Thyroid Disorders William Harper MD FRCPC Endocrinology Metabolism

Thyroid Disorders William Harper, MD, FRCPC Endocrinology & Metabolism Assistant Professor of Medicine, Mc. Master University

Case 1 • • 31 year old female Somalia Canada 3 years ago G 2 P 1 A 0, 11 weeks pregnant Well except fatigue Hb 108, ferritin 7 (Fe and LT 4 interaction? ) TSH 0. 2 m. U/L, FT 4 7 p. M Started on LT 4 0. 05 TSH < 0. 01 m. U/L FT 4 12 p. M, FT 3 2. 1 p. M

Case 1 1. How would you characterize her hypothyroidism? 2. What are the ramifications of pregnancy to thyroid function/dysfunction?
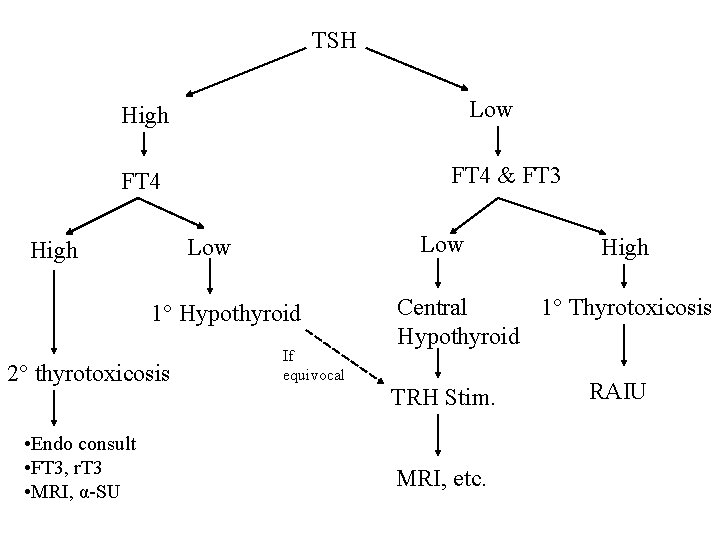
TSH Low High FT 4 & FT 3 FT 4 Low High 1° Hypothyroid 2° thyrotoxicosis • Endo consult • FT 3, r. T 3 • MRI, α-SU If equivocal High Central 1° Thyrotoxicosis Hypothyroid TRH Stim. MRI, etc. RAIU
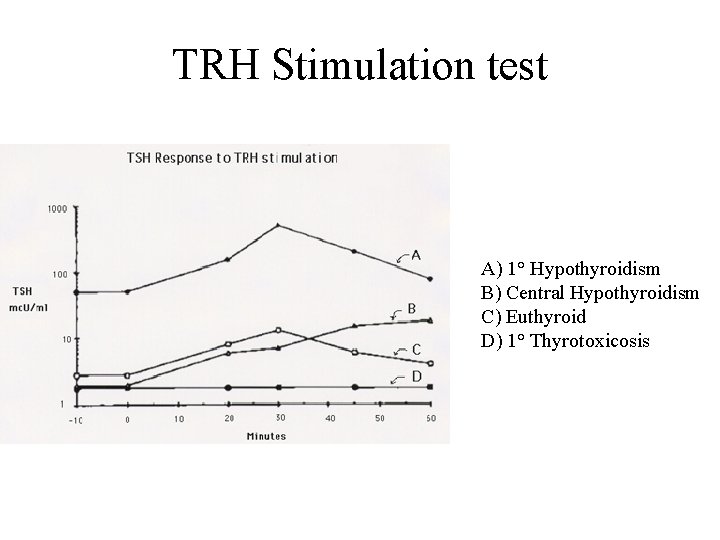
TRH Stimulation test A) 1° Hypothyroidism B) Central Hypothyroidism C) Euthyroid D) 1° Thyrotoxicosis

Case 1 • GH, IGF-1 normal • LH, FSH, E 2, progesterone, PRL normal for pregnancy • 8 AM cortisol 345, short ACTH test normal • MRI: normal pituitary • TGAB, TPOAB negative • LT 4 increased until FT 4 in hi-normal range • Normal pregnancy, delivery, baby, lactation • Considering TRH stim once done breast-feeding

Thyroid Tests 1. 2. 3. 4. 5. 6. Thyroid Function Iodine Kinetics Thyroid Structure FNA Thyroid Antibodies Thyroglobulin
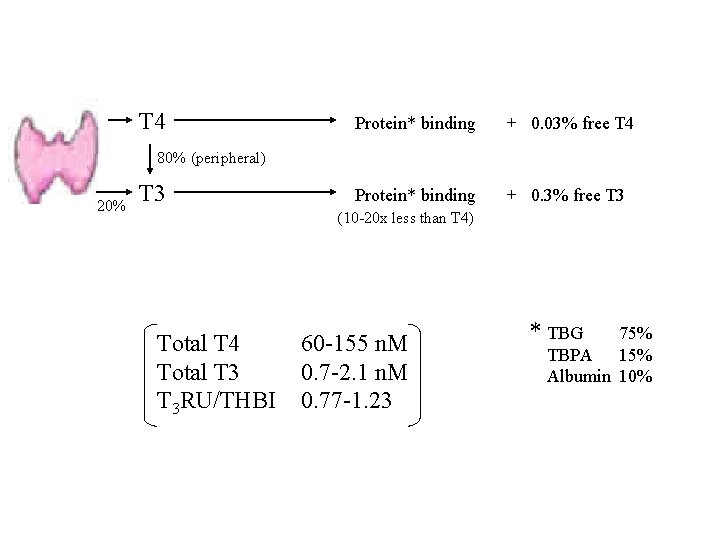
T 4 Protein* binding + 0. 03% free T 4 Protein* binding + 0. 3% free T 3 80% (peripheral) 20% T 3 (10 -20 x less than T 4) Total T 4 Total T 3 RU/THBI 60 -155 n. M 0. 7 -2. 1 n. M 0. 77 -1. 23 * TBG 75% TBPA 15% Albumin 10%

Thyroid Function Tests • TSH • Free T 4 (thyroxine) • Free T 3 (triiodothyronine) 0. 4 – 5. 0 m. U/L 9. 1 – 23. 8 p. M 2. 23 -5. 3 p. M

TSH Assay (0. 4 -5 m. U/L) • Early RIA < 1. 0 m. U/L • Thyrotoxicosis / 2º hypothyroidism – Unable to detect lower range of normal • Monoclonal SEN < 0. 1 m. U/L • Super SEN < 0. 01 m. U/L

Case 1 1. How would you characterize her hypothyroidism? 2. What are the ramifications of pregnancy to thyroid function/dysfunction?

Thyroid & Pregnancy: Normal Physiology • Increased estrogen increased TBG • Higher total T 4, T 3 (normal FT 4, FT 3 if thyroid gland working properly) • h. CG peak end of 1 st trimester, weak TSH agonist so may cause slight goitre • Fetal thyroid starts working at 11 wks • T 4 & T 3 do NOT cross placenta (or do so minimally) • Do cross placenta: PTU, MTZ, TSH-R Ab (stim or block) • MTZ aplasia cutis scalp defects
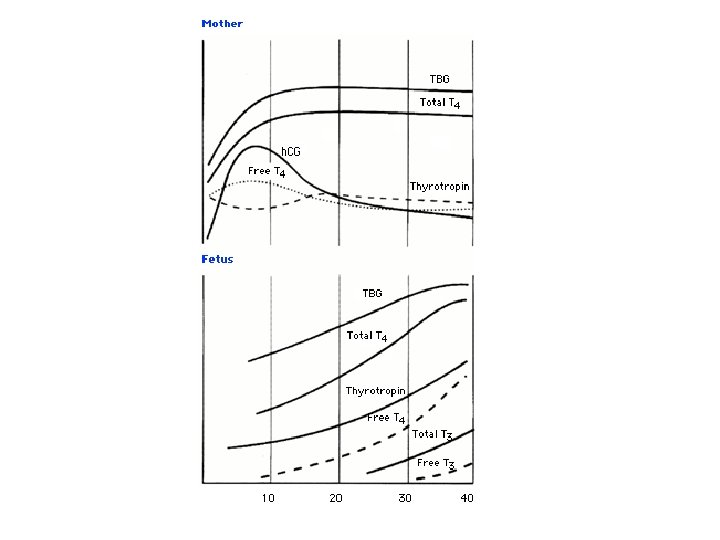

Thyroid & Pregnancy: Hypothyroidism • Will need ~ 25% increase in LT 4 during pregnancy due to increased TBG levels • Risks: increased spont abort, HTN, preterm pregnancy, 7 IQ points for fetus (NEJM, 341(8): 549 -555, Aug 31, 2001)

LT 4 dose adjustment in Pregnancy: Need TSH at baseline & q 2 mos while pregnant Starting LT 4: 2 ug/kg/d and check TSH q 4 wk until euthythyroid TSH Dose Adjustment TSH increased but < 10 Increase dose by 50 ug/d TSH 10 -20 TSH > 20 Increase dose by 50 -75 ug/d Increase dose by 100 ug/d

Thyrotoxicosis & Pregnancy • Risks: fetal anomalies, spont abort, preterm labor, fetal hyperthyoridism, thyroid storm in labor • No RAI ever • Rx options: ATD or 2 nd trimester thyroidectomy • PTU drug of choice (avoid MTZ due to scalp defects) • Aim to keep FT 4 levels in hi normal range • OK to breast feed on PTU as does not go into breast milk

Neonatal Grave’s • Rare < 2% infants born to Graves” moms • 2 types: Transplacental trnsfr of TSH-R ab (Ig. G) • Present at birth, self-limited • Rx PTU, Lugol’s, propanolol, prednisone • Prevention: TSI in mom 2 nd trimester, if 5 X normal then Rx mom with PTU (crosses placenta to protect fetus) even if mom is euthyroid (can give mom LT 4 which won’t cross placenta) Child develops own TSH-R ab • Strong family hx of Grave’s • Present @ 3 -6 mos • 20% mortality, persistant brain dysfunction

Postpartum & Thyroid • • 5% (3 -16%) postpartum women (25% T 1 DM) Up to 1 year postpartum (most 1 -4 months) Lymphocytic infiltration (Hashimoto’s) Postpartum Exacerbation of all autoimmune dx 25 -50% persistant hypothyroidism Small, diffuse, nontender goitre Transiently thyrotoxic Hypothyroid
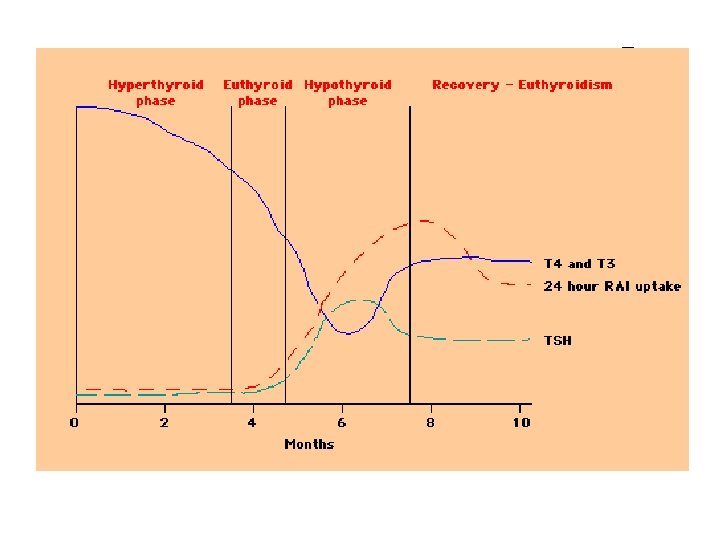

Postpartum & Thyroid • Distinguish Thyrotoxic phase from Grave’s: • No Eye disease • Less severe thyrotoxic, transient (repeat thyroid fn 2 -3 mos) • RAI (if not breast-feeding) • Rx: • Hyperthyroid symptoms: atenolol 25 -50 mg od • Hypothyroid symptoms: LT 4 50 -100 ug/d to start » Adjust LT 4 dose for symtoms and normalization TSH » Consider withdrawal at 6 -9 months (25 -50% persistent hypothyroid, hi-risk recur future preg)

Postpartum & Thyroid • Postpartum depression • When studied, no association between postpartum depression/thyroiditis • Overlapping symtoms, R/O thyroid before start antidepressents • Screening for Postpartum Thyroiditis HOW: TSH q 3 mos from 1 mos to 1 year postpartum? WHO: – – Symptoms of thyroid dysfn. Goitre T 1 DM Postpartum thyroiditis with prior pregnancy

Case 2 • 47 year old female • Concerned about weight gain over past 15 years (15 lbs). Otherwise asymptomatic • BMI 25, Thyroid: 40 gm, rubbery firm. • TSH 6. 7 m. U/L, FT 4 13 p. M, FT 3 2. 5 p. M • FHx: mother, sister – both on LT 4 • Medications: “Thyrosol” (health store) • Wondering about hypothyroidism causing her weight gain • Read on internet about “Wilson’s Disease”

Case 2 1. 2. 3. 4. When to treat “Subclinical” thyroid dysfunction? Naturopathic thyroid remedies Hypothryoidism Rx other than Levothyroxine What is Wilson’s Thyroid Disease?

Subclincal Hypothyroidism • TSH, normal FT 4 • Most asymptomatic & don’t need Rx (monitor TSH q 2 -5 y) • Rx Indications: – Increased risk of progression • TSH > 10, Female > 50 y. o. • Anti-TPO Ab titre > 1: 100, 000 ? • Goitre present ? – Dyslipidemia? • Total cholesterol (TC) 6 -8% if TSH > 10 and TC > 6. 2 n. M – Symptoms? – Pregnancy, Infertility, Ovulatory Dysfn.

Case 2 1. 2. 3. 4. When to treat “Subclinical” thyroid dysfunction? Naturopathic thyroid remedies (Thyrosol) Hypothryoidism Rx other than Levothyroxine What is Wilson’s Thyroid Disease?


Hashimoto’s Disease • Most common cause of hypothyroidism in North America (not idodine defeciency!) • Autoimmune • lymphocytic thyroiditis • Females > Males, Runs in Families • Antithyroid antibodies: • Thyroglobulin Ab • Microsomal Ab • TSH-R Ab (block)

Hashimoto’s Disease • Treatment: • Thyroid Hormone Replacement • Levothyroxine (T 4) • T 3? , T 4/T 3 combo? , dessicated thyroid? • No benefit to giving iodine! • In fact, iodine may decrease hormone production • Wolff-Chaikoff effect (lack of escape)

Case 2 1. 2. 3. 4. When to treat “Subclinical” thyroid dysfunction? Naturopathic thyroid remedies Hypothryoidism Rx other than Levothyroxine What is Wilson’s Thyroid Disease?

Treatment of Hypothyroidism • Iodine only if iodine deficiency is the cause • Rare in North America! • Replacement thyroid hormone medication: • • T 4? T 3? T 4 + T 3 Mixture? Thyroid Hormone from “natural sources” ?

Normal Daily Thyroid Secretion Rate: T 4 = 100 ug/day T 3 = 6 ug/day ( ratio T 4: T 3 = 14: 1 ) T 4 Protein* binding + 0. 03% free T 4 Protein* binding + 0. 3% free T 3 85% (peripheral conversion) 15% T 3 (10 -20 x less than T 4)
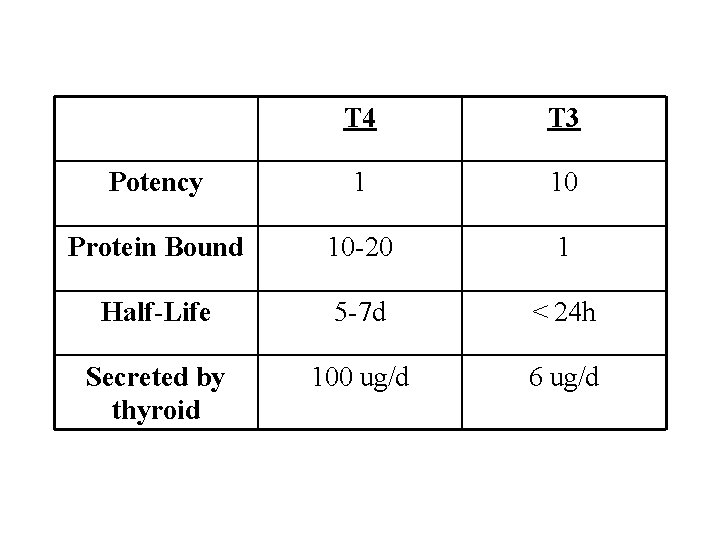
T 4 T 3 Potency 1 10 Protein Bound 10 -20 1 Half-Life 5 -7 d < 24 h Secreted by thyroid 100 ug/d 6 ug/d

Levothyroxine (T 4) • • Synthroid (Abbott), Eltroxin (GSK) Synthetically made 50 ug white pill no dye (hypoallergenic) Most commonly prescribed treatment for hypothyroidism • No T 3 (but 85% of T 3 comes from T 4 conversion) • All patients made euthyroid biochemically • Most (but not all) patients feel normal

Levothyroxine (T 4) • Average dose 1. 6 ug/kg • Age > 50 -60 or cardiac disease: must start at a low dose (25 ug/d) • Recheck thyroid hormone levels every 4 -6 weeks after a dose change • Aim for a normal TSH level

Levothyroxine (T 4) • Medical situations where T 4 medication may be affected. • Estrogen: Pregnancy, OCP, HRT • Need to increase T 4 dose! • Drugs that interfere with T 4 absorption • Iron, Calcium • Cholestyramine (cholesterol resin Rx) • At least 4 h between T 4 and these drugs!

“I still don’t feel normal on Synthroid even though my blood tests are normal. ” • Free T 4, Free T 3 • wide range of normal • TSH (0. 4 – 5. 0 m. U/L) • Narrow range of normal, but still a range! • Adjust dose for a lower TSH still in the normal range? • Tissue levels versus circulating levels? • No human studies • Rodents: High T 4 and normal T 3 tissue levels

Liothyronine (T 3) • Cytomel (Theramed) • Shorter half-life • Fluctuating levels (i. e. need a slow-release pill) • Twice daily dosing often needed • 10 x more potent: palpitations & other cardiac side effects • High T 3 levels, low T 4 levels (not physiologic either!)

T 3/T 4 Liotrix • • • Thyrolar Combo pill of T 3 and T 4 Ratio of T 4: T 3 = 4: 1 (not 14: 1) T 3 still not slow release Few small studies showing benefit • 1999 NEJM study 33 patients • Benefit: mood & cognitive function • Not available in Canada

Desiccated Thyroid (Armour) • Desiccated powder derived from thyroids of slaughtered pigs or cows • Vegetarian? • Mad Cow Disease? • Contains T 4 and T 3 • Still no slow-release of T 3 • Ratio of T 4: T 3 • Variable • Still not physiologic, often too high in T 3 (T 4: T 3 = 3: 1)

“In an ideal world…” • Mixed compound with T 4: T 3 = 14: 1 • T 3 component slow release formulation • Resultant: • Normal circulating TSH, FT 4, FT 3 • Normal tissue levels of T 4 and T 3 • Good, large studies (RCTs) demonstrating clear benefit over T 4 alone

Case 2 1. 2. 3. 4. When to treat “Subclinical” thyroid dysfunction? Naturopathic thyroid remedies Hypothryoidism Rx other than Levothyroxine What is Wilson’s Thyroid Disease?

“Wilson’s Syndrome” • Wilson’s disease: copper toxicity liver failure • “Wilson’s Syndrome” • Dr. E. D. Wilson “discovered” this condition and named it after himself in late 1980’s • Decreased body temperature (low normal range) • Hypothyroid symptoms (nonspecific) • Normal thyroid function tests • “Impaired T 4 T 3 conversion” • “Build up of reverse T 3” • Treat with “Wilson’s T 3 -therapy” (presumably T 3)
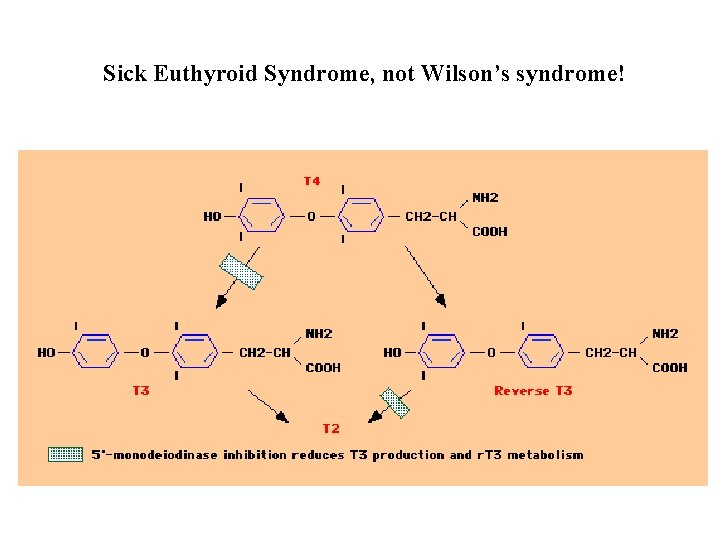
Sick Euthyroid Syndrome, not Wilson’s syndrome!

“Wilson’s Syndrome” • No scientific evidence that this condition exists • No randomized trials proving safety or any benefit of giving people T 3 when their thyroid hormone levels are normal • This condition not endorsed by: • Canadain Society of Endocrinology and Metabolism (CSEM) • American Thyroid Association (ATA) • Endocrine Society

Case 3 • 62 y male • Afib: amiodarone, warfarin x 11 months • 2 months: fatigue, muscle weakness, increasing dyspnea/edema, weight gain • O/E: HR 110 irreg-irreg, appears malnourished, JVP, SOA, lung crackles

Case 3 • • TSH < 0. 05 m. U/L, FT 4 60 p. M, FT 3 24 p. M INR 4. 2, Echo: LVH, normal LV syst fn. RAIU 2%, Thyroid scan: no gland seen Rx: Methimazole 40 mg/d, lasix, aldactone, ramipril, reduced warfarin • Cardiolgist: d/c amiodarone bisoprolol

Case 3 F/up @ 2 mos: • weight loss (more muscle, less fluid) • Resolved: Fatigue, SOB, SOA • HR 76 irreg-irreg • TSH < 0. 05, FT 4 8 p. M, FT 3 2. 1 p. M • INR 1. 5

Case 3 1. What is difference between thyrotoxicosis and hyperthyroidism? 2. What is “apathetic” hyperthyroidism? 3. Amiodarone induced thyrotoxicosis? 4. Thyroid & drug-interactions (warfarin)? 5. Subclinical Thyrotoxicosis?
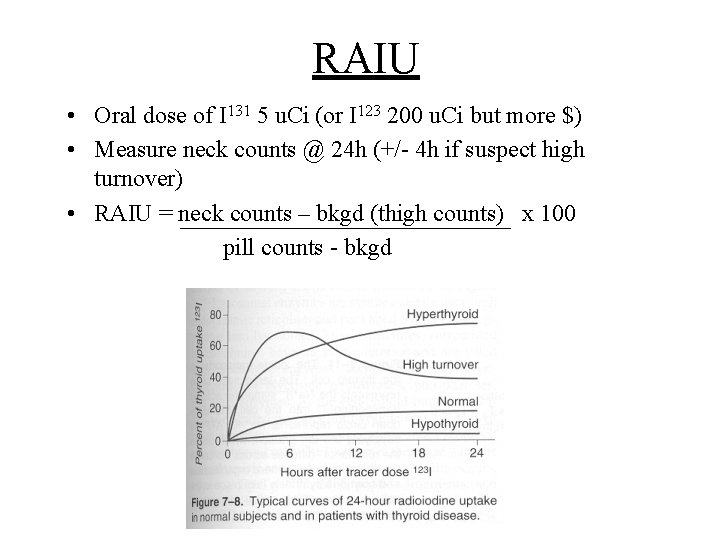
RAIU • Oral dose of I 131 5 u. Ci (or I 123 200 u. Ci but more $) • Measure neck counts @ 24 h (+/- 4 h if suspect high turnover) • RAIU = neck counts – bkgd (thigh counts) x 100 pill counts - bkgd

RAIU • Normal 4 h RAIU = 5 -15 % • 24 h RAIU: >25% Hyperthyroid 20 -25% Equivocal (check TSH) 9 -20% Normal 5 -9% Equivocal (check TSH) <5% Hypothyroid • Dependent on dietary iodine intake! • Must be: not pregnant! (ß-h. CG), no ATD x 7 d, no LT 4 x 4 d, no large doses of iodine or radiocontrast for 2 wk (prefer 4 -6 wk)


Thyrotoxicosis Treatment • Beta-blockers (hyperadrenergic symptoms) • Hyperthyroidism: • Anti-thyroid Drugs – Propylthiouracil (PTU), Methimazole • Radioiodine Ablation • Surgical Thyroidectomy • Thyroiditis: • ASA, NSAIDS, +/- corticosteroids • Iodine (high doses Wolff Chaikoff effect)

“Apathetic Hyperthyroidism” • Elderly population • Lack of tremor, diaphoresis, heat-intolerance, hyperdefecation and other classic symptoms from sympathetic over-activity • TMNG more likely than in young (but Grave’s still most common) • Less likely to have a goitre • Common symptoms: • • Weight loss, anorexia Constipation despite thyrotoxic Tachycardia, Afib, CHF, angina Cognitive Dysfunction

Amiodarone and Thyroid PHYSIOLOGIC EFFECTS 1) Increase iodine pool in body and therefore decrease RAIU. 2) Decrease peripheral deiodination of T 4 to T 3. 3) Decrease pituitary deiodination and therefore transient rise in TSH for 1 st 3 mos of Rx. Amiodarone Induced Thyroid Dysfunction: • 3 months to 4 years after starting amiodarone • Hypothyroidism 8% (subclinical hypothyroidism 20%) • Thyrotoxicosis 3% (10% iodine deficiency areas)

Amiodarone induced Hypothyroidism 1) Increased TSH (not useful 1 st 3 mos). 2) Decreased FT 4 3) Decreased FT 3 (not neccesary to measure) 4) More common in areas of hi iodine intake (North America) d/t Wolff Chaikoff effect. 5) Rx: • Stop amiodarone if possible. • LT 4 aim dose to keep FT 4 level at high normal to slightly above normal. • Unlike other types of hypothyroidism do NOT try to normalize TSH as this requires dose ~ 250 ug/d and clearly causes hyperthyroidism.

Amiodarone induced Thyrotoxicosis (AIT) 1) Decreased TSH 2) Increased FT 4 3) Increased FT 3 in some patients (inhibition of deiodinase) 4) More common in areas of low iodine intake (Europe) d/t Jodbasedow effect or iodine/amiodarone induced thyroid damage. 5) Two types of AIT: • Hyperthyroidism (RAIU low but measurable) – Jodbasedow, often goitre/nodule(s) • Thyroiditis (RAIU 0%) 6) May present without hyperthyroid symptoms and simply worsening of cardiac disorder (arrythmia, angina, CHF, etc).

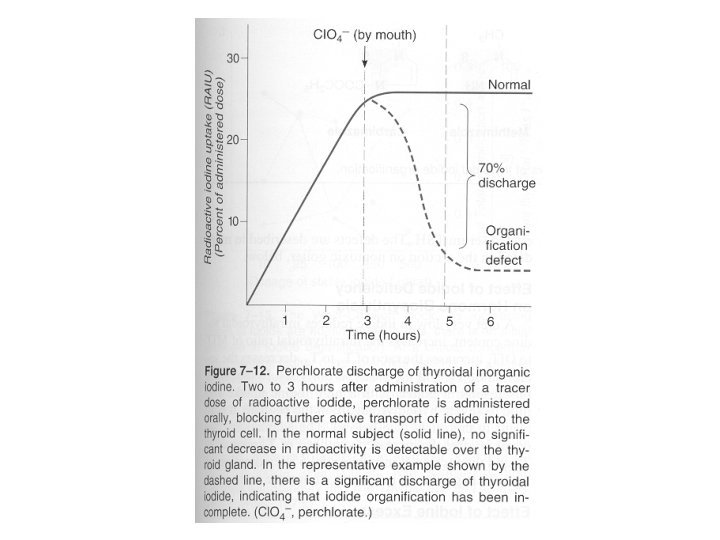
Amiodarone induced Thyrotoxicosis (AIT) Rx: • Stopping amiodarone may not help as amiodarone still present in body tissue stores for months • May need amiodarone to still treat arrythmias made worse by thyrotoxicosis • Radioactive I-131 useless d/t decreased RAIU. • Thionamide ATDs (PTU, methimazole): Rx of choice • Glucocorticoids if RAIU indicates thyroiditis & no response to ATD • Prednisone 40 mg/d • Surgery? Somewhat risky d/t unknown safety wrt thyroid storm & underlying heart condition that required amiodarone in the first place! • KCl. O 4 (potassium perchlorate)?

Thyroid & Drug Interactions 1) Warfarin • T 4 increases catabolism of vitamin K dependent clotting factors. • Increase LT 4/hyperthyroidism will increase sensitivity to warfarin (decrease dose). • Decrease LT 4/hypothyroidism will decrease sensitivity to warfarin (increase dose). 2) Cholestyramine • Binds T 4 & T 3 • 4 -5 h between resin & LT 4 or T 3. 3) Iron or Calcium • Also binds T 4 & T 3

Thyroid & Drug Interactions 4) Estrogens • Increase TBG, decrease FT 4 level • Need to increase LT 4 in some patients 5) Androgens/corticosteroids • Decrease TBG, increase FT 4 level • Need to decrease LT 4 in some patients 5) Diabetes • Increase LT 4/hyperthyroidism will increase insulin/OHA requirements. • Decrease LT 4/hypothyroidism will decrease insulin/OHA requirements.

Subclinical Hyperthyroidism • TSH, Normal FT 4 and FT 3 • Progression to overt hyperthyroidism low: • Men 0% per year • Women 1. 5% per year • TMNG or toxic adenoma present 5% per year • Indications to Rx: • • Any cardiac disease (CAD, AFIB, etc. ) Age > 60 (10 year risk AFIB 32%, 10% if normal TSH) TMNG or toxic adenoma Osteoporosis

Case 4 • 29 year old female, engaged to be married • T 1 DM • Thyroid U/S: • 2. 9 cm R lower pole • 2. 0 cm L lower pole, • Many others ranging from 0. 5 -1. 5 cm • TSH < 0. 05 m. U/L, FT 4 19 p. M, FT 3 6. 9 p. M • RAIU/Scan: 45% RAIU, hot nodule on Left

Case 4 • FNA of 3 cm nodule on Right: benign • Rx’s offered: • RAI ablation versus thyroidectomy • Patient chose Thyroidectomy

Thyroid Structure • Physical Exam • Thyroid Ultrasound • Thyroid Scan

Thyroid nodules • U/S more sensitive than P. E. , particularly for nodules that are < 1 cm or located posteriorly in the gland. • U/S also more SEN than thyroid scan • U/S too Sensitive? • Thyroid Incidentaloma (Carotid duplex, etc. )

Thyroid U/S Benign Characteristics Regular border Halo (sonolucent rim) Hyperechoic Egg shell calcification N/A Malignant Characteristics Irregular border No Halo Hypoechoic (more vascular) Microcalcification Intranodular vascular spots (color doppler)
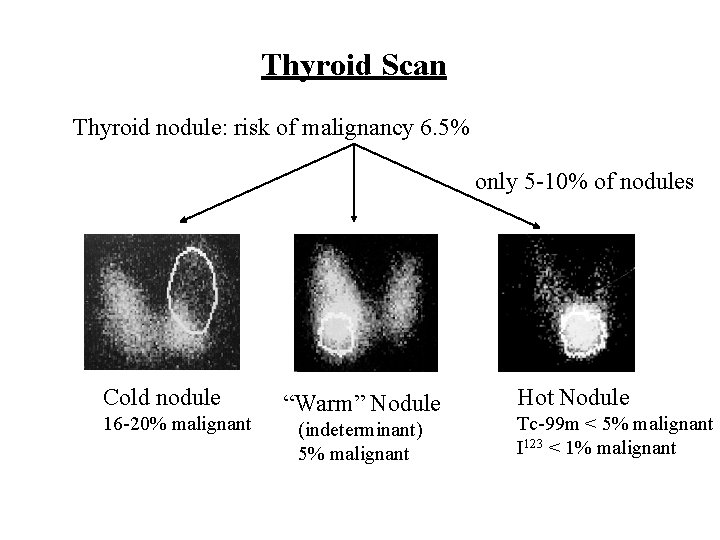
Thyroid Scan Thyroid nodule: risk of malignancy 6. 5% only 5 -10% of nodules Cold nodule 16 -20% malignant “Warm” Nodule (indeterminant) 5% malignant Hot Nodule Tc-99 m < 5% malignant I 123 < 1% malignant

Fine Needle Aspiration (FNA) • • • 25 G Needle, 10 cc syringe Done in Office +/- Local 3 -5 passes SEN 95 -99% (False Negative rate 1 -5%) SPEC > 95%

FNA Results • Nondiagnostic: repeat FNA • Benign: macrofollicular or "colloid" adenomas, chronic autoimmune (Hashimoto's) thyroiditis • Suspicious or Indeterminant: microfollicular or cellular adenomas (follicular neoplasm) • Malignant
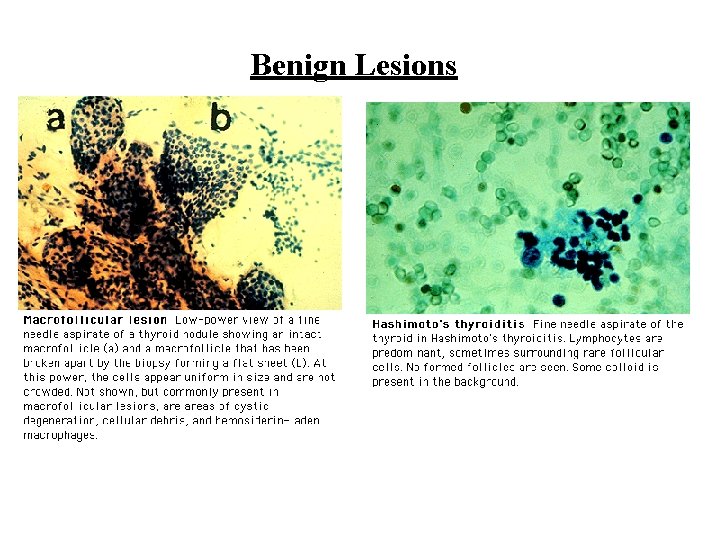
Benign Lesions
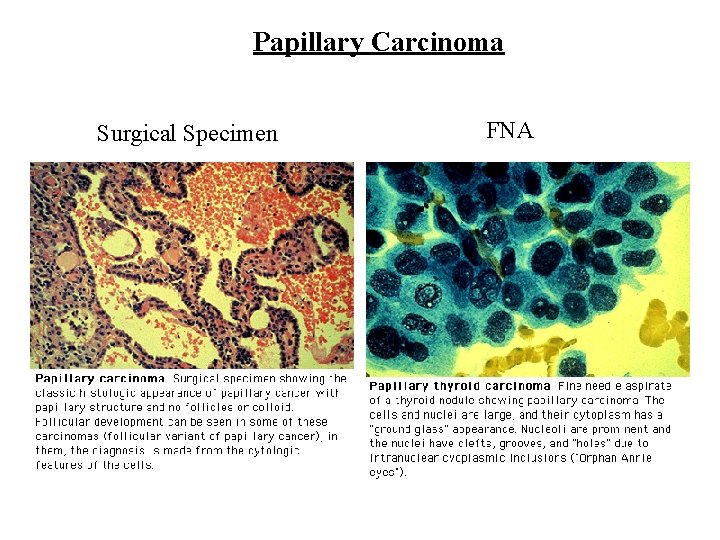
Papillary Carcinoma Surgical Specimen FNA
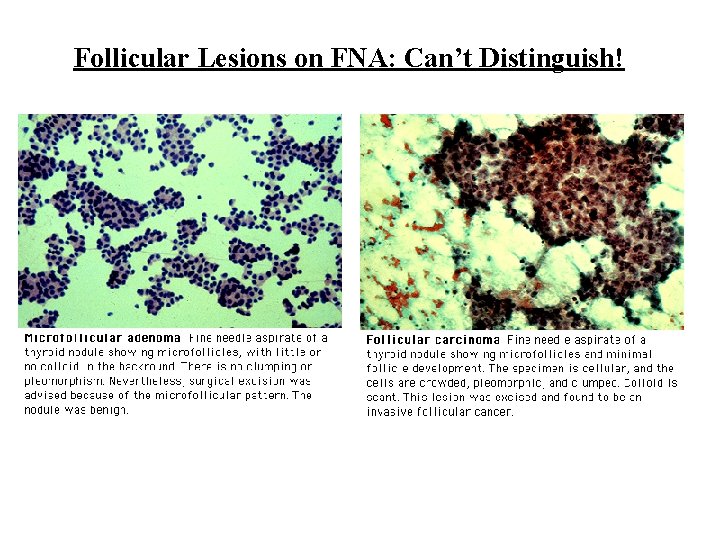
Follicular Lesions on FNA: Can’t Distinguish!
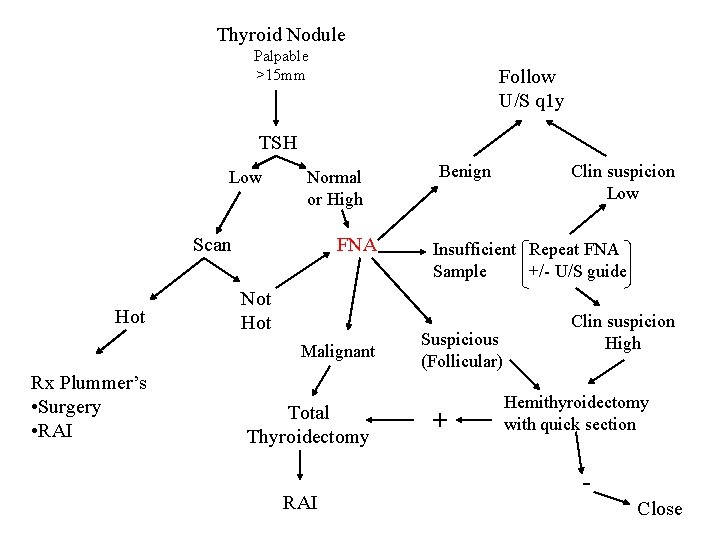
Thyroid Nodule Palpable >15 mm Follow U/S q 1 y TSH Low Normal or High Scan Hot FNA Not Hot Malignant Rx Plummer’s • Surgery • RAI Total Thyroidectomy RAI Benign Clin suspicion Low Insufficient Repeat FNA Sample +/- U/S guide Suspicious (Follicular) + Clin suspicion High Hemithyroidectomy with quick section Close
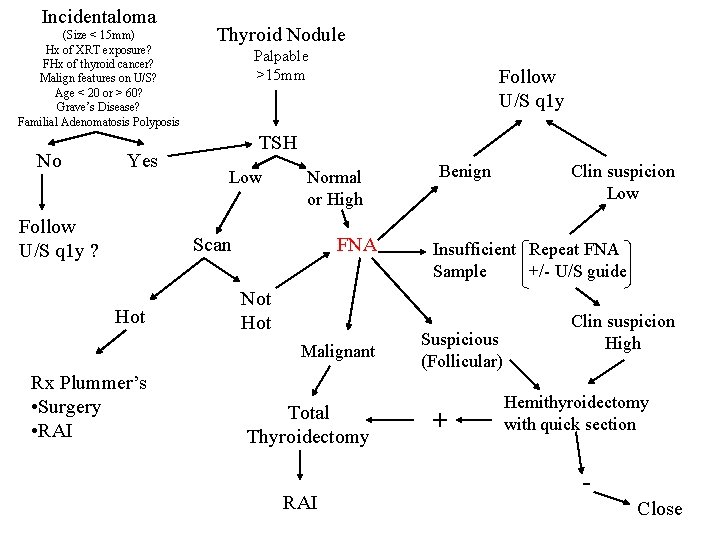
Incidentaloma (Size < 15 mm) Hx of XRT exposure? FHx of thyroid cancer? Malign features on U/S? Age < 20 or > 60? Grave’s Disease? Familial Adenomatosis Polyposis No Yes Follow U/S q 1 y ? Thyroid Nodule Palpable >15 mm TSH Low Normal or High Scan Hot Follow U/S q 1 y FNA Not Hot Malignant Rx Plummer’s • Surgery • RAI Total Thyroidectomy RAI Benign Clin suspicion Low Insufficient Repeat FNA Sample +/- U/S guide Suspicious (Follicular) + Clin suspicion High Hemithyroidectomy with quick section Close

Case 5 • • 19 year old female PMHx: Eating Disorder, Bulimia Weight loss despite witnessed food intake Tachycardia, palpitations FHx: Hypothyroidism (mother) No palpable goitre TSH < 0. 05 m. U/L, FT 4 23 p. M, FT 3 5. 0 p. M 24 h RAIU 2%, Thyroid Scan: no gland seen

Case 5 • TSH-R antibody negative • Thyroglobulin < 2 ng/m. L (undetectable)
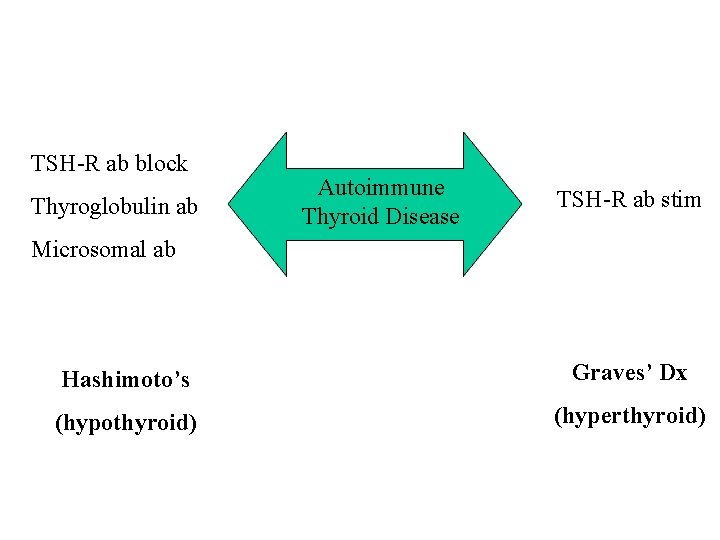
TSH-R ab block Thyroglobulin ab Autoimmune Thyroid Disease TSH-R ab stim Microsomal ab Hashimoto’s Graves’ Dx (hypothyroid) (hyperthyroid)

Thyroid Antibodies • Hashimoto’s • Thyroglobulin AB (<40 KIU/L) • Thyroid peroxidase AB (< 35 KIU/L) • Grave’s • • TSI or TSH Receptor Ab (Stim): Ig. G antibody SEN 60% SPEC 90% 2 -3 month turn-around time Indications: » Pregnant & present or past hx Grave’s: check 2 nd trimester (if hi-titre > 5 X normal needs PTU as TSI crosses placenta) » ? Euthyroid Grave’s ophthalmopathy » Alternating hyper/hypo function due to alternating Stim/Block TSI

Thyroglobulin (Tg) • • Normal < 40 ng/m. L Increased in all thyroid disease Thyrotoxicosis factitia: low or undetectable Tg Useful for thyroid cancer surveillance post surgery & radioiodine ablation • Not useful for thyroid cancer diagnosis • Thyroglobulin antibodies in Hashimoto’s patients may falsely elevate or decrease thyroglobulin levels
- Slides: 79