Thyroid Physiology and Thyroiditis Heidi Chamberlain Shea MD

Thyroid Physiology and Thyroiditis Heidi Chamberlain Shea, MD Endocrine Associates of Dallas

Case Presentation 23 year old female n n G 2 P 2 6 months post partum Palpitations that were intermittent for a couple of weeks and now resolved Now with 1 month of increased fatigue, hair loss and 10 pound weight gain

Case Presentation What is her diagnosis? Tests that should be done? Pathophysiology of her disease process?
Thyroid Trivia “Bronchocele” n Greek for tracheal outpouch 1500 AD described by Leonardo da Vinci 1656 AD “thyroid” n n Thomas Wharton Shield shaped cartilage
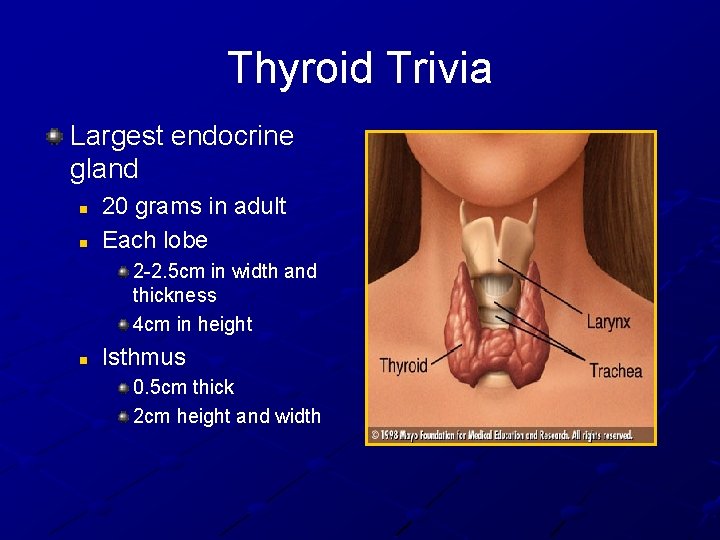
Thyroid Trivia Largest endocrine gland n n 20 grams in adult Each lobe 2 -2. 5 cm in width and thickness 4 cm in height n Isthmus 0. 5 cm thick 2 cm height and width
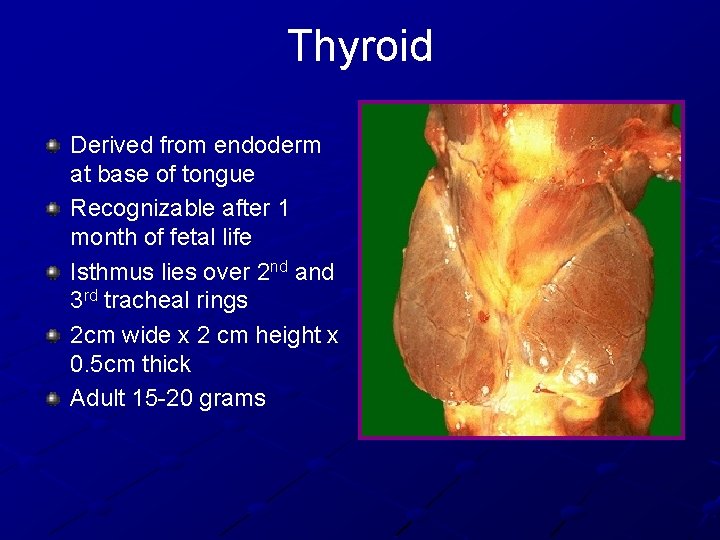
Thyroid Derived from endoderm at base of tongue Recognizable after 1 month of fetal life Isthmus lies over 2 nd and 3 rd tracheal rings 2 cm wide x 2 cm height x 0. 5 cm thick Adult 15 -20 grams

Thyroid Largest of the endocrine glands Blood flow 5 x the weight of the gland/minute Hormones produced n n 93% thyroxine (T 4) 7% triiodothyronine (T 3) 4 x the potency of thyroxine Responsible for the basal metabolic rate n n Deficiency = 40 -50% fall in metabolic rate Excess = 60 -100% increase in metabolic rate
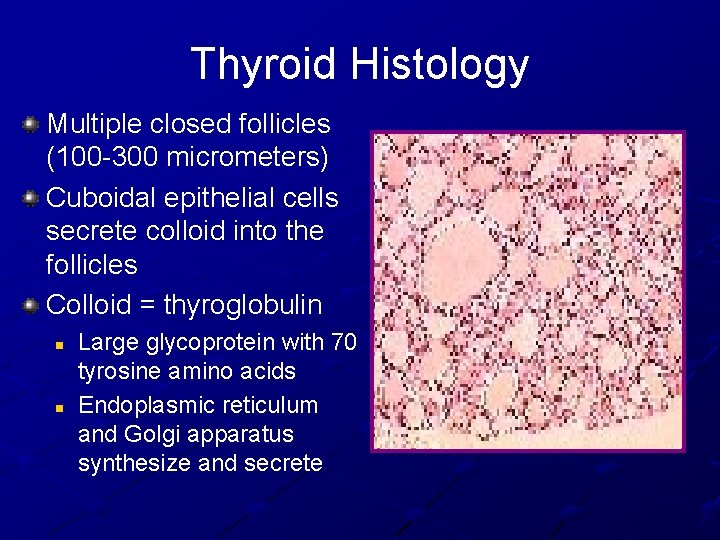
Thyroid Histology Multiple closed follicles (100 -300 micrometers) Cuboidal epithelial cells secrete colloid into the follicles Colloid = thyroglobulin n n Large glycoprotein with 70 tyrosine amino acids Endoplasmic reticulum and Golgi apparatus synthesize and secrete
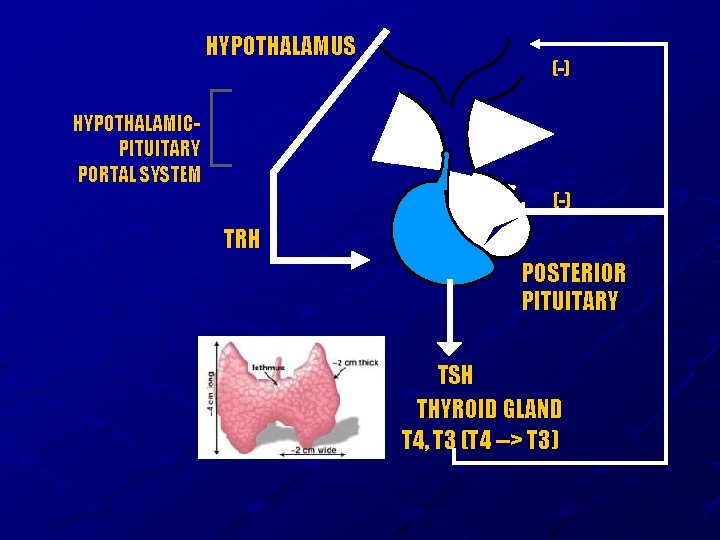
HYPOTHALAMUS (-) HYPOTHALAMICPITUITARY PORTAL SYSTEM (-) TRH (+) ANTERIOR PITUITARY POSTERIOR PITUITARY TSH THYROID GLAND T 4, T 3 (T 4 --> T 3)

TRH Produced by Hypothalamus Release is pulsatile, circadian Downregulated by T 4, T 3 Travels through portal venous system to adenohypophysis Stimulates TSH formation

TSH Produced by Adenohypophysis Thyrotrophs Upregulated by TRH Downregulated by T 4, T 3 Travels through portal venous system to cavernous sinus, body. Stimulates several processes n n n Iodine uptake Colloid endocytosis Growth of thyroid gland

Thyroid Physiology Uptake of Iodine by thyroid Coupling of Iodine to Thyroglobulin Storage of MIT / DIT in follicular space Re-absorption of MIT / DIT Formation of T 3, T 4 from MIT / DIT Release of T 3, T 4 into serum Breakdown of T 3, T 4 with release of Iodine

Thyroid and Iodine 50 mg of iodides are needed per year n n 1 mg/week Iodized salt 1 part Na iodide to 100, 000 parts Na. Cl Iodides are ingested and oxidized to iodine in the thyroid n n Nascent iodine(Io) or I 3 Peroxidase enzyme (hydrogen peroxide) 1/5 of ingested iodine utilized for hormone synthesis
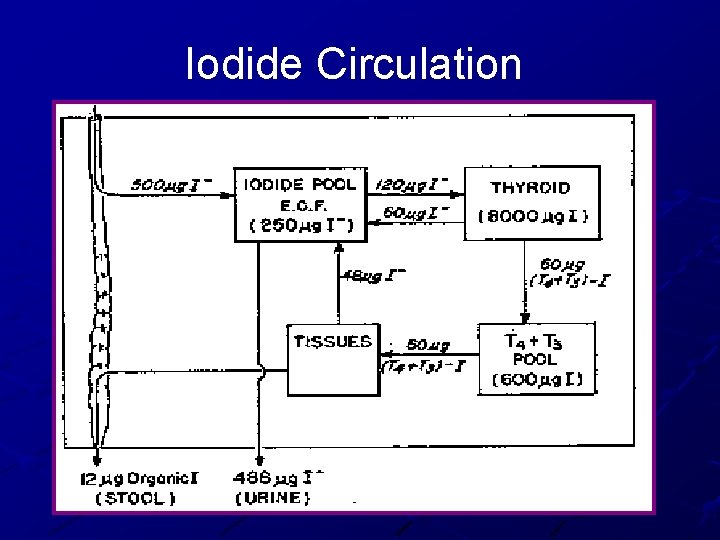
Iodide Circulation
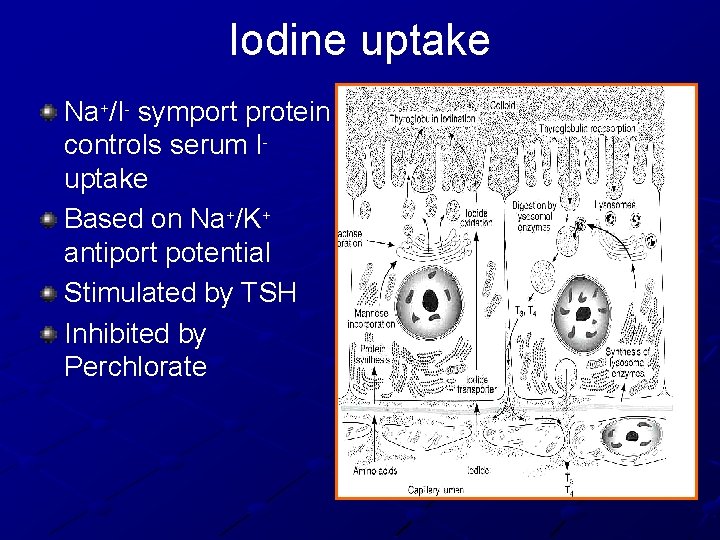
Iodine uptake Na+/I- symport protein controls serum Iuptake Based on Na+/K+ antiport potential Stimulated by TSH Inhibited by Perchlorate

Iodide Pump Thyroid gland actively pumps iodide into the cell via the basal membrane (iodide trapping) n n Iodide 30 x the concentration of blood Able to concentrate to 250 x the concentration in blood Rate of iodide trapping n TSH dependent

Thyroid Hormone Synthesis Tyrosine backbone Iodine n Iodinase enzyme (enzyme I) attaches iodine to thyroglobulin Number of iodines determine activity of thyroid hormone n n Thyroxine (4 iodines) Triiodothyronine (3 iodines)

MIT / DIT Formation Thyroid Peroxidase (TPO) n n Apical membrane protein Catalyzes iodide oxidation to reactive iodine Binds to Tyrosine residues of Thyroglobulin n n Antagonized by thionamides Coupling enzyme MIT with DIT= T 3 Two DIT’s= T 4 Pre-hormones secreted into follicular space

Transport of T 3 and T 4 When in circulation n 93% thyroxine and 7% triiodothyronine Conversion to active (T 3) is by slow deiodination process 99% of T 4 and T 3 bound to plasma proteins Causes slow release of hormone to tissue Thyroxine-binding globulin (TBG) Tyroxine-binding prealbumin and albumin

Secretion of Thyroid Hormone Stimulated by TSH Endocytosis of colloid on apical membrane Coupling of MIT & DIT residues n n n Catalyzed by TPO MIT + DIT = T 3 DIT + DIT = T 4 Hydrolysis of Thyroglobulin Release of T 3, T 4 Release inhibited by Lithium
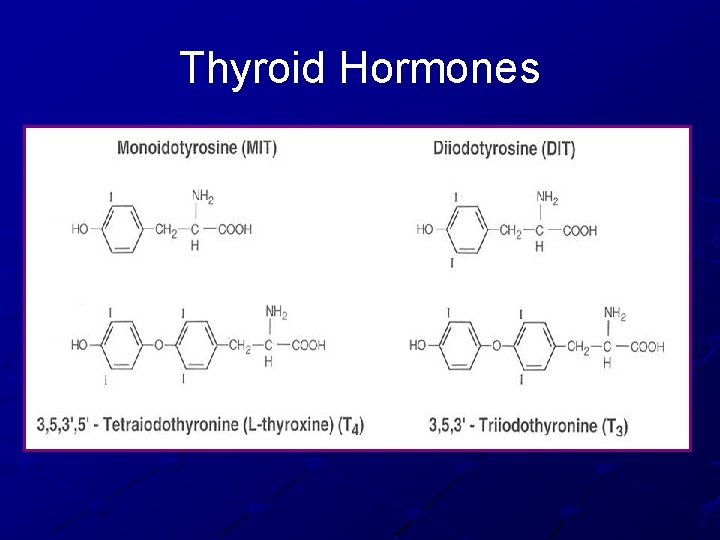
Thyroid Hormones
Thyroglobulin Storage Thyroglobulin molecule n n 30 thyroxine molecules Few triiodothyronine Sufficient supply for 2 -3 months Deiodinase enzyme recycles iodine when thyroglobulin utilized

Thyroid Hormone Metabolic effect of thyroxine noticed 2 -3 days after release Steady state of thyroid hormone 10 -12 days after ingestion Half life of 15 days Due to steady state, thyroid hormone is typically adjusted every 4 -6 weeks n Check T 4 vs. TSH in the short term assessment

Thyroid Hormone n Majority of circulating hormone is T 4 98. 5% T 4 1. 5% T 3 n Total Hormone load is influenced by serum binding proteins Thyroid Binding Globulin 70% Albumin 15% Transthyretin 10% n Regulation is based on the free component of thyroid hormone

Hormone Binding Factors Increased TBG n n High estrogen states (pregnancy, OCP, HRT, Tamoxifen) Liver disease (early) Decreased TBG n n Androgens or anabolic steroids Liver disease (late) Binding Site Competition n NSAID’s Furosemide IV Anticonvulsants (Phenytoin, Carbamazepine)
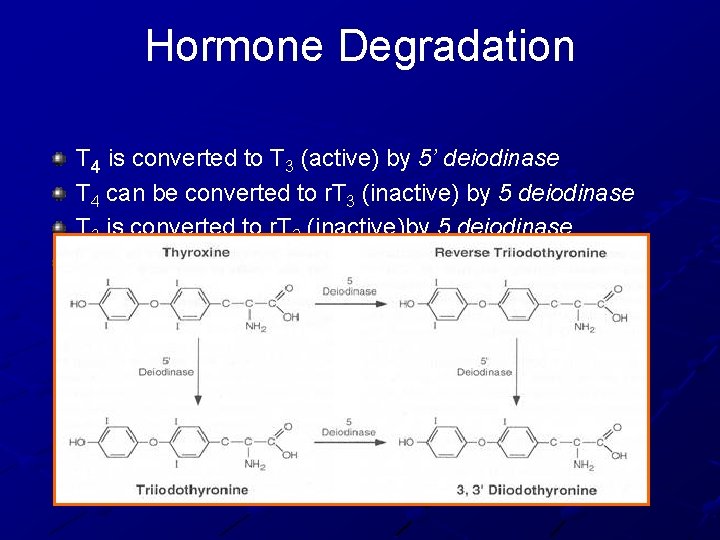
Hormone Degradation T 4 is converted to T 3 (active) by 5’ deiodinase T 4 can be converted to r. T 3 (inactive) by 5 deiodinase T 3 is converted to r. T 2 (inactive)by 5 deiodinase r. T 3 is inactive but measured by serum tests

Hypothyroidism Symptoms Nervous system n n n Forgetfulness and mental slowing Paresthesias Carpal tunnel Ataxia and decreased hearing Tendon jerk slowed with prolonged relaxation phase Cardiovascular n n n Bradycardia Decreased cardiac output Pericardial effusion Reduced voltage on EKG and flat T waves Dependent edema

Hypothyroidism Symptoms Gastrointestinal n n n Constipation Achlorhydria with pernicious anemia Ascitic fluid with high protein Renal n Reduced excretion of water load Hyponatremia n Decreased renal blood flow and glomerular filtration Pulmonary n n Responses to hypoxia and hypercapnia are decreased Pleural effusions high protein Musculoskeletal n n Arthralgia Joint effusions Muscle cramps CK can be elevated Anemia n n Normochromic normocytic Megaloblastic Pernicious anemia

Hypothyroidism Symptoms Skin and hair n n n Loss of lateral eye brows Dry, cool skin Facial features Coarse and puffy n Orange skin Metabolism n n n Carotene Decreased lipoprotein receptors Reproductive system n n Menorrhagia from anovulatory cycles Hyperprolactinemia No inhibition of thyroid hormone Hypothermia Intolerance to cold Increased cholesterol and triglyceride n Weight gain

Thyroid Hormone Metabolic effect of thyroxine noticed 2 -3 days after release Steady state of thyroid hormone 10 -12 days after ingestion Half life of 15 days Due to steady state, thyroid hormone is typically adjusted every 4 -6 weeks n Check T 4 vs TSH in the short term assessment

Hypothyroidism Etiologies Thyroiditis Thyroid ablation External radiotherapy Pharmacologic agents Infiltrative disorders Embryologic variants
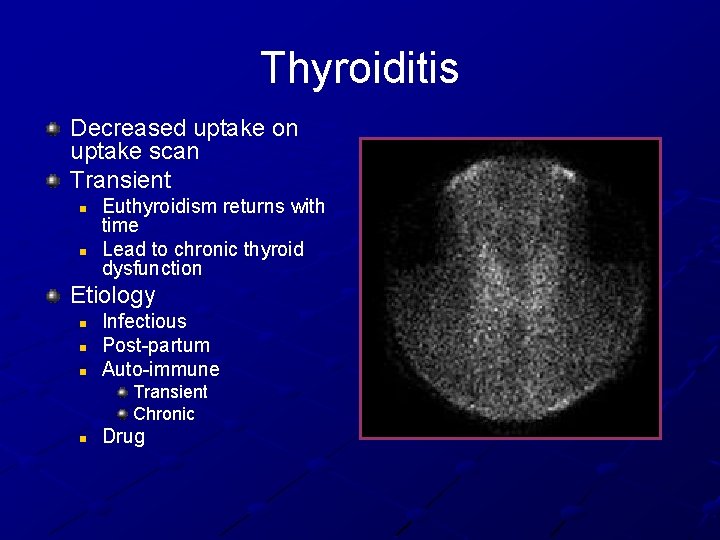
Thyroiditis Decreased uptake on uptake scan Transient n n Euthyroidism returns with time Lead to chronic thyroid dysfunction Etiology n n n Infectious Post-partum Auto-immune Transient Chronic n Drug

Thyroiditis Thyrotoxic phase n n Short phase Increased T 3 and T 4 Symptoms of hyperthyroidism Thionamides not effective Thyroid synthesis low n Can use beta-blockers Hypothyroid phase n n n Transient or permanent Symptomatic patients need replacement Can check for recovery with stopping after 3 -6 months
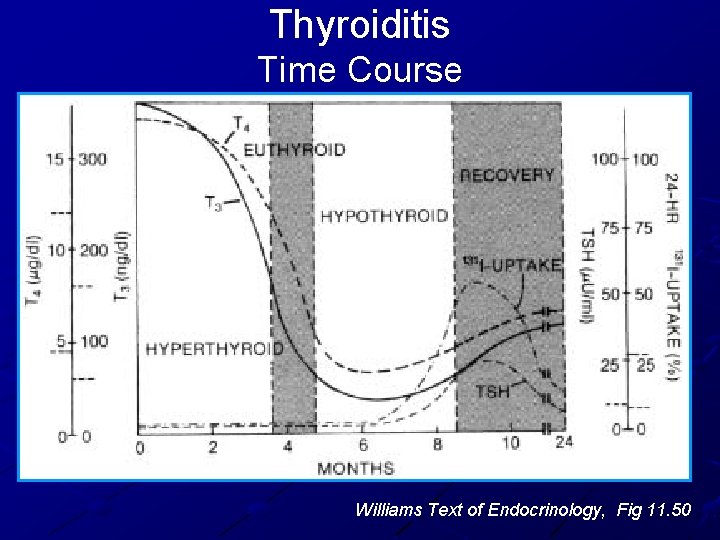
Thyroiditis Time Course Williams Text of Endocrinology, Fig 11. 50

Infectious Thyroiditis Etiology n n n Bacterial 90% Fungal Mycobacterial Parasitic Syphilitic Symptoms n n Thyroid pain and tenderness Fever Dysphagia Dysphonia Treatment n Treat the infection
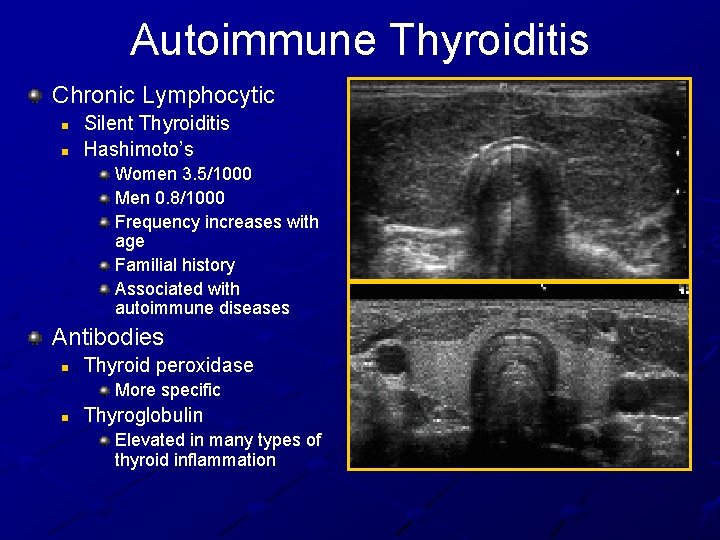
Autoimmune Thyroiditis Chronic Lymphocytic n n Silent Thyroiditis Hashimoto’s Women 3. 5/1000 Men 0. 8/1000 Frequency increases with age Familial history Associated with autoimmune diseases Antibodies n Thyroid peroxidase More specific n Thyroglobulin Elevated in many types of thyroid inflammation

Thyroiditis Postpartum thyroiditis n n 2 -21% of pregnancies Can occur up to one year post partum Usually transient and returns to euthyroid state Treat Hypothyroidism Symptoms with ‘hyperthyroidism’ Presence of TPO AB increases risk of long term hypothyroidism

Transient/Destructive Thyroiditis Subacute n n n 20% of thyrotoxic cases De Quervain’s thyroiditis Giant cell thyroiditis Pseudogranulomatous thyroiditis Subacute painful thyroiditis Symptoms n n Pain Fever Increased ESR Hoarseness or dysphagia Treatment n n ASA, NSAID Steroid rarely

Comparison of Thyroiditis Characteristic Silent thyroiditis Subacute thyroiditis Age of onset (yr) 5 -93 20 -60 Sex ratio (F: M) 2: 1 5: 1 Etiology Autoimmune Viral Pathology Lymphocytic infiltration Giant cells, granulomas Prodrome Pregnancy Viral illness Goiter Non-painful Painful Fever/malaise No Yes TPO/thyroglobulin AB High and rising Low, absent or transient ESR Normal High RAIU <5% Relapse Common Rare Permanent hypothyroidism Common Infrequent

Drug Induced Thyroid Dysfunction Lithium n n n Inhibits thyroid hormone secretion Hypothyroidism 3. 4% prevalence Interferon-α n n n Hyper/Hypothyroidism Transient thyroiditis TPO AB increases risk of thyroid dysfunction Interleukin-2 Aminoglutethimide Ethionamide Sulfonamides

Drug Induced Thyroid Dysfunction Amiodarone n n n 75 mg iodine/200 mg Hypothyroidism Thyrotoxicosis Type I and Type II n Increased blood flow vs. decreased blood flow Not responsive to thionamides

Hypothyroidism Infiltrative Disorders Amyloidosis Sarcoidosis Hemochromatosis Cystinosis Pneumocystis carinii Lymphoma Riedel’s thyroiditis n n n Invasive Fibrous Thyroiditis Thyroid tissue replaced by fibrous tissue Rapidly enlarging neck mass Compressive symptoms Surgical removal Steroids and tamoxifen

Thyroid Hormone Replacement 1. 3 ug/kg/day n 75 -100 ug per day Elderly or patients with angina n 12. 5 -25 ug/day Carefully increase every month IV dosing n Use 60% of oral dose Levothyroxine n n n Synthroid Levoxyl Unithroid Armour Thyroid n n n T 3/T 4 preparation Dessicated pig thyroid Not a consistent amount of T 3/T 4 Most T 3 preparations give higher than 1: 11 ratio of T 3: T 4

Case Presentation 23 year old female n n G 1 P 1 6 months post partum Palpitations that were intermittent for a couple of weeks and now resolved Now with 1 month of increased fatigue, hair loss and 10 pound weight gain

Case Presentation What is her diagnosis? n Post partum thyroiditis Tests that should be done? n n TSH 15 u. IU/ml, Free T 4 1. 2 ng/dl TPO AB negative Pathophysiology of her disease process? n Transient Treatment n n n Levothyroxine therapy Recheck every 6 -8 months After 3 -6 months may be able to wean replacement
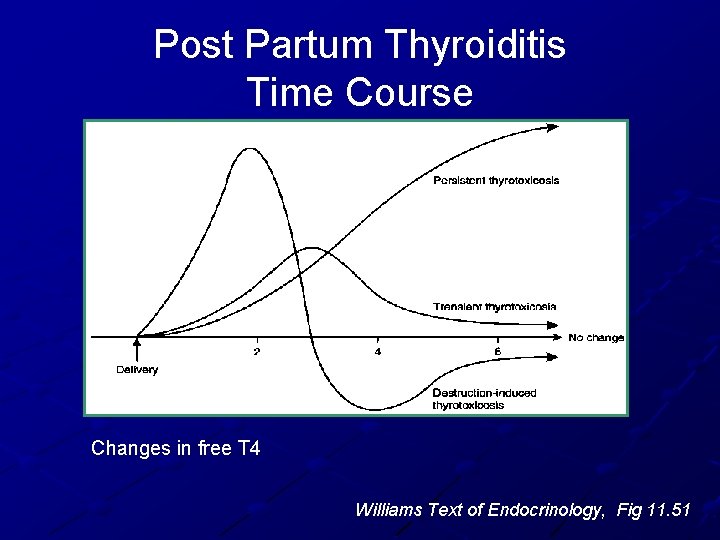
Post Partum Thyroiditis Time Course Changes in free T 4 Williams Text of Endocrinology, Fig 11. 51
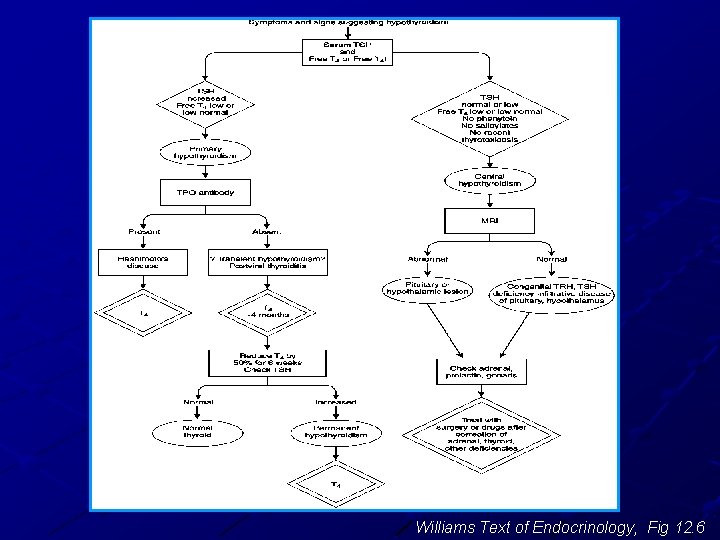
Williams Text of Endocrinology, Fig 12. 6
- Slides: 47