Tips and Traps when Using WRVUs to Measure



















- Slides: 24

Tips and Traps when Using WRVU’s to Measure Your Providers Compensation Thursday – October 11, 2018 presented by: Stan Kasmarcak, CPA Principal Alta Partners, LLC sjk@altapartnersllc. com phone: 440 -808 -3647 www. altapartnersllc. com

Alta Partners your partner for practice profitability Alta Partners provides physician billing, practice management, and healthcare consulting services throughout the states of Ohio, Kentucky, Michigan, Indiana, and Illinois…. not West Virginia… yet Founded in 2000; Alta is located in Westlake, OH (greater Cleveland) • Billing – Alta provides billing services to over 300 providers using several billing platforms – Specialize in FQHC, RHC billing • Practice Management – Manage physician practices throughout state – Employ practice staff at practices we manage • Healthcare Consulting – – – Practice Assessments Billing Assessments Physician Compensation Plan Design Healthcare Litigation Support Practice Valuation Services

Audience Survey for today’s talk. . . • Who is represented in today’s audience? – Hospital administrators? Hospital Finance? – Physician Practice Managers? – Private Practice? / Employed physician groups? • What are your biggest issues with your current physician compensation program? • Do you have production goals communicated to your physicians and/or colleagues in the practice? – patients seen, gross charges, WRVU’s? • Do you have incentives for your physicians / staff based on performance while on the job?

Today’s Agenda • Benefits of Using WRVU’s as a financial tool in physician practice management • How WRVU’s are calculated, who calculates them? , How reimbursement varies across country? • WRVU’s: Quantity - Production – • Median WRVU’s across select specialties WRVU’s: Price – – Reimbursement by WRVU’s Comparison with Ohio to National Averages • Usefulness in Budgeting / Comparative Analysis • Six Biggest Traps to watch for when Using WRVU’s to Compensate your Providers – • Survivor League Competition Conclusions / Questions

Relative Value Units (RVU’s) – Medicare’s methodology to measure work output • RBRVS scale (Resource Based Relative Value Scale) • Developed at Harvard University in the late 1980’s, updated annually • Fully implemented in 1992 by Medicare as a way to pay uniformly for physician services (OBRA of 1989 – prospective payment change for Medicare Part B) • Quantifies three types of resources used for EVERY CPT code: • • Physician Expense (also known as a Work RVU) Practice Expense Malpractice Expense These items are added up, adjusted for geographic price index, and multiplied by a conversion factor (CF) to determine what Medicare will pay for a specific CPT code in any given year

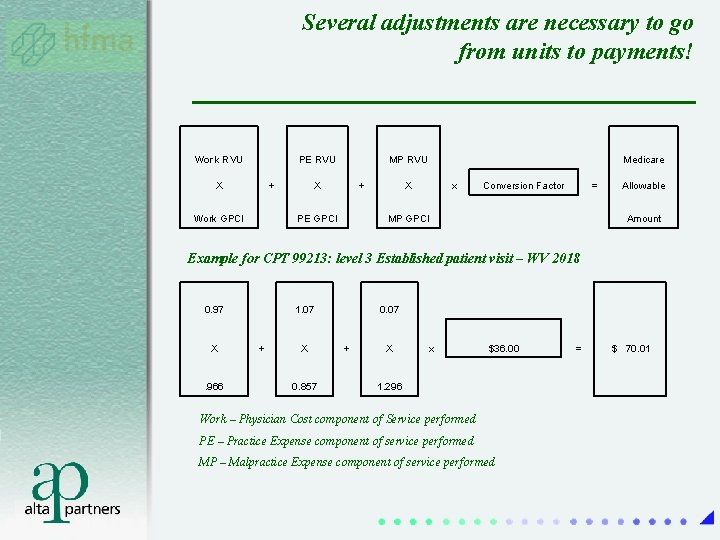
Several adjustments are necessary to go from units to payments! Work RVU PE RVU X + Work GPCI MP RVU X + PE GPCI Medicare X x Conversion Factor = MP GPCI Allowable Amount Example for CPT 99213: level 3 Established patient visit – WV 2018 0. 97 X . 966 1. 07 + X 0. 857 0. 07 + X x $36. 00 1. 296 Work – Physician Cost component of Service performed PE – Practice Expense component of service performed MP – Malpractice Expense component of service performed = $ 70. 01

Using WRVU’s is a great way to engage your physicians in a discussion about the health / productivity of their practice – WRVU’s provides a common basis for physicians to assess themselves whether its across the practice or across the country. WRVU value are easily attainable on internet and updated by CMS annually. All of which provides a good objective basis to work with, largely because there are no $ signs. – Web link to file: https: //www. cms. gov/Medicare-Fee-for-Service-Payment/Physician. Fee. Sched/PFS-Relative-Value. Files-Items/RVU 18 A. html? DLPage=1&DLEntries=10&DLSort=0&DLSort. Dir=descending – Physician are very familiar with clinical “base line” information and WRVU’s can be utilized in the same way to help evaluate if a particular result is considered “normal” or not and use to educate your providers • WRVU Productivity • Ave/ WRVU per patient visit - similar to Case Mix Index • Reimbursement / WRVU • Expenses / WRVU • Physician Compensation / WRVU – By incorporating WRVU’s into your financial reporting activities either as benchmarks, budgets, or targets – WRVU statistics will help enable you to determine what direction the practice is heading in. I will give you plenty of statistics today for you to help to assess your own practices’ effectiveness.

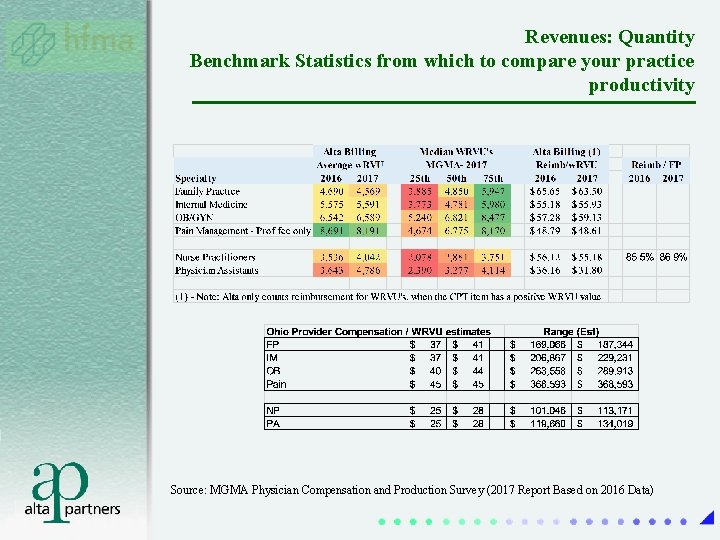
Revenues: Quantity Benchmark Statistics from which to compare your practice productivity Source: MGMA Physician Compensation and Production Survey (2017 Report Based on 2016 Data)

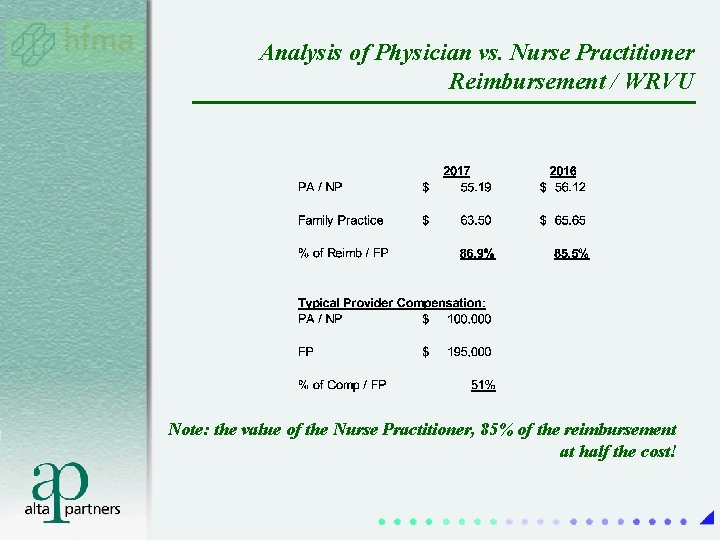
Analysis of Physician vs. Nurse Practitioner Reimbursement / WRVU Note: the value of the Nurse Practitioner, 85% of the reimbursement at half the cost!

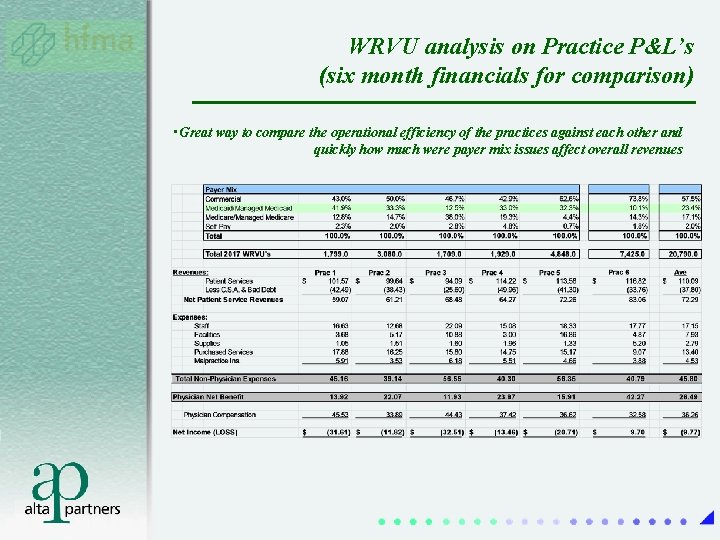
WRVU analysis on Practice P&L’s (six month financials for comparison) • Great way to compare the operational efficiency of the practices against each other and quickly how much were payer mix issues affect overall revenues

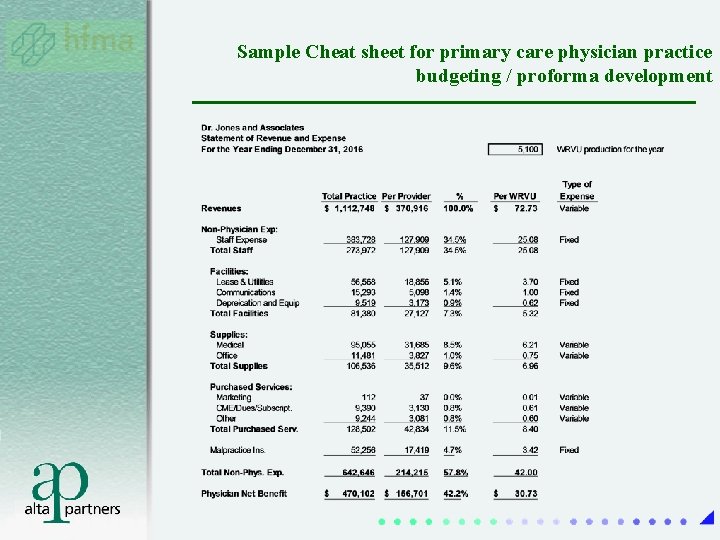
Sample Cheat sheet for primary care physician practice budgeting / proforma development

Tips and Traps when using WRVU’s Welcome to the WV HFMA Survivor League! See if your organization can manage through and say that your compensation program doesn’t fall into any of these WRVU Compensation Management Traps

Trap #1 - Not using the correct WRVU set! ALL WRVU’s need to be reviewed annually to ensure that the values used are correct and accurate in accordance for management of the physician compensation contracts. • Stan’s Rules for managing WRVU file sets / compensation contract management: 1. 2. 3. Use the SAME WRVU set for all physician contracts Use the current Year CMS WRVU values to automatically adjust for new CPT WRVU’s and eliminate giving credit when CPT’s are eliminated Watch your system to ensure, be aware, of ANY homemade WRVU’s being added into your system by billing.

A haunting example that can happen when homemade WRVU’s creep into your billing system True story: Doctor convinced administration / billing that she needed to have credit for a nurse who reviewed and monitored the patients vitals under a procedure known as conscious sedation, CPT 99144 / 99145. (Even though, by definition, the CPT is to credit the nurse ONLY for her time and effort). She said that it was worth 2. 5 WRVU’s credited to her and the billing WRVU table was adjusted to reflect this. Don’t let this happen to you! Comp at $65/WRVU Dr. Sheryl - Analysis of Production WRVU Reported Production Less: 99144, 99145 22, 167 100% (4, 538) -20% $1, 440, 823 (294, 938) Less: Modifier 50 WRVU overstatement (784) 16, 845 -4% (50, 973) 76% $1, 094, 912 WRVU, net BTW…. CPT 9144 paid, on average Dr. Sheryl Paid $65*2. 5 $ 30. 00 162. 50 Original Loss per 99144 $(132. 50) %

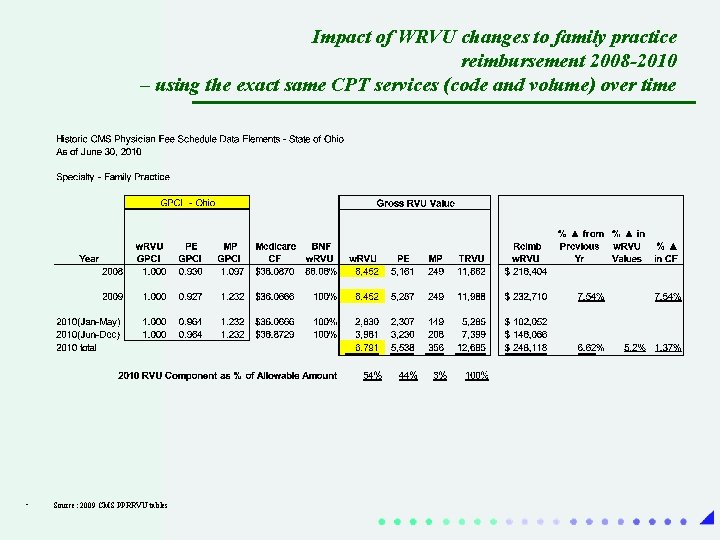
Trap #2 – Ensure that you have ability to adjust for significant changes in annual WRVU values as issued by CMS • All components of the RVU are reviewed and updated by CMS typically on a three year rotation – Physician work – Practice Expense – Malpractice – Since Provider contracts convert WRVU’s to compensation by using a conversion factor, be sure that you avoid the disaster of 2010 (see next slide), when the revision in WRVU’s went up for the same services by 5. 2%, and so did related provider compensation for many, many plans – Incorporate language that allows for a conversation factor change (for provider compensation) to be allowed in instances if WRVU values were to go up OR down by any appreciable amount.

Impact of WRVU changes to family practice reimbursement 2008 -2010 – using the exact same CPT services (code and volume) over time • Source: 2009 CMS PPRRVU tables

Trap #3 -Managing the special circumstance of OB Deliveries (more like a tip) Commercial Payers pay for OB cases based on the entire period of pregnancy and Medicaid pays for OB cases based on visits. IN ADDITION, because of OB rotations, different providers may be seeing the patient during the course of OB visits and/or at time of delivery. Because of these differences we recommend that you adjust the global delivery codes to the value of a delivery only, and then incorporate a means to count, track, and WRVU value each of the commercial patient visits CPT's Description Current Work RVU RVU / OB / PP With OB W/O OB Visits / RVU / OB/PP Visit Delivery Total Visits OB/PP Visit Portion RVU Diff Visits 59400, 59409 Uncomplicated Vaginal Delivery 32. 16 14. 37 17. 79 11 1. 62 11. 00 17. 79 14. 37 32. 16 59510, 59514 C-Section Delivery 35. 64 16. 13 19. 51 11 1. 77 1. 62 11. 00 17. 79 17. 85 35. 64 59610, 59612 VBAC 33. 87 16. 09 17. 78 11 1. 62 11. 00 17. 79 16. 08 33. 87

Trap #4: Do you calculate and compensate based on NET WRVU’s, not Gross • WRVU’s that are given credit to providers should closely mirror allowed charges in order to manage production with the reality of collections. • Consider these special cases: – Charge error adjustments – • Example; New patient charge originally, later, adjusted for Established patient charge • Is your provider getting credit for one charge… or two? – Insurance denial adjustments – – Is your organization classifying denials by type to report on later? • • Combined Charges / Part of procedure Provider not in network Multiple Provider Global period charges

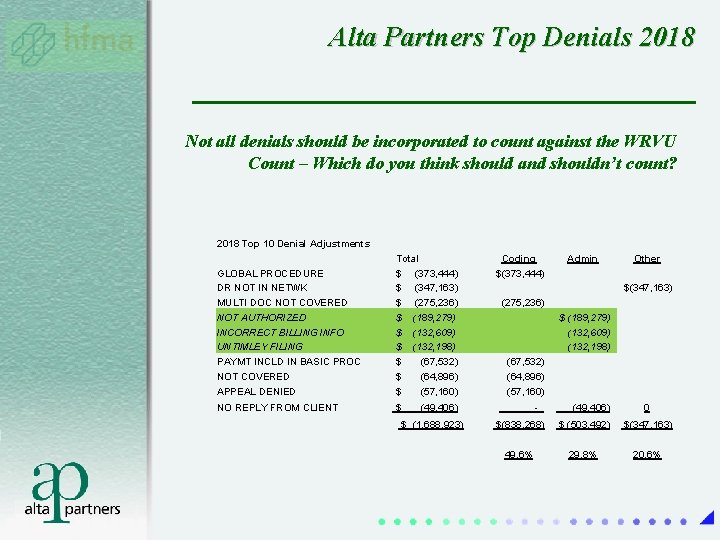
Alta Partners Top Denials 2018 Not all denials should be incorporated to count against the WRVU Count – Which do you think should and shouldn’t count? 2018 Top 10 Denial Adjustments GLOBAL PROCEDURE DR NOT IN NETWK MULTI DOC NOT COVERED NOT AUTHORIZED INCORRECT BILLING INFO UNTIMLEY FILING PAYMT INCLD IN BASIC PROC NOT COVERED APPEAL DENIED Total $ (373, 444) $ (347, 163) $ (275, 236) $ (189, 279) $ (132, 609) $ (132, 198) $ (67, 532) $ (64, 896) $ (57, 160) NO REPLY FROM CLIENT $ (49, 406) $ (1, 688, 923) Coding $(373, 444) Admin Other $(347, 163) (275, 236) (67, 532) (64, 896) (57, 160) $ (189, 279) (132, 609) (132, 198) - (49, 406) 0 $(838, 268) $ (503, 492) $(347, 163) 49. 6% 29. 8% 20. 6%

Made clear the rules that you wish to follow regarding denials Not all carriers follow the same rules for reimbursement. If you are paying your providers net of denials, you need to make sure you specify which set of rules you are “playing” by. CMS Part B Rules – I’ve seen this most often, if CMS would pay for the service, the provider gets credit even though, the claim wasn’t paid for some reason by the local carrier Local Carrier Rules – Truly matches compensation with revenues, however do you really want your provider wondering if they should do a procedure (or not) based on local carrier preference? , maybe? Maybe not?

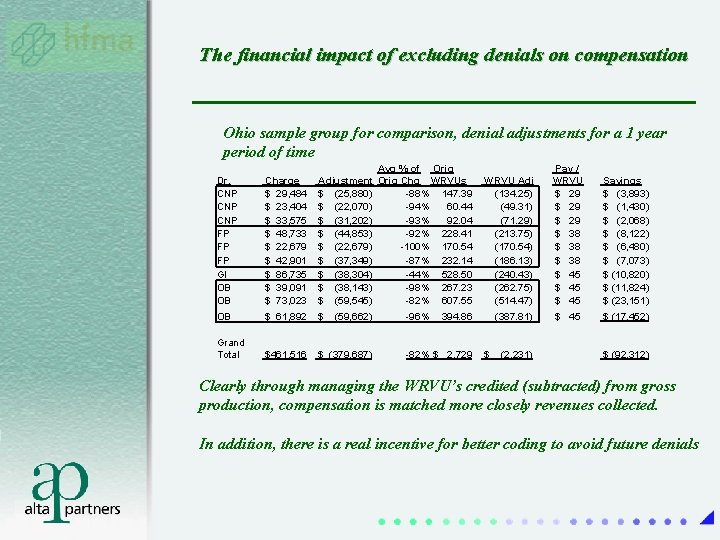
The financial impact of excluding denials on compensation Ohio sample group for comparison, denial adjustments for a 1 year period of time Avg % of Orig Adjustment Orig Chg WRVUs WRVU Adj $ (25, 880) -88% 147. 39 (134. 25) $ (22, 070) -94% 60. 44 (49. 31) $ (31, 202) -93% 92. 04 (71. 29) $ (44, 853) -92% 228. 41 (213. 75) $ (22, 679) -100% 170. 54 (170. 54) $ (37, 349) -87% 232. 14 (186. 13) $ (38, 304) -44% 528. 50 (240. 43) $ (38, 143) -98% 267. 23 (262. 75) $ (59, 545) -82% 607. 55 (514. 47) Dr. CNP CNP FP FP FP GI OB OB Charge $ 29, 484 $ 23, 404 $ 33, 575 $ 48, 733 $ 22, 679 $ 42, 901 $ 86, 735 $ 39, 091 $ 73, 023 OB $ 61, 892 $ (59, 662) -96% 394. 86 (387. 81) Grand Total $461, 516 $ (379, 687) -82% $ 2, 729 $ (2, 231) Pay / WRVU $ 29 $ 38 $ 45 Savings $ (3, 893) $ (1, 430) $ (2, 068) $ (8, 122) $ (6, 480) $ (7, 073) $ (10, 820) $ (11, 824) $ (23, 151) $ 45 $ (17, 452) $ (92, 312) Clearly through managing the WRVU’s credited (subtracted) from gross production, compensation is matched more closely revenues collected. In addition, there is a real incentive for better coding to avoid future denials

Trap #5: How do you manage multiple procedure payment reduction adjustments? • This discussion revolves around providers that perform multiple procedures at one encounter, get paid 100% for the first of the procedures, subsequent are paid at a lower rate, 50% or less, (MPPR adjustment for Medicare). • Do you adjust for the WRVU’s on subsequent procedures by the amount of the multiple procedure cost reduction? • Mixed schools of thought here to say the least. This affects your surgical professionals the most. A reduction is commensurate with the financial reality, but be prepared for a battle! – My suggestion, evaluate the prevalence of these adjustments, quantify the impact and adjust in your conversation factor, or if minor, don’t adjust at all.

Trap #6 – Communicating and calculating WRVU information Timely to your Providers • Are you able to report to your providers within two weeks after period end provider WRVU’s from which their production will be measured? • Credibility is everything – if your reports cannot be run without massaging data that takes weeks to compile and present - they are NO GOOD! • Are you firm on data input cut-offs? – Not entered/closed into the medical record not counted? Is this in the contract? • Are you calculating your WRVU production to the nearest quarter? - Not month and PLEASE, not by exact contract day!!

Thank YOU! Conclusions Q&A