Tocilizumab Robert A Montgomery M D D Phil

Tocilizumab Robert A. Montgomery, M. D. , D. Phil. Professor of Surgery Director of the NYU Langone Transplant Institute

Scope of the Problem • Sensitization to HLA molecules limits access to transplantation for about 30, 000 patients on the kidney waiting list • The post-transplant presence of DSA is perhaps the most significant contributor to premature graft loss • Acute AMR further accelerates the rate and speed of graft loss • Strategies to prevent or treat chronic microcirculation injury and transplant glomerulopathy from DSA remains an important unmet need

Need for Efficacious Therapies • Standard of care therapy (plasmapheresis and IVIg) can effectively ameliorate antibody mediated injury especially when the AMR is early and associated with acute renal dysfunction • Many drugs with autoimmune and oncologic indications have been repurposed to treat or prevent AMR because of attractive mechanisms of action • These add-on therapies may enhance the efficacy of SOC treatments and the search for more effective therapeutic agents continues

Therapies and Intervention For HLA DSA The Tackle Box Standard of Care (SOC) Add-ons to SOC • Plasmapheresis • Anti-CD 20 • Immunoabsorption • Complement Inhibitors (eculizumab and C 1 INH) • IVIg (high or low dose) • Steroids, ATG, Bela • [Rituximab] • Splenectomy • Proteosomal Inhibitors • Anti-BAFF/BLy. S • Ide. S • Anti-IL-6 R
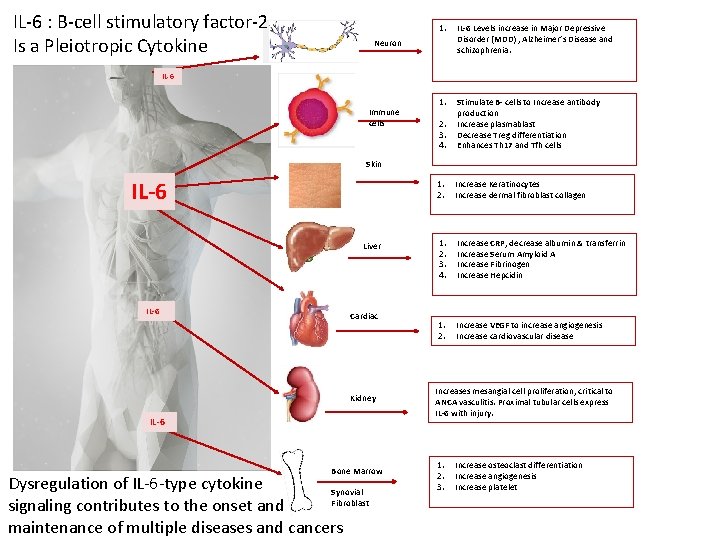
IL-6 : B-cell stimulatory factor-2 Is a Pleiotropic Cytokine 1. IL-6 Levels increase in Major Depressive Disorder (MDD) , Alzheimer’s Disease and schizophrenia. 1. 2. 3. 4. Stimulate B- cells to Increase antibody production Increase plasmablast Decrease Treg differentiation Enhances Th 17 and Tfh cells 1. 2. Increase Keratinocytes Increase dermal fibroblast collagen 1. 2. 3. 4. Increase CRP, decrease albumin & transferrin Increase Serum Amyloid A Increase Fibrinogen Increase Hepcidin 1. 2. Increase VEGF to increase angiogenesis Increase cardiovascular disease Neuron IL-6 Immune cells Skin IL-6 Liver IL-6 Cardiac Kidney IL-6 Bone Marrow Dysregulation of IL-6 -type cytokine Synovial Fibroblast signaling contributes to the onset and maintenance of multiple diseases and cancers Increases mesangial cell proliferation, critical to ANCA vasculitis. Proximal tubular cells express IL-6 with injury. 1. 2. 3. Increase osteoclast differentiation Increase angiogenesis Increase platelet

Tocilizumab • Humanized monoclonal antibody against the Interleukin-6 receptor (IL-6 R) • Its delivered by monthly infusion or subcutaneous injection • Used for rheumatoid arthritis, systemic juvenile arthritis, and Castleman’s disease. In Phase II/III trials for GVHD. • Very limited experience in solid organ transplantation • For naïve B-cells, IL-6 promotes activation and differentiation into plasmablasts and plasma cells • IL-6 may also be important for the maintenance of: • survival milieu in the long-lived plasma cell niche • Germinal center and Tfh/B-cell interactions
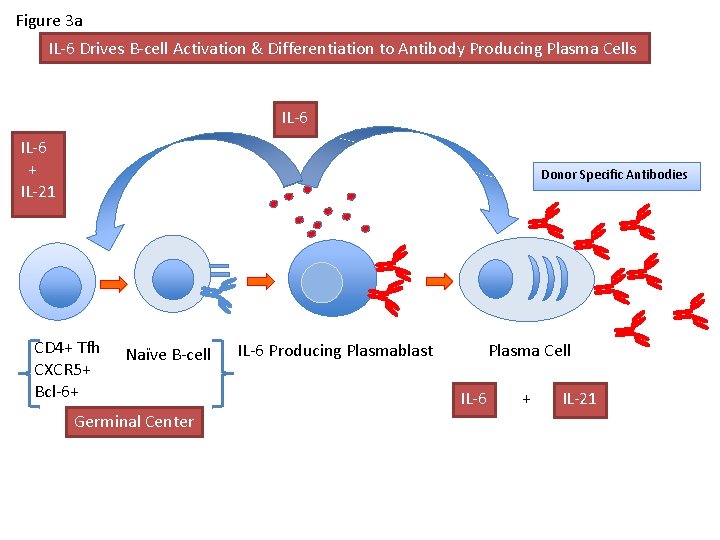
Figure 3 a IL-6 Drives B-cell Activation & Differentiation to Antibody Producing Plasma Cells IL-6 + IL-21 Donor Specific Antibodies CD 4+ Tfh CXCR 5+ Bcl-6+ Naïve B-cell Germinal Center IL-6 Producing Plasmablast Plasma Cell IL-6 + IL-21
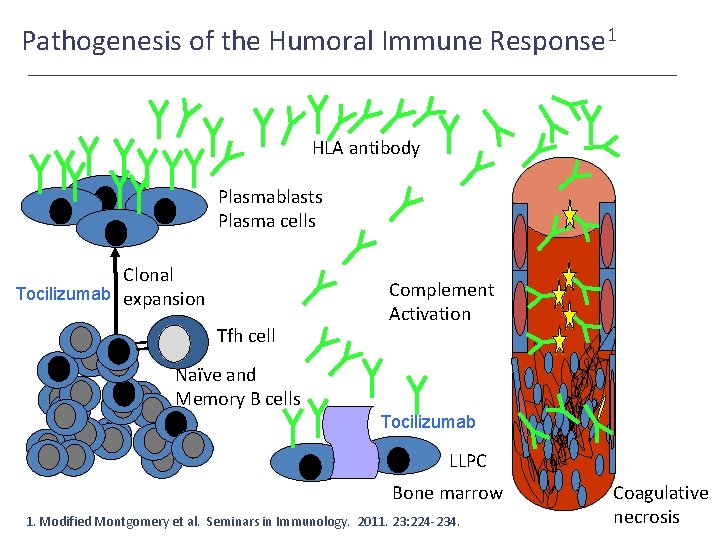
Pathogenesis of the Humoral Immune Response 1 HLA antibody Plasmablasts Plasma cells Clonal Tocilizumab expansion Tfh cell Complement Activation Naïve and Memory B cells Tocilizumab LLPC Bone marrow 1. Modified Montgomery et al. Seminars in Immunology. 2011. 23: 224 -234. Coagulative necrosis
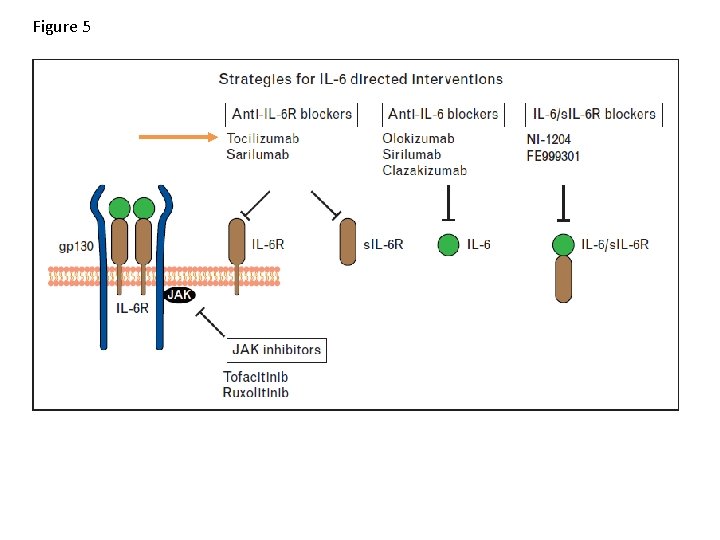
Figure 5
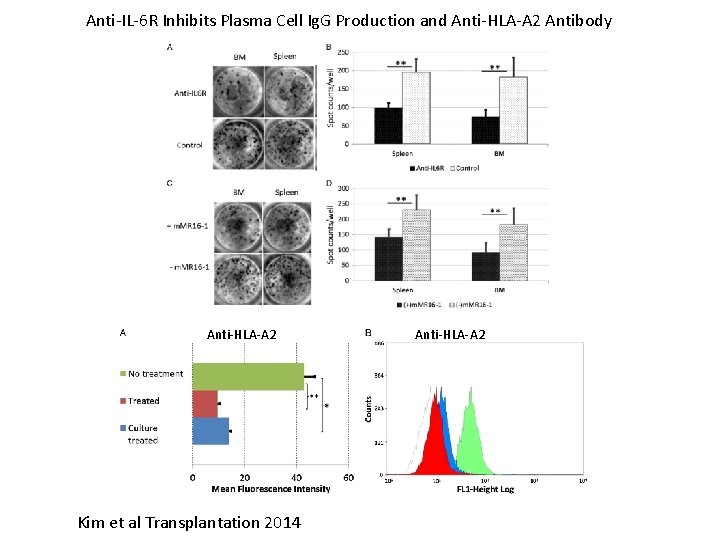
Anti-IL-6 R Inhibits Plasma Cell Ig. G Production and Anti-HLA-A 2 Antibody Anti-HLA-A 2 Kim et al Transplantation 2014 Anti-HLA-A 2

Vo et al. Transplantation. 2015; 99: 2356.
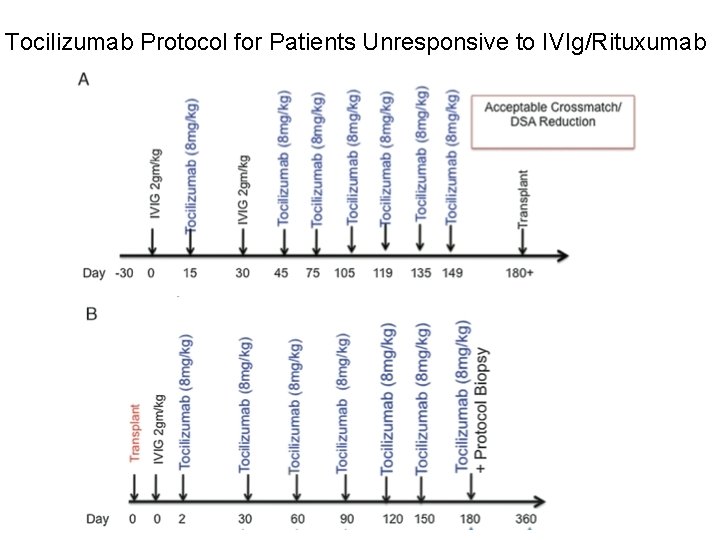
Tocilizumab Protocol for Patients Unresponsive to IVIg/Rituxumab
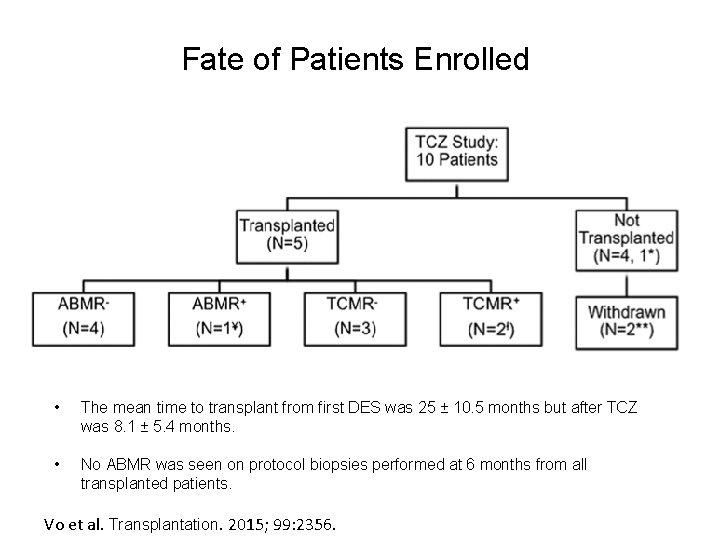
Fate of Patients Enrolled • The mean time to transplant from first DES was 25 ± 10. 5 months but after TCZ was 8. 1 ± 5. 4 months. • No ABMR was seen on protocol biopsies performed at 6 months from all transplanted patients. Vo et al. Transplantation. 2015; 99: 2356.
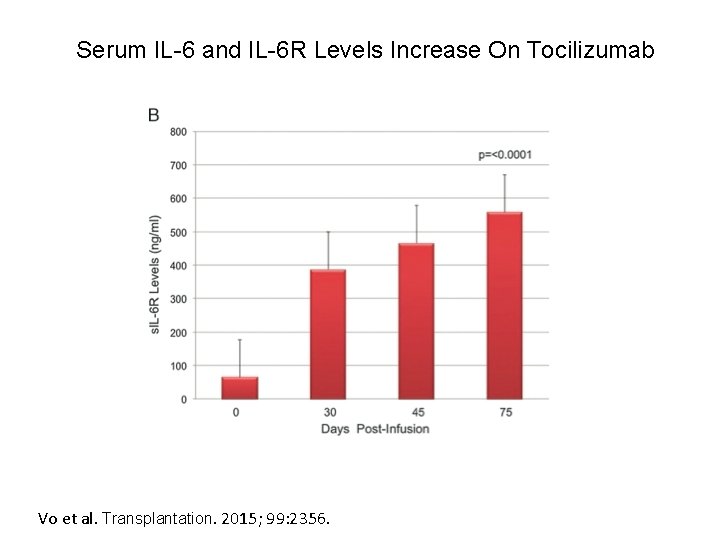
Serum IL-6 and IL-6 R Levels Increase On Tocilizumab Vo et al. Transplantation. 2015; 99: 2356.
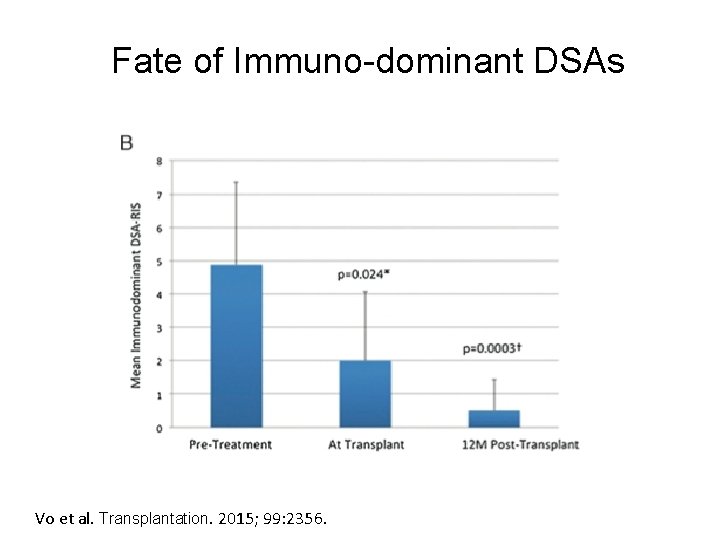
Fate of Immuno-dominant DSAs Vo et al. Transplantation. 2015; 99: 2356.
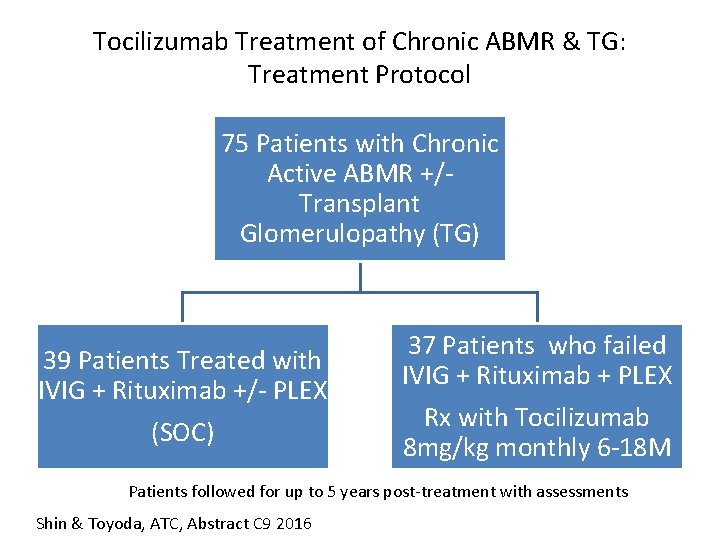
Tocilizumab Treatment of Chronic ABMR & TG: Treatment Protocol 75 Patients with Chronic Active ABMR +/Transplant Glomerulopathy (TG) 39 Patients Treated with IVIG + Rituximab +/- PLEX (SOC) 37 Patients who failed IVIG + Rituximab + PLEX Rx with Tocilizumab 8 mg/kg monthly 6 -18 M Patients followed for up to 5 years post-treatment with assessments Shin & Toyoda, ATC, Abstract C 9 2016
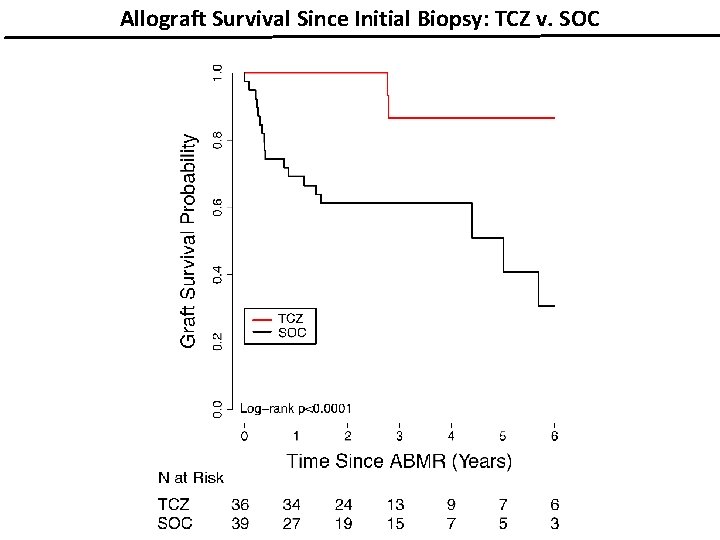
Allograft Survival Since Initial Biopsy: TCZ v. SOC
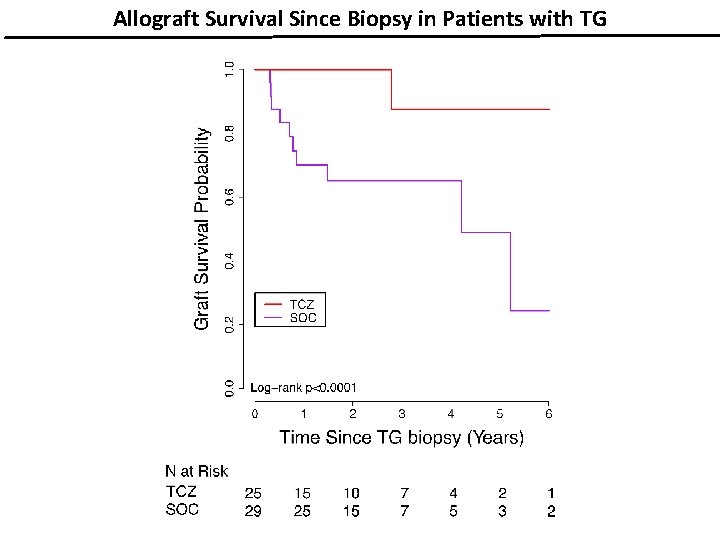
Allograft Survival Since Biopsy in Patients with TG
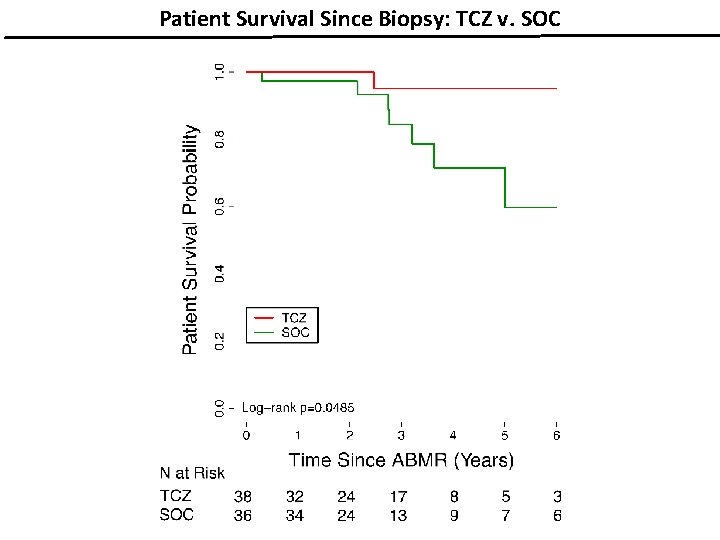
Patient Survival Since Biopsy: TCZ v. SOC
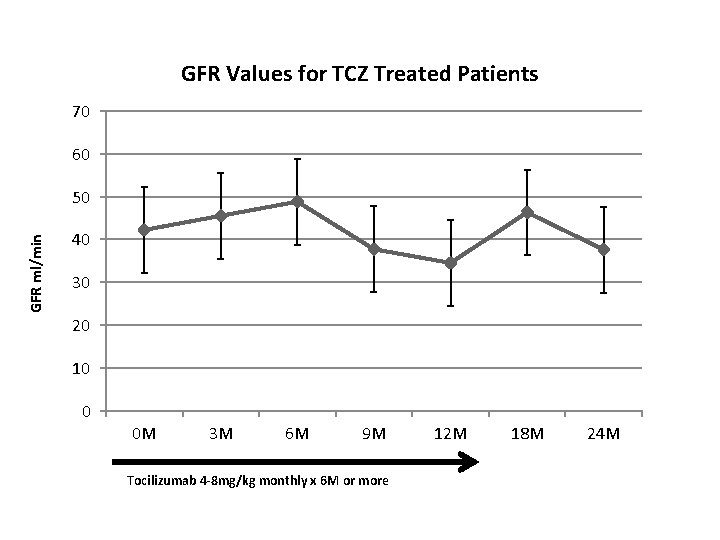
GFR Values for TCZ Treated Patients 70 60 GFR ml/min 50 40 30 20 10 0 0 M 3 M 6 M 9 M Tocilizumab 4 -8 mg/kg monthly x 6 M or more 12 M 18 M 24 M
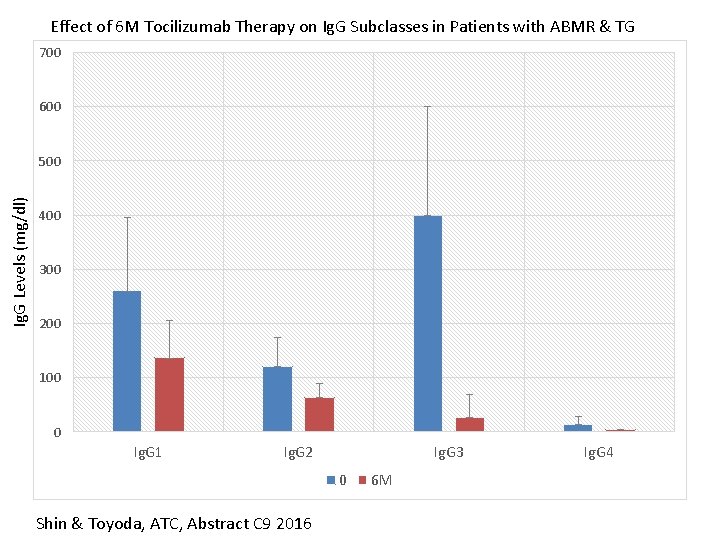
Effect of 6 M Tocilizumab Therapy on Ig. G Subclasses in Patients with ABMR & TG 700 600 Ig. G Levels (mg/dl) 500 400 300 200 100 0 Ig. G 1 Ig. G 2 Ig. G 3 0 Shin & Toyoda, ATC, Abstract C 9 2016 6 M Ig. G 4
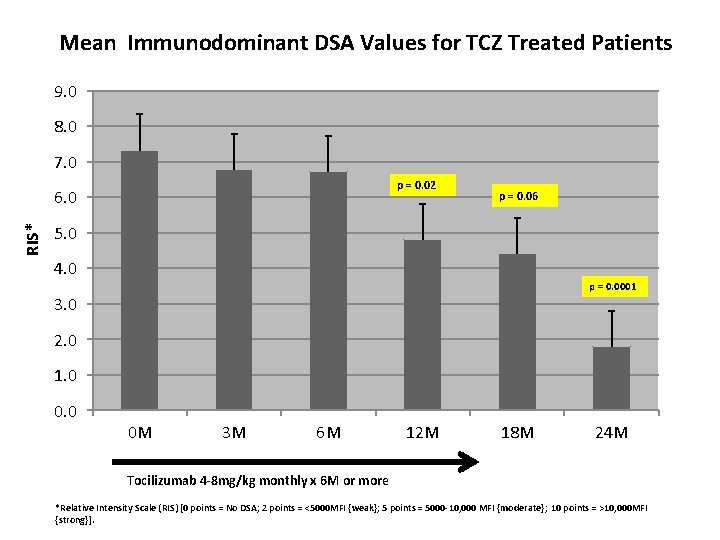
Mean Immunodominant DSA Values for TCZ Treated Patients 9. 0 8. 0 7. 0 p = 0. 02 RIS* 6. 0 p = 0. 06 5. 0 4. 0 p = 0. 0001 3. 0 2. 0 1. 0 0 M 3 M 6 M 12 M 18 M 24 M Tocilizumab 4 -8 mg/kg monthly x 6 M or more *Relative Intensity Scale (RIS) [0 points = No DSA; 2 points = <5000 MFI {weak}; 5 points = 5000 -10, 000 MFI {moderate}; 10 points = >10, 000 MFI {strong}].

Conclusions • Tocilizumab (anti-IL-6 R m. AB) has an attractive mechanism of action for desensitization and treatment of AMR • In two small uncontrolled clinical trials appears to have a good safety profile in patients pre and post-transplant • The drug may show promise as an add-on therapy to SOC for patients recalcitrant to desensitization with the Cedars protocol • It may also be one of the first drugs to extend the half-life of grafts chronically injured by persistent DSA
- Slides: 23