TimbySmith Introductory MedicalSurgical Nursing 10e Chapter 21 Caring

Timby/Smith: Introductory Medical-Surgical Nursing, 10/e Chapter 21: Caring for Clients with Lower Respiratory Disorders

Inflammation of Bronchial Mucous Acute Bronchitis Membranes; Tracheobronchitis n n n Cause: Bacterial and fungal infection; Chemical irritation Diagnostics: Sputum cultures; Chest film Signs/Symptoms: (Initial) Non-productive cough, Fever, Malaise; (Later) Bloodstreaked sputum, Coughing attacks; Inspiratory crackles Treatment: Antipyretics; Expectorants; Antitussives; Humidifiers; Broad-spectrum antibiotics Nursing Management

Pneumonia n Pathophysiology n n n Inflammatory Process Affecting Bronchioles and Alveoli; Alveoli Filled with Exudate Reduced Surface Area for Gas Exchange Classified by Cause Etiology n n Acute infection Radiation therapy Chemical ingestion, inhalation; Bacteria n n n n Steptococcus pneumoniae pneumocystis carinii(bacteria developed in AIDS pt) Virus Fungus Aspiration (stroke victims) Artificial Ventilation (VAP) Hypostasis

Pneumonia n At risk: n n n Very Young Elderly Hospitalized Intubated Immunocompromised Prevention n n (see box 21 -2) Pneumococcal Vaccine Flu Vaccine Coughing and Deep Breathing Hand Washing Frequent Mouth Care, Continuous Suction for VAP
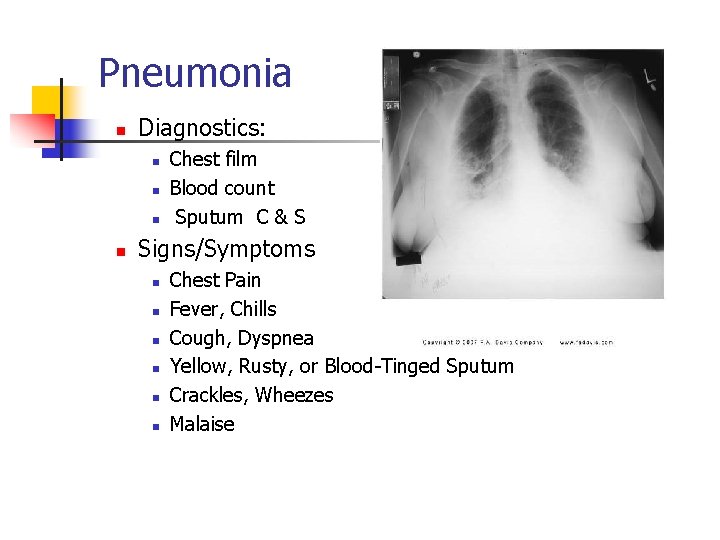
Pneumonia n Diagnostics: n n Chest film Blood count Sputum C & S Signs/Symptoms n n n Chest Pain Fever, Chills Cough, Dyspnea Yellow, Rusty, or Blood-Tinged Sputum Crackles, Wheezes Malaise

Pneumonia n Complications n n n n Pleurisy CHF empyema Pleural Effusion Atelectasis septicemia Signs and Symptoms in Elderly n New-Onset n n Confusion Lethargy Fever Dyspnea

Pneumonia n Treatment: n Antibiotic (bacterial) PO or IV n Hydration n Chest physical therapy n Analgesics/Antipyretics n Antiviral Medication (Zovirax) n Bronchodilators n Expectorants or cough suppressants n Oxygen Nursing Management n

Acute Inflammation of Parietal, Visceral Pleurae Pleurisy n n n Cause: Usually secondary to pneumonia, pulmonary infections, tuberculosis, lung cancer, pulmonary embolism Diagnostics: Chest radiography; Sputum culture; Thoracentesis: Fluid specimen, pleural biopsy Signs/Symptoms: Inspirational severe, sharp pain; Shallow respirations; Pleural fluid accumulation; Dry cough; Dyspnea; Friction rub, fever, elevated WBC Treatment: Treat underlying condition; NSAIDs Analgesics/antipyretic drugs Nursing Management
n Pathophysiology Pleural Effusion Abnormal Fluid Collection Between Visceral, n Parietal Pleurae. Pleural Fluid Not Reabsorbed, May Collapse Lung n Etiology n Transudative Heart Failure Liver or Kidney Disease PE n Exudative Pneumonia TB CA

Pleural Effusion cont. n Diagnostics n n Chest radiograph; CT scan Signs/Symptoms: Fever; Pain; Dyspnea; Dullness upon chest percussion; Dim breath sounds; Friction rub; Tachypnea; Cough n Treatment: Antibiotics; Analgesics; Thoracentesis; Chest tube n Nursing Management
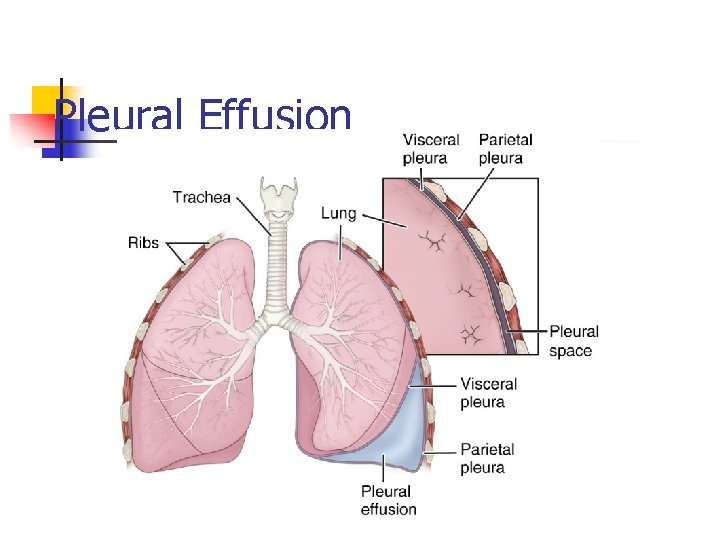
Pleural Effusion

n Acute Respiratory Disease of Short Duration Cause: Viral contamination via respiratory transmission; Mutations Influenza n n Fatalities related to secondary bacterial complications, esp. those immunocompromised n Diagnostics: Chest radiography; Sputum analysis n Signs/Symptoms: See Table 21 -2 n Treatment: Symptomatic n Nursing Management n Prevention Yearly Vaccination(85% effective) should not be give to clients with allergy to eggs At-Risk Individuals Health Care Workers Handwashing Avoidance of infected people

Tuberculosis n Pathophysiology n n n AFB Implant on Bronchioles or Alveoli Tubercle Formed Immune System Keeps in Check 5%-10% Infected Become Ill May Activate with Impaired Immunity

Pulmonary Tuberculosis n Primarily a bacterial infectious disease affects lungs; may infect kidneys, other organs; Affects one-third of world’s population; Leading cause of death from infectious disease, among those with HIV n Cause: Tubercle bacilli: Gram-positive; Transmitted via n n n droplet inhalation; Classifications Diagnostics: Chest radiographs; Tuberculin skin tests; CT scan; MRI; Gastric lavage; Gastric aspiration; Bronchoscopy; C & S tests Signs/Symptoms: Fatigue, weight loss; clients at risk; Low fever; Night sweats; Persistent Cough; Blood-streaked sputum; Weakness; Hemoptysis; Dyspnea At Risk: elderly; alcoholics; crowded living conditions; new immigrants; immunocompromised; lower socioeconomic status; homeless

Therapeutic Interventions n n Technique to destroy; Transmission Combination of Drugs for 6 - 24 Months (toxicity, resistance); n n n n INH Rifampin PZA Ethambutol Streptomycin Occasional Surgical Removal: Segmental resection; Wedge resection; Lobectomy; Pneumonectomy Isolation Nursing Management (see ATI pg 125 -126

Prevention of TB Spread n n Clean, Well-Ventilated Living Areas Isolation of Patients who have Active TB High-Efficiency Filtration Masks Gowns, Gloves, Goggles If Contact with Sputum Likely
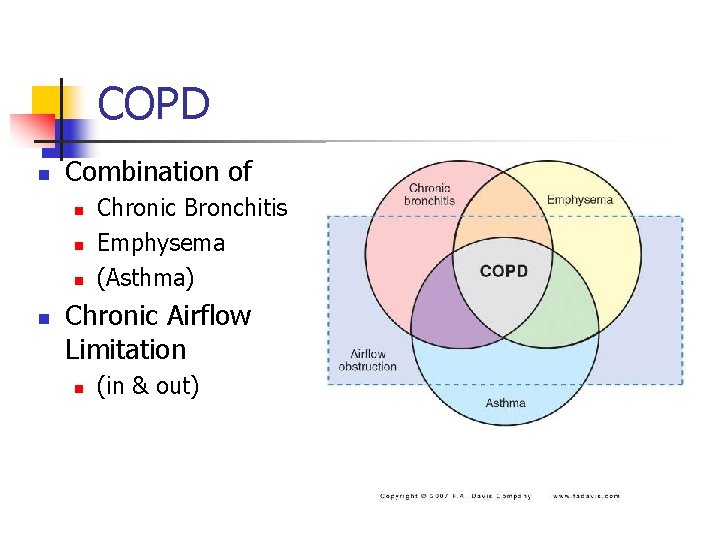
COPD n Combination of n n Chronic Bronchitis Emphysema (Asthma) Chronic Airflow Limitation n (in & out)
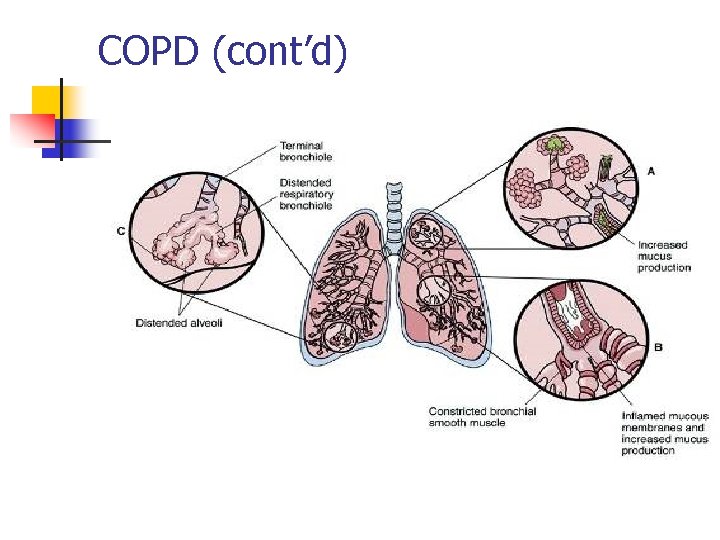
COPD (cont’d)

Airflow in lungs is. Pulmonary obstructed caused by Obstructive Disease bronchial obstruction, congenital abnormalities n n Increased resistance to expiration, creating prolonged expiratory phase of respiration n COPD n n n n Emphysema Chronic bronchitis Asthma Atelectasis Sleep apnea Cystic fibrosis bronchiectasis

COPD Etiology n n n Smoking Passive Smoke Exposure Pollutants Familial Predisposition α 1 AT Deficiency (Emphysema)
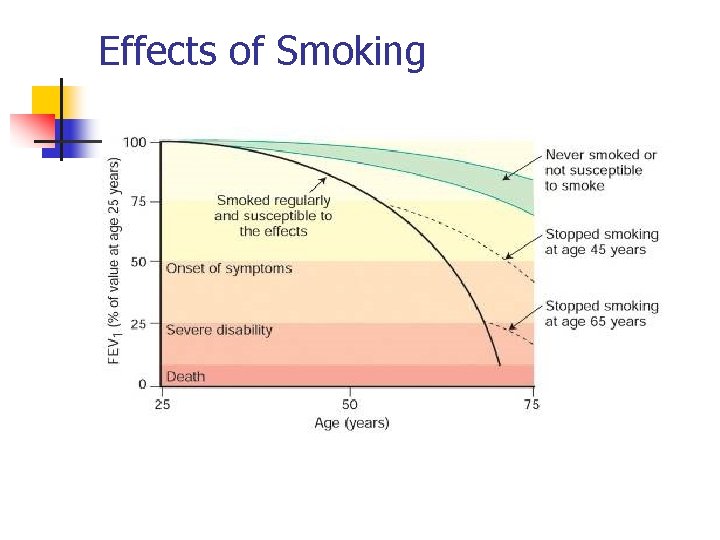
Effects of Smoking

COPD Prevention Smoking!!

COPD diagnositics n n n Chest X-Ray CT Scan ABGs CBC Spirometry Sputum Analysis n n n PFT PULSE OX H/H Chest physiotherapy AAT levels Peak expiratory flow meters

COPD signs and symptoms n n n n n Chronic Cough Chronic Dyspnea Prolonged Expiration Barrel Chest Activity Intolerance Diminished breath sounds Hypoxemia Hypercarbia Thin extremities n n n n Wheezing, Crackles Thick, Tenacious Sputum Increased Susceptibility to Infection Mucous Plugs Accessory muscles Rapid, Shallow respirations Pallor; cyanosis (late) Hyperresonance n (emphysema)

Complications of COPD n n Cor Pulmonale Weight Loss n Resting before eating n Avoid gas-producing food n Eat four to six small meals rather than three large ones n Take small bites and chew slow Pneumothorax Respiratory Failure

COPD Therapeutic Interventions n n n n Stop Smoking!! Oxygen 1 -2 L/m Supportive Care Pulmonary Rehab Surgery Mechanical Ventilation End-of-Life Planning n Medications n n Bronchodilators Corticosteroids Expectorants NMT/MDI
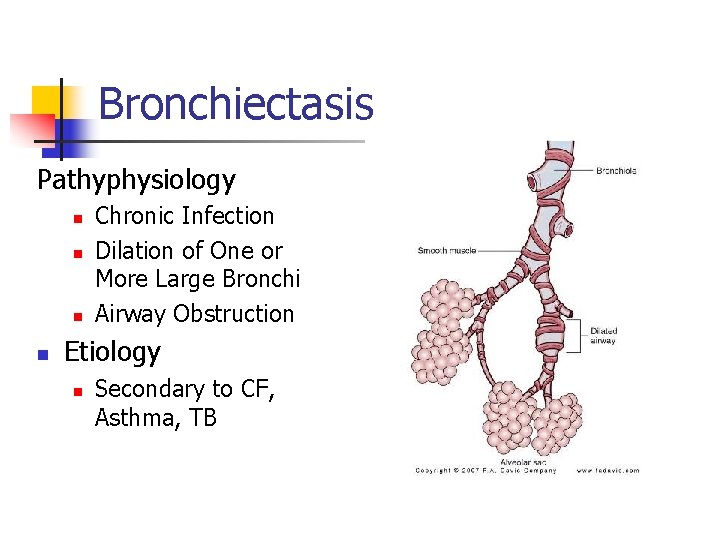
Bronchiectasis Pathyphysiology n n Chronic Infection Dilation of One or More Large Bronchi Airway Obstruction Etiology n Secondary to CF, Asthma, TB

Bronchiectasis Signs and Symptoms n n n n Dyspnea Cough Large Amounts of Sputum Anorexia Recurrent Infection Clubbing Crackles and Wheezes

Bronchiectasis Therapeutic Interventions n n n Antibiotics Mucolytics, Expectorants Bronchodilators Chest Physiotherapy Oxygen Surgical Resection

Collapse of Alveoli Prevents Gas Exchange Atelectasis n n Causes: Mucus plug; Aspiration; Prolonged bed rest; Fluid or air in thoracic cavity; Enlarged heart; Aneurysm; hypoventilation n Signs/Symptoms: (Small area) Few; (Large area): Cyanosis; Dyspnea; Fever; Pain; Tachycardia; Tachypnea; Increased secretions n Treatment: Removal of cause; Raise secretions; Bronchodilators; Humidification; O 2 administration n Nursing Management: TCDB; incentive spirometer; ambulate
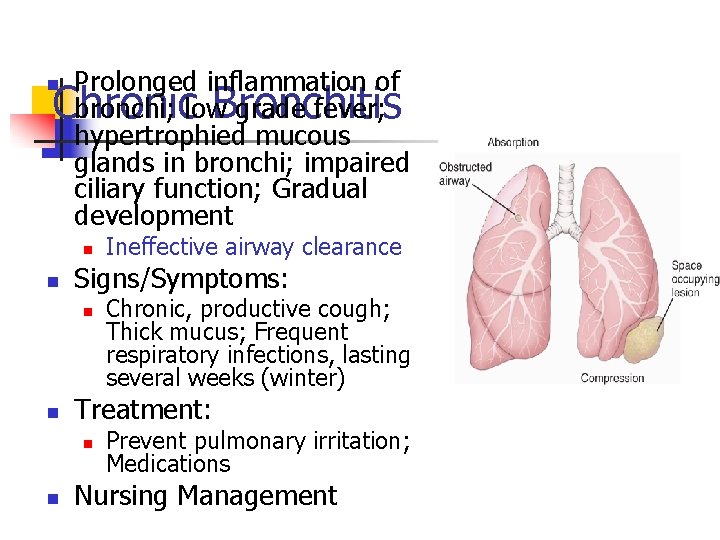
Prolonged inflammation of bronchi; low grade fever; Chronic Bronchitis hypertrophied mucous glands in bronchi; impaired ciliary function; Gradual development n n n Signs/Symptoms: n n Chronic, productive cough; Thick mucus; Frequent respiratory infections, lasting several weeks (winter) Treatment: n n Ineffective airway clearance Prevent pulmonary irritation; Medications Nursing Management

Abnormal Alveoli Distention, Destruction; loss Pulmonary Emphysema of elastic recoil; damage to pulmonary capillaries; air trapping; disabling disease n n n Impaired Gas Exchange Signs/Symptoms: (Initial) Exertional dyspnea; (Progressive) Chronic cough; Mucopurulent sputum; “Barrel chest”; Pursed-lip breathing; Prolonged, difficult expiration; Wheezing; (Advanced) Memory loss; CO 2 narcosis Treatment: Slow progression; Treat obstructed airways (Bronchodilators, O 2, ATB, physical therapy, corticosteroids (limited) Nursing Management
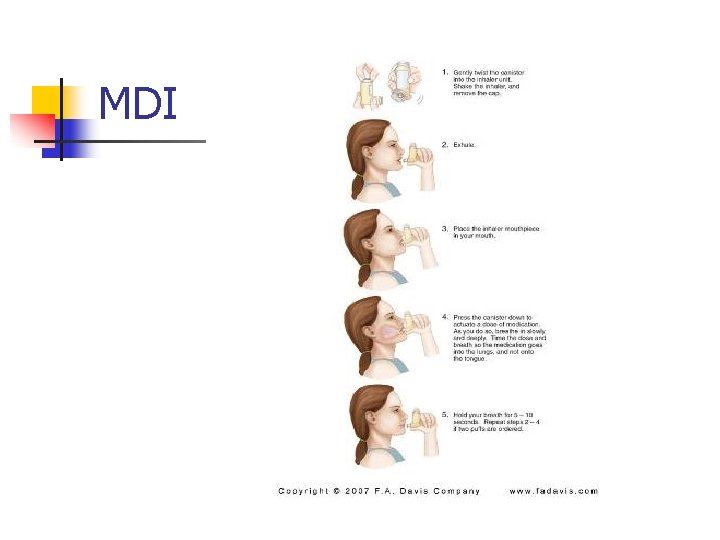
MDI
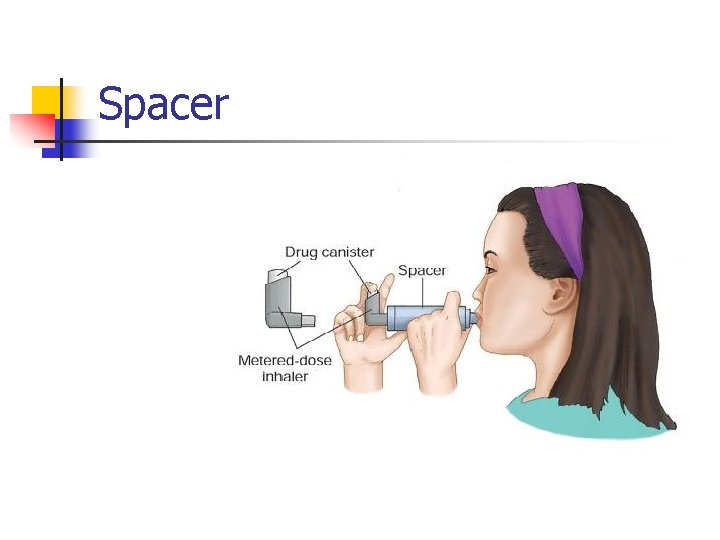
Spacer

NMT
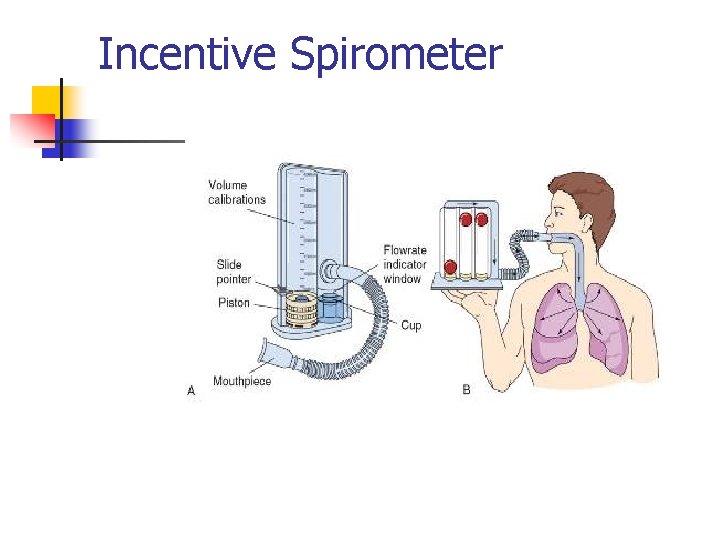
Incentive Spirometer
Chest Physiotherapy
Pulmonary Rehabilitation

n Reversible Obstructive Disease of Lower Asthma Airway; spasm of bronchial smooth muscles; air trapping n n n Cause: Inflammation; Airway hyperreactivity to stimuli (Allergic; Non-allergic; Mixed) Diagnostic: allergy skin testing Signs/Symptoms: Paroxysms of SOB, wheezing, coughing; Thick, tenacious sputum; use of accessory muscles; may be worse at night

Asthma n Triggers n n n Smoking Allergens Infection Sinusitis Stress GERD n Complication n Status Asthmaticus n n Severe, Sustained Asthma Worsening Hypoxemia Respiratory Alkalosis Progresses to Respiratory Acidosis May Be Life Threatening
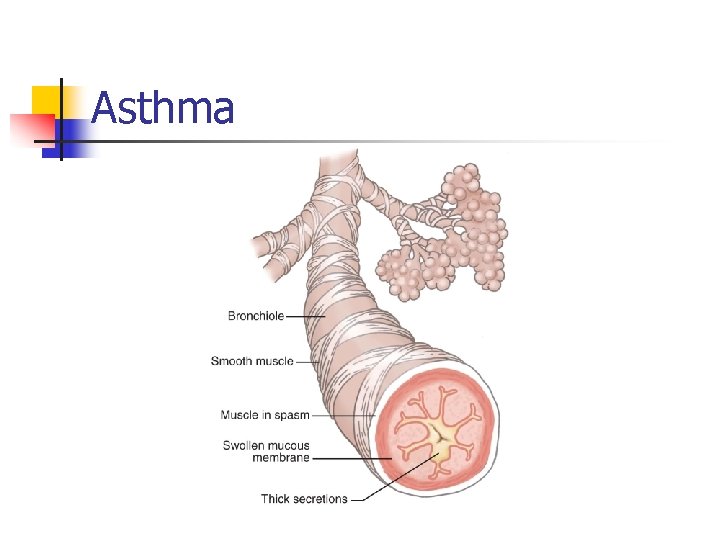
Asthma

Asthma Therapeutic Interventions n n n Monitor with Peak Flow Meter Avoid Triggers Avoid Smoking

Asthma Therapeutic Interventions (cont’d) n Bronchodilators n n Corticosteroids n n Adrenergic (Ventolin, Serevent) Leukotriene Inhibitors (Accolate, Singulair) Theophylline (Rare) Inhaled, IV, PO Mast Cell Inhibitors (Exercise Induced) Antihistamines Oxygen PRN

Nursing Diagnoses: COPD n n n n Impaired Gas Exchange Ineffective Airway Clearance Ineffective Breathing Pattern Activity Intolerance Imbalanced Nutrition Anxiety Fatigue

Impaired Gas Exchange n Monitor n n Lung Sounds, Respiratory Rate and Effort Dsypnea Mental Status Sa. O 2, ABGs n Position n n Fowler’s Good Lung Down Administer Oxygen Teach Breathing Exercises Discourage Smoking

Ineffective Airway Clearance n Monitor n n n Lung Sounds Sputum n n Encourage n n n Fluids Deep Breathing Coughing n n Administer Expectorants Turn q 2 h or Ambulate Suction prn Consider CPT or Mucus Clearance Device

Ineffective Breathing Pattern n Monitor n n n Respiratory Rate, Depth, Effort ABGs, Sa. O 2 Determine/Treat Cause n n Position Teach Diaphragmatic Breathing

Activity Intolerance n Monitor Response to Activity n n n Vital Signs Sa. O 2 Use Portable O 2 for Ambulation n n Allow Rest Between Activities Obtain Bedside Commode Increase Activity Slowly Refer to Pulmonary Rehabilitation

Patient Education n n Assist Patient to Stop Smoking! Pulmonary Rehabilitation Breathing Exercises Energy Conservation
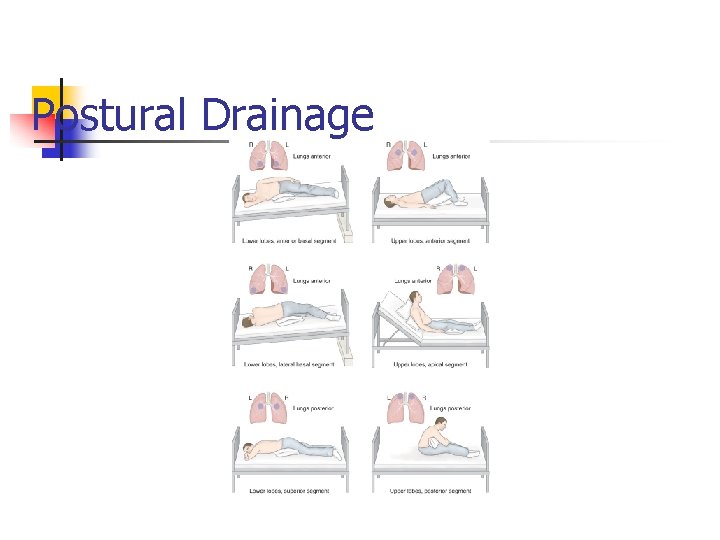
Postural Drainage

Cause: Exposure to organic, inorganic Occupational Lung Diseases dusts and noxious gases of long periods of time n • n n n Diagnostics: Chest radiograph; Pulmonary function tests Symptoms: Dyspnea; cough; (Coal dust) Black-streaked sputum Treatment: Conservative; Symptomatic; O 2 therapy for severe dyspnea Nursing Management

Continuous. Arterial High Pressure in the Pulmonary Hypertension Arteries n n n Cause: Rt Ventricular Failure; CAD; Valve Disease; Lung disease Diagnostics: EKG; ABG analysis; Cardiac catheterization; Pulmonary function tests; Echocardiography; Ventilation-perfusion scan; Pulmonary angiography Signs/Symptoms: Dyspnea on exertion; Weakness; fatigue; crackles; cyanosis; tachypnea Treatment: Vasodilators, Anticoagulants; (Rightsided failure) Digitalis, diuretics; Heart–lung transplantation; low sodium diet Nursing Management
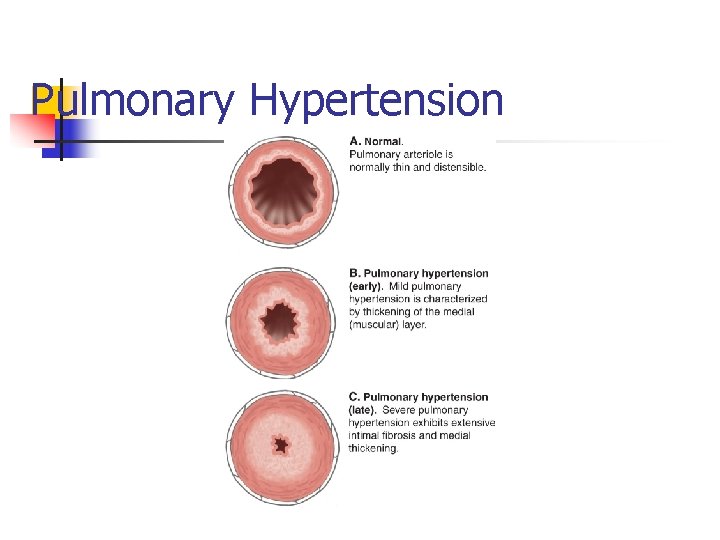
Pulmonary Hypertension

Pulmonary Embolism n Pathophysiology n n n Blood Clot in Pulmonary Artery or branches Ventilation-Perfusion Mismatch Impaired Gas Exchange Lung Infarction Etiology n n Thrombus formed in the venous system or right side of heart DVT Most Common Fat Emboli From Compound Fracture Amniotic Fluid Emboli During L&D
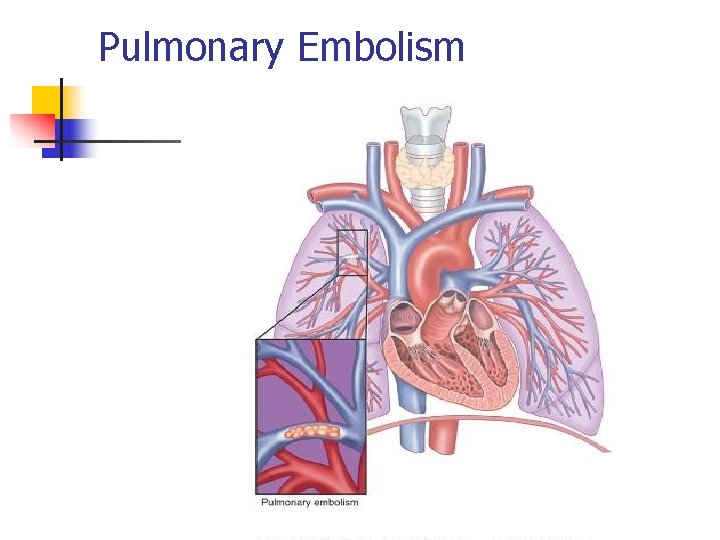
Pulmonary Embolism

Obstruction of Pulmonary Arteries or Pulmonary Branches Embolism n n n Cause: Thrombus formed in the venous system or right side of heart Diagnostics: Chest radiograph; Serum enzymes; Lung, CT scan; Pulmonary angiography; Ultrasonography; Impedance plethysmography; D -dimer Signs/Symptoms: (Small area) Pain; Tachycardia; Dyspnea (Large area) Severe dyspnea; Severe pain; Cyanosis; Tachycardia; Restlessness; Shock; Sudden death Treatment: Thrombolytics; Anticoagulation; Surgery; Procedures Nursing Management

Pulmonary Edema n Fluid Accumulation in Interstitium, Alveoli of Lungs n n Cause: Right side of heart delivers more blood to pulmonary circulation than left side can handle Signs/Symptoms: Dyspnea; Cyanotic extremities; Skin color; Continual bloodtinged (pink), frothy sputum; Cough Treatment: Emergency treatment for cardiogenic pulmonary edema Nursing Management

Inability to Exchange Sufficient Amounts Respiratory of O 2, CO 2 Failure n n n Cause: (Acute) Life-threatening, occurs suddenly; (Chronic) Underlying disease – COPD, aspiration, neuromuscular disorders Diagnostics: Chest radiography; Serum electrolytes; History; ABGs (Pa. O² <60 mm Hg; Pa. CO² >50 mm Hg) Signs/Symptoms: Restlessness; Wheezing; Cyanosis; Accessory muscle use for breathing Treatment: Endotracheal, tracheostomy tube; Humidified O 2 via nasal cannula, Venturi or rebreather masks; Mechanical ventilation Nursing Management
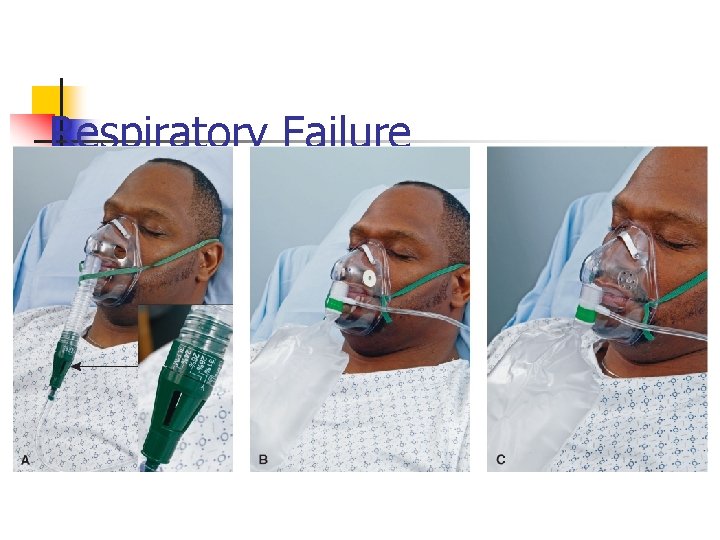
Respiratory Failure

Acute Respiratory Distress Syndrome (ARDs) n n Noncardiogenic Pulmonary Edema, secondary to other clinical condition; Can lead to respiratory failure, death Pathophysiology n n n Alveolocapillary Membrane Damage Pulmonary Edema Alveolar Collapse Lungs Stiff and Noncompliant Lungs May Hemorrhage

ARDs Etiology n n n n Acute Lung Injury n Septicemia n Shock n Aspiration Drug ingestion/overdose Hematologic disorders Metabolic disorders Trauma Surgery Embolism; Not Usually in Patients With Chronic Respiratory Disease

Diagnostics: Acute Chest Respiratory Distress Syndrome radiography n n n Signs/Symptoms n n n Evidence of acute respiratory failure ABGs Tachypnea Dyspnea, fine crackles Cyanosis Anxiety Restlessness; Mental confusion Treatment: n n Intubation Mechanical ventilation Colloids Nutritional support

Lung Cancer n n Common Cancer, esp. smokers; #1 cause of CA death in U. S. Types n n Small Cell Lung Cancer Large Cell Carcinoma Adenocarcinoma Squamous Cell Carcinoma

Lung Cancer Etiology n Smoking n n n Smokers 13× as Likely to Develop Cancer as Nonsmokers Environmental Tobacco Smoke Other Carcinogens n n n Asbestos Arsenic Pollution

Lung Cancer Diagnostic Tests n n n Chest X-Ray CT, PET Scan MRI Sputum Analysis Biopsy Additional Tests to Find Metastasis

Lung Cancer Signs and Symptoms n n None Until Late Dyspnea Cell type, tumor size + location, degree of metastasis determine Recurrent Infection Anorexia and Weight Loss n Cardinal signs n n n Cough Productive of mucopurulent or blood-streaked sputum Hemoptysis Pain Wheezing/Stridor

Therapeutic Interventions n n n Factor dependent, esp. on tumor classification, Stage (TNM System) Chemotherapy (Usually Palliative) Radiation (Usually Palliative)

Lung Cancer Complications n n n Pleural Effusion Superior Vena Cava Syndrome Ectopic Hormone Secretion n n ADH (SIADH) ACTH (Cushing’s Syndrome) Actelectasis Metastasis

Thoracic Surgery n n n n Remove, repair chest wall traumas, tumors; Obtain biopsy sample Thoracotomy Thoracentesis Pneumonectomy Lobectomy Resection Transplant

Thoracic Surgery Preoperative Care n n Monitor Respiratory Status Teach n n Routine Preop Teaching What to Expect Visit SICU Include Family

Thoracic Surgery Postoperative Care n n Intensive Care Setting Monitor n n n Vital Signs Sa. O 2, ABGs Hemodynamic Parameters Lung Sounds Ventilator Chest Tubes n n Surgery interferes with normal thoracic cavity pressures; Lung expansion Lungs must be post-operatively reinflated n Draining secretions, air, blood from thoracic cavity via surgically -placed catheter(s) n Connected to closed, underwater-seal drainage system: 1 – 2 catheters n Anterior: Removes air n Posterior: Removes fluid
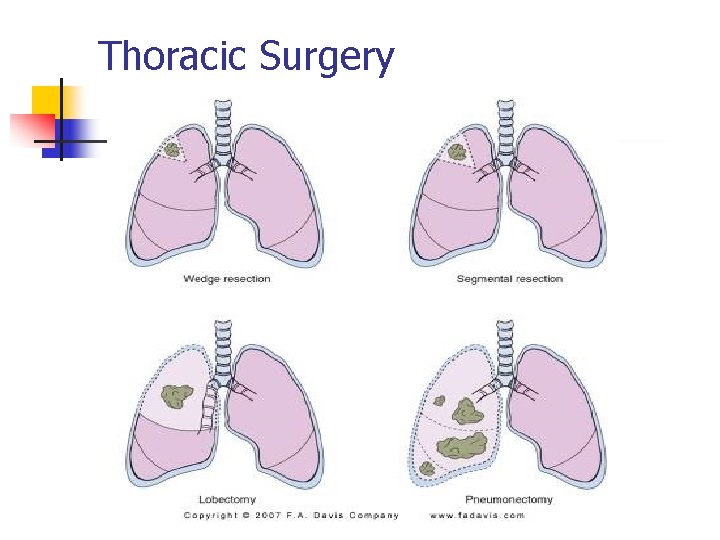
Thoracic Surgery
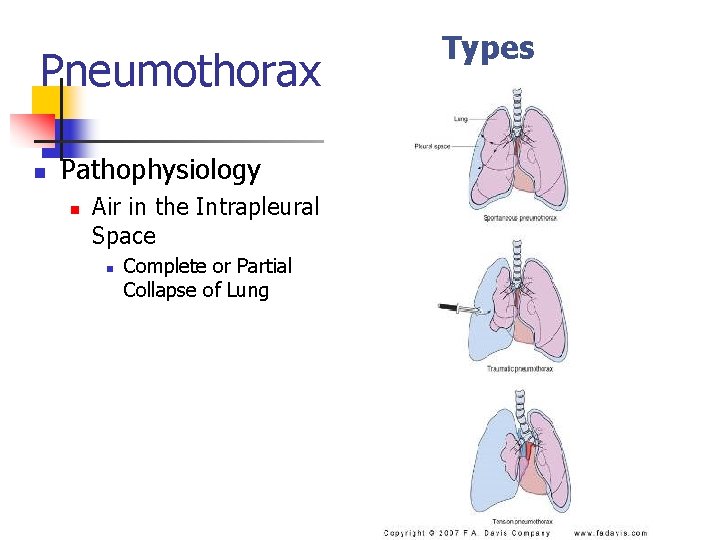
Pneumothorax n Pathophysiology n Air in the Intrapleural Space n Complete or Partial Collapse of Lung Types

Signs and Symptoms n n n Shallow, Rapid Respirations Asymmetrical Chest Expansion Dyspnea Chest Pain Absent Breath Sounds Over Affected Area n Tension Pneumothorax Signs and Symptoms n n Tracheal Deviation Bradycardia Cyanosis Shock and Death If Untreated

Pneumothorax n Diagnostic Tests n n History and Physical Examination Chest X-Ray ABGs, Sa. O 2 Therapeutic Interventions n n n Monitor ABGs and Respiratory Status Chest Tube to Water Seal Drainage Pleurodesis (Sclerosis) for Recurrent Collapse

Pneumothorax Nursing Care n n Monitor Respiratory Status Monitor Chest Drainage System n Equipment at bedside n n n Monitor and assess drainage system for n n n hemostats or clamps vaseline gauze amount of suction presence of air leaks integrity of the water seal chamber absence of kinks in the tubing Report Changes Promptly
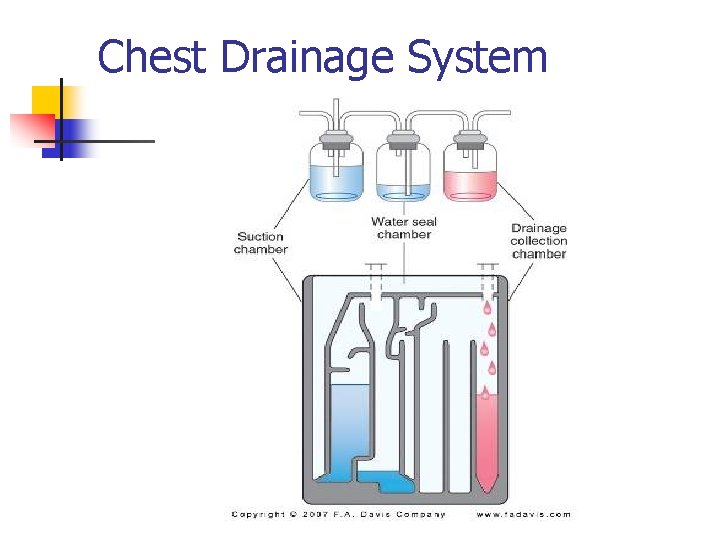
Chest Drainage System
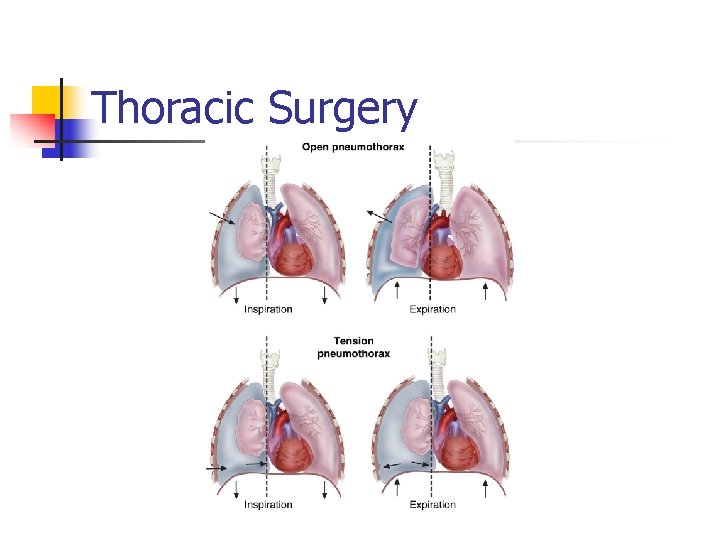
Thoracic Surgery

Rib Fractures/Flail Chest n Etiology n n Trauma Cough CPR Care n n Control Pain Encourage Coughing and Deep Breathing Promote Adequate Ventilation Cause n n n Multiple Rib Fractures Ribcage Not Able to Maintain Bellows Action Care n n Monitor ABGs Mechanical Ventilation

End of Presentation
- Slides: 80