir x 6 wks in symptomatic infants • Studies show improvement or no progression of hearing loss at 6 mos • No other outcomes evaluated (development, etc. ) • Neutropenia often leads to cessation of therapy • Treatment currently not recommended in asymptomatic infants due to side effects • Area of active research to include use of valgancyclovir, treating asx patients, etc.

Herpes Simplex (HSV) • HSV 1 or HSV 2 • Primarily transmitted through infected maternal genital tract • Rationale for C-section delivery prior to membrane rupture • Primary infection with greater transmission risk than reactivation

Clinical Manifestations • Most are asymptomatic at birth • 3 patterns of ~ equal frequency with symptoms between birth and 4 wks: • Skin, eyes, mouth (SEM) • CNS disease • Disseminated disease (present earliest) • Initial manifestations very nonspecific with skin lesions NOT necessarily present
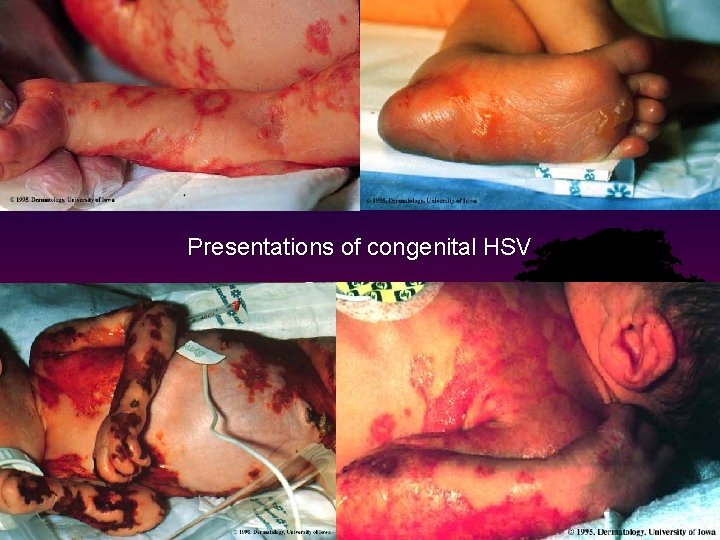
Presentations of congenital HSV

Diagnosis • Culture of maternal lesions if present at delivery • Cultures in infant: • Skin lesions, oro/nasopharynx, eyes, urine, blood, rectum/stool, CSF • CSF PCR • Serologies again not helpful given high prevalence of HSV antibodies in population

Treatment • High dose acyclovir 60 mg/kg/day divided q 8 hrs • X 21 days for disseminated, CNS disease • X 14 days for SEM • Ocular involvement requires topical therapy as well


Which TORCH Infection Presents With… • Snuffles? • syphilis • Chorioretinitis, hydrocephalus, and intracranial calcifications? • toxo • Blueberry muffin lesions? • rubella • Periventricular calcifications? • CMV • No symptoms? • All of them

Which TORCH Infections Can Absolutely Be Prevented? • Rubella • Syphilis

When Are TORCH Titers Helpful in Diagnosing Congenital Infection? • NEVER!

Questions?
- Slides: 47