Top 5 Post Operative Medical Complications based on

Top 5 Post Operative Medical Complications (based on symptoms and signs) March 2020 Yash Patel General Internal Medicine yash. patel@sinaihealth. ca

Top 5 Symptoms and Signs 1. 2. 3. 4. 5. Chest Pain Dyspnea High Blood Pressure Tachycardia Hyponatremia

Top 5 Symptoms and Signs 1. 2. 3. 4. 5. Chest Pain Dyspnea High Blood Pressure Tachycardia Hyponatremia

1. Chest Pain v. History-characteristics pain/associated symptoms/PMHx CAD v. Physical-VS, focused cardiac/respiratory exam v. Clinical Differential Diagnosis-angina, PE, pneumonia, other v. Investigations-ECG/Tp, CBC, CXT, possible CTpa
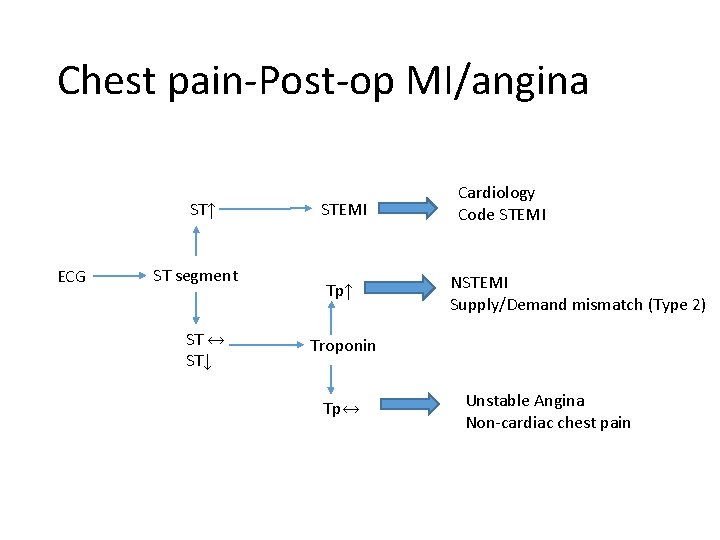
Chest pain-Post-op MI/angina ST↑ ECG ST segment ST ↔ ST↓ STEMI Tp↑ Cardiology Code STEMI NSTEMI Supply/Demand mismatch (Type 2) Troponin Tp↔ Unstable Angina Non-cardiac chest pain

Case 1 v 65 F v. No prior history v. RF: smoker v. Laproscopic cholecystectomy v. Intraop ST 2 mm depression/post op ECG – T-inversions v. No symptoms in PACU v. What next?

Scope of the problem v 500 -900, 000 events worldwide v 15 -25% in hospital mortality v. Survivors have an 18 x (6 -57) chance of death/reinfarction in next 6 months v. Cardiac arrest post op – 65% in hospital mortality v. Increased LOS by 11 days
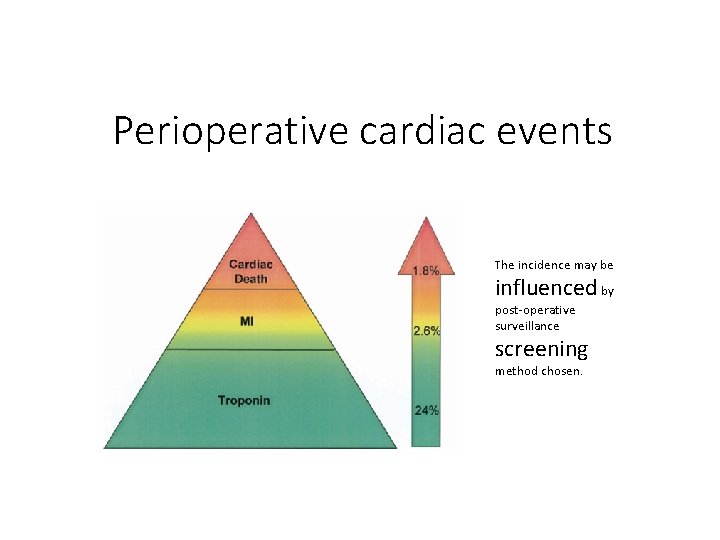
Perioperative cardiac events The incidence may be influenced by post-operative surveillance screening method chosen.
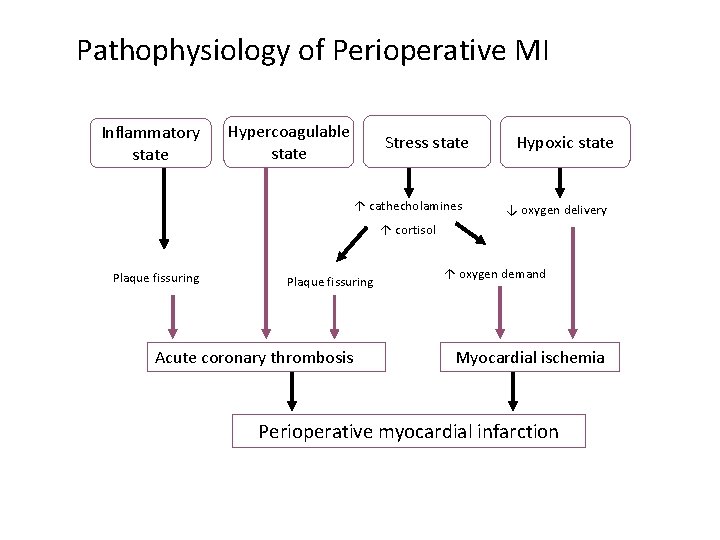
Pathophysiology of Perioperative MI Inflammatory state Hypercoagulable state Stress state ↑ cathecholamines Hypoxic state ↓ oxygen delivery ↑ cortisol Plaque fissuring Acutecoronarythrombosis ↑ oxygen demand Myocardialischemia Perioperative myocardial infarction
Diagnosis – Postop MI v Positive Cardiac Marker: v. Typical rise in troponin, or v. Typical fall of troponin detected at peak after surgery v. No alternative explanation for elevated troponin v Plus one of: v. Ischemic signs or symptoms v. Development of pathological Q waves v. ECG changes indicative of ischemia v. New wall motion abnormality

Presence of symptoms (POISE) v. Chest, epigastric, arm, wrist, jaw discomfort or SOB v. Only 35 -40% patients had typical symptoms v. Pain (lack there of) is affected by anesthesia, analgesia (including epidurals), delirium, altered LOC

ECG changes for diagnosis v. Q-waves > 30 ms in 2 contiguous leads v. ST elevation > 2 mm V 1 -3, > 1 mm elsewhere in 2 contiguous leads v. ST depression > 1 mm in 2 cont. leads v. Symmetric inversion of T waves > 1 mm in 2 leads
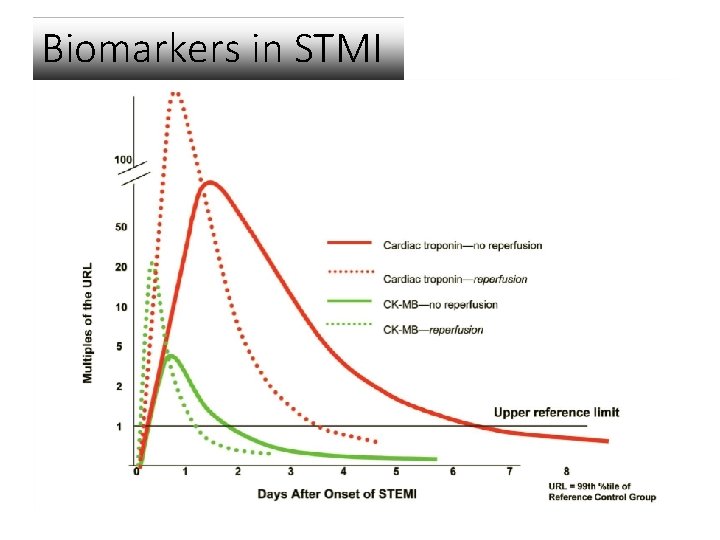
Biomarkers in STMI
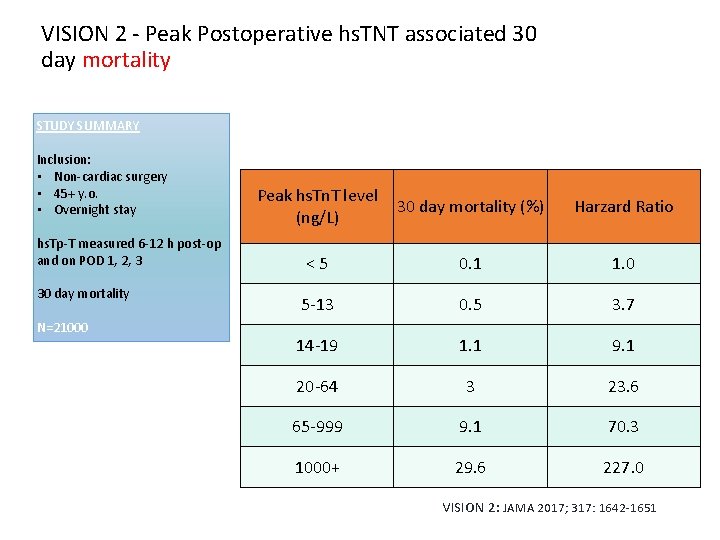
VISION 2 - Peak Postoperative hs. TNT associated 30 day mortality STUDY SUMMARY Inclusion: • Non-cardiac surgery • 45+ y. o. • Overnight stay hs. Tp-T measured 6 -12 h post-op and on POD 1, 2, 3 30 day mortality N=21000 Peak hs. Tn. T level (ng/L) 30 day mortality (%) Harzard Ratio <5 0. 1 1. 0 5 -13 0. 5 3. 7 14 -19 1. 1 9. 1 20 -64 3 23. 6 65 -999 9. 1 70. 3 1000+ 29. 6 227. 0 VISION 2: JAMA 2017; 317: 1642 -1651

Medical Treatment overview v. There is 1 RCT of therapy in perioperative MI v. Treat precipitants (e. g. hypotension, hypoxia, anemia) v. Anti-platelet/anticoagulation therapy has different risk-benefit ratio in the postoperative patient v. Other conventional therapy such as angiography/PCI may not have the same benefits

Antiplatelet & Anticoagulant Drugs v. Aspirin v 160 mg to chew v 80 mg or EC 81 mg daily v. Clopidogrel v 75 mg daily – consider 300 mg loading dose v. ASA+Clopidogrel have high bleeding rates peri-op v. Heparin v. IV v. LMWH

Therapeutic options v. Beta blockers v. ACEI v. Hypotension - especially in hypovolemic patient v. Acute renal failure v + sepsis, + contrast, + NSAIDs v. Nitrates for pain v. Consideration for cath if symptoms persist, ST elevation, shock

Case 1 v 65 F v. No prior history v. RF: smoker v. Laproscopic cholecystectomy v. Intraop ST 2 mm depression/post op ECG – Tinversions v. No symptoms in PACU v. What next?

Case 1 v. ECG normalized over next 2 days v. Troponins –ve x 24 hrs v. ASA, metoprolol given v. Post op ECG abnormalities common v. Often in laproscopic surgeries v. Often in women v. Will need outpatient follow-up/stress

Summary v. Post op MI common v. May be missed because of atypical symptoms v. Interaction of increased demand, hypercoagulability, increased shear forces v. Treat underlying precipitant v. Antiplatelets/anticoagulants have different risk benefit ratio

Chest Pain- pulmonary embolism Case 2 v 55 M POD#5 after Whipple’s for pancreatic cancer v. Dyspneic, diaphoretic, and chest pain in SDU v. ECG – 2 mm ST depressions in leads 2, 3, AVF/Sinus tachycardia v. What next?

Pulmonary Embolism v Frequent post-op pulmonary complication v Risk is dependent on the type of surgery and risk factors v Validated risk assessment tools (Wells-PE or Geneva Score) and algorithms using D-dimer developed for ER/outpatient use
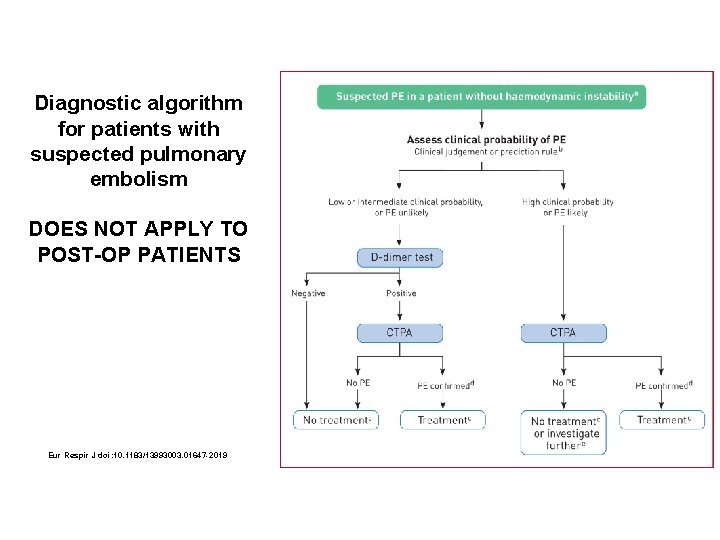
Diagnostic algorithm for patients with suspected pulmonary embolism DOES NOT APPLY TO POST-OP PATIENTS Eur Respir J doi: 10. 1183/13993003. 01647 -2019

Case 2 v 55 M POD#5 after Whipple’s for pancreatic cancer v. Dyspneic, diaphoretic, and chest pain in SDU v. ECG – 2 mm ST depressions in leads 2, 3, AVF v. What next?

Case 2 v. Possible ACS/NSTEMI or PE v. ASA 160 mg v. Beta block v. CTpa v. Start anti-coagulation if delay in obtaining CTpa

Chest Pain-Pulmonary Embolism Practical Approach v. Is there an alternate explanation for the chest pain or dyspnea? v. If NO then test for PE with CTpa v. Is PE the most likely diagnosis? v. If YES then test for PE with CTpa

Treatment of POST-OP Pulmonary Embolism v. What is the Bleeding Risk of FULL anticoagulation? v. HIGH BLEEDING RISK (usu. w/I 24 -48 hrs post-op): Unfractionated IV heparin v. NOT HIGH RISK: LMWH and then transition to DOAC v. DURATION OF THERAPY: “provoked PE” minimum of 3 MONTHS

Top 5 Symptoms and Signs 1. 2. 3. 4. 5. Chest Pain Dyspnea High Blood Pressure Tachycardia Hyponatremia

2. Dyspnea v. History: onset/severity/rest or exertion v. Physical: VS/RR-AMU/O 2 Sat/focused CV/RS exam v. Clinical Differential Diagnosis: HF, PE, pneumonia/effusion, COPD v. Investigations: CBC/lytes, CXR, ECG/Tp, +/-BNP, +/-ABG, +/-CTpa, +/-ECHO

Dyspnea-Heart Failure v. HF is a common condition requiring evaluation in the perioperative period v. HF is a risk factor for other cardiac complications after surgery v. Is the most frequent postop cardiac complication (1 -6 % of patients after major surgery)

Case 1 • 24 M desaturates in the PACU and needs Fi. O 2 0. 8 via FM. BP 205/95. CXR is performed • He just had uneventful lap appendectomy under GA • Anesthetist states that he had some laryngospasm after extubation • He has no PMHx and is quite fit.
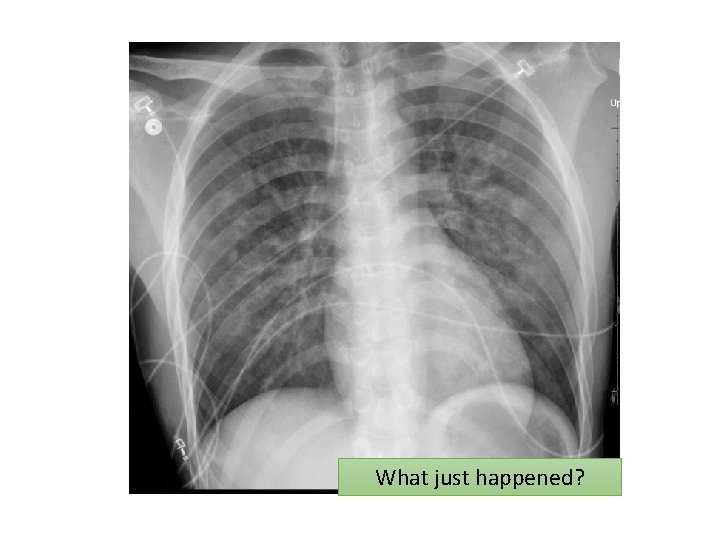
What just happened?

Negative Pressure Pulmonary Edema v. Postop pulmonary edema can have etiologies other than HF v. Pulmonary edema resulting from post-anesthetic laryngospasm v. Spontaneous respiration against obstructed upper airway (any cause) v. Frequently seen in young, healthy, athletic individuals

Negative pressure pulmonary edema (NPPE) v. Patient generates marked negative intrapleural pressure (-50 to -140 cm H 20 (normal -2 to -5) v. Increased venous return to R heart v↓↓ alveolar pressures v↓ output of the L ventricle (↑↑afterload) v. Result: ↑ pulmonary blood volume and microvascular pressure v = net shift into alveoli → pulmonary edema v. May develop up to 25 minutes after extubation CHEST 2016; 150(4): 927 -933

NPPE - Management v. Oxygen v. Relieve airway obstruction (if present) v. Positive pressure ventilation v. Non-invasive (CPAP/Bi. PAP) v. Full ventilation v+/- Sedation (if still intubated/agitated) v+/- Furosemide (IV 40 -80 mg) v. Prognosis v. Fluid resolves in 24 -48 hours (15%/hr) v. No impact on patient mortality if no known underlying cardiac disease v. Low risk of recurrence

Case 2 v 72 M develops SOB and low O 2 saturation on POD#3 after hemi-colectomy for colorectal cancer v. His clinical exam and CXR confirm that he is in HF v. PMHx: HTN, dyslipidemia, and CKD (Cr 150) v. At his preoperative evaluation he was fine with no HF or angina symptoms

Case 2 Questions v. What are the possible etiologies of postoperative HF? v. What evaluation should he undergo right now? v. How should his HF be treated?

Etiology v. Postoperative Heart Failure v. Cardiac Causes v. Ischemia/MI v. Valvular heart disease v. Poor LV function v. Diastolic dysfunction v. Arrhythmia

Etiology v. Postoperative Heart Failure v. Noncardiac Causes v. Large fluid volume/TACO v. Kidney injury v. Negative pressure pulmonary edema v. ARDS/TRALI

Postop Assessment/Management of HF v. Assessment v. Postop SOB can have many different etiologies NOT just HF v. Rule out cardiac ischemia as the cause (ECG/markers) v. Peri-op MI can present in atypical fashion without angina symptoms v. Review the total fluid administration (look at OR record, IV fluids etc)

Post-op heart failure v. Diastolic dysfunction and elevated LVEDP are common in older individuals v. LVEDP further goes up due to: v Excess intravascular fluid (pre-load) v IVF v redistribution of 3 rd spacing v poor ventricular filling – forward failure v Tachycardia v Loss of atrial kick (AF) v. This results in pulmonary edema v. Typically this occurs on day 2 -3 post op

Postop Management and Prognosis of HF v. Management v. ABCs v. Diuretics (e. g. furosemide IV 40 mg) v. Other medications as based on etiology of HF v. CPAP/Bi. Pap or full ventilation v. Prognosis v. Non-ischemic postop HF does not affect long-term outcome

Summary v. HF is common pre and post-op v. Immediate post-op pulmonary edema may be from NPPE v. Rule out ischemia as the cause of post-op HF v. Often related to IVF and redistribution of 3 rd spaced fluids in susceptible patient v. Treat with diuretics/O 2

Top 5 Symptoms and Signs 1. 2. 3. 4. 5. Chest Pain Dyspnea High Blood Pressure Tachycardia Hyponatremia

3. High Blood Pressure v. History v “acute end-organ damage”/HTN urgency (H/A, confusion, vision change, chest-pain, HF, oligouria/AKI) v PMHx-HTN v pain v. Physical v Check BP appropriate size cuff v CV-JVP/edema, neuro-screen, respiratory exam v. Clinical Differential Diagnosis v Primary hypertension vs. reactive acute process (pain, W/D, stress) v. Investigations- CBC, Lytes/Cr, ECG/Tp

Etiology-High Blood Pressure v. Normal response to the physiologic stress of surgery v. Look for acute illness/stressor: pain, infection, withdrawal (meds/ETOH), MI/HF v. Patients with PMHx hypertension have exaggerated BP response to physiologic stress of surgery

Management-High Blood Pressure v. Adequate pain control v. Restart meds if patient taking them preop v. Treat acute process/complication v. Sometimes need to start new medication (CCB, ACEi/ARB, diuretics) v. Most of the time patients DO NOT need any treatment of the elevated blood pressure post-op

Top 5 Symptoms and Signs 1. 2. 3. 4. 5. Chest Pain Dyspnea High Blood Pressure Tachycardia Hyponatremia

4. Tachycardia v. History vpalpitations, chest pain/HF, PMHx-Afib/SVT, Substance use/ETOH, pain v. Physcial- Cardiac/respiratory exam v. Clinical Differential Diagnosis v. Regular rhythm - sinus tach, atrial flutter, or other SVT v. Irregular rhythm - Afib or sinus tach+extrabeats v. Investigations: ECG/Tp, CBC/lytes, Ca, Mg, CXR

Tachycardia- Atrial Fibrillation Case v 45 M v. POD #3 colectomy for active UC v. PMH: nil else v. Sudden onset of palpitations, moderately SOB v. HR 176 irreg, BP 90/40, RR 24 Sat 90% r/a, T 38. 0 C v. CVS/Resp exam WNL v. Abdo distended, surgical site OK v. No leg edema
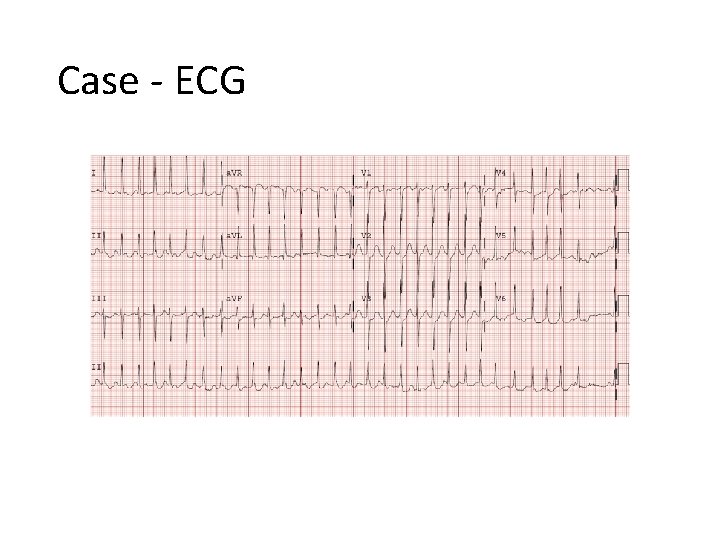
Case - ECG

Epidemiology v. Cardiac surgery v. CABG - 40% v. Valvular 35 -40% v. Combined 60% v. Non-cardiac surgery v 0. 37% - 8% v. General Surgery v. AF/Flut – 5. 4% v. Other SVT 3. 7% Jongnarangsin K, 2008 Newman MF, 2008 Walsh SR, 2007
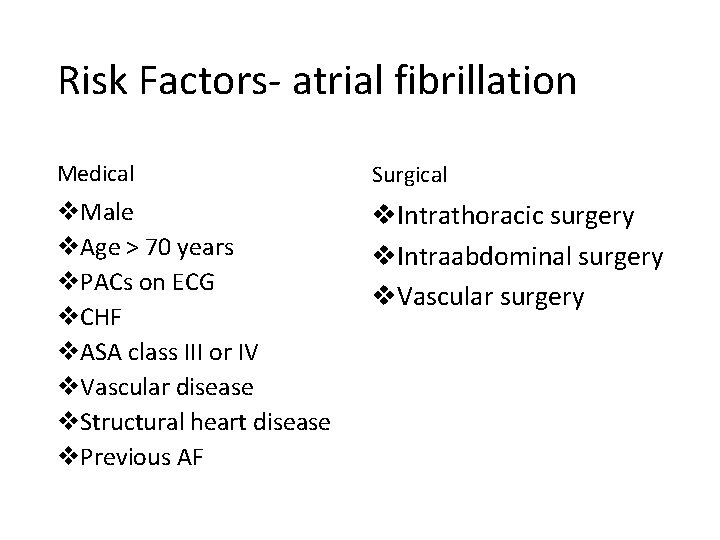
Risk Factors- atrial fibrillation Medical Surgical v. Male v. Age > 70 years v. PACs on ECG v. CHF v. ASA class III or IV v. Vascular disease v. Structural heart disease v. Previous AF v. Intrathoracic surgery v. Intraabdominal surgery v. Vascular surgery

Post-op factors v. Catecholamines v. Pain v. Anxiety v. Electrolyte imbalances v. Myocardial ischemia v. Volume overload (atrial stretch) v. Pulmonary embolism v. Infection v. Drug withdrawal v. Thyroid overactivity

Drug withdrawal v. Beta blockers v. Benzodiazepines v. Narcotics v. Alcohol

Evaluation- Atrial Fibrillation v. ECG v. Labs – K, Mg, Cr, TSH, CK, Tp v. CXR (CHF/Pneumonia) vurinalysis/blood cultures, if febrile v. Echo if suspect structural heart disease v? PE investigations

Management-Atrial Fibrillation v. Rate Control v. BP management v. Rhythm v. Anticoagulation

Rate control v Mainstay of therapy v Beta blockers v Metoprolol IV 5 mg every 5 mins x 3 v Oral for maintenance 12. 5 to 100 mg bid/tid v Diltiazem v 10 -20 mg iv bolus v Infusion 5 -15 mg/hr v Oral for rate maintenance 30 -90 mg q 6 h v Digoxin v 0. 25 mg IV every 4 -6 hrs up to 1 mg v Oral for maintenance 0. 0625 – 0. 25 mg daily v Amio – may be used for rate control Hollenberg, S, 2000

Low BP management v. Hypovolemia may drive up rate of AF v. Fluids are mainstay of BP support v. Unless in frank pulmonary edema v. Electrical cardioversion is rarely necessary v. Chemical cardioversion takes time and BP needs to be supported before v. AVOID giving dopamine, epi, nor-epi v. Phenylephrine may be used vno heart rate impact

Rhythm control v. Electrical cardioversion v. Hemodynamic instability refractory to fluids v. Severe pulmonary edema v. Ongoing cardiac ischemia

Rhythm control v> 50% of new onset post-op AF will revert spontaneously v. Even more (80%) with rate control and addressing the precipitant v. Amiodarone v 150 mg IV bolus over 10 mins v 1 mg/min x 6 hrs, then 0. 5 mg/min v. S/E Hypotension, bradycardia Walsh, SR, 2007 Hollenberg, S, 2000

Anticoagulation v. Risk of stroke is relatively small if AF transient v. Consider anticoagulation if in persistent AF after 48 hrs v. Balance stroke/embolism with risk of bleeding v. No good evidence of which agent to chose. Use based on risk of bleeding: IV UFH, LMWH, warfarin, DOAC
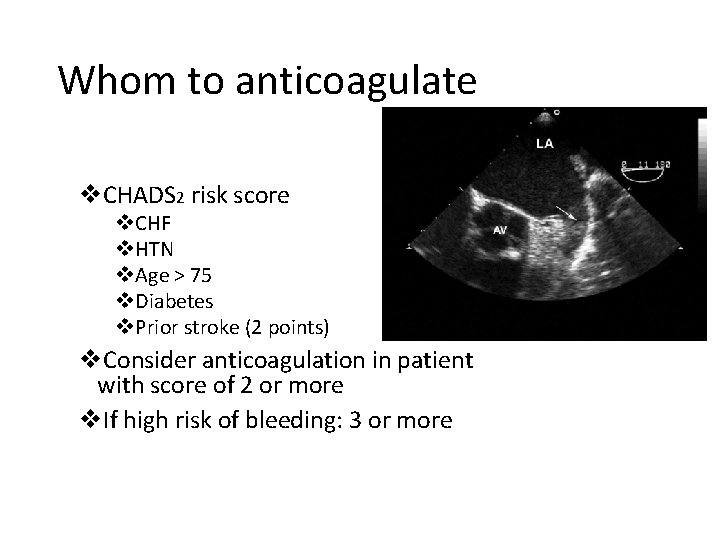
Whom to anticoagulate v. CHADS 2 risk score v. CHF v. HTN v. Age > 75 v. Diabetes v. Prior stroke (2 points) v. Consider anticoagulation in patient with score of 2 or more v. If high risk of bleeding: 3 or more

Top 5 Symptoms and Signs 1. 2. 3. 4. 5. Chest Pain Dyspnea High Blood Pressure Tachycardia Hyponatremia

5. Hyponatremia (hypo-osmolar) v. History v Pre-op Na, Trend postop Na, Acute or Chronic, Na<120 v Symptoms of severe hypo. Na (CNS changes, N/V, confusion, H/A v Review fluid management intra/postop, fluid in/output, insensible losses v. Physical v Volume Status Assessment (JVP/edema, postural BP/HR change) v. Investigations v Serum Osmo v Urine: Na, Osmo, Cr v TSH, +/- Cortisol v +/- CXR
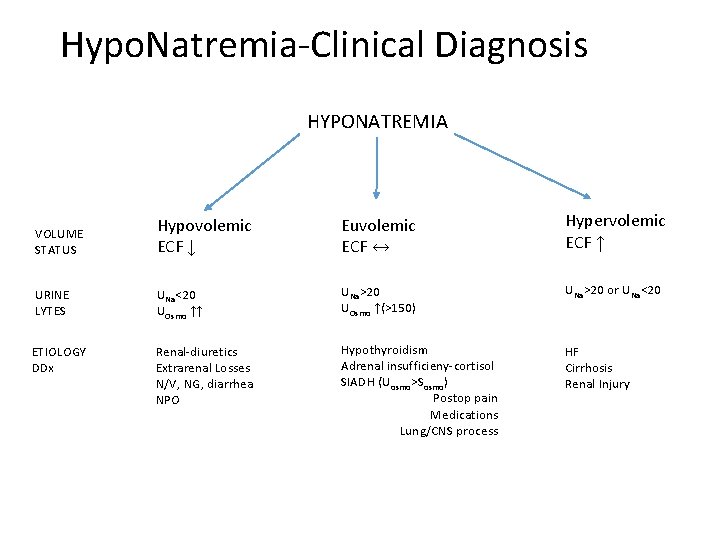
Hypo. Natremia-Clinical Diagnosis HYPONATREMIA VOLUME STATUS Hypovolemic ECF ↓ Euvolemic ECF ↔ Hypervolemic ECF ↑ URINE LYTES UNa<20 UOsmo ↑↑ UNa>20 UOsmo ↑(>150) UNa>20 or UNa<20 ETIOLOGY DDx Renal-diuretics Extrarenal Losses N/V, NG, diarrhea NPO Hypothyroidism Adrenal insufficieny-cortisol SIADH (Uosmo>Sosmo) Postop pain Medications Lung/CNS process HF Cirrhosis Renal Injury
![Hypo. Natremia-Treatment (correct [Na]<8 mmol/day) HYPONATREMIA VOLUME STATUS TREATEMENT Hypovolemic ECF ↓ Euvolemic ECF Hypo. Natremia-Treatment (correct [Na]<8 mmol/day) HYPONATREMIA VOLUME STATUS TREATEMENT Hypovolemic ECF ↓ Euvolemic ECF](http://slidetodoc.com/presentation_image_h2/c2caa6bdd9137b7c4f80ee5e419bf30c/image-67.jpg)
Hypo. Natremia-Treatment (correct [Na]<8 mmol/day) HYPONATREMIA VOLUME STATUS TREATEMENT Hypovolemic ECF ↓ Euvolemic ECF ↔ Hypervolemic ECF ↑ Correct fluid losses RL/NS 1. Fluid restriction 1000 -1500 cc/d 2. Solute induced obligate water loss (salt tabs 1000 mg/BID) Diuretics Salt restriction Fluid restriction
Summary: Top 5 Symptoms and Signs of Post-op Medical Complications 1. 2. 3. 4. 5. Chest Pain – Periop MI/PE Dyspnea - HF High Blood Pressure Tachycardia – Periop Afib Hyponatremia
- Slides: 68