Thyroid gland disorders Dr Mousa Tuwati Alfakhri Objectives

Thyroid gland disorders Dr Mousa Tuwati Alfakhri

Objectives • • Thyroid gland, anatomy and physiology Thyroid function tests Hyperthyroidism hypothyroidism
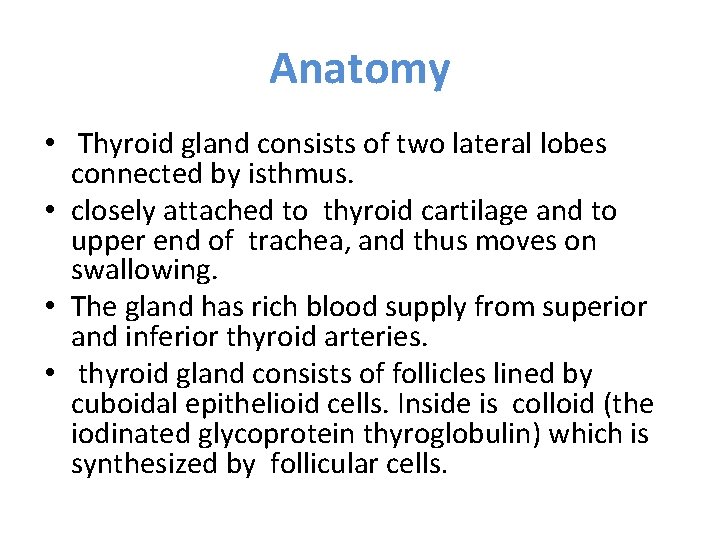
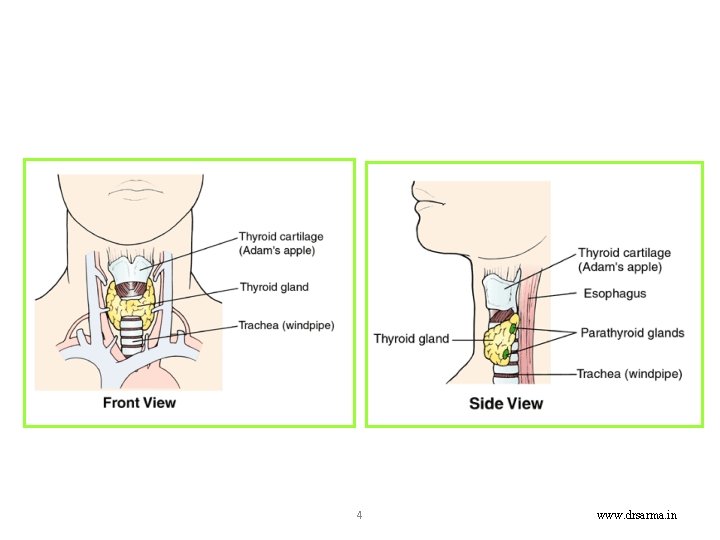
Anatomy • Thyroid gland consists of two lateral lobes connected by isthmus. • closely attached to thyroid cartilage and to upper end of trachea, and thus moves on swallowing. • The gland has rich blood supply from superior and inferior thyroid arteries. • thyroid gland consists of follicles lined by cuboidal epithelioid cells. Inside is colloid (the iodinated glycoprotein thyroglobulin) which is synthesized by follicular cells.
4 www. drsarma. in

In the Thyroid Gland There the following 5 steps in the hormonogenesis 1. Trapping of inorganic Iodine from dietary Iodides 2. Activation of inorganic Iodine to active iodide I 2 3. Incorporation of I 2 into Tyrosine of Thyroid Globulin to form MIT and DIT 4. Coupling of formed MIT and DIT to form T 4 & T 3 5

• Thyroid gland secret mainly T 4 (prohormone) 90% and only few T 3. • In plasma more than 99% of all T 4 and T 3 is bound to hormone-binding proteins (thyroxine-binding globulin, TBG). • Only free hormone is available for action in target tissues • In peripheral tissue T 4 is deiodinated and converted into T 3 which is the active form

hypothalamic-pituitary-thyroid axis HYPOTHALAMUS TRH ANT. PITUITARY TSH -R THYROID T 4 and T 3 PLASMA T 4 + FT 4 PLASMA T 3 + FT 3 TISSUES FT 4 to FT 3 7

Thyrotoxicosis

Objectives • • • Definitions Symptoms Signs Causes diagnosis Treatment

Definitions • Thyrotoxicosis: Hypermetabolic state caused by thyroid hormone excess at the tissue level. • Hyperthyroidism: Increased thyroid hormones synthesis and secretion. • All patients with hyperthyroidism have thyreotoxicosis • Not all patients with thyreotoxicosis are hyperthyroid

Symptoms of thyrotoxicosis Common symptoms • Weight loss despite normal or increased appetite • Heat intolerance • sweating • Palpitations • tremor • Dyspnoea • fatigue • Irritability • emotional lability Less common symptoms • • • Osteoporosis Diarrhoea Angina Anxiety, psychosis Muscle weakness Pruritus, alopecia Amenorrhoea/oligomenorrhoea Infertility, spontaneous abortion Loss of libido, impotence Excessive lacrimation

Signs of thyrotoxicosis common Signs • • • Weight loss Tremor Palmar erythema Sinus tachycardia Lid retraction, lid lag Rare signs • Gynaecomastia • Spider naevi • Onycholysis • Pigmentation Less common signs • Goitre with bruit(graves disease) • Atrial fibrillation • Systolic hypertension • increased pulse pressure • Cardiac failure • Hyper-reflexia • Ill-sustained clonus • Proximal myopathy

Causes of thyrotoxicosis • Graves’ disease 80% • Multinodular goitre 15% • Solitary thyroid adenoma 5% • Thyroiditis 3% Ø autimmune Ø Subacute (de Quervain’s) Ø Post-partum • Iodide-induced 1% Ø Drugs (amiodarone) Ø Radiographic contrast media • Extrathyroidal source of thyroid hormone 0. 02% Ø Factitious thyrotoxicosis Ø Struma ovarii(Ovarian teratoma containing thyroid tissue) • TSH-induced 0. 2% Ø TSH-secreting pituitary adenoma. Ø Choriocarcinoma and hydatidiform mole (Human chorionic gonadotrophin has thyroid-stimulating activity)

Graves’ disease • The most common cause of thyrotoxicosis (60 -80%). • Organ specific auto-immune disease • The most important autoantibody is Thyroid Stimulating Immunoglobulin (TSI) acts as TSH and stimulates T 4 and T 3 • Other antibodies: • Anti thyro peroxidase (anti-TPO) antibodies • Anti thyro globulin (anti-TG) v. Associated with other Autoimmune diseases Pernicious Anemia, T 1 DM RA, Myasthenia Gravis, Vitiligo, Adrenal insufficiency.

Epidemiology of Graves’ Disease • • Prevalence: 0. 6% of population Incidence: 0. 5/1000/year Female/male ratio: 5 – 10/1 Peak incidence: 30 – 60 years of age

Graves’ disease - pathogenesis Genetic and environmental factors Production of Ig. G antibodies (thyroid-stimulating immunoglobulins TSI or TSH-receptor antibodies TRAb) Stimulation thyroid hormone production and goitre formation

Precipitating And Predisposing Factors • Genetic Susceptibility(15% of pts with Graves’ have a close relative with the same disorder) • Stress : patients with Graves'hyperthyroidism give history of psychologic stress(loss of a spouse or road traffic accident) before onset of hyperthyroidism • Gender( F: M 7: 1) • Smoking(relative risk approximately 2. 0) and an even stronger risk factor for Graves' opthalmopathy • Pregnancy (30% of women give history of pregnancy in 12 months before onset of G D ) • Drugs(amiodarone, Interferon alpha, iodine)
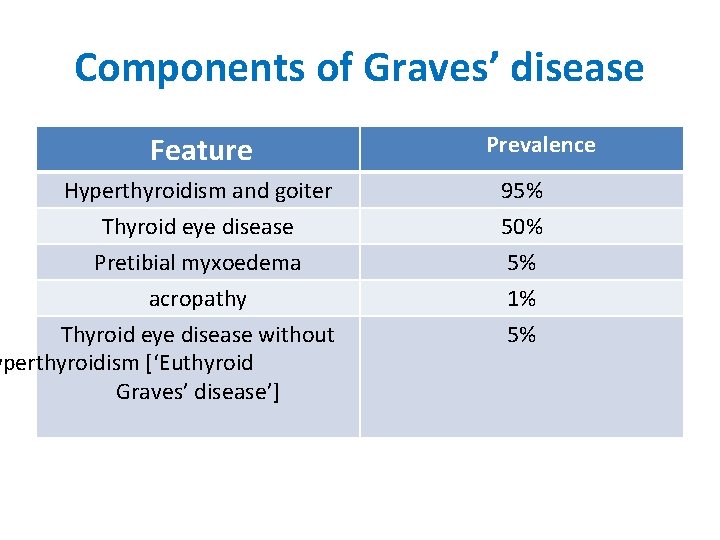

Components of Graves’ disease Feature Prevalence Hyperthyroidism and goiter Thyroid eye disease Pretibial myxoedema 95% 50% 5% acropathy Thyroid eye disease without yperthyroidism [‘Euthyroid Graves’ disease’] 1% 5%
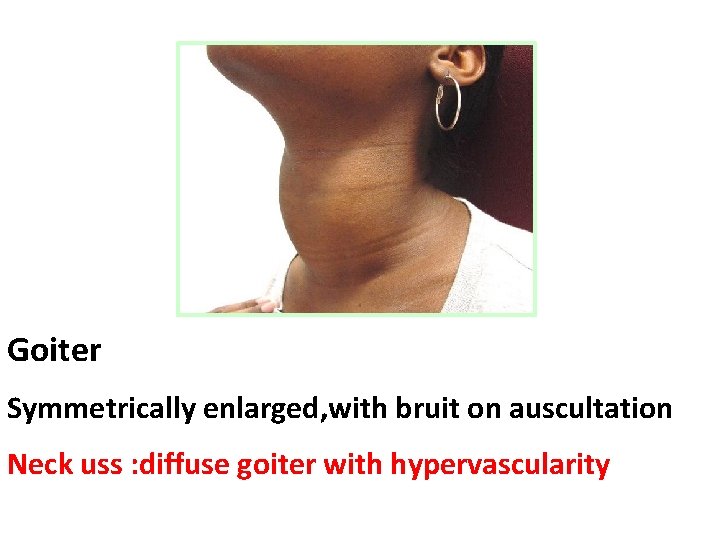
Goiter Symmetrically enlarged, with bruit on auscultation Neck uss : diffuse goiter with hypervascularity
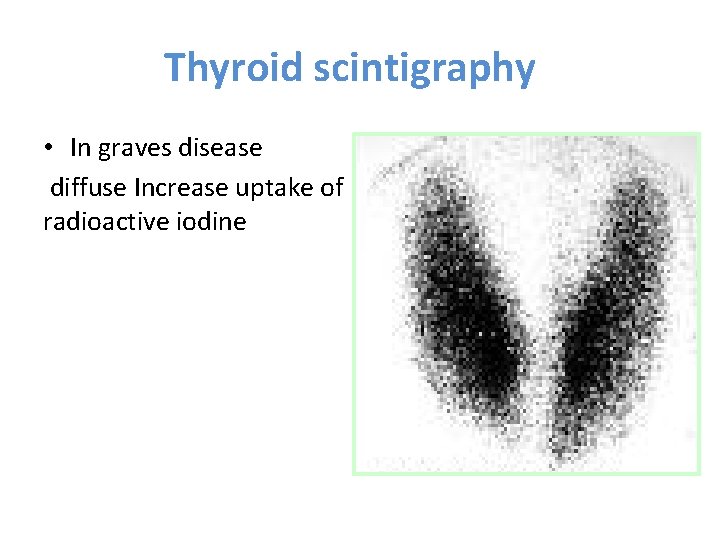
Thyroid scintigraphy • In graves disease diffuse Increase uptake of radioactive iodine
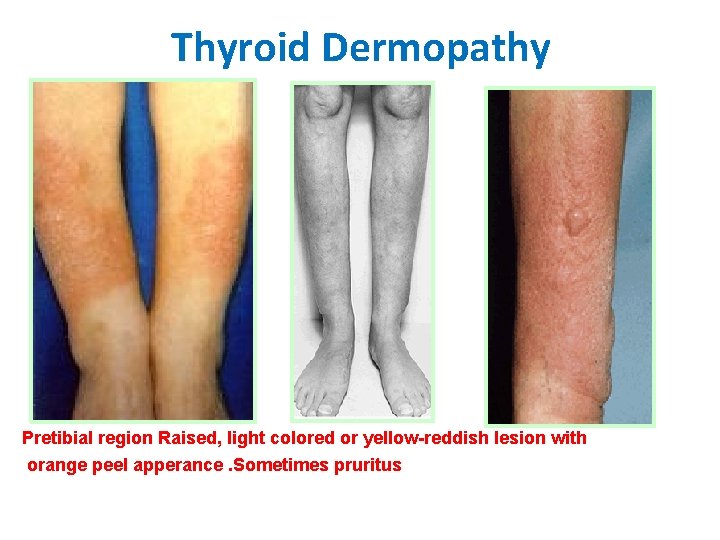
Thyroid Dermopathy Pretibial region Raised, light colored or yellow-reddish lesion with orange peel apperance. Sometimes pruritus
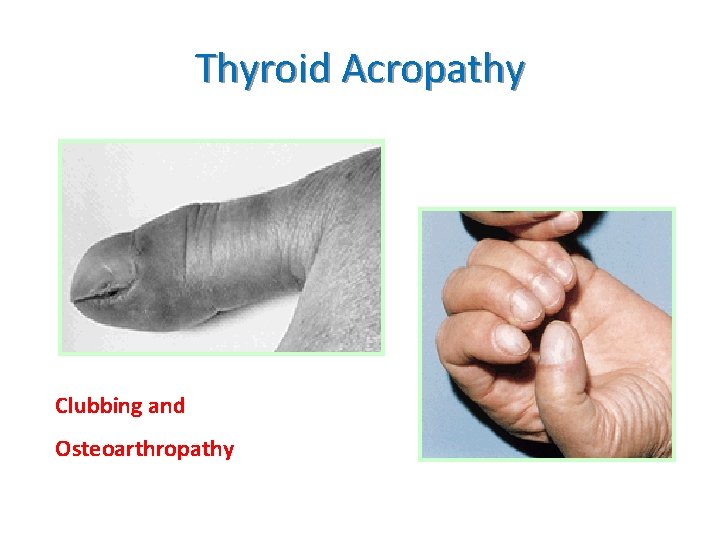
Thyroid Acropathy Clubbing and Osteoarthropathy
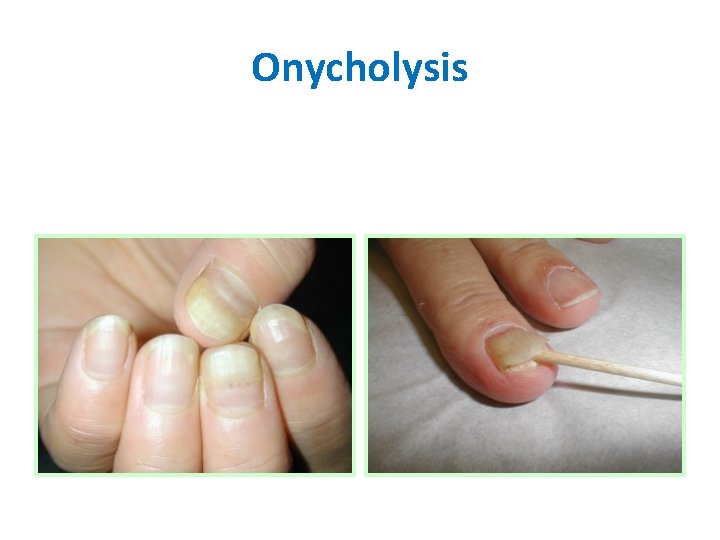
Onycholysis

Thyroid Ophthalmopathy Proptosis Lid lag
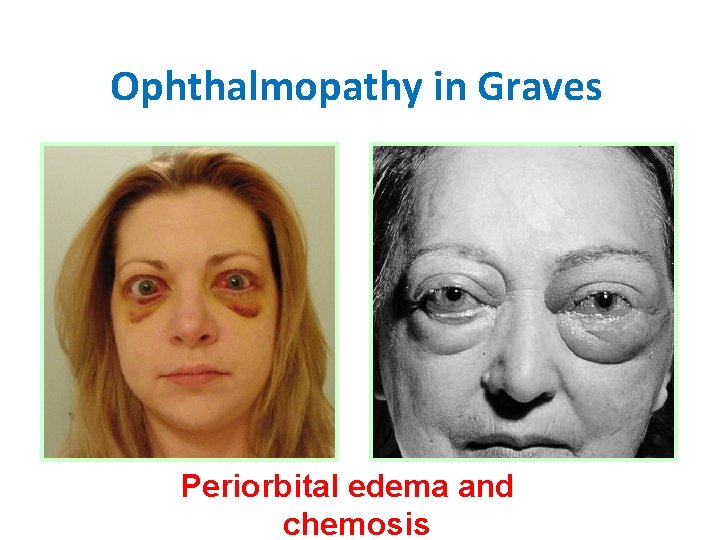
Ophthalmopathy in Graves Periorbital edema and chemosis

Toxic Multinodular Goiter (TMG) • TMG is the next most common hyperthyroidism 20% • More common in elderly individuals – long standing goiter • Milder manifestations (apathetic hyperthyroidism) • Mild elevation of FT 4 and FT 3 • Progresses slowly over time • Clinically multiple firm thyroid nodules • Scintigraphy shows - hot and normal areas
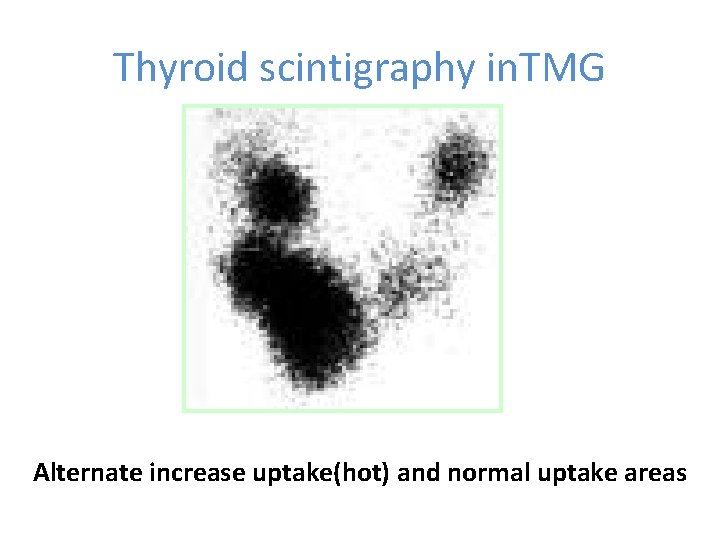
Thyroid scintigraphy in. TMG Alternate increase uptake(hot) and normal uptake areas

Sub Acute Thyroiditis (SAT) • is the next most common hyperthyroidism – 15% • T 4 and T 3 are extremely elevated in this condition • Immune destruction of thyroid due to viral infection • Destructive release of preformed thyroid hormone • Thyroid gland is painful and tender on palpation • Nuclear Scintigraphy scan - no RIU in the gland • Leucocytosis and high ESR • Treatment is NSAIDs and Corticosteroids

Toxic Single Adenoma (TSA) • TSA is a single hyper functioning follicular thyroid adenoma. • It is the cause in 5% of patients who are thyrotoxic • Nuclear Scintigraphy scan shows only a single hot nodule • TSH is suppressed by excess of thyroxines So the rest of the thyroid gland is suppressed
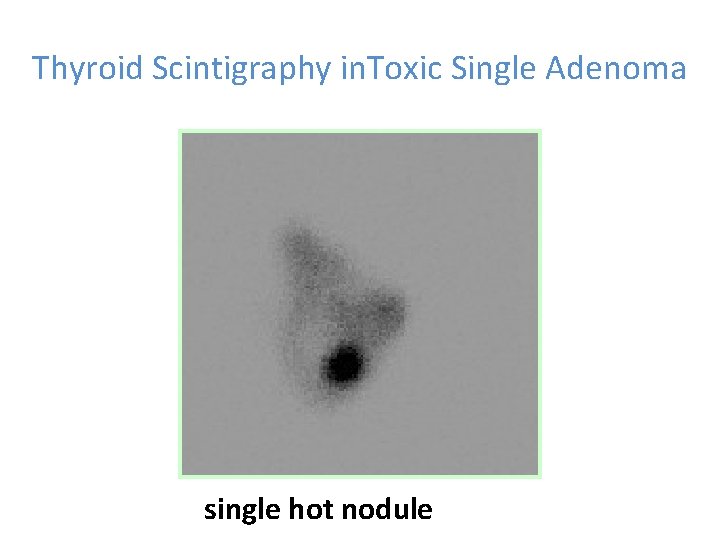
Thyroid Scintigraphy in. Toxic Single Adenoma single hot nodule

Diagnosis of thyrotoxicosis • Investigation to confirm diagnosis of thyrotoxicosis • Invetstigation to diagnose underlying cause

Investigation to confirm diagnosis of thyrotoxicosis • In primary hyperthyroidism Ø TSH is high Ø T 4 and T 3 are high in about 5 -10% of thyrotoxicosis T 4 is normal and T 3 is hight(T 3 toxicosis) • In TSH dependent causes(secondary thyrotoxicosis) of thyrtoxicosis such as. TSHsecreting pituitary adenoma and Choriocarcinoma and hydatidiform mole TSH is high and free T 3 and T 4 are high

Subclinical thyrotoxicosis • Serum TSH is undetectable, and serum T 3 and T 4 areat the upper end of the reference range. • This combinationis most often found in older patients with multinodulargoitre. • These patients are at increased risk of atrial fibrillation and osteoporosis • annualis follow up, as the conversion rate to overt thyrotoxicosis is 5% each year.

Invetstigation to diagnose underlying cause Thyroid scintigraphy A thyroid scan, which can be done at the same time as the RAIU, helps to distinguish among high RAIU disorders Graves disease shows diffuse isotope uptake toxic multinodular goiter shows patchy uptake a toxic adenoma shows uptake only in a single nodule
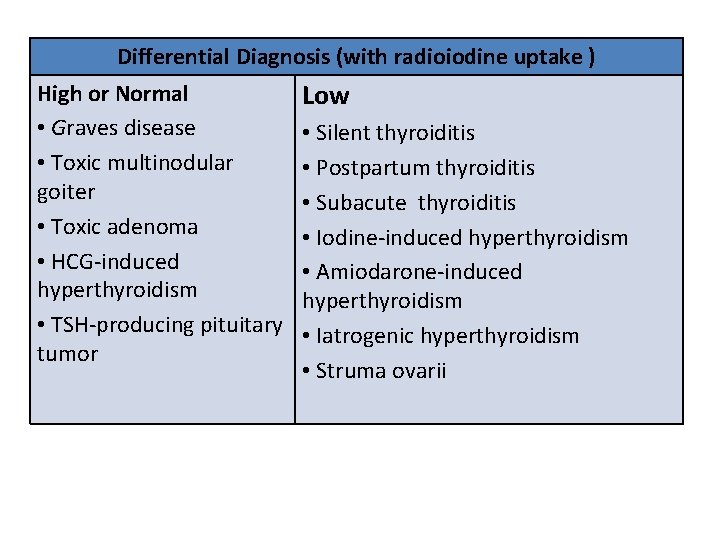
Differential Diagnosis (with radioiodine uptake ) High or Normal • Graves disease • Toxic multinodular goiter • Toxic adenoma • HCG-induced hyperthyroidism • TSH-producing pituitary tumor Low • Silent thyroiditis • Postpartum thyroiditis • Subacute thyroiditis • Iodine-induced hyperthyroidism • Amiodarone-induced hyperthyroidism • Iatrogenic hyperthyroidism • Struma ovarii

Other investigations for underlying causes • TSH-receptor antibodies (TRAb) (graves disease) • thyroid-peroxidase antibodies (TPO) autoimmune thyroid disease(greves disease, Hashimoto thyroiditis ). • thyroglobulin, erythrocyte sedimentation rate(subacute thyroiditis) • human chorionic gonadotropin(Choriocarcinoma and hydatidiform mole )
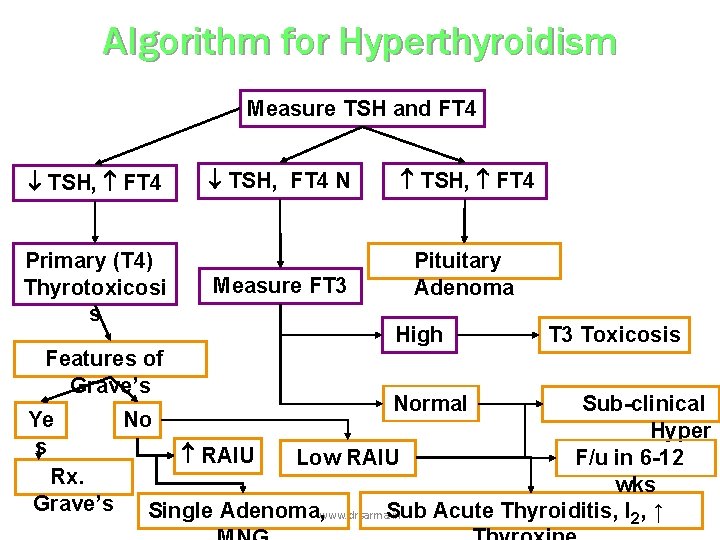
Algorithm for Hyperthyroidism Measure TSH and FT 4 TSH, FT 4 Primary (T 4) Thyrotoxicosi s Features of Grave’s TSH, FT 4 N TSH, FT 4 Measure FT 3 Pituitary Adenoma High Normal T 3 Toxicosis Sub-clinical Ye No Hyper s RAIU Low RAIU F/u in 6 -12 Rx. wks Grave’s Sub Acute Thyroiditis, I 2, ↑ Single Adenoma, www. drsarma. in
GRAVES’ DISEASE – TREATMENT General principles of treatment RADIOIODINE MEDICAL Treatments available for Graves’ disease SURGICAL

Medical treatment 1. Antithyroid drugs 2. β – blockers

β – blockers to decrease the sympathetic excess Ø Propranalol, Atenelol, Metoprolol if β – blockers contraindicated calcium chanel blockers used

Antithyroid drugs Goal: G Permanent remission of hyperthyroidism Limitations: G High recurrence rate of hyperthyroidism G Possible side effects

Anti Thyroid Drugs (ATD) Imp. considerations Methimazole Propylthiouracil Efficacy Very potent Potent Duration of action Long acting BID/OD In pregnancy Mechanism of action Conversion of T 4 to T 3 Adverse reactions Short acting QID/TID Safely can be Contraindicated given Iodination, Coupling Inhibits No action conversion Rashes, Neutropenia ↑Neutropenia

Adverse effects of Antithyroid drugs • • Mild leukopenia (12 – 25%) Agranulocytosis (0. 1 – 0. 5%) Aplastic anemia Thrombocytopenia Cholestasis Hepatocellular necrosis Lupus-like syndrome Nephrotic syndrome

Radio Active Iodine (RAI Rx) Ø Destruction of thyrocytes by β-radiation Ø The effect is less rapid than ATD or Thyroidectomy Ø It is effective, safe, and does not require hospitalization. Ø Very few adverse effects as no other tissue absorbs RAI Ø Goal is to make the patient hypothyroid Ø Never given for children and pregnant/ lactating women Ø Not recommended with patients of severe Ophthalmopathy

Indications for radioiodine therapy • • Patient preference Poor-compliance with antithyroid drugs Recurrence after thyroidectomy Severe uncontrolled disease

Complcations Radioiodine Therapy Ø Permanent hypothyroidism Ø Transient hypothyroidism Ø Thyroiditis Ø Thyrotoxic crisis Ø Possible exacerbation of ophtalmopathy (preventable by glucocorticoids)

Surgical treatment Total thyroidectomy is now considered the operation of choice because of the risk of relapse with partial thyroidectomy

Thyroid crisis or ‘thyroid storm’ • is Acute life threatening exacerbation of thyrotoxicosis rare condition, with a mortality of 10%, • hyperpyrexia, severe tachycardia, extreme restlessness, cardiac failure and liver dysfunction. • usually precipitated by stress, infection or surgery in an unprepared patient, or radioiodine therapy. • Treatment is urgent • Propranolol in full doses is started immediately together with potassium iodide, antithyroid drugs, corticosteroids

- Slides: 49