TimbySmith Introductory MedicalSurgical Nursing 11e Chapter 16 Caring

Timby/Smith: Introductory Medical-Surgical Nursing, 11/e Chapter 16: Caring for Clients With Fluid, Electrolyte, and Acid–Base Imbalances Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Fluid and Electrolyte Balance • Body fluids – Components • Water and chemicals • Electrolytes: substances that carry electrical charge when dissolved in fluid • Acids: release hydrogen into fluid • Bases: substances bind with hydrogen – Purpose: regulate fluid volume, buffer blood to keep its p. H neutral Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins
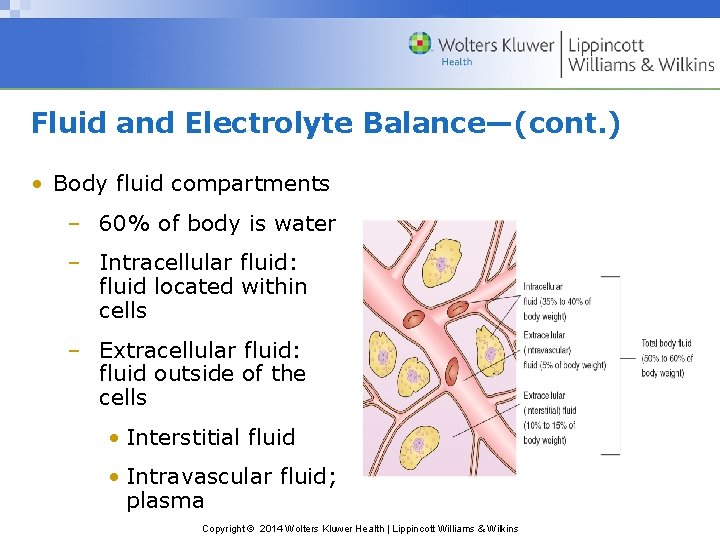
Fluid and Electrolyte Balance—(cont. ) • Body fluid compartments – 60% of body is water – Intracellular fluid: fluid located within cells – Extracellular fluid: fluid outside of the cells • Interstitial fluid • Intravascular fluid; plasma Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Intake and Output • Average fluid intake – Adult: 2500 m. L/day (Range: 1800 to 3600 m. L/day) – Sources: food and liquids • Fluid elimination – Sources • Urination, bowel elimination, perspiration, breathing • Insensible losses: sweat, exhaled air Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Distribution of Fluids and Electrolytes • Physiologic process: translocation of fluid and exchange of chemicals (electrolytes, acids, bases) is continuous – Five processes • Osmosis: movement of water through a semipermeable membrane; tonicity • Filtration: promotes movement of fluid according to pressure differences; kidneys • Passive and facilitated diffusion; example: insulin facilitates distribution of glucose inside cells • Active transport: sodium–potassium pump; requires ATP Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Mechanisms of Fluid and Electrolyte Regulation • Mechanisms to maintain normal fluid volume and electrolyte concentrations – Types • Osmoreceptors: neurons that sense blood concentration; simulates release of ADH; baroreceptors • Renin-angiotensin-aldosterone system: chemicals released to increase BP and blood volume • Natriuretic peptides: ANP and BNP released; increases urine production Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Fluid Imbalances • Hypovolemia: low volume of extracellular fluid – Causes: vomiting, diarrhea, wounds, profuse urination; hemoconcentration • Dehydration: extracellular and intracellular fluids are reduced – Assessment Findings: thirst • Diagnostic Findings: elevated Hct and blood cell counts, elevated urine specific gravity – Medical Management: restore fluid deficit; oral or IV • Nursing Management: 8 to 10 glasses water/day; avoid caffeine beverages; restrict sodium Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins
Fluid Imbalances—(cont. ) • Hypervolemia: high volume of water in intravascular fluid compartment – Causes: excessive oral intake, IV fluids, heart failure, kidney disease, adrenal gland dysfunction; circulatory overload – Assessment Findings: weight gain, elevated BP, pitting or nonpitting edema, dependent edema, moist lung sounds • Diagnostic Findings: low Hct and blood cell count, low specific gravity; hemodilution – Medical Management: restrict oral or parenteral fluid; diuretics; limit sodium Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Nursing Care Plan: Hypervolemia • Nursing diagnosis: Excess Fluid Volume related to intake that exceeds fluid loss – Baseline and daily weights (weight gain 2 lb/24 hours) – Accurate intake and output – Auscultate lung sounds – Measure BP, heart rate, respiratory rate – Inspect skin for edema, cracks, and breakdown Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Question A client is at risk for impaired skin integrity due to compromised circulation related to heart failure. Interventions to maintain intact skin includes: A) Changing the client’s position every 4 hours B) Restricting ambulation C) Applying elastic stockings D) Keeping client’s legs lower than the heart Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Answer C) Applying elastic stockings Rationale: Elastic stockings support valves in the veins and prevent fluid from pooling in dependent areas such as the feet and ankles. Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Third-Spacing • Third-spacing—translocation of fluid from intravascular to tissue compartments – Causes: hypoalbuminemia, burns, severe allergic reactions – Assessment Findings: ascites, generalized edema • Diagnostic Findings: hemoconcentration, CVP normal, blood counts borderline – Medical Management: albumin infusion, IV diuretic Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Electrolyte Imbalances • Electrolyte imbalances occur as deficits and/or excess; accompanied by fluid changes – Causes • Deficits: administration of IV fluids, vomiting, diarrhea, diuretics • Excess: orally consumed, parenteral administration of electrolytes, kidney failure, endocrine dysfunction, crushing injuries, burns • Priority electrolytes imbalances: sodium, potassium, calcium, magnesium Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Sodium Imbalances • Functions: maintaining normal nerve and muscle activity, regulating osmotic pressure, preserving acid–base balance • Hyponatremia – Causes: profuse diaphoresis, diuresis, loss of GI secretions (suctioning, drains), Addison’s disease – Assessment Findings: mental confusion, muscular weakness, anorexia, elevated body temperature, tachycardia – Medical Management: foods high in sodium, IV sodium chloride Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Sodium Imbalances—(cont. ) • Hypernatremia – Causes: diarrhea, excessive salt intake, high fever, excessive water loss, decreased water intake – Assessment Findings: thirst; dry, sticky mucous membranes; decreased urine output; fever • Diagnostic Finding: >145 m. Eq/L – Medical Management: water intake, hypotonic IV solution (0. 45% Na. Cl or 5% Dextrose) • Nursing Management: I&O; assess vital signs; dietary restrictions or supplements Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Potassium Imbalances • Function: maintaining normal nerve and muscle activity • Hypokalemia – Causes: potassium-wasting diuretics (Lasix, Hydro. DIURIL), GI tract fluid loss (suctioning, drains, vomiting), corticosteroids, IV insulin and glucose – Assessment Findings: fatigue, weakness, nausea, cardiac dysrhythmias, paresthesias • Diagnostic Finding: <3. 5 m. Eq/L – Medical Management: potassium-sparing diuretics (Aldactone), K+ foods, oral supplements (K-Lor), IV Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Potassium Imbalances—(cont. ) • Hyperkalemia – Causes: renal failure, potassium-sparing diuretics, supplements, diet sodas, crushing injuries, Addison’s disease, parenteral potassium salts – Assessment Findings: diarrhea, nausea, muscle weakness, cardiac dysrhythmias • Diagnostic Finding: >5. 5 m. Eq/L – Medical management: decreasing K+ intake, administration of insulin and glucose, Kayexalate, peritoneal dialysis or hemodialysis • Nursing Management: medications, diet teaching Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Calcium Imbalances • Hypocalcemia • Function: blood clotting, transmission of nerve impulses, regulated by parathyroid gland – Causes: vitamin D deficiency, hypoparathyroidism, burns, pancreatitis, corticosteroids, blood administration, intestinal malabsorption – Assessment Findings: tingling, circumoral paresthesia, muscle cramps, positive Chvostek’s sign, Trousseau’s sign, bleeding, tetany • Diagnostic Finding: serum calcium <8. 8 mg/d. L – Medical Management: oral calcium and vitamin D, IV calcium Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Calcium Imbalances—(cont. ) • Hypercalcemia – Causes: parathyroid tumors, multiple fractures, Paget’s disease, prolonged immobilization, chemotherapy agents, multiple myeloma – Assessment Findings: deep bone pain, constipation, anorexia, polyuria, pathologic fractures, kidney stones • Diagnostic Finding: serum calcium >10 mg/d. L – Medical Management: cause, IV sodium chloride, Lasix, corticosteroids or plicamycin – Nursing Management: diet teaching, fluids, fall safety Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Magnesium Imbalances • Function: transmission of nerve impulses, activation of enzyme systems including functioning of B vitamins • Hypomagnesemia – Causes: alcoholism, diabetic ketoacidosis, renal disease, burns, malnutrition, intestinal malabsorption, diuresis, prolonged gastric suction – Assessment Findings: tachycardia, paresthesias, neuromuscular irritability, HTN, mental changes – Diagnostic Finding: serum magnesium <1. 3 m. Eq/L – Medical Management: oral or IV magnesium, diet supplements Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Magnesium Imbalances—(cont. ) • Hypermagnesemia – Causes: renal failure, Addison’s disease, excessive antacid or laxative use, hyperparathyroidism – Assessment Findings: flushing, hypotension, lethargy, bradycardia, muscle weakness, coma – Diagnostic Finding: serum magnesium >2. 1 m. Eq/L – Medical Management: decreasing oral magnesium or parenteral replacement, mechanical ventilation • Nursing Management: BP and respiratory monitoring Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Question Which of the following interventions would be appropriate when caring for a client with hypercalcemia? A) Encourage fluids. B) Promote bed rest. C) Administer calcium supplement tablets. D) Administer antibiotics. Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Answer A) Encourage fluids. Rationale: Hypercalcemia is a condition in which serum calcium is elevated. By providing increased amounts of fluid, calcium excretion is promoted and the amount of circulating calcium decreases. Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Acid–Base Balance • Regulation of normal plasma p. H (7. 35 to 7. 45= normal) • Carbonic acid (H 2 CO 3) and bicarbonate (HCO 3) – Chemical: adding or removing hydrogen ions – Organ: lungs regulate carbonic acid levels and kidneys regulate bicarbonate levels; decompensation • Imbalance types – Acidosis: excessive accumulation of acids or excessive loss of bicarbonate in body fluids – Alkalosis: excessive accumulation of bases or loss of acid in body fluids Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Acid–Base Imbalances • Metabolic Acidosis (p. H <7. 35 to 7. 45) – Causes: shock, cardiac arrest, starvation, diabetic ketoacidosis, renal failure, ASA overdose, loss of intestinal fluid, wound drainage – Assessment Findings: deep and rapid breathing, Kussmaul’s breathing, nausea, headache, flushing, abdominal pain, weakness • Anion gap – Medical Management: cause, replacing fluids and electrolytes, IV bicarbonate Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Acid–Base Imbalances—(cont. ) • Metabolic Alkalosis (p. H >7. 45) – Causes: excessive bicarbonate-containing drugs, diuretic therapy, vomiting, gastric suctioning – Assessment Findings: anorexia, nausea, paresthesias, confusion, hypertonic reflexes, decreased respirations – Medical Management: cause, potassium administration, sodium chloride administration • Nursing Management: ABG findings; reports assessment findings Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Acid–Base Imbalances—(cont. ) • Respiratory Acidosis (p. H <7. 35) – Causes: pneumothorax, pulmonary edema, asthma, pneumonia, drug overdose, head injuries CF – Assessment Findings: cyanosis, tremors, respiratory insufficiency – Medical Management: mechanical ventilation, airway suctioning, bronchodilators, and antibiotics • Arterial blood gas (ABC): values to determine acid –base balances: p. H, HCO 3, Pa. CO 2 Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Acid–Base Imbalances—(cont. ) • Respiratory Alkalosis (p. H 7. 45) – Causes: anxiety, fever, overactive thyroid, ASA poisoning, mechanical ventilation – Assessment Findings: increased respiratory rate, light -headedness, numbness and tingling of fingers and toes, paresthesias, sweating, panic – Medical Management: rebreathe expired air (brown bag breathing), sedation • Nursing management: report assessment findings, monitor laboratory values Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Question Which acid–base disturbance would be most characteristic of a narcotic overdose? A) Metabolic Acidosis B) Respiratory Acidosis C) Metabolic Alkalosis D) Respiratory Alkalosis Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Answer B) Respiratory acidosis Rationale: A narcotic overdose slows the rate and depth of breathing. This leads to retention of carbon dioxide (acid). Hypoventilation problems produce respiratory acidosis. Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins
- Slides: 30