THYROID DISEASE THYROID GLAND Two lobes Situated in

THYROID DISEASE

THYROID GLAND • Two lobes • Situated in the lower neck • Synthesise, stores, release T 3 & T 4 (triiodothyronine & thyroxine) BIOSYNTHESIS • Dietary iodine Inorganic iodide • Iodide + Tyrosine Monoiodotyrosine • Monoiodotyrosine + Iodide Diiodotyrosine • A coupling reaction binds MIT & DIT T 3 & T 4
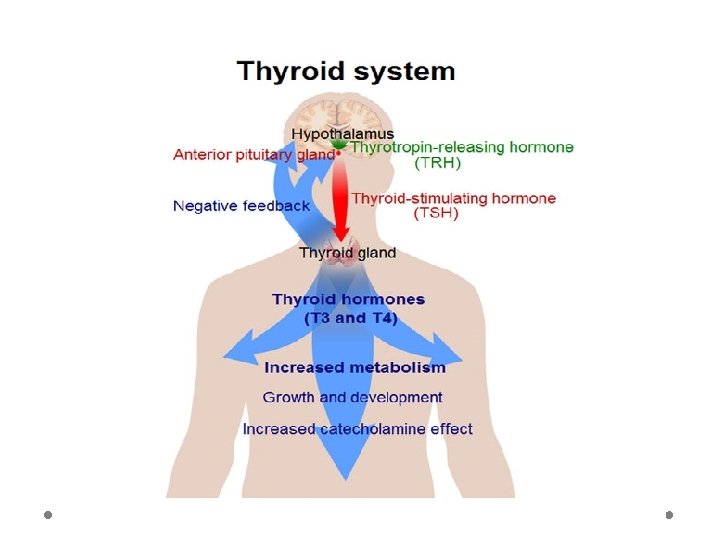
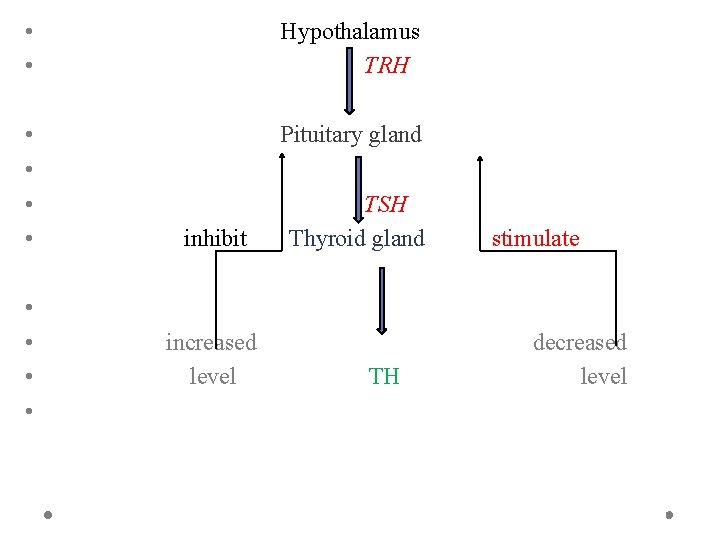
• • Hypothalamus TRH • • Pituitary gland • • inhibit increased level TSH Thyroid gland TH stimulate decreased level

• HORMONE TRANSPORT • TSH Stimulation Released to circulation T 3 & T 4 Cleaved from thyroglobulin • In circulation , TH Bound to plasma proteins Advantages ØProtect from premature metabolism and excretion. ØProlongs half life in circulation. ØReach its site of action. §Hormone is metabolized by deiodination.

HORMONE FUNCTION ØGrowth and development ØIncreasing rate of metabolism ØIncrease metabolic rate in CVS increases blood flow, cardiac output, heart rate. ØRegulating cerebral conduction in CNS ØSleep ØLipid metabolism

THYROID FUNCTIONS TEST ØSerum total thyroxine (TT 4) ØSerum total triiodothyronine (TT 3) ØResin triiodothyronine uptake (RT 3 U) ØSerum thyrotropin assays ØFree thyroxine index

Serum total thyroxine (TT 4) üTest indicating hormone availability to tissues üTotal (free & bound) T 4 is determined by radioimmunoassay. üDisease & condition interactions are possible üNormal range : 5 -12 mcg/d. L

Serum total triiodothyronine (TT 3) üMeasures total (free & bound) T 3 üUseful for early detection or to rule out hyperthyroidism üNot diagnostically significant for hypothyroidism üNormal range : 80 -180 ng/d. L

Resin triiodothyronine uptake (RT 3 U) üTest clarifies whether abnormal T 4 levels are the result of a thyroid disorder or abnormalities in the binding proteins. üEvaluate binding capacity of thyroxine binding globulin (TBG). üIf abnormalities in binding proteins underlie the abnormal levels of TH , TH level decreases with TBG level increases. üNormal range – 35 % to 45 %

üSeveral drugs can cause changes in the resin triiodothyronine uptake ØAsparaginase ØContraceptives ØOral corticosteroids ØEstrogens ØFluorouracil

Serum thyrotropin (TSH) assays üMost sensitive test for detecting the hypothyroid state üSlight decrease in TH level release more TSH üDone by immunoradiometric or immunometric (using monoclonal antibody) method. üUsed for diagnostic and monitoring purpose.

üControl over treatment (TSH < 0. 4 ml. U/L) üOver treatment may cause Øreduced bone density ØECG changes ØAtrial fibrillation ØLFT elevation

Free thyroxine index ØEstimation of the free T 4 level through a mathematical interpretation of the relationship between resin triiodothyronine uptake and T 4 levels. FTI = TT 4×RT 3 U/mean serum RT 3 U. ØNormal range – 5. 5 to 10. 5 ØElevated in hyperthyroidism.

THYROID DISEASE HYPOTHYROIDISM HYPERTHYROIDISM
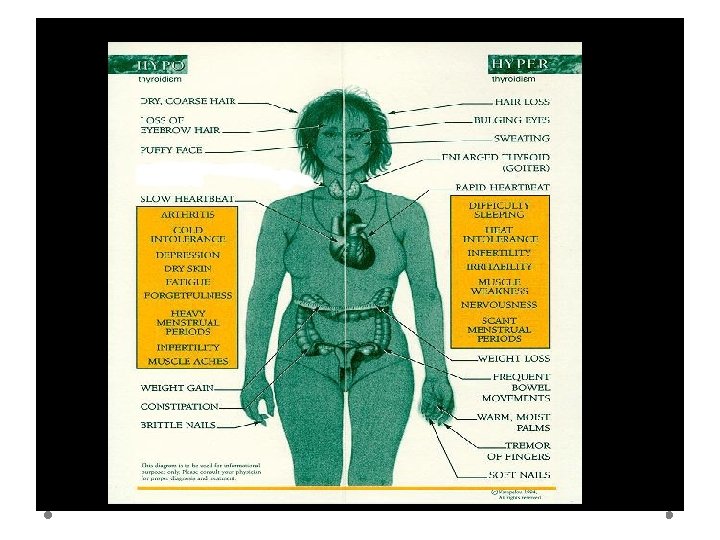
HYPOTHYROIDISM ØInability of thyroid gland to supply sufficient thyroid hormone. PRIMARY SECONDARY TYPES TERTIARY SUBCLINICAL

PRIMARY HYPOTHYROIDISM üResult of gland destruction or dysfunction caused by disease or medical therapies (e. g. Radiation or surgical procedure) üOr failure of the gland to develop or congenital incompetence (cretinism) SECONDARY HYPOTHYROIDISM ü Result of pituitary disorder that inhibits TSH secretion. So lack of appropriate stimulation. TERTIARY HYPOTHYROIDISM üDue to defect of hypothalamus to secrete TRH , to stimulate pituitary.

SUBCLINICAL HYPOTHYROIDISM üRefers to patient without clinical symptoms üNormal free thyroxine level and elevated TSH level. üTreatment not recommended.

CAUSES 1)Hashimoto thyroiditis üAutoimmune disorder üIn which the thyroid gland is gradually destroyed by a variety of cell - and antibody-mediated immune processes. 2) Treatment of hyperthyroidism ü over usage of antithyroid drugs

3)Goiter ENDEMIC • Due to inadequate dietary intake of iodine SPORADIC • Due to ingestion of drugs and foods containing progoitrin.
ØProgoitrin hydrolysis Goitrin (activated) Ø Goitrins inhibit oxidation of iodine to iodide. ØSo they decrease the TH production. Food & drugs containing Progoitrin Food Drug • Cabbage, Spinach, Mustard, Cauliflower, Peanuts etc. • Propylthiouracil, Phenylbutazone, Cobalt, Lithium etc.

SIGNS AND SYMPTOMS EARLY…………. ØLethargy ØFatigue ØForgetfulness ØUnexplained weight gain ØSensitivity to cold ØConstipation PROGRESSIVE……………. . ØDry, inelastic skin ØSlowed speech and thought ØPuffy face ØIf untreated – MYXEDEMA COMA

THERAPEUTIC AGENTS 1) Desiccated thyroid preparations Ø Prepared from beef and pork Ø Now not much used due to lack of bio equivalency with new agents. 2)Fixed-ratio liotrix preparations Ø Synthetic thyroid agent Ø Combination of T 3 & T 4 Ø Not considered drug of choice for replacement therapy because offers no therapeutic advantage over levothyroxine sodium and may result in excessive serum T 3 concentrations. Ø Adverse effects (T 3) includes tremor, headache, palpitations etc

3) Levothyroxine (levothroid, synthroid, levoxyl) ØAgent of choice. ØPredictable result & lack T 3 induced side effects. ØAverage adult maintenance dose is 75 -150 µg/day Precautions and monitoring ØElderly patient and patient with cardiac disease – begin therapy with low dose (25 µg/day) ØGradually increase the dose – usually <100µg/day ØPossibility of cardiac complications (angina , palpitations, arrhythmias) ØMonitor sensitive TSH test , T 4 levels. ØLong term therapy can cause thyrotoxicosis (T 4).

• • 1) 2) 3) Accelerate bone loss Drug interactions Cholestyramine & colestipol – 6 hr gap is needed Calcium carbonate Estrogens & selective estrogen receptor modulators – reduce the free T 4 levels & TSH levels. 4) Raloxifene – malabsorption 5) Ciprofloxacin

MYXEDEMA COMA Ø Life threatening complication with high mortality rate. Ø Most common in – preexisting or under diagnosed hypothyroidism. Ø ü ü ü Predisposing factors includes……. Alcohol, sedative, or narcotic use Over use of antithyroid drug Sudden discontinuation of TH therapy. Infections Exposure to cold Radiation therapy etc.

Complications üComa üHypothermia üRespiratory failure üHypo metabolism Electrolyte imbalance üCardiac effects – decrease heart rate , cardiac output. TREATMENT ØRapid restoration of T 3 & T 4 levels to normal ØA loading dose of levothyroxine 400 -500µg given as IV bolus. ØLiothyronone 25µg orally every 6 hr ØContinued till improvement noted.

HYPERTHYROIDISM §Thyrotoxicosis §Over activity of thyroid gland GRAVES DISEASE (Diffuse toxic goiter) üMost common form üAutoimmune disorder – antibodies bind to and activate TSH receptor------over production of TH Signs and symptoms ØEnlarged goiter ØAnxiety, insomnia, irritability ØTremor and muscle weakness

ØStare, Exophthalmos ØHeat intolerance ØPalpitations, tachycardia ØWeight loss ØPeriorbital edema PLUMMER DISEASE (Toxic nodular goiter) üLess common üIncidence is highest in patients <50 years of age Signs & symptoms üSame as for Graves disease with nodular masses üCardiac abnormalities – CHF, tachyarrhythmias

JODBASEDOW PHENOMENON ØOver production of thyroid hormone following a sudden , large increase in iodine ingestion ØOr by introduction of iodide or iodine in contrast agents or drugs (amioderone). FACTITIOUS HYPERTHYROIDISM ØAbusive ingestion of thyroid replacement agents to lose weight ØDiagnosis is aided by ………………. üAbsence of glandular swelling, exophthalmos üLack of autoimmune activity (Graves disease)

TREATMENT BETA BLOCKERS ØPropranolol ØReduce peripheral manifestations like tachycardia, sweating, tremor, nervousness etc. ØAlso inhibit peripheral conversion of T 4 to T 3 ANTITHYROID AGENTS 1)Propylthiouracil 2)Methimazole ØDirect interfere with thyroid hormone synthesis. ØInhibit iodine oxidation and coupling

PROPYLTHIOURACIL ØFor adults the initial dose is 300 -450 µg/day as tid ØAdult with severe disease require 600 -1200 µg/day initially. ØInitial dose is continued for about 2 months , then a maintenance Ø dose of 100 -150 µg/day is given as od or bd up to 1 year. ØThen gradually discontinued over 1 -2 months

METHIMAZOLE ØInitial dose range is 5 -60 µg/day as tid ØAfter 2 month of therapy a maintenance dose of 5 -30 µg/day is initiated, continued up to 1 year and gradually discontinued over 1 -2 months PRECAUTIONS & MONITORING ØSerum thyroid levels & free thyroxine index should be monitored. ØAdverse effects includes……. üDermatologic reactions – rash, urticaria, pruritus, hair loss, skin pigmentation üHeadache, drowsiness, nausea, vomiting, vertigo, loss of taste, myalgia, joint pain etc.

Ø ü ü ü Serious adverse effects includes……. Hematological abnormalities Drug fever Hepatitis
RADIO ACTIVE IODINE ØThyroid gland picks up iodine-131 ØThis treatment takes advantage of the fact that thyroid cells are the only cells in the body which have the ability to absorb iodine ØBy giving a radioactive form of iodine, the thyroid cells which absorb it will be damaged or killed. ADVANTAGES 1. High cure rate 2. Avoid surgical risk 3. Less expensive

DISADVANTAGES 1. Risk of delayed hypothyroidism (excessive cell death). 2. Genetic damage DOSAGE ØA dose of 80 -100 m. Ci of iodine 131/estimated gram of thyroid gland recommended. PRECAUTIONS & MONITORING üGenerally reserved for patients past the child bearing years. üMonitored for early recurrent of hyperthyroidism and later for hypothyroidism.

SURGERY ØSubtotal thyroidectomy ØIf drug therapy fails or radioactive iodine is undesirable ØRapid cure ØSuccess rate is high ØDifficult procedure & complications

THYROID STORM Ø Ø Ø ü ü Ø Sudden exacerbation of hyperthyroidism Rapid release of thyroid hormone Fatal, if not treated Leads to dehydration, shock and death Precipitating factors includes Thyroid trauma Surgery Radio active iodine Infection and sudden stopping of antithyroid therapy TT 4 level – 25 -30 µg/d. L (Normal 5 -12 µg/d. L)

ØFever, tachycardia, restlessness, tremor TREATMENT ØPropylthiouracil – 150 -250 µg orally Q 6 H ØBlock peripheral T 4 T 3 ØMethimazole – 15 mg orally Q 6 H (if necessary) ØPropranolol – 20 -200 mg orally Q 6 H or 1 -3 mg iv Q 4 -6 H (unless contraindicated) ØPotassium iodide – 50 -100 mg Q 12 H (minimize intrathyroidal iodine uptake) ØSupportive therapy – rest, rehydration, cooling, sedation etc.

REFERENCES q Textbook Of Therapeutics – Drug And Disease management ; 8 th edition – Eric T. Herfindal q Pharmacotherapy- A Pathophysiologic Approach ; 7 th edition - Joseph T. Dipiro Clinical Pharmacy and Therapeutics ; 4 th edition Roger Walker and Cate whittlesea Comprehensive Pharmacy Review ; 7 th edition Leon Shargel Essentials of medical Pharmacology ; 6 th edition K DTripathi

Thank you
- Slides: 42