Topics Background Information Drips Sores Role of STDs


Topics Ø Background Information Ø “Drips” Ø “Sores” Ø Role of STDs in HIV Transmission

Background Information

용어의 변천 Ø Venereal disease (VD), Jean Fernel (1558) – Syphilis, Gonorrhea, Chancroid – Lymphogranuloma venereum, Donovanosis Ø Sexually transmitted disease (STD), WHO (1974) – Nonspecific urethritis, trichomoniasis, genital herpes, genital warts, hepatitis B, and many others Ø Sexually transmitted infection (STI), (2000 -) – Asymptomatic infected people Ø Reproductive tract infection (RTI) – Bacterial vaginosis

성병의 증상 및 무증상 감염 Background 1. “Drips” (discharges) – Gonorrhea – Chlamydia – Nongonococcal urethritis / mucopurulent cervicitis – Trichomonas vaginitis / urethritis – Candidiasis (vulvovaginal, less problems in men)

성병의 증상 및 무증상 감염 Background 2. “Sores” (ulcers) – Syphilis – Genital herpes (HSV-2, HSV-1) – Others uncommon in South Korea Lymphogranuloma venereum Chancroid Granuloma inguinale 3. “Warts” (condyloma) – Genital HPV (Condyloma acuminata) 4. Asymptomatic infection – Chlamydia

“Drips” –Gonorrhea –Nongonococcal urethritis –Chlamydia –Mucopurulent cervicitis –Trichomonas vaginitis and urethritis –Candidiasis

Gonorrhea - 임상양상 Ø Urethritis - male – Incubation: 1 -14 d (usually 2 -5 d) – Sx: Dysuria and urethral discharge (5% asymptomatic) – Dx: Gram stain urethral smear (+) > 98% culture – Complications Ø Urogenital infection - female – Endocervical canal primary site – 70 -90% also colonize urethra – Incubation: unclear; sx usually in l 0 d – Sx: majority asymptomatic; may have vaginal discharge, dysuria, urination, labial pain/swelling, abd. pain – Dx: Gram stain smear (+) 50 -70% culture – Complications Drips
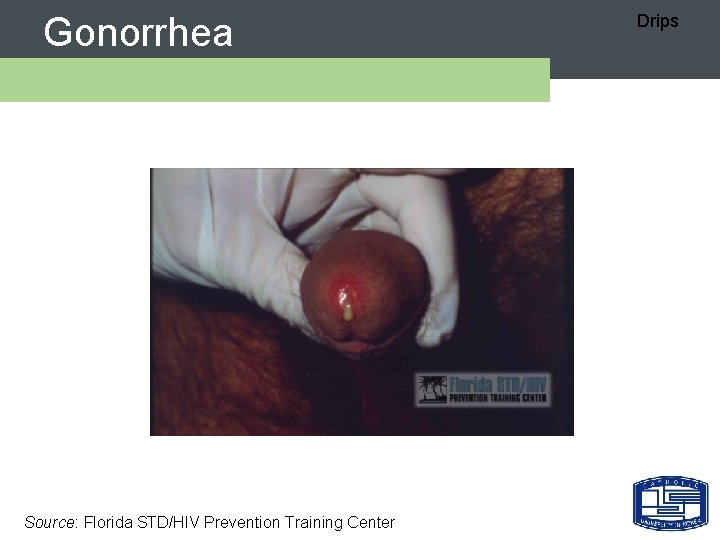
Gonorrhea Source: Florida STD/HIV Prevention Training Center Drips
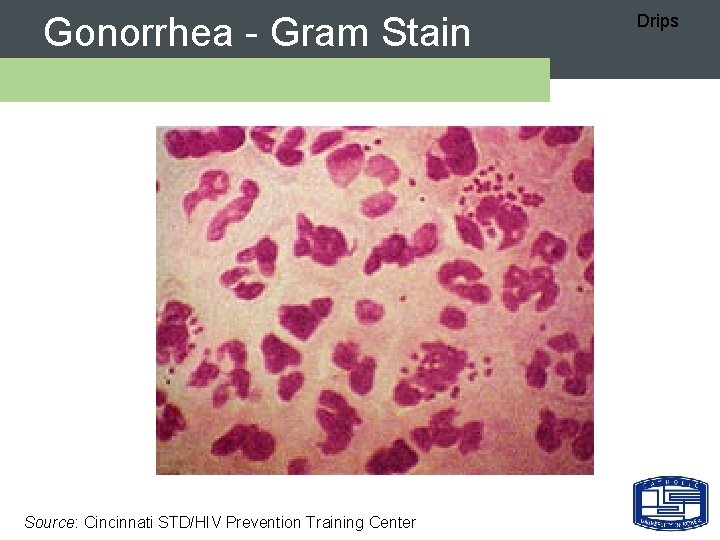
Gonorrhea - Gram Stain Source: Cincinnati STD/HIV Prevention Training Center Drips
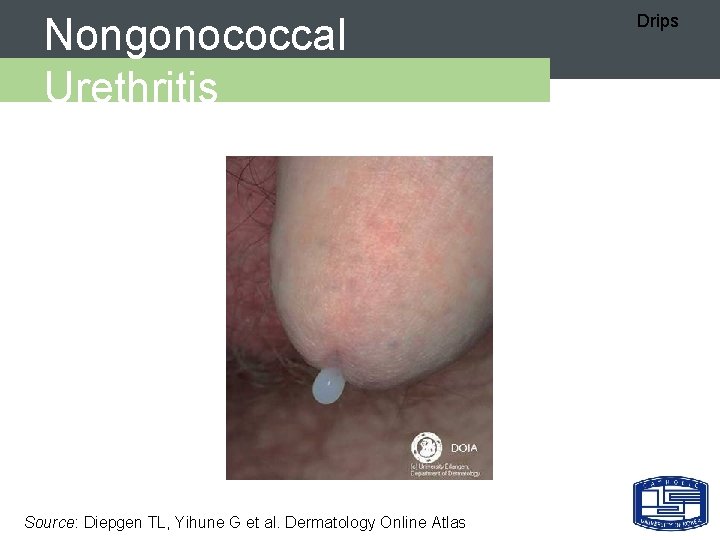
Nongonococcal Urethritis Source: Diepgen TL, Yihune G et al. Dermatology Online Atlas Drips

Nongonococcal Urethritis Drips Ø Etiology: – 20 -40% C. trachomatis – 20 -30% genital mycoplasmas (Ureaplasma urealyticum, Mycoplasma genitalium) – Occasional Trichomonas vaginalis, HSV – Unknown in ~50% cases Ø Sx: Mild dysuria, mucoid discharge Ø Dx: Urethral smear 5 PMNs (usually 15)/OI field Urine microscopic 10 PMNs/HPF Leukocyte esterase (+)

Chlamydia trachomatis Drips Ø More than three million new cases annually Ø Responsible for causing cervicitis, urethritis, proctitis, lymphogranuloma venereum, and pelvic inflammatory disease Ø Direct and indirect cost of chlamydial infections run into billions of dollars Ø Potential to transmit to newborn during delivery – Conjunctivitis, pneumonia

Laboratory Tests for Chlamydia Drips Ø Tissue culture has been the standard – Specificity approaching 100% – Sensitivity ranges from 60% to 90% Ø Non-amplified tests – Enzyme Immunoassay (EIA), e. g. Chlamydiazyme sensitivity and specificity of 85% and 97% respectively useful for high volume screening false positives – Nucleic Acid Hybridization (NA Probe), e. g. Gen-Probe Pace 2 sensitivities ranging from 75% to 100%; specificities greater than 95% detects chlamydial ribosomal RNA able to detect gonorrhea and chlamydia from one swab need for large amounts of sample DNA

Laboratory Tests for Chlamydia (continued) Drips Ø Nucleic Acid Amplification Tests (NAATs) – Polymerase chain reaction (PCR) – Ligase chain reaction (LCR) – Strand displacement amplification (SDA) Ø Sensitivities with PCR and LCR 95% and 8598% respectively; specificity approaches 100% Ø NAATs ability to detect chlamydia in first void urine



Multiplex PCR Ø 남성 요도염 또는 여성 STI 6종 검사 – – – Neisseria gonorrhoeae Chlamydia trachomatis Mycoplasma genitalium Ureaplasma urealyticum Mycoplasma hominis (? ? Pathogen이 아닐 가능성) Trichomonas vaginalis Ø 한 검체로 동시검사하는 장점 Ø 각 원인균이 동일한 중요성을 가지고 있는가?

Multiplex PCR Ø 전립선염 15종 – 요도염 6종 – Escherichia coli – Pseudomonas aeruginosa – Enterococcus faecalis – Proteus spp – Staphylococcus aureus – Klebsiella spp – Strepptpcoccus spp – Enterobacter spp – Veillonella spp Ø 상기 원인균들이 실제 전립선염 원인균으로 작용하고 있는가?




치료 Ø Gonorrhea – Spectinomycin 2 g IM once – Ceftriaxone 250 mg IM once Ø Chlamydia and other NGU – Azithromycin 1 g PO single dose – Doxycyclin 100 mg bid for 7 days Ø Trichomoniasis – Metronidazole 2 g PO single dose – Metronidazole 500 mg bid for 7 days – 술 먹지 마세요!

Recurrent urethritis Ø 원인 – 항생제 내성 – 약을 제대로 먹지 않음 – 파트너 치료 안됨 – Trichomonas vaginalis – HSV urethritis – 다른 문제? : urethral foreign bodies, periurethral fistula, abscess Ø 치료 – Longer duration of treatment – Azithromycin ↔ Doxycycline – Metronidazole 2 g PO once

“Sores” –Syphilis –Genital Herpes (HSV-2, HSV-1)

Genital Ulcer Diseases – Does It Hurt? Ø Painful – Chancroid – Genital herpes simplex Ø Painless – Syphilis – Lymphogranuloma venereum – Granuloma inguinale Sores
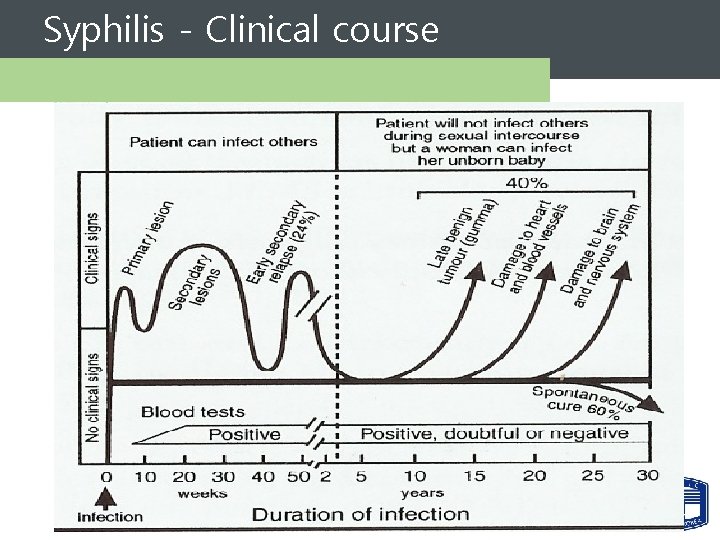
Syphilis - Clinical course

Primary Syphilis - 임상양상 Sores Ø Incubation: 10 -90 days (average 3 weeks) Ø Chancre – Early: macule/papule erodes – Late: clean based, painless, indurated ulcer with smooth firm borders – Unnoticed in 15 -30% of patients – Resolves in 1 -5 weeks – HIGHLY INFECTIOUS
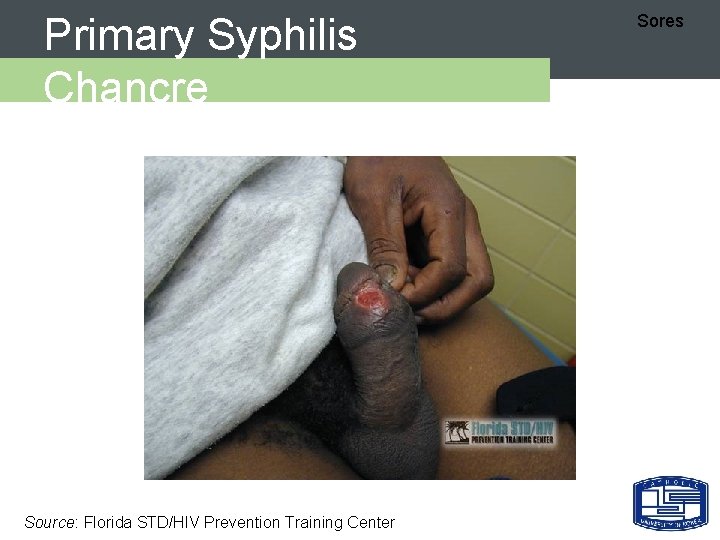
Primary Syphilis Chancre Source: Florida STD/HIV Prevention Training Center Sores

Secondary Syphilis - 임상양상 Sores Ø Represents hematogenous dissemination of spirochetes Ø Usually 2 -8 weeks after chancre appears Ø Findings: – rash - whole body (includes palms/soles) – mucous patches – condylomata lata - HIGHLY INFECTIOUS – constitutional symptoms Ø Sn/Sx resolve in 2 -10 weeks
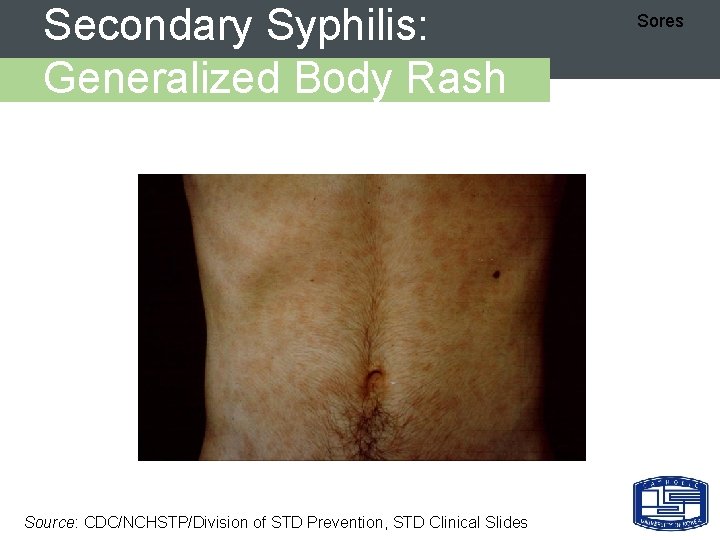
Secondary Syphilis: Generalized Body Rash Source: CDC/NCHSTP/Division of STD Prevention, STD Clinical Slides Sores
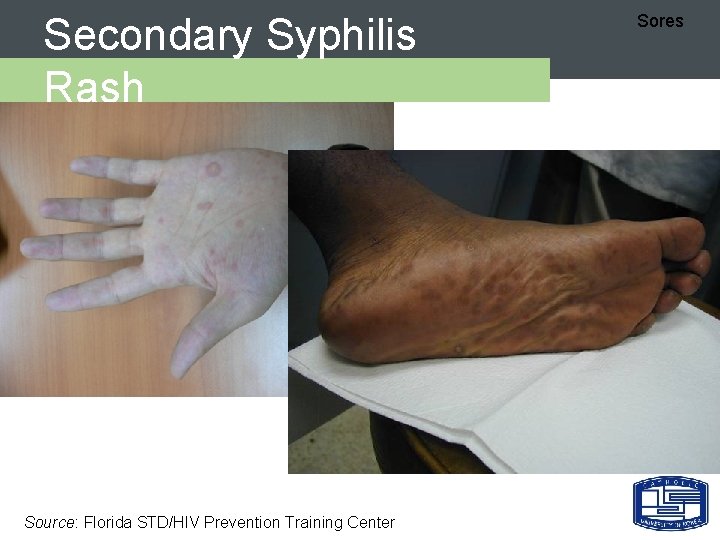
Secondary Syphilis Rash Source: Florida STD/HIV Prevention Training Center Sores
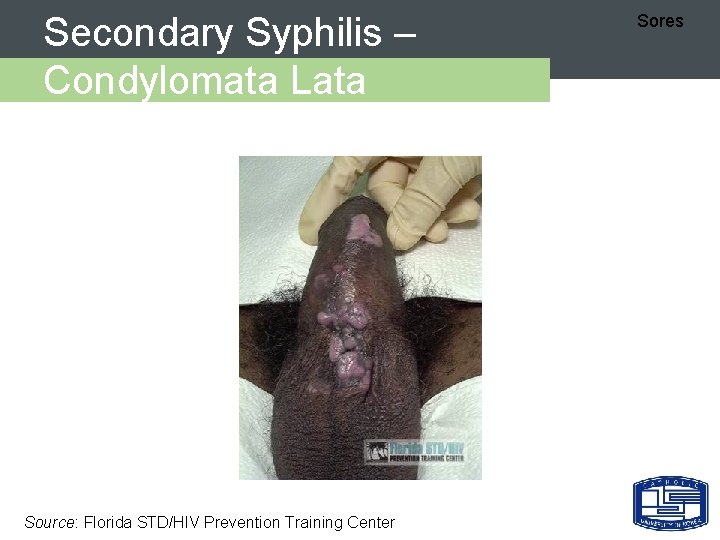
Secondary Syphilis – Condylomata Lata Source: Florida STD/HIV Prevention Training Center Sores

Syphilis - Testing Strategies Ø Routine Screening – – Nontreponemal test + Confirmatory treponemal test – VDRL (or RPR) + TPHA – Best combination Ø Follow-up & Monitoring after treatment – 치료 전 반드시 titer!! (Nontreponemal test titer ) – VDRL titer or RPR titer – 같은 방법으로 F/U (ex. VDRL)
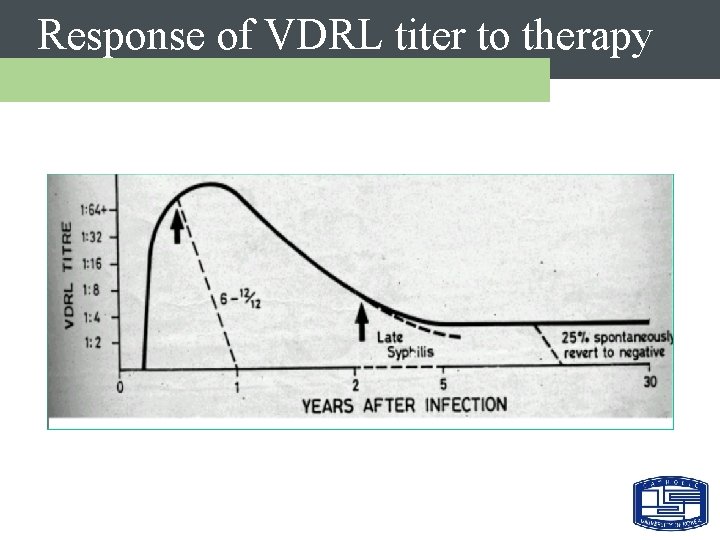
Response of VDRL titer to therapy
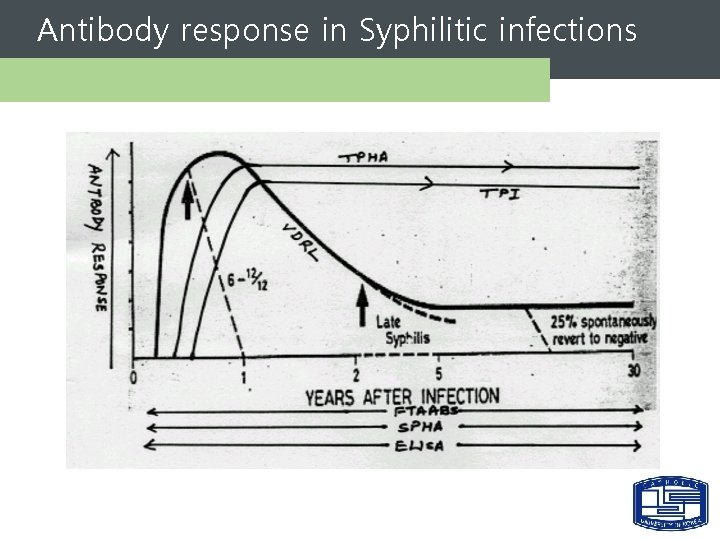
Antibody response in Syphilitic infections

Syphilis - Treatment Ø Benzathine Penicillin G 240만 IU IM (한올제약 마이 신주) – Primary, secondary, early latent : once – Late latent or unknown duration : three doses at 1 -week interval Ø Aqueous crystalline Penicillin G IV (근화제약 페니 실린지칼륨주) – Neurosyphilis Ø Doxycycline PO Ø Tetracycline PO Ø Ceftriaxone IM or IV Ø Azithromycin PO

Syphilis - Follow-up Ø VDRL titer (RPR titer) Ø Every 3 – 6 months Ø Until seronegative or serofast If not, CSF examination Ø Persistent syphilitic lesion or titer not decreasing (4 folds) Retreatment

Persistently positive VDRL Ø Serofast state Ø Treatment failure: more likely with erythromycin or tetracycline Ø Reinfection Ø Biological false-positives

Serofast state Ø Positive VDRL for life Ø Fixed low titer Ø Usually at titers 1: 8 Ø Due to late treatment

Lack of documented adequate treatment Ø Stable low titer VDRL extending back over years Ø Usually do not have active syphilis Ø Consider asymptomatic neurosyphilis Ø Treat for latent syphilis

Random positive VDRL Ø Without any symptoms or prior history of syphilis Ø Patient’s denial of any exposure Ø TPHA & VDRL titer Ø Consider asymptomatic neurosyphilis Ø Treat for latent syphilis


Syphilis - Summary Ø Initial screening: VDRL (or RPR) + TPHA Ø Before treatment: VDRL (or RPR) titer, HIV & other STD tests Ø Treatment according to the guideline Ø Follow-up: VDRL (or RPR) titer Ø If suspicious, but negative, repeat to confirm.
- Slides: 45