TimbySmith Introductory MedicalSurgical Nursing 11e Chapter 11 Pain

Timby/Smith: Introductory Medical-Surgical Nursing, 11/e Chapter 11: Pain Management Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Pain • Pain is a privately experienced, unpleasant sensation usually associated with disease or injury. – Emotional component—suffering • Classification – Source: nociceptive or neuropathic – Onset, intensity, and duration: acute or chronic Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Nociceptive Pain • Noxious stimuli that are transmitted from the point of cellular injury over peripheral sensory nerves to pathways between the spinal cord and thalamus and from the thalamus to the cerebral cortex of the brain • Nociceptive pain types – Somatic pain – Visceral pain Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Nociceptive: Somatic Pain • Caused by mechanical, chemical, thermal, or electrical injuries or disorders affecting bones, joints, muscles, skin, or other structures composed of connective tissue – Superficial somatic pain/cutaneous pain: from insect bite or paper cut; perceived as sharp or burning discomfort – Deeper somatic pain: caused by trauma; produces sensations that are sharp, throbbing, and intense – Dull, aching, diffuse discomfort with long-term disorders • Example: arthritis Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Nociceptive: Visceral Pain • Arises from internal organs such as the heart, kidneys, and intestine that are diseased or injured – Causes: ischemia, compression of an organ, intestinal distention, contraction – Is usually diffuse, poorly localized, accompanied by ANS symptoms such as nausea, vomiting, pallor, hypotension, and sweating • Referred pain: discomfort in a general area of the body but not in the exact site where an organ is located Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins
Neuropathic Pain • Pain processed abnormally by the nervous system • Results from damage to either the pain pathways in peripheral nerves or pain-processing centers in the brain – Examples: phantom limb pain, spinal cord injuries, strokes, diabetes, and herpes zoster (shingles) – Cancer pain: nociceptive or neuropathic • Nerve damage: radiation or drugs Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Acute Pain • Acute pain: less than 6 months – Associated with tissue trauma: eases with healing – Manifestations: elevated blood pressure and heart and respiratory rates, diaphoresis, and dilated pupils • Chronic pain: lasts longer than 6 months – Affects quality of life; others begin to show negative reactions to sufferer – Breakthrough pain – Manifestations: similar to the symptoms of depression, including hopelessness, weight loss, fatigue, or physical immobility Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Question Chronic pain is described as an unpleasant sensory and emotional experience associated with: A) Actual tissue damage B) Actual or potential tissue damage C) Only observable pain behaviors D) Physiologic signs and symptoms that the pain exists Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Answer B) Actual or potential tissue damage Rationale: Chronic pain is associated with actual or potential tissue damage. Chronic pain is associated with many pain behaviors that people do not normally associate with pain. There is no change in vital signs with chronic pain. Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins
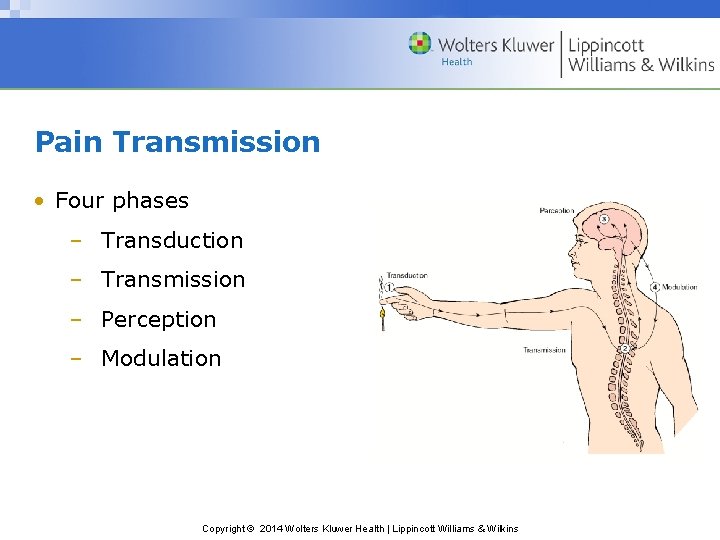
Pain Transmission • Four phases – Transduction – Transmission – Perception – Modulation Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Transduction • Conversion of chemical information in the cellular environment to electrical impulses that move toward the spinal cord – Initiated by cellular disruption • Nociceptors: specialized pain receptors located in the free nerve endings of peripheral sensory nerves – A-delta fibers: can carry pain impulses fast or slow; get sharp, acute initial pain – C-fibers: throbbing, aching, or burning after initial pain • Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins
Transmission • Peripheral nerve fibers form synapses with neurons in the spinal cord. • Impulses move from the spinal cord to the brain. Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Perception • Brain experiences pain at a conscious level; locates pain, its intensity, and what it means; and gives emotional response. – Pain threshold: point at which the pain-transmitting neurochemicals reach the brain, causing conscious awareness • Hyperalgesia – Pain tolerance: amount of pain a person endures once threshold has been reached • Variables: age, gender, fatigue Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Modulation • Brain transmits a response down the spinal nerves to the point where the pain transmission originated to alter the pain experience. – Endogenous opioids—neurochemical – Painful sensation is reduced. Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Pain Assessment • Client’s description of its onset, quality, intensity, location, and duration – What makes the pain better or worse? • Nonverbal behaviors: clenched jaw, frowning, crying, rocking, or fidgeting – Allodynia—exaggerated pain response • Assessment biases: client’s pain misunderstood Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins
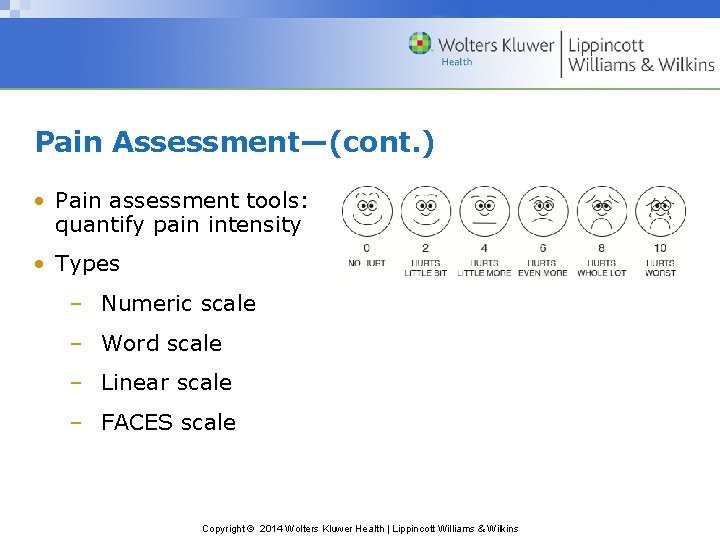

Pain Assessment—(cont. ) • Pain assessment tools: quantify pain intensity • Types – Numeric scale – Word scale – Linear scale – FACES scale Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Assessment Standards • Accredited healthcare facilities – Right to assessment and pain management – Assessment is appropriate for age, developmental level, condition, and culture. – Pain is reassessed regularly. – Healthcare workers are educated on pain management. – Client’s choices of pain management are respected. Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Pain Management • Drug and nondrug interventions • Techniques for pain management – Blocking brain perception – Interrupting pain-transmitting chemicals – Combining analgesics – Substituting sensory stimuli – Altering pain transmission Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Question To evaluate adequately the effectiveness of pain control regimens, the nurse should: A) Be casual and informal B) Not bother if the client is quiet C) Use a pain assessment tool D) Rely on the feedback from the client’s family member Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Answer C) Use a pain assessment tool Rationale: An effective pain treatment requires a thorough pain assessment. Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Pain Management—(cont. ) • Techniques used to prevent, reduce, or relieve pain – Drug therapy • Opioids—narcotic: interfere with pain perception centrally (at the brain); used for mild to moderate pain • Oxycodone, morphine sulfate • Nonopioids—non-narcotic: alter neurotransmission at the peripheral level (sight of injury); for mild pain • Ketorolac tromethamine (Toradol), Tylenol Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Methods of Pain Medication Administration • Routes – Analgesic drugs: oral, rectal, transdermal, or parenteral • Equianalgesic dose – Patient-controlled analgesia (PCA) – Intraspinal analgesia – Palliative sedation: relieving intractable pain experienced by dying client Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Addiction • Repetitive pattern of drug seeking and drug use to satisfy a craving for a drug’s mind-altering or mood-altering effects • Fewer than 1% of clients who need drugs for pain relief, even for more than 6 months become addicted • Fears – Refuse or self-limit prescribed drug therapy – Nurses administer subtherapeutic doses. Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Tolerance • Condition in which a client needs increasingly larger doses of a drug to achieve the same effect as when the drug was first administered – Consequence of poor pain control • An ineffective dose should be increased by 25% to 50% – Consult with physician Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Physical Dependence • Person experiences physical discomfort, known as withdrawal symptoms, when a drug taken routinely for some time is abruptly discontinued. • To avoid withdrawal symptoms, drugs should be discontinued gradually. – Lowered over 1 week or longer Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Question A client taking opioids for cancer pain begins to require more medication to provide the same amount of analgesia. This is known as: A) Physical dependence B) Drug tolerance C) Drug addiction D) Obsessive-compulsive Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Answer C) Drug tolerance Rationale: Drug tolerance is the need for an increased opioid dose to maintain the same effect. Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Nondrug Interventions • Alternative nondrug methods − Transcutaneous electrical nerve stimulation (TENS) and percutaneous electrical nerve stimulation (PENS) − Acupuncture and acupressure − Heat or cold application − Spinal surgery: rhizotomy, cordotomy − Other • Distraction, relaxation, imagery Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Nursing Management • Performs a comprehensive assessment of each client’s pain on admission – Determines the onset, quality, intensity, location, and duration of pain • Administration of analgesics every 3 hours rather than PRN often provides a uniform level of pain relief. • Collaborates with client: informs of pain relief options • Assess complications related to pain or prolonged pain medication; risk for falls, knowledge deficit, constipation Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Nursing Care Plan: Acute Pain • Nursing diagnosis: Acute Pain • Expected outcome: Client will rate pain intensity at tolerable level of “ 5” within 30 minutes of pain management technique. • Interventions – Assess client’s pain and its characteristics at least every 2 hours while awake. – Modify or eliminate factors that contribute to pain. – Administer prescribed analgesics or alternative pain management techniques promptly. Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins
- Slides: 30