Tickborne Illness Welcome to the module on Tickborne

Tick-borne Illness

Welcome to the module on Tickborne Illness 2 �Please take this brief pre-module quiz https: //goo. gl/forms/ELCFFYKc. Kyh. R 5 EA 62

This module works a lot better in “presentation” mode 3

Outline �Introduction �Lyme Disease �Anaplasma/Ehrlichia �Babesia �Assorted other TBI’s HINT: click on any of the links to short-cut directly to that section!

Return to Outline �Introduction �Lyme Disease �Anaplasma/Ehrlichia �Babesia �Assorted other TBI’s

Return to Outline Introduction �A 32 year old healthy woman who lives in New England presents with fever to 101. 5˚F �A week ago, she scratched her leg behind the knee �Underneath her fingernail, she noticed a “poppy seed” �Patient/husband unsure what it was, as it was too small to see much �However, when husband squeezed, it burst and had blood within it

Return to Outline Introduction �What infections is this patient at risk for? �How will we diagnosis her illness? �How will we treat her?
Return to Outline � Introduction �Lyme Disease �Anaplasma/Ehrlichia �Babesia �Assorted other TBI’s • Epidemiology • Clinical manifestations • Diagnosis • Treatment • Post-Lyme Syndrome • Chronic Lyme: facts and myths
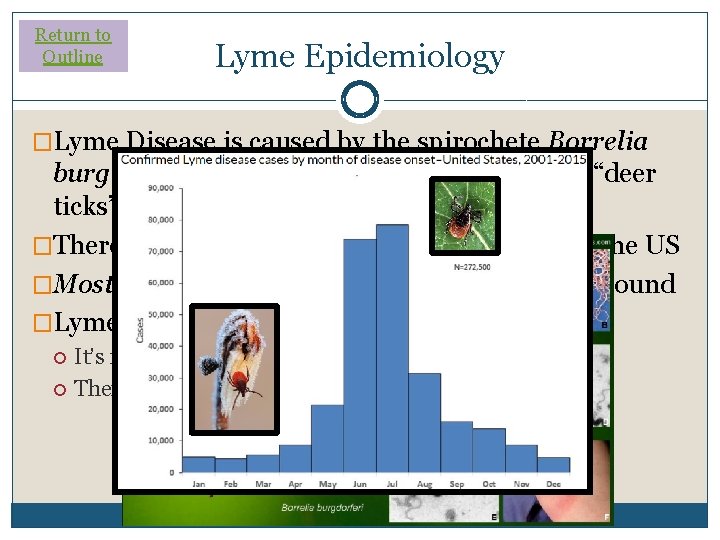
Return to Outline Lyme Epidemiology �Lyme Disease is caused by the spirochete Borrelia burgdorferi and spread by Ixodes scapularis “deer ticks” �There are probably ~40, 000 cases per year in the US �Most occur in summer, but cases happen year round �Lyme Disease is on the rise It’s not just increased recognition and testing There are more ticks that spread Lyme
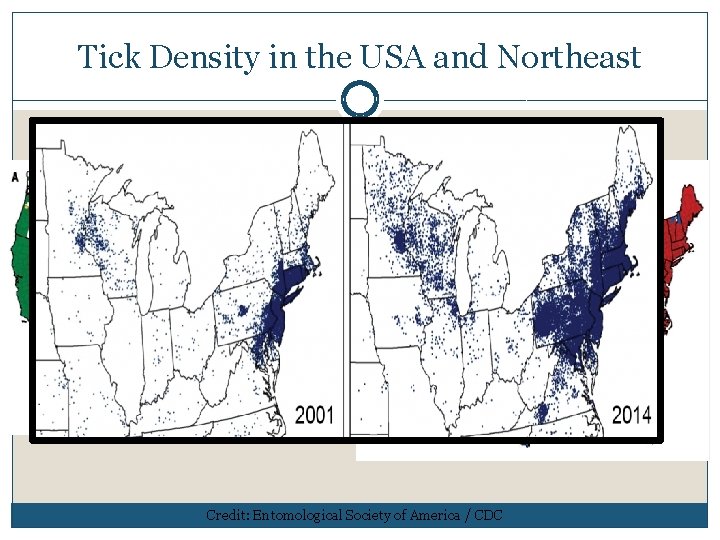
Tick Density in the USA and Northeast 1998 2015 Credit: Entomological Society of America / CDC
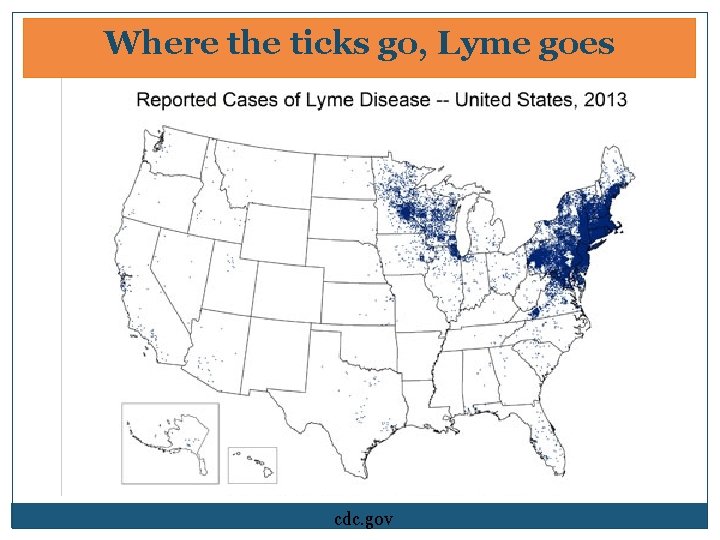
Where the ticks go, Lyme goes cdc. gov

Return to Outline Blame the deer? �With the fall in natural predators, New England deer populations have exploded. Is this the problem? Actually not particularly �Deer can have more than 30, 000 ticks on them! But the deer do NOT carry Borrelia burgdorferi Because tick-density is so high on deer, would have to eliminate MOST of the deer population to have an impact

Return to Outline Blame the deer? �It matters much more how many MICE are around �For instance, if it’s a high acorn-production year, there are more Lyme cases the next year, because of more mice
Lyme Disease: clinical manifestations Transmission via tick bite There are 3 Early Localized broad types of Disseminated Lyme Disease Late
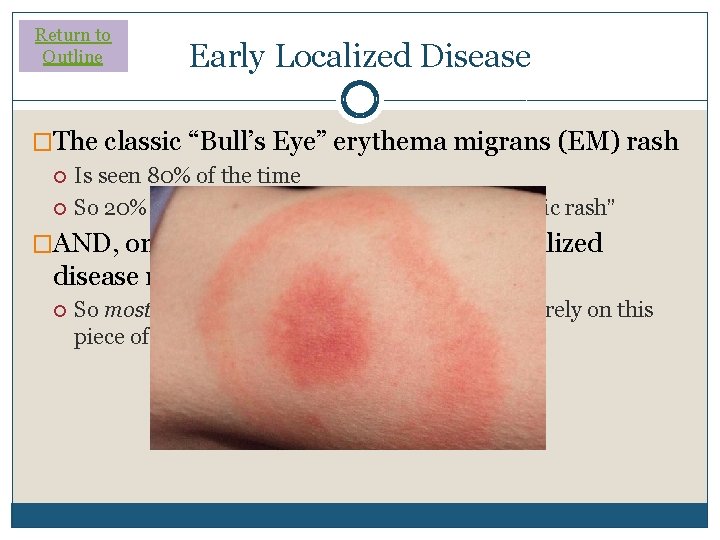
Return to Outline Early Localized Disease �The classic “Bull’s Eye” erythema migrans (EM) rash Is seen 80% of the time So 20% of folks with Lyme won’t have this “classic rash” �AND, only 25% of patients with early localized disease recall a tick bite So most patients will not recall a tick bite…don’t rely on this piece of history
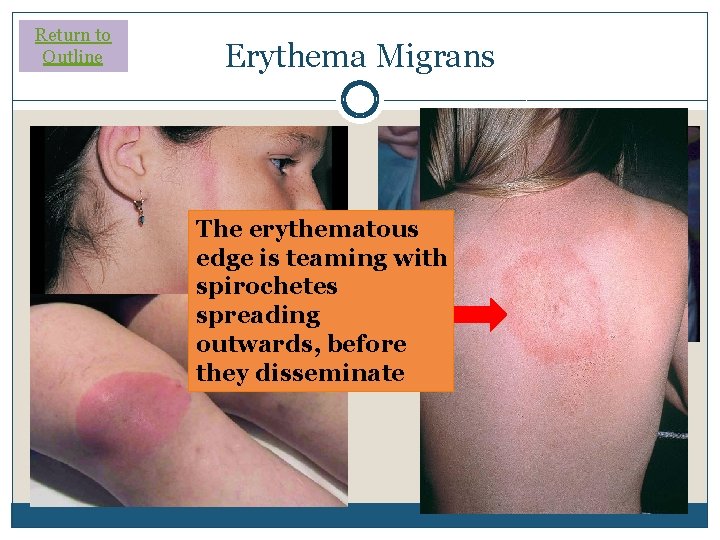
Return to Outline Erythema Migrans The erythematous edge is teaming with spirochetes spreading outwards, before they disseminate
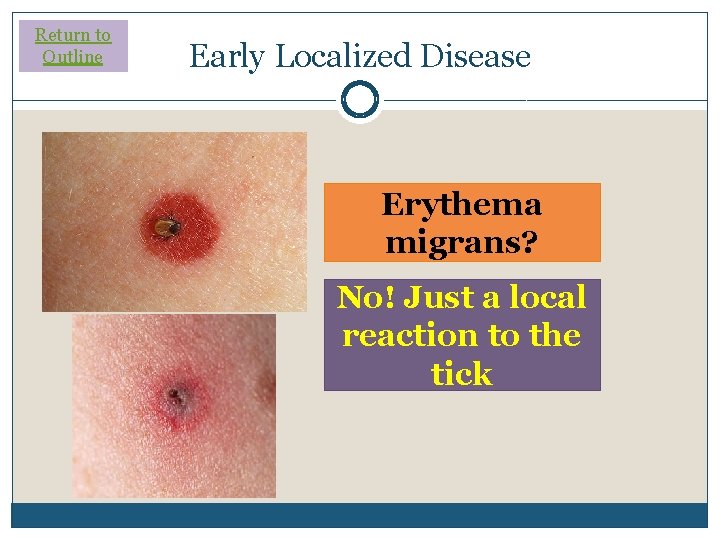
Return to Outline Early Localized Disease Erythema migrans? No! Just a local reaction to the tick
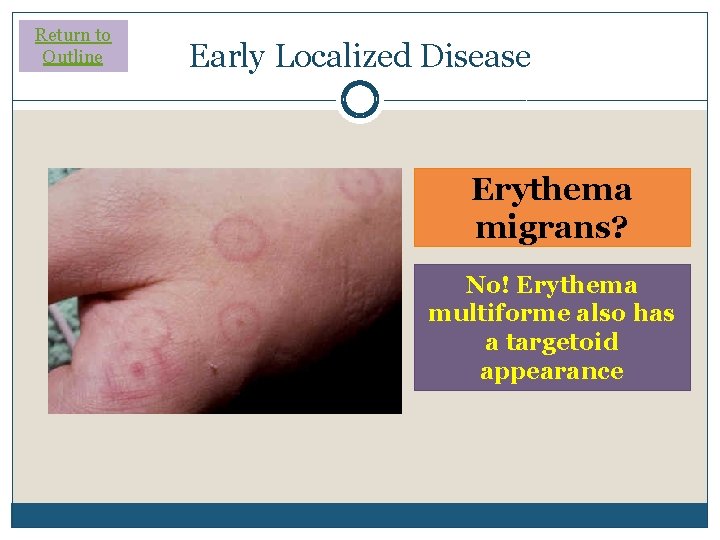
Return to Outline Early Localized Disease Erythema migrans? No! Erythema multiforme also has a targetoid appearance
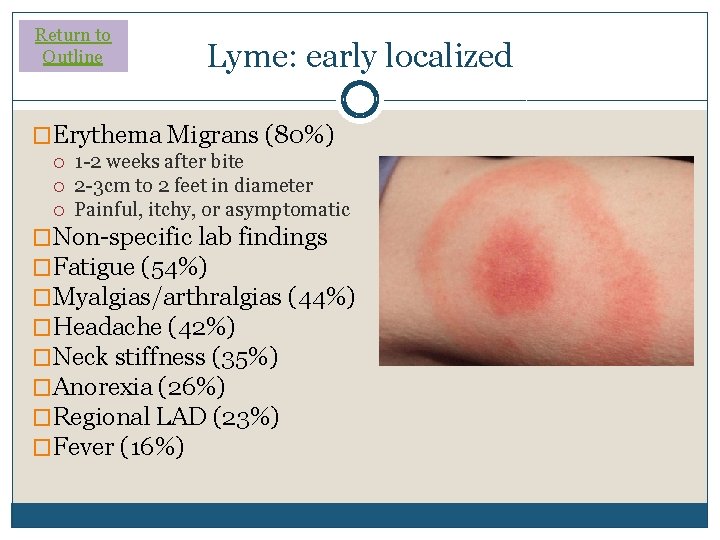
Return to Outline Lyme: early localized �Erythema Migrans (80%) 1 -2 weeks after bite 2 -3 cm to 2 feet in diameter Painful, itchy, or asymptomatic �Non-specific lab findings �Fatigue (54%) �Myalgias/arthralgias (44%) �Headache (42%) �Neck stiffness (35%) �Anorexia (26%) �Regional LAD (23%) �Fever (16%)
Lyme Disease: clinical manifestations Transmission via tick bite Early Disseminated Early Localized Late

Return to Outline Lyme: Early Disseminated �Early disseminated rash �Neurologic findings Lymphocytic meningitis, radiculopathies, cranial nerve palsies (CN 7 especially) �Carditis Anything from 1 st degree to 3 rd degree block
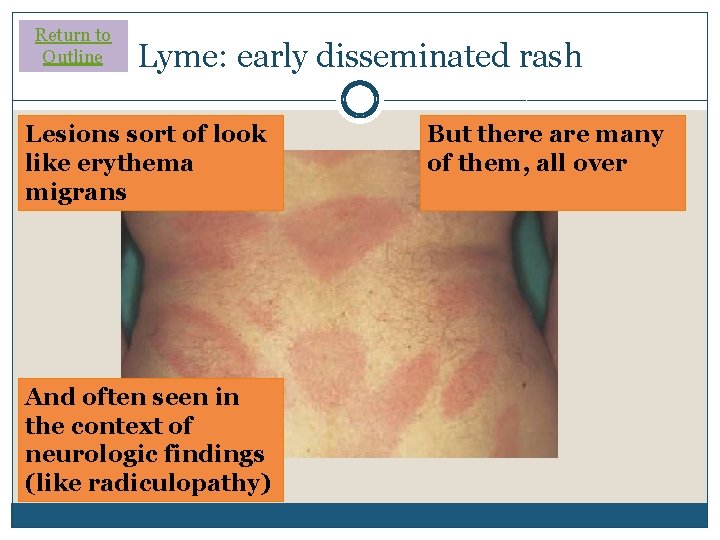
Return to Outline Lyme: early disseminated rash Lesions sort of look like erythema migrans And often seen in the context of neurologic findings (like radiculopathy) But there are many of them, all over

Lyme: early disseminated Spirochetemia �Try to say “spirochetemia” 5 times fast A bit hard, but this is what is happening �In one study, of 213 patients with early Lyme, B. burgdorferi spirochetes were found in the blood in 44% of cases �Although those with spirochetemia were more likely to have symptoms and have multiple lesions… 23% of them were asymptomatic �This is a slippery, hard to diagnose organism! Even disseminated disease does not always cause symptoms

Lyme: early disseminated Neurologic issues �Neurologic issues can occur early OR late in Lyme disease Usually weeks to several months…but can be days Common misconception CNS symptoms are only seen in late disease �Clinical picture is broad �Lymphocytic meningitis �Radiculopathies �Cranial nerve palsies Return to Outline

Lyme: early disseminated Neurologic issues Lyme Meningitis • Hard to distinguish from viral meningitis �Neurologic issues can occur early OR late in Lyme • Only 2% of Lyme disease meningitis cases have meningitis in Usually weeks to several months…but can be days isolation: usually Common misconception CNS symptoms are only seen in late other Lyme disease symptoms present • Diagnose with CSF �Clinical picture is broad antibodies and PCR �Lymphocytic meningitis • Sensitivity ~90%, so �Radiculopathies negative tests don’t �Cranial nerve palsies rule Lyme out if the clinical picture fits • However, there should be CSF lymphocytes > 5 in almost all cases

Lyme: early disseminated Neurologic issues Lyme Radiculopathy �Neurologic issues can occur early OR late in Lyme • Commonly missed form of early Usually weeks to several months…but can be days disseminated Lyme • ~3% of Lyme cases Common misconception CNS symptoms are only seen in late • Pain is quite disease prominent �Clinical picture is broad • Can look just like sciatica, or similar �Lymphocytic meningitis pain in a different �Radiculopathies region �Cranial nerve palsies • Often needs to be disease treated empirically in the right clinical context

Lyme: early disseminated Neurologic issues �Neurologic issues can occur early OR late in Lyme disease Usually weeks to several months…but can be days Common misconception CNS symptoms are only seen in late disease �Clinical picture is broad �Lymphocytic meningitis Cranial Nerve Palsy �Radiculopathies • CN 7 most common, causing Bell’s Palsy • One of only a few things that can cause bilateral Bells’ Palsy �Cranial nerve palsies

Lyme: early disseminated Cardiac �Lyme Carditis Occurs in early disseminated phase, about 1 -28 weeks after infection About 1% of Lyme cases get Lyme Carditis Fairly wide range of disease, from mild to deadly Frequency Palpitations Conduction abnormalities: 1 st to 3 rd degree AV block Pericarditis Myocarditis Left ventricular failure
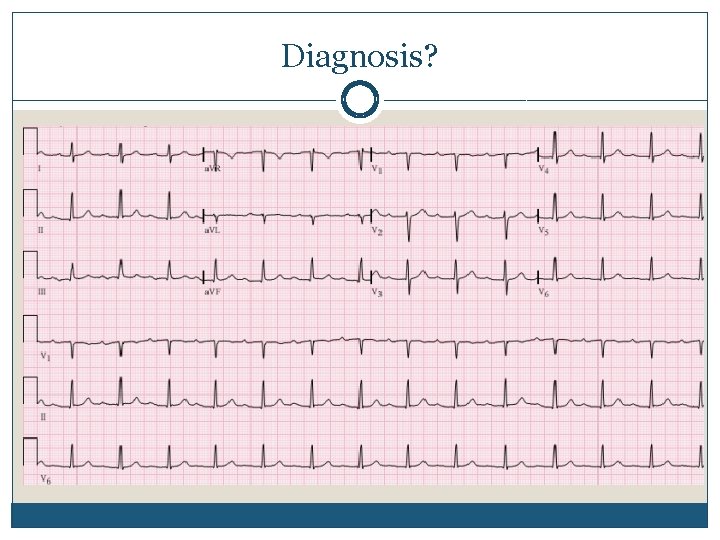
Diagnosis?
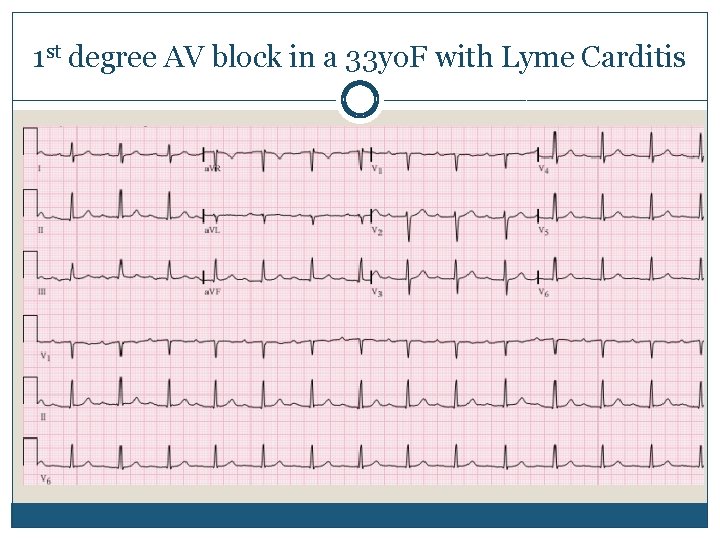
1 st degree AV block in a 33 yo. F with Lyme Carditis

Lyme: early disseminated Cardiac �Conduction delay 1 st to 3 rd degree Typically lasts 3 -42 days � Pacemaker is NOT indicated, even for high- degree block, as there should be improvement with treatment Patients may need a temporary pacer Return to Outline
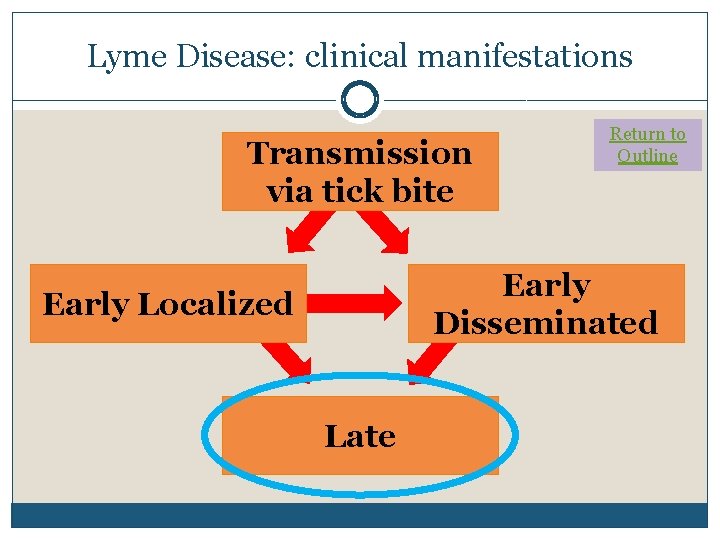
Lyme Disease: clinical manifestations Transmission via tick bite Return to Outline Early Disseminated Early Localized Late

Return to Outline Late Lyme �Occurs months to years after infection �Remember, many patients will be unaware of a tick bite, and only 80% get erythema migrans, so this may be the presenting symptom �Arthritis: usually 1 joint, though can be a few Usually the knee Eventually occurs in 60% of untreated patients �Chronic neurologic effects Peripheral neuropathy or encephalitis
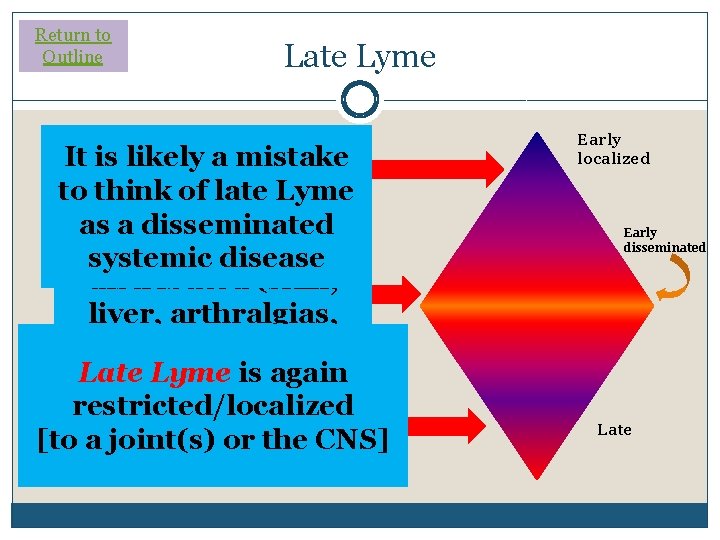
Return to Outline Late Lyme It is likely. Lyme a mistake Early is to think of late Lyme localized (mostly Early Disseminated as a disseminated to the skin) Lyme is widely systemic disease distributed (skin, liver, arthralgias, blood, CNS, heart) Late Lyme is again restricted/localized [to a joint(s) or the CNS] Early localized Early disseminated Late

Return to Outline Late Lyme: Arthritis �Monoarthritis of the knee is most common �Otherwise, large joints usually affected: shoulders, ankles, elbows �Large joint effusions are common; pain is actually relatively less common

Return to Outline Diagnosis of Lyme Disease �Diagnosis of Lyme Disease can be challenging �Pre-test probably, based on 1) exposure history to ticks and endemic areas; 2) symptoms and physical exam findings, is important to consider �There is also a lot of misinformation out there �Requires a combination of appropriate risk factors, appropriate symptoms, exam findings, and laboratory diagnosis
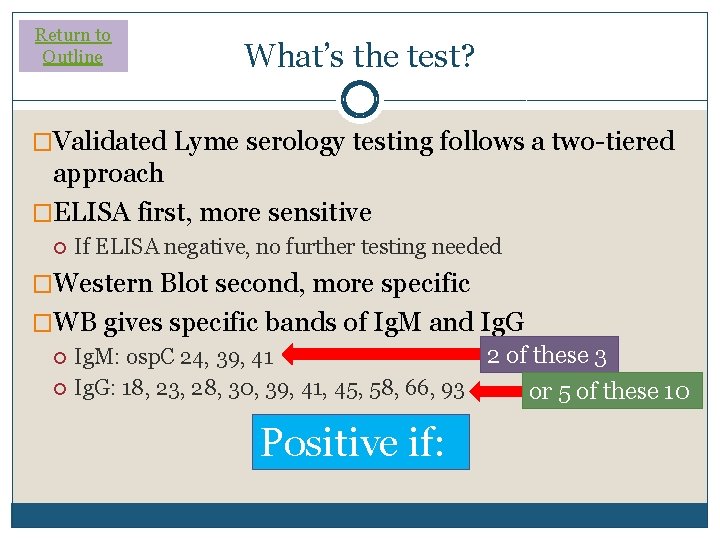
Return to Outline What’s the test? �Validated Lyme serology testing follows a two-tiered approach �ELISA first, more sensitive If ELISA negative, no further testing needed �Western Blot second, more specific �WB gives specific bands of Ig. M and Ig. G 2 of these 3 Ig. M: osp. C 24, 39, 41 Ig. G: 18, 23, 28, 30, 39, 41, 45, 58, 66, 93 Positive if: or 5 of these 10

Return to Outline More about Lyme Serologies � Why are we looking at so many bands? Why so complicated? Many of the bands are relatively non-specific and seen in other inflammatory states � Lyme Ig. M and Ig. G bands can remain positive for years “In the absence of specific clinical findings, Seeing Ig. M does not guarantee there is acute infection Lyme disease testing has a very low positive Re-infection diagnosis often has to be made clinically, or via chagning bands predictive value. Thus, the misattribution of � ~5% of the population in the Northeast US has a positive chronic symptoms to Lyme disease is an Lyme Serology at baseline! inevitable consequence of high-volume, low. In the absence of symptoms, a positive serology is of little clinical utility probability testing” It does NOT mean that the patient has chronic, undiagnosed infection - Paul Lantos. “Chronic Lyme Disease”. IDCNA 2015 � Don’t test unless there are symptoms consistent with Lyme Disease!

Misleading information about Lyme Serologies �If you take antibiotics early in the course, serologies will be negative This can happen. However, if it does, it’s because the infection is gone early…little need to worry about ongoing Lyme �Serologies are very insensitive If you want to learn more, check out This is DEFINITELY true early in the course of Lyme (at the EM stage) However, for late Lyme, they are highly sensitive When analyzed, such tests can have false-positive rates of >55% these articles: • False and Misleading Information �There are better tests out there about Lyme Disease There are many non-standardized, non-FDA approved tests • Chronic Lyme Disease performed at non-standardized laboratories

Diagnosis of Lyme Disease: Early Localized �Mostly a clinical diagnosis �Erythema migrans and exposure to an endemic area, with or without a tick exposure, is enough to make the diagnosis �Lyme serologies are likely to be negative this early About 25% of Lyme serologies will be positive at this phase �Repeat convalescent serologies in a few weeks should be positive Return to Outline

Diagnosis of Lyme Disease: Early Disseminated �Unlike early localized, in early disseminated Lyme, serologies are usually positive (80 -90% range) Cutaneous Early Disseminated • Clinical picture based on exam • Accompanied by fever, headache, arthralgias, LAD • If serology positive, that’s helpful, but not required • Repeat convalescent serology in a few weeks should be positive

Diagnosis of Lyme Disease: Early Disseminated �Unlike early localized, in early disseminated Lyme, serologies are usually positive (80 -90% range) Early Disseminated: Lyme Carditis • Consistent clinical picture • Usually accompanied by fever, headache, EM, arthralgias • Serology usually positive • Repeat convalescent serology in a few weeks should be positive

Diagnosis of Lyme Disease: Early Disseminated �Unlike early localized, in early disseminated Lyme, serologies are usually positive (80 -90% range) Early Disseminated: Neuro. Lyme • Consistent clinical picture • Serum serology almost always positive sensitive (90+%) • CSF serology reasonably sensitive • Should have lymphocytic CSF pleocytosis (mean 160 WBCs) • CSF PCR not sensitive, but quite specific

Diagnosis of Lyme Disease: Late �Serologies are nearly universally positive in late Lyme disease �A negative Lyme serology nearly-excludes the diagnosis Return to Outline

Return to Outline Study here Early localized: serology Early disseminated: sensitivities are not goodserology sensitivities are pretty good Late disease: serology sensitivities VERY good
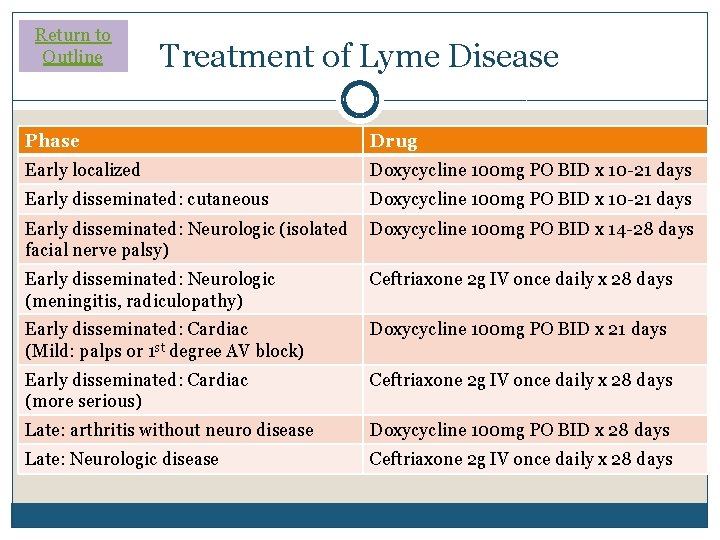
Return to Outline Treatment of Lyme Disease Phase Drug �IDSA guidelines (2006) exist Early localized Doxycycline 100 mg PO BID x 10 -21 days Early disseminated: cutaneous Doxycycline 100 mg PO BID x 10 -21 days Early disseminated: Neurologic (isolated Doxycycline 100 mg PO BID x 14 -28 days facial nerve palsy) Early disseminated: Neurologic (meningitis, radiculopathy) Ceftriaxone 2 g IV once daily x 28 days Early disseminated: Cardiac (Mild: palps or 1 st degree AV block) Doxycycline 100 mg PO BID x 21 days Early disseminated: Cardiac (more serious) Ceftriaxone 2 g IV once daily x 28 days Late: arthritis without neuro disease Doxycycline 100 mg PO BID x 28 days Late: Neurologic disease Ceftriaxone 2 g IV once daily x 28 days

Return to Outline Treatment of Lyme Disease �Alternative agents (for allergies or pregnancy) include amoxicillin and cefuroxime �Short (1 o day) vs longer (20 day) treatment for EM have similar outcomes from this study

Return to Outline Post-Lyme Disease Syndrome �After treatment for Lyme disease, a minority of patients (<10%) will have ongoing symptoms such as headache, fatigue, cognitive disability, and myalgias/arthralgias �This is termed Post-Lyme Disease Syndrome (PLDS) �The etiology is not well-established �However, extensive search for ongoing, active disease has been negative �Unfortunately, there is much misinformation that such symptoms represent ongoing “Chronic Lyme Disease, ” and require long courses of antibiotics This is not recommended

Return to Outline Want to learn more about the “Chronic Lyme Disease” issue? � MMWR Report on serious complication from “CLD treatment” � Review of unorthodox treatments used for CLD � General excellent review of problems with CLD � Cases of cancer misdiagnosed as CLD � Differentiating re-infection from “failed therapy” � NEJM critical appraisal of CLD � Is there validity to the “round body” idea? � Does 12 weeks of extra antibiotics work for post-Lyme disease symptoms? � ILADS is a prominent “alternative” group that, in the opinion of the authors, offers significant misinformation on Lyme and “chronic Lyme disease” and supports highly non-evidence based therapies that offer little benefit but evidence of harm

Take home on the “Chronic Lyme Issue” �“Even if CLD lacks biological legitimacy, its importance as a phenomenon can be monumental to the individual patient. This is because many if not most patients who believe they have this condition are suffering, in many cases for years. Many have undergone frustrating, expensive, and ultimately fruitless medical evaluations, and many have become quite disaffected with a medical system that has failed to provide answers, let alone relief. ” Lantos. “Chronic Lyme Disease”. IDCNA 2015

Return to Outline �Introduction �Lyme Disease �Anaplasma/Ehrlichia �Babesia �Assorted other TBI’s
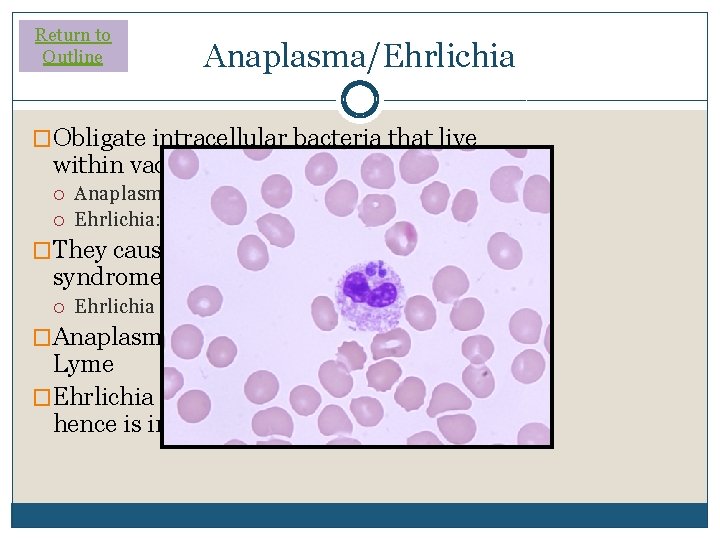
Return to Outline Anaplasma/Ehrlichia �Obligate intracellular bacteria that live within vacuoles in leukocytes Anaplasma: lives in neutrophils Ehrlichia: lives in monocytes �They cause a near-identical clinical syndrome Ehrlichia a bit worse / more dangerous �Anaplasma is spread by the same tick as Lyme �Ehrlichia is spread by a different tick (and hence is in a different geographic area)
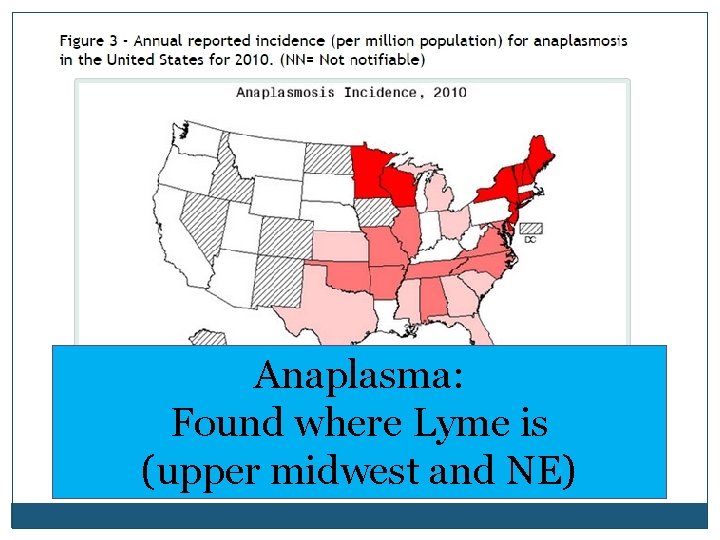
Anaplasma: Found where Lyme is (upper midwest and NE) cdc. gov
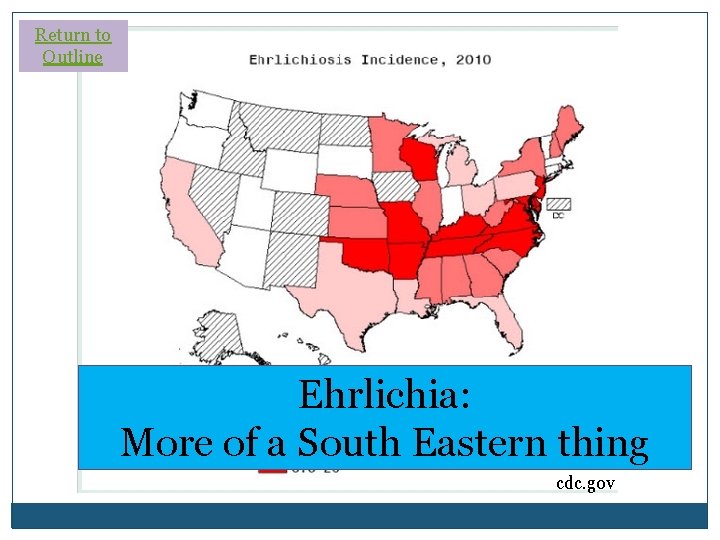
Return to Outline Ehrlichia: More of a South Eastern thing cdc. gov
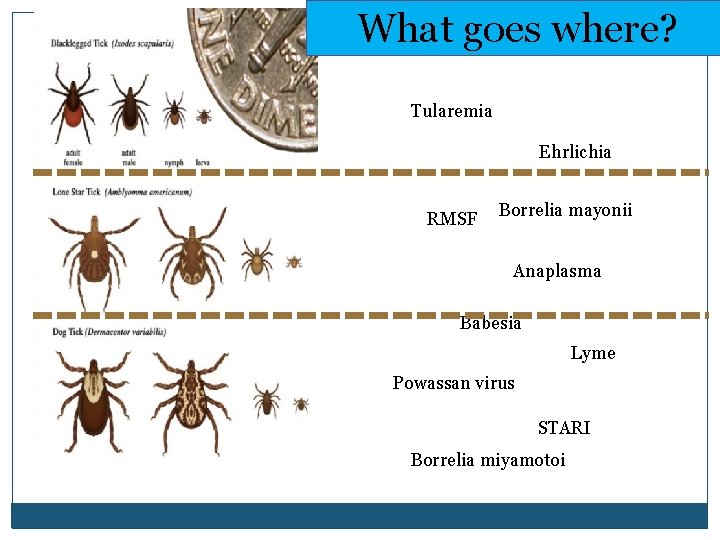
What goes where? Tularemia Ehrlichia RMSF Borrelia mayonii Anaplasma Babesia Lyme Powassan virus STARI Borrelia miyamotoi
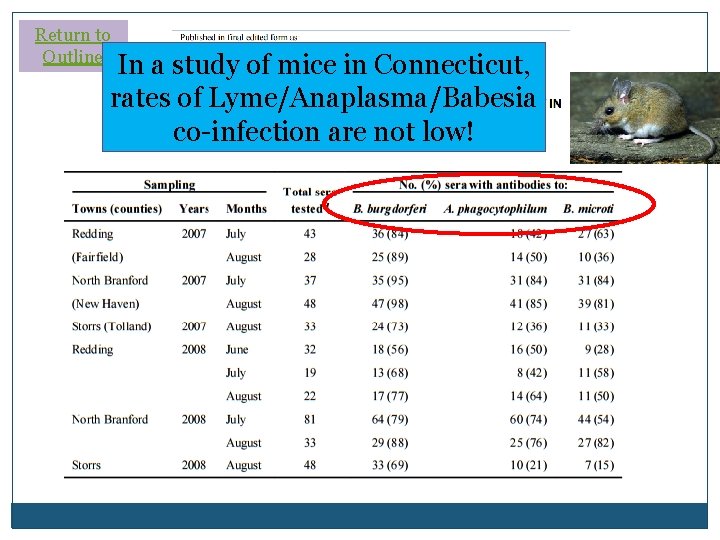
Return to Outline In a study of mice in Connecticut, rates of Lyme/Anaplasma/Babesia co-infection are not low!
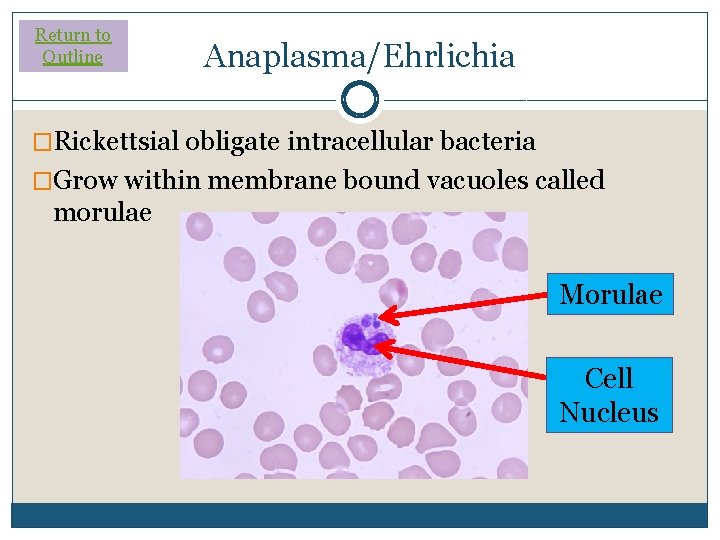
Return to Outline Anaplasma/Ehrlichia �Rickettsial obligate intracellular bacteria �Grow within membrane bound vacuoles called morulae Morulae Cell Nucleus
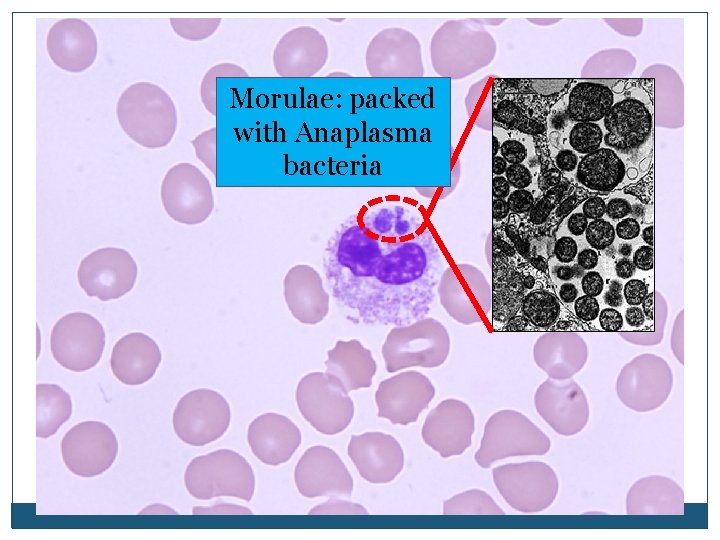
Morulae: packed with Anaplasma bacteria
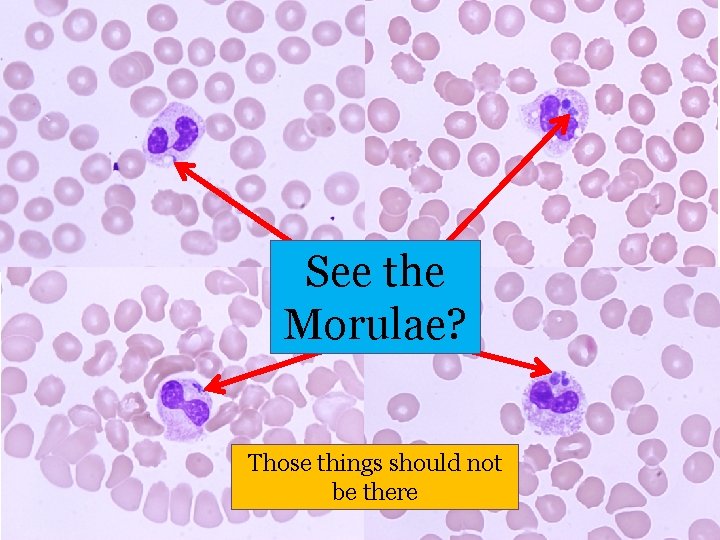
See the Morulae? Those things should not be there

Anaplasma: clinical presentation Fairly “flu like” And challenging to pick apart from Lyme Ehrlichia is similar, but more prominent headache and CNS findings Fever Myalgia Headache Cough 85% 73% 42% 30% Nausea/diarrhea Abdominal pain Rash Confusion 27% 18% 6% 3%

Diagnosing HME and HGA Ehrlichia Anaplasma Blood smear from the “Buffy Coat” layer is a nice way to look for morulae In the first week, PCR and smear best way to make the diagnosis In the second week, same After 3 weeks, serologies are very sensitive Return to Outline Dumler JS et al. CID 2007; 45: S 45

How Much Does the CBC Help? � Retrospective cross-sectional case study of 144 patients with Anaplasmosis and matched controls with another acute febrile illness.
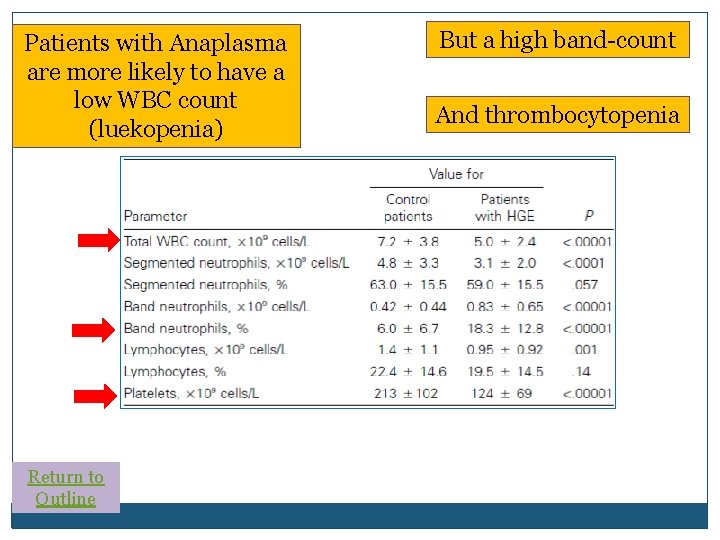
Patients with Anaplasma are more likely to have a low WBC count (luekopenia) Return to Outline But a high band-count And thrombocytopenia
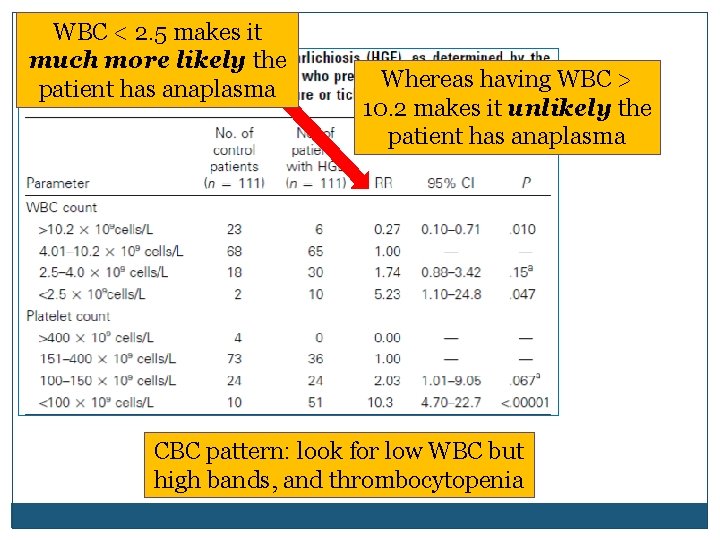

WBC < 2. 5 makes it much more likely the patient has anaplasma Whereas having WBC > 10. 2 makes it unlikely the patient has anaplasma CBC pattern: look for low WBC but high bands, and thrombocytopenia
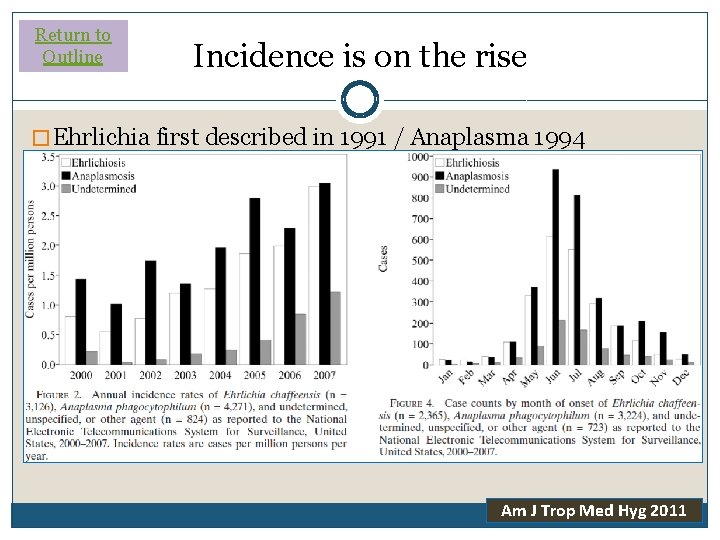
Return to Outline Incidence is on the rise � Ehrlichia first described in 1991 / Anaplasma 1994 � Case rate 3 x higher between 2000 2007 Mortality rate 0. 5 -2% and hospitalization rate 35 -50% Case rates highest in summer (June-August = 62%) Highest % of cases in the 60 -69 yr decade Ehrlichia: “life-threatening complications” = 9. 2% Anaplasmosis: “life-threatening complications” = 3. 0% Am J Trop Med Hyg 2011
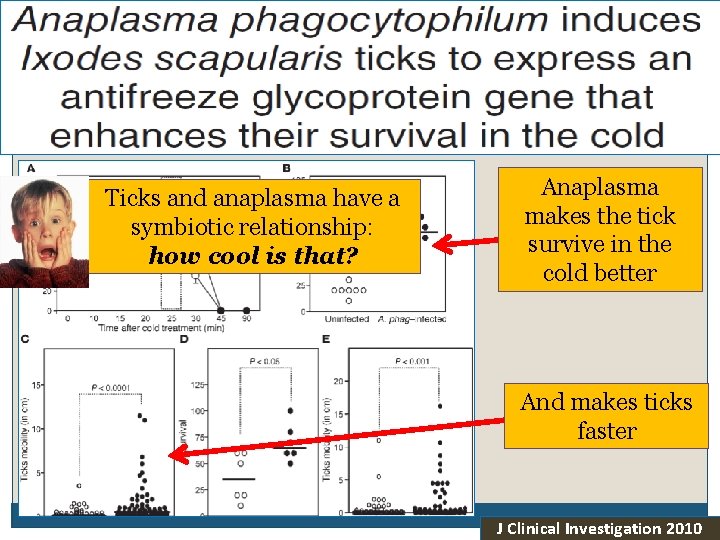
Thoughts on Evolution Ticks and anaplasma have a symbiotic relationship: how cool is that? Anaplasma makes the tick survive in the cold better And makes ticks faster J Clinical Investigation 2010

Treatment of Anaplasma/Ehrlichia Very similar to Lyme Disease! Doxycycline will get both very well Return to Outline Wormser GP et al. CID 2006. 43: 1089 Dumler JS et al. CID 2007; 45: S 45

Return to Outline �Introduction �Lyme Disease �Anaplasma/Ehrlichia �Babesia �Assorted other TBI’s
Return to Outline Babesia “The Malaria of New England”
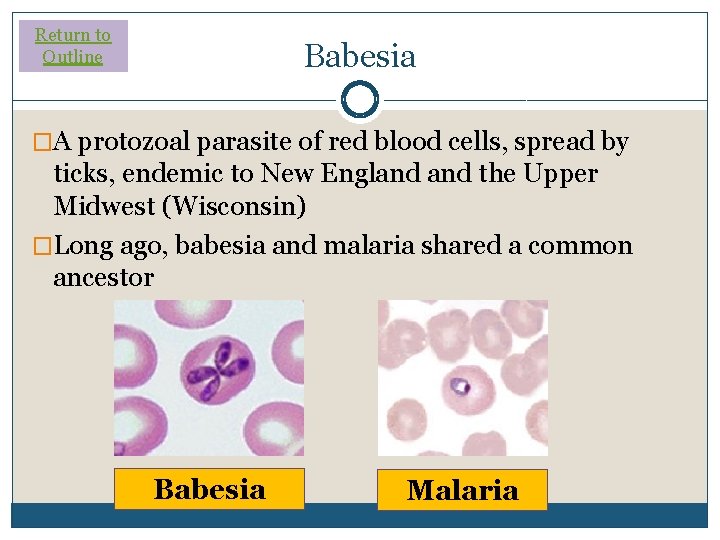
Return to Outline Babesia �A protozoal parasite of red blood cells, spread by ticks, endemic to New England the Upper Midwest (Wisconsin) �Long ago, babesia and malaria shared a common ancestor Babesia Malaria
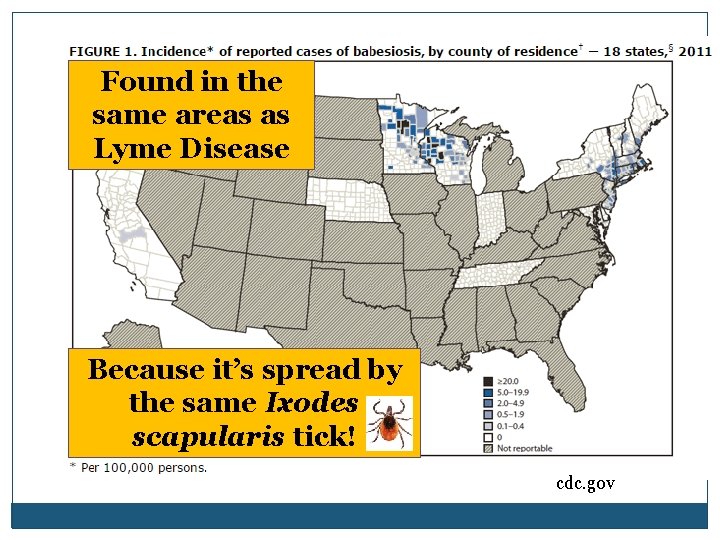
Found in the same areas as Lyme Disease Because it’s spread by the same Ixodes scapularis tick! cdc. gov

Return to Outline Babesia pathogenesis �The babesia protozoa divides by binary fission �Thus you will always see factors of 2 (either 1, 2, or 4 protozoa in each cell) �When 4 protozoa line up nicely, it’s called a “Maltese Cross” �Eventually, protozoa will rupture the RBC, causing hemolysis �The spleen is hugely important for clearing infected RBC’s out of circulation

Babesia pathogenesis: all about that parasitemia �How sick one gets depends on the parasite burden in the blood �Severe disease tends to occur when >4% of RBCs are infected �In patients with a functional spleen, parasitemia ranges 1 -20% Most cases have <1% parasitemia �In asplenic patients, parasitemia has been described as high as 80% and babesia is MUCH more fulminant and deadly

Case Return to Outline A 65 year-old man is seen in your office for fever and headache that has been present for the last 2 days. For the past month he had been on Nantucket Island, MA with his two grandsons who had returned from Nigeria. He was in his usual excellent health until 5 weeks ago when he developed a non-pruritic, erythematous, 10 cm circular skin lesion on the his left thigh (ten days after he returned from Nantucket) He was seen by his physician who prescribed doxycycline for 21 days.
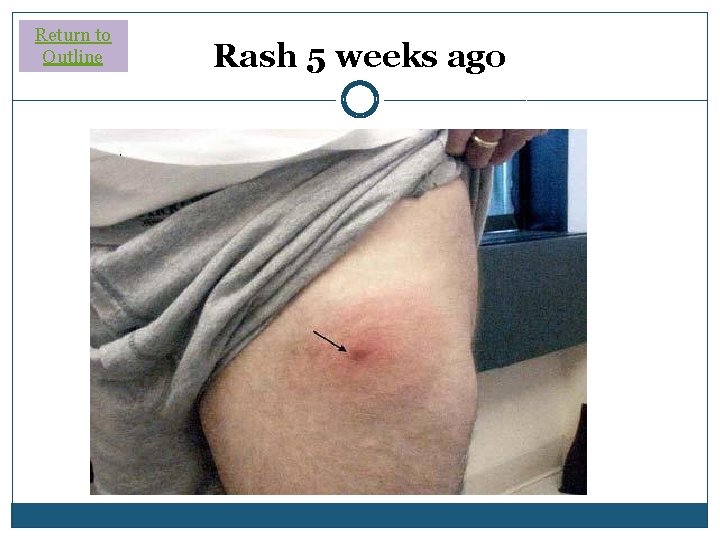
Return to Outline Rash 5 weeks ago
Return to Outline Case continued � The rash on his leg resolved after 6 days of antibiotics and he felt well until 2 days ago when he began to feel feverish. Over the past 48 hours he has had chills, fever, marked fatigue and loss of appetite. A mild headache which began two days ago has worsened so that he does not feel able to go to work. On physical examination temperature is 101. 4 F, pulse 100/min, blood pressure 112/68 mm Hg, respirations 14/min. He is mildly uncomfortable because of the headache but nontoxic appearing. There is no rash. The neck is not stiff.

Return to Outline Case continued � Laboratory studies reveal WBC 6, 100, Hgb 11. 8, Hct 36, platelets 102, 000, bilirubin 1. 6, AST 92, ALT 106, and LDH 368. Glucose, electrolytes, BUN and creatinine are normal. � What do you think is going on? Yes, it’s babesiosis! Are you surprised he got sick 5 weeks after his initial Lyme erythema migrans was found and treated?
Return to Outline Babesiosis: clinical features �Incubation period can be 1 -12 weeks! �Babesia is divided into: • • • • • Risk Mild factors Disease for Usually, <4% parasitemia Severe Disease Fever (often quite high, like Asplenia >103 F) (!!!!!) HIV Fatigue/weakness TNFa blockers Headache Rituximab Arthralgia N/V Educate these Diarrhea patients Dark urinewho live in Hemolytic anemia endemic areas to Thrombocytopenia, recognize and avoid transaminitis ticks/babesia! Severe Disease • • Usually, >4%, especially > 10% parasitemia Same signs/symptoms as mild, but worse ARDS DIC CHF Renal failure Splenic rupture Hgb < 10
Return to Outline Babesiosis: clinical features �Incubation period can be 1 -12 weeks! �Babesia is divided into: Mild Disease • Should be treated if found, but often selfresolves in 7 -10 days in immunocompetent hosts Severe Disease • Always needs treatment, sometimes quite aggressive (more to come)

Return to Outline Co-Infection �Be VERY aware that a patient with babesia likely has a co-infection �Need a reminder of what diseases are spread by the same ticks?
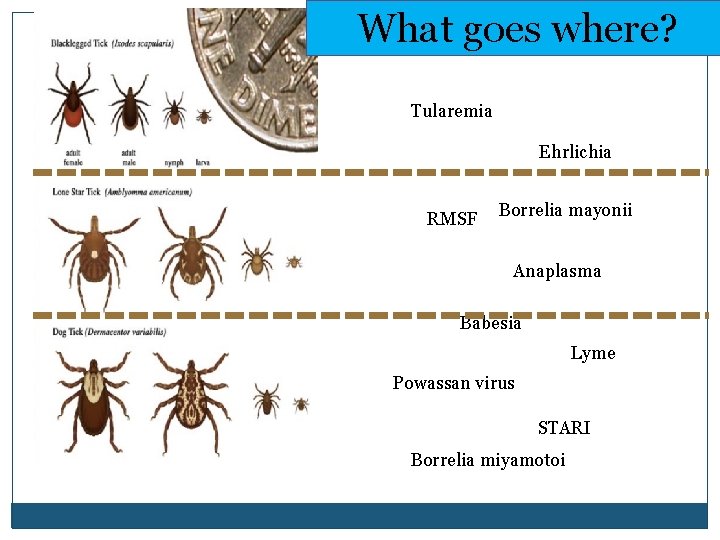
What goes where? Tularemia Ehrlichia RMSF Borrelia mayonii Anaplasma Babesia Lyme Powassan virus STARI Borrelia miyamotoi

Return to Outline Co-Infection �Be VERY aware that a patient with babesia likely has a co-infection �In one report, two-thirds (!) of patients with babesia were co-infected with Lyme And one-third were co-infected with anaplasma �Consider an empiric 10 -21 day course of doxycycline for any patient with proven babesiosis Note that the opposite is not true: if a patient has Lyme, risk of co-infection is only ~5%, so would prove Babesia before treating for it, if clinically suspected

Return to Outline Diagnosing babesiosis �Available tests Blood parasite smear Babesia PCR Babesia serology � Send ‘em all?
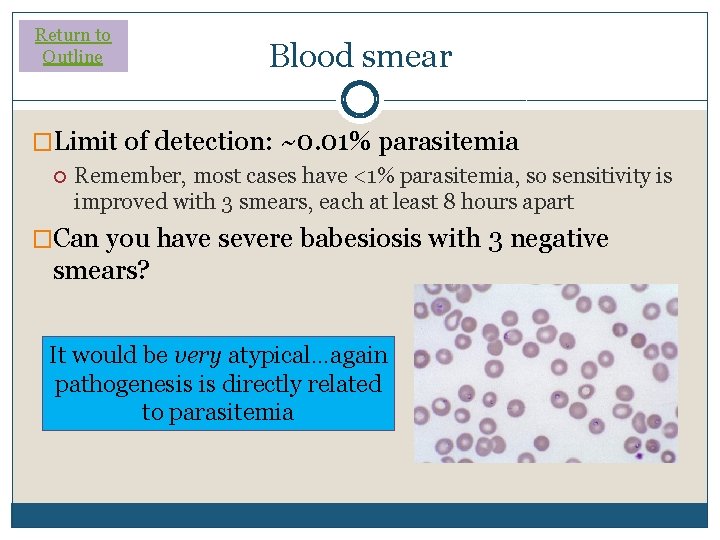
Return to Outline Blood smear �Limit of detection: ~0. 01% parasitemia Remember, most cases have <1% parasitemia, so sensitivity is improved with 3 smears, each at least 8 hours apart �Can you have severe babesiosis with 3 negative smears? It would be very atypical…again pathogenesis is directly related to parasitemia

Return to Outline Babesia PCR �Can detect %0. 0001 parasitemia �Much more sensitive (~thousand-fold!) than smear In fact, it is so sensitive, we are seeing patients with asymptomatic, very low level parasitemia during blood donation �Best used to diagnose mild cases with low level parasitemia, or to screen the blood supply Best to get the blood smears first, use PCR only if suspicion high but smears negative If smear negative, parasitemia is going to be low, and thus patient in a lower-risk setting

Xenodiagnosis: inject a hamster with blood from a patient and see if the hamster gets babesia! Works reasonably well! But a bit burdensome to do…and sad hamsters…so not really done

Return to Outline Babesia serology �Often negative first 1 -2 weeks of symptoms Note similarity to Lyme and Anaplasma serologies �Almost always positive by 3 -4 weeks of symptoms Again, note similarity to other tick-borne infections

Return to Outline Diagnosing babesiosis �Available tests Blood parasite smear Babesia PCR Babesia serology � Send ‘em all? Risk factors for severe disease: smear x 3 and PCR Clinical picture of severe disease: smear x 3 Clinical picture of mild disease: smear x 3 +/- PCR Serologies: send a few weeks after symptoms to see if you were right.
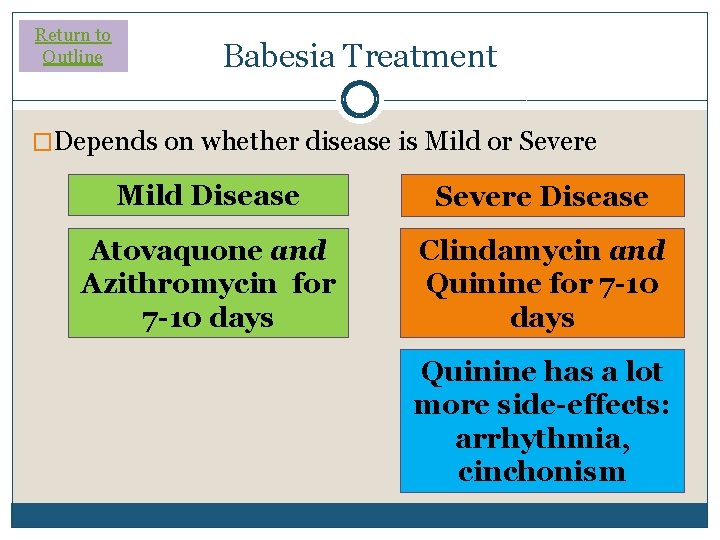
Return to Outline Babesia Treatment �Depends on whether disease is Mild or Severe Mild Disease Severe Disease Atovaquone and Azithromycin for 7 -10 days Clindamycin and Quinine for 7 -10 days Quinine has a lot more side-effects: arrhythmia, cinchonism

Classic paper on this Both combinations worked equally well, but patients with severe disease were excluded That said, side-effects much higher in clinda/quinine group

�Criticisms Classic paper on this Excluded patients with severe symptoms (DIC, CHF, splenic rupture) Parasitemia average was low: 0. 5% (range 0. 05 -12%) So for severe disease, we don’t really know which is better, and clinda/quinine is standard, so that is still used Return to Outline
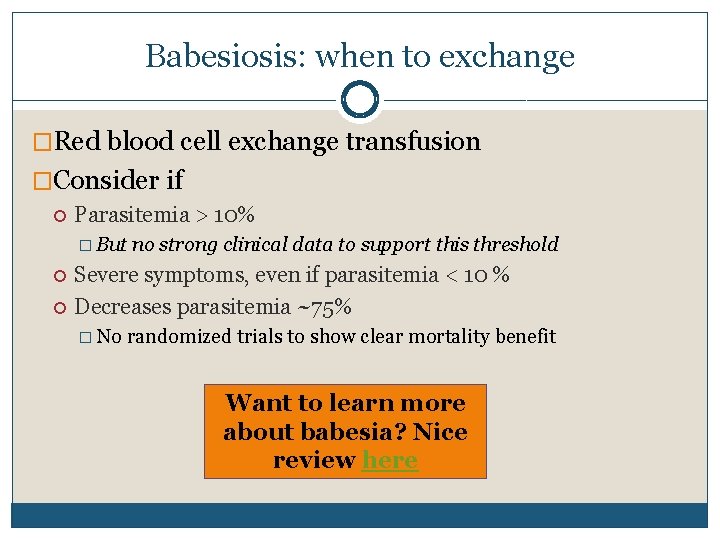
Babesiosis: when to exchange �Red blood cell exchange transfusion �Consider if Parasitemia > 10% � But no strong clinical data to support this threshold Severe symptoms, even if parasitemia < 10 % Decreases parasitemia ~75% � No randomized trials to show clear mortality benefit Want to learn more about babesia? Nice review here

Return to Outline �Introduction �Lyme Disease �Anaplasma/Ehrlichia �Babesia �Assorted other TBI’s

Return to Outline Other Tick Borne Illnesses �Powassan Virus �Atypical Borrelia species �Rocky Mountain Spotted Fever �Others (up-to-date link from the CDC)

Return to Outline Powassan Virus �Newly described in 2006 �Tick born illness �Incubation period 7 -28 days �Causes meningitis and encephalitis � 10% case fatality rate �½ of survivors have neurologic sequelae �Testing available through state labs �No treatment or vaccine Source: https: //www. cdc. gov/powassan/statistics. html
Return to Outline Atypical Borrelia species Borrelia miyamotoi Borrelia mayonii �Found in 1995 in Japan �Found in February 2016 in Minnesota and Wisconsin 2001 �Rash is more diffuse, �More joint pain, less otherwise similar to rash than in B. Lyme burgdorferi �Unknown number of US �Unknown number of cases in US cases �Treatment same as Lyme disease �Found in Conn. , USA in
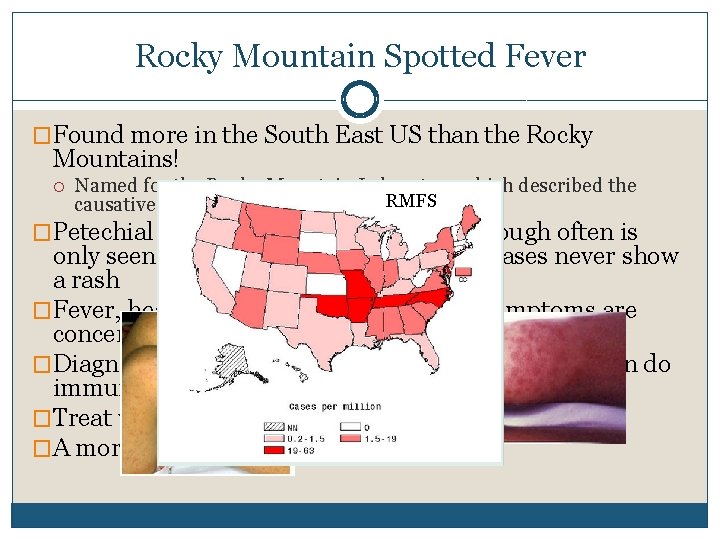
Rocky Mountain Spotted Fever �Found more in the South East US than the Rocky Mountains! Named for the Rocky Mountain Laboratory which described the causative agent, Rickettsia ricketisii. RMFS �Petechial rash is the classic symptom, though often is only seen late in the course, and 10% of cases never show a rash �Fever, headache, Pulmonary, and CNS symptoms are concerning. Untreated case fatality 20 -80% �Diagnosis made clinically, with serologies, or you can do immunostaining or PCR of skin biopsy samples �Treat with doxycycline �A more thorough review is here

Congratulations on finishing the Tick-borne Illness Module! �Please take this brief pre-module quiz https: //goo. gl/forms/Gpvlbqu. ICT 3 Vzkc. H 3 Return to Outline
- Slides: 98