Thrombotic complications in pediatric patients 16 Acute otitis

Thrombotic complications in pediatric patients






16 בן Acute otitis media Mastoiditis Viral meningitis Inflammatory bowel disease Common variable immunodeficiency sigmoid sinus thrombosis : CT • •

Thrombotic events in children • Age-related features • Adults guidelines not optimal for children

• Presentation may be more extensive • Over 50% of events: in upper venous system, secondary to central venous lines (CVLs) • More unusual locations • Essentially in all children: severe underlying disorders.

5. Different underlying pathology (for example, Congenital Heart Disease) 6. Patients with homozygous Protein S or Protein C deficiency present at birth with purpura fulminans, entity essentially unknown in adult population. 7. Hemostatic system of the young differs from the adult.

Incidence of thrombotic complications in children appear to be increasing: • Unlike venous thromboembolism in adults, VTE in children is usually a complication of a primary illness or therapy. • As survival rates for major childhood illnesses such as CHD and cancer improve, the incidence of VTE is increasing dramatically.

Risk factors: Multiple in the majority of patients.

: Age distribution Two age groups together account for approximately 70% of thrombosis: Early infancy: • Risk approximately 40 times greater than in any other age during childhood: • Small vesell diameter, high hematocrit, immature hemostatic system with decrease reserve capacity to insults.

Around puberty, late teenage years: • Hormonal changes • Oral contraceptives • Pregnancy

Venous thromboembolism From the data in the literature: • 4% idiopathic • 12% only one risk factor • 84% two or more risk factors
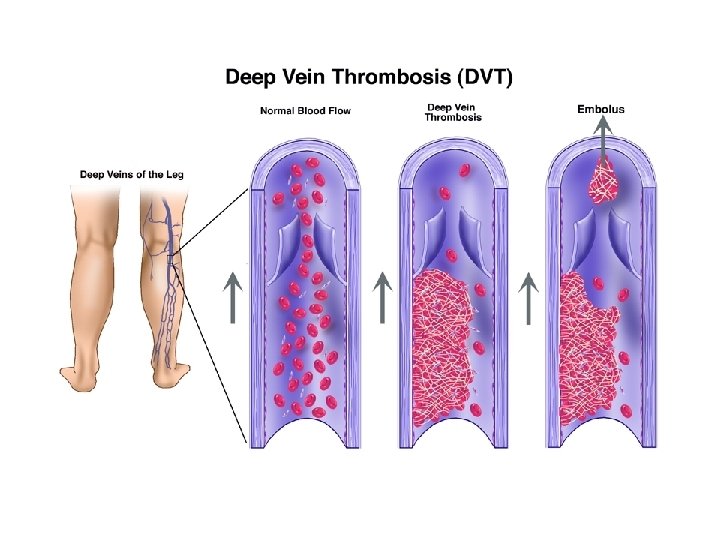

• Upper limb DVT more frequently associated with CVLs. • Long term parenteral nutrition using CVL: high risk situation • Gold standard for diagnosis: venography • CVL’s predispose to thrombosis by introducing foreign surface, damaging the endothelium, disturbing blood flow, content of fluid infusions)

(. Central Venous lines (cont • Leading cause of thromboembolic disease in children. • Incidence underestimated, perhaps because of different diagnostic modalities. • Symptoms: Catheter malfunction, requirement of local thrombolytic therapy to restore patency, recurrent sepsis, multiple CVL replacements, development of superficial collaterals, swelling, pain.

: Consecuences NOT TRIVIAL • Can lead to repeat anesthesia for CVL replacement • Lethal Pulmonary embolism • Superior Vena Cava Syndrome • Chylothorax

: Long term problems • Postphlebitic syndrome • Recurrent thrombosis • Side effects of long-term anticoagulants Canadian registry of 525 children: Death from untreated thrombosis: 2. 9% Recurrent thromboembolic disease: 3. 3% Postphlebitic syndrome: 12. 8% Urgent need to develop safe strategies for preventing CVL-related thrombosis

Right atrial thrombosis • Children tend to be young • CVL’s present in over 80% of cases • Most common underlying disease: CHD • Patients may be asymptomatic • Diagnosis: on routine echocardiography or present with CVL malfunction, sepsis, CHF

Paradoxical emboli VTE can also present as stroke with paradoxical emboli (in children with right-to-left shunt)
Cerebral vein thrombosis Largest group of affected children: • Newborns within 1 st month of life • Most common symptoms: headache, seizures, lethargy, intermittent hyper-excitability. • Most common underlying disorders: Cardiac disease, thrombophilia • Diagnostic test of choice: MRI / MRV






Thrombotic complications in ALL: • Disease process itself • L-Asparaginase • Effect of other chemotherapeutic agents

Congenital / acquired Cardiac disease Cardiac catheterization risk of at least 40% in small children if heparin is not used. Mechanical prosthetic valves • Considerable risk. • Require lifelong anticoagulation Cardiomyopathies

ARTERIAL THROMBOEMBOLIC DISEASE 1. 2. 3. 4. 5. 6. Kawasaki’s disease Surgery Arterial catheters Takayasu’s arteritis Arterial occlusion of transplanted organs CNS arterial thromboembolic events

CNS arterial thromboembolic events • CT-MRI have greatly facilitated diagnosis • Incidence of ischemic stroke: 0. 063 – 1. 2 per 10, 000 children per year. • Thirty percent 1 st month of life • Predisposing disorders: sickle cell anemia CHF prematurity leukemia

Clinically: • Infarcts in utero • Newborns: lethargy, seizures, rarely focal neurological deficit appreciable. • Older children: may present with hemiparesis, with or without seizures. • TIA’s not unusual. • MRI / MRA: diagnostic test of choice.


Kawasaki’s disease • • • Fever Lymphadenopathy Conjunctivitis Mucositis Rash Incidence of aneurysms and / or thrombosed coronary arteries: 15 -30% • Two percent die from rupture of coronary arteries or AMI.

Surgery: • Procedures for CHD (Fontan operation) Arterial catheters: • Placed for diagnostic, therapeutic and monitoring purposes, most common cause in pediatric patients. Arterial occlusion of transplanted organs: • Small children: hepatic, renal arteries.

Takayasu’s arteritis • Rare chronic, idiopathic, inflammatory disease of large arteries, predominantly affecting asian females. • Clinical presentation: limb or organ ischemia due to gradual stenosis of related arteries. • Diagnosis: angiography. Aortic lesions in 2/3 (aortic arch, carotids, renal arteries primarily affected).

Other predisposing risk factors: Nephrotic syndrome • Incidence of thrombosis: 4 -28% Surgery / Trauma • In contrast to adults, surgical procedures in children usually no significant risk, even in the presence of prothrombotic disorder. • Following puberty, risk begins to increase.

• Pediatric patients with thromboembolic complications should be investigated for a congenital and/or acquired prothrombotic state, regardless of the presence of acquired risk factors. • Family history – Investigation of parents • All results should be compared to ageappropriate reference ranges.

: Hypercoagulable states • Collection of clinical conditions that shift the balance between the pro and the anticoagulant forces in favor of coagulation. • • Virchow triad- Risk factors for thrombogenesis: Vessel wall Disturbances in blood flow Changes in constituents of blood
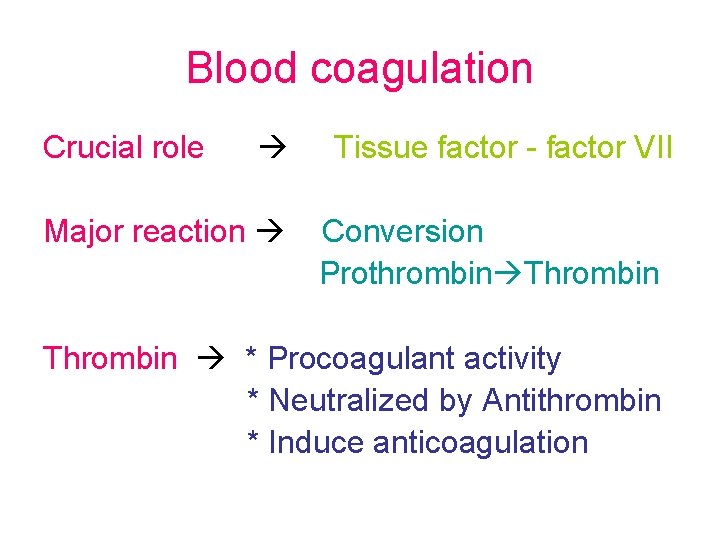
Blood coagulation Crucial role Major reaction Tissue factor - factor VII Conversion Prothrombin Thrombin * Procoagulant activity * Neutralized by Antithrombin * Induce anticoagulation

Thrombotic process • Thrombi may form in any part of the cardiovascular system (veins, arteries, heart, microcirculation) • Complications of thrombosis: -effects of local obstruction of the vessel -distant embolization -consumption of hemostatic elements (less often).

Arterial thrombi: under conditions of high flow, composed mainly of platelets aggregation bound together by fibrin strands. Venous thrombi: in areas of stasis. Composed of red cells with large amounts of interspersed fibrin and fewer platelets.

Pathogenesis of thrombosis Breakdown in the balance between thrombogenic factors and protective mechanisms.


Thrombotic disorders Patients clinically suspected can be divided in 2 categories: • Inherited • Acquired Heterogeneous group of diseases with increased risk of thrombotic complications.

Suspicion of underlying thrombophilia: • Unexplained thrombosis in younger than 40 -45 years of age. • Recurrent thromboembolic event. • Thrombosis of visceral, cerebral or cutaneous vessel. • Positive family history. • Thrombosis in unusual sites.

Risk factors for thrombosis (1) Acquired: Surgery Trauma Immovilization Increasing age Malignancy Nephrotic Syndrome

Risk factors for thrombosis (2) • • • Antiphospholipid antibodies Hyperhomocysteinemia Previous thrombotic event Pregnancy – Puerperium Oral contraceptives Drugs (L-Asparaginase) Myeloproliferative disorders Paroxysmal Nocturnal Hemoglobinuria Hormonal replacement therapy

Inherited risk factors (1) Common: • Factor V Leiden • Prothrombin 20210 • Elevated levels of coagulation factors (II, VIII, IX, XI)

Inherited risk factors (2) Rare: Antithrombin Protein S Protein C

Inherited risk factors (3) Very rare: Dysfibrinogenemia Homocystinuria

Inherited risk factors (3) Other: Plasminogen deficiency Thrombomodulin mutations


Thrombophilia studies-2006 (1) Hematology (Coagulation) laboratory: • Blood count + peripheral blood smear • PT-PTT • Fibrinogen • Thrombin time • Lupus anticoagulant • APC-R • Antithrombin • Protein S • Protein C • Factor IX • Factor VIII • Factor XI

Thrombophilia studies (2) Hematology (Molecular Biology) laboratory • Factor V Leiden • Prothrombin 20210 • MTHFR mutation

Thrombophilia studies (3) Immunology laboratory • Anticardiolipine Ab Ig. M-Ig. G • Anti β 2 Glycoprotein 1 Ig. M-Ig. G • Antinuclear Ab - Anti DNA

Thrombophilia studies (4) Biochemistry laboratory • Homocysteine


- Slides: 61