THYROID DISORDERS Hyperthyroidism Prepared by Stephanie N Ammari

THYROID DISORDERS Hyperthyroidism Prepared by : Stephanie N. Ammari Resources : Davidson , Medstudy
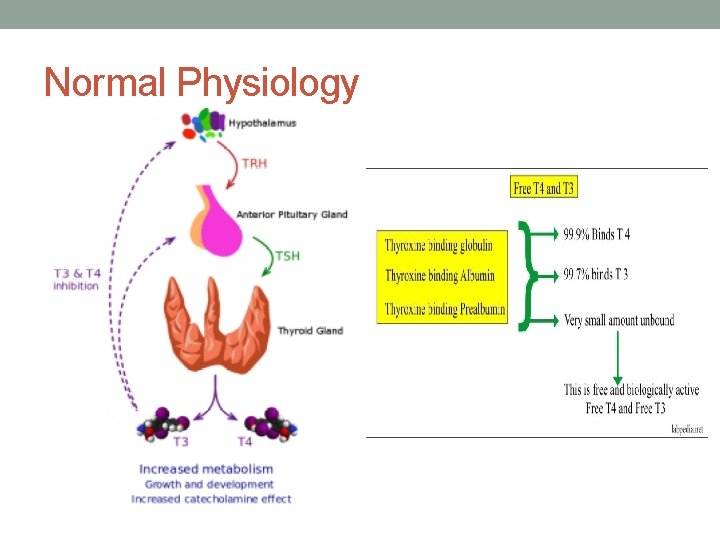
Normal Physiology

THYROID FUNCTION TESTS • TFTs include TSH, FT 4, and sometimes FT 3. • When screening for primary thyroid disease: start with a TSH to detect abnormalities of thyroid function (both hyper- and hypothyroidism). • If the TSH is high, then order a FT 4 to assess for hypothyroidism. • If the TSH is low, then order a FT 3 + FT 4 to assess for hyperthyroidism.
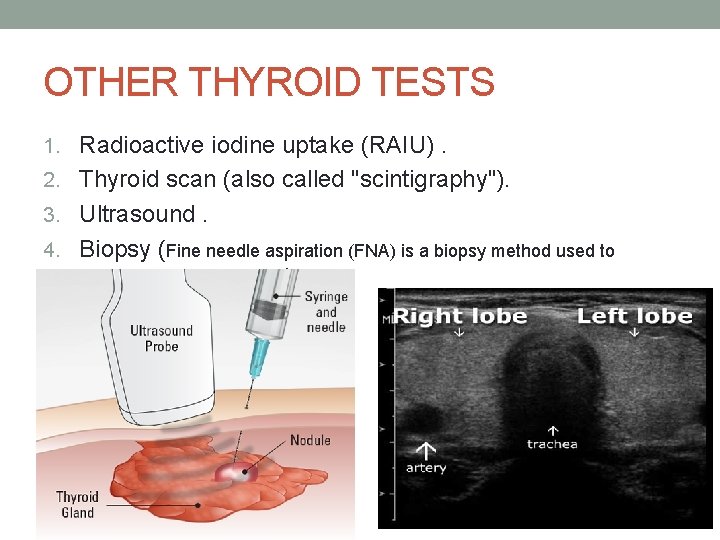
OTHER THYROID TESTS 1. Radioactive iodine uptake (RAIU). 2. Thyroid scan (also called "scintigraphy"). 3. Ultrasound. 4. Biopsy (Fine needle aspiration (FNA) is a biopsy method used to evaluate a thyroid nodule ).
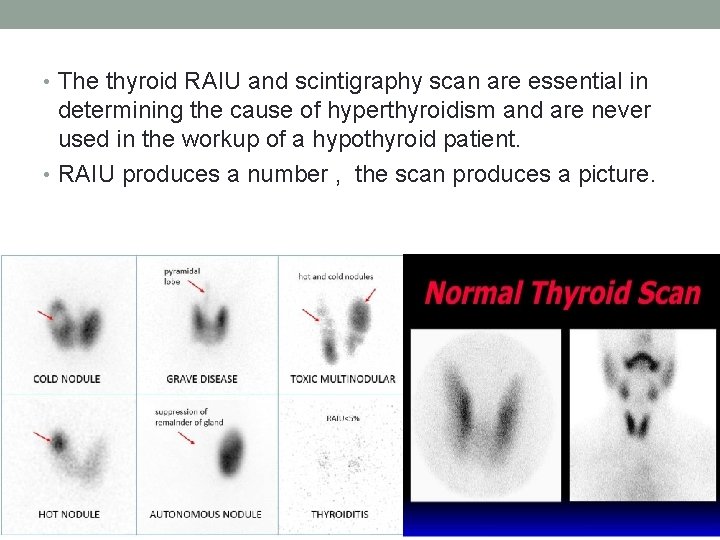
• The thyroid RAIU and scintigraphy scan are essential in determining the cause of hyperthyroidism and are never used in the workup of a hypothyroid patient. • RAIU produces a number , the scan produces a picture.

Hyperthyroidism ( thyrotoxicosis ) • The most common cause of hyperthyroidism is autoimmune Graves disease. Other causes : 1. toxic multinodular goiter (MNG) 2. toxic adenomas. 3. thyrotoxicosis due to chronic autoimmune thyroiditis (hashitoxicosis). • Transient illnesses not associated with long-term primary hyperthyroid disease : Subacute and postpartum thyroiditis.

Symptoms • Anxiety and restlessness • Irritability • Insomnia • Impaired concentration (even confusion or psychosis) • Weight loss despite normal diet • Diarrhea • Heat intolerance • Alopecia • Dyspnea • Menstrual irregularities (oligo- or amenorrhea, impaired fertility) • In males: gynecomastia, decreased libido, impaired spermatogenesis, and/or erectile dysfunction

Physical Exam • Warm skin. • The "hyperthyroid stare"( exophthalmos). • Lid-lag & lid retraction. • Hypertension. • Increased heart rate. • Atrial fibrillation or ectopy in up to 20% of patients (more common in elderly). • Thyroid Acropachy. • In Goiter : diffuse enlargement of thyroid gland

Graves Disease • The thyrotoxicosis results from the production of immunoglobulin G (Ig. G) antibodies directed against the TSH receptor on the thyroid follicular cell, which stimulate thyroid hormone production and proliferation of follicular cells, leading to goitre in the majority of patients. • These antibodies are termed thyroid-stimulating immunoglobulins or TSH receptor antibodies (TRAb) and can be detected in the serum of 80– 95% of patients with Graves’ disease.

Graves Disease • Graves’ disease has a strong genetic component. • Genomewide association studies have identified polymorphisms at the MHC, CTLA 4, PTPN 22, TSHR 1 and FCRL 3 loci as predisposing genetic variants. • A suggested trigger for the development of thyrotoxicosis in genetically susceptible individuals may be infection with viruses or bacteria.
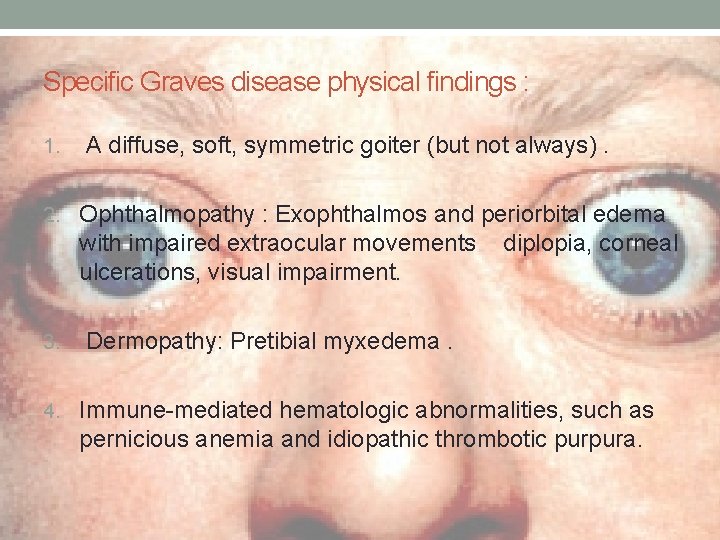
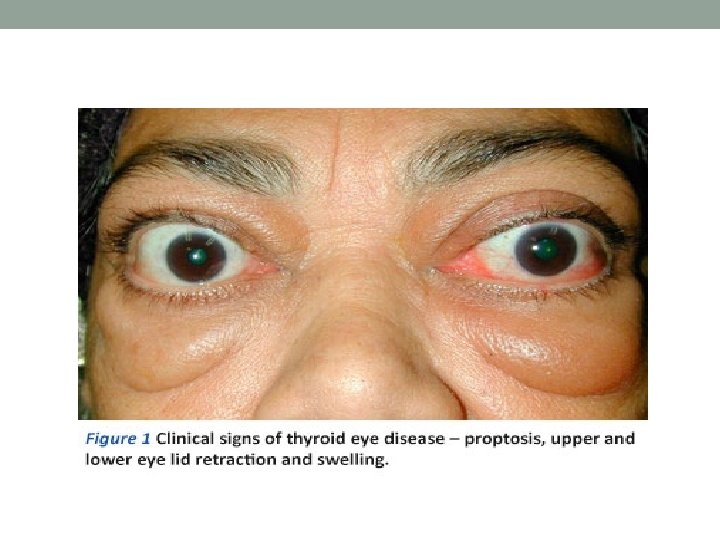
Specific Graves disease physical findings : 1. A diffuse, soft, symmetric goiter (but not always). 2. Ophthalmopathy : Exophthalmos and periorbital edema with impaired extraocular movements ulcerations, visual impairment. 3. diplopia, corneal Dermopathy: Pretibial myxedema. 4. Immune-mediated hematologic abnormalities, such as pernicious anemia and idiopathic thrombotic purpura.
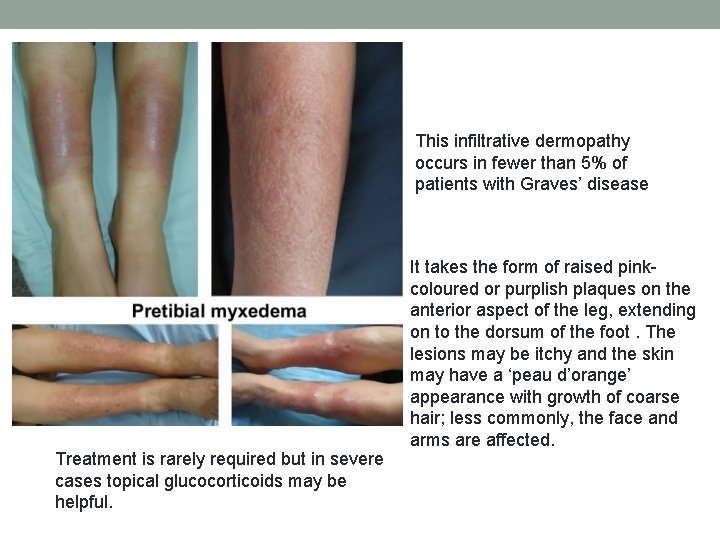
This infiltrative dermopathy occurs in fewer than 5% of patients with Graves’ disease Treatment is rarely required but in severe cases topical glucocorticoids may be helpful. It takes the form of raised pinkcoloured or purplish plaques on the anterior aspect of the leg, extending on to the dorsum of the foot. The lesions may be itchy and the skin may have a ‘peau d’orange’ appearance with growth of coarse hair; less commonly, the face and arms are affected.
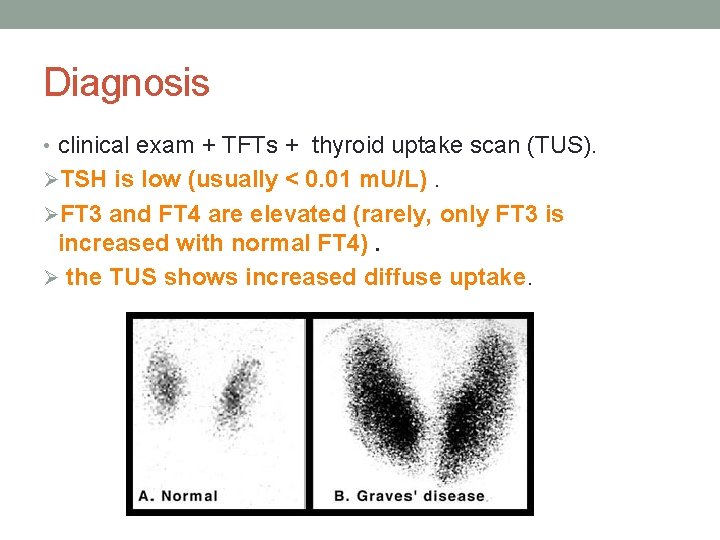
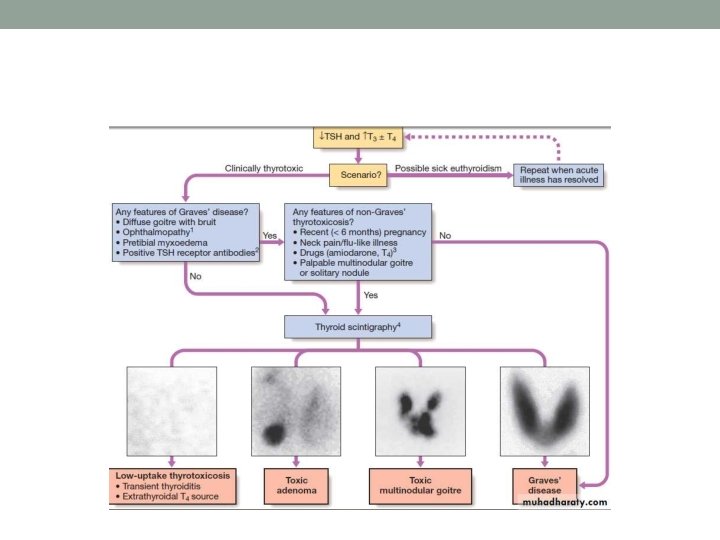
Diagnosis • clinical exam + TFTs + thyroid uptake scan (TUS). ØTSH is low (usually < 0. 01 m. U/L). ØFT 3 and FT 4 are elevated (rarely, only FT 3 is increased with normal FT 4). Ø the TUS shows increased diffuse uptake.

• Other common lab abnormalities: elevated alkaline phosphatase, hypercalcemia, and thrombocytopenia. • Autoantibodies are generally not measured, but TSI (thyroid-stimulating immunoglobulins) are positive in > 90% of cases of Graves disease.
![Treatment • Treat with antithyroid drugs (methimazole [MMI] or propylthiouracil [PTU]) and/or thyroid ablation Treatment • Treat with antithyroid drugs (methimazole [MMI] or propylthiouracil [PTU]) and/or thyroid ablation](http://slidetodoc.com/presentation_image_h2/6e98e9ae05c85014232938d37299811d/image-16.jpg)
Treatment • Treat with antithyroid drugs (methimazole [MMI] or propylthiouracil [PTU]) and/or thyroid ablation with ᶦᶟᶥ I or surgery.

Treatment • MMI is the preferred drug in non-pregnant patients because of lower toxicity than PTU. • PTU : üis still 1 st line treatment for Graves disease in pregnant patients in the 1 st trimester and is still used for thyroid storm. üPTU received a FDA boxed warning for increased risk of death due to acute liver failure or severe liver injury.

Treatment • The most serious side effects of PTU and MMI are hepatic toxicity and agranulocytosis, which are rare and unpredictable. • LFTs and CBCs do not require monitoring. • Check only if the patient becomes symptomatic (jaundice, dark urine, prolonged fever/sore throat). • Side effects almost always disappear when the drug is promptly discontinued. • Beta-blockers help patients with adrenergic symptoms while waiting on the effects of PTU or MMI.

Treatment Thyroid ablation using ᶦᶟᶦ I. ØVirtually all patients are pretreated with beta-blockers, and many patients are treated with MMI (or PTU) prior to radioiodine ablation. ØMost patients become hypothyroid months to years after ᶦᶟᶦ I therapy.

Surgery may be indicated in : 1. pregnancy. 2. in patients with an associated cold nodule or relapse after radiation. 3. in some young patients with a large goiter. # Worrisome complications of surgery are loss of all parathyroids and damage to recurrent laryngeal nerves.

Thyroid Storm • Storm is the 2 nd thyroid emergency that is associated with a high mortality rate (the other is myxedema coma). • Storm is most often a precipitated event in patients known or suspected to have undiagnosed or inadequately treated hyperthyroidism. • Precipitating events include surgery, infections, or an iodine load, such as amiodarone or contrast dye.

Symptoms & Dx • Symptoms of storm are identical to symptoms of hyperthyroidism, only more exaggerated: Hypertension – tachycardia- congestive heart failure –fever – psychosis or delirium. Some patients have constitutional symptoms of nausea, vomiting, and diarrhea. Oddly, some patients develop jaundice • Diagnose the condition with measurement of TSH and FT 4: In virtually all cases, TSH is immeasurable and FT 4 markedly increased.

Thyroid storm • Storm is characterized by a severe level of metabolic stress that the patient can no longer tolerate. • This severe stress results in a relative adrenal insufficiency, even though the adrenal glands may be functioning perfectly and secreting a large amount of cortisol. • Patients in storm die from cardiovascular collapse.

Tx of Thyroid Storm v. The most important aspect of treatment is large amounts of glucocorticoids. v. Provide supportive care in the ICU with diligent attention to volume status, temperature, and heart rate. v. Give empiric broad-spectrum antimicrobial coverage until infection is excluded. v. Other aspects of treatment include the following: • Interrupt the physiologic response to excess thyroid hormone: IV propranolol or esmolol. • Block new hormone synthesis: high-dose thionamide (PTU or MMI). • Block release of preformed hormone from the gland: stable iodide. • Block peripheral conversion of T 4 to T 3 : iodinated contrast agent, propranolol, and corticosteroids. PTU also does this (but not MMI).

Thyroiditis # Thyroiditis is divided into the following categories: • Acute: caused by bacterial infection of the gland (rare). • Subacute: caused by viruses (also called "granulomatous"). • Chronic: Autoimmune-mediated disease is the most common cause (Hashimoto's). Painless and postpartum thyroiditis are considered variants of "chronic. "

Subacute (de Quervain’s) thyroiditis • Subacute thyroiditis is a transient inflammation of the thyroid • • • gland occurring after infection with Coxsackie, mumps or adenoviruses. The condition can also be precipitated by drugs, including interferon-α and lithium. Affected patients are usually females aged 20– 40 years. In its classical painful form, There is pain in the region of the thyroid that may radiate to the angle of the jaw and the ears, and is made worse by swallowing, coughing and movement of the neck. The thyroid is usually palpably enlarged and tender. Systemic upset is common. Painless transient thyroiditis can also occur after viral infection and in patients with underlying autoimmune disease.
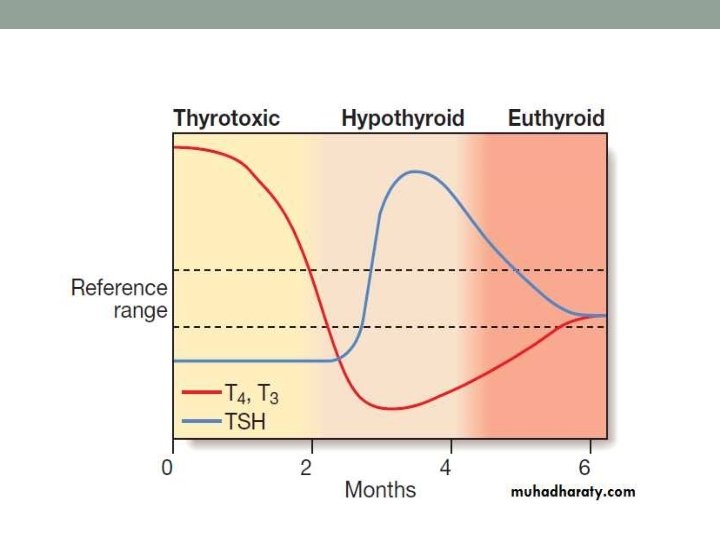

Subacute thyroiditis • Labs/studies: • Initially, T 3 and T 4 are increased, TSH is suppressed, and RAIU is initially decreased. • ESR is increased but is too nonspecific to use in diagnosis. • Over time, temporary overt hypothyroidism develops in some with low T 4 and increased TSH. • RAIU returns to normal. Eventually, T 4 and TSH normalize

Subacute thyroiditis • The disorder is self-limited and usually does not require treatment. • For severe cases, treat inflammation as needed with ASA or NSAIDs. • Glucocorticoids are given as an 8 -week taper in refractory/systemic cases. • Occasionally, a patient may need beta-blockers to ameliorate thyrotoxicosis symptoms or levothyroxine for overt hypothyroidism. • Reevaluate periodically until the patient's thyroid function normalizes.

Postpartum thyroiditis • is fairly common, affecting up to 10 -15% of postpartum women. • symptomatic thyrotoxicosis presenting for the first time within 12 • • • months of childbirth is likely to be due to post-partum thyroiditis The clinical course and treatment are similar to those of painless subacute thyroiditis. Patients present with hyper- or hypothyroid symptoms and a painless goiter. ESR is normal, but many patients do have anti-TPO antibodies. RAIU is decreased. Don't hesitate to treat the hypothyroidism-or to give beta-blockers as needed for thyrotoxicosis. Patients universally recover but need annual follow-up because of the risk of overt hypothyroidism later. Post-partum thyroiditis tends to recur after subsequent pregnancies, and eventually patients progress over a period of years to permanent hypothyroidism.

Toxic Adenoma • A toxic thyroid adenoma is a benign area of autonomous hyperfunctioning thyroid tissue. • Most occur as a single nodule of hyperfunctioning tissue within normal tissue that grows slowly, eventually becoming large enough to suppress TSH production. • These are usually diagnosed by TFTs, which demonstrate overproduction of FT/FT 4 and suppression of TSH, and thyroid scan (focal uptake in "hot" nodule).

Treatment of thyroid adenomas • If the patient is hyperthyroid, use ablative treatment or perform surgery. Antithyroid drugs do not work long term. • For the euthyroid patient with a thyroid adenoma …. If the thyroid adenoma is compressing underlying structures or is cosmetically problematic, surgery is the best treatment. Percutaneous ethanol injection of autonomous functioning thyroid nodules is an alternative to surgery and RAI, with restoration of normal thyroid function in the majority of cases.
Multinodular Goiter • Toxic MNG. • Nontoxic MNG.

Toxic MNG • refers to a MNG with thyrotoxicosis. • TSH is suppressed, and FT 3 and FT 4 are often increased. • The thyroid scan usually shows 1 or more hot nodules. • Toxic MNG may temporarily be treated with antithyroid medications. • Normal treatment is ablative therapy with radioactive iodine. This does not destroy all the nodules, but it does destroy those that are hyperfunctioning. • Surgery is used in cases that are refractory, or in symptomatic cases, especially if a large goiter is compressing surrounding structures.

Subclinical Hyperthyroidism • a low or undetectable (TSH) level with a normal serum free T 4 and normal serum total T 3 levels. • It can be caused by increased endogenous production of thyroid hormone (e. g. , in Graves disease, toxic nodular goiter, or transient thyroiditis), by administration of thyroid hormone to treat malignant thyroid disease, or by unintentional excessive replacement therapy. • The American Thyroid Association and the American Association of Clinical Endocrinologists recommend treating patients with thyroid- stimulating hormone levels less than 0. 1 m. IU per L if they are older than 65 years or have comorbidities such as heart disease or osteoporosis.
- Slides: 36